Abstract
The tumour microenvironment regulates tumour progression and the spread of cancer in the body. Targeting the stromal cells that surround cancer cells could, therefore, improve the effectiveness of existing cancer treatments. Here, we show that magnetic nanoparticle clusters encapsulated inside a liposome can, under the influence of an external magnet, target both the tumour and its microenvironment. We use the outstanding T2 contrast properties (r2 = 573–1,286 s−1 mM−1) of these ferri-liposomes, which are ∼95 nm in diameter, to non-invasively monitor drug delivery in vivo. We also visualize the targeting of the tumour microenvironment by the drug-loaded ferri-liposomes and the uptake of a model probe by cells. Furthermore, we used the ferri-liposomes to deliver a cathepsin protease inhibitor to a mammary tumour and its microenvironment in a mouse, which substantially reduced the size of the tumour compared with systemic delivery of the same drug.
Similar content being viewed by others
Main
Cancer is the second leading cause of death after cardiovascular diseases in developed countries. Despite rapid developments in medicinal and pharmaceutical chemistry, chemotherapy is still a major challenge. In the last decade, the development of effective targeted drug delivery systems for treating cancer has been a top priority in biomedical technology. However, although there have been methodological advances, stromal tumour components (termed the tumour microenvironment1) are generally not included in the treatment area. Recently, the tumour-cell-centred view of the metastatic process has been revised, and research regarding crosstalk between tumour cells and their surrounding tissue supports the notion that the microenvironment determines tumour progression at least as much as the tumour cells2. Thus, targeting the stromal cells that constitute an integral part of the cancer is a strategy that could greatly increase the effectiveness of traditional anticancer treatments. The tumour microenvironment includes many diverse components, including extracellular matrix components and various stroma cells, so active targeting mediated by a specific ligand is not possible. An effective delivery system that will target both tumours and their stromal components remains to be developed3.
Magnetic drug targeting, using magnetic nanoparticles and an external magnetic field focused on the target tissue, has already been described as a promising approach for the specific delivery of therapeutic agents4,5,6,7,8,9. Moreover, magnetic nanoparticles have recently gained additional attention because of their potential as contrast agents for noninvasive magnetic resonance (MR) imaging (MRI)10,11,12,13,14,15. Two types of MR contrast agents are used to enhance the visualization of properties correlated with patient anatomy and physiology: T1 contrast agents that shorten the spin–lattice relaxation time of nearby protons, and T2 contrast agents that enhance spin–spin relaxation to reduce the signal of media-containing structures. Currently, the most prominent T2 contrast agents are based on super-paramagnetic iron oxide nanoparticles, which, in contrast to the T1 contrast agents, remain intravascular for a longer time, enabling a longer image-acquisition time window.
We have developed a universal lipidated magnetic nanocarrier (called a ferri-liposome) that has enhanced MRI contrast properties and is effectively taken up by tumours and their stromal components. Chemical compounds within the ferri-liposomes are successfully released when administered in vivo and can be visualized at tissue and cellular levels.
Development and characterization of ferri-liposomes
Ferrimagnetic iron oxide (magnetite, Fe3O4; FMIO) nanoparticles were prepared by mechanochemical synthesis using saline crystal hydrates16. The use of saline crystal hydrates instead of conventional methods using anhydrous salts changes the solid-phase mechanism to a soft mechanochemical synthesis in aqueous media, resulting in a significantly increased reaction rate. This modification also results in ultrasmall spherical particles with diameters of 3–14 nm (>70% of particles were less than 8 nm; Fig. 1a,b).
Schematic on the left corresponds to the experimental data on the right. a, Transmission electron micrographs of FMIO nanoparticles. Inset: corresponding electron diffraction pattern. b, Size distribution of FMIO nanoparticles (average size, D = 6.65 nm). c, Field-emission gun scanning electron microscopy of the aqueous colloidal system of FMIO nanoparticles. d, DLS measurement of FMIO colloidal dispersion showing the distribution of diameters of the nanoparticle clusters and their average size (D = 56.56 nm). e, AFM image of liposome-encapsulated FMIO nanoparticles (ferri-liposome). f, Liposome size as determined by DLS (average size, D = 92.3 nm).
The main limiting factor in using magnetic nanoparticles in vivo is their low colloidal stability. Therefore, to prevent their agglomeration, we developed an optimized two-step procedure for preparing a biocompatible aqueous colloidal system from powdered FMIO nanoparticles, leading to a narrower particle size distribution of nanoclusters (Fig. 1c; see Supplementary Methods). The concentration of FMIO nanoparticles was measured by flame atomic absorption spectrometry, and the unit average size of nanoparticles was determined by dynamic light scattering (DLS) (Fig. 1d). The resulting FMIO nanoparticles had a negative surface zeta potential of 27.9 ± 4.3 mV at pH 7.4 and 37 °C. In addition, their suspension exhibited high colloidal stability under physiological conditions as well as at other pH values and ionic strengths (Supplementary Fig. S1).
Magnetic nanoparticles encapsulated within a phospholipid bilayer, forming liposomes, have been reported to have considerable structural and pharmacokinetic advantages for drug delivery11,17,18. Owing to their ability to encapsulate both hydrophobic and hydrophilic therapeutics, they prevent local dilution of the drug and limit its interaction with the surrounding environment, enabling reduction of the therapeutic dose and toxicity. In the present work, stabilized FMIO nanoparticles were encapsulated in sterically stabilized polyethylene glycol (PEG)-coated liposomes (PEGylated, Stealth Liposomes), forming ferri-liposomes with a diameter of 100 nm. Modification of the liposome surface with PEG is known to greatly reduce the opsonization of liposomes and their subsequent clearance by the reticuloendothelial (mononuclear-phagocyte) system11,19,20,21, resulting in a substantially prolonged circulation half-life. This was confirmed in a cellular experiment (Supplementary Fig. S2). The liposomes loaded with FMIO particles appeared, under atomic force microscopy (AFM), as spheroids with diameters of 0.09–0.11 µm (Fig. 1e), consistent with the average diameter of 92.3 nm measured for ferri-liposomes using DLS (Fig. 1f). Because of their size, hydrophobic and hydrophilic character and biocompatibility, together with their internal hollow space (Supplementary Fig. S3), the system of ferri-liposomes enables simultaneous encapsulation of FMIO nanoparticles with other substances such as pharmaceutical drugs or DNA, and their subsequent targeted delivery in an organism.
MR contrast properties of FMIO nanoparticles
The MR contrast properties of the stabilized FMIO nanoparticles were evaluated in vitro using 1% agarose phantoms (T2 ≈ 80 ms), which simulate tumour tissue22. The phantoms contained two types of FMIO nanoparticles with mean hydrodynamic diameters of 39 nm and 57 nm, respectively. The longitudinal (T1) and transverse (T2) relaxation times were measured at different concentrations of FMIO nanoparticles, and the relaxivities were determined to be r1 = 12 s−1 mM−1 and r2 = 573 s−1 mM−1 for the 39 nm nanoparticles and r1 = 31 s−1 mM−1 and r2 = 1,286 s−1 mM−1 for the 57 nm nanoparticles (Fig. 2a). FMIO nanoparticles showed several-fold higher relaxivities than commercially available super-paramagnetic iron oxide nanoparticles (Feridex, Bayer HealthCare Pharmaceuticals)23 and the standard gadolinium-based T1 contrast agent Magnevist (Bayer HealthCare Pharmaceuticals) (Fig. 2a). Moreover, a 20–70% improvement in the r2 relaxivity was found when compared to the best iron oxide-based nanoparticles described in the literature24,25,26. The high r2 relaxivity may be due to clustering of the FMIO nanoparticles24,27,28, and this is further supported by the higher relaxivity observed for nanoparticles with a higher hydrodynamic diameter of clusters. These results show that FMIO nanoparticles are high-performance MRI contrast agents that enable highly sensitive T2-weighted MRI measurements.
a, Spin–lattice 1/T1 (left) and spin–spin 1/T2 (right) relaxation rates of 39 nm and 57 nm FMIO nanoparticles at different concentrations, compared to commercially available MR contrast agents (Ferridex17 and Magnevist). Relaxivity rates r1 and r2 were obtained by comparing the measured (symbols) and theoretical (lines) values. b, T1- and T2-weighted MR images of agarose phantoms at different concentrations of 39 nm and 57 nm FMIO nanoparticles. c, Schematic (left) and T2-weighted MR image (right) of four phantom-probes containing 1% agarose (samples 1 and 3), and 3.4 mM FMIO nanoparticles either injected into the centre of the 1% agarose gel (sample 2) or diffused into the 1% agarose in the presence of a magnetic field (sample 4). Bottom panel shows signal intensity profiles along lines i and ii. Sample 5 is a small probe containing a solution of CuSO4·H2O in the phantom.
To verify the effectiveness of the FMIO nanoparticles as positive T1 and negative T2 contrast agents, we obtained T1-weighted and T2-weighted images of the control phantom and of phantoms with 0.017 mM and 0.17 mM each of the 39 nm and 57 nm FMIO nanoparticles (Fig. 2b). The signal intensity of these phantoms was significantly diminished on the T2-weighted MR scans, whereas the same concentration of FMIO nanoparticles demonstrated enhanced MRI signal on the T1-weighted images compared to the control phantom (Fig. 2b). Hence, unique simultaneous T1 and T2 MR contrast properties of FMIO nanoparticles were demonstrated, enabling their use as single contrast agents for both T1- and T2-weighted MR scans, thereby enhancing the diagnostic properties of MR imaging. Moreover, the twofold higher sensitivity of the 57 nm FMIO nanoparticles relative to the smaller 39 nm nanoclusters in T2-weighted MR scans (Fig. 2b) suggests the former to be extremely effective contrast agents. However, in drug-delivery applications the smaller 39 nm nanoclusters, with their still superior contrast properties, are preferable.
To demonstrate the effectiveness of the suspension of magnetic nanoparticles on targeting and their MRI contrast properties, two techniques for delivering FMIO nanoparticles into the agarose phantoms were used: (i) direct injection of the FMIO nanoparticle solution with an 0.3 mm needle into the centre of the phantom (sample 2 in Fig. 2c) and (ii) application of the FMIO nanoparticle dispersion to the phantom surface by positioning the magnetic field (B = 0.33 T) at the bottom of the vial (sample 4 in Fig. 2c). The MRI signal intensity was compared with pure agarose phantoms (samples 1 and 3 in Fig. 2c) and normalized to a small probe containing a solution of CuSO4·H2O (sample 5 in Fig. 2c). As seen on the T2-weighted MR image and from the MR signal intensity profile (Fig. 2c), both delivery methods were effective, demonstrating a clear difference between the MR signal of the FMIO nanoparticles and the agarose phantom. Moreover, the MR signal of sample 4 disappeared completely, indicating successful penetration of the FMIO nanoparticles through the phantom matter as a result of targeting by an external magnetic field. Collectively, these results demonstrate that FMIO nanoparticles can be used for multifunctional targeted delivery, enabling simultaneous MR detection. In addition, the MRI contrast properties of FMIO nanoparticles remain the same after their encapsulation into the liposomes (Supplementary Fig. S4), supporting the use of ferri-liposomes in medical applications.
Ferri-liposome as MRI-visible drug delivery system in vivo
To establish the efficacy of the prepared ferri-liposomes for in vivo applications we used a genetically engineered mouse model of human breast cancer (MMTV-PyMT), resulting in a widespread transformation of the mammary epithelium and the development of multifocal mammary adenocarcinomas29. Ferri-liposomes were first demonstrated to be non-cytotoxic in mouse embryonic fibroblasts (MEFs) and primary mouse tumour cells (Supplementary Fig. S5). Possible adverse effects of FMIO nanoparticles were also evaluated in an acute toxicity experiment using rats. No significant differences in blood biochemistry or histopathological analysis were observed 7 and 12 days after administration between control animals and animals treated with 500 mg kg−1 FMIO nanoparticles (Supplementary Table S1 and Fig. S6). Having shown that the system was suitable for in vivo applications, ferri-liposomes were injected intraperitoneally into an MMTV-PyMT tumour-bearing mouse while a magnetic field was applied for 1 h to the first left inguinal mammary tumour. Tumour tissue with a high MR signal appears yellow-red on T2-weighted MR images (Fig. 3a), while FMIO nanoparticles delivered by ferri-liposomes appear as a dark area, 1 and 48 h post-injection (Fig. 3a, Supplementary Fig. S7), confirming their successful targeting to the tumour region and their apparent MRI contrast effect. Furthermore, as well as spreading through the tumour tissue, nanoparticles were detected in the tumour surroundings, the tumour microenvironment (Supplementary Fig. S7). This ability of ferri-liposomes could be of particular value for developing novel strategies to treat cancer, with the further advantage of the possibility of being regulated by a magnetic field (Supplementary Fig. S8). The effectiveness of the system was confirmed by intravenous administration of ferri-liposomes (Supplementary Fig. S9). Collectively, these results demonstrate both the efficacy of ferri-liposomes for magnetic field targeted drug delivery and the possibility of monitoring their distribution by non-invasive MRI technology.
a, T2-weighted MR images of an MMTV-PyMT transgenic mouse before and 1 h and 48 h after intraperitoneal injection of ferri-liposomes followed by 1 h of magnetic field application to the lower right tumour (white arrow). Inset: red rectangle shows the region of the MRI images. b, Fluorescence images of primary MMTV-PyMT tumour cells and MEFs incubated with Alexa Fluor 555-functionalized ferri-liposomes for 3 h at 37 °C. Scale bar, 20 µM. Data are representative of three separate experiments. c, Optical imaging of FVB.luctg/+;PyMTtg/+ mice that have been intraperitoneally administered with ferri-liposomes (FL) carrying D-luciferin in the presence (targeted FL) and absence (non-targeted FL) of magnet application. A high-intensity luciferase signal was detected only in the tumour region exposed to the magnet (black arrow). The scale is in photons s−1 sm−2 sr−1.
The intracellular delivery of targeted ferri-liposomes was validated in tumour and stromal cells using a fluorescent marker (Alexa Fluor 555) as a model drug. The Alexa Fluor 555- functionalized ferri-liposome suspension was incubated for 3 h with primary MMTV-PyMT tumour cells and MEFs. Fluorescence microscopy analysis revealed very efficient internalization of the Alexa Fluor 555 by both types of cells (Fig. 3b). Moreover, compartmentalization of fluorescent particles in intracellular vesicles of primary tumour cells and fibroblasts provides clear evidence for successful endocytosis of the ferri-liposome cargo. This carrier system therefore represents a promising candidate for targeted drug delivery into both the tumour and its microenvironment, enabling more effective cancer therapy.
To confirm the release of drug encapsulated in ferri-liposomes in vivo, we crossed MMTV-PyMT mice (PyMTtg/+) with the FVB/N mouse strain expressing firefly luciferase under the control of the ß-actin promoter (FVB.luctg/+)30. The resulting double transgenic mice (FVB.luctg/+;PyMTtg/+) develop breast tumours with simultaneous expression of luciferase throughout the body. Twenty four hours after administration and targeting of ferri-liposomes loaded with the luciferase substrate (D-luciferin) to the tumour, a luminescent signal was imaged exclusively in the tumour region exposed to the 0.33 T magnet (Fig. 3c), indicating effective release of the cargo from the targeted ferri-liposomes in vivo. The efficiency of the system was also confirmed by intravenous administration of ferri-liposomes (Supplementary Fig. S10). Furthermore, nanoparticles were successfully excreted from the body without any evident accumulation (Supplementary Fig. S11, S12), which fulfils another critical parameter for their in vivo application.
Ferri-liposome delivers cargo to inhibit tumour growth
Initial testing of the ferri-liposome system for targeted drug delivery was performed with a standard cancer chemotherapy drug, doxorubicin. Even a single-dose treatment with doxorubicin targeted by ferri-liposomes resulted in a 90% reduction of tumour volume two weeks after administration, compared with a 60% decrease obtained by standard doxorubicin administration (Supplementary Fig. S13). However, we aimed at a bigger challenge: to convert a compound known to be ineffective due to poor bioavailability into an effective one. For this purpose we selected JPM-565, a small-molecule broad-spectrum inhibitor of cysteine cathepsins31,32, which is very potent in treating pancreatic islet cell cancer in a mouse model33,34. However, due to its very poor bioavailability, JPM-565 is not effective in the MMTV-PyMT mouse breast cancer model35, but, through genetic ablation of several cathepsins, tumour progression in this breast cancer model can be attenuated36,37,38. There is increasing evidence that cysteine cathepsins contribute to tumour progression via several possible mechanisms, including activation of the extracellular proteolytic cascade(s), degradation of the extracellular matrix, and inactivation of adhesion molecules such as E-cadherin37,39. Their inhibition could therefore form a potent strategy for tumour treatment40. Moreover, the cysteine cathepsins participating in multiple stages of tumour progression37,38,41,42,43 originate largely from the cells of the microenvironment36,44,45, thereby offering the opportunity to simultaneously validate the novel concept of targeting the tumour microenvironment as well as the novel drug delivery system in order to improve cancer treatment.
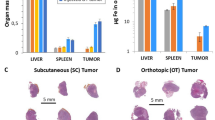
To overcome the limitations of the transgenic MMTV-PyMT mouse model having multifocal mammary tumours that are difficult to follow, and to secure the functional immune system (as compared to the xenograft approach), an orthotopically transplanted mouse mammary tumour model was developed by inoculating 5 × 105 primary MMTV-PyMT tumour cells into the mammary gland of a congenic immunocompetent recipient mouse (FVB/N mouse strain) (Fig. 4a). In contrast to the original transgenic model, the orthotopic transplanted model results in a single tumour that can be easily monitored due to the lower heterogeneity regarding tumour latency and growth, thus making it an ideal model for drug efficacy studies.
a, Schematic showing the treatment experiment design. Cells from the transgenic (Tg) MMTV-PyMT mouse with multifocal tumours were cultured and inoculated into an immunocompetent FVB/N mouse to form a model with a monofocal tumour that can be easily monitored. b, Table showing the treatment groups. Mice were treated with stabilizing buffer containing different compounds and magnetic targeting combinations as represented by the ‘ + ’ and ‘ − ’ signs. c, Tumour volumes for each treatment day for the different treatment groups. *P < 0.05, **P < 0.01 and **P < 0.001, compared with the other groups. d, Activity of cysteine cathepsins in tumour tissue after JPM-565 administration (NS, not significant). e, The percentage of Ki67+ cells as calculated by computer-assisted data analyses. Data are presented as means and standard errors, n = 5. Statistics were analysed using Student's t-test. NS, not significant. f, Fluorescent images of control tumours and tumours treated with JPM-565 targeted by ferri-liposomes (JPM + FLt). E-cadherin is stained green and nucleus is stained with Hoechst 33342 (blue). Higher-magnification images (right column) of white rectangles from the middle column illustrate the different patterns of E-cadherin localization. Scale bars, 100 µm and 25 µm (higher magnification images).
Starting with a tumour volume of 125 mm3, ferri-liposomes containing JPM-565 at a concentration of 100 mg kg−1 were injected intraperitoneally 10 times every second day with a magnetic field focused on the tumour (Fig. 4a). Tumour sizes were measured the day after each injection. At the end of treatment, tumours were excised and their volumes determined. The anti-tumour effect of non-loaded ferri-liposomes and different therapeutic modalities and forms of JPM-565 were compared (Fig. 4b). Mice treated with targeted JPM-565 loaded ferri-liposomes displayed a significant lag in tumour growth (as exemplified by the smaller tumours; Supplementary Fig S14) compared with all other groups (Fig. 4c), suggesting cathepsin inhibition was successful. This was confirmed by the substantial reduction of cysteine cathepsin activity measured exclusively in tumour samples from this group (Fig. 4d), which contrasts with the observation of no difference in cathepsin expression in all the groups (Supplementary Fig. S15). In agreement with previous studies33,35, a significant inhibition of cysteine cathepsins was observed in organs close to the peritoneum (Supplementary Fig. S16). Subsequent clearance from the peritoneum through the lymph nodes was also confirmed (Supplementary Fig. S17).
To address the role of cysteine cathepsins in tumour biological processes, we investigated the effect of cathepsin inhibition on tumour proliferation, vascularization and invasiveness. Cell proliferation was quantified by immunohistochemical detection of the proliferation marker Ki67, revealing a significant decrease in the proliferation rate of tumours treated with targeted JPM-565 compared to the other groups (Fig. 4e, Supplementary Fig. 18), corroborating reduced tumour growth in that cohort of mice. Based on the distribution of the endothelial cell marker CD31, no difference in vascularization of the tumour samples was observed following treatment (Supplementary Fig. 19). However, there was a trend for translocation of the cell-adhesion protein E-cadherin from the cytosol to the cell surface following treatment with targeted JPM-565 (Fig. 4f), resulting in decreased invasiveness and progression of the cancer.
To confirm the targeting of JPM-565 to the tumour, the treatment scheme was mimicked by loading ferri-liposomes with a fluorescent marker (Alexa Fluor 546). Evidently, these ferri-liposomes were successfully targeted to the tumour site, and uptake of their content by cells of the tumour microenvironment was clearly established (Fig. 5a,b). Moreover, we have demonstrated in vivo that the marker was compartmentalized in the intracellular vesicles of the tumour stroma cells (Fig. 5a, inset). The latter is of particular importance because cathepsins from tumour stroma are believed to play an important role in the processes leading to tumour progression.
a, Fluorescent images of tissues confirm the presence of intraperitoneally administered Alexa Fluor 546-functionalized ferri-liposomes (red) in the tumour microenvironment. Inset: higher-magnification image of an individual cell of the tumour stroma outlined by the white rectangle in the main panel. b, Haematoxylin and eosin staining of the corresponding section. Stromal (ST) and tumour (T) compartments of the tumour tissue are indicated, with their boundary demarcated by a dotted line. Scale bars in a and b, 200 µm and 20 µm (inset). c,d, Uptake of Alexa Fluor 555-functionalized ferri-liposomes (red) by both stroma (white arrows) and tumour cells (pink arrows), after double intravenous injection of ferri-liposomes. Tissues were co-stained with tumour-associated macrophages (CD206-FITC; green) in c and tumour cell marker (E-cadherin; green fluorescence) in d. Scale bars in c and d, 40 µm.
Although intraperitoneal administration of therapeutic agents is an important adjunct to surgery and systemic chemotherapy of cancer in selected patients46, we have evaluated the effectiveness of intravenous administration of our delivery system for targeting a tumour and its microenvironment in the MMTV-PyMT transgenic female mouse. The fluorescence of ferri-liposome cargo (Alexa Fluor 555) was found to be co-localized both with the stroma (Fig. 5c, CD206 marker for tumour-associated macrophages) and the tumour cells (Fig. 5d, epithelial marker E-cadherin) in the targeted PyMT tumour tissue. These results clearly demonstrate the potential applicability of the ferri-liposomes in a variety of therapeutic scenarios.
Conclusion
A new delivery platform for targeting both the tumour and its microenvironment, based on ferrimagnetic nanoclusters, has been developed. Ferri-liposomes were shown to act as a universal drug delivery system, confirmed by targeting of several chemically different types of cargo. Furthermore, based on the nanoparticles with superior MRI contrast properties, the ferri-liposome system could provide the non-invasive, real-time MRI strategy with unlimited depth penetration and significantly improved sensitivity. The combination of the favourable biodistribution of these nanoparticles to tumours and their microenvironments, as well as their prominent MRI properties, offers the exciting possibility of the simultaneous delivery and detection of therapeutic agents in vivo. The feasibility of this approach was confirmed in vivo by the use of the MR technique and fluorescent and bioluminescent markers, revealing ferri-liposomes to be highly promising candidates for cancer treatment. As such, the cathepsin inhibitor JPM-565 was targeted by ferri-liposomes to the peri-tumoral region of mouse breast cancer, resulting in a significant reduction in tumour growth. Overall, we believe that this multifunctional MRI-visible targeted delivery system based on FMIO nanoparticles with superior properties constitutes a major advance in the application of nanotechnologies in medicine, and has opened up new possibilities for the diagnosis and treatment of important human diseases such as cancer.
Methods
Preparation of ferri-liposomes
FMIO nanoparticles (magnetite, Fe3O4) were manufactured by mechanochemical synthesis using saline crystal hydrates as described16. Sodium chloride, as an inert component, was added in the ratio 1:2. The mixture was sealed by steel balls in a planetary mill, washed with distilled water and, optionally, dried in a laminar flow cabinet at room temperature. FMIO nanoparticles were suspended in a stabilizing buffer (20 mM sodium citrate buffer, pH 7.4, containing 108 mM NaCl, 10 mM HEPES), sonicated (Ultrasonic Disintegrator, Branson) and centrifuged to separate the remaining undisrupted agglomerates. The resulting stable colloidal dispersion of non-aggregating nanoparticle clusters was characterized using flame atomic absorption spectrometry (SpectrAA 110, Varian), DLS (using a PDDLS/BatchPlus System, Precision Detectors) and field-emission gun scanning electron microscopy (SEM) using an FE-SEM SUPRA 35VP (Carl Zeiss). The zeta potential of FMIO nanoparticles was measured by a PALS Zeta Potential Analyzer at pH 7.4 and 37 °C.
FMIO nanoparticle-loaded liposomes (ferri-liposomes) were prepared from 95% L-a-phosphatidylcholine (Avanti Lipids) and 5% 1,2-distearoyl-sn-glycero-3-phosphoethanolamine-N-[methoxy(polyethylene glycol)-2000] (Avanti Lipids), and purified (Supplementary Methods).
For ex vivo and in vivo studies, ferri-liposomes were functionalized with Alexa Fluor 546-labelled dextran (Invitrogen), non-conjugated Alexa Fluor 555 (Invitrogen), D-luciferin (Sigma) or JPM-565 (DTP, NCI) (Supplementary Methods).
In vitro and in vivo MRI
All MR experiments were performed on a TecMag Apollo MRI spectrometer with a superconducting 2.35 T horizontal bore magnet (Oxford Instruments), using a 25 mm saddle-shaped Bruker RF coil. Spin–lattice and spin–spin relaxation times (T1 and T2) were measured for different concentrations of FMIO nanoparticles in 1% agarose at room temperature, using inversion recovery and spin-echo techniques, respectively. The longitudinal (r1) and transverse (r2) relaxivities were calculated from ri = (1/Ti –1/Ti0)/c, where c is the concentration of FMIO nanoparticles in mM, Ti is the relaxation time at concentration c, Ti0 is the relaxation time of 1% agarose, and i = 1 and 2 for T1 and T2, respectively.
Two-dimensional MR images were taken using a standard multislice spin-echo pulse sequence with an echo time (TE) of 8.5 ms and a repetition time (TR) of 400 ms for T1-weighted MR images, and with TE = 60 ms and TR = 2,000 ms for T2-weighted MR images. The field of view was 40 mm, with an in-plane resolution of 156 µm and a slice thickness of 1 mm. For in vivo detection see Supplementary Fig. S7.
Assessment of ferri-liposome internalization ex vivo
Primary MMTV-PyMT cells and mouse embryonic fibroblasts (MEFs) were isolated (Supplementary Methods) and cultured with Alexa Fluor 555-functionalized ferri-liposomes in normal culture medium on Lab-Tek Chamber Slides (Nunc). After incubation for 3 h with nanoparticles, cells were washed with PBS, stained with Hoechst 33342 (Fluka) and examined with an Olympus fluorescence microscope (Olympus IX 81) with Imaging Software for Life Science Microscopy Cellf.
Assessment of ferri-liposome targeting and internalization in vivo by bioluminescence
For in vivo control of ferri-liposome distribution and content release, ferri-liposomes functionalized with D-luciferin were administered intraperitoneally (30 mg kg−1 of D-luciferin) to a 10-week-old FVB.luctg/+;PyMTtg/+ mouse, and a magnet was attached to the first right pectoral mammary tumour. Twenty-four hours after ferri-liposome administration, the magnet was detached and the mouse was imaged non-invasively using an IVIS Imaging System (IVIS 100 Series). In the control experiment the magnet was omitted. During the scan, mice were kept under gaseous anaesthesia (5% isofluorane) and at 37 °C.
Treatment study
Primary MMTV-PyMT tumour cells, obtained as described36, were culture-expanded, suspended in serum free Dulbecco's Modified Eagle Medium (DMEM) (Invitrogen), and 5 × 105 cells were inoculated into the left inguinal mammary gland of the congenic recipient mouse (FVB/N mouse strain). The dosing regimen for JPM-565 treatment was determined based on previous reports33,34,35,47. JPM-565 had no discernable toxic side effects in the animal trials33,47. When tumour volume (Tv) reached 125 mm3, mice were treated with stabilizing buffer containing either of the compounds (Fig. 4b). JPM-565 was administered at a dose of 100 mg kg−1 every second day in 10 intraperitoneal injections, and progression of tumours was investigated (Supplementary Methods). Histological measurement of proliferation by Ki67 staining, and tumour vascularization rate by CD31 staining, were performed as described38,48.
Analysis of ferri-liposome targeted delivery in vivo at the tissue and cellular level
Alexa Fluor 546-functionalized ferri-liposomes were injected intraperitoneally, daily, to the orthotopic transplanted breast cancer mouse model for 3 days. Alexa Fluor 555-functionalized ferri-liposomes were injected intravenously, daily, into the MMTV-PyMT transgenic breast cancer mouse model for 2 days. A magnetic field was applied to the tumour for 12 h immediately after each injection. Rabbit anti-mouse E-cadherin (Abcam) and rat anti-mouse monoclonal FITC-conjugated CD206 (AbD Serotec) were used for Fig. 5c,d (Supplementary Methods).
Statistical analysis
Quantitative data are presented as means ± standard error. Differences were compared using Student's t-test. When P-values were 0.05 or less, differences were considered statistically significant.
References
Liotta, L. A. & Kohn, E. C. The microenvironment of the tumour-host interface. Nature 411, 375–379 (2001).
Mueller, M. M. & Fusenig, N. E. Friends or foes—bipolar effects of the tumour stroma in cancer. Nature Rev. Cancer 4, 839–849 (2004).
Santos, A. M., Jung, J., Aziz, N., Kissil, J. L. & Puré, E. Targeting fibroblast activation protein inhibits tumor stromagenesis and growth in mice. J. Clin. Invest. 119, 3613–3625 (2009).
Rosi, N. L. & Mirkin, C. A. Nanostructures in biodiagnostics. Chem. Rev. 105, 1547–1562 (2005).
Arrueboa, M., Fernández-Pachecoa, R., Ibarraa, M. R. & Santamaría, S. Magnetic nanoparticles for drug delivery. Nanotoday 2, 22–32 (2007).
Galanzha, E. I. et al. In vivo magnetic enrichment and multiplex photoacoustic detection of circulating tumour cells. Nature Nanotech. 4, 855–860 (2009).
Namiki, Y. et al. A novel magnetic crystal–lipid nanostructure for magnetically guided in vivo gene delivery. Nature Nanotech. 4, 598–606 (2009).
Kim, J. W., Galanzha, E. I., Shashkov, E. V., Moon, H. M. & Zharov, V. P. Golden carbon nanotubes as multimodal photoacoustic and photothermal high-contrast molecular agents. Nature Nanotech. 4, 688–694 (2009).
Vlaskou, D. et al. Magnetic and acoustically active lipospheres for magnetically targeted nucleic acid delivery. Adv. Funct. Mater. 20, 3881–3894 (2010).
Bulte, J. W. M. et al. Selective Mr imaging of labeled human peripheral-blood mononuclear-cells by liposome mediated incorporation of dextran-magnetite particles. Magn. Reson. Med. 29, 32–37 (1993).
Bulte, J. W., de Cuyper, M., Despres, D. & Frank, J. A. Short- vs. long-circulating magnetoliposomes as bone marrow-seeking MR contrast agents. J. Magn. Reson. Imaging 9, 329–335 (1999).
Bulte, J. W. M., de Cuyper, M., Despres, D. & Frank, J. A. Preparation, relaxometry, and biokinetics of PEGylated magnetoliposomes as MR contrast agent. J. Magn. Magn. Mater. 194, 204–209 (1999).
Lee, J. et al. Artificially engineered magnetic nanoparticles for ultra-sensitive molecular imaging. Nature Med. 13, 95–99 (2007).
Torchilin, V. Multifunctional and stimuli-sensitive pharmaceutical nanocarriers. Eur. J. Pharm. Biopharm. 71, 431–444 (2009).
Medarova, Z., Pham, W., Farrar, C., Petkova, V. & Moore, A. In vivo imaging of siRNA delivery and silencing in tumors. Nature Med. 13, 372–377 (2007).
Naiden, E. et al. Magnеtiс pгopеrtiеs and stгuсtural parameters of nanosizеd oхidе fеrrimagnеt powdеrs produсеd by mесhanoсhemiсal synthеsis frоm salt solutions. Phys. Solid State 5, 891–900 (2003).
Bogdanov, A. A., Martin, C., Weissleder, R. & Brady, T. J. Trapping of dextran-coated colloids in liposomes by transient binding to aminophospholipid—preparation of ferrosomes. Biochim. Biophys. Acta Biomembranes 1193, 212–218 (1994).
Di Paolo, D. et al. Liposome-mediated therapy of neuroblastoma. Methods Enzymol. 465, 225–249 (2009).
Torchilin, V. P. et al. Poly(ethylene glycol) on the liposome surface - on the mechanism of polymer-coated liposome longevity. Biochim. Biophys. Acta Biomembranes 1195, 11–20 (1994).
Fortin-Ripoche, J. P. et al. Magnetic targeting of magnetoliposomes to solid tumors with MR imaging monitoring in mice: feasibility. Radiology 239, 415–424 (2005).
Martina, M. S. et al. Generation of superparamagnetic liposomes revealed as highly efficient MRI contrast agents for in vivo imaging. J. Am. Chem. Soc. 127, 10676–10685 (2005).
Stollfuss, J. C. et al. Rectal carcinoma: high-spatial-resolution MR imaging and T2 quantification in rectal cancer specimens. Radiology 241, 132–141 (2006).
Seo, W. S. et al. FeCo/graphitic-shell nanocrystals as advanced magnetic-resonance-imaging and near-infrared agents. Nature Mater. 5, 971–976 (2006).
Ai, H. et al. Magnetite-loaded polymeric micelles as ultrasensitive magnetic-resonance probes. Adv. Mater. 17, 1949–1952 (2005).
Shapiro, M. G., Atanasijevic, T., Faas, H., Westmeyer, G. G. & Jasanoff, A. Dynamic imaging with MRI contrast agents: quantitative considerations. Magn. Reson. Imaging 24, 449–462 (2006).
Na, H. B. et al. Development of a T1 contrast agent for magnetic resonance imaging using MnO nanoparticles. Angew Chem. Int. Ed. 46, 5397–5401 (2007).
Zhao, M., Josephson, L., Tang, Y. & Weissleder, R. Magnetic sensors for protease assays. Angew Chem. Int. Ed. 42, 1375–1378 (2003).
Atanasijevic, T., Shusteff, M., Fam, P. & Jasanoff, A. Calcium-sensitive MRI contrast agents based on superparamagnetic iron oxide nanoparticles and calmodulin. Proc. Natl Acad. Sci. USA 103, 14707–14712 (2006).
Guy, C. T., Cardiff, R. D. & Muller, W. J. Induction of mammary tumors by expression of polyomavirus middle T oncogene: a transgenic mouse model for metastatic disease. Mol. Cell Biol. 12, 954–961 (1992).
Wender, P. A. et al. Real-time analysis of uptake and bioactivatable cleavage of luciferin-transporter conjugates in transgenic reporter mice. Proc. Natl Acad. Sci. USA 104, 10340–10345 (2007).
Greenbaum, D., Medzihradszky, K. F., Burlingame, A. & Bogyo, M. Epoxide electrophiles as activity-dependent cysteine protease profiling and discovery tools. Chem. Biol. 7, 569–581 (2000).
Greenbaum, D. et al. Chemical approaches for functionally probing the proteome. Mol. Cell Proteomics 1, 60–68 (2002).
Joyce, J. A. et al. Cathepsin cysteine proteases are effectors of invasive growth and angiogenesis during multistage tumorigenesis. Cancer Cell 5, 443–453 (2004).
Bell-McGuinn, K., Garfall, A., Bogyo, M., Hanahan, D. & Joyce, J. A. Inhibition of cysteine cathepsin protease activity enhances chemotherapy regimens by decreasing tumor growth and invasiveness in a mouse model of multistage cancer. Cancer Res. 67, 7378–7385 (2007).
Schurigt, U. et al. Trial of the cysteine cathepsin inhibitor JPM-OEt on early and advanced mammary cancer stages in the MMTV-PyMT-transgenic mouse model. Biol. Chem. 389, 1067–1074 (2008).
Vasiljeva, O. et al. Tumor cell-derived and macrophage-derived cathepsin B promotes progression and lung metastasis of mammary cancer. Cancer Res. 66, 5242–5250 (2006).
Vasiljeva, O. & Turk, B. Dual contrasting roles of cysteine cathepsins in cancer progression: apoptosis versus tumour invasion. Biochimie 90, 380–386 (2008).
Sevenich, L. et al. Synergistic antitumor effects of combined cathepsin B and cathepsin Z deficiencies on breast cancer progression and metastasis in mice. Proc. Natl Acad. Sci. USA 107, 2497–2502 (2010).
Gocheva, V. & Joyce, J. A. Cysteine cathepsins and the cutting edge of cancer invasion. Cell Cycle 6, 60–64 (2007).
Turk, V., Kos, J. & Turk, B. Cysteine cathepsins (proteases)—on the main stage of cancer? Cancer Cell 5, 409–410 (2004).
Rossi, A., Deveraux, Q., Turk, B. & Sali, A. Comprehensive search for cysteine cathepsins in the human genome. Biol. Chem. 385, 363–372 (2004).
Mohamed, M. M. & Sloane, B. F. Cysteine cathepsins: multifunctional enzymes in cancer. Nature Rev. Cancer 6, 764–775 (2006).
Vasiljeva, O. et al. Emerging roles of cysteine cathepsins in disease and their potential as drug targets. Curr. Pharm. Des. 13, 387–403 (2007).
Sloane, B. F. et al. Cathepsin B and tumor proteolysis: contribution of the tumor microenvironment. Semin. Cancer Biol. 15, 149–157 (2005).
Gocheva, V. et al. IL-4 induces cathepsin protease activity in tumor-associated macrophages to promote cancer growth and invasion. Genes Dev. 24, 241–255 (2010).
Ceelen, W. P. & Flessner, M. F. Intraperitoneal therapy for peritoneal tumors: biophysics and clinical evidence. Nature Rev. Clin. Oncol. 7, 108–115 (2010).
Sadaghiani, A. M. et al. Design, synthesis, and evaluation of in vivo potency and selectivity of epoxysuccinyl-based inhibitors of papain-family cysteine proteases. Chem. Biol. 14, 499–511 (2007).
Vasiljeva, O. et al. Reduced tumour cell proliferation and delayed development of high-grade mammary carcinomas in cathepsin B-deficient mice. Oncogene 27, 4191–4199 (2008).
Acknowledgements
The authors thank Yu.F. Ivanov (Tomsk Scientific Center) for transmission electron microscopy, G. Kapun (National Institute of Chemistry) for scanning electron microscopy, M. Škarabot (Jozef Stefan Institute) for atomic force microscopy, J. Ščančar and M. Vahčič (Jozef Stefan Institute) for flame atomic absorption spectrometry, I.V. Sukhodolo, R.I. Pleshko, A.N. Dzuman, I.V. Milto and L.M. Ogorodova (Siberian State Medical University) for help in the acute toxicity study, and A. Sepe, M. Butinar, M. Trstenjak-Prebanda and A. Petelin (Jozef Stefan Institute), O.G. Terekhova (Tomsk Scientific Center), M. Tacke and N. Klemm (Institut für Molekulare Medizin und Zellforschung) for technical and methodological assistance, G. Salvesen (Sanford-Burnham Medical Research Institute) for valuable discussions, and R.H. Pain (Jozef Stefan Institute) for critical reading of the manuscript. JPM-565 was kindly provided by the Drug Synthesis and Chemistry Branch, Developmental Therapeutics Program, Division of Cancer Treatment and Diagnosis, National Cancer Institute. The research leading to these results was supported in part by the European Community's Seventh Framework Programme FP7/2007-2011 (grant agreement no. 201279, Microenvimet, O.V., T.R., C.P. and B.T.), the Slovenian Research Agency (research grant no. P1-0140, B.T.), the Russian Foundation for Basic Research (project no. 07-04-12170, E.P.N.), the United States Civilian Research and Development Foundation (project no. Y4-C16-05, A.A.M and V.I.I.) and the DFG SFB 850 (to T.R., C.P. and R.Z.).
Author information
Authors and Affiliations
Contributions
G.M., U.M., I.P., S.G.P., B.T. and O.V. conceived and designed the experiments. G.M., U.M., L.B. and O.V. performed the experiments. G.M., U.M., S.G.P., B.T. and O.V. analysed the data. T.R., C.P. and R.Z. contributed transgenic mouse models and animal imaging. M.B. contributed JPM-565 inhibitor. A.A.M., V.I.I., E.P.N. and S.G.P. supplied the magnetic nanoparticles. S.G.P., V.T., B.T. and O.V. supervised the project. G.M., S.G.P., B.T. and O.V. wrote the manuscript. All authors discussed the results and commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information
Supplementary information (PDF 3236 kb)
Rights and permissions
About this article
Cite this article
Mikhaylov, G., Mikac, U., Magaeva, A. et al. Ferri-liposomes as an MRI-visible drug-delivery system for targeting tumours and their microenvironment. Nature Nanotech 6, 594–602 (2011). https://doi.org/10.1038/nnano.2011.112
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nnano.2011.112
This article is cited by
-
Delivery of Corn-Derived Nanoparticles with Anticancer Activity to Tumor Tissues by Modification with Polyethylene Glycol for Cancer Therapy
Pharmaceutical Research (2023)
-
Evaluation of novel cathepsin-X inhibitors in vitro and in vivo and their ability to improve cathepsin-B-directed antitumor therapy
Cellular and Molecular Life Sciences (2022)
-
Rat Blood Leukocytes after Intravenous Injection of Magnetoliposomes on the Basis of Nanomagnetite
Bulletin of Experimental Biology and Medicine (2021)