Abstract
Study design:
Long-term follow-up study.
Objectives:
To determine whether gastrointestinal transit times (GITTs) and colonic dimensions change during the first or subsequent decades after spinal cord injury (SCI).
Setting:
Aarhus University Hospital, Denmark.
Methods:
GITT and colonic dimensions were evaluated by means of radio-opaque markers. Group A (n=12) was investigated 1 year after SCI and again 13 (range 11–14) years later. Group B (n=10) was studied 19 (range 9–36) years after injury and again 12 (range 11–12) years later. All had been treated with conservative bowel management.
Results:
In group A, the median GITT 1 year after injury was 4.3 (range 1.1–6.5) days and 13 years later, it was 3.2 (range 1.3–6.5) days, P=0.96. In group B, the median GITT 19 year after injury was 3.4 (range 0.6–5.9) days and 12 years later, it was 3.2 (range 1.9–5.5) days, P=0.77. None of the two groups experienced a significant change in the diameter of the caecum/ascending colon, transverse colon, descending colon or the sigmoid during long-term follow-up. Megacolon was present in four patients at baseline and in five at follow-up.
Conclusion:
GITTs and colonic dimensions did not change, neither during the first decade nor long after SCI.
Similar content being viewed by others
Introduction
Constipation, fecal incontinence and abdominal pain are common symptoms after spinal cord injury (SCI).1, 2, 3, 4, 5, 6 Unfortunately, constipation-related symptoms and their impact on the quality of life increase with time since injury,1, 5 and abdominal pain is especially common in subjects who are at least 5 years after injury.6
Constipation is usually evaluated by symptom scores or, objectively, by radio-opaque markers or scintigrafy. Colonic or gastrointestinal transit times (GITTs) after SCI have previously been described in cross-sectional studies7, 8, 9, 10, 11 and in a single follow-up study within the first year after injury.12 However, long-term results are not available. Also, it has been suggested that megacolon is a common condition in subjects with long-standing spinal cord injuries13 but, again, long-term prospective evaluations are lacking. Accordingly, the aims of the present study were to evaluate the long-term effects of SCI on GITTs and colonic dimensions.
Materials and methods
In order to assess changes in GITTs and colonic dimension during the first decade after cord injury and in the long-term, we studied two groups of individuals: Group A was studied at a median 1.0 (range 0.5–1.2) years after injury and again 12.8 (range 10.9–13.6) years later. Group B was studied at a median 18.7 (range 8.9–35.8) years after injury and again 12.2 (11.0–12.3) years later. Both groups were recruited among participants from two previous studies performed at our unit:
Group A: GITTs, segmental colonic transit times, colonic diameters, gastrointestinal symptoms and use of medication were registered 1 year after SCI in 18 subjects12 during the period 1 January 1996 to 31 December 1997. In 2009, 16 were still alive and 12 accepted to participate in follow-up (Figure 1).
Group B: in 1997, 18 subjects with SCI participated in the short-term (four weeks) evaluation of a new prokinetic drug (Prucalopride, Janssen-Cilag, Birkerød, Denmark).14 All were 9–36 years after injury. Before inclusion, the same parameters as described for group A were determined. In 2009, 17 were still alive and 10 accepted to participate in the present study (Figure 1).
Background data on participants are shown in Table 1. Level and completeness of injury were classified according to international guidelines.15 None of the subjects included for follow-up had undergone colorectal surgery or developed other conditions that could affect their bowel function. Medication used at baseline and at follow-up in 2009 was compared. Patients were instructed to use exactly the same laxative and dose during the follow-up investigation as was listed in their file during baseline studies.
The study was performed according to the Helsinki II declaration and approved by the local Ethics Committee. Informed consent was obtained before inclusion.
Gastrointestinal and segmental transit times
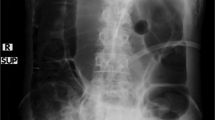
Gastrointestinal and segmental colonic transit times were determined by the method described by Abrahamson et al.16 Participants took one gelatine capsule (P & A Mauch, Münchenstein, Switzerland) every day for 6 consecutive days. Each capsule contained 10 radio-opaque polyurethane markers containing 40% barium sulfate. On day 7, a single anterior–posterior plain abdominal X-ray picture was taken. The method for calculation of GITTs and segmental colonic transit times has previously been described in detail.12, 16 The upper limit of GITTs that can be determined by this method is 6.5 days. A consultant colonic radiologist and the first author independently evaluated all X-rays. In case of discrepancy between results, a conclusion was reached after joint discussion.
Colonic dimensions
We defined megacolon as a segmental colonic diameter >mean+2 s.d. for healthy controls investigated with double-contrast barium enema.17 This corresponds to diameters of the ascending colon >8.7 cm, transverse colon >8.0 cm, descending colon >5.6 cm and the sigmoid >6 cm. The height of the first lumbar vertebra and the diameter of the femoral head were used to correct for differences in radiographic magnification. During analysis, the investigator did not know whether the X-ray picture had been taken at baseline or at follow-up. For the examination of the abdominal X-ray pictures, we attempted to blind the investigators as to the time of investigation. This was, however, not possible as old and new radiographs differ from a technical point of view.
Statistical analysis
Calculation of sample size was based on data from a previous study,12 with median GITTs at baseline of 3.6 days and an s.d. of 1.8 days. A target difference of 2 days (between baseline and follow-up), a power of the test of 90% and a significant level (alpha) of 5% gave a sample size of nine in each group.
Analysis of all the data was performed with the program STATA/IC 10 for Windows (StataCorp, College Station, TX, USA). As data for gastrointestinal and segmental colonic transit times, as well as colonic diameters deviated from the normal distribution (normal probability plots), the non-parametric Wilcoxon's matched-pairs signed-rank test was used for comparisons. Descriptive statistics were performed on background data and bowel function; data are presented as proportions or for quantitative variables, as median with range. P<0.05 was considered statistically significant.
Results
Gastrointestinal transit times and segmental colonic transit times are presented in Table 2. Apart from a decrease in rectosigmoid transit time from 1 to 13 years after SCI, no statistically significant changes were found. Likewise, no statistically significant changes in colonic dimensions were observed (Table 3). Two group A and three group B participants had a single mega-colon segment at baseline and at follow-up. Additional two group B participants had a single megacolon segment at follow-up.
Bowel symptoms and use of laxatives are shown in Table 4. There was a trend toward more use of digital stimulation or evacuation of the rectum. Otherwise, there were no major changes in bowel function or use of laxatives. Dividing subjects into those with complete (n=12) and those with incomplete lesions (n=10) did not change the overall pattern; likewise, no change of the overall pattern resulted from dividing the subjects into those with supraconal lesions (n=14) and those with conal/cauda equine lesions (n=6) (data not shown).
Discussion
Long-term follow-up on colorectal function has shown that symptoms of constipation and abdominal pain increase with time after SCI.5, 6 We therefore speculated that GITTs would also become more severely prolonged in the long-term. The present study is the first to provide long-term follow-up on colorectal transit times and colonic dimensions. Compared with healthy subjects and in accordance with previous studies, most spinal cord injured subjects had prolonged gastrointestinal and segmental colonic transit times. Baseline GITT in group A was 1 year after injury and in group B, the median was 19 years after injury. Compared with baseline values, no major changes occurred during the first or later decades after injury. Furthermore, our results indicate that those subjects with most severely prolonged colonic transit continued to have so 10 years later.
Megacolon after long-term SCI has been a concern to many. Harari et al.13 defined megacolon as a segmental colonic diameter of >6 cm or a rectal diameter of >4.5 cm, and reported it to be present in 73% of the chronic spinal cord injured patients studied. A generally accepted definition of megacolon is not available,18 but from our clinical experience as colorectal surgeons and gastroenterologists, we find that the diameters previously reported are too small. Therefore, we applied a definition inspired by double-contrast barium enema radiograph evaluations, thereby accepting somewhat larger diameters. Whether this is valid is, of course, debatable. However, no major changes in colonic dimensions appeared during the follow-up periods. Accordingly, our results suggest that, in the majority of patients, a prolonged colonic transit time after SCI does not cause megacolon.
Altered use of laxatives is a potential source of error in long-term studies of bowel function after SCI. Most subjects used the same laxative in almost the same dose at baseline and at follow-up 12–13 years later. GITTs in subjects using stimulant laxatives (n=4) were comparable with the rest of the group. As we had very thorough data on their use of laxatives at baseline, we were able to have patients use the same drug and dose during the assessment of GITTs at follow-up.
Selection bias may have influenced our results. The 12 subjects in group A were recruited from the 18 subjects completing a study 13 years earlier.12 Those 18 were recruited among the 26 consecutive, newly spinal cord injured patients in our uptake area. Subjects in group A were comparable with the general SCI population in terms of age at injury and completeness of lesion. However, there was a tendency toward longer baseline GITTs in those participating at follow-up (median 4.3 days) as compared with those who did not (median 2.8 days). Subjects in group B had volunteered for a clinical trial on prokinitics and they generally included a larger proportion with complete lesions than expected from the entire Danish spinal cord injured population. This could lead to selection of those with the most severe symptoms. On the other hand, some subjects with very severe bowel dysfunction would have been offered surgery and would therefore not be available for the group B study at baseline.
As constipation-related symptoms become more severe as time since injury passes,5 we expected median total gastrointestinal transit to follow. Sample size calculated ahead of study start overshot this effect, and as a consequence, the study is underpowered to show a transit time difference of less than 1 day. Others found poor correlation between total GITT and symptoms as well.19
The methodological strength of this study lies in its prospective long-term follow-up design. It overcomes some of the limitations of cross-sectional studies. Furthermore, baseline data, bowel function, medical and surgical history are all accounted for. Other methodological challenges have to be discussed. For the examination of the radiographs, blinding the time of investigation was not possible because of technical differences in old and modern radiographs. However, this is unlikely to have influenced results significantly, as there was no trend toward larger or smaller measurements associated with old or new radiographs. When measuring the diameters of the various sections of the colon, we experienced problems. Typically, a redundant sigmoid was overlying another segment, making the transverse colonic and sigmoid diameters difficult to measure.
In a large prospective follow-up of neurogenic bowel dysfunction in Danish spinal cord injured5 patients, we found that symptoms of constipation became more severe with time since injury, but this did not lead to a change in pharmacological treatment of bowel function. In the present study, numbers are too small to draw any firm conclusions about colorectal functional change over time. However, in support of the external validity of our results, there was a tendency toward more use of anorectal digitations during defecation at long-term follow-up. Also, selection of symptomatically stable patients may explain unaltered treatment over time.
In conclusion, the study demonstrated that GITT and colonic proportions did not become more abnormal, neither during the first decade nor later after injury.
References
Krogh K, Nielsen J, Djurhuus JC, Mosdal C, Sabroe S, Laurberg S . Colorectal function in patients with spinal cord lesions. Dis Colon Rectum 1997; 40: 1233–1239.
Stone JM, Nino-Murcia M, Wolfe VA, Perkash I . Chronic gastrointestinal problems in spinal cord injury patients: a prospective analysis. Am J Gastroenterol 1990; 85: 1114–1119.
Lynch AC, Wong C, Anthony A, Dobbs BR, Frizelle FA . Bowel dysfunction following spinal cord injury: a description of bowel function in a spinal cord-injured population and comparison with age and gender matched controls. Spinal Cord 2000; 38: 717–723.
Menter R, Weitzenkamp D, Cooper D, Bingley J, Charlifue S, Whiteneck G . Bowel management outcomes in individuals with long-term spinal cord injuries. Spinal Cord 1997; 35: 608–612.
Faaborg PM, Christensen P, Finnerup N, Laurberg S, Krogh K . The pattern of colorectal dysfunction changes with time since spinal cord injury. Spinal Cord 2008; 46: 234–238.
Finnerup NB, Faaborg P, Krogh K, Jensen TS . Abdominal pain in long-term spinal cord injury. Spinal Cord 2008; 46: 198–203.
Valles M, Mearin F . Pathophysiology of bowel dysfunction in patients with motor incomplete spinal cord injury: comparison with patients with motor complete spinal cord injury. Dis Colon Rectum 2009; 52: 1589–1597.
Leduc BE, Spacek E, Lepage Y . Colonic transit time after spinal cord injury: any clinical significance? J Spinal Cord Med 2002; 25: 161–166.
Nino-Murcia M, Stone JM, Chang PJ, Perkash I . Colonic transit in spinal cord-injured patients. Invest Radiol 1990; 25: 109–112.
Beuret-Blanquart F, Weber J, Gouverneur JP, Demangeon S, Denis P . Colonic transit time and anorectal manometric anomalies in 19 patients with complete transection of the spinal cord. J Auton Nerv Syst 1990; 30: 199–207.
Menardo G, Bausano G, Corazziari E, Fazio A, Marangi A, Genta V et al. Large-bowel transit in paraplegic patients. Dis Colon Rectum 1987; 30: 924–928.
Krogh K, Mosdal C, Laurberg S . Gastrointestinal and segmental colonic transit times in patients with acute and chronic spinal cord lesions. Spinal Cord 2000; 38: 615–621.
Harari D, Minaker KL . Megacolon in patients with chronic spinal cord injury. Spinal Cord 2000; 38: 331–339.
Krogh K, Jensen MB, Gandrup P, Laurberg S, Nilsson J, Kerstens R et al. Efficacy and tolerability of prucalopride in patients with constipation due to spinal cord injury. Scand J Gastroenterol 2002; 37: 431–436.
Marino RJ, Barros T, Biering-Sorensen F, Burns SP, Donovan WH, Graves DE et al. International standards for neurological classification of spinal cord injury. J Spinal Cord Med 2003; 26 (Suppl 1): S50–S56.
Abrahamsson H, Antov S, Bosaeus I . Gastrointestinal and colonic segmental transit time evaluated by a single abdominal x-ray in healthy subjects and constipated patients. Scand J Gastroenterol Suppl 1988; 152: 72–80.
Preston DM, Lennard-Jones JE, Thomas BM . Towards a radiologic definition of idiopathic megacolon. Gastrointest Radiol 1985; 10: 167–169.
Gladman MA, Knowles CH . Novel concepts in the diagnosis, pathophysiology and management of idiopathic megabowel. Colorectal Dis 2008; 10: 531–538.
Media S, Christensen P, Lauge I, Al-Hashimi M, Laurberg S, Krogh K . Reproducibility and validity of radiographically determined gastrointestinal and segmental colonic transit times in spinal cord-injured patients. Spinal Cord 2009; 47: 72–75.
Acknowledgements
The study received financial support from Coloplast A/S, Humlebaek, Denmark. Dr Christensen and Dr Krogh have received support from the Danish Research Council.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Faaborg, P., Christensen, P., Rosenkilde, M. et al. Do gastrointestinal transit times and colonic dimensions change with time since spinal cord injury?. Spinal Cord 49, 549–553 (2011). https://doi.org/10.1038/sc.2010.162
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2010.162
Keywords
This article is cited by
-
Neural pathways for colorectal control, relevance to spinal cord injury and treatment: a narrative review
Spinal Cord (2018)
-
Bowel Dysfunction in Spinal Cord Injury: Current Perspectives
Cell Biochemistry and Biophysics (2014)