Abstract
The human population is ageing worldwide. The World Health Organization estimated that the world’s population of people aged 60 years and older will increase to at least 30%, coinciding with a growing frequency of cognitive and cardiovascular disease. Recently, in preclinical studies platelet Factor 4 (PF4) was presented as a pro-cognitive factor. This molecule is released by platelets in the circulation and could be present in blood products destined for transfusion. We wondered if PF4 levels are correlated to the age of the blood donor or to the storage time of platelet concentrates (PCs) intended for transfusion? We observed higher levels of PF4 in PCs from elderly donors compared to younger donors, while PC storage time did not determine PF4 levels expression.
Similar content being viewed by others
On 15 June 1667, Dr Jenys, assisted by Dr Emmerez performed the first fully documented blood transfusion. Approximately twelve ounces of lamb's blood were transfused into the veins of a 15-year-old boy who had been suffering from uncontrollable fever for two months. Interestingly, one year later, a dementia patient was also given a blood transfusion by Denys and Emmerez. This marked the advent of a putative link between blood transfusion and cognitive pathologies—currently a forgotten “connection”.
More recently, studies making use of heterochronic parabiosis connecting old and young mice have demonstrated systemic rejuvenating properties1,2. In addition, blood plasma transfer from young to older mice reversed age-related cognitive impairments, although the exact mechanisms involved are unclear1,2,3,4,5. A few molecules however have been placed in the limelight to be involved in this proces. Eotaxin-1 or TIMP-2 detected in blood components prepared for transfusion have been associated with cognitive function and ageing6, as well as Platelet Factor 4 (PF4), which is mainly released from platelet α-granules7.
Platelets are anucleate cells and are well known for their haemostatic function, but less for their immune function. Platelets are mostly transfused as platelet concentrates (PCs), generated from full blood donations. Importantly, they are potent secretors of numerous soluble factors, such as prostaglandins and cytokines including PF47.
PF4 was one of the first cytokines to be discovered (first as chemokine ligand 4) and has been highly conserved during evolution8,9. The main physiological function of PF4 is the promotion of blood haemostasis but it also mediates the immune response. During coagulation and clot formation, PF4 interact with the endothelium, monocytes and neutrophils and participate in the generation of Neutrophil Extracellular Traps10,11. In addition, PF4 binds to bacteria12. The host can subsequently generate auto-antibodies against PF4, mediating the opsonisation of bacteria and FCγRIIa on platelets, which are able to kill bacteria12,13. Because of the ability of PF4 to generate auto-antibodies it is also a major player in heparin induced thrombocytopenia and vaccine-induced immune thrombotic thrombocytopenia14,15,16,17,18.
Recently published reports propose a new role for PF4 to be involved in cognitive disorders3,4,5. Indeed, PF4 administration decrease hippocampal neuroinflammation and improved cognition in aged mice3. Administration of Klotho, a cognition-enhancing protein, increases PF4 levels. PF4 permeates the brain and enhances cognition in mice4. PF4 is released by physical-activity-inducing-activated platelet, and PF4 induces proliferation of hippocampal precursor cell, leading to cognitive enhancement5.
A significant proportion of patients who undergo major surgery experience temporary or permanent decline in cognitive performance: Post-Operative Cognitive Dysfunction (POCD)19. These patients received mainly platelet concentrate (PC) transfusion. During collection, preparation and storage, PCs destined for transfusion experience stress-induced lesions20. Platelet processing may alter structure and function, such as an increased Biological Response Modifier (BRM) secretion. These BRMs range from cytokines to extracellular vesicles, lipids and soluble Danger-Associated Molecular Patterns21,22,23. Not a lot is known of PF4 modulation during PC storage.
We therefore wondered whether donor age influences the levels of “rejuvenating” PF4 and whether PF4 levels alter during storage of PCs. Our study investigated the effects of donor age and single donor apheresis platelet concentrate (SDA-PC) storage time on PF4 levels.
Results
Blood donor characteristics
Recent reports demonstrated that PF4 is involved in systemic inflammation and cognitive repair1,3,4,5. These observations made us wonder whether SDA-PC level of PF4 are linked to donor age and/or storage time. We obtained residual fractions of transfused SDA-PCs, from which platelets were discarded to keep only the supernatant for PF4 analysis (Supplementary Fig. 1a). We analysed in total 1,707 SDA-PCs (1,092 males and 615 females) from donors aged 18 to 65 years (Supplementary Fig. 1b). The SDA-PCs were also subdivided into three categories based on storage time: 0, [1–3], and [3–5] days. Stored SDA-PCs could be transfused until study day 5 at the time of the study after which they are discarded. The majority of donors were male aged 30 to 60 (Supplementary Fig. 1c). The same pattern was observed with different storage times (Supplementary Fig. 1c).
PF4 levels associated with increasing age
During the first analysis, PF4 levels from SDA-PCs were plotted according to the donor’s age, regardless of PC storage time (Fig. 1a). PF4 was significantly elevated in elderly donors (over 60), as compared to younger donors (Fig. 1a). At storage time [0], PF4 levels correlated positively with donor age (Fig. 1b,c). No statistically significant correlation was observed between donor’s age and PF4 expression at storage time [1–3] and [3–5] (Fig. 1c). It is in line with an increase of platelet’s activation when Platelet Rich Plasma is stimulated with the platelet agonist thrombin receptor activator peptide (TRAP). We observed a significant increase of PF4 levels in the supernatant of PRP stimulated with TRAP (136.9 ng/ml + 10.5), as compared to unstimulated PRP (84.3 + 8.5 ng/ml) (Fig. 1d).
Evaluation of SDA-PC PF4 levels depending on donor age and storage time independently. (a) Velocity plot of the expression of SDA-PC PF4 based on different donor age, 2-way ANOVA, *p < 0.05; non-significant (ns); large dash present median of data and small dash the quartiles. (b) Graph illustrating PF4 expression in function of donor age at day [0] of storage time. Regression line in red, spearman correlation r = 0.08; p value = 0.02 *. (c) Spearman’s correlation matrix between PF4 concentration and age, based on storage time. Red square corresponds to positive correlation with p value < 0.05; white square corresponds to no correlation with p value < 0.05. (d) Graph bar representing the release of PF4 after a stimulation with TRAP platelet agonist in Platelet Rich Plasma (PRP); n = 21; Wilcoxon test p < 0.0001 **** (e) PF4 expression during storage period regardless of donor age, 2-way ANOVA, ***p < 0.001 ****p < 0.0001. (f) Graph illustrating PF4 expression in function of storage time independently of age donor. Regression line in red, spearman correlation r = 0.31 p value = 1.32 e-13 *. (g) Spearman’s correlation matrix between PF4 concentration and storage time. White square corresponds to no correlation with p value < 0.05.
Moreover, PF4 expression did not seem to be linked to sex of the donor, since we did not observe any significant differences of PF4 level in male or female donors in all different age categories (Supplemental Fig. 2a,b).
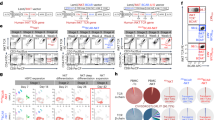
Evaluation of SDA-PC PF4 levels depending on donor’s age and storage time. (a) PF4 expression based on donor age and storage time 2-way ANOVA, **p < 0.01, ****p < 0.0001, non-significant difference (ns). (b) Graph bar represents PF4 expression based on storage time ([0], [1–3] and [3–5] days, 2-way ANOVA, *p < 0.05 (c) Spearman’s correlation matrix based on different donor age groups, storage time and PF4 concentrations. Red square corresponds to positive correlation with p value < 0.05; white square corresponds to no correlation with p value < 0.05.
PF4 levels correlated with storage time
We wondered whether PF4 levels could be modulated by the storage of SDA-PCs, regardless of donor age. Interestingly, storage appeared to significantly modulate, decreasing PF4 levels (Fig. 1e). No significant correlations were detected by spearman correlation between sample stored between [0–5] days and PF4 level (Fig. 1f,g).
When dividing the SDA-PCs in different donor age groups followed by a subanalysis on storage time, we noted that PF4 levels were significantly higher at storage time [0] compared to [1–3] days of storage, for all donor ages. We noticed a significant decrease of PF4 levels between [0] and [1–3], in donors of [18–30], [30–60] and [60–70] years old (Fig. 2a). Furthermore, a slight increase in PF4 expression was, however, noted between days [1–3] and [3–5] only for donors between [18–30] and [30–60] years (Fig. 2a). The same pattern was observed with [60–70] year old donors, but not significant (Fig. 2a). Interestingly, PF4 levels did not differ for donors aged [18–30] and [60–70] between [0] to [3–5] days of storage, while they did significantly differ for donors aged [30–60] (Fig. 2a). No significative correlation was noticed between [0] and [3–5] storage time in [18–30] and [60–70] aged donors (Fig. 2b).
We compared the influence of storage time on PF4 levels in different age groups (Fig. 2c). We also analysed the storage time data set plotted with donor age (Fig. 2c). No significant change in PF4 levels over storage times [1–3] and [3–5] were observed with the different donor ages (Fig. 2c). However, a significant increase in PF4 levels between younger (18–30) and older (60–70) donors was observed at storage time [0] (Fig. 2a). Finally, there is no significant, positive correlation between PF4 and storage time and donor age (Fig. 2b).
PF4 expression was neither modulated by sex of the donor (Supplemental Fig. 2), nor was there a correlation between storage and sex (Fig. 3). There is no significant difference between PF4 levels in male and female donors during the storage of the SDA-PC (Fig. 3a), neither a significant correlation between age and storage in male donors (Fig. 3b).
Evaluation of SDA-PC PF4 levels depending on donor’s age, storage time and sex. (a) Graph bar represents PF4 expression based on storage time ([0], [1–3] and [3–5] days, 2-way ANOVA. Light Blue for male donors (M) and light pink for female donors (F). (b) Spearman’s correlation matrix based on different donor age groups, storage time and PF4 concentrations. White square corresponds to no correlation with p value < 0.05.
Discussion
Recent reports demonstrated a lower expression of PF4 in elderly human donors and mice3,24. Remarkably, the exogenous administration of PF4 appeared to be beneficial for the restoration of cognitive function in aged mice, hinting towards a novel revolutionary therapeutic strategies to combat cognitive disorders5. However, our data showed quite the opposite. We measured higher PF4 levels in supernatants of SDA-PCs from elderly donors compared to younger donors, but we did not evaluate cognitive function of the donors.
Among different studies, the normal value of PF4 was 6.6 ng/ml (median) with 90% confidence interval between 1.7 ng/ml and 20.9 ng/ml25, 7.4 ng/ml (90% confidence interval 4 to 24)26, or 102 ng/ml + 32 (range 50–160) in plasma27. In our study, we have almost a factor 10 to 100 increase, since we measured PF4 in the supernatant of SDA-PC, which is a concentrate of platelets thus logically containing higher levels of platelet-secreted factors. In blood, the range for human platelets is around 120,000 to 450,000 platelets/mL, whereas the platelet concentration in SDA-PCs is around 1,500,000 platelets per mL. In the study from Schroer et al., the authors detected around 75 ng/mL of PF4 in young male mice. Over the time course of 24 h, they injected PF4 8 times in a concentration of 5 µg/mL to detect changes in inflammation and cognitive function in mice3. Schroer et al. perform their study only on male human blood donors, while the age groups were similar to the ones from our study. They categorized however the young group from [22–34] years old and the elderly as [61 to 75] years old3. In our study, our elderly group is under 65 years old, younger donor as studied by Schroer et al., maybe it can explain the difference in level of PF4. Moreover, PCs could contain activated platelet and the increase in PF4 level is a reflection of platelet activation in PCs. We also mixed genders during the first analysis, after which we also performed distinguishing PF4 level data by sex of donor (Supplemental Figs. 2 and 3). We did not notice any modulations of PF4 based on gender.
PF4 levels increase slightly during storage time of the SDA-PCs (Fig. 4).
Summary of the study. Left panel. Our study compared the level of platelet factor 4 (PF4), mainly produced/stored by platelet, in single donor apheresis platelet concentrate (SDA-PC), based on the age of the donor (physiological time). Right panel. Our study, also, compared the PF4 level during the storage time of SDA-PC. We conclude that elderly donors have a higher concentration of PF4 in SDA-PCs, compared to younger donors (left panel). We also conclude that PF4 level is modulated through the storage time with no difference between the beginning [0] days and the end of the storage [3–5] days (right panel).
Storage time of SDA-PCs (from day [0] to [3–5]) may impact PF4 levels, depending on donor age (Fig. 2a). We observed a slight but significant decrease of PF4 levels between [0] and [1–3] days of storage, which could be explained by PF4 consumption by or binding to platelets, via receptors such as CXCR3, LRP/LDLR, or proteoglycans8,9.
An initial glance at SDA-PC storage did not highlight any significant changes in PF4 levels (Fig. 2c). Based on our data and the work of Leiter et al.5, new transfusion approaches could be explored. The scientific community and blood bank worldwide should study the impact of PCs from elderly donors or shortly stored (both rich in PF4) in their transfusion protocols, which could serve as a an add-on running therapies for patients with cognitive disease. Considering that PF4 is proposed as a pro-cognitive factor with potentially beneficial therapeutic applications in age-related neurodegenerative diseases1,3,4,5, PF4-enriched-PCs could provide beneficial therapeutic transfusions in age-related neurodegenerative disease. A possible PF4 spike in SDA-PCs during preparation and storage could improve the potential of PC transfusion in age-related neurodegenerative diseases. This hypothesis needs to be further studied, as the world population is ageing which coincides with an increase of neurodegenerative and cognitive diseases.
Our study aligns with numerous works related to personalized transfusions, which is based on transfusing the best blood products tailored to the individual patient28. This approach will still require however extensive research, to equip physicians in transfusion medicine with a range of novel toolsets. This will enable the reevaluation of the interplay between donor and recipient characteristics, thereby enhancing the significance of personalized transfusion medicine.
Since JB Denys and P. Emmerez in the seventeenth century, the advent of a putative link between blood transfusion and cognitive pathologies—a forgotten “connection”—is still open for investigation. Heterochronic parabiosis can connect an elderly mouse to a younger mouse, after which the biological fluids such as blood are shared. Using this technic, several studies pointed out that it is possible to commence a rejuvenating process, such as a reprogramming of the transcriptome by inhibiting their ageing signature2,29,30. The immune system is also affected by the heterochronic parabiosis30,31. Indeed, younger mice in the parabiosis system are not able to “rejuvenate” the immune system of the elderlies mice31. In line with observations from Denys & Emmerez and the literature on parabiosis, the scientific community needs to test transfusions on older mice with a PF4 rich product and evaluate the rejuvenation of the mice. Combined with other studies, PF4 is a promising molecule possibly crucial for neurodegenerative and cognitive diseases, and could be used both as a biomarker and as a therapeutic.
Methods
Ethics and blood donors
This study complies with all relevant ethical regulations. Fresh blood from healthy donors was obtained from Etablissement Français du Sang (EFS) upon approval of the project by Ministry of Higher Education and Research (authorization number CODECOH DC-2019-3803 & AC-2020-3959). The study was approved by the national review board for biomedical research in March 2017 (Comité de Protection des Personnes Sud-Est I, Saint-Etienne -, France; ID RCB Number: 2014- A00405-42), in agreement with the General Data Protection Regulation (Regulation (EU) 2016/679 and Directive 95/46/EC) and the French data protection law (Law n°78-17 on 06/01/1978 and Décret n°2019-536 on 29/05/2019). Informed consent was obtained from all subjects and/or their legal guardian(s). Our study involves 1,707 donors (1,092 males and 615 females) between 18 and 70 years of age (Supplemental Fig. 1).
Blood preparation
As described previously32, single-donor apheresis (SDA) PCs were collected from donors and processed at the EFS. Briefly, SDA-PCs were leuko-reduced to < 106/bag and suspended in 35% native plasma/65% nutritive solution (InterSol™(Fenwal, Lake Zurich, IL, USA), called PAS-C/PAS-III), or SSP+™ (Macopharma, Tourcoing, France), called modified PAS-E/PAS-IIIM. SDA-PCs were kept at 22 + 2 °C under shaking (60 rpm) until they were transfused. At the time of the study, SDA-PCs were transfused until 5 days post-collection, after which they were destroyed.
For the study, SDA-PCs stored 0 to 5 days were used for transfusion. The left-over of transfusion was collected and platelets contained in SDA-PCs were discarded after centrifugation (450 g, 10 min), after which the supernatants were stored at -80 °C until PF4 measurement32. The supernatants of SDA-PC were quickly thawed before the PF4 measurement by ELISA (Supplemental Fig. 1a).
Platelet Rich Plasma preparation
Platelet-rich plasma (PRP) was prepared as previously described33. Briefly, peripheral blood was collected from healthy donors in endotoxin-free tubes with 3.2% sodium citrate (Becton Dickinson, Franklin Lakes, New Jersey, USA) and centrifuged at 150 g for 10 min at 22 °C. PRP was stimulated for 30 min at room temperature with 50 µg/mL thrombin receptor activator peptide (TRAP-SFLLRN, Sigma-Aldrich, Burlington, Massachusetts, USA). After stimulation, PRP was centrifuged at 2500 g 10 min, and the supernatants were collected and kept frozen at −80 °C until further analysis.
ELISA PF4
ELISA kit (PF4 DuoSet, ref. DY795—R&D Systems, Minnesota, USA) was used to measure PF4 levels, following the manufacturer’s instructions. Absorbance at 450 nm was determined with an ELISA plate reader (Magellan Sunrise, Tecan Group Ltd., Mannedorf, Switzerland).
Statistical analysis
The statistical analysis was carried out using GraphPad version 9 (La Jolla, CA). Normality of the data set was analysed through Kolmogorov–Smirnov test. Our data sets were not normally distributed. Comparison between sets of data was performed with a 2-ways ANOVA test, with Tukey multiple comparisons correction. Correlation matrix was performed with a spearman correlation.
Biorender
The cartoon at Fig. 3 was made via Biorender, Agreement numbers BA266PYIBY and UB26G9VXSY.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Villeda, S. A. et al. Young blood reverses age-related impairments in cognitive function and synaptic plasticity in mice. Nat Med 20, 659–663. https://doi.org/10.1038/nm.3569 (2014).
Ximerakis, M. et al. Heterochronic parabiosis reprograms the mouse brain transcriptome by shifting aging signatures in multiple cell types. Nat Aging 3, 327–345. https://doi.org/10.1038/s43587-023-00373-6 (2023).
Schroer, A. B. et al. Platelet factors attenuate inflammation and rescue cognition in ageing. Nature 620, 1071–1079. https://doi.org/10.1038/s41586-023-06436-3 (2023).
Park, C. et al. Platelet factors are induced by longevity factor klotho and enhance cognition in young and aging mice. Nat Aging 3, 1067–1078. https://doi.org/10.1038/s43587-023-00468-0 (2023).
Leiter, O. et al. Platelet-derived exerkine CXCL4/platelet factor 4 rejuvenates hippocampal neurogenesis and restores cognitive function in aged mice. Nat. Commun. 14, 4375. https://doi.org/10.1038/s41467-023-39873-9 (2023).
Hoefer, J., Dal-Pont, C., Jochberger, S., Fantin, R. & Schennach, H. The “rejuvenating factor” TIMP-2 is detectable in human blood components for transfusion. Vox Sang. 116, 533–539. https://doi.org/10.1111/vox.13023 (2021).
Liu, Z. Y. et al. New perspectives on the induction and acceleration of immune-associated thrombosis by PF4 and VWF. Front. Immunol. 14, 1098665. https://doi.org/10.3389/fimmu.2023.1098665 (2023).
Taddese, B. et al. Evolution of chemokine receptors is driven by mutations in the sodium binding site. PLoS Comput. Biol. 14, e1006209. https://doi.org/10.1371/journal.pcbi.1006209 (2018).
Liu, Z. et al. Platelet factor 4(PF4) and its multiple roles in diseases. Blood Rev. 64, 101155. https://doi.org/10.1016/j.blre.2023.101155 (2023).
Arepally, G. M. & Padmanabhan, A. Heparin-induced thrombocytopenia: A focus on thrombosis. Arterioscler Thromb. Vasc. Biol. 41, 141–152. https://doi.org/10.1161/ATVBAHA.120.315445 (2021).
Greinacher, A. & Warkentin, T. E. Platelet factor 4 triggers thrombo-inflammation by bridging innate and adaptive immunity. Int. J. Lab Hematol. 45(Suppl 2), 11–22. https://doi.org/10.1111/ijlh.14075 (2023).
Arman, M. et al. Amplification of bacteria-induced platelet activation is triggered by FcgammaRIIA, integrin alphaIIbbeta3, and platelet factor 4. Blood 123, 3166–3174. https://doi.org/10.1182/blood-2013-11-540526 (2014).
Palankar, R. et al. Platelets kill bacteria by bridging innate and adaptive immunity via platelet factor 4 and FcgammaRIIA. J. Thromb. Haemost. 16, 1187–1197. https://doi.org/10.1111/jth.13955 (2018).
Greinacher, A. Clinical practice. Heparin-Induced Thrombocytopenia. N. Engl. J. Med. 373, 252–261. https://doi.org/10.1056/NEJMcp1411910 (2015).
Greinacher, A. et al. Thrombotic thrombocytopenia after ChAdOx1 nCov-19 vaccination. N. Engl. J. Med. 384, 2092–2101. https://doi.org/10.1056/NEJMoa2104840 (2021).
Giles, J. B. et al. Genome-wide association study of platelet factor 4/heparin antibodies in heparin-induced thrombocytopenia. Blood Adv. 6, 4137–4146. https://doi.org/10.1182/bloodadvances.2022007673 (2022).
Schultz, N. H. et al. Thrombosis and thrombocytopenia after ChAdOx1 nCoV-19 vaccination. N. Engl. J. Med. 384, 2124–2130. https://doi.org/10.1056/NEJMoa2104882 (2021).
Scully, M. et al. Pathologic antibodies to platelet factor 4 after ChAdOx1 nCoV-19 vaccination. N. Engl. J. Med. 384, 2202–2211. https://doi.org/10.1056/NEJMoa2105385 (2021).
Monk, T. G. & Price, C. C. Postoperative cognitive disorders. Curr. Opin. Crit. Care 17, 376–381. https://doi.org/10.1097/MCC.0b013e328348bece (2011).
Ng, M. S. Y., Tung, J. P. & Fraser, J. F. Platelet storage lesions: What more do we know now?. Transfus. Med. Rev. https://doi.org/10.1016/j.tmrv.2018.04.001 (2018).
Duchez, A. C. et al. Bioactive lipids as biomarkers of adverse reactions associated with apheresis platelet concentrate transfusion. Front. Immunol. 14, 1031968. https://doi.org/10.3389/fimmu.2023.1031968 (2023).
Boudreau, L. H. et al. Platelets release mitochondria serving as substrate for bactericidal group IIA-secreted phospholipase A2 to promote inflammation. Blood 124, 2173–2183. https://doi.org/10.1182/blood-2014-05-573543 (2014).
Cognasse, F. et al. Assessment of the soluble proteins HMGB1, CD40L and CD62P during various platelet preparation processes and the storage of platelet concentrates: The BEST collaborative study. Transfusion 63, 217–228. https://doi.org/10.1111/trf.17200 (2023).
Wang, H. et al. Quantitative iTRAQ-based proteomic analysis of differentially expressed proteins in aging in human and monkey. BMC Genomics 20, 725. https://doi.org/10.1186/s12864-019-6089-z (2019).
Kaplan, K. L. & Owen, J. Plasma levels of beta-thromboglobulin and platelet factor 4 as indices of platelet activation in vivo. Blood 57, 199–202 (1981).
Chesterman, C. N., McGready, J. R., Doyle, D. J. & Morgan, F. J. Plasma levels of platelet factor 4 measured by radioimmunoassay. Br. J. Haematol. 40, 489–500. https://doi.org/10.1111/j.1365-2141.1978.tb05819.x (1978).
Cella, G. et al. Platelet factor 4 release induced by intravenous administration of heparin. Folia Haematol. Int. Mag. Klin. Morphol. Blutforsch. 112, 165–174 (1985).
D’Alessandro, A. & Liumbruno, G. Personalised transfusion medicine. Blood Transfus 17, 255–257. https://doi.org/10.2450/2018.0142-19 (2019).
Conboy, M. J., Conboy, I. M. & Rando, T. A. Heterochronic parabiosis: Historical perspective and methodological considerations for studies of aging and longevity. Aging Cell 12, 525–530. https://doi.org/10.1111/acel.12065 (2013).
Ma, S. et al. Heterochronic parabiosis induces stem cell revitalization and systemic rejuvenation across aged tissues. Cell Stem Cell 29, 990–1005. https://doi.org/10.1016/j.stem.2022.04.017 (2022).
Pishel, I. et al. Accelerated aging versus rejuvenation of the immune system in heterochronic parabiosis. Rejuven. Res. 15, 239–248. https://doi.org/10.1089/rej.2012.1331 (2012).
Cognasse, F. et al. Platelet soluble CD40-ligand level is associated with transfusion adverse reactions in a mixed threshold-and-hit model. Blood 130, 1380–1383. https://doi.org/10.1182/blood-2017-03-773945 (2017).
Cognasse, F. et al. Toll-like receptor 4 ligand can differentially modulate the release of cytokines by human platelets. Br. J. Haematol. 141, 84–91. https://doi.org/10.1111/j.1365-2141.2008.06999.x (2008).
Chabert, A. et al. Acetylsalicylic acid differentially limits the activation and expression of cell death markers in human platelets exposed to Staphylococcus aureus strains. Sci. Rep. 7, 5610. https://doi.org/10.1038/s41598-017-06024-2 (2017).
Acknowledgements
This work was supported by grants from the Etablissement Français du Sang, the Association “Les Amis de Rémi” Savigneux, France and the French “Agence Nationale de la Recherche” (National Research Agency), under grant (ANR-22-CE17-0063, project HEASY_PLAT). We are extremely grateful to the blood donors who made this research possible.
Author information
Authors and Affiliations
Contributions
Contribution: F.C. designed the study, supervised the research, secured funding and obtained approval from the ethics committee; A.C.D., M.H., H.H.C. and F.C. analysed data and wrote the manuscript. C.A.A., M.A.E., M.P., A.P. collected samples, did the experiments and statistical analyses. All authors participated in all steps of the process and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Duchez, A.C., Heestermans, M., Arthaud, CA. et al. In platelet single donor apheresis, platelet factor 4 levels correlated with donor’s age and decreased during storage. Sci Rep 14, 6231 (2024). https://doi.org/10.1038/s41598-024-56826-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-56826-4
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.