Abstract
As a member of the potassium calcium-activated channel subfamily, increasing evidence suggests that KCNN4 was associated with malignancies. However, the roles and regulatory mechanisms of KCNN4 in PDAC have been little explored. In this work, we demonstrated that the level of KCNN4 in PDAC was abnormally elevated, and the overexpression of KCNN4 was induced by transcription factor AP-1. KCNN4 was closely correlated with unfavorable clinicopathologic characteristics and poor survival. Functionally, we found that overexpression of KCNN4 promoted PDAC cell proliferation, migration and invasion. Conversely, the knockdown of KCNN4 attenuated the growth and motility of PDAC cells. In addition to these, knockdown of KCNN4 promoted PDAC cell apoptosis and led to cell cycle arrest in the S phase. In mechanistic investigations, RNA-sequence revealed that the MET-mediated AKT axis was essential for KCNN4, encouraging PDAC cell proliferation and migration. Collectively, these findings reveal a function of KCNN4 in PDAC and suggest it’s an attractive therapeutic target and tumor marker. Our studies underscore a better understanding of the biological mechanism of KCNN4 in PDAC and suggest novel strategies for cancer therapy.
Similar content being viewed by others
Introduction
Pancreatic ductal adenocarcinoma (PDAC) is one of the most deadly solid tumors with a terrible prognosis (5-year survival rate is less than 6%), and it was estimated to be the second leading cause of cancer-related deaths in 2030 [1,2,3]. Since the pancreas has an anatomically inaccessible location that prevents routine examination, more than half of PDAC patients were diagnosed at the advanced stages and no longer suitable for surgical resection. Moreover, nearly 80% of the patients who underwent surgical resection are at risk for recurrence [4, 5]. Currently, chemotherapy is a rare option for the treatment of PDAC, but drug resistance led to huge obstacles to improve overall survival [6,7,8]. Hence, despite tremendous efforts that have been made to study PDAC, no prominently therapeutic strategies have emerged. As a result, it is very important to further investigate the molecular mechanisms underlying PDAC and find out new targets for PDAC.
The protein encoded by KCNN4 (potassium calcium-activated channel subfamily N member 4) is part of a potentially heterotetrameric voltage-independent potassium channel that is activated by intracellular calcium. Activation is followed by membrane hyperpolarization, which promotes activated TRPV channels and subsequently, calcium influx [9]. Previous studies have demonstrated that KCNN4 plays an important role in inflammatory disease [10, 11]. Recently, emerging evidence has revealed that KCNN4 was overexpressed in malignancies, also closely related to the occurrence and progression of malignancy [12,13,14,15,16]. However, the functions and regulatory mechanisms of KCNN4 in PDAC have been little explored.
A pivotal tyrosine kinase receptor (MET) is one of the classic oncogenes for cancers [17, 18]. Previous studies have proved that MET was frequently highly expressed in PDAC, and the activation of MET triggers pleiotropic biological responses, which include migration, invasion, angiogenesis, EMT, and activates AKT signaling pathway [17, 19, 20]. AKT is not only a serine/threonine kinase but also a signaling molecule of cell growth and differentiation, as well as play a key role in the PI3K signaling pathway. Among the dysregulated signaling pathways, the PI3K/AKT pathway has been reported as the frequently altered signaling pathway in cancer and correlative with the development of cancer, including PDAC [21,22,23]. Thus, exploring the relation between KCNN4 and MET/AKT signaling pathway is significant for the development of effective therapeutic strategies in PDAC.
In this study, we showed that KCNN4 was aberrantly upregulated in PDAC, it induced proliferation and migration in vitro, and promoted oncogenesis in vivo. Besides, the overexpression of KCNN4 was positively correlated with the progression of PDAC and was related to the poorer prognosis of patients with PDAC. Significantly, we further revealed that KCNN4 promotes the proliferation and migration of PDAC via the Ca2+/MET/AKT axis and identified KCNN4 as a potential therapeutic target in PDAC.
Materials and methods
Plasmids and siRNAs
pLKO.1-shScramble and pLKO.1-shKCNN4 vectors were obtained from Sigma-Aldrich (St. Louis, MO, USA). pLenti-CMV-GFP/puro and pLenti-CMV-KCNN4 vectors were obtained from Biogot Technology. pLVX-JUN, pLVX-MET vectors were obtained from Miaoling Biotechnology. shKCNN4-1 targeted the human KCNN4 mRNA sequences (5ʹ-CCGGGCCTGGATGTTCTACAAACATCTCGAGATGTTTGTAGAACATCCAGGCTTTTTG-3ʹ) and shKCNN4-2 targeted the human KCNN4 mRNA sequences (5′-CCGGCGCTCTCAATCAAGTCCGCTTCTCGAGAAGCGGACTTGATTGAGAGCGTTTTTG-3ʹ). All the siRNA were purchased from GenePharma. SiKCNN4 targeted the human KCNN4 mRNA sequences (5ʹ-GCCGUGCGUGCAGGAUUUA-3ʹ) [15], sicJun-1 and sicJun-2 targeted the human cJun sequences (5ʹ-UCAUCUGUCACGUUCUUGGTT-3ʹ) and (5ʹ-CAGCUUCCUGCCUUUGUAATT-3ʹ) [24, 25], siMET-1 and siMET-2 targeted the human MET sequences (5ʹ-GUGUUGUAUGGUCAAUAACTT-3ʹ) and (5ʹ-CGGAUAUCAGCGAUCUUCUTT-3ʹ) [19] and the negative control sequence was (5ʹ-UUCUCCGAACGUGUCACGUTT-3ʹ).
Wound-healing assay
PDAC cells were plated in 6-well plates (each sample repeated 3 times) at a suitable density and cultured with DMEM containing 1% FBS and a wound was manually scratched by a sterile 10 μL pipette tip. After 24 h and 48 h, each wound was pictured in five random fields under a Fluorescence Inversion Microscope.
Cell cycle analysis
The cells were grown in a 6-well plate, and each sample was repeated 3 times. After 72 h, the cells were respectively collected and then fixed with ice-cold 75% ethanol overnight. After that, the cells were treated with RNase A and stained with PI. Finally, the detection by flow cytometry and the data were analyzed with ModFit software.
Xenograft tumor model
All animal studies were performed according to the animal experiment protocol approved by Nanjing Medical University. ASPC1 cells (5 × 106) stably transfected with KCNN4 knockdown plasmid or control plasmid were subcutaneously injected into the back of NCG mice (for 10 NCG mice), respectively. The tumor volume was measured every week. Five weeks later, the mice were sacrificed (euthanasia), and tumor tissues were excised, measured, and weighed. All efforts were made to minimize the suffering of the animals and the number of animals used.
RNA-sequence
The ASPC1-shNC and ASPC1-shKCNN4 cell lysates were prepared with Trizol, and the global gene expression library was detected by RNA sequencing in Novogene (Beijing, China). Moreover, bioprocess analyses were put into effect with Enrichr tools.
Luciferase reporter assay
HEK293T cells were plated into 12-well plates (4 × 105 cells per well) overnight and then co-transfected with reporter plasmid, renilla plasmid and pLVX-JUN (the overexpression of JUN) plasmid for 48 h. Then, the cells were lysed, and the luciferase activity was measured with a dual-luciferase reporter assay system (Promega).
FLUO-3 AM staining
ASPC1-shNC and ASPC1-shKCNN4 cells were grown in a confocal dish (5 × 105 cells per well), the next step was according to the manufacturer’s protocol. Then, the cells were analyzed by laser scanning confocal microscope.
Statistical analysis
All data were analyzed by the GraphPad Prism software and presented as the mean ± SEM. The Student’s t test (two-tailed) was used for comparison among groups. P value < 0.05 was considered statistically significant.
Results
KCNN4 regulated by AP-1 was significantly up-regulated and predicted a poor prognosis in PDAC
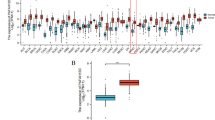
To understand the role of potassium channels in PDAC, we examined 24 potassium channel genes in paired PDAC tissues. The heatmap showed the significantly dysregulated potassium channel genes in PDAC and matched normal tissues. Among them, KCNN4 was identified to be the most significantly overexpressed potassium channel gene in PDAC (Fig. 1a, b). Consistently, we further analyzed the expression profile of KCNN4 by Gene Expression Omnibus (GEO) dataset (GSE16515, GSE28735, GSE15471) containing expression profile data of 100 microdissected PDAC and matching normal pancreatic tissue samples (Fig. S1a). We also observed that the expression of KCNN4 was enhanced significantly in PDAC tumor tissues. Meanwhile, the expression of KCNN4 in different malignancy was examined in the TCGA database, which also showed that the level of KCNN4 was increased obviously in PDAC (Fig. S1b). To confirm that, the expression of KCNN4 in PDAC clinical tissues (Table S1) and cell lines were further analyzed by immunohistochemistry, Western blotting and qPCR. As shown in Fig. 1c, d and Fig. S1c, d, the expression of KCNN4 significantly increased in PDAC clinical tissues and PDAC cell lines. Besides, we found that the overexpression of KCNN4 was closely correlated with a poor outcome of PDAC patients analyzed from the TCGA dataset (Fig. 1e), which revealed that KCNN4 is an unfavorable factor of PDAC.
a The heatmap showed the different expression patterns of 24 potassium channel genes in the PDAC tumor tissues (T) and matched normal (MN) tissues based on the clinical sample expression profile data. b KCNN4 was identified to be the most significantly overexpressed potassium channel gene in PDAC. c The level of KCNN4 in clinical PDAC tissue section was detected by immunohistochemical staining. d The level of KCNN4 in normal pancreatic cells HPNE and PDAC cell lines was assessed by Western blotting. e Overexpression KCNN4 was associated with poor survival of PDAC patients analyzed from OncoLnc-linked TCGA database. f Three AP-1 conjectural binding sites in the promoter region of KCNN4 were identified by analysis with JASPAR and PROMO databases. g HEK293T cells were co-transfected with pGL3-KCNN4 reporter plasmid, renilla plasmid, pLVX-zsgreen plasmid or pLVX-JUN plasmid, luciferase activities were detected with a dual-luciferase reporter assay system. h PDAC cell lines were treated with or without AP-1 inhibitor (SP600125, 20 μM) for 6 h or 12 h, the mRNA level of KCNN4 was detected by qPCR. i PDAC cell lines were treated with AP-1 inhibitor (SP600125, 20 μM) for 48 h, the level of KCNN4 was detected by Western blotting. j Knockdown or overexpression of c-Jun in PDAC cells, the levels of c-Jun and KCNN4 were detected by Western blotting. Data are shown as mean ± SEM. **P < 0.01; ***P < 0.001.
To illustrate the underlying mechanisms of KCNN4-related overexpression in PDAC, 2000 bp promoter regions of KCNN4 were analyzed by PROMO and JASPAR databases. We found that three putative activator protein-1 (AP-1, it has been reported to be overexpressed in human PDAC [26]) binding sequences (TGAGACA, TGAGTGA and TGACTCT) upstream to the TSS (transcription start site) of KCNN4 (Fig. 1f). To verify whether KCNN4 expression was regulated by AP-1 in PDAC, the activity of the KCNN4 promoter was examined by luciferase reporter assay, we found that the transcription of luciferase gene controlled by KCNN4 promoter was activated by AP-1 (Fig. 1g). Similarly, when used SP600125 (AP-1 inhibitor) [24, 27] to treat the PDAC cell lines (ASPC1, PANC1 and SW1990) or knockdown c-Jun by small interfering RNA (siRNA), the level of KCNN4 was markedly inhibited. Whereas, when AP-1 was overexpressed in ASPC1 cells, the levels of KCNN4 and JUN were up-regulated (Figs. 1h–j, S1e–h). Taken together, these results suggested that KCNN4 was overexpressed in PDAC, and its elevation was regulated by AP-1.
KCNN4 regulates cell growth and proliferation of PDAC
To investigate the biological functions of KCNN4 in PDAC, we initially constructed two short hairpin RNAs (shRNA) and siRNA targeting KCNN4 to specifically knockdown the expression of KCNN4 or overexpression of KCNN4 in PDAC cells (Figs. 2a, S2a–d). CCK8 assay, trypan blue staining assay, and colony formation assay revealed that knockdown of KCNN4 significantly suppressed the proliferation of PDAC cells (Fig. 2b–f). Consistent with these, overexpression of KCNN4 dramatically promotes the proliferation of PDAC cells (Fig. 2g). Besides, we found that knockdown of KCNN4 significantly suppressed cell growth, while re-expressed KCNN4 in KCNN4-knockdown ASPC1 cells restored the growth of cells (Fig. 2h). These results proved that KCNN4 promotes the proliferation of PDAC cells in vitro. Likewise, to verify this function in vivo, ASPC1 cells with stable knockdown of KCNN4 or transformed with the control vector were subcutaneously injected into the back of NCG mice, then the lower tumor weight and volume were observed in the knockdown of the KCNN4 group compared with the control group (Fig. 2i). These results showed that the knockdown of KCNN4 suppressed tumor growth in vivo.
a Knockdown or overexpression of KCNN4 in ASPC1 or SW1990 cells, the level of KCNN4 was assessed by Western blotting. b Knocking down KCNN4 in ASPC1 cells by shRNA, the growth or the viability of the cells was measured by trypan blue staining or CCK8 assay. c Silencing KCNN4 in PANC1 cells by shRNA, the growth or the viability of the cells was measured by trypan blue staining or CCK8 assay. d SW1990 cells were transfected with negative control siRNA or KCNN4-specific siRNA to knockdown KCNN4, the growth or the viability of the cells was measured by trypan blue staining or CCK8 assay. e Silencing KCNN4 in ASPC1 cells by shRNA, the growth of cells was measured by colony formation assay. f Knockdown of KCNN4 in PANC1 cells by shRNA, the growth of cells was measured by colony formation assay. g The overexpression of KCNN4 in ASPC1 and PANC1 cells by transfected with plenti-KCNN4 plasmid, the growth of the cells was measured by trypan blue staining. h Silencing KCNN4 or re-expression of KCNN4 in ASPC1 cells, the mRNA level of KCNN4 was assessed by qPCR, and the viability of the cells was detected by CCK8 assay. i Knockdown plasmid of KCNN4 in ASPC1 cells was subcutaneously injected into NCG mice, the tumor volumes were measured every week, and the tumor weights were measured after 5 weeks inoculation. Data are shown as mean ± SEM. *P < 0.05; **P < 0.01; ***P < 0.001.
KCNN4 promoted the migration, invasion, and epithelial-mesenchymal transition of PDAC
Considering that PDAC is more prone to metastasis, we further assessed whether KCNN4 affected the migration and invasion of PDAC cells. Transwell assay proved that knockdown of KCNN4 dramatically suppressed the migration and invasion of PDAC cells (Figs. 3a, S3a, b), while overexpression of KCNN4 promoted this process (Figs. 3b, S3c). Besides, wound healing assay also confirmed that knockdown of KCNN4 attenuated the motility of PDAC cells (Figs. 3c, S3d). The epithelial-mesenchymal transition (EMT) has been reported to drive morphogenesis and initiate tumor progression [28]. Thus, we detected the expression of EMT-related markers (E-cadherin and vimentin) in ASPC1 cells by immunoblotting. As shown in Figs. 3d, S3e, knockdown of KCNN4 dramatically suppressed the process of EMT, while overexpression of KCNN4 accelerated the process of EMT. Immunofluorescence assay has further confirmed these results (Fig. 3e). Taken together, our results demonstrate that KCNN4 promotes the EMT and motility of PDAC.
a The migrated or invasive cells after knockdown of KCNN4 by shRNA in ASPC1 cells were measured by transwell assay with or without matrigel, scale bar, 200 μm, and the viability of the cells was measured by CCK8 assay. b The migrated or invasive of KCNN4-overexpressed PANC1 cells were measured by transwell assay with or without matrix, scale bar, 200 μm, and the viability of the cells was measured by CCK8 assay. c After silencing KCNN4 in ASPC1 cells, the migration ability was examined by wound healing assay, scale bar, 500 μm. d Western blotting was used to detect the levels of KCNN4 and the EMT markers (E-cadherin and vimentin). e Immunofluorescence staining of E-cadherin (Red), vimentin (Green), and DAPI (Blue) in ASPC1 cells analyzed by laser scanning confocal microscope, scale bar, 50 μm. Data are shown as mean ± SEM. *P < 0.05; **P < 0.01; ***P < 0.001.
Knockdown of KCNN4 promoted apoptosis and induced S cell cycle arrest in PDAC
Given that apoptotic resistance and rapid cell division are common characteristics of tumor progression, we sought to determine whether KCNN4 regulates the apoptosis and cell cycle of PDAC. TUNEL staining assay revealed that the percentage of TUNEL-positive cells was increased in KCNN4-knockdown ASPC1 cells (Fig. 4a). Similarly, more TUNEL-positive cells were found in the xenograft tumors generated by ASPC1-shKCNN4 cells (Fig. 4b). Moreover, flow cytometry experiments also confirmed that silencing KCNN4 dramatically increased the percentage of apoptosis of PANC1 and ASPC1 cells (Figs. 4c, S4a), suggesting that the deficiency of KCNN4 increased apoptosis in PDAC cells. To evaluate the impact of KCNN4 on the cell cycle in PDAC, cells were stained with propidium iodide (PI) and examined using flow cytometry. As shown in Figs. 4d, S4b, knockdown of KCNN4 in PANC1 and ASPC1 cells led to fewer cells in the G1 phase and more cells in the S phase. Taken together, these findings suggest that the deficiency of KCNN4 promoted apoptosis and induced cell cycle arrest in the S phase in PDAC cells.
a Knockdown of KCNN4 in ASPC1 cells using shRNA, and the percentage of apoptotic cells was analyzed by TUNEL assay, scale bar, 50 μm. b TUNEL assay analysis of apoptosis in tumor xenografts generated by subcutaneous injection of ASPC1-shKCNN4 cells in NCG mice, scale bar, 50 μm. c Knockdown of KCNN4 in PANC1 cells using shRNA, the percentage of apoptotic cells was detected by Annexin V-FITC/PI staining assay. d KCNN4 in PANC1 cells was silenced using shRNA, and the cell cycle was detected by flow cytometry. Data are shown as mean ± SEM. **P < 0.01; ***P < 0.001.
KCNN4 facilitated the progression of PDAC by regulating MET/AKT pathway
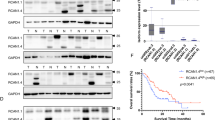
The biological mechanism of how KCNN4 promotes the progression of PDAC is still unclear. To determine these, we investigated the genes, which are significantly associated with KCNN4 expression based on the TCGA database, and the genes were subjected to pathway enrichment analysis. Pathway enrichment analysis shows that the AKT pathway had a close correlation with downstream of KCNN4 (Fig. 5a). To further confirm the mechanism of KCNN4 in PDAC, an RNA sequence was performed using control and KCNN4-knockdown ASPC1 cells to analyze the differentially expressed genes, and the genes whose expression was down-regulated more than 2 folds were used to pathway enrichment. The results confirmed that the AKT pathway had a close correlation with KCNN4 (Fig. S5a). Interestingly, MET as a classical upstream mediator of the AKT pathway [19, 20], was enriched in the AKT pathway in the RNA sequence results (Fig. 5b). Besides, correlation analyses based on the TCGA database and the immunoblotting result showed that the expression of KCNN4 was closely associated with that of MET (Figs. 5c, S5b). Immunoblotting revealed that MET was also overexpressed in PDAC cell lines (Figs. 5d, S5c). Based on these, we hypothesized that the MET/AKT pathway is involved in facilitation of the progression of PDAC by KCNN4. To support this notion, we silenced KCNN4 in ASPC1 cells and found that knockdown of KCNN4 significantly reduced the levels of MET and phosphorylated AKT, while re-expressed KCNN4 restored this process, but the expression of ERK and p-ERK was not affected (Figs. 5e, S5d, e). Similarly, IHC staining confirmed that the levels of MET and phosphorylated AKT were markedly reduced in tumor xenografts induced by subcutaneous inoculation of ASPC1-shKCNN4 cells (Fig. 5f). Moreover, the immunoblotting assay showed that the deficiency of MET suppressed the phosphorylation of AKT, while overexpression of MET enhanced the level of p-AKT (Figs. 5g, S5f, g). Moreover, according to the results of the Western blots, silencing KCNN4 reduced MET expression, while knocking down MET did not affect the protein level of KCNN4. This indicates that KCNN4 is upstream of MET, and MET did not regulate KCNN4 with negative feedback. CCK8 and transwell assay showed that knockdown of MET significantly suppressed the proliferation and migration of PDAC cells (Fig. 6a–c). Besides, the overexpression of KCNN4 in PANC1 cells promoted proliferation and migration, which were significantly inhibited when these cells were treated with siMET (Fig. 5h, i). Thus, these data indicate that KCNN4 facilitates PDAC progression through regulating MET/AKT pathway.
a Pathway enrichment analysis of the genes highly related to KCNN4 expression, based on the TCGA database. b Heatmap representation of genes differentially expressed in KCNN4-knockdown ASPC1 cells identified by RNA-seq. c The correlation between KCNN4 and MET was analyzed based on TCGA database. d The protein levels of MET in HPNE and PDAC cell lines were assessed by Western blotting. e KCNN4-knockdown ASPC1 cells were reconstituted by infection of KCNN4-overexpression lentivirus, the protein levels of KCNN4, MET, AKT, p-AKT, ERK and p-ERK were detected by immunoblotting. f The levels of KCNN4, MET, AKT and p-AKT were assessed by immunohistochemical staining in tumor xenografts generated by subcutaneous injection of ASPC1-shKCNN4 cells in NCG mice. g After knockdown or overexpression of MET in ASPC1 cells, the levels of KCNN4, MET, AKT and the phosphorylation of AKT were detected by immunoblotting. h KCNN4-overexpression and control PANC1 cells were treated with or without siMET, the migration of cells was measured by transwell assay, scale bar, 200 μm, and the viability of the cells was measured by CCK8. i KCNN4-overexpression and control PANC1 cells were treated with or without siMET, the viability of the cells was measured by CCK8. Data are shown as mean ± SEM. ***P < 0.001.
a Knockdown of KCNN4 by shRNA or inhibition of KCNN4 with TRAM-34, the intracellular calcium was measured by FLUO-3 AM staining, scale bar, 50 μm. b ASPC1 and SW1990 cells were treated with indicated concentrations of BAPTA for 24 h, the levels of KCNN4, MET, AKT and p-AKT were examined by Western blotting, and the expression levels in ASPC1 cells were quantified and normalized using Image J analysis software. c ASPC1 and SW1990 cells were treated with indicated concentrations of 1-EBIO, the levels of MET, AKT and p-AKT were examined by Western blotting, and the expression levels in ASPC1 cells were quantified and normalized using Image J analysis software. d SW1990 cells were treated with BAPTA, and the viability of cells was measured by CCK8 assay. e SW1990 cells were treated with BAPTA, and the migration of cells was measured by transwell assay, scale bar, 200 μm. Data are shown as mean ± SEM. *P < 0.05; **P < 0.01; ***P < 0.001.
KCNN4 modulated MET expression by controlling intracellular Ca2+ concentration
We then sought to get a more profound understanding of the way that KCNN4 regulates the expression of MET in PDAC. Previous studies showed that KCNN4 activation induces an increased calcium influx in cancer cells and then promotes the development of cancers [9, 16]. To determine whether the calcium influx is involved in the expression of MET, we first validated whether KCNN4 regulates the intracellular Ca2+ concentration in PDAC. As shown in Fig. 6a, knockdown of KCNN4 by shRNA or treatment with TRAM-34 (KCNN4 inhibitor) in ASPC1 cells dramatically suppressed the calcium mobilization. We then treated PDAC cells with a calcium chelating agent (BAPTA) to chelate intracellular Ca2+, and the levels of MET and p-AKT were assessed by immunoblotting. As shown in Figs. 6b and S6d, e, BAPTA dose-dependently suppressed the expression of MET and the phosphorylation of AKT. Consistent with these findings, calcium activator (1-EBIO) significantly facilitated the expression of MET and the phosphorylation of AKT in PDAC cells (Figs. 6c, S6f). These results demonstrate that KCNN4-modulated MET expression is dependent on calcium mobilization. Importantly, the proliferation and migration of PDAC cells were dose-dependently decreased by BAPTA (Figs. 6d, e, S6g–i), suggesting that calcium mobilization is essential for KCNN4 to activate the MET/AKT pathways and accelerate the progression of PDAC.
TRAM-34 impeded the proliferation and migration of PDAC cells
The aforementioned results encouraged us to evaluate the therapeutic role of KCNN4 in PDAC. As the most commonly used inhibitor of KCNN4, TRAM-34 was selected to treat PDAC cells [13, 29]. Western blotting showed that TRAM-34 significantly alleviated the levels of KCNN4, MET, and phosphorylated AKT (Figs. 7a, S7a). Most strikingly, CCK8, colony formation, and transwell assays showed that inhibition of KCNN4 by TRAM-34 dramatically attenuated both proliferation and migration of PDAC cells, while only slightly reduced the growth of the normal pancreatic cells (HPNE cells) (Figs. 7b–d, S7b, c). Moreover, to confirm the effect of TRAM-34 in vivo, ASPC1 cells were subcutaneously injected into the back of NCG mice. After 2 weeks, the mice were treated with control (DMSO) or TRAM-34, then the lower tumor weight and volume were observed in the TRAM-34 group compared with the control group (Fig. 7e). Thus, these studies imply that KCNN4 may be a therapeutic target for PDAC.
a ASPC1 and PANC1 cells were treated with indicated concentrations of TRAM-34, the levels of KCNN4, MET, AKT, and p-AKT were examined by Western blotting, and the expression levels in ASPC1 cells were quantified and normalized using Image J analysis software. b HPNE, PANC1, ASPC1, and SW1990 cells were treated with indicated concentrations of TRAM-34, and the viability of cells was measured by CCK8 assay. c ASPC1 cells were treated with indicated concentrations of TRAM-34, and the growth of cells was measured by colony formation assay. d ASPC1 cells were treated with TRAM-34, and the migration of cells was measured by transwell assay, scale bar, 200 μm, and the viability of the cells was measured by CCK8. e ASPC1 cells were subcutaneously injected into NCG mice, after 2 weeks, control (DMSO) or TRAM-34 was intraperitoneally injected every other day, then the tumor weights and volume were measured after 5 weeks inoculation. Data are shown as mean ± SEM. *P < 0.05; **P < 0.01; ***P < 0.001.
Discussion
In this study, we reported that KCNN4 plays an important role in the development of PDAC. PDAC is one of the most deadly cancer with a terrible prognosis of a 5-year survival rate of less than 6% [1, 30]. In reality, although largish advances appeared in the diagnosis and treatment of PDAC, no prominently therapeutic strategies have emerged. Therefore, there is an urgent need to find a new treatment scheme for PDAC. Previously, numerous researchers have demonstrated that KCNN4 was closely related to the occurrence and development of malignancy. Although KCNN4 has been involved in the progression of numerous malignancy, the precise mechanism of impact of KCNN4 on the biological processes of PDAC is largely unknown. To investigate the expression and function of KCNN4 in PDAC, we first discovered that KCNN4 was notably upregulated in PDAC and associated with a poor outcome. Subsequently, we found that transcription factor AP-1 is involved in the regulation of KCNN4 overexpression in PDAC. We further demonstrated that overexpression of KCNN4 promoted the growth, metastasis and EMT, while knockdown of KCNN4 caused promoted apoptosis and S phase cell cycle arrest in PDAC. Besides, KCNN4 inhibitor TRAM-34 significantly suppressed the proliferation and metastasis of PDAC cells. Thus, our findings identify that KCNN4 promotes PDAC proliferation and metastasis and provides a new potential strategy for PDAC treatment.
To further explored the precise mechanism of KCNN4 in the progression of PDAC, the RNA sequence results showed that the MET/AKT pathway had a close correlation with downstream of KCNN4. As a critical carcinogenic signaling pathway, MET/AKT signaling pathway has been reported frequently altered in cancers and correlated with the development of PDAC [19, 20, 31, 32]. However, the relationship between KCNN4 and MET/AKT signaling pathway remains to be clarified. Our Western blotting and IHC staining assays revealed that the knockdown of KCNN4 dramatically suppressed the expression of MET and the phosphorylation of AKT. Furthermore, when knockdown of MET, the proliferation and migration ability of PDAC cells were decreased significantly. All these data suggest that KCNN4 is a novel mediator of the MET/AKT signaling pathway.
A key question that comes here is how KCNN4 regulates the expression of MET. Previous studies revealed that intracellular Ca2+ concentration is essential for KCNN4 to promote cancer cell proliferation and metastasis [9, 33]. So, we speculated whether calcium mobilization is involved in the activation of the MET/AKT signaling pathway by KCNN4. Our results proved that knockdown or inhibition of KCNN4 dramatically suppressed the calcium mobilization in PDAC cells and chelating intracellular Ca2+ reduced the expression of MET and the phosphorylation of AKT. Therefore, our data suggest that calcium mobilization is essential for KCNN4 to activate the MET/AKT signaling pathway.
Conclusions
In conclusion, we emphasized a new molecule mechanism, in which KCNN4 aberrantly up-regulates MET by controlling intracellular Ca2+ concentration, and the up-regulated MET significantly activated the AKT signaling pathway, which subsequently promotes PDAC proliferation and metastasis. Our findings provide a novel insight into the roles of KCNN4 in inducing progression of PDAC, which could lead to the development of a potential biomarker and therapeutic target for PDAC therapy.
References
Ling J, Chiao PJ. Two birds with one stone: therapeutic targeting of IL1alpha signaling pathways in pancreatic ductal adenocarcinoma and the cancer-associated fibroblasts. Cancer Discov. 2019;9:173–5.
Zhang J, Yang J, Lin C, Liu W, Huo Y, Yang M, et al. Endoplasmic reticulum stress-dependent expression of ERO1L promotes aerobic glycolysis in pancreatic cancer. Theranostics. 2020;10:8400–14.
Luna J, Boni J, Cuatrecasas M, Bofill-De Ros X, Núñez-Manchón E, Gironella M, et al. DYRK1A modulates c-MET in pancreatic ductal adenocarcinoma to drive tumour growth. Gut. 2019;68:1465–76.
Shi Y, Gao W, Lytle NK, Huang P, Yuan X, Dann AM, et al. Targeting LIF-mediated paracrine interaction for pancreatic cancer therapy and monitoring. Nature. 2019;569:131–35.
Yin L, Pu N, Thompson ED, Miao Y, Wolfgang CL, Yu J. Improved assessment of response status in patients with pancreatic cancer treated with neoadjuvant therapy using somatic mutations and liquid biopsy analysis. Clin Cancer Res. 2021;27:740–8.
Wang Z, Qin J, Zhao J, Li J, Li D, Popp M, et al. Inflammatory IFIT3 renders chemotherapy resistance by regulating post-translational modification of VDAC2 in pancreatic cancer. Theranostics. 2020;10:7178–92.
Ding L, Madamsetty VS, Kiers S, Alekhina O. Glycogen synthase kinase-3 inhibition sensitizes pancreatic cancer cells to chemotherapy by abrogating the TopBP1/ATR-mediated DNA damage response. Clin Cancer Res. 2019;25:6452–62.
Grbovic-Huezo O, Pitter KL, Lecomte N, Saglimbeni J, Askan G, Holm M. Unbiased in vivo preclinical evaluation of anticancer drugs identifies effective therapy for the treatment of pancreatic adenocarcinoma. Clin Cancer Res. 2020;27:740–8.
Lallet-Daher H, Roudbaraki M, Bavencoffe A, Mariot P, Gackière F, Bidaux G, et al. Intermediate-conductance Ca2+-activated K+ channels (IKCa1) regulate human prostate cancer cell proliferation through a close control of calcium entry. Oncogene. 2009;28:1792–806.
Kang H, Kerloc’h A, Rotival M, Xu X, Zhang Q, D’Souza Z, et al. Kcnn4 is a regulator of macrophage multinucleation in bone homeostasis and inflammatory disease. Cell Rep. 2014;8:1210–24.
Grössinger EM, Kang M, Bouchareychas L. Ca2+-dependent regulation of NFATc1 via KCa3.1 in inflammatory osteoclastogenesis. J Immunol. 2018;200:749–57.
Bulk E, Ay AS, Hammadi M, Ouadid-Ahidouch H, Schelhaas S, Hascher A, et al. Epigenetic dysregulation of KCa 3.1 channels induces poor prognosis in lung cancer. Int J Cancer. 2015;137:1306–17.
Turner KL, Honasoge A, Robert SM, McFerrin MM, Sontheimer H. A proinvasive role for the Ca2+-activated K+ channel KCa3.1 in malignant glioma. Glia. 2014;62:971–81.
Du Y, Song W, Chen J, Chen H, Xuan Z, Zhao L, et al. The potassium channel KCa3.1 promotes cell proliferation by activating SKP2 and metastasis through the EMT pathway in hepatocellular carcinoma. Int J Cancer. 2019;145:503–16.
Lai W, Liu L, Zeng Y, Wu H, Xu H, Chen S, et al. KCNN4 channels participate in the EMT induced by PRL-3 in colorectal cancer. Med Oncol. 2013;30:566.
Wang ZH, Shen B, Yao HL, Jia YC, Ren J, Feng YJ, et al. Blockage of intermediate-conductance-Ca2+-activated K+ channels inhibits progression of human endometrial cancer. Oncogene. 2007;26:5107–14.
Gherardi E, Birchmeier W, Birchmeier C, Vande Woude G. Targeting MET in cancer: rationale and progress. Nat Rev Cancer. 2012;12:89–103.
Esfahani SA, Heidari P, Kim SA, Ogino S, Mahmood U. Optical imaging of mesenchymal epithelial transition factor (MET) for enhanced detection and characterization of primary and metastatic hepatic tumors. Theranostics. 2016;6:2028–38.
Guo X, Zhou Q, Su D, Luo Y, Fu Z, Huang L, et al. Circular RNA circBFAR promotes the progression of pancreatic ductal adenocarcinoma via the miR-34b-5p/MET/Akt axis. Mol Cancer. 2020;19:83.
Liu H, Deng H, Zhao Y, Li C, Liang Y. LncRNA XIST/miR-34a axis modulates the cell proliferation and tumor growth of thyroid cancer through MET-PI3K-AKT signaling. J Exp Clin Cancer Res. 2018;37:279.
Fang C, Guo X, Lv X, Yin R, Lv X, Wang F, et al. Dysbindin promotes progression of pancreatic ductal adenocarcinoma via direct activation of PI3K. J Mol Cell Biol. 2017;9:504–15.
Chen Y, Bai X, Zhang Q, Wen L, Su W, Fu Q, et al. The hepatitis B virus X protein promotes pancreatic cancer through modulation of the PI3K/AKT signaling pathway. Cancer Lett. 2016;380:98–105.
Chalabi-Dchar M, Cassant-Sourdy S, Duluc C, Fanjul M, Lulka H, Samain R, et al. Loss of somatostatin receptor subtype 2 promotes growth of KRAS-induced pancreatic tumors in mice by activating PI3K signaling and overexpression of CXCL16. Gastroenterology. 2015;148:1452–65.
Du S, Li Z, Xie X, Xu C, Shen X, Wang N, et al. IL-17 stimulates the expression of CCL2 in cardiac myocytes via Act1/TRAF6/p38MAPK-dependent AP-1 activation. Scand J Immunol. 2020;91:e12840.
Sun D, Zhang M, Li Y, Mei S, Qin J, Yan J. c-Jun/Ap1 is upregulated in an Ang II induced abdominal aortic aneurysm formation model and mediates Chop expression in mouse aortic smooth muscle cells. Mol Med Rep. 2019;19:3459–68.
Park J, Eisenbarth D, Choi W, Kim H, Choi C, Lee D, et al. YAP and AP-1 cooperate to initiate pancreatic cancer development from ductal cells in mice. Cancer Res. 2020;80:4768–79.
Guo L, Guo Y, Xiao S, Shi X. Protein kinase p-JNK is correlated with the activation of AP-1 and its associated Jun family proteins in hepatocellular carcinoma. Life Sci. 2005;77:1869–78.
Thiery JP, Acloque H, Huang RY, Nieto MA. Epithelial-mesenchymal transitions in development and disease. Cell. 2009;139:871–90.
Bonito B, Sauter DR, Schwab A, Djamgoz MB, Novak I. KCa3.1 (IK) modulates pancreatic cancer cell migration, invasion and proliferation: anomalous effects on TRAM-34. Pflug Arch. 2016;468:1865–75.
Chang J, Tian J, Zhu Y, Zhong R, Zhai K, Li J, et al. Exome-wide analysis identifies three low-frequency missense variants associated with pancreatic cancer risk in Chinese populations. Nat Commun. 2018;9:3688.
Massihnia D, Avan A, Funel N, Maftouh M, van Krieken A, Granchi C, et al. Phospho-Akt overexpression is prognostic and can be used to tailor the synergistic interaction of Akt inhibitors with gemcitabine in pancreatic cancer. J Hematol Oncol. 2017;10:9.
Escorcia FE, Houghton JL, Abdel-Atti D, Pereira PR, Cho A, Gutsche NT, et al. ImmunoPET predicts response to met-targeted radioligand therapy in models of pancreatic cancer resistant to met kinase inhibitors. Theranostics. 2020;10:151–65.
Divolis G, Mavroeidi P, Mavrofrydi O, Papazafiri P. Differential effects of calcium on PI3K-Akt and HIF-1α survival pathways. Cell Biol Toxicol. 2016;32:437–49.
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (82072739), The Recruitment Program of Overseas High-Level Young Talents, “Innovative and Entrepreneurial Team” (No. (2018) 2015), Science and Technology Grant (BE2019758), the Six Talent Peaks Project (TD-SWYY-007) and the Natural Science Foundation (BK20190657) of Jiangsu Province; CSCO-Bristol-Myers Squibb Cancer Immunology Research Fund (YBMS2019-071); China Postdoctoral Science Foundation (2019M651897).
Author information
Authors and Affiliations
Contributions
XM, CFZ, and PX equally performed the majority of experiments, analyzed the data and wrote the paper; MD, ZJM, HJX, YL, HKB, and XG helped on some experiments; QS, GRZ, and YLJ provide clinical samples and critical discussion; CH and AA support on analysis and revision; XM, CFZ, and HPX designed the research and summarized the data. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Rights and permissions
About this article
Cite this article
Mo, X., Zhang, Cf., Xu, P. et al. KCNN4-mediated Ca2+/MET/AKT axis is promising for targeted therapy of pancreatic ductal adenocarcinoma. Acta Pharmacol Sin 43, 735–746 (2022). https://doi.org/10.1038/s41401-021-00688-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-021-00688-3
Keywords
This article is cited by
-
ACYP2 functions as an innovative nano-therapeutic target to impede the progression of hepatocellular carcinoma by inhibiting the activity of TERT and the KCNN4/ERK pathway
Journal of Nanobiotechnology (2024)
-
Establishment of a prognostic model for pancreatic cancer based on mitochondrial metabolism related genes
Discover Oncology (2024)
-
Predicting tumor repopulation through the gene panel derived from radiation resistant colorectal cancer cells
Journal of Translational Medicine (2023)
-
CHKB-AS1 enhances proliferation and resistance to NVP-BEZ235 of renal cancer cells via regulating the phosphorylation of MAP4 and PI3K/AKT/mTOR signaling
European Journal of Medical Research (2023)
-
A potent ion channel blocker, hydroquinidine, exhibits strong anti-cancer activity on colon, pancreatic, and hepatocellular cancer cells
Molecular Biology Reports (2023)