Abstract
Background/Objectives
Ostracism may lead to increased food intake, yet it is unclear whether greater reactivity to ostracism contributes to higher body mass index (BMI). We investigated whether children who exhibited greater stress to social exclusion subsequently consume more energy and whether this predicts BMI 6- and 18-months later.
Subjects/Methods
Children (8.5 years-old) (N = 262, males = 50.4%; Chinese = 58.4%) completed a laboratory-based manipulation of social exclusion (the Cyberball task) prior to an ad-libitum snack. Heart rate variability (HRV) was measured during the inclusion and exclusion conditions and proportionate changes were calculated as a physiological measure of exclusion-related stress. Social anxiety and social-emotional assets were also measured as moderators.
Results
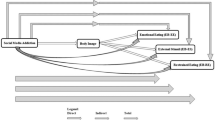
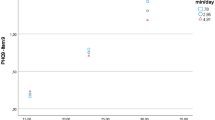
Greater stress (as measured physiologically or by self-report) did not directly, or indirectly via energy intake, predict later BMI (at 9- and 10-years). However, among children reporting higher social anxiety, greater stress as measured by proportionate changes in HRV was associated with increased energy intake (B = 532.88, SE = 226.49, t(255) = 2.35, [CI95 = 86.85,978.92]). A significant moderated mediation was also observed (index: (b = 0.01, bootSE = 0.01, [CI95 = 0.001, 0.036]), such that among children reporting higher social anxiety, greater stress from social exclusion predicted increased energy intake from a subsequent snack, which in turn predicted higher BMI 1.5 years later.
Conclusion
This prospective study suggests that a pattern of greater snack intake in response to heightened vulnerability to the effects of ostracism may contribute to increases in child BMI scores.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
All materials and data are not in the public domain but can be requested by contacting the corresponding authors. The design and analysis plans were not preregistered.
References
Williams, KD (2007). Ostracism. In Annual Review of Psychology (58, pp. 425–52). Annual Reviews. https://doi.org/10.1146/annurev.psych.58.110405.085641.
Zadro L, Williams KD, Richardson R. How low can you go? Ostracism by a computer is sufficient to lower self-reported levels of belonging, control, self-esteem, and meaningful existence. J Exp Soc Psychol. 2004;40:560–7.
Abrams D, Weick M, Thomas D, Colbe H, Franklin KM. On-line ostracism affects children differently from adolescents and adults. Br J Dev Psychol. 2011;29:110–23.
Sebastian C, Viding E, Williams KD, Blakemore SJ. Social brain development and the affective consequences of ostracism in adolescence. Brain Cogn. 2010;72:134–45.
Valkenburg PM, Peter J. Preadolescents’ and adolescents’ online communication and their closeness to friends. Developmental Psychol. 2007;43:267–77.
Arslan G. Social Exclusion, Social Support and Psychological Wellbeing at School: A Study of Mediation and Moderation Effect. Child Indicators Res. 2018;11:897–918.
Lim EX, Sim AY, Forde CG, Cheon BK. The role of perceived stress and gender on portion selection patterns. Physiol Behav. 2018;194:205–11.
Sproesser G, Schupp HT, Renner B. The Bright Side of Stress-Induced Eating: Eating More When Stressed but Less When Pleased. Psychol Sci. 2014;25:58–65.
Hayman LW, McIntyre RB, Abbey A. The bad taste of social ostracism: The effects of exclusion on the eating behaviors of African-American women. Psychol Health. 2015;30:518–33.
Oliver G, Wardle J. Perceived effects of stress on food choice. Physiol Behav. 1999;66:511–5.
Oliver G, Wardle J, Gibson EL. Stress and food choice: A laboratory study. Psychosomatic Med. 2000;62:853–65.
Torres SJ, Nowson CA. Relationship between stress, eating behaviour and obesity. Nutrition. 2007;23:887–94.
Caspi A, Harrington HL, Moffitt TE, Milne BJ, Poulton R. Socially isolated children 20 years later: Risk of cardiovascular disease. Arch Pediatr Adolescent Med. 2006;160:805–11.
Pink AE, Lee M, Price M, Williams C. A serial mediation model of the relationship between alexithymia and BMI: The role of negative affect, negative urgency and emotional eating. Appetite. 2019;133:270–8.
Baumeister RF, Nathan Dewall C, Ciarocco NJ, Twenge JM. Social exclusion impairs self-regulation. J Personality Soc Psychol. 2005;88:589–604.
Oaten M, Williams KD, Jones A, Zadro L. The effects of ostracism on self-regulation in the socially anxious. J Soc Clin Psychol. 2008;27:471–504.
Troisi JD, Gabriel S. Chicken soup really is good for the soul: “Comfort food” fulfills the need to belong. Psychol Sci. 2011;22:747–53.
Tomiyama AJ, Dallman MF, Epel ES. Comfort food is comforting to those most stressed: Evidence of the chronic stress response network in high stress women. Psychoneuroendocrinology. 2011;36:1513–9.
Tryon MS, DeCant R, Laugero KD. Having your cake and eating it too: A habit of comfort food may link chronic social stress exposure and acute stress-induced cortisol hyporesponsiveness. Physiol Behav. 2013;114-5:32–37.
Van Strien T, Roelofs K, De Weerth C. Cortisol reactivity and distress-induced emotional eating. Psychoneuroendocrinology. 2013;38:677–84.
Reinhard MA, Dewald-Kaufmann J, Wüstenberg T, Musil R, Barton BB, Jobst A, et al. The vicious circle of social exclusion and psychopathology: a systematic review of experimental ostracism research in psychiatric disorders. Eur Arch Psychiatry and Clin Neurosci. 2020;270:521–32.
Wölfer R, Scheithauer H. Ostracism in childhood and adolescence: Emotional, cognitive, and behavioral effects of social exclusion. Soc Influence. 2013;8:217–36.
Salvy SJ, Bowker JC, Nitecki LA, Kluczynski MA, Germeroth LJ, Roemmich JN. Effects of ostracism and social connection-related activities on adolescents’ motivation to eat and energy intake. J Pediatr Psychol. 2012;37:23–32.
Salvy SJ, Bowker JC, Nitecki LA, Kluczynski MA, Germeroth LJ, Roemmich JN. Impact of Simulated Ostracism on Overweight and Normal-Weight Youths’ Motivation to Eat and Food Intake. Appetite. 2011;56:39.
Senese VP, Pezzella M, Pasquariello L, Ali S, Rohner RP. Effects of social exclusion and maternal rejection on Children’s high-caloric food consumption. Appetite. 2020;145:104494.
Arias Ramos N, Calvo Sánchez MD, Fernández-Villa T, Ovalle Perandones MA, Fernández García D, Marqués-Sánchez P. Social exclusion of the adolescent with overweight: study of sociocentric social networks in the classroom. Pediatr Obes. 2018;13:614–20.
Hajek A, König HH. The association between obesity and social exclusion in middle-aged and older adults: Findings from a nationally representative study in Germany. BMC Geriatrics. 2018;18:1–7.
Wang ML, Pbert L, Lemon SC. Influence of family, friend and coworker social support and social undermining on weight gain prevention among adults. Obesity. 2014;22:1973–80.
Winston GJ, Phillips EG, Wethington E, Devine C, Wells M, Peterson JC, et al. Social network characteristics associated with weight loss among black and hispanic adults. Obesity. 2015;23:1570–6.
Jackson SL, Cunningham SA. Social Competence and Obesity in Elementary School. Am J Public Health. 2015;105:153.
Hajek A, Kretzler B, König HH. The association between obesity and social isolation as well as loneliness in the adult population: A systematic review. Diab, Metabolic Syndr Obes. 2021;14:2765–73.
Kim HG, Cheon EJ, Bai DS, Lee YH, Koo BH. Stress and Heart Rate Variability: A Meta-Analysis and Review of the Literature. Psychiatry Investig. 2018;15:235.
Zadro L, Boland C, Richardson R. How long does it last? The persistence of the effects of ostracism in the socially anxious. J Exp Soc Psychol. 2006;42:692–7.
Merrell, KW (2011). Social and Emotional Assets and Resilience Scales (SEARS). Psychological Assessment Resources.
Williams, KD (2001). Ostracism: The Power of Silence. New York: Guildford Press.
Hartgerink CHJ, Van Beest I, Wicherts JM, Williams KD. The ordinal effects of ostracism: A meta-analysis of 120 cyberball studies. PLoS ONE. 2015;10:e0127002.
Soh SE, Saw SM, Tint MT, Chong YS, Gluckman PD, Rifkin-Graboi A, et al. Cohort profile: Growing up in Singapore towards healthy outcomes (GUSTO) birth cohort study. Int J Epidemiol. 2014;43:1401–9.
Fogel A, Fries LR, McCrickerd K, Goh AT, Quah PL, Chan MJ, et al. Oral processing behaviours that promote children’s energy intake are associated with parent-reported appetitive traits: Results from the GUSTO cohort. Appetite. 2018;126:8–15.
Bennett C, Blissett J. Measuring hunger and satiety in primary school children. Validation of a new picture rating scale. Appetite. 2014;78:40–8.
Laurent J, Catanzaro SJ, Rudolph KD, Joiner TE, Potter KI, Lambert S, et al. A measure of positive and negative affect for children: Scale development and preliminary validation. Psychol Assess. 1999;11:326–38.
Williams KD, Cheung CKT, Choi W. Cyberostracism: Effects of being ignored over the internet. J Personality Soc Psychol. 2000;79:748–62.
De Geus EJ, Willemsen GH, Klaver CH, van Doornen LJ. Ambulatory measurement of respiratory sinus arrhythmia and respiration rate. Biol Psychol. 1995;41:205–227.
Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Heart rate variability: standards of measurement, physiological interpretation and clinical use. Circulation. 1996;93:1043–65.
Halko ML, Sääksvuori L. Competitive behavior, stress, and gender. J Econ Behav Organization. 2017;141:96–109.
Png IPL, Tan CHY. Cost of Cash. Service Sci. 2021;13:88–108.
Gonsalkorale K, Williams KD. The KKK won’t let me play: Ostracism even by a despised outgroup hurts. Eur J Soc Psychol. 2007;37:1176–86.
Mulder RH, Bakermans-Kranenburg MJ, Veenstra J, Tiemeier H, van IJzendoorn MH. Facing ostracism: micro-coding facial expressions in the Cyberball social exclusion paradigm. BMC Psychol. 2023;11:1–14.
White T, Muetzel RL, El Marroun H, Blanken LME, Jansen P, Bolhuis K, et al. Paediatric population neuroimaging and the Generation R Study: the second wave. Eur J Epidemiol. 2018;33:99.
March, J (2013). The Multidimensional Anxiety Scale for Children (2nd ed.). Multi-Health Systems.
Anant N, Kaur D, Nadarajan R, Phua DY, Chong YS, Gluckman PD, et al. Validating the Children’s Depression Inventory-2: Results from the Growing Up in Singapore Towards Healthy Outcomes (GUSTO) study. PLOS ONE. 2023;18:e0286197.
Kovacs, M (2015). Children’s Depression Inventory (CDI and CDI 2). In The Encyclopedia of Clinical Psychology (pp. 1–5). John Wiley & Sons, Ltd. https://doi.org/10.1002/9781118625392.wbecp419.
WHO. (2007). Growth reference data for 5-19 years. https://www.who.int/toolkits/growth-reference-data-for-5to19-years/application-tools.
Hayes, AF (2018). Introduction to Mediation, Moderation, and Conditional Process Analysis (2nd ed.). Guildford Press.
Williamson VG, Lee AM, Miller D, Huo T, Maner JK, Cardel M. Psychological resilience, experimentally manipulated social status, and dietary intake among adolescents. Nutrients. 2021;13:1–16.
Tomiyama AJ. Weight stigma is stressful. A review of evidence for the Cyclic Obesity/Weight-Based Stigma model. Appetite. 2014;82:8–15.
Salvy S-J, Bowker JC. Peers and Obesity during Childhood and Adolescence: A Review of the Empirical Research on Peers, Eating, and Physical Activity. J Obes Weight Loss Ther. 2014;4:207.
Westermann S, Rief W, Euteneuer F, Kohlmann S. Social exclusion and shame in obesity. Eating Behav. 2015;17:74–6.
Hebebrand J, Hinney A. Environmental and Genetic Risk Factors in Obesity. Child Adolescent Psychiatr Clin North America. 2009;18:83–94.
Masood B, Moorthy M. Causes of obesity: a review. Clin Med. 2023;23:284.
Omer TAM. The causes of obesity: an in-depth review. Adv Obes Weight Manag Control. 2020;10:90–4.
DeWall CN, Baumeister RF.Alone but feeling no pain: Effects social exclusion on physical pain tolerance and pain threshold, affective forecasting, and interpersonal empathy.2006;91:1–15. https://doi.org/10.1037/0022-3514.91.1.1.
Burrows T, Golley RK, Khambalia A, Mcnaughton SA, Magarey A, Rosenkranz R, et al. The quality of dietary intake methodology and reporting in child and adolescent obesity intervention trials: A systematic review. Obes Rev. 2012;13:1125–38.
Burrows TL, Truby H, Morgan PJ, Callister R, Davies PSW, Collins CE. A comparison and validation of child versus parent reporting of children’s energy intake using food frequency questionnaires versus food records: Who’s an accurate reporter? Clin Nutr. 2013;32:613–8.
Holt MK, Kantor GK, Finkelhor D. Parent/child concordance about bullying involvement and family characteristics related to bullying and peer victimization. J School Violence. 2009;8:42–63.
Shemesh E, Annunziato RA, Ambrose MA, Ravid NL, Mullarkey C, Rubes M, et al. Child and parental reports of bullying in a consecutive sample of children with food allergy. Pediatrics. 2013;131:e10.
Acknowledgements
We would like to thank Ang Li Ting for their assistance with data management and Darren Jeffian Wijaya for their assistance with data curation. We would also like to thank and acknowledge the wider GUSTO study group and research assistants, please see supplementary materials and [37] for all members names.
Funding
The study is supported by the National Research Foundation (NRF) under the Open Fund-Large Collaborative Grant (OF-LCG; MOH-000504) administered by the Singapore Ministry of Health’s National Medical Research Council (NMRC) and the Agency for Science, Technology and Research (A*STAR). Any opinions, findings, and conclusions or recommendations expressed in this material are those of the author(s) and do not reflect the views of the A*STAR. In Research, Innovation and Enterprise 2025 (RIE2025), GUSTO is supported by funding from the NRF’s Human Health and Potential (HHP) Domain, under the Human Potential Programme. BKC’s contribution to this manuscript was supported by the Intramural Research Program of the Eunice Kennedy Shriver National Institute of Child Health and Human Development (HD009004-01656312).
Author information
Authors and Affiliations
Contributions
Conceptualization: AEP, RT, BFPB, BKC. Methodology: JYT, YSC, MM, KHT, FY, BFPB, BKC. Investigation: BC, FK, RN, JYP. Resources: JYT, YSC, MM, KHT, FY, BFPB, BKC. Data Curation: AEP, RT, BC, FK, RN, JYP, CHYT. Formal Analysis: AEP, RT. Writing – Original Draft: AEP, RT. Writing – Review and Editing: AEP, RT, BC, FK, RN, JYP, CHYT, JYT, MM, BFPB, BKC. Project administration: BC, FK, RN, JYT.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pink, A.E., Teo, R., Chua, B. et al. The effects of acute social ostracism on subsequent snacking behavior and future body mass index in children. Int J Obes 48, 867–875 (2024). https://doi.org/10.1038/s41366-024-01489-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-024-01489-4