Abstract
Biologic therapies have been licensed to treat rheumatic diseases for more than a decade. In parallel, they have gained acceptance in a variety of non-rheumatic diseases, where their impact has been no less revolutionary. In this Review, we examine the application of biologics in a number of non-rheumatic autoimmune and inflammatory disorders—psoriasis, inflammatory bowel disease, uveitis, asthma, diabetes, congestive cardiac failure and multiple sclerosis. In particular, we have sought information, or lessons, that could influence their application in rheumatic diseases. For example, we highlight the potential to stratify asthma into groups that might require different targeted approaches, and focus on some of the less common adverse events associated with biologic therapies in multiple sclerosis. Similarly, we examine type 1 diabetes mellitus in the context of potential therapeutic induction of immune tolerance. Working collaboratively, across specialties, there is significant synergy to be gained in regard to understanding how biologic therapies work, how best to use them, and the adverse effects we should be conscious of.
Key Points
-
Biologic therapies are increasingly used in non-rheumatic diseases
-
As in rheumatic disease, biologics might provide a therapeutic option for otherwise refractory non-rheumatic disease
-
These agents may also provide proof-of-concept for proposed mechanisms of immunopathology, such as IL-1β blockade in type 2 diabetes mellitus
-
In other situations their effects can be paradoxical, such as worsening of heart failure and occasional induction of psoriasis and uveitis during tumor necrosis factor blockade
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Strand, V., Kimberly, R. & Isaacs, J. D. Biologic therapies in rheumatology: lessons learned, future directions. Nat. Rev. Drug Discov. 6, 75–92 (2007).
Kircik, L. H. & Del Rosso, J. Q. Anti-TNF agents for the treatment of psoriasis. J. Drugs Dermatol. 8, 546–559 (2009).
Brimhall, A. K. et al. Safety and efficacy of alefacept, efalizumab, etanercept and infliximab in treating moderate to severe plaque psoriasis: a meta-analysis of randomized controlled trials. Br. J. Dermatol. 159, 274–285 (2008).
Reich, K. et al. Comparative effects of biological therapies on the severity of skin symptoms and health-related quality of life in patients with plaque-type psoriasis: a meta-analysis. Curr. Med. Res. Opin. 24, 1237–1254 (2008).
Saad, A. A. et al. Efficacy and safety of anti-TNF therapies in psoriatic arthritis: an observational study from the British Society for Rheumatology Biologics Register. Rheumatology (Oxford) 49, 697–705 (2010).
Harrison, M. J. et al. Rates of new-onset psoriasis in patients with rheumatoid arthritis receiving anti-tumour necrosis factor α therapy: results from the British Society for Rheumatology Biologics Register. Ann. Rheum. Dis. 68, 209–215 (2009).
Ko, J. M., Gottlieb, A. B. & Kerbleski, J. F. Induction and exacerbation of psoriasis with TNF-blockade therapy: a review and analysis of 127 cases. J. Dermatolog. Treat. 20, 100–108 (2009).
Malaviya, R. et al. Etanercept induces apoptosis of dermal dendritic cells in psoriatic plaques of responding patients. J. Am. Acad. Dermatol. 55, 590–597 (2006).
Goedkoop, A. Y. et al. Early effects of tumour necrosis factor α blockade on skin and synovial tissue in patients with active psoriasis and psoriatic arthritis. Ann. Rheum. Dis. 63, 769–773 (2004).
Purvis, H. A. et al. Low-strength T-cell activation promotes Th17 responses. Blood 116, 4829–4837 (2010).
Chan, J. R. et al. IL-23 stimulates epidermal hyperplasia via TNF and IL-20R2-dependent mechanisms with implications for psoriasis pathogenesis. J. Exp. Med. 203, 2577–2587 (2006).
Ma, H. L. et al. IL-22 is required for Th17 cell-mediated pathology in a mouse model of psoriasis-like skin inflammation. J. Clin. Invest. 118, 597–607 (2008).
Leonardi, C. L. et al. Efficacy and safety of ustekinumab, a human interleukin-12/23 monoclonal antibody, in patients with psoriasis: 76-week results from a randomised, double-blind, placebo-controlled trial (PHOENIX 1). Lancet 371, 1665–1674 (2008).
Papp, K. A. et al. Efficacy and safety of ustekinumab, a human interleukin-12/23 monoclonal antibody, in patients with psoriasis: 52-week results from a randomised, double-blind, placebo-controlled trial (PHOENIX 2). Lancet 371, 1675–1684 (2008).
Griffiths, C. E. et al. Comparison of ustekinumab and etanercept for moderate-to-severe psoriasis. N. Engl. J. Med. 362, 118–128 (2010).
Kimball, A. B. et al. Safety and efficacy of ABT-874, a fully human interleukin 12/23 monoclonal antibody, in the treatment of moderate to severe chronic plaque psoriasis: results of a randomized, placebo-controlled, phase 2 trial. Arch. Dermatol. 144, 200–207 (2008).
National Electronic Library for Medicines. Marketing authorisation application for briakinumab (Ozespa®) withdrawn [online], (2011).
Hanauer, S. B. et al. Maintenance infliximab for Crohn's disease: the ACCENT I randomised trial. Lancet 359, 1541–1549 (2002).
Rutgeerts, P. et al. Infliximab for induction and maintenance therapy for ulcerative colitis. N. Engl. J. Med. 353, 2462–2476 (2005).
Sands, B. E. et al. Infliximab maintenance therapy for fistulizing Crohn's disease. N. Engl. J. Med. 350, 876–885 (2004).
Hanauer, S. B. et al. Human anti-tumor necrosis factor monoclonal antibody (adalimumab) in Crohn's disease: the CLASSIC-I trial. Gastroenterology 130, 323–333 (2006).
Sandborn, W. J. et al. Certolizumab pegol for the treatment of Crohn's disease. N. Engl. J. Med. 357, 228–238 (2007).
Sandborn, W. J. et al. Etanercept for active Crohn's disease: a randomized, double-blind, placebo-controlled trial. Gastroenterology 121, 1088–1094 (2001).
Taylor, P. C. Pharmacology of TNF blockade in rheumatoid arthritis and other chronic inflammatory diseases. Curr. Opin. Pharmacol. 10, 308–315 (2010).
Nesbitt, A. et al. Mechanism of action of certolizumab pegol (CDP870): in vitro comparison with other anti-tumor necrosis factor alpha agents. Inflamm. Bowel Dis. 13, 1323–1332 (2007).
ten Hove, T. et al. Infliximab treatment induces apoptosis of lamina propria T lymphocytes in Crohn's disease. Gut 50, 206–211 (2002).
Di Sabatino, A. et al. Defective mucosal T cell death is sustainably reverted by infliximab in a caspase dependent pathway in Crohn's disease. Gut 53, 70–77 (2004).
Stallmach, A., Hagel, S. & Bruns, T. Adverse effects of biologics used for treating IBD. Best Pract. Res. Clin. Gastroenterol. 24, 167–182 (2010).
FDA. Questions and Answers—TNF Blockers [online], (2009).
Siegel, C. A. et al. Risk of lymphoma associated with combination anti-tumor necrosis factor and immunomodulator therapy for the treatment of Crohn's disease: a meta-analysis. Clin. Gastroenterol. Hepatol. 7, 874–881 (2009).
Van Assche, G. et al. Withdrawal of immunosuppression in Crohn's disease treated with scheduled infliximab maintenance: a randomized trial. Gastroenterology 134, 1861–1868 (2008).
Dick, A. D. et al. Neutralizing TNF-alpha activity modulates T-cell phenotype and function in experimental autoimmune uveoretinitis. J. Autoimmun. 11, 255–264 (1998).
Robertson, M. et al. Neutralizing tumor necrosis factor-α activity suppresses activation of infiltrating macrophages in experimental autoimmune uveoretinitis. Invest. Ophthalmol. Vis. Sci. 44, 3034–3041 (2003).
Sharma, S. M., Nestel, A. R., Lee, R. W. & Dick, A. D. Clinical review: Anti-TNFα therapies in uveitis: perspective on 5 years of clinical experience. Ocul. Immunol. Inflamm. 17, 403–414 (2009).
Braun, J. et al. Decreased incidence of anterior uveitis in patients with ankylosing spondylitis treated with the anti-tumor necrosis factor agents infliximab and etanercept. Arthritis Rheum. 52, 2447–2451 (2005).
Rudwaleit, M. et al. Adalimumab effectively reduces the rate of anterior uveitis flares in patients with active ankylosing spondylitis: results of a prospective open-label study. Ann. Rheum. Dis. 68, 696–701 (2009).
Smith, J. A. et al. A randomized, placebo-controlled, double-masked clinical trial of etanercept for the treatment of uveitis associated with juvenile idiopathic arthritis. Arthritis Rheum. 53, 18–23 (2005).
Lim, L. L., Fraunfelder, F. W. & Rosenbaum, J. T. Do tumor necrosis factor inhibitors cause uveitis? A registry-based study. Arthritis Rheum. 56, 3248–3252 (2007).
Reddy, A. R. & Backhouse, O. C. Does etanercept induce uveitis? Br. J. Ophthalmol. 87, 925 (2003).
Wenzel, S. E. Asthma: defining of the persistent adult phenotypes. Lancet 368, 804–813 (2006).
Miranda, C. et al. Distinguishing severe asthma phenotypes: role of age at onset and eosinophilic inflammation. J. Allergy Clin. Immunol. 113, 101–108 (2004).
Moffatt, M. F. et al. A large-scale, consortium-based genomewide association study of asthma. N. Engl. J. Med. 363, 1211–1221 (2010).
Walker, S., Monteil, M., Phelan, K., Lasserson, T. J. & Walters, E. H. Anti-IgE for chronic asthma in adults and children. Cochrane Database of Systematic Reviews, Issue 2, Art. No.: CD003559. doi:10.1002/14651858.CD003559.pub3 (2006).
Holgate, S. et al. Efficacy of omalizumab, an anti-immunoglobulin E antibody, in patients with allergic asthma at high risk of serious asthma-related morbidity and mortality. Curr. Med. Res. Opin. 17, 233–240 (2001).
Holgate, S. T. et al. Efficacy and safety of a recombinant anti-immunoglobulin E antibody (omalizumab) in severe allergic asthma. Clin. Exp. Allergy 34, 632–638 (2004).
Busse, W. W. et al. Randomized trial of omalizumab (anti-IgE) for asthma in inner-city children. N. Engl. J. Med. 364, 1005–1015 (2011).
Bousquet, J. et al. Indirect evidence of bronchial inflammation assessed by titration of inflammatory mediators in BAL fluid of patients with asthma. J. Allergy Clin. Immunol. 88, 649–660 (1991).
Broide, D. H. et al. Evidence of ongoing mast cell and eosinophil degranulation in symptomatic asthma airway. J. Allergy Clin. Immunol. 88, 637–648 (1991).
Sanderson, C. J. Interleukin-5, eosinophils, and disease. Blood 79, 3101–3109 (1992).
Collins, P. D., Marleau, S., Griffiths-Johnson, D. A., Jose, P. J. & Williams, T. J. Cooperation between interleukin-5 and the chemokine eotaxin to induce eosinophil accumulation in vivo. J. Exp. Med. 182, 1169–1174 (1995).
Büttner, C., Lun, A., Splettstoesser, T., Kunkel, G. & Renz, H. Monoclonal anti-interleukin-5 treatment suppresses eosinophil but not T-cell functions. Eur. Respir. J. 21, 799–803 (2003).
Flood-Page, P. T. et al. Eosinophil's role remains uncertain as anti-interleukin-5 only partially depletes numbers in asthmatic airway. Am. J. Respir. Crit. Care Med. 167, 199–204 (2003).
Leckie, M. J. et al. Effects of an interleukin-5 blocking monoclonal antibody on eosinophils, airway hyper-responsiveness, and the late asthmatic response. Lancet 356, 2144–2148 (2000).
Green, R. H. et al. Asthma exacerbations and sputum eosinophil counts: a randomised controlled trial. Lancet 360, 1715–1721 (2002).
ten Brinke, A. et al. Factors associated with persistent airflow limitation in severe asthma. Am. J. Respir. Crit. Care Med. 164, 744–748 (2001).
Haldar, P. et al. Mepolizumab and exacerbations of refractory eosinophilic asthma. N. Engl. J. Med. 360, 973–984 (2009).
Nair, P. et al. Mepolizumab for prednisone-dependent asthma with sputum eosinophilia. N. Engl. J. Med. 360, 985–993 (2009).
Howarth, P. H. et al. Tumour necrosis factor (TNFα) as a novel therapeutic target in symptomatic corticosteroid dependent asthma. Thorax 60, 1012–1018 (2005).
Berry, M. et al. Pathological features and inhaled corticosteroid response of eosinophilic and non-eosinophilic asthma. Thorax 62, 1043–1049 (2007).
Wenzel, S. E. et al. Bronchoscopic evaluation of severe asthma. Persistent inflammation associated with high dose glucocorticoids. Am. J. Respir. Crit. Care Med. 156, 737–743 (1997).
Erin, E. M. et al. The effects of a monoclonal antibody directed against tumor necrosis factor-α in asthma. Am. J. Respir. Crit. Care Med. 174, 753–762 (2006).
Morjaria, J. B. et al. The role of a soluble TNFα receptor fusion protein (etanercept) in corticosteroid refractory asthma: a double blind, randomised, placebo controlled trial. Thorax 63, 584–591 (2008).
Wenzel, S. E. et al. A randomized, double-blind, placebo-controlled study of tumor necrosis factor-α blockade in severe persistent asthma. Am. J. Respir. Crit. Care Med. 179, 549–558 (2009).
Aujla, S. J. & Alcorn, J. F. TH17 cells in asthma and inflammation. Biochim. Biophys. Acta doi:10.1016/j.bbagen.2011.02.002.
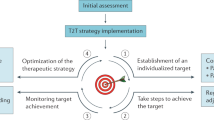
Isaacs, J. D. & Ferraccioli, G. The need for personalised medicine for rheumatoid arthritis. Ann. Rheum. Dis. 70, 4–7 (2011).
Chatenoud, L. & Bluestone, J. A. CD3-specific antibodies: a portal to the treatment of autoimmunity. Nat. Rev. Immunol. 7, 622–632 (2007).
Chatenoud, L., Primo, J. & Bach, J. F. CD3 antibody-induced dominant self tolerance in overtly diabetic NOD mice. J. Immunol. 158, 2947–2954 (1997).
Herold, K. C. et al. Anti-CD3 monoclonal antibody in new-onset type 1 diabetes mellitus. N. Engl. J. Med. 346, 1692–1698 (2002).
Herold, K. C. et al. A single course of anti-CD3 monoclonal antibody hOKT3gamma1(Ala-Ala) results in improvement in C-peptide responses and clinical parameters for at least 2 years after onset of type 1 diabetes. Diabetes 54, 1763–1769 (2005).
Herold, K. C. et al. Treatment of patients with new onset Type 1 diabetes with a single course of anti-CD3 mAb Teplizumab preserves insulin production for up to 5 years. Clin. Immunol. 132, 166–173 (2009).
Keymeulen, B. et al. Insulin needs after CD3-antibody therapy in new-onset type 1 diabetes. N. Engl. J. Med. 352, 2598–2608 (2005).
Keymeulen, B. et al. Four-year metabolic outcome of a randomised controlled CD3-antibody trial in recent-onset type 1 diabetic patients depends on their age and baseline residual beta cell mass. Diabetologia 53, 614–623 (2010).
Keymeulen, B. et al. Transient Epstein–Barr virus reactivation in CD3 monoclonal antibody-treated patients. Blood 115, 1145–1155 (2010).
Diabetes.co.uk Diabetes drug teplizumab fails in tests [online], (2010).
Diabetes.co.uk Diabetes drug otelixizumab fails in late trials [online], (2011).
Cooles, F. A. & Isaacs, J. D. Treating to re-establish tolerance in inflammatory arthritis—lessons from other diseases. Best Pract. Res. Clin. Rheumatol. 24, 497–511 (2010).
Isaacs, J. D. The changing face of rheumatoid arthritis: sustained remission for all? Nat. Rev. Immunol. 10, 605–611 (2010).
Maedler, K., Dharmadhikari, G., Schumann, D. M. & Størling, J. Interleukin-1 beta targeted therapy for type 2 diabetes. Expert Opin. Biol. Ther. 9, 1177–1188 (2009).
Sauter, N. S., Schulthess, F. T., Galasso, R., Castellani, L. W. & Maedler, K. The antiinflammatory cytokine interleukin 1 receptor antagonist protects from high-fat diet-induced hyperglycemia. Endocrinology 149, 2208–2218 (2008).
Larsen, C. M. et al. Interleukin-1-receptor antagonist in type 2 diabetes mellitus. N. Engl. J. Med. 356, 1517–1526 (2007).
Pickersgill, L. M. & Mandrup-Poulsen, T. R. The anti-interleukin-1 in type 1 diabetes action trial—background and rationale. Diabetes Metab. Res. Rev. 25, 321–324 (2009).
Deswal, A. et al. Safety and efficacy of a soluble P75 tumor necrosis factor receptor (Enbrel, etanercept) in patients with advanced heart failure. Circulation 99, 3224–3226 (1999).
Chung, E. S. et al. Randomized, double-blind, placebo-controlled, pilot trial of infliximab, a chimeric monoclonal antibody to tumor necrosis factor-alpha, in patients with moderate-to-severe heart failure: results of the anti-TNF Therapy Against Congestive Heart Failure (ATTACH) trial. Circulation 107, 3133–3140 (2003).
Mann, D. L. et al. Targeted anticytokine therapy in patients with chronic heart failure: results of the Randomized Etanercept Worldwide Evaluation (RENEWAL). Circulation 109, 1594–1602 (2004).
Listing, J. et al. Does tumor necrosis factor α inhibition promote or prevent heart failure in patients with rheumatoid arthritis? Arthritis Rheum. 58, 667–677 (2008).
Arnett, H. A., Wang, Y., Matsushima, G. K., Suzuki, K. & Ting, J. P. Functional genomic analysis of remyelination reveals importance of inflammation in oligodendrocyte regeneration. J. Neurosci. 23, 9824–9832 (2003).
Boyko, A. N. Clinical effects and tolerability of high-dose, high-frequency recombinant interferon β-1a in patients with multiple sclerosis: maximizing therapy through long-term adherence. Expert Opin. Biol. Ther. 10, 653–666 (2010).
Carter, N. J. & Keating, G. M. Glatiramer acetate: a review of its use in relapsing-remitting multiple sclerosis and in delaying the onset of clinically definite multiple sclerosis. Drugs 70, 1545–1577 (2010).
Polman, C. H. et al. A randomized, placebo-controlled trial of natalizumab for relapsing multiple sclerosis. N. Engl. J. Med. 354, 899–910 (2006).
Kleinschmidt-DeMasters, B. K. & Tyler, K. L. Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis. N. Engl. J. Med. 353, 369–374 (2005).
Langer-Gould, A., Atlas, S. W., Green, A. J., Bollen, A. W. & Pelletier, D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N. Engl. J. Med. 353, 375–381 (2005).
Van Assche, G. et al. Progressive multifocal leukoencephalopathy after natalizumab therapy for Crohn's disease. N. Engl. J. Med. 353, 362–368 (2005).
FDA. FDA Drug Safety Communication: Safety update on Progressive Multifocal Leukoencephalopathy (PML) associated with Tysabri (natalizumab) [online], (2011).
Khalili, K., Gordon, J. & White, M. K. The polyomavirus, JCV and its involvement in human disease. Adv. Exp. Med. Biol. 577, 274–287 (2006).
Major, E. O. Progressive multifocal leukoencephalopathy in patients on immunomodulatory therapies. Annu. Rev. Med. 61, 35–47 (2010).
Lindå, H. et al. Progressive multifocal leukoencephalopathy after natalizumab monotherapy. N. Engl. J. Med. 361, 1081–1087 (2009).
Tan, C. S. & Koralnik, I. J. Progressive multifocal leukoencephalopathy and other disorders caused by JC virus: clinical features and pathogenesis. Lancet Neurol. 9, 425–437 (2010).
Carson, K. R. et al. Progressive multifocal leukoencephalopathy after rituximab therapy in HIV-negative patients: a report of 57 cases from the Research on Adverse Drug Events and Reports project. Blood 113, 4834–4840 (2009).
Buch, M. H. et al. Updated consensus statement on the use of rituximab in patients with rheumatoid arthritis. Ann. Rheum. Dis. 70, 909–920 (2011).
Chen, Y. et al. Asymptomatic reactivation of JC virus in patients treated with natalizumab. N. Engl. J. Med. 361, 1067–1074 (2009).
Hauser, S. L. et al. B-cell depletion with rituximab in relapsing-remitting multiple sclerosis. N. Engl. J. Med. 358, 676–688 (2008).
Coles, A. J. et al. Alemtuzumab vs. interferon beta-1a in early multiple sclerosis. N. Engl. J. Med. 359, 1786–1801 (2008).
Coles, A. J. et al. Pulsed monoclonal antibody treatment and autoimmune thyroid disease in multiple sclerosis. Lancet 354, 1691–1695 (1999).
Isaacs, J. D. & Thiel, A. Stem cell transplantation for autoimmune disorders. Immune reconstitution. Best Pract. Res. Clin. Haematol. 17, 345–358 (2004).
Jones, J. L. et al. IL-21 drives secondary autoimmunity in patients with multiple sclerosis, following therapeutic lymphocyte depletion with alemtuzumab (Campath-1H). J. Clin. Invest. 119, 2052–2061 (2009).
Acknowledgements
C. P. Vega, University of California, Irvine, CA, is the author of and is solely responsible for the content of the learning objectives, questions and answers of the Medscape, LLC-accredited continuing medical education activity associated with this article.
Author information
Authors and Affiliations
Contributions
All authors contributed equally to researching data for the article, discussing content, writing the article and review/editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
J. D. Isaacs has acted as a consultant to Pfizer and Roche, received speakers bureau/honoraria from Abbott and Roche, received grant/research support from Biogen Idec, GlaxoSmithKline, Pfizer, Roche and UCB, and is a patent holder/applicant with GlaxoSmithKline. The other authors declare no competing interests.
Rights and permissions
About this article
Cite this article
Bell, G., Reynolds, G. & Isaacs, J. Biologic therapies in non-rheumatic diseases: lessons for rheumatologists?. Nat Rev Rheumatol 7, 507–516 (2011). https://doi.org/10.1038/nrrheum.2011.106
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2011.106