Abstract
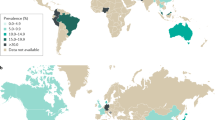
IBS is a common disorder that affects approximately 5–20% of the populations of Western countries; the main symptoms are abdominal pain and erratic, altered bowel habits, often accompanied by bloating. Despite an array of available pharmacological and nonpharmacological treatments aimed at a wide variety of gastrointestinal and brain targets, many patients do not report adequate symptom relief. The effect of IBS on an individual can be enormous, and the societal and financial costs overall are high, which is indicative of an unmet need for effective IBS treatments. Intense research efforts are ongoing that range from the development of new molecules for pharmacological therapies to testing the utility of internet technology to facilitate widespread delivery of efficacious behavioural therapy. This Review discusses the latest treatments for IBS, including novel nonpharmacological and pharmacological approaches. We have included estimates of the number needed to treat and the number needed to harm for selected treatments. Emerging and potential future treatments are included, with the data supporting an optimistic view about the future of IBS therapeutics. The ability to optimize therapy by individualizing management whilst also avoiding harm remains the key to achieving the best possible outcomes with currently available therapeutics.
Key Points
-
IBS is common and affects the quality of life of patients with this syndrome
-
Current therapies focus on symptom relief not cure
-
The patient–physician relationship and education about the condition remain key to optimal management of IBS
-
Emerging nonpharmacological therapies include a low FODMAP diet and exercise
-
Current drug therapies used as single therapy do not provide adequate symptom relief for many patients with IBS
-
New pharmacological therapies are emerging, including drugs that act locally in the intestinal lumen, but the cost-effectiveness of these therapies is largely undetermined
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Saito, Y., Schoenfeld, P. & Locke, G. R. III. The epidemiology of irritable bowel syndrome in North America: a systematic review. Am. J. Gastroenterol. 97, 1910–1915 (2002).
Hungin, A. P., Chang, L., Locke, G. R. III, Dennis, E. H. & Barghout, V. Irritable bowel syndrome in the United States: prevalence, symptom patterns and impact. Aliment. Pharmacol. Ther. 21, 1365–1375 (2005).
Gwee, K. A. Irritable bowel syndrome in developing countries—a disorder of civilization or colonization? Neurogastroenterol. Motil. 17, 317–324 (2005).
Malagelada, J. R. A symptom-based approach to making a positive diagnosis of irritable bowel syndrome with constipation. Int. J. Clin. Pract. 60, 57–63 (2006).
Jones, M. P. et al. Psychological variables add incremental value to miological makers in differentiating IBS from health volunteer [abstract Tu1392]. Gastroenterology 142 (Suppl. 1), S-820 (2012).
Koloski, N. A., Talley, N. J. & Boyce, P. M. The impact of functional gastrointestinal disorders on quality of life. Am. J. Gastroenterol. 95, 67–71 (2000).
Wilson, A. et al. Quality of life in managed care patients with irritable bowel syndrome. Manag. Care Interface 17, 24–28 (2004).
Miller, V., Hopkins, L. & Whorwell, P. J. Suicidal ideation in patients with irritable bowel syndrome. Clin. Gastroenterol. Hepatol. 2, 1064–1068 (2004).
Leong, S. et al. The economic consequences of irritable bowel syndrome: a US employer perspective. Arch. Intern. Med. 163, 929–935 (2003).
Martin, R. et al. Irritable bowel syndrome: towards a cost-effective approach. Am. J. Manag. Care 7, S268–S275 (2001).
Dean, B. B. et al. Impairment in work productivity and health-related quality of life in patients with IBS. Am. J. Manag. Care 11, S17–S26 (2005).
Drossman, D. A., Whitehead, W. E. & Camilleri, M. Irritable bowel syndrome: a technical review of practice guideline development. Gastroenterology 112, 2120–2137 (1997).
Harvey, R. F., Salih, S. Y. & Read, A. E. Organic and functional disorders in 2000 gastroenterology outpatients. Lancet 1, 632–634 (1983).
Hahn, B. A., Saunders, W. B. & Maier, W. C. Differences between individuals with self-reported irritable bowel syndrome (IBS) and IBS-like symptoms. Dig. Dis. Sci. 42, 2585–2590 (1997).
Guilarte, M. et al. Diarrhoea-predominant IBS patients show mast cell activation and hyperplasia in the jejunum. Gut 56, 203–209 (2007).
Spiller, R. & Garsed, K. Postinfectious irritable bowel syndrome. Gastroenterology 136, 1979–1988 (2009).
Drossman, D. A. Gastrointestinal illness and the biopsychosocial model. Psychosom. Med. 60, 258–267 (1998).
Faresjö, A. et al. Psychological factors at work and in everyday life are associated with irritable bowel syndrome. Eur. J. Epidemiol. 22, 473–480 (2007).
Koloski, N. A. et al. The brain-gut pathway in functional gastrointestinal disorders is bidirectional: a 12-year prospective population-based study. Gut 61, 1284–1290 (2012).
Whitehead, W. E. et al. Reports of 'satisfactory relief' by IBS patients receiving usual medical care are confounded by baseline symptom severity and do not accurately reflect symptom improvement. Am. J. Gastroenterol. 101, 1057–1065 (2006).
Drossman, D. & Thompson, W. G. The irritable bowel syndrome: review and a graduated multicomponent treatment approach. Ann. Intern. Med. 116, 1009–1116 (1992).
Owens, D. M., Nelson, D. K. & Talley, N. J. The irritable bowel syndrome: long-term prognosis and the physician-patient interaction. Ann. Intern. Med. 122, 107–112 (1995).
Talley, N. J. Conquering irritable bowel syndrome (BC Decker, Hamilton, 2006).
Kaptchuk, T. J. et al. Components of placebo effect: randomised controlled trial in patients with irritable bowel syndrome. BMJ 336, 999–1003 (2008).
Kaptchuk, T. J. et al. Placebos without deception: a randomized controlled trial in irritable bowel syndrome. PLoS ONE 5, e15591 (2010).
Conboy, L. A. et al. Investigating placebo effects in irritable bowel syndrome: a novel research design. Contemp. Clin. Trials 27, 123–134 (2006).
Heitkemper, M. M. et al. Self-management for women with irritable bowel syndrome. Clin. Gastroenterol. Hepatol. 2, 585–596 (2004).
Larsson, K. et al. A group-based patient education programme for high-anxiety patients with Crohn or ulcerative colitis. Scand. J. Gastroenterol. 38, 763–769 (2003).
Ringström, G. et al. Structured patient education is superior to written information in the management of patients with irritable bowel syndrome: a randomized controlled study. Eur. J. Gastroenterol. Hepatol. 22, 420–428 (2010).
Whorwell, P. J., Prior, A. & Faragher, E. B. Controlled trial of hypnotherapy in the treatment of severe refractory irritable bowel syndrome. Lancet 2, 1232–1234 (1984).
Harvey, R. F., Hinton, R. A., Gunary, R. M. & Barry, R. E. Individual and group hypnotherapy in the treatment of refractory irritable bowel syndrome. Lancet 1, 424–425 (1989).
Galovski, T. E. & Blanchard, E. B. The treatment of irritable bowel syndrome with hypnotherapy. Appl. Psychophysiol. Biofeedback 23, 219–232 (1998).
Palsson, O. S., Turner, M. J., Johnson, D. A., Burnett, C. K. & Whitehead, W. E. Hypnosis treatment for severe irritable bowel syndrome: investigation of mechanisms and effects on symptoms. Dig. Dis. Sci. 47, 2605–2614 (2002).
Miller, V. et al. Hypnotherapy for irritable bowel syndrome: an audit of 1000 patients [abstract Sa1407]. Gastroenterology 142 (Suppl. 1), S-296 (2012).
Lindfors, P. et al. Effects of gut-directed hypnotherapy on IBS in different clinical settings—results from two randomized, controlled trials. Am. J. Gastroenterol. 107, 276–285 (2012).
Houghton, L. A., Heyman, D. J. & Whorwell, P. J. Symptomatology, quality of life and economic features of irritable bowel syndrome—the effect of hypnotherapy. Aliment. Pharmacol. Ther. 10, 91–95 (1996).
Carruthers, H. R., Morris, J., Tarrier, N. & Whorwell, P. J. Mood color choice helps predict response to hypnotherapy in patients with irritable bowel syndrome. BMC Complement. Altern. Med. 10, 75 (2010).
Lackner, J. M., Mesmer, C., Morley, S., Dowzer, C. & Hamilton, S. Psychological treatments for irritable bowel syndrome: a systematic review and meta-analysis. J. Consult. Clin. Psychol. 72, 1100–1113 (2004).
Ford, A. C., Talley, N. J., Schoenfeld, P. S., Quigley, E. M. & Moayyedi, P. Efficacy of antidepressants and psychological therapies in irritable bowel syndrome: systematic review and meta-analysis. Gut 58, 367–378 (2009).
Ljótsson, B. et al. Internet-delivered exposure-based treatment vs. stress management for irritable bowel syndrome: a randomized trial. Am. J. Gastroenterol. 106, 1481–1491 (2010).
Gaylord, S. A. et al. Mindfulness training reduces the severity of irritable bowel syndrome in women: results of a randomized controlled trial. Am. J. Gastroenterol. 106, 1678–1688 (2011).
Koloski, N. A., Talley, N. J., Huskic, S. S. & Boyce, P. M. Predictors of conventional and alternative health care seeking for irritable bowel syndrome and functional dyspepsia. Aliment. Pharmacol. Ther. 17, 841–851 (2003).
Manheimer, E. et al. Acupuncture for irritable bowel syndrome: systematic review and meta-analysis. Am. J. Gastroenterol. 107, 835–847 (2012).
Liu, J. P., Yang, M., Liu, Y. X., Wei, M. L. & Grimsgaard, S. Herbal medicines for treatment of irritable bowel syndrome. Cochrane Database Syst. Rev., Issue 1. Art. No.: CD004116. http://dx.doi.org/10.1002/14651858.CD004116.pub2.
Madisch, A., Holtmann, G., Plein, K. & Hotz, J. Treatment of irritable bowel syndrome with herbal preparations: results of a double-blind, randomized, placebo-controlled, multi-centre trial. Aliment. Pharmacol. Ther. 19, 271–279 (2004).
Krueger, D. et al. The multi-herbal drug STW 5 (Iberogast) has prosecretory action in the human intestine. Neurogastroenterol. Motil. 21, 1203-e110 (2009).
Whorton, J. Inner hygiene: constipation and the pursuit of health in modern society (Oxford University Press, New York, 2000).
Ford, A. C. et al. Effect of fibre, antispasmodics, and peppermint oil in the treatment of irritable bowel syndrome: systematic review and meta-analysis. BMJ 337, a2313 (2008).
Bijkerk, C. J. et al. Soluble or insoluble fibre in primary care? Randomised placebo controlled trial. BMJ 339, b3154 (2009).
Simrén, M. et al. Food-related gastrointestinal symptoms in the irritable bowel syndrome. Digestion 63, 108–115 (2001).
Park, M. I. & Camilleri, M. Is there a role of food allergy in irritable bowel syndrome and functional dyspepsia? Neurogastroenterol. Motil. 18, 595–607 (2006).
Wahnschaffe, U., Schulzke, J. D., Zeitz, M. & Ullrich, R. Predictors of clinical response to gluten-free diet in patients diagnosed with diarrhea-predominant irritable bowel syndrome. Clin. Gastroenterol. Hepatol. 5, 844–850 (2007).
Vazquez-Roque, M. I. et al. HLA-DQ genotype is associated with accelerated small bowel transit in patients with diarrhea-predominant irritable bowel syndrome. Eur. J. Gastroenterol. Hepatol. 23, 481–487 (2011).
Biesiekierski, J. R. et al. Gluten causes gastrointestinal symptoms in subjects without celiac disease: a double-blind randomized placebo-controlled trial. Am. J. Gastroenterol. 106, 508–514 (2011).
Shepherd, S., Parker, F. C., Muir, J. G. & Gibson, P. R. Dietary triggers of abdominal symptoms in patients with irritable bowel syndrome: randomized placebo-controlled evidence. Clin. Gastroenterol. Hepatol. 7, 765–771 (2008).
Staudacher, H. M., Whelan, K., Irving, P. M. & Lorner, M. C. Comparison of symptom response following advice for a diet low in fermentable carbohydrates (FODMAPs) versus standard dietary advice in patients with irritable bowel syndrome. J. Hum. Nutr. Diet. 24, 487–495 (2011).
Colwell, L. J., Prather, C. M., Phillips, S. F. & Zinsmeister, A. R. Effects of an irritable bowel syndrome educational class on health-promoting behaviours and symptoms. Am. J. Gastroenterol. 93, 901–905 (1998).
Mannerkorpi, K. Exercise in fibromyalgia. Curr. Opin. Rheumatol. 17, 190–194 (2006).
Johannesson, E., Simrén, M., Strid, H., Bajor, A. & Sadik, R. Physical activity improves symptoms in irritable bowel syndrome: a randomized controlled trial. Am. J. Gastroenterol. 106, 915–922 (2010).
Drossman, D. et al. Rome III The functional gastrointestinal disorders (Degnon Associates, McLean Virginia, 2006).
Patcharatrakul, T. & Gonlachanvit, S. Outcome of biofeedback therapy in dyssynergic defecation patients with and without irritable bowel syndrome. J. Clin. Gastroenterol. 45, 593–598 (2011).
Whorwell, P. J. et al. Efficacy of an encapsulated probiotic Bifidobacterium infantis 35624 in women with irritable bowel syndrome. Am. J. Gastroenterol. 101, 326–333 (2006).
O'Mahony, L. et al. Lactobacillus and bifidobacterium in irritable bowel syndrome: symptom responses and relationship to cytokine profiles. Gastroenterology 128, 541–551 (2005).
Moayyedi, P. et al. The efficacy of probiotics in the therapy of irritable bowel syndrome: a systematic review. Gut 59, 325–332 (2010).
Brenner, D. M., Moeller, M. J., Chey, W. D. & Schoenfeld, P. S. The utility of probiotics in the treatment of irritable bowel syndrome: a systematic review. Am. J. Gastroenterol. 104, 1033–1049 (2009).
McFarland, L. V. & Dublin, S. Meta-analysis of probiotics for the treatment of irritable bowel syndrome. World J. Gastroenterol. 14, 2650–2661 (2008).
National Institute for Health and Clinical Excellence (NICE). Irritable bowel syndrome in adults: diagnosis and management of irritable bowel syndrome in primary care (National Collaborating Centre for Nursing and Supportive Care, UK, 2008).
Hoveyda, N. et al. A systematic review and meta-analysis: probiotics in the treatment of irritable bowel syndrome. BMC Gastroenterol. 9, 15 (2009).
Huertas-Ceballos, A., Logan, S., Bennett, C. & MacArthur, C. Dietary interventions for recurrent abdominal pain (RAP) and irritable bowel syndrome (IBS) in childhood. Cochrane Database Syst. Rev., Issue 1. Art. No.:CD003019 http:dx.doi.org/10.1002/14651858.CD003019.pub2.
Whelan, K. Probiotics and prebiotics in the management of irritable bowel syndrome: a review of recent clinical trials and systematic reviews. Curr. Opin. Clin. Nutr. Metab. Care 14, 581–587 (2011).
Drossman, D. A. et al. Clinical trial: lubiprostone in patients with constipation-associated irritable bowel syndrome—results of two randomized, placebo-controlled studies. Aliment. Pharmacol. Ther. 29, 329–341 (2009).
Chey, W. D. et al. Safety and patient outcomes with lubiprostone for up to 52 weeks in patients with irritable bowel syndrome with constipation. Aliment. Pharmacol. Ther. 35, 587–599 (2012).
Joswick, T. R., Woldegeorgis, F. & Ueno, R. Patient response to lubiprostone for the treatment of moderate to severe irritable bowel syndrome with constipation (IBS-C) [abstract Su1198]. Gastroenterology 142 (Suppl. 1), S-449 (2012).
Chey, W., Paré, P., Viegas, A., Ligozio, G. & Shetzline, M. A. Tegaserod for female patients suffering from IBS with mixed bowel habits or constipation: a randomized controlled trial. Am. J. Gastroenterol. 103, 1217–1225 (2008).
Thompson, C. A. Novartis suspends tegaserod sales at FDA's request. Am. J. Health Syst. Pharm. 64, 1020 (2007).
Tack, J. et al. Systematic review: cardiovascular safety profile of 5-HT4 agonists developed for gastrointestinal disorders. Aliment. Pharmacol. Ther. 35, 745–767 (2012).
Camilleri, M., Kerstens, R., Rykx, A. & Vandeplassche, L. A placebo-controlled trial of prucalopride for severe chronic constipation. N. Engl. J. Med. 358, 2344–2354 (2008).
Quigley, E. M., Vandeplassche, L., Kerstens, R. & Ausma, J. Clinical trial: the efficacy, impact on quality of life, and safety and tolerability of prucalopride in severe chronic constipation—a 12 week, randomized, double blind, placebo-controlled study. Aliment. Pharmacol. Ther. 29, 315–328 (2009).
Tack, J., van Outryve, M., Beyens, G., Kerstens, R. & Vandeplassche, L. Prucalopride (Resolor) in the treatment of severe chronic constipation in patients dissatisfied with laxatives. Gut 58, 357–365 (2009).
Johnston, J. M. et al. Linaclotide improves abdominal pain and bowel habits in a phase IIb study of patients with irritable bowel syndrome with constipation. Gastroenterology 139, 1877–1886 (2010).
Lembo, A. et al. Efficacy of linaclotide for patients with chronic constipation. Gastroenterology 138, 886–895 (2010).
Locke, G. R. et al. Effects of linaclotide treatment on patient-reported ratings of change for symptoms of irritable bowel syndrome with constipation (IBS-C): Pooled 12-week findings from two phase 3 trials. Gastroenterology 142 (Suppl. 1), S-737 (2012).
Chey, W. D. et al. Linaclotide for irritable bowel syndrome with constipation: a 26-week, randomized, double-blind, placebo-controlled trial to evaluate efficacy and safety. Am. J. Gastroenterol. http://dx.doi.org/10.1038/ajg.2012.254.
Rao, M. et al. A 12-week, randomized, controlled trial with a 4-week randomized withdrawal period to evaluate the efficacy and safety of linaclotide in irritable bowel syndrome with constipation. Am. J. Gastroenterol. http://dx.doi.org/10/1038/ajg.2012.255.
Tack, J. F., Miner, P. B., Fishcer, L. & Harris M. S. Randomised clinical trial: the safety and efficacy of AST-120 in non-constipating irritable bowel syndrome—a double blind, placebo controlled study. Aliment. Pharmacol. Ther. 34, 868–877 (2011).
Pimental, M. et al. Rifaximin therapy for patients with irritable bowel syndrome without constipation. N. Engl. J. Med. 364, 22–32 (2011).
Menees, S., Maneerattannaporn, M., Kim, H. M. & Chey, W. D. The efficacy and safety of rifaximin for the irritable bowel syndrome: a systematic review and meta-analysis. Am. J. Gastroenterol. 107, 28–35 (2012).
Pimentel, M. et al. Effects of rifaximin treatment and retreatment in nonconstipated IBS subjects. Dig. Dis. Sci. 56, 2067–2072 (2011).
Shah, E., Kim, S., Chong, K., Lembo, A. & Pimentel, M. Evaluation of harm in the pharmacotherapy of irritable bowel syndrome. Am. J. Gastroenterol. 125, 381–393 (2012).
Chang, L. et al. A dose-ranging, phase II study of the efficacy and safety of alosetron in men with diarrhea-predominant IBS. Am. J. Gastroenterol. 100, 115–123 (2005).
Cremonini, F., Delgado-Aros, S. & Camilleri, M. Efficacy of alosetron in irritable bowel syndrome: a meta-analysis of randomised, placebo-controlled trials. Neurogastroenterol. Motil. 15, 79–86 (2003).
Chang, L. et al. Incidence of ischemic colitis and serious complications of constipation among patients using alosetron: systematic review of clinical trials and post-marketing surveillance data. Am. J. Gastroenterol. 101, 1069–1079 (2006).
Ford, A. et al. Efficacy of 5-HT3 antagonists and 5-HT4 agonists in irritable bowel syndrome: systematic review and meta-analysis. Am. J. Gastroenterol. 104, 1831–1843 (2009).
Chang, L., Tong, K. & Ameen, V. Ischemic colitis and complications of constipation associated with the use of alosetron under a risk management plan: clinical characteristics, outcomes and incidences. Am. J. Gastroenterol. 105, 866–875 (2010).
Rahimi, R., Nikfar, S. & Abdollahi, M. Efficacy and tolerability of alosetron for the treatment of irritable bowel syndrome in women and men: a meta-analysis of eight randomized, placebo-controlled, 12-week trials. Clin. Ther. 30, 884–901 (2008).
Matsueda, K., Harasawa, S., Hongo, M., Hiwatashi, N. & Sasaki, D. A phase II trial of the novel serotonin type 3 receptor antagonist in Japanese male and female patients with diarrhea-predominant irritable bowel syndrome. Digestion 77, 225–235 (2008).
Matsueda, K., Harasawa, S., Hongo, M., Hiwatashi, N. & Sasaki, D. A randomized, double-blind, placebo-controlled trial of the effectiveness of the novel serotonin type 3 receptor antagonist ramosetron in both male and female Japanese patients with diarrhea predominant irritable bowel syndrome. Scand. J. Gastroenterol. 43, 1202–1211 (2008).
Hirata, T. et al. Effects of serotonin 5-HT3 receptor antagonists on stress-induced colonic hyperalgesia and diarrhoea in rats: a comparative study with opioid receptors agonists, a muscarinic receptors antagonist and a synthetic polymer. Neurogastroenterol. Motil. 20, 557–565 (2008).
Hirata, T., Funatsu, T., Keto, Y., Nakata, M. & Sasamata, M. Pharmacological profile of ramosetron, a novel therapeutic agent for IBS. Inflammopharmacology 15, 5–9 (2007).
Lee, K. J. et al. Efficacy of ramosetron in the treatment of male patients with irritable bowel syndrome with diarrhea: a multicenter, randomized clinical trial, compared with mebeverine. Neurogastroenterol. Motil. 23, 1098–1104 (2011).
Camilleri, M. LX-1031, a tryptophan 5-hydroxylase inhibitor, and its potential in chronic diarrhoea associated with increased serotonin. Neurogastroenterol. Motil. 23, 193–200 (2011).
Asano, T. et al. Effects of β-(1,3–1,6)-D-glucan on irritable bowel syndrome related colonic hypersensitivity. Biochem. Biophys. Res. Commun. 420, 444–449 (2012).
Ciacci, C. et al. Effect of β-glucan, inositol and digestive enzymes in GI symptoms of patients with IBS. Eur. Rev. Med. Pharmacol. Sci. 15, 637–643 (2011).
Tillisch, K. et al. Neurokinin-1-receptor antagonism decreases anxiety and emotional arousal circuit response to noxious visceral distension in women with irritable bowel syndrome: a pilot study. Aliment. Pharmacol. Ther. 35, 360–367 (2012).
Bonnafous, C. et al. Influence of dexloxiglumide on visceromotor and pain response induced by rectal distension in rats. Gastroenterology 122 (Suppl.), A527 (2002).
Whorwell, P. et al. A phase III, 6-month, double-blind, placebo-controlled trial of the selective CCK-1 antagonist dexloxiglumide in constipation-predominant IBS: the DARWIN study [abstract 1050]. Gastroenterology 134 (Suppl. 1), A157 (2008).
Larsson, M., Bayati, A., Lindström, E. & Larsson, H. Involvement of κ-opioid receptors in visceral nociception in mice. Neurogastroenterol. Motil. 20, 1157–1164 (2008).
Szarka, L. A. et al. Efficacy of on-demand asimadoline, a peripheral κ-opioid agonist, in females with irritable bowel syndrome. Clin. Gastroenterol. Hepatol. 5, 1268–1275 (2007).
Floyd, B. N. et al. Effect of a κ-opioid agonists, i.v. JNJ-38488502, on sensation of colonic distensions in healthy male volunteers. Neurogastroenterol. Motil. 28, 239–249 (2009).
Kirwan, W. O., Smith, A. N., Mitchell, W. D., Falconer, J. D. & Eastwood, M. A. Bile acids and colonic motility in the rabbit and the human. Gut 16, 894–902 (1975).
Odunsi, S. T. et al. Effects of chenodeoxycholic acid on gastrointestinal and colonic transit and bowel function in healthy volunteers [abstract T1247]. Gastroenterology 136 (Suppl. 1), A-531 (2009).
Money, M. E., Walkowiak, J., Virgilio, C. & Talley, N. J. Pilot study: a randomised, double blind, placebo controlled trial of pancrealipase for the treatment of postprandial irritable bowel syndrome-diarrhoea. Frontline Gastroenterol. 2, 48–56 (2011).
Money, M. E., Hofmann, A. F., Hagey, L. R., Walkowiak, J. & Talley, N. J. Treatment of irritable bowel syndrome-diarrhea with pancrealipase or coleseveelam and association with steatorrhea. Pancreas 38, 232–233 (2009).
Camilleri, M. Review article: new receptor targets for medical therapy in irritable bowel syndrome. Aliment. Pharmacol. Ther. 31, 35–46 (2010).
Lobo, B. et al. Clinical benefit in IBS after disodium cromoglycate involves mast cell-mediated recovery of health-like innate immunity genes expression profile in the jejunal mucosa [abstract 156]. Gastroenterology 123 (Suppl. 1), A-30 (2009).
Klooker, T. et al. Treatment with the mast cell stabilizer ketoifen decreases visceral hypersensitivity and improves symptoms in IBS patients [abstract OP397]. Proceedings of the United European Gastroenterology Federation (UEGF) Meeting, Vienna, Austria (2008).
Corinaldesi, R. et al. Effect of mesalazine on mucosal immune biomarkers in irritable bowel syndrome: a randomized controlled proof of concept study. Aliment. Pharmacol. Ther. 30, 245–252 (2009).
Leventer, S. M. et al. Clinical trial: dextofisopam in the treatment of patients with diarrhoea-predominant or alternating irritable bowel syndrome. Aliment. Pharmacol. Ther. 27, 197–206 (2008).
Grover, M. et al. Atypical antipsychotic quetiapine in the management of severe refractory functional gastrointestinal disorders. Dig. Dis. Sci. 54, 1284–1291 (2009).
Houghton, L. A. et al. Effects of a second-generation α2δ ligand (pregabalin) on visceral sensation in hypersensitive patients with irritable bowel syndrome. Gut 56, 1218–1225 (2007).
Lee, K. J., Kim, J. H. & Cho, S. W. Gabapentin reduces rectal mechanosensitivity and increases rectal compliance in patients with diarrhoea-predominant irritable bowel syndrome. Aliment. Pharmacol. Ther. 22, 981–988 (2005).
Sweetser, S. et al. Do corticotropin releasing factor-1 receptors influence colonic transit and bowel function in women with irritable bowel syndrome? Am. J. Physiol. 296, G1299–G1306 (2009).
Borody, T. J. et al. Bowel-flora alteration: a potential cure for inflammatory bowel disease and irritable bowel syndrome? Med. J. Aust. 150, 604 (1989).
Andrews, P., Borody, T. J., Shortis, N. P. & Thompson, S. Bacteriotherapy for chronic constipation—a long term follow-up [abstract]. Gastroenterology 108 (Suppl. 2), A563 (1995).
Borody, T. J. & Khoruts, A. Fecal microbiota transplantation and emerging applications. Nat. Rev. Gastroenterol. Hepatol. 9, 88–96 (2012).
Ford, A. C. & Vandvik, P. O. Irritable bowel syndrome. Clin. Evid. (Online) 2012, 0410 (2012).
Miller, V. & Whorwell, P. J. Hypnotherapy for functional gastrointestinal disorders: a review. Intl. J. Clin. Exp. Hypn. 57, 279–292 (2009).
Whorwell, P. Hypnotherapy—a wasted resource? Nat. Rev. Gastroenterol. Hepatol. 9, 12–13 (2012).
Crowell, M. D. Lubiprostone: trials and tribulations. Nat. Rev. Gastroenterol. Hepatol. 6, 259–260 (2009).
Simren, M. et al. The IBAT inhibitor A3309—a promising treatment option for patients with chronic idiopathic constipation [abstract S1299]. Gastroenterology 138 (Suppl. 1), S-223 (2010).
Author information
Authors and Affiliations
Contributions
M. Halland researched data for the article, contributed to discussion of the article content, wrote the article and reviewed/edited the manuscript before submission. N. J. Talley contributed to discussion of the article content and reviewed/edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
N. J. Talley has consulted for ARYx, Astellenas Pharma, Boehringer Ingelheim, Care Capital, ConCERT Pharma, Doyen, Edusa Pharmaceuticals, Falk, Forest, Ironwood Pharmaceuticals, Janssen, Johnson & Johnson, Meritage Pharma, NicOx, Novartis, Pfizer, Proctor & Gamble, Prometheus, Salix Pharmaceuticals, Sanofi–Aventis, Shire, Theravance, Tranzyme, UpToDate, XenoPort and Zeria, received speakers fees from Abbott, Accreddit Ed, AstraZeneca, Focus Medical, Ironwood Pharmaceuticals and Salix Pharmaceuticals and has patents with Prometheus and separately for biomarkers, and has received research support from Falk, Forest, Janssen and Takeda. M. Halland declares no competing interests.
Rights and permissions
About this article
Cite this article
Halland, M., Talley, N. New treatments for IBS. Nat Rev Gastroenterol Hepatol 10, 13–23 (2013). https://doi.org/10.1038/nrgastro.2012.207
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrgastro.2012.207
This article is cited by
-
A randomized, double-blind, placebo-controlled study to assess efficacy of mirtazapine for the treatment of diarrhea predominant irritable bowel syndrome
BioPsychoSocial Medicine (2021)
-
miR-16 and miR-103 impact 5-HT4 receptor signalling and correlate with symptom profile in irritable bowel syndrome
Scientific Reports (2017)
-
Board Review Vignette: Irritable Bowel Syndrome
American Journal of Gastroenterology (2016)
-
Mechanisms and efficacy of dietary FODMAP restriction in IBS
Nature Reviews Gastroenterology & Hepatology (2014)
-
Treatment of abdominal pain in irritable bowel syndrome
Journal of Gastroenterology (2014)