Abstract
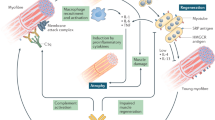
The signaling pathways involved in the immunobiology of polymyositis, dermatomyositis, and inclusion-body myositis are outlined in this Review, which is based on research performed during the past 10 years. In dermatomyositis, the complement cascade is activated and the expression of cytokines and chemokines is upregulated. In polymyositis and inclusion-body myositis, autoinvasive CD8+ T cells are clonally expanded. This T-cell subset possesses conserved amino-acid sequences in complementarity-determining region 3 of the T-cell receptor and, via the perforin pathway, exerts a myotoxic effect on muscle fibers that express major histocompatibility complex (MHC) class I molecules. In all inflammatory myopathies, molecules associated with T-cell transmigration and cytokine signaling, as well as chemokines and their receptors, are strongly expressed by endothelial and inflammatory cells. Early in the pathogenesis of polymyositis and inclusion-body myositis, expression of MHC class I molecules on muscle fibers is upregulated, even in the absence of autoinvasive CD8+ T cells. Emerging data indicate that such continuous upregulation of the expression of MHC class I molecules on muscle fibers leads to an endoplasmic reticulum stress response, intracellular accumulation of misfolded glycoproteins, and activation of nuclear factor κB pathways, which can further stimulate formation of MHC class I–CD8 complexes, resulting in a self-sustaining inflammatory response. Advances in our understanding of the signaling pathways involved in the pathogenesis of these inflammatory myopathies are expected to result in the identification of novel therapeutic targets for these diseases.
Key Points
-
Dermatomyositis is a complement-mediated microangiopathy, which leads to destruction of endomysial capillaries
-
In polymyositis and inclusion-body myositis (IBM), the muscle fibers overexpress major histocompatibility complex class I molecules and autoinvasive T cells are clonally expanded
-
In polymyositis and IBM, the T cells form immunologic synapses with the muscle fibers; however, the antigen or antigens they recognize are still unknown
-
In IBM, an autoimmune and a degenerative process occur in parallel; the continuous upregulation of major histocompatibility complex class I molecules on muscle fibers is a major culprit in inducing an endoplasmic reticulum stress response and accumulation of misfolded glycoproteins within the muscle fibers
-
New immunomodulating agents against signaling pathways involved in T-cell or B-cell activation offer promise for future therapies
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Dalakas MC (1991) Polymyositis, dermatomyositis and inclusion-body myositis. N Engl J Med 325: 1487–1498
Engel AG and Hohlfeld R (2004) The polymyositis and dermatomyositis syndromes. In Myology (edn 3), 1321–1366 (Eds Engel AG and Franzini-Armstrong C) New York: McGraw-Hill Book Co.
Mastaglia FL and Phillips BA (2002) Idiopathic inflammatory myopathies: epidemiology, classification and diagnostic criteria. Rheum Dis Clin N Am 28: 723–741
Dalakas MC and Hohlfeld R (2003) Polymyositis and dermatomyositis. Lancet 362: 971–982
Dalakas MC (2004) Inflammatory disorders of muscle: progress in polymyositis, dermatomyositis and inclusion body myositis. Curr Opin Neurol 17: 561–567
Dalakas MC (1998) Molecular immunology and genetics of inflammatory muscle diseases. Arch Neurol 55: 1509–1512
Koffman BM et al. (1998) HLA allele distribution distinguishes sporadic inclusion body myositis from hereditary inclusion body myopathies. J Neuroimmunol 84: 139–142
Price P et al. (2004) Two major histocompatibility complex haplotypes influence susceptibility to sporadic inclusion body myositis: critical evaluation of an association with HLA-DR3. Tissue Antigens 64: 575–580
Badrising UA et al. (2004) Associations with autoimmune disorders and HLA class I, and II antigens in inclusion body myositis. Neurology 63: 2396–2398
Kissel JT et al. (1986) Microvascular deposition of complement membrane attack complex in dermatomyositis. N Engl J Med 314: 329–334
Dalakas MC et al. (1993) A controlled trial of high-dose intravenous immunoglobulin infusions as treatment for dermatomyositis. N Engl J Med 329: 1993–2000
Illa I et al. (1997) Signal transducer and activator of transcription 1 in human muscle: implications in inflammatory myopathies. Am J Pathol 151: 81–88
Greenberg SA et al. (2005) Interferon-alpha/beta-mediated innate immune mechanisms in dermatomyositis. Ann Neurol 57: 664–678
Tezak Z et al. (2002) Gene expression profiling in DQA1*0501+ children with untreated dermatomyositis: a novel model of pathogenesis. J Immunol 168: 4154–4163
Askanas V and Engel WK (2003) Proposed pathogenetic cascade of inclusion-body myositis: importance of amyloid-beta, misfolded proteins, predisposing genes, and aging. Curr Opin Rheumatol 15: 737–744
Karpati G et al. (1988) Expression of immunoreactive major histocompatibility complex products in human skeletal muscles. Ann Neurol 23: 64–72
Michaelis D et al. (1993) Constitutive and cytokine-induced expression of human leukocyte antigens and cell adhesion molecules by human myotubes. Am J Pathol 143: 1142–1149
Wiendl H et al. (2005) Immunobiology of muscle: advances in understanding an immunological microenvironment. Trends Immunol 26: 373–380
Nagaraju K et al. (2000) Conditional up-regulation of MHC class I in skeletal muscle leads to self-sustaining autoimmune myositis and myositis-specific autoantibodies. Proc Natl Acad Sci USA 97: 9209–9214
Goebels N et al. (1996) Differential expression of perforin in muscle-infiltrating T cell in polymyositis and dermatomyositis. J Clin Invest 97: 2905–2910
Schmidt J et al. (2004) Upregulated inducible costimulator and ICOS-ligand in inclusion body myositis muscle: significance for CD8+ T cell cytotoxicity. Brain 127: 1182–1190
Behrens L et al. (1997) Cytotoxic mechanisms in inflammatory myopathies: co-expression of Fas and protective Bcl-2 in muscle fibres and inflammatory cells. Brain 120 (Pt 6): 929–938
Schneider C et al. (1996) MHC class I mediated cytotoxicity does not induce apoptosis in muscle fibers nor in inflammatory T cells: studies in patients with polymyositis, dermatomyositis, and inclusion body myositis. J Neuropathol Exp Neurol 55: 1205–1209
O'Hanlon TP et al. (1994) Predominant T cell receptor variable and joining gene expression by muscle-infiltrating lymphocytes in the idiopathic inflammatory myopathies. J Immunol 152: 2569–2576
Benveniste O et al. (2001) Severe perturbations of the blood T cell repertoire in polymyositis, but not dermatomysitis patients. J Immunol 167: 3521–3529
Nishio J et al. (2001) Clonal biases of peripheral CD8 T cell repertoire directly reflect local inflammation in polymyositis. J Immunol 167: 4051–4058
Amemiya K et al. (2000) Clonal restriction of T-cell receptor expression by infiltrating lymphocytes in inclusion body myositis persists over time: studies in repeated muscle biopsies. Brain 123: 2030–2039
Hofbauer M et al. (2003) Clonal tracking of autoaggressive T cells in polymyositis by combining laser microdissection, single-cell PCR and CDR3 spectratype analysis. Proc Natl Acad Sci USA 100: 4090–4095
Behrens L et al. (1998) Human muscle cells express a functional costimulatory molecule distinct from B7.1 (CD80) and B7.2 (CD86) in vitro and in inflammatory lesions. J Immunol 161: 5943–5951
Murata K and Dalakas MC (1999) Expression of the costimulatory molecule BB-1, the ligands CTLA-4 and CD28 and their mRNA in inflammatory myopathies. Am J Pathol 155: 453–460
Wiendl H et al. (2003) Muscle fibers and cultured muscle or cells express the B7.1/2 related costimulatory molecule ICOSL: implications for the pathogenesis of inflammatory myopathies. Brain 126: 1026–1035
Howard OM et al. (2002) Histidyl-tRNA synthetase and asparaginyl-tRNA synthetase, autoantigens in myositis, activate chemokine receptors on T lymphocytes and immature dendritic cells. J Exp Med 196: 781–791
Figarella-Branger D et al. (2003) Cytokines, chemokines, and cell adhesion molecules in inflammatory myopathies. Muscle Nerve 28: 659–682
De Bleecker JL et al. (2002) Differential expression of chemokines in inflammatory myopathies. Neurology 58: 1779–1785
Raju R et al. (2003) Expression of interferon-gamma inducible chemokines in the muscles of patients with inclusion body myositis. J Neuroimmunol 141: 125–131
Choi YC and Dalakas MC (2000) Expression of matrix metalloproteinases in the muscle of patients with inflammatory myopathies. Neurology 54: 65–71
Leff RL et al. (1992) Viruses in the idiopathic inflammatory myopathies: absence of candidate viral genomes in muscle. Lancet 339: 1192–1195
Illa I et al. (1991) Immunocytochemical and virological characteristics of HIV-associated inflammatory myopathies: similarities with seronegative polymyositis. Ann Neurol 29: 474–481
Cupler EJ et al. (1996) Inclusion body myositis in HIV-I and HTLV-I infected patients. Brain 119: 1887–1893
Dalakas MC (2005) Inflammatory, immune and viral aspects of inclusion body myositis. Neurology 66 (Suppl): S33–S38
Ozden S et al. (2004) Direct evidence for a chronic CD8+-T-cell-mediated immune reaction to tax within the muscle of a human T-cell leukemia/lymphoma virus type 1-infected patient with sporadic inclusion body myositis. J Virol 78: 10320–10327
Grandea AG 3rd and Van Kaer L (2001) Tapasin: an ER chaperone that controls MHC class I assembly with peptide. Trends Immunol 22: 194–199
Nagaraju K et al. (2005) Activation of the endoplasmic reticulum stress response in autoimmune myositis: potential role in muscle fiber damage and dysfunction. Arthritis Rheum 52: 1824–1835
Ferrer I et al. (2004) Proteasomal expression, induction of immunoproteasome subunits, and local MHC class I presentation in myofibrillar myopathy and inclusion body myositis. J Neuropathol Exp Neurol 63: 484–498
Vattemi G et al. (2004) Endoplasmic reticulum stress and unfolded protein response in inclusion body myositis muscle. Am J Pathol 164: 1–7
Banwell BL and Engel AG (2000) AlphaB-crystallin immunolocalization yields new insights into inclusion body myositis. Neurology 54: 1033–1041
Schmidt J et al. (2005) Distinct interplay between inflammatory and degeneration-associated molecules in sporadic IBM. Neurology 64 (Suppl 1): A331–A332
Greenberg SA (2001) DNA microarray gene expression analysis technology and its application to neurological disorders. Neurology 57: 755–761
Raju R and Dalakas MC (2005) Gene expression profile in the muscles of patients with inflammatory myopathies: effect of therapy with IVIg and biological validation of clinically relevant genes. Brain 128: 1887–1896
Lindberg C et al. (2003) Anti-T-lymphocyte globulin treatment in inclusion body myositis: a randomized pilot study. Neurology 61: 260–262
Acknowledgements
This research was supported by the Intramural Research Program of the NIH, National Institute of Neurological Disorders and Stroke, National Institutes of Health, Bethesda, MD, USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Dalakas, M. Mechanisms of Disease: signaling pathways and immunobiology of inflammatory myopathies. Nat Rev Rheumatol 2, 219–227 (2006). https://doi.org/10.1038/ncprheum0140
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncprheum0140
This article is cited by
-
Clinical significance of soluble CD163 in polymyositis-related or dermatomyositis-related interstitial lung disease
Arthritis Research & Therapy (2017)
-
The Immune Response and the Pathogenesis of Idiopathic Inflammatory Myositis: a Critical Review
Clinical Reviews in Allergy & Immunology (2017)
-
Immunotherapies for Immune-Mediated Myopathies: A Current Perspective
Neurotherapeutics (2016)
-
ATOH8: a novel marker in human muscle fiber regeneration
Histochemistry and Cell Biology (2015)
-
Roles of mast cells in the pathogenesis of inflammatory myopathy
Arthritis Research & Therapy (2014)