Abstract
Homeostasis implies a balance between cell growth and cell death. This balance is essential for the development and maintenance of multicellular organisms. Homeostasis is controlled by several mechanisms including apoptosis, a process by which cells condemned to death are completely eliminated. However, in some cases, total destruction and removal of dead cells is not desirable, as when they fulfil a specific function such as formation of the skin barrier provided by corneocytes, also known as terminally differentiated keratinocytes. In this case, programmed cell death results in accumulation of functional cell corpses. Previously, this process has been associated with apoptotic cell death. In this overview, we discuss differences and similarities in the molecular regulation of epidermal programmed cell death and apoptosis. We conclude that despite earlier confusion, apoptosis and cornification occur through distinct molecular pathways, and that possibly antiapoptotic mechanisms are implicated in the terminal differentiation of keratinocytes.
Similar content being viewed by others
Introduction
Homeostasis within an organism is maintained through different forms of programmed cell death. Programs such as apoptosis, necrosis or autophagy ultimately result in the elimination of particular cells from a tissue. However, in specialized forms of differentiation, dead cell corpses are not removed but maintained to fulfil a specific function. These developmental cell death programs result in the production of differentiated ‘storage’ cells containing large amounts of specific proteins or other substances. Examples of such differentiation programs occur in the stalk of the slime mold Dictyostelium, during xylogenesis in plants, erythrocyte differentiation, lens fiber formation and cornification of keratinocytes in the skin.
Both apoptosis and keratinocyte cornification share some similarities at the cellular and molecular level, such as loss of an intact nucleus and other organelles, cytoskeleton and cell shape changes, involvement of proteolytic events and mitochondrial changes. The aim of this review is to compare these crucial events, taking place in both keratinocyte differentiation and apoptosis and to summarize the current evidence that supports the idea that both forms of cell death are distinct processes.
General features of keratinocyte apoptosis and cornification
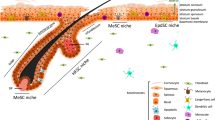
The rapid process of apoptosis, accomplished within a few hours in individual cells, has been extensively studied and characterized during the last decade (Figure 1). During the course of apoptosis, the function of organelles ceases, but the organelles themselves are not degraded. The plasma membrane remains intact preventing leakage of the cellular content into the environment. Membrane blebbing results in formation of separate apoptotic bodies that are finally recognized and phagocytozed by macrophages or neighboring cells.
Morphological and biochemical changes during keratinocyte cornification and apoptosis. (1) The basal layer of the epidermis consists of undifferentiated, mitotic keratinocytes that are attached to the basement membrane. (2) In the spinous layer, the keratinocytes detach from the basal membrane and start to undergo differentiation. The cells flatten and differentiation-specific proteins such as keratins 1 and 10 are expressed. In addition, orchestrated cytoskeleton reorganization occurs through the epithelial sheet. The cell surface extensions or spines end in desmosomes. (3) The granular layer of the epidermis is characterized by the presence of keratohyalin granules. The keratin filament network is crosslinked, DNA is degraded, organelles are destroyed, and the plasma membrane is replaced by the cornified envelope and ceramide deposition from the lamellar bodies. (4) The cornified layer consists of dead cells. (5) The cells are not removed by the phagocytic Langerhans’ cells, but are shed into the environment during desquamation. (6) Upon induction of apoptosis, the caspase cascade becomes activated and apoptotic cells start blebbing. (7) Chromatin and cytoplasm undergo condensation, internucleosomal DNA cleavage occurs, the cytoskeleton is dismantled, the cell membrane ‘invaginates’, and apoptotic bodies are formed. Organelle damage results in release of molecules such as cytochrome c from mitochondria into the cytosol. In contrast, the plasma membrane remains intact avoiding cytoplasm leakage to the environment. (8) Finally, apoptotic bodies are phagocytozed and degraded inside lysosomes
All components required for apoptosis are present in keratinocytes. UVB irradiation acts as a physiological trigger to induce apoptotic or ‘sunburn’ cells in the skin, occurring mainly in the proliferative basal layer.1 The reason for the increased resistance of suprabasal keratinocytes to UVB-induced apoptosis is not clear. Although, it has been shown that Bcl-xL, which is normally localized in the suprabasal layers, cooperates with the antiapoptotic PI3K-Akt pathway to enhance keratinocyte survival upon UVB irradiation.2 UVB-induced apoptosis entails a complex network of signaling pathways activated in response to DNA damage and receptor clustering ultimately converging in the activation of caspases, which are the final executioners of UVB-induced cell death.3 UVB has been reported to trigger activation of the death receptors Fas and TNF-R1 in ligand-dependent and -independent ways.3, 4 The UVB-induced clustering of death receptors can initiate the extrinsic pathway of apoptosis through the formation of the death-inducing signaling complex (DISC).5 Indeed, in Fas ligand-deficient mice, sunburn cell formation is reduced.6 Caspase-8 is activated by Fas-associated death domain (FADD)-mediated recruitment to the Fas DISC. Once released from the complex, it cleaves the Bcl-2 family member Bid. Truncated Bid translocates to the mitochondria where it induces cytochrome c release. Bid can also be cleaved by postmitochondrial-generated caspase activity in UVB-irradiated keratinocytes,7 thereby creating a proapoptotic amplification loop. In accordance, Bcl-2 overexpression led to the protection against UVB-induced apoptosis in these cells, indicating that mitochondrial damage is decisive for the progression of the apoptotic process. Cytochrome c release leads to the activation of the apoptosome, an oligomeric complex of Apaf-1 (apoptosis activating factor 1) and caspase-9, resulting in the amplification of the caspase cascade leading to cell death. Interestingly, UVB irradiation induces, in a p53-dependent way, enhanced expression of Apaf-1 in keratinocyte cultures.1
UVB irradiation induces DNA damage and thereby also activates the intrinsic cell death pathway that leads to mitochondrial damage and cytochrome c release in a receptor-independent way. p53 and Bax are major players in the intrinsic pathway and the mitochondria act as the integrating sensors controlling the apoptosome-mediated activation of caspase-9.8 DNA damage leads to the stabilization of p53 and subsequent induction of Puma and Noxa, both proapoptotic members of the Bcl-2 family. Probably, Puma and/or Noxa target and activate Bax after UVB irradiation, but this has not been confirmed yet by genetic studies. The conformational change and redistribution of Bax from the cytoplasm to the outer mitochondrial membrane induces mitochondrial cytochrome c release and is of major importance in UVB-induced apoptosis.9 Recently, it has been shown that p38 MAPK is required for the UVB-induced Bax conformational change and translocation.9
In keratinocytes, the β1-integrins mediate adhesion to the extracellular matrix, and also regulate the initiation of terminal differentiation and cell-detachment apoptosis or anoikis. Epidermal keratinocytes differentiate when they detach from the basement membrane and migrate to the suprabasal layers. This differentiation signal is transduced by unoccupied β1-integrins.10 In experimental keratinocyte suspension cultures, unoccupied β1-integrins can also induce an apoptotic signaling cascade resulting in upregulated Bax expression and mitochondrial damage.11 However, since apoptosis can occur without evidence of differentiation and vice versa, these processes do not seem to be interdependent.11 In addition, apoptosis does not occur spontaneously in the epidermis when the keratinocytes detach from the basement membrane, migrate to the suprabasal layers and start to differentiate.
Cornification is a slow coordinated process that takes about 2 weeks (Figure 1), occurs simultaneously in the different suprabasal layers of the epidermis and requires the consecutive expression of typical differentiation-associated proteins.12 A keratin filament network is formed and at the transition from the granular to cornified layer, other structural proteins are crosslinked to this protein network.13 The keratinocytes become metabolically inactive, the organelles are degraded and the resulting fully differentiated squames are flattened dead cells that resemble ‘protein sacs’ consisting of more than 80% keratins crosslinked to other cornified envelope proteins.14 During assembly of the epidermal cornified cell envelope, the plasma membrane fuses with the membranes of the lamellar bodies.15 The latter contain lipids that eventually replace the original plasma membrane and play a role in water maintenance. Ultimately, corneocytes are sloughed into the environment. In contrast to apoptotic cells, corneocytes are not phagocytozed by other cells.16
In addition to the interfollicular epidermis, the hair follicle and sebaceous gland, both epidermal derivatives, are also the result of keratinocyte differentiation. The hair follicle consists of an outer root sheath, continuous with the epidermis, which surrounds the hair follicle. Differentiation of the hair shaft is established by the horizontal movements of cells from the basal layer of the outer root sheath to the center of the follicle. The innermost regions of the developing hair follicle become the cortex and cuticle of the hair fiber, while the outer layers become parts of the inner root sheath that covers the hair shaft. Upon hair follicle differentiation, cells forming the cortex, cuticle and inner root sheat keratinize and eventually undergo terminal differentiation and programmed cell death.17 This type of cell death is different from apoptosis that is occurring during the regression phase (catagen) of the hair follicle.18 The sebaceous gland is localized on the lateral wall of the hair follicle. Increased cell volume, accumulation of lipid droplets in the cytoplasm and nuclear degeneration are phenomena indicating terminal differentiation of sebocytes. Sebocyte differentiation eventually leads to holocrine secretion and cell death.19 However, the molecular pathways leading to sebocyte elimination are still unknown.
Cytoskeleton rearrangements
Apoptosis occurs in individual cells surrounded by viable neighboring cells and can be clearly identified by specific morphological changes. Among the striking features are membrane ruffling and blebbing, and loss of focal adhesion sites eventually resulting in the formation of apoptotic bodies and detachment from the substratum. These changes in cell shape require extensive remodeling of the cytoskeleton. Cytokeratin 18 is phosphorylated at a serine residue and cleaved after an aspartate residue during apoptosis and is cleaved in vitro by executioner caspase-3, -6 and -7.20 However, cytokeratin 18 is not expressed in the epidermis.21 Other intermediate filament proteins, such as lamin A (nuclear) and vimentin (cytoplasmic), are also substrates for apoptotic caspases.22 Actin is a substrate for caspases during apoptosis and overexpression of actin fragments induces an apoptotic morphology.23 Membrane blebbing requires the phosphorylation of myosin light chain, a substrate of Rho kinases (ROCKs). During apoptosis, ROCKI, but not ROCKII, is cleaved and activated by caspase-3 and it has been suggested that ROCKI is implicated in apoptotic blebbing.24 Taken together, these different observations indicate that apoptosis leads to dismantling of the cytoskeleton.
As cornification is associated with sheet formation and stratification, cytoskeleton reorganization is not restricted to individual cells, but orchestrated across the entire epithelial sheet. The actin filament network becomes associated with adhesion structures during differentiation, starting at the apical surface of epidermal layers. Using mutant ROCKI or ROCK inhibitors, it was shown that ROCK activity is required to establish a higher-ordered architecture of the actin cytoskeleton during the initial steps of epidermal sheet formation.25 Since active, processed caspase-3 is not detectable in normal newborn or adult skin,26, 27 it is unlikely that caspase-3 is involved in ROCKI activation during epidermal differentiation. These findings also indicate that ROCKI activity probably requires an apoptotic environment to induce membrane blebbing. ROCK inhibition also results in inhibition of keratinocyte terminal differentiation and an increase in keratinocyte proliferation.28 Accordingly, ROCKII activation induced cell cycle arrest and the expression of terminal differentiation markers. These results indicate that ROCK plays a critical role in regulating the balance between proliferation and differentiation in human keratinocyte cultures.
Keratins are the major components of the keratinocyte cytoskeleton. Five different types of keratins can be distinguished, of which type I and type II keratins are the major groups. Polymerization of keratins results in heteropolymers of type I and type II keratins. Strikingly, all type I keratins except the epidermal keratins 9 and 10 contain a conserved caspase cleavage site.22 However, these keratins are not cleaved during epidermal differentiation and it is even not clear whether the specialized epidermal keratins are cleaved in apoptotic conditions. Undifferentiated keratinocytes specifically express keratins 5 and 14, while the outer layers of the epidermis express keratins 1, 2, 9 and 10. The importance of keratins for the structural integrity and barrier function of the skin is demonstrated by inherited skin disorders caused by keratin mutations, and keratin knockout mice or mice expressing keratin mutants.29
In addition, it is of major importance for the epidermal architecture that extensive intercellular contacts are maintained by means of specialized structures such as desmosomes (connecting the intermediate filament network of neighboring cells) and adherens junctions (connecting the actin network of neighboring cells).30 These findings support the cardinal role of the maintenance of the structural integrity of the keratin cytoskeleton and adhesion complexes for the epidermal structure. They indicate that it would be deleterious to activate the apoptotic caspase cascade, as it would cause disintegration of the cytoskeleton and intercellular organization of the keratinocytes, as occurs in other types of cells condemned to death by apoptosis.
Nuclear events
A common feature of apoptosis and cornification is the destruction of the nucleus. However, this event occurs by different molecular mechanisms in the two processes. Nuclear degradation during UV-induced apoptosis is marked by internucleosomal DNA cleavage executed by caspase-activated DNAse (CAD).31, 32 Defects in nuclear degradation during epidermal cornification were not reported in CAD-deficient mice.31 The nucleus is not completely degraded during apoptosis, as nuclear fragments are detectable in the apoptotic bodies that are cleared by uptake by other cells. The DNA is further broken down after engulfment.31
The nuclei of cornifiying keratinocytes do not show chromatin condensation or DNA laddering.33 In addition, TUNEL-positive cells are observed only sporadically in the adult epidermis.32 Finally, the nuclei completely disappear and no nuclear fragments or remnants remain in the corneocytes. The DNAse responsible for DNA degradation during keratinocyte cornification has not been identified so far. In the embryonic epidermis (15.5 dpc), but not in newborn or adult epidermis, caspase-3 becomes upregulated by Notch-1, gets activated by an unknown mechanism and seems to be involved in keratinocyte differentiation.27 Hence, one could speculate that CAD activation and internucleosomal DNA degradation would render differentiating keratinocytes TUNEL positive. Intriguingly, TUNEL positivity was not decreased in caspase-3 knockout embryonic epidermis compared to the wild type.27
Nuclear destruction during keratinocyte differentiation clearly differs from nuclear degradation observed during apoptosis. During apoptosis, several structural nuclear proteins, such as lamins, are degraded by caspases leading to nuclear collapse.34 The pathways leading to nuclear breakdown during cornification remain elusive. Desquamin is the sole epidermis-derived protease activity, described to date, which has been proposed to be involved in this event. Desquamin, originally discovered as a lectin-like protein, is expressed in the transition zone between the granular and cornified layer.35 Desquamin is able to degrade isolated nuclei,36 leaving nuclear inclusions intact while degrading the surrounding basophilic nuclear matrix. This could make the DNA more prone to DNAse activity in cells. However, despite the fact that desquamin activity has been described more than 10 years ago, the molecular identity of this enzyme remains to be determined.
Transcription factors
p53 family
The p53 transcription factor family contains three members: p53, p63 and p73 (Figure 2).37 The number of UVB-induced sunburn cells in p53−/− mice is only ∼20% of those observed in wild-type mice, indicating a crucial role of p53 in UVB-induced apoptosis.38 Mice expressing mutant p53 or those deficient in p53 develop normally and epidermal formation is not impaired, suggesting that there is no role for p53 in cornification. However, these mice are more sensitive to induction of squamous cell carcinoma after chronic UVB irradiation.39
p53 family members and their involvement in apoptosis and keratinocyte differentiation. The p53 transcription factor family contains three genes: p53, p63 and p73.37 The domain structure of these family members is conserved. p63 and p73 contain, compared to p53, an additional PR (proline-rich) and SAM (sterile alpha motif) domain at their C-terminus. In addition, p63 and p73 have many different isoforms, generated by alternative splicing or promoter use, with distinct N- and/or C-termini implicating the TA (transactivation), PR and SAM domain. The p63 gene is crucial for epidermal and ectodermal differentiation and this role is reflected in the identification of p63 as the causative gene in different diseases such as EEC (ectrodactyly-ectodermal dysplasia clefting), LMS (limb-mammary syndrome), AEC (ankyloblepheron-ectodermal dysplasia-clefting), ADULT (acro-dermato-ungual-lacrimal-tooth) syndrome and SHFM (split hand/foot malformation)124
p63-deficient mice have defects in the formation of limbs and skin, and lack hair follicles and teeth.40 The crucial role of p63 in epidermal differentiation is evident from the fact that p63−/− mice have no keratinocytes at all. In wild-type mice, the epidermal expression of a transactivation-deficient p63 isoform, which can inhibit p53-transactivating activity, decreases dramatically after UVB irradiation. In accordance, transgenic overexpression of a transactivating-deficient p63 isoform in mice decreases the UVB-induced apoptotic response in the epidermis.41 The results with the transgenic mice suggest that downregulation of transactivating-deficient p63 may be required for an optimal UVB-mediated apoptotic response. As in the case of p63, overexpression of p73 in keratinocytes results in promoter activation of loricrin, involucrin and transglutaminase I (TG1).42 However, developmental defects in p73-deficient mice are related to neuronal differentiation and not to skin abnormalities.43
In summary, members of the p53 transcription factor family play vital roles in signal transduction leading towards apoptosis and keratinocyte differentiation. However, there is no redundancy between the different family members. In apoptotic signaling, it is mainly p53 that is implicated, whereas keratinocyte differentiation requires p63 activity.
NF-κB
Disruption of the NF-κB pathway by synthetic inhibitors or a dominant negative form of IκBα renders keratinocytes more susceptible to apoptosis induced by TNFα, FasL or UV irradiation.44, 45 In general, NF-κB activation results in protection against apoptosis by upregulating antiapoptotic genes such as members of the Bcl-2 family and cellular inhibitors of apoptosis (c-IAPs). In addition, NF-κB can also act as a positive regulator of cell cycle progression and it has been implicated in invasion and metastatic growth of tumor cells. Therefore, NF-κB has recently emerged as a major culprit in a variety of human cancers, mainly because of its ability to protect transformed cells from apoptosis.46
NF-κB is not activated in proliferating epidermal cells, but p65 is activated and translocated to the nucleus upon differentiation.47 In the epidermis, the expression of NF-κB-dependent antiapoptotic proteins such as c-IAP-1, c-IAP-2, TRAF1 and TRAF2 is increased in differentiating keratinocytes.44 In addition, transgenic overexpression of dominant negative IκBα in murine skin results in premature spontaneous cell death exhibiting apoptotic properties.45 This suggests an important role for NF-κB in protection of keratinocytes against apoptosis when the cells undergo the program of cornification.
Furthermore, ablation of genes encoding proteins that regulate NF-κB signaling gives rise to different types of defects in skin formation. NF-κB activation occurs through phosphorylation and subsequent proteolytic breakdown of IκB (inhibitor of NF-κB). The kinase complex responsible for the phosphorylation contains IKKα, IKKβ and the regulatory subunit IKKγ/NEMO. IKKα deficiency in mice is associated with defects in epidermal differentiation, hair follicle formation and development of limbs and tail.48 The epidermis is thickened, the upper layer is parakeratotic and it is not possible to distinguish a granular layer. However, it is important to note that the defects in epidermal differentiation in IKKα knockouts were demonstrated to be independent from its kinase activity that regulates NF-κB.49 The differentiation abnormalities can be restored by grafting the IKKα−/− skin onto wild-type skin, suggesting that normal skin contains a soluble IKKα-regulated factor that controls keratinocyte differentiation. IKKβ deficiency in the skin decreases the proliferation rate of isolated primary keratinocytes and impairs NF-κB activation in response to TNF or IL-1β.50 However, skin-specific deletion of IKKβ does not affect epidermal differentiation as such, nor does it lead to premature apoptosis during keratinocyte cornification, but rather disrupts immune homeostasis in the skin.50 Mutations in the human X-linked gene encoding NEMO/IKKγ are linked to the male-lethal skin disease incontinentia pigmenti.51 Affected female neonates develop blisters and, paradoxically, an inflammatory response in the epidermis. This is followed by hyperkeratotic lesions that are eventually shed, leaving behind areas of hyperpigmentation in a pattern that respects the lines of Blaschko's. These lines represent a form of human mosaicism due to genetically distinct cell populations participating in epidermis formation. In the case of the X-linked NEMO gene, this may be due to random inactivation of one of the X chromosomes. Disruption of the IKKγ gene in mice results in a model for incontinentia pigmenti.52
RIP4, a member of the RIP kinase family involved in NF-κB signaling, is crucial for normal epidermal differentiation, as RIP4 knockouts die shortly after birth due to abnormal keratinocyte differentiation.53 The skin of these mice is thicker, and the outermost cornified layers are absent. Whether p65 is still translocated to the nucleus in suprabasal keratinocytes or whether NF-κB is still activated during skin differentiation remains to be determined. RIP4 is cleaved by caspases during Fas-induced apoptosis, and it has been suggested that this results in a C-terminal RIP4 fragment that blocks NF-κB-dependent expression of antiapoptotic proteins.54
These transgene and knockout studies suggest that NF-κB signaling is required for normal keratinocyte differentiation. Its precise function may reside in protecting the cells from the classical apoptotic pathway through the induction of antiapoptotic mechanisms, allowing the cells to follow the terminal differentiation pathway towards the formation of a protective barrier. Remarkably, IKKα drives keratinocyte terminal differentiation in a kinase- and NF-κB-independent way.
Proteases
Protease activity is indispensable during both keratinocyte differentiation and apoptosis. However, different enzymes are implicated in these processes.
Caspases
Caspases are essential executioners of apoptosis.55 Although different caspases are expressed in the adult epidermis (caspase-1, -2, -3, -4, -6, -7, -8, -9, -11 and -14),26, 56 evidence that the proapoptotic caspases take part in normal skin formation is absent. Despite an early suggestion that caspase-3 is required for corneocyte formation,57 several other data point out that apoptotic caspases are not activated during adult keratinocyte cornification. First, other research groups showed that caspase-3 and other apoptotic caspases remain unprocessed in differentiating keratinocytes.26 Secondly, the use of caspase inhibitors to examine the involvement of proapoptotic caspases in keratinocyte cornification indicates that (i) when applied at 25 μM in organotypic skin cocultures, zVAD-fmk can block caspase-3 processing in UVB-induced apoptosis, but had no effect on keratinocyte differentiation that could be identified using light microscopy (Lippens S and Declercq W, unpublished data). However, application of broad-range caspase inhibitors at concentrations >100 μM resulted in inhibition of keratinocyte cornification.57, 58 Yet, it is noteworthy that in the latter experiments the inhibitors were used at concentrations that also inhibit other proteases such as calpains and cathepsins.59, 60 (ii) In vitro, calcium ionophore A23187-induced cornified envelope formation is not influenced by pretreatment of the cells with caspase inhibitors.33 (iii) Subcutaneous injection of zVAD-fmk in murine models for systemic lupus erythematosus, a non-organ-specific autoimmune disease in which apoptotic cells in the skin are believed to be the source of self antigens, had an inhibitory effect on the number of apoptotic cells in the epidermis and dermis, but did not change skin formation in general.61 Taken together, these data suggest that proapoptotic caspases are not involved in keratinocyte cornification.
Remarkably, it was recently suggested that caspase-3 is involved in differentiation of embryonic keratinocytes.27 Embryonic keratinocyte differentiation is delayed in caspase-3 knockout mice, but newborn and adult skin formation is not affected.27, 62 This finding suggests that activation of proapoptotic caspases is not necessarily correlated with apoptosis, but can be part of a differentiation pathway. PKC-δ, a positive regulator of keratinocyte differentiation that can be activated by caspase-3 cleavage, is cleaved and activated during growth and differentiation of embryonic keratinocytes.27 However, it remains to be determined whether these cleaved PKC-δ products are absent in caspase-3-deficient mice. Although caspase-3 may be involved in the commitment of embryonic keratinocytes to convert from proliferation to differentiation, it is not required for the differentiation program that engages cornification and constant renewal of the epidermis.27
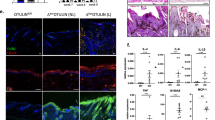
Importantly, one member of the caspase family, the nonapoptotic caspase-14, seems to be expressed and processed in association with keratinocyte differentiation.26, 63 The expression of caspase-14 is highly restricted to the skin and some other epithelial layers such as the choroid plexus, the retinal pigment epithelium and Hassall's bodies.64 In the skin, caspase-14 expression occurs in the differentiating suprabasal cells (Figure 3).26, 63, 64 Activation of caspase-14 is associated with stratum corneum formation, and active caspase-14 was shown to be present in stratum corneum extracts,63, 65, 66 suggesting a role for caspase-14 during keratinocyte cornification. Interestingly, caspase-14 expression is reduced in the parakeratotic regions in psoriatic patients.65 To date, no caspase-14 substrates have been identified. However, recently, it was shown that processed caspase-14 preferably recognizes the WEHD tetrapeptide motif, a preference shared with caspase-1.67 This observation is in accordance with the fact that in a phylogenetic analysis, caspase-14 was classified as an inflammatory caspase.55 It remains to be determined whether caspase-14 could act as a cytokine activator, as other inflammatory caspases do. Caspase-14 is processed in vivo at Ile152,68 implying that caspase-14 is not activated by upstream caspases or by self-processing. The possible involvement of caspase-14 in skin differentiation will only become apparent once caspase-14-deficient mice become available.
Structure of caspase-14 and its expression in the epidermis. (a) Schematic structure of procaspase-14 as compared to other short-prodomain caspases (human).125 In general, these caspases have a prodomain ranging from 23 to 28 amino acids. There is currently no evidence that caspase-14 contains a prodomain. Note that human caspase-14 is not processed at a canonical Asp residue due to self-processing or cleavage by upstream caspases, but instead at Ile152.68 (b) Expression of caspase-14 in adult murine epidermis. Caspase-14 is expressed in all suprabasal layers including the stratum spinosum (ss), the stratum granulosum (sg) and the stratum corneum (sc)
Cathepsins
Cathepsins are implicated in both apoptosis and epidermal differentiation. Depending on the cell type and death trigger, pharmacological inhibition of cathepsin D can lead to blockage of cytochrome c release, caspase activation or delayed cell death.69, 70 However, studies with cathepsin D knockout mice indicate a dual role for cathepsin D in apoptosis. On the one hand, cathepsin D-deficient fibroblasts are protected against etoposide-induced killing and on the other hand, cathepsin D seems to be required for metabolic maintenance and protection against apoptosis in retinal photoreceptor cells.71, 72 In agreement with its role in cell survival, cathepsin D knockout mice suffer from intestinal necrosis and lymphoid organ destruction.73 In differentiating keratinocytes, cathepsin D is involved in proteolytic processing of transglutaminase 1. In the skin of cathepsin D-deficient mice, formation of cornified envelopes is altered, resulting in a thicker stratum corneum with low expression levels of terminal differentiation markers such as involucrin, loricrin and filaggrin.74
Cathepsin B-deficient mice show no release of cytochrome c during TNF-mediated hepatocyte apoptosis and liver injury, and present no aberrant skin phenotype,75 suggesting that either cathepsin B is not implicated in skin differentiation or other cathepsins compensate for its function.
The importance of cathepsins in skin formation is also reflected in other cathepsin knockout studies revealing that normal epidermal homeostasis and hair follicle formation require cathepsin L.76 The mutant furless and nackt mice, which show defects in hair follicle development, have an inactivating mutation in the cathepsin L gene.76 Genetic mapping revealed that the mutations in the autosomal recessive Papillon–Lefevre syndrome, marked by premature tooth loss and palmoplantar keratosis, result in loss-of-function of the cathepsin C gene.77 Furthermore, cathepsin L2 has been detected in stratum corneum extracts.78 This protease seems to be activated during epidermal differentiation and secreted into the intercellular space.
Calpains
Calpains are cytosolic neutral cystein proteases that are activated upon increased Ca2+ levels. Autoproteolytic cleavage of the enzymes further enhances their activity. Calpains are divided into two broad classes, ubiquitous and tissue-specific. In mammals, two major calpains exist: μ-calpain (calpain I) and m-calpain (calpain II), activated in vitro by μM and mM Ca2+ concentrations, respectively. So far, no difference in the substrate specificity of the two isozymes has been found.
Reports on calpain activity during apoptosis are not consistent in their conclusions. Depending on the nature and severity of the apoptotic stimulus and the cell type studied, calpains seem to play both promoting as well as protective roles.79, 80, 81, 82 Calpains can cleave several apoptotic proteins (e.g. Apaf-1, Bax, BID) and cytoskeletal proteins (e.g. fodrin, actin, vimentin and keratins), which are also substrates for caspases.81, 83, 84 Furthermore, there exists also crosstalk between the calpain and caspase protease systems. Calpains mediate cleavage of caspases-3, -7, -8, -9 and -12 resulting in their activation or inhibition.85, 86, 87 Despite the presence of calpains in the epidermis, no processing of proapoptotic caspases occurs.26 There is also evidence that caspases can upregulate calpain activity through direct cleavage of calpastatin, the endogenous protein inhibitor of calpains.88 Therefore, caspases were suggested to indirectly upregulate calpain activity. Most cell death systems leading to activation of calpains seem to produce an apoptotic-like morphology.79 In addition, calpains can participate in plasma membrane permeabilization leading to secondary necrosis.89
In the epidermis, where an increasing calcium gradient towards the skin surface exists, different cleavage events are calcium dependent. Both μ- and m-calpain are present in the suprabasal layers of the epidermis.90 Evidence for the involvement of calpains in keratinocyte differentiation is based on the use of synthetic calpain inhibitors that result in blocking of profilaggrin and TG1 cleavage.91, 92 These observations could not be corroborated by genetic approaches because mice deficient in the regulatory subunit develop defects in vasculogenesis and erythropoiesis and die early during embryonic development, which impedes evaluation of the importance of this protease in epidermal differentiation.93 μ-Calpain-null mice have no apparent embryological or epidermal defects, suggesting that m-calpain compensates for μ-calpain during development.94 m-Calpain-deficient mice have not been generated so far.
Taken together, gene-targeting studies indicate that proteases involved in apoptosis do not necessarily participate in epidermal differentiation and vice versa. However, cathepsin D fulfils a role both in the apoptotic pathway and in keratinocyte cornification, probably by cleaving different substrates in both processes.
Mitochondrial factors and apoptosome formation
Mitochondria and the Bcl-2 family members play an important role during apoptotic cell death.95 Upon keratinocyte terminal differentiation, the expression of the Bcl-2 family members is altered. The antiapoptotic Bcl-2 is expressed in undifferentiated keratinocytes, but it is downregulated when the cells leave the basal layer and start to differentiate.96 Conversely, both proapoptotic Bax and Bak and the antiapoptotic Bcl-XL are expressed in the suprabasal layers of the epidermis.2, 97, 98
Abnormalities in skin formation have not been reported for any of the Bcl-2 family member knockouts,99 except for Bcl-2 knockout mice that have an altered hair follicle cyclus compared to wild-type mice. The first anagen phase or growth phase is retarded (5–6 weeks compared to 4 weeks) and graying occurs during the catagen or apoptosis-driven involution phase.100 The graying is probably due to melanocyte apoptosis during the first catagen phase. Skin-specific bcl-2 transgenesis induces acceleration of the first anagen phase.101 In these mice, keratinocyte differentiation is not affected, but upon exposure to UV light fewer apoptotic cells are observed.101 These data indicate that Bcl-2 is important for keratinocyte apoptosis, but not for keratinocyte cornification. Epidermal specific overexpression of the antiapoptotic Bcl-XL and proapoptotic Bcl-XS, respectively, decreased and increased sensitivity towards apoptosis induced by UVB,102 but general epidermal formation was not affected in these animals. Together, these results suggest that the program leading to keratinocyte differentiation does not involve the classical mitochondrial apoptotic pathway.
Although a drop in mitochondrial membrane potential and the release of cytochrome c during in vitro keratinocyte terminal differentiation has been reported,58 these mitochondrial changes do not lead to a classical apoptotic phenotype. Instead, it was suggested that cytochrome c release during keratinocyte differentiation leads to transcription factor activation and gene expression.103 Although Apaf-1 and caspase-9, both required for the formation of the apoptosome, are present in epidermal keratinocytes,1, 44 cytochrome c release in differentiating keratinocytes did not result in apoptosis. This may be due to low levels of released cytochrome c or an increase in antiapoptotic proteins during keratinocyte differentiation. In this respect, the NF-κB signaling pathway is of major importance (see above). In addition, it has been reported that hsp70 and hsp90 are constitutively expressed in the epidermis.104, 105 These two heat–shock proteins are both able to inhibit the apoptosome formation,106, 107 and hsp70 can also antagonize the proapoptotic effects of apoptosis-inducing factor.108 Overexpression of hsp70 can prevent UVB-induced apoptosis in an epidermal carcinoma line,109 and hsp70-deficient mice are more susceptible to UVB-induced apoptosis.110 Taken together, these observations may reflect the presence of strong antiapoptotic mechanisms, which may protect keratinocytes from environmental stress-induced apoptosis.
Transglutaminases
Keratinocyte cornification requires the involvement of transglutaminases,111 enzymes with crosslinking activity. Upon Ca2+-dependent activation, transglutaminases catalyze formation of ɛ-(γ-glutamyl)lysine bonds. Three types of transglutaminases are found in keratinocytes: transglutaminase I (TG1), transglutaminase III (TG3) and transglutaminase V (TG5). During cornified envelope formation, membrane-associated transglutaminase activity is found first, followed by cytoplasmic transglutaminase activity, whereas apoptotic keratinocytes exhibit only cytoplasmic transglutaminase activity.33 TG1 is attached to the inner side of the plasma membrane and probably involved in the initial crosslinking during the cornification process.112 Mutations of the human TG1 gene have been correlated with lamellar ichthyosis, a skin disorder caused by defects in the cornification program.113 A similar phenotype is observed in mice lacking the TG1 gene.114 These mice have defects in the formation of the epidermal barrier and the cornified envelopes, and die shortly after birth; however, no effects on apoptosis have been reported. TG2 knockout mice do not have any defects in the keratinocyte differentiation program, and its role in apoptosis remains unclear.115 However, TG2 is also sporadically expressed in the basal layer of the epidermis, where it is involved in wound healing.116 TG3 is a soluble enzyme believed to be responsible for the later phase of envelope assembly.117 Although the expression pattern of TG5 is not restricted to the epidermis, it probably plays a role in cornified envelope assembly.118
Final destination of cell corpses
The very final stage of apoptosis is the uptake of apoptotic bodies by means of phagocytosis. To avoid inflammation, the cell membrane of apoptotic cells remains intact to prevent leakage of the cell contents. For the same reason, the fast and efficient ‘clearance’ of the apoptotic bodies is of great importance. Macrophages specifically distinguish apoptotic cells from other cells. This is accomplished by phosphatidylserine exposure, an early apoptotic event that allows recognition or uptake of the apoptotic cell by the macrophage.119 Mutation analysis in Caenorhabditis elegans led to the identification of different genes crucial for engulfment of dead cells. One of these genes is ced-7, of which ATP-binding-cassette transporter 1 (ABC1) is the human homolog.120 ABC1 is responsible for redistribution of phosphatidylserine at the plasma membrane.121
The skin also contains phagocytosis-competent cells, the Langerhans’ cells, which are elements of the adaptive immune system. These cells are responsible for antigen uptake, processing and presentation, upon which they migrate to the lymph nodes. However, Langerhans’ cells do not phagocytoze terminally differentiated dead keratinocytes.16, 122 The corneocytes remain attached to underlying skin for some time in order to fulfil the barrier function of the skin. In addition, it is currently not clear whether terminally differentiating keratinocytes expose PS at their surface. When the corneocytes are replaced by differentiating keratinocytes from the inward layers, the components of corneodesmosomes or desmosomes between the outermost corneocytes are proteolytically degraded by proteases that remained inactive until this very final stage of skin formation.123 Finally, the detached cells are shed into the environment.
Conclusions
Taken together, both keratinocyte differentiation and apoptosis require DNA degradation, nuclear destruction and substantial proteolytic activity, and both lead to cell death. Nevertheless, the final outcomes of these two cell death programs are completely different. While apoptosis is a suicidal program aimed at eliminating individual cells, programmed cell death during epidermal development results in cornification of the keratinocytes that remain and establish a tight barrier of dead cells protecting the organism from environmental insults. The molecular signal transduction pathways and crucial regulatory mechanisms of apoptosis and cornification of keratinocytes are clearly different. Similarities between both processes may lay in the fact that some proteins such as calpains, cathepsins, transglutaminases and transcription factors such as NF-kB and p53 family members participate in both signal transduction pathways (Figure 4). However, profound differences can be found at several levels: (1) p53, a major integrator of nuclear damage-induced cell death, has no obvious role in epidermal differentiation, while for terminal keratinocyte differentiation p63 is crucial; (2) caspases, the key regulators of apoptosis initiation and excecution, apparently play no role in adult keratinocyte differentiation, except maybe for the nonapoptotic caspase-14; (3) cathepsin L and C are implicated in hair follicle development and epidermal differentiation, while cathepsin B-deficient mice show impaired TNF-induced apoptosis in the liver but present no apparent skin phenotype; (4) transglutaminases I, III and V participate in the formation of cornified envelopes, whereas TG2 may contribute to apoptosis and (5) NF-κB protects most cell types, including keratinocytes, from apoptosis. Interestingly, NF-κB seems required to mount an antiapoptotic program in suprabasal keratinocytes to allow them to undergo cornification and prevent premature apoptosis.
Apoptosis-related signaling molecules in epidermal differentiation. In basal keratinocytes, p63 maintains the proliferative potential of amplifying cells and controls stratification of the epidermis.40, 126 Upon differentiation, the expression of the p63 isoforms is altered, a process that may be required for allowing terminal keratinocyte differentiation.127 NF-κB becomes activated in the suprabasal keratinocytes and participates in the upregulation of antiapoptotic genes. IKKα is crucial for cornification, surprisingly this function is independent from its kinase activity and NF-κB-inducing capacity.49 RIP4, a RIP family member involved in NF-κB signaling, is also essential for normal keratinocyte differentiation as RIP4−/− mice lack cornified layers.53 ROCK family members stimulate the ordering of the actin cytoskeleton (ROCKI) and terminal keratinocyte differentiation (ROCKII).25, 28 The expression pattern of Bcl-2 family members changes upon keratinocyte differentiation. Their role is not related to skin differentiation as such, but they participate in the control of cellular integrity upon exposure of the skin to damaging agents (e.g. UVB). Caspase-14 expression is upregulated during keratinocyte differentiation.26, 63, 64 The activation of caspase-14, the only caspase that is activated in normal skin, is associated with epidermal cornification, but its precise role remains to be uncovered. During cornification, cathepsin D, among other proteases, can lead to the proteolytic activation of TG1.74 TG1 crosslinks proteins and is important for the correct assembly of the cornified envelope.113, 114 Desquamin, a protease of which the molecular identity remains to be determined, is expressed at the transition zone between the granular and cornified layer. It has been suggested that desquamin is involved in the degradation of the nuclear matrix.36 Cathepsin L2 is secreted in the intercellular space and probably participates in the desquamation event
Abbreviations
- DISC:
-
death-inducing signaling complex
- FADD:
-
Fas-associated death domain
- Apaf-1:
-
apoptosis-activating factor 1
- ROCKs:
-
Rho kinases
References
Qin JZ, Chaturvedi V, Denning MF, Bacon P, Panella J, Choubey D and Nickoloff BJ (2002) Regulation of apoptosis by p53 in UV-irradiated human epidermis, psoriatic plaques and senescent keratinocytes. Oncogene 21: 2991–3002
Umeda J, Sano S, Kogawa K, Motoyama N, Yoshikawa K, Itami S, Kondoh G, Watanabe T and Takeda J (2003) In vivo cooperation between Bcl-xL and the phosphoinositide 3-kinase-Akt signaling pathway for the protection of epidermal keratinocytes from apoptosis. FASEB J. 17: 610–620
Kulms D, Zeise E, Poppelmann B and Schwarz T (2002) DNA damage, death receptor activation and reactive oxygen species contribute to ultraviolet radiation-induced apoptosis in an essential and independent way. Oncogene 21: 5844–5851
Leverkus M, Yaar M and Gilchrest BA (1997) Fas/Fas ligand interaction contributes to UV-induced apoptosis in human keratinocytes. Exp. Cell Res. 232: 255–262
Beyaert R, Van Loo G, Heyninck K and Vandenabeele P (2002) Signaling to gene activation and cell death by tumor necrosis factor receptors and Fas. Int. Rev. Cytol. 214: 225–272
Hill LL, Ouhtit A, Loughlin SM, Kripke ML, Ananthaswamy HN and Owen-Schaub LB (1999) Fas ligand: a sensor for DNA damage critical in skin cancer etiology. Science 285: 898–900
Assefa Z, Garmyn M, Vantieghem A, Declercq W, Vandenabeele P, Vandenheede JR and Agostinis P (2003) Ultraviolet B radiation-induced apoptosis in human keratinocytes: cytosolic activation of procaspase-8 and the role of Bcl-2. FEBS Lett. 540: 125–132
Sitailo LA, Tibudan SS and Denning MF (2002) Activation of caspase-9 is required for UV-induced apoptosis of human keratinocytes. J. Biol. Chem. 277: 19346–19352
Van Laethem A, Van Kelst S, Lippens S, Declercq W, Vandenabeele P, Janssens S, Vandenheede JR, Garmyn M and Agostinis P (2004) Activation of p38 MAPK is required for Bax translocation to mitochondria, cytochrome c release and apoptosis induced by UVB irradiation in human keratinocytes. FASEB J. 18: 1946–1948
Levy L, Broad S, Diekmann D, Evans RD and Watt FM (2000) Beta1 integrins regulate keratinocyte adhesion and differentiation by distinct mechanisms. Mol. Biol. Cell 11: 453–466
Mitra RS, Wrone-Smith T, Simonian P, Foreman KE, Nunez G and Nickoloff BJ (1997) Apoptosis in keratinocytes is not dependent on induction of differentiation. Lab. Invest. 76: 99–107
Fuchs E and Raghavan S (2002) Getting under the skin of epidermal morphogenesis. Nat. Rev. Genet. 3: 199–209
Presland RB and Dale BA (2000) Epithelial structural proteins of the skin and oral cavity: function in health and disease. Crit. Rev. Oral Biol. Med. 11: 383–408
Fuchs E (1990) Epidermal differentiation. Curr. Opin. Cell Biol. 2: 1028–1035
Swartzendruber DC, Wertz PW, Kitko DJ, Madison KC and Downing DT (1989) Molecular models of the intercellular lipid lamellae in mammalian stratum corneum. J. Invest. Dermatol. 92: 251–257
Boehncke WH, Dorhage KW, Harms D, Radzun HJ, Hauschild A and Sterry W (1993) Discrimination between immunoaccessory and phagocytic monocytes/macrophages of the skin in paraffin-embedded tissue by the monoclonal antibody Ki-M1P. Br. J. Dermatol. 129: 124–130
Paus R and Cotsarelis G (1999) The biology of hair follicles. N. Engl. J. Med. 341: 491–497
Lindner G, Botchkarev VA, Botchkareva NV, Ling G, van der Veen C and Paus R (1997) Analysis of apoptosis during hair follicle regression (catagen). Am. J. Pathol. 151: 1601–1617
Wrobel A, Seltmann H, Fimmel S, Muller-Decker K, Tsukada M, Bogdanoff B, Mandt N, Blume-Peytavi U, Orfanos CE and Zouboulis CC (2003) Differentiation and apoptosis in human immortalized sebocytes. J. Invest. Dermatol. 120: 175–181
Caulin C, Salvesen GS and Oshima RG (1997) Caspase cleavage of keratin 18 and reorganization of intermediate filaments during epithelial cell apoptosis. J. Cell Biol. 138: 1379–1394
Moll R, Franke WW, Schiller DL, Geiger B and Krepler R (1982) The catalog of human cytokeratins: patterns of expression in normal epithelia, tumors and cultured cells. Cell 31: 11–24
Oshima RG (2002) Apoptosis and keratin intermediate filaments. Cell Death Differ. 9: 486–492
Mashima T, Naito M and Tsuruo T (1999) Caspase-mediated cleavage of cytoskeletal actin plays a positive role in the process of morphological apoptosis. Oncogene 18: 2423–2430
Sebbagh M, Renvoize C, Hamelin J, Riche N, Bertoglio J and Breard J (2001) Caspase-3-mediated cleavage of ROCK I induces MLC phosphorylation and apoptotic membrane blebbing. Nat. Cell Biol. 3: 346–352
Vaezi A, Bauer C, Vasioukhin V and Fuchs E (2002) Actin cable dynamics and Rho/Rock orchestrate a polarized cytoskeletal architecture in the early steps of assembling a stratified epithelium. Dev. Cell 3: 367–381
Lippens S, Kockx M, Knaapen M, Mortier L, Polakowska R, Verheyen A, Garmyn M, Zwijsen A, Formstecher P, Huylebroeck D, Vandenabeele P and Declercq W (2000) Epidermal differentiation does not involve the pro-apoptotic executioner caspases, but is associated with caspase-14 induction and processing. Cell Death Differ. 7: 1218–1224
Okuyama R, Nguyen BC, Talora C, Ogawa E, Di Vignano AT, Lioumi M, Chiorino G, Tagami H, Woo M and Dotto GP (2004) High commitment of embryonic keratinocytes to terminal differentiation through a Notch1-caspase 3 regulatory mechanism. Dev. Cell 6: 551–562
McMullan R, Lax S, Robertson VH, Radford DJ, Broad S, Watt FM, Rowles A, Croft DR, Olson MF and Hotchin NA (2003) Keratinocyte differentiation is regulated by the Rho and ROCK signaling pathway. Curr. Biol. 13: 2185–2189
Porter RM and Lane EB (2003) Phenotypes, genotypes and their contribution to understanding keratin function. Trends Genet. 19: 278–285
Garrod DR, Merritt AJ and Nie Z (2002) Desmosomal cadherins. Curr. Opin. Cell Biol. 14: 537–545
Nagata S, Nagase H, Kawane K, Mukae N and Fukuyama H (2003) Degradation of chromosomal DNA during apoptosis. Cell Death Differ. 10: 108–116
Mass P, Hoffmann K, Gambichler T, Altmeyer P and Mannherz HG (2003) Premature keratinocyte death and expression of marker proteins of apoptosis in human skin after UVB exposure. Arch. Dermatol. Res. 295: 71–79
Takahashi H, Aoki N, Nakamura S, Asano K, Ishida-Yamamoto A and Iizuka H (2000) Cornified cell envelope formation is distinct from apoptosis in epidermal keratinocytes. J. Dermatol. Sci. 23: 161–169
Biggiogera M, Bottone MG, Scovassi AI, Soldani C, Vecchio L and Pellicciari C (2004) Rearrangement of nuclear ribonucleoprotein (RNP)-containing structures during apoptosis and transcriptional arrest. Biol. Cell 96: 603–615
Brysk MM, Bell T and Rajaraman S (1991) Sensitivity of desquamin to proteolytic degradation. Pathobiology 59: 109–112
Selvanayagam P, Lei G, Bell T, Ram S, Brysk H, Rajaraman S and Brysk MM (1998) Desquamin is an epidermal ribonuclease. J. Cell. Biochem. 68: 74–82
Melino G, Lu X, Gasco M, Crook T and Knight RA (2003) Functional regulation of p73 and p63: development and cancer. Trends Biochem. Sci. 28: 663–670
Lu YP, Lou YR, Peng QY, Xie JG and Conney AH (2004) Stimulatory effect of topical application of caffeine on UVB-induced apoptosis in the epidermis of p53 and Bax knockout mice. Cancer Res. 64: 5020–5027
Li G, Tron V and Ho V (1998) Induction of squamous cell carcinoma in p53-deficient mice after ultraviolet irradiation. J. Invest. Dermatol. 110: 72–75
Yang A, Schweitzer R, Sun D, Kaghad M, Walker N, Bronson RT, Tabin C, Sharpe A, Caput D, Crum C and McKeon F (1999) p63 is essential for regenerative proliferation in limb, craniofacial and epithelial development. Nature 398: 714–718
Liefer KM, Koster MI, Wang XJ, Yang A, McKeon F and Roop DR (2000) Down-regulation of p63 is required for epidermal UV-B-induced apoptosis. Cancer Res. 60: 4016–4020
De Laurenzi V, Rossi A, Terrinoni A, Barcaroli D, Levrero M, Costanzo A, Knight RA, Guerrieri P and Melino G (2000) p63 and p73 transactivate differentiation gene promoters in human keratinocytes. Biochem. Biophys. Res. Commun. 273: 342–346
Yang A, Walker N, Bronson R, Kaghad M, Oosterwegel M, Bonnin J, Vagner C, Bonnet H, Dikkes P, Sharpe A, McKeon F and Caput D (2000) p73-deficient mice have neurological, pheromonal and inflammatory defects but lack spontaneous tumours. Nature 404: 99–103
Chaturvedi V, Qin JZ, Denning MF, Choubey D, Diaz MO and Nickoloff BJ (1999) Apoptosis in proliferating, senescent, and immortalized keratinocytes. J. Biol. Chem. 274: 23358–23367
Seitz CS, Freiberg RA, Hinata K and Khavari PA (2000) NF-kappaB determines localization and features of cell death in epidermis. J. Clin. Invest. 105: 253–260
Greten FR and Karin M (2004) The IKK/NF-kappaB activation pathway – a target for prevention and treatment of cancer. Cancer Lett. 206: 193–199
Seitz CS, Lin Q, Deng H and Khavari PA (1998) Alterations in NF-kappaB function in transgenic epithelial tissue demonstrate a growth inhibitory role for NF-kappaB. Proc. Natl. Acad. Sci. USA 95: 2307–2312
Hu Y, Baud V, Delhase M, Zhang P, Deerinck T, Ellisman M, Johnson R and Karin M (1999) Abnormal morphogenesis but intact IKK activation in mice lacking the IKKalpha subunit of IkappaB kinase. Science 284: 316–320
Hu Y, Baud V, Oga T, Kim KI, Yoshida K and Karin M (2001) IKKalpha controls formation of the epidermis independently of NF-kappaB. Nature 410: 710–714
Pasparakis M, Courtois G, Hafner M, Schmidt-Supprian M, Nenci A, Toksoy A, Krampert M, Goebeler M, Gillitzer R, Israel A, Krieg T, Rajewsky K and Haase I (2002) TNF-mediated inflammatory skin disease in mice with epidermis-specific deletion of IKK2. Nature 417: 861–866
Smahi A, Courtois G, Vabres P, Yamaoka S, Heuertz S, Munnich A, Israel A, Heiss NS, Klauck SM, Kioschis P, Wiemann S, Poustka A, Esposito T, Bardaro T, Gianfrancesco F, Ciccodicola A, D'Urso M, Woffendin H, Jakins T, Donnai D, Stewart H, Kenwrick SJ, Aradhya S, Yamagata T, Levy M, Lewis RA and Nelson DL (2000) Genomic rearrangement in NEMO impairs NF-kappaB activation and is a cause of incontinentia pigmention. The International Incontinentia Pigmenti (IP) Consortium. Nature 405: 466–472
Schmidt-Supprian M, Bloch W, Courtois G, Addicks K, Israel A, Rajewsky K and Pasparakis M (2000) NEMO/IKK gamma-deficient mice model incontinentia pigmenti. Mol. Cell 5: 981–992
Holland P, Willis C, Kanaly S, Glaccum M, Warren A, Charrier K, Murison J, Derry J, Virca G, Bird T and Peschon J (2002) RIP4 is an ankyrin repeat-containing kinase essential for keratinocyte differentiation. Curr. Biol. 12: 1424–1428
Meylan E, Martinon F, Thome M, Gschwendt M and Tschopp J (2002) RIP4 (DIK/PKK), a novel member of the RIP kinase family, activates NF-kappa B and is processed during apoptosis. EMBO Rep. 3: 1201–1208
Lamkanfi M, Declercq W, Kalai M, Saelens X and Vandenabeele P (2002) Alice in caspase land. A phylogenetic analysis of caspases from worm to man. Cell Death Differ. 9: 358–361
Takahashi T, Ogo M and Hibino T (1998) Partial purification and characterization of two distinct types of caspases from human epidermis. J. Invest. Dermatol. 111: 367–372
Weil M, Raff MC and Braga VM (1999) Caspase activation in the terminal differentiation of human epidermal keratinocytes. Curr. Biol. 9: 361–364
Allombert-Blaise C, Tamiji S, Mortier L, Fauvel H, Tual M, Delaporte E, Piette F, DeLassale EM, Formstecher P, Marchetti P and Polakowska R (2003) Terminal differentiation of human epidermal keratinocytes involves mitochondria- and caspase-dependent cell death pathway. Cell Death Differ. 10: 850–852
Foghsgaard L, Wissing D, Mauch D, Lademann U, Bastholm L, Boes M, Elling F, Leist M and Jaattela M (2001) Cathepsin B acts as a dominant execution protease in tumor cell apoptosis induced by tumor necrosis factor. J. Cell Biol. 153: 999–1010
Schotte P, Declercq W, Van Huffel S, Vandenabeele P and Beyaert R (1999) Non-specific effects of methyl ketone peptide inhibitors of caspases. FEBS Lett. 442: 117–121
Seery JP, Cattell V and Watt FM (2001) Cutting edge: amelioration of kidney disease in a transgenic mouse model of lupus nephritis by administration of the caspase inhibitor carbobenzoxy-valyl-alanyl-aspartyl-(beta-o-methyl)-fluoromethylketone. J. Immunol. 167: 2452–2455
Woo M, Hakem R, Soengas MS, Duncan GS, Shahinian A, Kagi D, Hakem A, McCurrach M, Khoo W, Kaufman SA, Senaldi G, Howard T, Lowe SW and Mak TW (1998) Essential contribution of caspase 3/CPP32 to apoptosis and its associated nuclear changes. Genes Dev. 12: 806–819
Eckhart L, Declercq W, Ban J, Rendl M, Lengauer B, Mayer C, Lippens S, Vandenabeele P and Tschachler E (2000) Terminal differentiation of human keratinocytes and stratum corneum formation is associated with caspase-14 activation. J. Invest. Dermatol. 115: 1148–1151
Lippens S, VandenBroecke C, Van Damme E, Tschachler E, Vandenabeele P and Declercq W (2003) Caspase-14 is expressed in the epidermis, the choroid plexus, the retinal pigment epithelium and thymic Hassall's bodies. Cell Death Differ. 10: 257–259
Lippens S, Kockx M, Denecker G, Knaapen M, Verheyen A, Christiaen R, Tschachler E, Vandenabeele P and Declercq W (2004) Vitamin D3 induces caspase-14 expression in psoriatic lesions and enhances caspase-14 processing in organotypic skin cultures. Am. J. Pathol. 165: 833–841
Fischer H, Stichenwirth M, Dockal M, Ghannadan M, Buchberger M, Bach J, Kapetanopoulos A, Declercq W, Tschachler E and Eckhart L (2004) Stratum corneum-derived caspase-14 is catalytically active. FEBS Lett. 577: 446–450
Mikolajczyk J, Scott FL, Krajewski S, Sutherlin DP and Salvesen GS (2004) Activation and substrate specificity of caspase-14. Biochemistry 43: 10560–10569
Chien AJ, Presland RB and Kuechle MK (2002) Processing of native caspase-14 occurs at an atypical cleavage site in normal epidermal differentiation. Biochem. Biophys. Res. Commun. 296: 911–917
Johansson AC, Steen H, Ollinger K and Roberg K (2003) Cathepsin D mediates cytochrome c release and caspase activation in human fibroblast apoptosis induced by staurosporine. Cell Death Differ. 10: 1253–1259
Bidere N, Lorenzo HK, Carmona S, Laforge M, Harper F, Dumont C and Senik A (2003) Cathepsin D triggers Bax activation, resulting in selective apoptosis-inducing factor (AIF) relocation in T lymphocytes entering the early commitment phase to apoptosis. J. Biol. Chem. 278: 31401–31411
Wu GS, Saftig P, Peters C and El-Deiry WS (1998) Potential role for cathepsin D in p53-dependent tumor suppression and chemosensitivity. Oncogene 16: 2177–2183
Koike M, Shibata M, Ohsawa Y, Nakanishi H, Koga T, Kametaka S, Waguri S, Momoi T, Kominami E, Peters C, Figura K, Saftig P and Uchiyama Y (2003) Involvement of two different cell death pathways in retinal atrophy of cathepsin D-deficient mice. Mol. Cell. Neurosci. 22: 146–161
Saftig P, Hetman M, Schmahl W, Weber K, Heine L, Mossmann H, Koster A, Hess B, Evers M, von Figura K and Peters C (1995) Mice deficient for the lysosomal proteinase cathepsin D exhibit progressive atrophy of the intestinal mucosa and profound destruction of lymphoid cells. EMBO J. 14: 3599–3608
Egberts F, Heinrich M, Jensen JM, Winoto-Morbach S, Pfeiffer S, Wickel M, Schunck M, Steude J, Saftig P, Proksch E and Schutze S (2004) Cathepsin D is involved in the regulation of transglutaminase 1 and epidermal differentiation. J. Cell Sci. 117: 2295–2307
Guicciardi ME, Deussing J, Miyoshi H, Bronk SF, Svingen PA, Peters C, Kaufmann SH and Gores GJ (2000) Cathepsin B contributes to TNF-alpha-mediated hepatocyte apoptosis by promoting mitochondrial release of cytochrome c. J. Clin. Invest. 106: 1127–1137
Roth W, Deussing J, Botchkarev VA, Pauly-Evers M, Saftig P, Hafner A, Schmidt P, Schmahl W, Scherer J, Anton-Lamprecht I, Von Figura K, Paus R and Peters C (2000) Cathepsin L deficiency as molecular defect of furless: hyperproliferation of keratinocytes and pertubation of hair follicle cycling. FASEB J. 14: 2075–2086
Toomes C, James J, Wood AJ, Wu CL, McCormick D, Lench N, Hewitt C, Moynihan L, Roberts E, Woods CG, Markham A, Wong M, Widmer R, Ghaffar KA, Pemberton M, Hussein IR, Temtamy SA, Davies R, Read AP, Sloan P, Dixon MJ and Thakker NS (1999) Loss-of-function mutations in the cathepsin C gene result in periodontal disease and palmoplantar keratosis. Nat. Genet. 23: 421–424
Bernard D, Mehul B, Thomas-Collignon A, Simonetti L, Remy V, Bernard MA and Schmidt R (2003) Analysis of proteins with caseinolytic activity in a human stratum corneum extract revealed a yet unidentified cysteine protease and identified the so-called ‘stratum corneum thiol protease’ as cathepsin l2. J. Invest. Dermatol. 120: 592–600
Mathiasen IS, Sergeev IN, Bastholm L, Elling F, Norman AW and Jaattela M (2002) Calcium and calpain as key mediators of apoptosis-like death induced by vitamin D compounds in breast cancer cells. J. Biol. Chem. 277: 30738–30745
Witkowski JM, Zmuda-Trzebiatowska E, Swiercz JM, Cichorek M, Ciepluch H, Lewandowski K, Bryl E and Hellmann A (2002) Modulation of the activity of calcium-activated neutral proteases (calpains) in chronic lymphocytic leukemia (B-CLL) cells. Blood 100: 1802–1809
Reimertz C, Kogel D, Lankiewicz S, Poppe M and Prehn JH (2001) Ca(2+)-induced inhibition of apoptosis in human SH-SY5Y neuroblastoma cells: degradation of apoptotic protease activating factor-1 (APAF-1). J. Neurochem. 78: 1256–1266
Liu X, Van Vleet T and Schnellmann RG (2004) The role of calpain in oncotic cell death. Annu. Rev. Pharmacol. Toxicol. 44: 349–370
Wang KK (2000) Calpain and caspase: can you tell the difference? Trends Neurosci. 23: 20–26
Pariat M, Carillo S, Molinari M, Salvat C, Debussche L, Bracco L, Milner J and Piechaczyk M (1997) Proteolysis by calpains: a possible contribution to degradation of p53. Mol. Cell. Biol. 17: 2806–2815
Bizat N, Hermel JM, Humbert S, Jacquard C, Creminon C, Escartin C, Saudou F, Krajewski S, Hantraye P and Brouillet E (2003) In vivo calpain/caspase cross-talk during 3-nitropropionic acid-induced striatal degeneration: implication of a calpain-mediated cleavage of active caspase-3. J. Biol. Chem. 278: 43245–43253
Nakagawa T and Yuan J (2000) Cross-talk between two cysteine protease families. Activation of caspase-12 by calpain in apoptosis. J. Cell Biol. 150: 887–894
Chua BT, Guo K and Li P (2000) Direct cleavage by the calcium-activated protease calpain can lead to inactivation of caspases. J. Biol. Chem. 275: 5131–5135
Wang KK, Posmantur R, Nadimpalli R, Nath R, Mohan P, Nixon RA, Talanian RV, Keegan M, Herzog L and Allen H (1998) Caspase-mediated fragmentation of calpain inhibitor protein calpastatin during apoptosis. Arch. Biochem. Biophys. 356: 187–196
Neumar RW, Xu YA, Gada H, Guttmann RP and Siman R (2003) Cross-talk between calpain and caspase proteolytic systems during neuronal apoptosis. J. Biol. Chem. 278: 14162–14167
Miyachi Y, Yoshimura N, Suzuki S, Hamakubo T, Kannagi R, Imamura S and Murachi T (1986) Biochemical demonstration and immunohistochemical localization of calpain in human skin. J. Invest. Dermatol. 86: 346–349
Kim SY and Bae CD (1998) Calpain inhibitors reduce the cornified cell envelope formation by inhibiting proteolytic processing of transglutaminase 1. Exp. Mol. Med. 30: 257–262
Yamazaki M, Ishidoh K, Suga Y, Saido TC, Kawashima S, Suzuki K, Kominami E and Ogawa H (1997) Cytoplasmic processing of human profilaggrin by active mu-calpain. Biochem. Biophys. Res. Commun. 235: 652–656
Arthur JS, Elce JS, Hegadorn C, Williams K and Greer PA (2000) Disruption of the murine calpain small subunit gene, Capn4: calpain is essential for embryonic development but not for cell growth and division. Mol. Cell. Biol. 20: 4474–4481
Azam M, Andrabi SS, Sahr KE, Kamath L, Kuliopulos A and Chishti AH (2001) Disruption of the mouse mu-calpain gene reveals an essential role in platelet function. Mol. Cell. Biol. 21: 2213–2220
Kuwana T and Newmeyer DD (2003) Bcl-2-family proteins and the role of mitochondria in apoptosis. Curr. Opin. Cell Biol. 15: 691–699
Lu QL, Poulsom R, Wong L and Hanby AM (1993) Bcl-2 expression in adult and embryonic non-haematopoietic tissues. J. Pathol. 169: 431–437
Krajewski S, Krajewska M, Shabaik A, Wang HG, Irie S, Fong L and Reed JC (1994) Immunohistochemical analysis of in vivo patterns of Bcl-X expression. Cancer Res. 54: 5501–5507
Krajewski S, Krajewska M and Reed JC (1996) Immunohistochemical analysis of in vivo patterns of Bak expression, a proapoptotic member of the Bcl-2 protein family. Cancer Res. 56: 2849–2855
Droin NM and Green DR (2004) Role of Bcl-2 family members in immunity and disease. Biochim. Biophys. Acta 1644: 179–188
Veis DJ, Sorenson CM, Shutter JR and Korsmeyer SJ (1993) Bcl-2-deficient mice demonstrate fulminant lymphoid apoptosis, polycystic kidneys, and hypopigmented hair. Cell 75: 229–240
Muller-Rover S, Rossiter H, Paus R, Handjiski B, Peters EM, Murphy JE, Mecklenburg L and Kupper TS (2000) Overexpression of Bcl-2 protects from ultraviolet B-induced apoptosis but promotes hair follicle regression and chemotherapy-induced alopecia. Am. J. Pathol. 156: 1395–1405
Pena JC, Fuchs E and Thompson CB (1997) Bcl-x expression influences keratinocyte cell survival but not terminal differentiation. Cell Growth Differ. 8: 619–629
Grether-Beck S, Felsner I, Brenden H and Krutmann J (2003) Mitochondrial cytochrome c release mediates ceramide-induced activator protein 2 activation and gene expression in keratinocytes. J. Biol. Chem. 278: 47498–47507
Huang L, Mivechi NF and Moskophidis D (2001) Insights into regulation and function of the major stress-induced hsp70 molecular chaperone in vivo: analysis of mice with targeted gene disruption of the hsp70 or hsp70.3 gene. Mol. Cell. Biol. 21: 8575–8591
Laplante AF, Moulin V, Auger FA, Landry J, Li H, Morrow G, Tanguay RM and Germain L (1998) Expression of heat shock proteins in mouse skin during wound healing. J. Histochem. Cytochem. 46: 1291–1301
Pandey P, Saleh A, Nakazawa A, Kumar S, Srinivasula SM, Kumar V, Weichselbaum R, Nalin C, Alnemri ES, Kufe D and Kharbanda S (2000) Negative regulation of cytochrome c-mediated oligomerization of Apaf-1 and activation of procaspase-9 by heat shock protein 90. EMBO J. 19: 4310–4322
Beere HM, Wolf BB, Cain K, Mosser DD, Mahboubi A, Kuwana T, Tailor P, Morimoto RI, Cohen GM and Green DR (2000) Heat-shock protein 70 inhibits apoptosis by preventing recruitment of procaspase-9 to the Apaf-1 apoptosome. Nat. Cell Biol. 2: 469–475
Ravagnan L, Gurbuxani S, Susin SA, Maisse C, Daugas E, Zamzami N, Mak T, Jaattela M, Penninger JM, Garrido C and Kroemer G (2001) Heat-shock protein 70 antagonizes apoptosis-inducing factor. Nat. Cell Biol. 3: 839–843
Park KC, Kim DS, Choi HO, Kim KH, Chung JH, Eun HC, Lee JS and Seo JS (2000) Overexpression of HSP70 prevents ultraviolet B-induced apoptosis of a human melanoma cell line. Arch. Dermatol. Res. 292: 482–487
Kwon SB, Young C, Kim DS, Choi HO, Kim KH, Chung JH, Eun HC, Park KC, Oh CK and Seo JS (2002) Impaired repair ability of hsp70.1 KO mouse after UVB irradiation. J. Dermatol. Sci. 28: 144–151
Candi E, Schmidt R and Melino G (2005) The cornified envelope: a model of cell death in the skin. Nat. Rev. Mol. Cell. Biol. 6: 328–340
Chakravarty R, Rong XH and Rice RH (1990) Phorbol ester-stimulated phosphorylation of keratinocyte transglutaminase in the membrane anchorage region. BIOCHEM J. 271: 25–30
Russell LJ, DiGiovanna JJ, Rogers GR, Steinert PM, Hashem N, Compton JG and Bale SJ (1995) Mutations in the gene for transglutaminase 1 in autosomal recessive lamellar ichthyosis. Nat. Genet. 9: 279–283
Matsuki M, Yamashita F, Ishida-Yamamoto A, Yamada K, Kinoshita C, Fushiki S, Ueda E, Morishima Y, Tabata K, Yasuno H, Hashida M, Iizuka H, Ikawa M, Okabe M, Kondoh G, Kinoshita T, Takeda J and Yamanishi K (1998) Defective stratum corneum and early neonatal death in mice lacking the gene for transglutaminase 1 (keratinocyte transglutaminase). Proc. Natl. Acad. Sci. USA 95: 1044–1049
De Laurenzi V and Melino G (2001) Gene disruption of tissue transglutaminase. Mol. Cell. Biol. 21: 148–155
Haroon ZA, Lai TS, Hettasch JM, Lindberg RA, Dewhirst MW and Greenberg CS (1999) Tissue transglutaminase is expressed as a host response to tumor invasion and inhibits tumor growth. Lab. Invest. 79: 1679–1686
Kim HC, Lewis MS, Gorman JJ, Park SC, Girard JE, Folk JE and Chung SI (1990) Protransglutaminase E from guinea pig skin. Isolation and partial characterization. J. Biol. Chem. 265: 21971–21978
Candi E, Oddi S, Paradisi A, Terrinoni A, Ranalli M, Teofoli P, Citro G, Scarpato S, Puddu P and Melino G (2002) Expression of transglutaminase 5 in normal and pathologic human epidermis. J. Invest. Dermatol. 119: 670–677
Kunisaki Y, Masuko S, Noda M, Inayoshi A, Sanui T, Harada M, Sasazuki T and Fukui Y (2004) Defective fetal liver erythropoiesis and T lymphopoiesis in mice lacking the phosphatidylserine receptor. Blood 103: 3362–3364
Wu YC and Horvitz HR (1998) The C. elegans cell corpse engulfment gene ced-7 encodes a protein similar to ABC transporters. Cell 93: 951–960
Luciani MF and Chimini G (1996) The ATP binding cassette transporter ABC1, is required for the engulfment of corpses generated by apoptotic cell death. EMBO J. 15: 226–235
Doolin EJ, Strande LF, Chen MK, Kain MS and Hewitt CW (1999) The effect of leukocyte infiltration on apoptosis in an in vitro thermal injury bioartificial living skin equivalent model. J. Burn Care Rehabil. 20: 374–376
Simon M, Jonca N, Guerrin M, Haftek M, Bernard D, Caubet C, Egelrud T, Schmidt R and Serre G (2001) Refined characterization of corneodesmosin proteolysis during terminal differentiation of human epidermis and its relationship to desquamation. J. Biol. Chem. 276: 20292–20299
van Bokhoven H and McKeon F (2002) Mutations in the p53 homolog p63: allele-specific developmental syndromes in humans. Trends Mol. Med. 8: 133–139
Lamkanfi M, Declercq W, Kalai M, Saelens X and Vandenabeele P (2002) The caspase family In Caspases: Their Role in Cell Death and Cell Survival Los M, Walczak H (eds) (Georgetown: Landes Bioscience, Kluwer Academic Press)
Mills AA, Zheng B, Wang XJ, Vogel H, Roop DR and Bradley A (1999) p63 is a p53 homologue required for limb and epidermal morphogenesis. Nature 398: 708–713
Koster MI, Kim S, Mills AA, DeMayo FJ and Roop DR (2004) p63 is the molecular switch for initiation of an epithelial stratification program. Genes Dev. 18: 126–131
Acknowledgements
We apologize to the many scientists who made major contributions to this field, but have not been cited due to space limitations. This work is supported in part by the Interuniversitaire Attractiepolen (IUAP-V), the Fonds voor Wetenschappelijk Onderzoek-Vlaanderen (Grants 31.5189.00, 3G.0006.01 and G.0133.05) and the EC-RTD (grant QLRT-CT-1999-00739), the UGent-co-financing EU project (011C0300) and GOA project (12050502). G Denecker is supported by the Fonds voor Wetenschappelijk Onderzoek Vlaanderen and P Ovaere by a grant from the IWT. We thank A Bredan for editorial help and W Drijvers for art work.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Edited by G Melino
Rights and permissions
About this article
Cite this article
Lippens, S., Denecker, G., Ovaere, P. et al. Death penalty for keratinocytes: apoptosis versus cornification. Cell Death Differ 12 (Suppl 2), 1497–1508 (2005). https://doi.org/10.1038/sj.cdd.4401722
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401722
Keywords
This article is cited by
-
Proteomics reveals that quinoa bioester promotes replenishing effects in epidermal tissue
Scientific Reports (2020)
-
p63 cooperates with CTCF to modulate chromatin architecture in skin keratinocytes
Epigenetics & Chromatin (2019)
-
Cornification of nail keratinocytes requires autophagy for bulk degradation of intracellular proteins while sparing components of the cytoskeleton
Apoptosis (2019)
-
Transient elevation of cytoplasmic calcium ion concentration at a single cell level precedes morphological changes of epidermal keratinocytes during cornification
Scientific Reports (2018)
-
Phospholipase Cδ1 regulates p38 MAPK activity and skin barrier integrity
Cell Death & Differentiation (2017)