Abstract
Study design:
Measurement of haemodynamic responses, cutaneous blood flow and sweat release during penile vibratory stimulation (PVS) in spinal cord-injured men.
Objective:
To assess the validity of using markers of sympathetic activity (cutaneous blood flow and sweat release) as a measure of incipient autonomic dysreflexia during PVS in spinal cord-injured men.
Setting:
Prince of Wales Medical Research Institute, Australia.
Subjects:
Ten spinal cord-injured men with injuries ranging from C3 to T6.
Methods:
Continuous arterial pressure, intermittent auscultation, heart rate (HR), respiration, cutaneous blood flow and sweat release from both finger and toe were recorded during PVS.
Results:
Vibration of the penis caused immediate cutaneous vasoconstriction, but negligible sweat release, in the hands and feet of the quadriplegics and the feet of the paraplegics. Systolic blood pressure (BP) increased by up to 90 mm Hg, and a compensatory vagal bradycardia was observed in five of the six quadriplegics and two of the four paraplegic subjects.
Conclusion:
Given that there was—in general—an inverse relationship between BP and skin blood flow, we conclude that continuous measurements of skin blood flow above and below the lesion can provide important information on the state of the sympathetic nervous system and early identification of reflexly evoked increases in sympathetic vasoconstrictor drive, below a spinal lesion. Coupled with a decrease in HR, this cutaneous vasoconstriction infers an increased BP.
Similar content being viewed by others
Introduction
Although spinal cord injury (SCI) can cause devastating changes in the somatic nervous system, relatively little is known about changes to the sympathetic nervous system. As the sympathetic supply to the viscera and blood vessels is derived from the thoracolumbar segments of the spinal cord, interruption of descending sympathetic pathways can cause partial or complete loss of sympathetic control below the lesion. With high lesions, the loss of vasoconstrictor drive results in a low resting blood pressure (BP) and orthostatic hypotension;1 control of cutaneous blood flow and hence thermoregulatory control are also compromised. However, as segmental circuitry is intact, visceral or somatic stimuli originating below the lesion can cause reflex activation of vasoconstrictor neurones and a consequent increase in BP.2, 3 This condition, known as autonomic dysreflexia, is considered a medical emergency, as arterial pressure can rise so suddenly and remain at dangerously elevated levels that life-threatening complications can occur.1, 4 It is common for midthoracic lesions and above,5 that is above the level of sympathetic outflow to the splanchnic circulation, where many vascular beds may have lost central control. The only means available to offset the hypertension is through vagal slowing of the heart. Although autonomic dysreflexia has been reported in low thoracic (T8–T10) lesions,6 usually enough vascular beds are under supraspinal control that adequate vasodilatation can be brought about through the normal baroreceptor-mediated withdrawal of vasoconstrictor drive.1
Autonomic dysreflexia is defined as an increase in systolic BP greater than 20 mm Hg above baseline, combined with one or more subjective or objective symptoms.2 The symptoms of autonomic dysreflexia including a throbbing headache, tingling in the head, nasal congestion, sweating and flushing above the lesion, and pupillary dilation, prompt medical staff to measure BP and locate the source of sensory irritation. However, there is no correlation between the magnitude of the hypertensive response and headache.1 For scientific purposes, the definition of autonomic dysreflexia includes a BP increase combined with a visualized vasoconstriction below the lesion.2 Autonomic dysreflexia is a potentially dangerous side effect of penile vibratory stimulation (PVS), which is the preferred method of obtaining sperm for fertility assessment and fertilization purposes in SCI men.7, 8, 9 As ejaculation during sexual intercourse cannot be achieved by 90% of men with SCI,10 PVS is a medically necessary procedure to facilitate ejaculation in these men.9 Typically, BP and heart rate (HR) are monitored intermittently during the procedure, with the patient being monitored for signs of autonomic dysreflexia and asked to report the onset of headache. However, as clinical indicators do not always correlate with the magnitude of BP rise, we wanted to investigate whether cutaneous vasoconstriction and sweat release were a more robust measure of incipient dysreflexia. We recorded BP using radial arterial tonometry and intermittent auscultation, and two markers of cutaneous sympathetic activity—skin blood flow and sweat release—in men who had suffered a defined SCI.
Methods
Ten male volunteers, who had sustained SCIs between 4 months and 5 years previously, were studied. Six subjects were quadriplegic (C3–C7) and four were paraplegic (T3–T6). Injuries were classified as complete or incomplete according to the American Spinal Injury Association (ASIA) Impairment Scale (AIS),11 with injuries ranging from AIS A to D. Subjects with unstable BP at rest, or those taking antihypertensive medications or with ongoing infection or other comorbidity, were excluded. No subject suffered from diabetes or any other neuropathies that may have affected the vasomotor and sudomotor responses.
Procedure
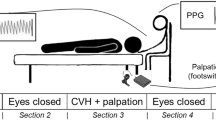
Subjects were studied in a semirecumbent position at a comfortable ambient temperature. Care was taken to ensure a calm and quiet environment to minimize spontaneous arousal responses. BP was recorded continuously using radial arterial tonometry (CBM-7000; Colin Corp., Komaki, Japan) and intermittently with manual sphygmomanometry. Increases in cutaneous sympathetic nerve activity were recorded indirectly as reductions in relative skin blood volume—measured from photoelectric plethysmographs on the pads of the index finger and big toe (Pulse Plethysmograph; ADInstruments, Sydney, Australia)—and sweat release, measured from changes in electrical conductance across the skin of the hand and foot (GSR Amplifier; ADInstruments). Respiration was recorded using a strain gauge transducer wrapped around the chest (Pneumotrace; Morro Bay, CA, USA).
After resting BP had been monitored for 10 min, a 100-Hz, 2.5-mm amplitude vibration was applied to the penis for 2–5 min (Ferticare Personal Vibrator, Albertslund, Denmark). The number of vibration trials varied between individuals. Vibration was interrupted if the subject ejaculated or autonomic dysreflexia occurred.
Vibration was monitored using a piezoelectric transducer applied to the vibrator. All parameters including intermittent manual sphygmomanometry measurements were stored on computer using a computer-based data acquisition and analysis system (PowerLab 16SP, Chart 5 software; ADInstruments).
Analysis
Relative changes in skin blood volume were measured from the pulse amplitude, which was taken from the raw plethysmography trace that had been high-pass filtered (1 Hz). HR was calculated from this derived channel. For each subject, an average baseline was calculated from a 10 s period before the vibration and the peak response measured as the greatest fall in amplitude. The paired t-test was used to show statistical significance between baseline values and peak responses. A probability level less than 5% (one-tailed) was regarded as significant.
Statement of ethics
We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research, with the study receiving ethical approval from the Human Research Ethics Committees of The University of New South Wales and Prince of Wales Hospital. All subjects provided written or verbal (witnessed) informed consent to the procedures.
Results
Vibration of the penis evoked increases in BP in 9 of 10 subjects, though in one of these subjects diastolic pressure increased by only 5 mm Hg. As spontaneous and evoked movements of the subject often caused artefacts in the continuous (tonometric) BP record, we shall report data obtained from intermittent sphygmomanometric readings acquired at rest and during vibration. The mean duration of the vibration was 208±27 s.
Individual increases in systolic and diastolic pressures are given in Table 1. Systolic pressure increased by 18–90 mm Hg (15–113%) in the six quadriplegics and, in two of the four paraplegics, by 15–25 mm Hg (13–23%). With the exception of one quadriplegic, who developed tachycardia during the vibration (HR increased by 24 b.p.m., a 36% increase), a compensatory bradycardia occurred in all quadriplegics and in two of the paraplegics. One paraplegic subject who showed no overt increase in BP during the vibration did develop bradycardia. BP had returned to baseline levels within 6–22 min. The peak increases in systolic and diastolic pressure were significantly different from baseline (P=0.0003 and P=0.002, respectively). Cutaneous vasoconstriction in the toes was apparent for all subjects; the mean fall in cutaneous perfusion was 70±3% (P<0.0001) and the mean duration 226±37 s. Cutaneous vasoconstriction was measured in the hand in four quadriplegics: the mean fall in perfusion and duration of the vasoconstriction were 81±2% (P=0.001) and 218±55 s, respectively.
Blood pressure responses from continuous (tonometric) BP recording could only be obtained in four subjects due to spontaneous and evoked movements causing artefacts and loss of signal. Peak systolic pressure in these four subjects increased by 13–85 mm Hg (9–72%), whereas diastolic pressure increased by 18–51 mm Hg (18–98%).
Characteristic features of impending ejaculation, such as abdominal spasms and tightness, occurred in all subjects, but emission occurred only in four. For the successful vibration trials, it took 67–344 s for the emission to occur.
Experimental records from one subject, who sustained a complete C5 injury 4 months previously, are illustrated in Figure 1. This represents the second of four unsuccessful attempts to induce ejaculation and is chosen because the BP records (radial arterial tonometry) are largely free from movement artefacts. The subject had no sensation below nipple line but knew when the vibrator was going to be applied. It can be seen that as soon as the vibrator made contact with the penis a decrease in blood volume in the fingers, and to some extent in the toes, occurred. Although this was associated with a deep breath, the reduction in pulsatile blood volume reflects a sympathetically mediated vasoconstriction of cutaneous blood vessels; sweat release—another marker of cutaneous sympathetic nerve activity—also occurred concurrently. Vibration of the penis caused an immediate increase in arterial pressure—systolic pressure increasing by 26–146 mm Hg and diastolic pressure by 15–86 mm Hg. This increase in arterial pressure, which was maintained for the 5 min of vibration, evoked a sustained baroreflex-mediated bradycardia; HR fell by 23–49 b.p.m. The reduction in cutaneous blood volume waned towards the end of the stimulation but a pronounced vasoconstriction in the finger occurred on terminating the vibration. This was associated with a transient increase in arterial pressure. The subject reported no signs of dysreflexia.
Heart rate, blood pressure (radial artery tonometry), skin blood flow (IR plethysmography, finger and toe) and sweat release (finger and toe) responses during vibration of the penis in a C5 AIS A spinal subject. The period of stimulation can be seen at the bottom of the figure, which was monitored using a piezoelectric transducer applied to the vibrator.
Records from four consecutive periods of stimulation in the same subject as illustrated in Figure 1 are shown in Figure 2. It can be seen that the magnitude of the haemodynamic responses was greater with subsequent stimuli. Vibration was applied for only 50 s in the fourth period of stimulation, but systolic pressure increased by 40 to ∼150 mm Hg and did not return to control levels for some 4 min following termination of the vibration. This build-up effect has been seen in our earlier study;12 however, the interval between each stimulus in that study was approximately 30 s to 1 min. Despite the continued hypertension, the subject reported only ‘tingling in the head.’
Heart rate and blood pressure responses during four consecutive periods of penile vibration in the same C5 AIS A subject as illustrated in Figure 1. The first three periods of stimulation include 20 s of baseline and the first 90 s of the vibration. The second period commenced 12 min following the end of the first period, the third commenced 19 min after the end of the second period. The fourth period of stimulation, which followed the third period by 10 min, lasted for only 50 s and includes the entire vibratory period with a 20 s baseline period. The black bar represents the period of vibration; the asterisks indicate movement artefacts.
Peak BP responses and averaged data from HR and cutaneous vasoconstriction for all subjects are shown in Table 1.
Discussion
We have shown that PVS causes a robust cutaneous vasoconstriction below the lesion: in the majority of subjects, this reflected the increase in BP and compensatory reduction in HR. Cutaneous vasoconstriction below the lesion was seen in all subjects and occurred irrespective of whether the vibration caused ejaculation or not. However, sweat release was inconsistent, with 5 of 10 subjects having sudomotor responses in either the finger or the toe but not for all their individual trials of vibration. Therefore, compared with sudomotor responses, vasomotor responses were more reliable in detecting cutaneous sympathetic activity. Moreover, the information that can be obtained from vasomotor responses is often more comprehensive than that can be obtained from sudomotor responses.
It has been found that in able-bodied men, there is a modest increase in BP and HR during genital stimulation, reaching its peak at ejaculation and quickly returning to baseline.13, 14 However, it has been shown in our study and many others that SCI men with lesions above T6 can suffer from autonomic dysreflexia during genital stimulation. One subject had tachycardia and a small increase in systolic pressure during PVS: this subject was incomplete (C3/C4 AIS D), so it may be that sympathetic pathways to his heart were largely intact. Tachycardia during PVS has previously been reported in SCI men,15 with tachycardia in numerous autonomic dysreflexia cases also being found.4
Recent times have shown considerable advances in rehabilitation medicine16 as well as in assisted reproductive techniques for individuals with sexual dysfunction.17 As the majority of men who suffer from an SCI are in their reproductive years, procreation is of major concern to them and their partners. Therefore, techniques such as PVS and electroejaculation offer a significant advantage to these individuals. However, as an exaggerated increase in BP can be an undesirable side effect of both PVS and electroejaculation, the need to carefully monitor BP during these techniques is paramount.
Earlier studies7, 9, 18, 19 have shown that there is a significant elevation of BP in SCI men undergoing PVS. However, there appear to be no studies that have correlated cutaneous vasoconstriction with BP during this procedure. Given the associated risks that accompany these large increases in BP and as continuous BP monitoring is not always feasible during the procedure, continuous monitoring of skin blood flow below the lesion may be a more suitable parameter to indirectly monitor sympathetic nerve activity. Using electrical stimuli applied to the abdominal wall in SCI subjects, we recently demonstrated the utility of using skin perfusion as an indicator of the state of cutaneous vasoconstrictor drive, and indirectly, of muscle (and splanchnic) vasoconstrictor drive.12
Limitations
By recording continuous BP, through radial arterial tonometry, we believed at the outset that we would have a robust measure of the BP increase induced by PVS. However, because radial arterial tonometry is sensitive to movement of the wrist, which often occurred during spasms or overt body movements during the vibration, we usually lost our continuous BP signal. Therefore, the majority of BP measurements reported in this study were obtained by intermittent manual sphygmomanometry. This has its own limitations: the time taken for inflation and deflation means that the peak pressure response may have occurred before the manual measurement is obtained. However, the continuous measurement of BP does allow us to examine the initial time course before loss of the continuous BP signal.
We propose that cutaneous vasoconstriction below the lesion can be used as an indicator of sympathetic vasoconstrictor activity and infer what is happening in other vascular beds, that is muscle and splanchnic. We do not propose that there is a linear relationship between the magnitude of the cutaneous vasoconstriction and the magnitude of the BP increase. Moreover, there may be differences in the vascular responsiveness to noradrenaline in the cutaneous, skeletal muscle and splanchnic beds. Nevertheless, we postulate that cutaneous vasoconstriction below lesion indicates general vasoconstriction as the result of a viscerosympathetic or (in the present case) somatosympathetic reflex, which then leads to a pressor response. The magnitude of the increase in BP is dependent on the volume of blood vessels constricted, which we cannot determine simply from the measurement of blood flow in a single toe.
Importantly, as we are measuring only cutaneous vasoconstriction from one toe, this does not represent the entire vasculature below the lesion. However, we do know from microneurographic studies that there is coactivation of cutaneous and muscle vasoconstrictor neurones following stimulation below lesion in subjects with SCI.3 Although constriction of cutaneous (capacitance) vessels will result in the displacement of blood to active circulation, there is no doubt that the increase in BP is due to the activation of muscle vasoconstrictor neurones and, most likely, splanchnic vasoconstrictor neurones, through a spinal viscerosympathetic reflex. Indeed, the magnitude of the pressor response implies the constriction of many arterioles and, given that the splanchnic outflow originates below T6, it is highly likely that constriction within the splanchnic vascular bed contributes to the increase in BP.2
Conclusion
As a patient's subjective reports may not provide an adequate measure of incipient autonomic dysreflexia, we need a more sensitive indicator of the increases in BP. Given that there was—in general—an inverse relationship between BP and skin blood flow, we conclude that continuous measurements of skin blood flow above and below the lesion can provide important information on the state of the sympathetic nervous system and early identification of reflexly evoked increases in sympathetic vasoconstrictor drive below a spinal lesion. Coupled with a decrease in HR, this cutaneous vasoconstriction infers an increased BP. However, at this stage, we have simply provided the physiological substrate for the utility of measuring cutaneous perfusion below a spinal lesion; until such a device has been developed and validated clinically, our suggestion remains conjecture. Nevertheless, we do believe that a fall in cutaneous blood flow, coupled with a fall in HR, does infer an increase in BP—brought about by reflexly evoked increases in vasoconstrictor (muscle, splanchnic and cutaneous) drive.
References
Teasell RW, Arnold JM, Krassioukov A, Delaney GA . Cardiovascular consequences of loss of supraspinal control of the sympathetic nervous system after spinal cord injury. Arch Phys Med Rehabil 2000; 81: 506–516.
Karlsson AK . Autonomic dysreflexia. Spinal Cord 1999; 37: 383–391.
Stjernberg L, Blumberg H, Wallin GB . Sympathetic activity in man after spinal cord injury. Outflow to muscle below the lesion. Brain 1986; 109: 695–715.
Kewalramani LS . Autonomic dysreflexia in traumatic myelopathy. Am J Phys Med 1980; 59: 1–21.
Guttmann L, Whitteridge D . Effects of bladder distention on autonomic mechanism after spinal cord injuries. Brain 1947; 70: 361–404.
Gimovski ML, Ojeda A, Ozaki R, Zerne S . Management of autonomic hyperreflexia associated with a low thoracic spinal cord lesion. Am J Obstet Gynecol 1985; 153: 223–224.
Szasz G, Carpenter C . Clinical observations in vibratory stimulation of the penis of men with spinal cord injury. Arch Sex Behav 1989; 18: 461–474.
Brackett NL, Ferrell SM, Aballa TC, Amador MJ, Padron OF, Sonksen J et al. An analysis of 653 trials of penile vibratory stimulation in men with spinal cord injury. J Urol 1998; 159: 1931–1934.
Brackett NL . Semen retrieval by penile vibratory stimulation in men with spinal cord injury. Hum Reprod Update 1999; 5: 216–222.
Bors E, Comarr AE . Neurological disturbances of sexual function with special reference to 529 patients with spinal cord injury. Urol Surv 1960; 10: 191–222.
Marino RJ, Barros T, Biering-Sorensen F, Burns SP, Donovan WH, Graves DE et al. International standards for neurological classification of spinal cord injury. J Spinal Cord Med 2003; 26 (Suppl 1): S50–S56.
Brown R, Engel S, Elam M, Wallin G, Macefield V . Assessing the integrity of sympathetic pathways following spinal cord injury. Auton Neurosci Basic Clin 2007; 134: 61–68.
Nemec ED, Mansfield L, Kennedy JW . Heart rate and blood pressure responses during sexual activity in normal males. Am Heart J 1976; 92: 274–277.
Kruger T, Exton MS, Pawlak C, von zur Muhlen A, Hartmann U, Schedlowski M . Neuroendocrine and cardiovascular response to sexual arousal and orgasm in men. Psychoneuroendocrinology 1998; 23: 401–411.
Claydon VE, Elliott SL, Sheel AW, Krassioukov A . Cardiovascular responses to vibrostimulation for sperm retrieval in men with spinal cord injury. J Spinal Cord Med 2006; 29: 207–216.
Devivo MJ, Stover SL . Long term survival and causes of death. In: Stover SL, Delisa JA, Whiteneck GG (eds). Spinal Cord Injury: Clinical Outcomes from the Model Systems. Aspen Publishers Inc.: Gaithersburg, Maryland, 1995, pp 289–316.
Sønksen J, Ohl DA . Penile vibratory stimulation and electroejaculation in the treatment of ejaculatory dysfunction. Int J Androl 2002; 25: 324–332.
Sheel W, Krassioukov A, Inglis T, Elliott L . Autonomic dysreflexia during sperm retrieval in spinal cord injury: influence of lesion level and sildenafil citrate. J Appl Physiol 2005; 99: 53–58.
Comarr AE . Sexuality and fertility among spinal cord and/or cauda equina injuries. J Am Paraplegia Soc 1985; 8: 67–75.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brown, R., Stolzenhein, G., Engel, S. et al. Cutaneous vasoconstriction as a measure of incipient autonomic dysreflexia during penile vibratory stimulation in spinal cord injury. Spinal Cord 47, 538–544 (2009). https://doi.org/10.1038/sc.2008.158
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2008.158
Keywords
This article is cited by
-
Autonomic dysreflexia in urological practice: pathophysiology, prevention and treatment considerations
World Journal of Urology (2024)
-
Management of ejaculatory disorders in infertile men
Asian Journal of Andrology (2012)