Abstract
The rail industry in Australia screens workers for probable obstructive sleep apnea (OSA) due to known safety risks. However, existing criteria to trigger screening only identify a small proportion of workers with OSA. The current study sought to examine the relationship between OSA risk and rail incidents in real-world data from Australian train drivers, and conducted a proof of concept analysis to determine whether more conservative screening criteria are justified. Health assessment (2016–2018) and subsequent rail incident data (2016–2020) were collected from two passenger rail service providers. Predictors included OSA status (confirmed no OSA with a sleep study, controlled OSA, unknown OSA [no recorded sleep assessment data] and confirmed OSA with no indication of treatment); OSA risk according to the current Standard, and OSA risk according to more conservative clinical markers (BMI threshold and cardiometabolic burden). Coded rail safety incidents involving the train driver were included. Data were analysed using zero-inflated negative binomial models to account for over-dispersion with high 0 counts, and rail safety incidents are reported using Incidence Risk Ratios (IRRs). A total of 751 train drivers, typically middle-aged, overweight to obese and mostly men, were included in analyses. There were 43 (5.7%) drivers with confirmed OSA, 62 (8.2%) with controlled OSA, 13 (1.7%) with confirmed no OSA and 633 (84.4%) drivers with unknown OSA. Of the 633 train drivers with unknown OSA status, 21 (3.3%) met ‘at risk’ criteria for OSA according to the Standard, and incidents were 61% greater (IRR: 1.61, 95% Confidence Interval (CI) 1.02–2.56) in the years following their health assessment compared to drivers who did not meet ‘at risk’ criteria. A more conservative OSA risk status using lower BMI threshold and cardiometabolic burden identified an additional 30 ‘at risk’ train drivers who had 46% greater incidents compared to drivers who did not meet risk criteria (IRR (95% CI) 1.46 (1.00–2.13)). Our more conservative OSA risk criteria identified more workers, with greater prospective incidents. These findings suggest that existing validated tools could be considered in future iterations of the Standard in order to more sensitively screen for OSA.
Similar content being viewed by others
Introduction
Obstructive sleep apnea (OSA) is a sleep breathing disorder characterised by intermittent narrowing and/or closure of the upper airway during sleep. In the transport sector, OSA is consistently associated with excessive daytime sleepiness, fatigue, and inattention1,2,3,4. In the rail industry, the cognitive deficits associated with OSA have been linked with significant safety incidents5,6,7,8.
In Australia, the need for standardised management of rail worker health became evident in 2003 following a passenger train derailment in Waterfall, New South Wales (NSW), that resulted in seven fatalities after the driver collapsed from a cardiac event at the controls9. A year later, the National Transport Commission (NTC) published the National Standard for Health Assessment of Rail Safety Workers (the Standard)10, requiring periodic assessments of individual worker health. Worker history includes medical conditions, sleepiness (Epworth Sleepiness Score11), AUDIT questionnaire of alcohol consumption12, K-10 questionnaire for psychological distress13, and smoking status. A history of involvement in accidents or near misses may be provided by the employer. Clinical examination within the Standard involves hearing, vision and musculoskeletal capacity testing, cardiovascular examination, and calculation of overall cardiac risk level based on age, sex, smoking status, blood pressure, fasting cholesterol and diabetic status. Specific to OSA, the Standard currently assesses OSA risk according to a combination of self-reported sleepiness, or work performance indicators of excessive sleepiness, and some clinical markers including body mass index (BMI), blood pressure, and diabetes status.
Since the Standard was introduced, research has sought to evaluate its application for health screening and clinical assessment14,15,16. A 2015 publication highlighted that OSA within the rail workforce was more prevalent than initially reported, with an increase from 2% in 2009, to 7% in 2012 after revised screening criteria were introduced in the 2012 revision of the Standard17. Yet, these rates are still markedly lower than the anticipated prevalence of OSA in this worker population given high rates in the general population18. A recent population-level study involving gold standard polysomnography estimated OSA prevalence (based on an apnea hypopnea index (AHI) of >15 or obstructive sleep apnea syndrome, AHI > 5 with excessive sleepiness) as high as 47% in middle-aged males, and 24% in middle-aged females18. Thus, the Standard itself still currently references OSA prevalence rates which are >50% lower than recently documented rates (see Fig. 1). This highlights a substantial, hidden burden of undetected OSA in the general population, including in safety critical workers.
In a recent retrospective study of the association between OSA severity and safety incidents occurrence, 44% of rail safety workers with confirmed OSA were found to have at least one incident in the 3 years prior to their health assessment8. Undiagnosed and untreated OSA also exposes rail workers to potential major physical and mental health problems. Moreover, the cognitive deficits associated with OSA (e.g., excessive daytime sleepiness, fatigue, and inattention) contribute to ‘operational’ incidents (e.g., failure to stop at a scheduled station, departing earlier than scheduled from the station) which are not safety-related, but still very costly to rail service providers all the same. Without accurately identifying OSA cases in train driver populations, it is not possible to fully elucidate the relationship with safety, nor to appropriately manage the risk.
In order to facilitate evidence-based decisions relating to OSA screening and management, this study used clinical health and rail incident data from train drivers in NSW to answer the overarching research question: what is the relationship between obstructive sleep apnea and prospective rail operational and safety incidents? The aims of the study were to:
-
(1)
Compare OSA ‘risk’ status from the Standard with confirmed OSA status to determine whether application of the Standard criteria accurately classifies workers;
-
(2)
investigate the association between ‘OSA risk’ as identified in the Standard with real-world rail safety and operational incidents (‘rail incidents’) in Australian train drivers; and to
-
(3)
determine whether a more conservative risk threshold for OSA using existing health record data is warranted based on associations with rail incidents following a health assessment.
Methods
Data were drawn from two passenger rail service providers in NSW, Australia. An a priori decision was made to consider health assessment data for all train drivers collected in the timeframe 2016–2018, irrespective of sleep study screening status. This decision was made due to the low prevalence rates of OSA in historic studies of rail safety workers, and to allow for analysis of ‘at risk’ but undiagnosed or unknown OSA status relative to subsequent incident data.
All incident data over the period 2016–2020 were provided for train drivers with a health assessment in this timeframe. When completing their health assessment, employees signed individual informed consent for their health data to be accessed for the purposes of audit or research. Data were deidentified after linkage to protect confidentiality of workers. Research ethics approval was provided by Central Queensland University (approval no. 0000023385), and Flinders University (project no. 5174), and all research was performed in accordance with relevant guidelines and regulations.
OSA status and risk
Three variables were considered as predictors for analysis.
OSA status by current gold standard measurement
OSA status was determined from an overnight polysomnographic sleep study during the health assessment for some participants. Others had existing diagnoses recorded in the health records. Train drivers were coded as either ‘confirmed no OSA’ (sleep study completed with no diagnosis of OSA), ‘controlled OSA’ (sleep study with diagnosis of OSA plus notes about treatment), ‘unknown OSA’ (train drivers with no recorded sleep study or notes indicative of diagnosis of OSA), and ‘confirmed’ OSA (train drivers with a diagnosis of OSA but no indication of treatment initiation in the 2016-2018 health assessment data).
OSA risk by the current version of the Standard
The second variable was OSA risk according to the Standard (section 18.6, ‘sleep disorders’)10. Train drivers were coded as ‘at risk’ according to the Standard if they had demonstrated sleepiness (ESS ≥ 16) or body mass index (BMI) >40, or BMI > 35 with comorbid type 2 diabetes or high blood pressure requiring medications for control.
OSA risk by conservative clinical markers
The final variable was OSA risk according to clinical markers. For the purpose of this variable, to be ‘at risk’ by BMI category, workers had to meet BMI threshold (≥37.5 kg/m2), and/or have a BMI > 35 with an indication of current cardiometabolic burden (e.g., type II diabetes19, high blood pressure requiring ≥ 1 medications20,21, systolic blood pressure ≥ 135 & diastolic blood pressure ≥ 85 and/or any heart diseases22). This more conservative criteria for OSA risk was selected given the associations with OSA in existing literature, and availability of clinical marker data in the cohort to demonstrate proof of concept.
Comparison between risk and Gold Standard polysomnography
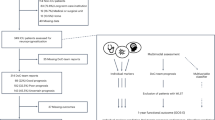
The classification of OSA risk by the current version of the standard (binary outcome, at risk/not at risk) was compared to OSA diagnosis according to polysomnography (OSA/no OSA) using a confusion matrix as depicted conceptually in Table 1. A true negative is a driver that screened negative according to the Standard criteria, and negative on a sleep study (a “confirmed no OSA”). A false positive is a driver that screened negative using the Standard, but a positive diagnosis using gold polysomnography. Furthermore, we define the misclassification of OSA risk according to the Standard by dividing the number of false positives by the total number of positive cases according to gold-standard polysomnography. For the purpose of this analysis, whether the OSA was controlled/treated is not taken into account, given that a driver would have had a to fulfill criteria in the first place to be subsequently treated. However, we also calculated the false positive probability/misclassification probability for controlled/not-controlled OSA separately. A similar analysis was conducted for OSA risk as defined using more conservative clinical markers instead of the Standard.
Operational and safety incidents
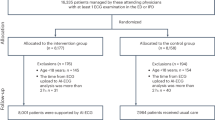
The primary outcome in the study was the number of significant operational and safety incidents per worker following a health assessment in the period 2016–2018 (see Fig. 2). Operational and safety incidents were extracted from the Incident Information Management System—a state-wide incident reporting/monitoring system accessed by a wide range of rail professional staff employed by rail service providers in NSW to report incidents. Incidents deemed to be significant enough for inclusion were based on a detailed taxonomy, developed by coding incidents using conventional content analysis23,24.
The resulting taxonomy (see Table 2) had 14 overall categories made up of 34 subcategories. Given the range of incident types within the Incident Information Management System, they were also coded as either ‘safety’ (incidents increasing safety risk and defined primarily by safety impacts) or ‘operational’ (incidents impacting scheduling and defined primarily by service impacts), recognising the dual key performance indicators shaping the rail system, but also the complexity of the relationship between them as they related to health (e.g., Failure to stop at a scheduled station is an operational incident, but can be caused by inattention and microsleeps, both of which are associated with OSA). The process for extraction of incidents including the total number of incidents is summarised in Fig. 2.
Additional health status and demographic data
Participant age, sex, hypertension status, heart disease status, diabetes status, ESS11 and K-10 scores13 were extracted from health records. Blood pressure values (systolic and diastolic) were taken from the cardiovascular examination, and qualitatively from relevant notes provided by clinicians during health assessments, including comments on OSA severity, metrics from sleep studies, and OSA treatment status.
Data analysis
Data were analysed in R Studio25, using the pscl package. Prospective count of incidents (i.e., operational and safety) were analysed using zero-inflated negative binomial models. This approach is appropriate when data are over-dispersed with high 0 counts, as is the case with safety critical incidents. This approach has been used previously in accident prediction models26. All incident data were adjusted for sex and reported as incidence risk ratios (IRRs). The database reflected all driver data available from two rail providers in the target window, and a retrospective power calculation was not conducted27.
Results
Workers included in the study
A total of 751 train drivers with health assessment data in the period 2016-2018 were included in analyses. Where workers had multiple assessments in the timeframe, the earliest assessment with sufficient data to calculate risk scores for OSA referral according to the Standard was included in analyses (Supplementary Figure 1 provides a summary of the number of assessments conducted per train driver in the health assessment window).
Table 3 shows the demographic and health characteristics of the sample. Included workers were typically middle-aged, with BMI scores placing them in the overweight or obese categories. Workers were predominantly male, typical of train driving cohorts in Australia28. Hypertension and diabetes were common in the sample, particularly in workers with OSA (both controlled OSA and confirmed OSA). Sleepiness scores did not differ across OSA categories, and overall scores were well below both the thresholds for identifying sleepiness according to the Standard10, and the typical ESS scores reported for middle-aged Australians in the general population18.
Aim 1: Compare OSA risk status from the Standard with confirmed OSA to determine whether application of the Standard criteria accurately classifies workers
The Standard relies on both self-reported and objective clinical risk factors to identify workers at risk of OSA. Figure 3 demonstrates available data from health assessments to classify workers as ‘at risk’ of OSA according to the Standard sleep disorder assessment trigger (p. 144 of the Standard10). Data were not consistently recorded or available in the current health assessment records to meet all self-reported indicators. As reported in Table 3, mean ESS scores were lower than required for a trigger of temporarily unfit for duty. Review of all 751 train drivers with available health assessment data indicated that no workers met the ≥16 ESS score, even amongst those with a confirmed OSA diagnosis.
Criteria for referral for a sleep study according to the 2017 National Standard for Health Assessment of Rail Safety Workers10. Note grey text indicates that subjective details were not consistently recorded or reported in the health assessment data provided. BMI, body mass index.
Comparison of classification of ‘at risk’ of OSA from the Standard versus polysomnography ‘confirmed’ OSA is provided in Table 4. These findings highlight that the criteria for ‘at risk’ of OSA in the Standard misclassifies 23.2% (10/43) of workers with confirmed OSA (on a sleep study), and 38.7% (24/62) of workers with controlled OSA.
Aim 2: Investigate the association between OSA risk as identified in the Standard with real-world rail safety and operational incidents (‘rail incidents’) in Australian train drivers
To determine whether ‘at risk’ train drivers according to the Standard experienced greater operational and/or safety incidents in the time following the health assessment window, we analysed data from 633 train drivers who had an ‘unknown’ OSA status (workers who had not undergone a sleep study to confirm OSA). A total of 723 of the 896 (80.7%) events were attributable to these 633 drivers. Of these 633 train drivers, 21 (3.3%) met ‘at risk’ criteria for OSA according to the Standard. These ‘at risk’ train drivers had 61% greater incidents in the years following their health assessment compared to drivers who did not meet ‘at risk’ criteria in the unknown OSA group (Fig. 4, Incidence Risk Ratio (IRR): 1.61, 95% Confidence Interval (CI) 1.02–2.56).
Number of incidents per participant for participant at risk (shaded) and not at risk (black) of OSA according to the current Standard. Note that there is a greater proportion of participants at risk of OSA with more than two events in the 2016–2020 window, and a lower proportion of participants at risk of OSA with no incidents in the timeframe.
Aim 3: Determine whether a more conservative risk threshold for OSA using existing health record data is warranted based on associations with rail incidents following a health assessment
To determine whether a lower threshold for OSA screening identified significantly greater incidents, we changed the thresholds for the ‘at risk due to clinical markers or risk factors’ trigger criteria. These criteria were drawn directly from available data in the existing health assessment measures. The difference between the trigger criteria in the Standard, and our altered thresholds are demonstrated in Fig. 4.
Application of a lower threshold using existing clinical metrics available in the worker databases, but with more conservative cut points (see Fig. 5), identified an additional 30 ‘at risk’ train drivers, taking the total to 51 (8.1% of the workers with unknown OSA status). Applying these criteria, ‘at risk’ train drivers had 46% greater incidents compared to drivers who did not meet risk criteria (IRR (95% CI) 1.46 (1.00–2.13)).
Comparison of existing ‘at risk’ criteria in the National Standard for Health Assessment of Rail Safety Workers10 to the lowered thresholds used for re-analysis. Note BMI, body mass index, BP, blood pressure.
A final, a posteriori, analysis was conducted to explore the impact of the relationship between OSA risk and operational and/or safety incidents when the BMI cutpoint was varied. Specifically, we set out to determine whether the association with incidents in ‘at risk’ workers remained as BMI cutpoint was progressively reduced. Findings from this analysis are illustrated in Fig. 6, reflecting IRRs and corresponding screening rate as a percentage of workers in the sample if the criteria were amended to the respective BMI levels. These findings are also shown in Table 5, with the indicative ‘greater’ incident rate. Together, these findings demonstrate a dose–response relationship between BMI levels used for screening criteria and prospective incidents likelihood. While 95% CI intervals are relatively large, there is a consistent 40–60% increase in incident likelihood for BMI levels ≥ 36.5 kg/m2, and this effect is consistently significant for BMI ≥ 38 kg/m2.
The (a) association between different BMI thresholds and risk of (safety and/or operational) incidents, along with (b) corresponding changes in screening rates (%) in train drivers. Note In Panel A, circles represent the estimand, and lines the 95% confidence intervals. In Panel B, screening rate is presented as a percentage (%) of the unknown OSA category. Data presented are unadjusted. BMI, body mass index.
Discussion
This study examined associations between obstructive sleep apnea (OSA) status based on reported OSA diagnosis in health assessments, OSA risk according to clinical risk factors in the existing Standard, and occurrence of rail incidents using real-world data. The parameters currently being used to screen for OSA in the Standard were found to misclassify workers ‘at risk’ of OSA. Specifically, 23.2% of workers with confirmed OSA, and 38.7% of workers with controlled OSA, would not have triggered a sleep study using clinical risk factors similar to the Standard, if they did not have confirmed OSA diagnosis already. We also show greater rail incidents for workers at risk of OSA (but not diagnosed) according to the Standard. Prospective analysis found that lowering the threshold for screening according to clinical risk factors (a combination of lowered BMI and less conservative indications of current clinical markers) identified greater rail incidents. These findings extend recent retrospective analyses which highlight the need to consider more stringent screening of OSA in rail workers8, and use more conservative clinical marker thresholds for risk criteria when screening for OSA in train drivers as a proof of concept reflecting the need to review criteria. Future studies should now carefully consider the appropriateness of specific clinical cut points when screening for OSA in larger studies.
The findings of this study extend previous research about the utility and design of the sleep disorder screening component of the current version of the Standard8 by highlighting a need to reconsider screening criteria for OSA. While progress has been made in identifying OSA since implementation of the Standard8,14,17, OSA prevalence rates in train drivers according to health assessments in these analyses remain markedly lower than prevalence in the general population of similarly aged adults. While one possible interpretation could be that since introduction, workers with OSA are either treated or have left the organisation, this is unlikely as there remain higher rates of risk factors for OSA (including obesity and comorbidities) in this worker demographic than comparably aged adults in Australia18. The consequence is high misclassification rates of workers with confirmed OSA and controlled OSA according to health assessment data, and thus the risk of rail incidents attributable to unmanaged OSA is likely still common in train drivers. This was confirmed in the current study by greater incident rates in high-risk workers according to real world data.
Our findings suggest a few key areas for consideration in future revisions of the Standard. One, it is evident from review of the Epworth Sleepiness Scale (ESS) scores collected at worker health assessments that self-reported sleepiness according to the ESS Score is unlikely to add particular value to screening criteria. None of the impacted train drivers in this analysis reported sleepiness scores which would trigger a sleep study, and ESS scores were lower than population averages reported for middle-aged Australians18. Workplace health assessments can be perceived with high suspicion in this industry. In some instances, self-reporting that avoids triggering health assessments is the prevailing attitude16. Consequently, self-report triggers for health assessment should be applied with caution. Reducing reliance on self-report of sleepiness and increasing use of more conservative physiological status and comorbidity data may facilitate more informed decision making around the need for OSA screening and management. Existing, validated tools such as the STOP-BANG29 and others30,31 are acceptable, incorporate subjective and objective indicators of OSA, and are easily implemented. Which of these screening criteria better predict OSA risk for rail safety incidents remains to be studied prospectively.
The consequence of revising the current risk thresholds for sleep disorder screening is the unavoidable increase in screening rates and referrals for sleep studies across organisations. This comes with inevitable costs related to diagnosing and managing OSA in worker populations. However, we were able to show that a small adjustment in clinical risk factors (specifically, BMI) reflects a relatively modest increase in screening, whilst also capturing workers at risk for a greater number of incidents. Given that OSA is associated with major incidents, and in some cases fatalities, in the rail industry32, the increased costs associated with screening are likely to be offset by the potential to reduce risk of major incidents in train drivers. Management is also likely to improve the negative associations of OSA sickness absenteeism33, poorer quality of life34, hypertension20 and poorer mental health35 which are all costly to the individual, the workplace and the health system.
Strengths, limitations, and future directions
These findings should be considered in light of methodological limitations inherent with interpreting real-world data. A limitation of our analyses is that our altered threshold for OSA ‘at risk’ status was drawn only from available health assessment data. Recording of OSA status, including severity, was reliant on the quality of health assessment notes. For example, the apnea hypopnoea index (AHI) is the indicator used to diagnosis OSA. The AHI was not routinely recorded for all workers with OSA, particularly if the worker was not a new diagnosis of OSA during the study window, and was considered ‘controlled’ OSA. Given that OSA severity is associated with different impacts on road and rail safety, it may be beneficial for authorised health professionals to record the AHI consistently as a metric of OSA severity, to ensure meaningful comparison by severity is feasible in future studies, as this was not possible within the current study. Another limitation is that the provided analyses relied on a specified window of health assessment data (2016-2018), which lead to a modest sample size available for analysis. For the incident analysis, we also assumed that the health assessment used to determine OSA status or risk is an accurate representation, and that this did not change during the subsequent incident period. This meant we were unable to determine whether some workers had sought treatment within the assessed analysis window. Consequently, we recommend that these analyses should be repeated with a larger sample size, including multiple health assessments during the incident period, before definitive conclusions can be drawn about the relationship between OSA risk status and rail safety incidents.
It is also worth considering in future whether emerging technologies could be used to better quantify OSA severity in train drivers, rather than relying on self-report, screeners and/or single night polysomnography (PSG). New metrics of OSA severity, including measures of hypoxia36,37, sleep fragmentation38,39 and autonomic responses40,41 have been shown to better predict cardio-metabolic risk associated with OSA. The implementation of these approaches in this worker population may also be helpful in future for identifying workers at risk of significant incidents, and should be considered where possible in future analyses. Also of relevance, night-to-night variability in OSA severity can be significant, leading to misclassification of disease severity and misdiagnosis in 20–50% of cases when diagnosis is made using single-night PSG42,43. Multi-night assessment of OSA severity using low-cost ‘nearable’ sleep measurement devices has been shown to provide more reliable estimates of OSA severity and associated health outcomes compared to traditional PSG20,44. Using similar approaches for this worker population may facilitate more detailed analysis of the application of the Standard, and any future amendments or iterations, relative to OSA status in train drivers. This would also facilitate evidence-based continuous improvement of sleep disorder screening recommendations in future, to ensure workers most impacted by OSA are appropriately screened and treated.
The database from which incident data were extracted was very comprehensive. However, we were not able to incorporate detailed information about worker schedules, including shift work schedules, which would be beneficial in future studies given previous findings of OSA syndrome symptoms worsening during daytime sleep for shift workers45 which could have implications for driver safety. This limits our ability to further explore the relationship between OSA, shift work schedules and incidents in this sample. We were also not able to account for workers leaving the industry or driving time per week in the current analyses which would be beneficial in future analyses. There was a discordance between our OSA at risk screening criteria and the Standard in 21 participants (3.3%) who should have been screened for OSA. This may be because we were not able to replicate the Standard OSA risk exactly due to missing data in our sample, however, the more likley explanation is that some of these drivers may also have been screened in an earlier clinical assessment, which would have been missed. Further, in the window of interest to this study, incident records were susceptible to change in terminology, detail and classification, including errors and inconsistencies in entry of incident data. This meant that data needed to be coded manually, but is also likely to have resulted in some incidents coded in a fashion which meant relevant operational or safety incident data could not be included. This raises a general need for better and more consistent entry of incident data over time to quantify impacts of health conditions on rail safety incidents more broadly.
Conclusion
Undiagnosed and unmanaged OSA poses significant health and safety risks for the rail industry. In Australia, a national Standard has been applied to try to manage this risk for some time. However, the utility of this Standard appears to be limited by use of screening questions and risk factor criteria that are likely to only identify the most severe of OSA cases, leaving others undiagnosed and unmanaged. We demonstrated considerable OSA misclassification based on existing Standard criteria for OSA screening compared to confirmed OSA status within the health assessment window. This study also showed a clear relationship between OSA status and subsequent rail incidents in train drivers using the existing Standard. Finally, we demonstrated that lowering the risk threshold according to clinical risk factors for OSA below what is required for the current Standard still identified workers with greater incidents. These results are the first of their kind for rail and suggest a need to reconsider the risk factors and screening approaches for OSA in future iterations of the Standard.
Data availability
All data generated or analysed during this study are included in this published article [and its supplementary information files]. Due to data privacy and confidentiality requirements, raw data are not available for public access, and data access should be discussed with the corresponding author.
References
Vakulin, A. et al. Individual variability and predictors of driving simulator impairment in patients with obstructive sleep apnea. J. Clin. Sleep Med. 10, 647–655 (2014).
George, C. F. P. Sleep apnea, alertness, and motor vehicle crashes. Am. J. Respir. Crit. Care Med. 176, 954–956 (2007).
Alhejaili, F. et al. Prevalence of obstructive sleep apnea among saudi pilots. Nat. Sci. Sleep 13, 537–545 (2021).
Gurubhagavatula, I., Tan, M. & Jobanputra, A. M. OSA in professional transport operations: Safety, regulatory, and economic impact. Chest 158, 2172–2183 (2020).
Chapman, J., Naweed, A., Wilson, C. & Dorrian, J. Sleep for heart health: investigating the relationship between work day sleep, days off sleep, and cardiovascular risk in Australian train drivers. Ind. Health 57, 691–700 (2019).
Filtness, A. J. & Naweed, A. Causes, consequences and countermeasures to driver fatigue in the rail industry: The train driver perspective. Appl. Ergon. 60, 12–21 (2017).
Dorrian, J., Chapman, J., Bowditch, L., Balfe, N. & Naweed, A. A survey of train driver schedules, sleep, wellbeing, and driving performance in Australia and New Zealand. Sci. Rep. 12, 1–11 (2022).
Abeyaratne, M., Casolin, A. & Luscombe, G. Safety incidents and obstructive sleep apnoea in railway workers. Occup. Med. 73(2), 97–102 (2023).
Hocking, B. The Inquiry into the Waterfall train crash: implications for medical examinations of safety-critical workers. Med. J. Aust. 184, 126–128 (2006).
National Transport Commission. National Standard for Health Assessment of Rail Safety Workers. (2017).
Johns, M. W. A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14, 540–545 (1991).
Babor, T.F., Higgins-Biddle, J.C., Saunders, J.B. & Monteiro, M. G. Audit. The Alcohol Use Disorders Identification Test (AUDIT): guidelines for use in primary care (2001).
Kessler, R. C. et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol. Med. 32, 959–976 (2002).
Mina, R. & Casolin, A. The Australian national standard for rail workers five years on. Occup. Med. 62, 642–647 (2012).
Mina, R. & Casolin, A. National standard for health assessment of rail safety workers: the first year. Med. J. Aust. 187, 394–397 (2007).
Naweed, A., Chapman, J. & Trigg, J. Tell them what they want to hear and get back to work: Insights into the utility of current occupational health assessments from the perspectives of train drivers. Transp. Res. Part A: Policy Pract. 118, 234–244 (2018).
Colquhoun, C. P. & Casolin, A. Impact of rail medical standard on obstructive sleep apnoea prevalence. Occup. Med. 66, 62–68 (2016).
McArdle, N. et al. Prevalence of common sleep disorders in a middle-aged community sample. J. Clin. Sleep Med. 18, 1503–1514 (2022).
Punjabi, N. M. et al. Sleep-disordered breathing, glucose intolerance, and insulin resistance: The sleep heart health study. Am. J. Epidemiol. 160, 521–530 (2004).
Lechat, B. et al. High night-to-night variability in sleep apnea severity is associated with uncontrolled hypertension. NPJ Digit. Med. 6, 57 (2023).
Nieto, F. J. et al. Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. JAMA 283, 1829–1836 (2000).
Gottlieb, D. J. et al. Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure: the sleep heart health study. Circulation 122, 352–360 (2010).
Hsieh, H.-F. & Shannon, S. E. Three approaches to qualitative content analysis. Qual. Health Res. 15, 1277–1288 (2005).
Naweed, A., Bowditch, L., Chapman, J., Dorrian, J. & Balfe, N. On good form? Analysis of rail signal passed at danger pro formas and the extent to which they capture systems influences following incidents. Saf. Sci. 151, 105726 (2022).
R Core Team. RStudio: Integrated Development Environment for R v3.6.2. R Foundation for Statistical Computing, Vienna, Austria. URL https://www.r-project.org/ (2019).
Mathew, J. & Benekohal, R. F. Highway-rail grade crossings accident prediction using zero inflated negative binomial and empirical bayes method. J. Safety Res. 79, 211–236 (2021).
Jiroutek, M. R. & Turner, J. R. Why it is nonsensical to use retrospective power analyses to conduct a postmortem on your study. J. Clin. Hypertens. 20, 408–410 (2018).
Australasian Railway Association. Workforce Development Report - Rail Workforce Data 2014. (2014).
Nagappa, M. et al. Validation of the STOP-bang questionnaire as a screening tool for obstructive sleep apnea among different populations: A systematic review and meta-analysis. PLoS One 10, e0143697 (2015).
de Menezes-Júnior, L. A. A. et al. The predictive values of BOAH and No-apnea score for screening obstructive sleep apnea in rotating shift worker drivers. Sleep Med X 6, 100084 (2023).
de Menezes Júnior, L. A. A. et al. Diagnostic accuracy of the Berlin questionnaire and the NoSAS score in detecting risk for obstructive sleep apnea in rotating shift workers. Sleep Breath. 26, 743–751 (2022).
McKay, M. P. Fatal consequences: Obstructive sleep apnea in a train engineer. Ann. Fam. Med. 13, 583–586 (2015).
Reynolds, A. C. et al. Sickness absenteeism is associated with sleep problems independent of sleep disorders: Results of the 2016 Sleep Health Foundation national survey. Sleep Health 3, 357–361 (2017).
Bjornsdottir, E. et al. Quality of life among untreated sleep apnea patients compared with the general population and changes after treatment with positive airway pressure. J. Sleep Res. 24, 328–338 (2015).
Edwards, C., Almeida, O. P. & Ford, A. H. Obstructive sleep apnea and depression: A systematic review and meta-analysis. Maturitas 142, 45–54 (2020).
Azarbarzin, A. et al. The hypoxic burden of sleep apnoea predicts cardiovascular disease-related mortality: the osteoporotic fractures in men study and the sleep heart health study. Eur. Heart J. 40, 1149–1157 (2019).
Azarbarzin, A. et al. The sleep apnea-specific hypoxic burden predicts incident heart failure. Chest 158, 739–750 (2020).
Lechat, B. et al. New and emerging approaches to better define sleep disruption and its consequences. Front. Neurosci. 15, 751730 (2021).
Lechat, B. et al. A novel electroencephalogram-derived measure of disrupted delta wave activity during sleep predicts all-cause mortality risk. Ann. Am. Thorac. Soc. 19, 649–658 (2022).
Azarbarzin, A. et al. The sleep apnea-specific pulse-rate response predicts cardiovascular morbidity and mortality. Am. J. Respir. Crit. Care Med. 203, 1546–1555 (2021).
Solelhac, G. et al. Pulse wave amplitude drops index: A biomarker of cardiovascular risk in obstructive sleep apnea. Am. J. Respir. Crit. Care Med. https://doi.org/10.1164/rccm.202206-1223OC (2023).
Lechat, B. et al. Multi-night prevalence, variability, and diagnostic misclassification of obstructive sleep Apnea. Am. J. Respir. Crit. Care Med. https://doi.org/10.1164/rccm.202107-1761OC (2021).
Punjabi, N. M., Patil, S., Crainiceanu, C. & Aurora, R. N. Variability and misclassification of sleep apnea severity based on multi-night testing. Chest 158, 365–373 (2020).
Lechat, B. et al. Single-night diagnosis of sleep apnea contributes to inconsistent cardiovascular outcome findings. Chest https://doi.org/10.1016/j.chest.2023.01.027 (2023).
Paciorek, M. et al. Obstructive sleep apnea in shift workers. Sleep Med. 12, 274–277 (2011).
Acknowledgements
This study was funded and supported by Transport for NSW and Sydney Trains (RSH/6060). The authors gratefully acknowledge research assistance from Teal Evans.
Author information
Authors and Affiliations
Contributions
The study was designed by A.N., and A.C.R. Data acquisition were conducted by A.N., A.C.R., and A.C. Data processing and analyses of health data were conducted by A.C.R, and B.L. and data processing and analyses of safety incident data were conducted by A.N., and J.C. Data interpretation by A.C.R., A.N., B.L., J.C., R.J.A., S.A.F, and A.C. The manuscript was written by A.C.R. and A.N. with development of specific sections by B.L. and initial review by A.C. Further critical revision and final approval was from all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Figure
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Naweed, A., Lechat, B., Chapman, J. et al. Reconsidering screening thresholds in health assessments for obstructive sleep apnea using operational and safety incident data. Sci Rep 14, 10844 (2024). https://doi.org/10.1038/s41598-024-61118-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-61118-y
Keywords
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.