Abstract
Objectives
To determine, among neonates at-risk for hyperbilirubinemia, whether measuring end-tidal carbon monoxide concentration (ETCOc) twice before 48 hours could identify those who would develop hyperbilirubinemia and differentiate hemolytic vs. non-hemolytic causes.
Methods
Prospective study on neonates meeting criteria “at-risk for hyperbilirubinemia.” Routine bilirubin measurements and 10-day follow-up were used to categorize neonates as; (1) normal (no hyperbilirubinemia, all bilirubins <95th percentile of Bhutani nomogram), (2) having hemolytic hyperbilirubinemia (bilirubin ≥95th percentile, DAT+, elevated retic, or G6PD+), or (3) having non-hemolytic hyperbilirubinemia.
Results
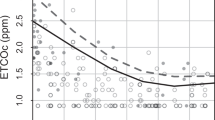
386 neonates were enrolled. 321 (83%) did not develop hyperbilirubinemia and 65 (17%) did, of which 29 were judged hemolytic and 36 non-hemolytic. High ETCOc differentiated the hemolytic group (p < 0.001). First-day ETCOc correlated with bilirubin and with reticulocyte count (r = 0.896 and 0.878) and sensitivity and specificity for predicting hyperbilirubinemia were excellent (83% and 95%).
Conclusions
ETCO measurement in the first 48 hours after birth predicts hemolytic hyperbilirubinemia.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Kemper AR, Newman TB, Slaughter JL, Maisels MJ, Watchko JF, Downs SM, et al. Clinical Practice Guideline Revision: Management of Hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 2022;150:e2022058859.
De Winter DP, Hulzebos C, Van ‘t Oever RM, De Haas M, Verweij EJ, Lopriore E. History and current standard of postnatal management in hemolytic disease of the fetus and newborn. Eur J Pediatr. 2022;182:489–500.
Du L, Ma X, Shen X, Bao Y, Chen L, Bhutani VK. Neonatal hyperbilirubinemia management: Clinical assessment of bilirubin production. Semin Perinatol. 2021;45:151351.
Tidmarsh GF, Wong RJ, Stevenson DK. End-tidal carbon monoxide and hemolysis. J Perinatol. 2014;34:577–81.
American Academy of Pediatrics Subcommittee on Hyperbilirubinemia. Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics 2004;114:297–316.
Krog GR, Donneborg ML, Hansen BM, Lorenzen H, Clausen FB, Jensen KV, et al. Prediction of ABO hemolytic disease of the newborn using pre- and perinatal quantification of maternal anti-A/anti-B IgG titer. Pediatr Res. 2021;90:74–81.
Bakkeheim E, Bergerud U, Schmidt-Melbye AC, Akkök CA, Liestøl K, Fugelseth D, et al. Maternal IgG anti-A and anti-B titres predict outcome in ABO-incompatibility in the neonate. Acta Paediatr. 2009;98:1896–901.
Kardum D, Serdarušić I, Biljan B, Šantić K, Živković V, Kos M. Cord blood bilirubin and prediction of neonatal hyperbilirubinemia and perinatal infection in newborns at risk of hemolysis. Jornal de Pediatria. 2021;97:440–4.
Khairy MA, Abuelhamd WA, Elhawary IM, Mahmoud Nabayel AS. Early predictors of neonatal hyperbilirubinemia in full term newborn. Pediatr Neonatol. 2019;60:285–90.
Mehta R, Petrova A. Direct antiglobulin test in the prediction of hyperbilirubinemia and predischarge bilirubin levels in infants with mother-infant blood type incompatibility. Pediatr Neonatol. 2021;62:406–11.
Das S, Shastry S, Chakravarthy PK, Baliga PB. Clinical implication of immunohaematological tests in ABO haemolytic disease of newborn: Revisiting an old disease. Transfus Med. 2021;31:30–35.
Karabulut B, Arcagok BC. A neglected and promising predictor of severe hyperbilirubinemia due to Hemolysis: Carboxyhemoglobin. Fetal Pediatr Pathol. 2020;39:124–31.
Sarici SU, Yurdakök M, Serdar MA, Oran O, Erdem G, Tekinalp G, et al. An early (sixth-hour) serum bilirubin measurement is useful in predicting the development of significant hyperbilirubinemia and severe ABO hemolytic disease in a selective high-risk population of newborns with ABO incompatibility. Pediatrics. 2002;109:e53.
Han S, Yu Z, Liu L, Wang J, Wei Q, Jiang C, et al. A model for predicting significant hyperbilirubinemia in neonates from China. Pediatrics. 2015;136:e896–905.
Stevenson DK, Fanaroff AA, Maisels MJ, Young BW, Wong RJ, Vreman HJ, et al. Prediction of hyperbilirubinemia in near-term and term infants. J Perinatol. 2001;21:S63–72.
Bhutani VK, Srinivas S, Castillo Cuadrado ME, Aby JL, Wong RJ, Stevenson DK. Identification of neonatal haemolysis: an approach to predischarge management of neonatal hyperbilirubinemia. Acta Paediatr. 2016;105:e189–94.
Okuyama H, Yonetani M, Uetani Y, Nakamura H. End-tidal carbon monoxide is predictive for neonatal non-hemolytic hyperbilirubinemia. Pediatr Int. 2001;43:329–33.
Bhatia A, Chua MC, Dela Puerta R, Rajadurai VS. Noninvasive detection of hemolysis with ETCOc measurement in neonates at risk for significant Hyperbilirubinemia. Neonatology. 2020;117:612–8.
Bao Y, Zhu J, Ma L, Zhang H, Sun L, Xu C, et al. An end-tidal carbon monoxide nomogram for term and late preterm Chinese newborns. J Pediatr. 2022;250:16–21.e3.
Bahr TM, Shakib JH, Stipelman CH, Kawamoto K, Lauer S, Christensen RD. Improvement initiative: end-tidal carbon monoxide measurement in newborns receiving phototherapy. J Pediatr. 2021;238:168–73.e2.
Zhan YL, Peng HB, Jin ZC, Su JF, Tan XY, Zhao L, et al. Higher ETCOc predicts longer phototherapy treatment in neonatal hyperbilirubinemia. Front Pediatr. 2023;11:1154350.
Javier MC, Krauss A, Nesin M. Corrected end-tidal carbon monoxide closely correlates with the corrected reticulocyte count in coombs’ test-positive term neonates. Pediatrics. 2003;112:1333–37.
Acknowledgements
We thank Capina company for providing the ETCO instruments and equipment. We thank our patients and their parents for participating in our study. We thank Dr. Xueyu Chen (Shenzhen Maternity and Child Healthcare Hospital, The First School of Clinical Medicine, Southern Medical University) for her competent advice.
Funding
This research was supported by the Shenzhen Fund for Guangdong Provincial Highlevel Clinical Key Specialties (No. SZGSP009).
Author information
Authors and Affiliations
Contributions
Xiaoqin Cheng conceptualized and designed the study, included patients, collected the data, performed the statistical analyses, drafted the initial manuscript, and reviewed and revised the manuscript. Bingchun Lin, Yong Yang, Yanliang Yu, and Yongping Fu revised the manuscript. Chuanzhong Yang provided guidance for this study. All authors approved the final manuscript as submitted and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, X., Lin, B., Yang, Y. et al. End-tidal carbon monoxide concentrations measured within 48 hours of birth predict hemolytic hyperbilirubinemia. J Perinatol (2024). https://doi.org/10.1038/s41372-024-01967-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41372-024-01967-7