Abstract
Background:
Eosinophils reside in normal gastrointestinal tracts and increase during disease states. Receptors for eosinophil-derived granule proteins (EDGPs) have not been identified, but highly cationic molecules, similar to eosinophil proteins, bind extracellular calcium–sensing receptors (CaSRs). We hypothesized that stimulation of CaSRs by eosinophil proteins activates epithelial cells.
Methods:
Caco2 intestinal epithelial cells, AML14.3D10 eosinophils, wild-type (WT) human embryonic kidney 293 (HEK293) cells not expressing CaSRs (HEK-WT), and CaSR-transfected HEK293 cells (HEK-CaSR) were stimulated with an eosinophil protein analog poly-L-arginine (PA) and phosphorylated extracellular signal–regulated kinase (pERK)1 and pERK2 were measured. Functional activation was measured with collagen lattice contraction assays.
Results:
Coculture of Caco2 cells with AML14.3D10 eosinophils augmented lattice contraction as compared with lattices containing Caco2 cells alone. PA stimulation of Caco2 lattices augmented contraction. HEK-CaSR stimulation with PA or Ca2+ resulted in greater pERK activation than that of stimulated HEK-WT cells. PA stimulated greater HEK-CaSR lattice contraction than unstimulated lattices. Contraction of PA-stimulated and PA-unstimulated HEK-WT lattices did not differ.
Conclusion:
Exposure of intestinal epithelia to the EDGP analog PA stimulates CaSR-dependent ERK phosphorylation and epithelial-mediated collagen lattice contraction. We speculate that EDGP release within the epithelial layers activates the CaSR receptor, leading to matrix contraction and tissue fibrosis.
Similar content being viewed by others
Main
Tissue remodeling can be characterized by a number of different mucosal responses including changes in barrier function, mucus secretion, muscle contraction, and collagen deposition. Eosinophils may play a key role in the remodeling process and have been shown to diminish epithelial barrier function, increase mucus secretion, and stimulate contraction and collagen deposition (1,2). They have been implicated in tissue remodeling in the lung, where they increase under asthmatic conditions, and eosinophil granule proteins have elicited increased expression of profibrotic, transforming growth factor-β in lung fibroblasts in vitro (3). The relative contribution and mechanistic role of eosinophils and eosinophil-derived granule proteins (EDGPs) in tissue remodeling in the gastrointestinal tract are not certain. Tissue fibrosis, which is one of the important aspects of tissue remodeling, is characterized by excessive deposition and contraction of the extracellular matrix (4). An in vitro model, the collagen lattice contraction assay, offers an easily controlled and flexible environment to study factors contributing to matrix contraction (5). Although muscle fiber contraction and fibroblast activity have been thought to account for much of this activity in vivo, contraction of nonmuscle cells, such as epithelia, also occurs in remodeling and epithelial cells also interact with the extracellular matrix, but these events are less well defined.
The extracellular calcium–sensing receptor (CaSR) is a G-protein coupled receptor that is a member of the C family of G-protein coupled receptors. CaSR is expressed on extracellular Ca2+–regulating cells such as parathyroid, renal tubular, and bone cells (6). CaSR is also expressed throughout the gastrointestinal system in basal cells of the esophagus (7), gastric G and parietal cells (8,9,10), I cells of the duodenum (11), and surface and crypt epithelia of the colon (12). CaSR activation is known to increase intracellular mitogen activated protein kinase activity including extracellular signal–regulated kinase (ERK) activation (6). Increased ERK activation has been associated with overexpression of profibrotic genes in dermal fibroblasts (13,14), and mitogen activated protein kinase inhibitors have been shown to inhibit both fibroblast-populated collagen lattice contraction and wound contraction in an in vivo rat model (15). It is currently understood that CaSR is a multimodal sensor of multivalent cations such as poly-L-arginine (PA), polyamines, L-amino acids, and pH in addition to ionized Ca2+. Previously, we have reported CaSR activation by an EDGP, major basic protein (MBP) stimulated fibroblast growth factor-9 expression and secretion from an esophageal cell line (16). The aim of the current experiments was to determine if PA, a previously used analog for EDGPs, could activate CaSR expressing epithelial cells.
Results
AML14.3D10 Eosinophils and the EDGP Analog PA Augment Epithelial-Mediated Collagen Lattice Contraction
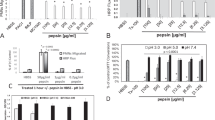
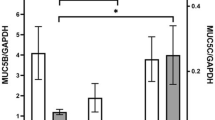
Although eosinophils are known to reside adjacent to the gastrointestinal epithelium, their potential role in remodeling of the extracellular matrix via epithelial cells has not been investigated. To address this, we hypothesized that EDGPs stimulate gastrointestinal tissue contraction, and therefore the impact of eosinophils on epithelial cell–populated collagen lattice contraction was measured. Coculture of Caco2 cells with AML14.3D10 eosinophils (3D10 eosinophils) led to significant contraction as compared with those of Caco2 cells or 3D10 eosinophils alone ( Figure 1 ) (43.0 ± 1.0% vs. 34.3 ± 2.2%, P < 0.02; Caco2 with eosinophils vs. Caco2 alone). We next used the highly charged MBP analog, PA, in the collagen lattice contraction assay. PA (0.5 μmol/l and 1 μmol/l) stimulated a concentration- and time-dependent contraction of Caco2-populated lattices that was significantly augmented as compared with those of unstimulated controls ( Figure 2a,b ) (46.4 ± 1.6 vs. 36.7 ± 1.3, P < 0.001; PA vs. media alone). Cell viability of Caco2 and AML14.3D10 cells was assured by trypan blue staining (96 ± 2% viability in cocultured, PA stimulated and unstimulated cells).
Eosinophil–epithelial coculture results in increased collagen lattice contraction. Contraction of collagen lattices populated with 3D10 eosinophils and Caco2 cells over time. 3D10 eosinophils (5 × 105 cells/ml) and Caco2 cells (5 × 105 cells/ml) were suspended in collagen lattices either alone or in coculture. Lattice surface area was measured at indicated time points. Contraction is reported as mean percentage of initial surface area ± SD. Lattice contraction was augmented when Caco2 cells were suspended with 3D10 eosinophils (triangles) as compared with Caco2 cells alone (squares). Lattices with 3D10 eosinophils alone (circles) and acellular collagen lattices (data not shown) did not contract (P < 0.02 Caco2 with eosinophils vs. Caco2).
Eosinophil granule protein analog stimulation of epithelial cells results in increased collagen lattice contraction. (a) Contraction of Caco2-populated collagen lattices exposed to 0.5 and 1 μmol/l poly-l-arginine (PA) or media alone (CTL). Lattice surface area was measured at 48 h. PA-treated lattices display concentration-dependent augmentation in contraction as compared with untreated lattices (*P = 0.01, **P < 0.01). (b) Contraction of Caco2-populated collagen lattices exposed to 1 μmol/l PA over time (initial time point vs. 24 and 48 h; **P < 0.01). Percentages of initial surface areas at 0, 24, and 48 h following lattice solidification are displayed. All values represent mean percentage of initial surface area ± SD of five lattices from one of two representative experiments. CTL, unstimulated control lattices.
CaSR Expression
Monomeric CaSR is present in the stably CaSR-transfected human embryonic kidney (HEK) cells (HEK-CaSRs) and the Caco2 cells but absent in the late-passage (p11) HT-29 cells (Supplementary Figure S1 online). Under nonreducing conditions, higher molecular weight CaSR protein (~250 kDa) was also found in both the HEK-CaSR cells and the Caco2 cells but was absent in late-passage HT-29 cells (data not shown).
EDGP Analog Activates Epithelial Cells
Given these findings, we were interested in determining how the EDGPs may be activating intestinal epithelial cells. To date, receptors for EDGPs have not been identified. Knowing that EDGPs and especially the MBP analog, PA, are highly charged cationic proteins, we examined the impact of PA on the CaSR that is known to be expressed on Caco2 cells (17). Phosphorylated ERK (pERK) was measured to assess cell activation in response to PA stimulation. Western blot analysis revealed that PA activated pERK at 5 min, an effect that was sustained to 1 h as seen in Figure 3a,b .
Eosinophil granule protein analog stimulates epithelial ERK phosphorylation. Influence of poly-L-arginine (PA) on ERK 1/2 phosphorylation in Caco2 epithelial cells. (a) Caco2 cells were stimulated with PA (1 μmol/l) for indicated times. Cell lysates were harvested and western blot was performed for phosphorylated ERK 1/2 (pERK). GAPDH indicates equivalent protein loading. (b) Densitometry analysis displaying pERK/GAPDH ratio. ERK, extracellular signal–regulated kinase; GAPDH, glyceraldehyde 3-phosphate dehydrogenase.
ERK Activation by Eosinophil Granule Protein Analog Is CaSR Dependent
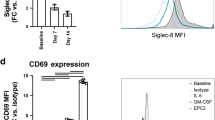
We next examined whether CaSR was necessary for PA activation of epithelial cells. Wild-type HEK cells (HEK-WTs), which do not express CaSR, were transiently transfected with full-length CaSR (HEK-Ts) ( Figure 4a ). Stimulation of HEK-T cells with PA led to pERK activation as compared with that of HEK-WT cells, with calcium used as a CaSR-positive control and epidermal growth factor activation as a non-CaSR control ( Figure 4b ). PA stimulation led to robust ERK signal by 5 min as determined by qualitative western blot analysis ( Figure 4c ). ERK activation was also evaluated using quantitative chemiluminescent Meso Scale technology (Meso Scale Diagnostics, Gaithersburg, MD). Both PA (1 μmol/l) and calcium (20 mmol/l) stimulation led to an increase in ERK activation in stably transfected HEK-CaSR cells ( Figure 5 ) as compared with HEK-WT cells (fold increase stimulated pERK over unstimulated control: 1.2 ± 0.45 vs. 7.9 ± 1.1, P < 0.01, HEK-WT vs. HEK-CaSR (PA); 2.0 ± 0.57 vs. 8.9 ± 1.9, P < 0.01, HEK-WT vs. HEK-CaSR (Ca)) ( Figure 5 ). The HEK-WT and HEK-CaSR cells display similar 8–10-fold increases in pERK with epidermal growth factor stimulation (8.4 ± 0.9 vs. 9.6 ± 2.5, HEK-WT and HEK-CaSR, respectively, P =0.48) ( Figure 5 ). The same pattern of ERK activation was seen in HEK-T cells and controls (data not shown).
Epithelial ERK phosphorylation by poly-L-arginine (PA) is CaSR dependent. Influence of Ca, PA, and EGF on wild-type (WT) and CaSR-transfected HEK cells. (a) mRNA was harvested and reverse transcription PCR for CaSR and β-actin performed on WT HEK cells (HEK-WT), transiently CaSR-transfected HEK cells (HEK-T), and HEK cells stably transfected with CaSR (HEK-CaSR). CTL represents negative control without mRNA. (b) HEK-WT and HEK-T cells (Origene, Rockville, MD) were exposed to Ca (20 mmol/l), PA (1 μmol/l), or EGF (100 ng/ml) for 5 min and western blot on cell lysates was performed for phosphorylated ERK (pERK). In HEK-T cells, both 1 μmol/l PA and 20 mmol/l calcium induce ERK activation along with 100 ng/ml EGF. (c) Time course of ERK phosphorylation with PA (1 μmol/l) stimulation and media control in a HEK-CaSR cell line that stably expresses CaSR. CaSR, extracellular calcium–sensing receptor; EGF, epidermal growth factor; CTL, unstimulated control lattice; ERK, extracellular signal–regulated kinase; HEK, human embryonic kidney.
Epithelial ERK phosphorylation by PA is CaSR dependent. Fold increase in percentage of ERK phosphorylation (pERK/total ERK) over control following 5-min stimulation of wild-type HEK cells (white bars) and HEK cells stably transfected with CaSR (black bars) with PA, Ca, and EGF. pERK and total ERK were quantified from cell lysates using chemiluminescence (Meso Scale Discovery, Meso Scale Diagnostics, Gaithersburg, MD). Results reflect the mean ± SD of five independent experiments (*P < 0.01, †Not significant). CaSR, extracellular calcium–sensing receptor; EGF, epidermal growth factor; ERK, extracellular signal–regulated kinase; HEK, human embryonic kidney; PA, poly-L-arginine; pERK, phosphorylated ERK.
Gain of CaSR Function Augments Cell-Mediated Collagen Lattice Contraction in Response to Granule Protein Analog Stimulation
We next determined if gain of CaSR ligation resulted in a functional impact. PA stimulation (1 μmol/l) significantly increased contraction of collagen lattices populated with HEK-CaSR cells as compared with both unstimulated HEK-CaSR lattices and PA-stimulated HEK-WT lattices at 24 h (percentage initial surface area: 58.8 ± 2.9% vs. 71.0 ± 3.9%, PA-stimulated HEK-CaSR vs. unstimulated HEK-CaSR lattices, respectively, P < 0.01, and 58.8 ± 2.9% vs. 71.8 ± 2.0%, PA-stimulated HEK-CaSR vs. PA-stimulated HEK-WT lattices, respectively, P < 0.01) ( Figure 6 ). PA stimulation did not significantly affect collagen lattice contraction in HEK-WT–populated collagen lattices as compared with HEK-WT–unstimulated control lattices (71.8 ± 2.0% vs. 69.6 ± 1.0%, PA vs. unstimulated control lattices, respectively, not significant).
CaSR contributes to collagen lattice contraction. Contraction of HEK-WT (white bars) and HEK-CaSR (black bars) populated collagen lattices stimulated with PA and media control. HEK-WT and HEK-CaSR cells were suspended in collagen lattices at 5 × 105 cells/ml and exposed to 1 μmol/l PA or not. Percentage of initial lattice surface area at 24 h is reported. Values represent mean ± SD of five lattices (*P < 0.001). CaSR, extracellular calcium–sensing receptor; HEK, human embryonic kidney; PA, poly-L-arginine; WT, wild-type.
Discussion
Eosinophils are present in the gastrointestinal mucosa and can reside directly adjacent to the basolateral surface of epithelial cells (18). During inflammatory states, eosinophils secrete EDGPs into tissue spaces (19). In studies examining pulmonary and gastrointestinal inflammation, eosinophils have been shown to participate in the remodeling process. In vitro studies support a role of eosinophils in remodeling because they can stimulate mast cell histamine release, fibroblast cytokine release, and muscle contraction. Although EDGPs are associated with these roles, no cell surface receptors have been identified, and molecular mechanisms have not been fully defined. Here, we show that PA, an analog of eosinophil-derived MBP, stimulates CaSR-dependent activation of the epithelium and epithelial-mediated collagen lattice contraction. This work suggests that the EDGP, MBP, may exert biological activity via CaSR.
Mucosal tissues are composed of a variety of molecular and cellular components. In a number of organ systems, extracellular matrices can be remodeled by resident and recruited cells, such as eosinophils, to form scar tissue and to contract. Although lung epithelial cells have previously been shown to contract collagen lattices and appear to play a role in tissue remodeling, the role of gastrointestinal epithelial cells in tissue remodeling is less well defined (20). As we have previously described, the collagen lattice contraction assay was used here to provide a functional readout of the remodeling process as it pertains to epithelial–eosinophil interactions (5).
Whereas several studies identified EDGPs’ cytotoxicity, a process thought to be related to increasing cell membrane permeability (21), little is known about how EDGPs may activate resident and recruited cells in mucosal surfaces in a nontoxic fashion (22). Given that CaSR is expressed on the intestinal epithelia along the length of the intestinal tract and is ligated by highly charged molecules, we wondered whether this receptor could provide a link by which epithelial cells sense the extracellular milieu. Results presented here support a dynamic interaction between PA and epithelial cells in which the EDGP analog stimulates robust ERK activation and functional response related to collagen lattice contraction.
Previously, we have shown that knockdown of the CaSR in esophageal epithelial cells prevented the stimulation of fibroblast growth factor-9 secretion by an MBP peptide (16). Loss of CaSR expression by transient transfection with small interfering RNA duplex has also been shown to prevent Ca2+-stimulated inhibition of defective Wnt/β-catenin signaling in colon cancer cells (23) and stimulation of bone morphogenetic protein-2 and Wnt5a from colonic myofibroblasts (24). In the current experiments, we have relied on CaSR-transfected HEK cells to examine these responses and compared their response with added calcium in untransfected HEK cells that do not express the CaSR. Usually, the HEK-CaSR cells respond maximally with either hormone secretion (25) or intracellular Ca2+ transients at 3–10 mmol/l (26). The twofold increase in Ca2+ required for maximal effect here probably represents reduced expression of the CaSR from lowered transfection efficiency. It is also possible that mutations of the extracellular domain of the CaSR increased the Ca2+ concentration required to activate the receptor, as has been previously reported (27). Our results comparing calcium addition with HEK cells that did not express the CaSR with those with some CaSR expression show that very little activation occurred without CaSR expression. In addition, significant augmentation of lattice contraction with PA stimulation occurred only in cells with CaSR expression. This strongly suggests that the CaSR mediated the activation and contraction responses seen in the HEK-CaSR cells.
Although this study provides evidence to support the role of MBP as a ligand for the CaSR, several issues remain to be addressed. First, our previous study exposed an intact epithelial monolayer to PA, whereas in the current study epithelial cells were dispersed throughout the collagen lattice (1). Interactions among epithelial cells, collagen, and other matrix proteins probably influence their response to PA in a different fashion. Second, direct biochemical evidence of CaSR ligation by EDGPs has not yet been demonstrated. Third, the observed results could be explained by the cationic charge associated with PA and not a specific feature of the EDGP, MBP. Finally, the exact distribution of CaSR protein on epithelial cell lines requires definition. Here, we demonstrated the presence of CaSR on Caco2 cells by western blots using HEK-CaSR cells as a positive control. Consistent with this finding was our previous study showing that HT-29 cells express CaSR protein, which was reduced by RNA interference technique (23). Given that others have reported that the CaSR promoter is epigenetically silenced in several adenocarcinoma cell lines (28), it was important to confirm that the CaSR was present in the Caco2 cells. It is noteworthy that detectable but faint CaSR transcript is present in both Caco2 and HT-29 cells (28), and the current experiments demonstrate CaSR protein in the Caco2 cells. It is probable that with passage, the CaSR in the HT-29 cells becomes methylated and its expression is lost with increased passage. Indeed, our earlier work showing CaSR protein and its knockdown used cells only from p1 to p6 (23). Caco2 cells differentiate with confluence, and it has been observed that with confluence CaSR expression in Caco2 cells increases (data not shown); it is likely that selection of clones that express various levels of the CaSR occurs during passage in this cell line. Nevertheless, in the current experiments, the Caco2 cells expressed the CaSR, and it is likely that proteins secreted from the eosinophil cell line were acting as agonist(s) of the CaSR to stimulate wound closure.
In conclusion, our results show that exposure of intestinal epithelia to the EDGP analog, PA, stimulates CaSR-dependent ERK phosphorylation and epithelial-mediated collagen lattice contraction. We believe that further work is needed to determine whether eosinophil release of MBP activates the CaSR receptor, leading to matrix contraction and tissue fibrosis.
Methods
Cell Culture
All cell incubations were performed at 37 °C in a humidified incubator with 5% CO2. Caco2 intestinal epithelial cells and HEK293 cells were obtained from American Type Culture Collection (ATCC, Manassas, VA). Caco2 and HEK293 cells lines were maintained in T75 flasks using Dulbecco’s Modified Eagle’s Medium (Fisher, Pittsburgh, PA) supplemented with 10% fetal bovine serum and 100 U/ml penicillin and 100 μ/ml streptomycin (Gibco, Grand Island, NY). AML14.3D10 cells (3D10 cells) were generously provided by Cassandra Paul (Wright State University, Dayton, OH) and were maintained in RPMI 1640 medium supplemented with 10% fetal bovine serum (2 mmol/l L-glutamine, 1 mmol/l sodium pyruvate), 5 × 10−5 M 2-mercaptoethanol, 100 U/ml penicillin, and 100 μ/ml streptomycin (Gibco, Grand Island, NY) as previously reported (1). HEK293 cells stably transfected with CaSR (HEK-CaSR) were grown and maintained under the same conditions as HEK293 WT cells (HEK-WT). Cells were passaged weekly at subconfluence by trypsinization (0.25%, 1 mmol/l EDTA).
CaSR Western Analysis
Early-passage, stably transfected HEK-CaSR cells, late-passage (p11) HT-29 adenocarcinoma cells, and early-passage Caco2 adenocarcinoma cells were processed for protein analysis. In brief, all the cells grown on six-well plates were washed once with ice-cold phosphate-buffered saline containing 1 mmol/l sodium orthovanadate and 25 mmol/l NaF, then 100 µl of ice-cold lysis buffer was added (20 mmol/l Tris HCl, pH 7.4, 150 mmol/l NaCl, 1 mmol/l EDTA, 1 mmol/l ethyleneglycol-bis(baminoethylether)-N,N9-tetraacetic acid, 25 mmol/l NaF, 1% Triton X-100, 10% glycerol, 1 mmol/l dithiothreitol, 1 mmol/l sodium vanadate, 50 mmol/l glycerophosphate, and 10 µg/ml of aprotinin, leupeptin, calpain inhibitior, and Pefabloc (100 µg/ml), the last being freshly made). After being sonicated for 5 s, lysates were centrifuged at 10,000g for 10 min at 4 °C. Protein concentrations were assessed (HEK-CaSR, HT-29 cells 100 µg; Caco2, 200 µg). Each aliquot was mixed with 2X-SDS-Laemmli gel–loading buffer containing 100 mmol/l dithiothreitol and denatured at 65 °C for 30 min. Proteins were resolved electrophoretically on a 6.5% acrylamide gel in running buffer and transferred to an Immobilon membrane (Millipore, Billerica, MA). Membranes were first blocked for 1 h at room temperature in phosphate-buffered saline containing 0.25% TritonX-100 and 5% dry milk, then incubated with anti-CaSR antibody (Abnova, Walnut, CA) at 1:400 in phosphate-buffered saline with 0.25% TritonX-100 and 1% dry milk overnight at 4 °C. Blots were washed five times for 10 min at room temperature with phosphate-buffered saline with 1% TritonX-100 and 0.15% dry milk, then incubated for 1 h with a secondary antibody conjugated with horseradish peroxidase (1:2,000) in blocking solution. Blots were washed a second time (5 × 10 min) and the bands were visualized by chemiluminescence according to the manufacturer’s instructions (SuperSignal: Pierce Biotechnology, Rockford, IL). Blots were stripped and reprobed with anti-β-actin (Sigma Chemical, St. Louis, MO) at a dilution of 1:500.
Cell Stimulation and Protein Analysis
Adherent Caco2, HEK-WT, and WT HEK cells stably (HEK-CaSR) or transiently transfected (HEK-T) with CaSR were stimulated by adding PA, Mr5,000–15,000 (Sigma Chemical), calcium, or human recombinant epidermal growth factor (Gibco) directly to the media overlying cells in a six-well plate for indicated times. Cells were then lysed and immunoblotted with ppERK1/2 antibody (Cell Signaling, Beverly, MA) as above. Before stimulation, cells were deprived of calcium and serum using high-glucose Dulbecco’s Modified Eagle Medium without pyridoxine, L-glutamine, or sodium pyruvate (Gibco) and then supplemented with 0.5 mmol/l Ca and 1% fetal bovine serum for 12 h. Total and pERK 1/2 from cell lysates were quantified using the chemiluminescent Meso Scale Discovery phospho (T/Y: 202/204; 185/187)/total ERK 1/2 Multi-Spot Assay System (Meso Scale Diagnostics, Gaithersburg, MD). Percentage of ERK 1/2 phosphorylation was calculated according to the manufacturer’s instructions.
Collagen Lattice Contraction Assay
Cell-populated collagen lattices were prepared using previously reported methods (5). Briefly, collagen solution (3 mg/ml) was made by solubilizing type I rat tail collagen (Sigma, St. Louis, MO) in 0.1% acetic acid. AML14.3D10 cells in suspension and trypsinized, suspended HEK and Caco2 cells were mixed as described with 3 mg/ml collagen solution and a titrated volume of NaOH to produce a solidified cell–populated collagen lattice with neutral pH and cell concentrations of 5 × 105 cells/ml. Lattices of 0.5 ml were poured into wells of a 24-well plate (Costar; Corning, Corning, NY) to solidify. After 30 min, 0.5 ml of culture medium was laid over the lattices, and then lattices were freed from the well walls with a pipette tip. Images were acquired at specific time points following lattice solidification with a digital camera at a fixed distance from the lattice, and surface area was calculated using ImageJ software v. 1.32 (http://rsb.info.nih.gov/ij/; National Institutes of Health, Bethesda, MD). Results are reported as a percentage of initial lattice surface area or as a percentage contraction (100, percentage initial surface area). Lattices were stimulated with PA Mr5,000–15,000 (Sigma) by using prepared medium with indicated concentration of PA to resuspend cells and in media overlaying lattices.
Transient Transfection
HEK293 cells were transiently transfected with full-length CaSR cDNA clone in pCMV6-XL4 vector or vector alone (Origene Technologies, Rockville MD) using Polyfect according to the manufacturer’s instructions (QIAGEN, Valencia, CA).
Assessment of Gene-Specific mRNA
Transcriptional analysis of HEK cells for expression of human CaSR was assessed by analyses of RNA from monolayers of HEK cells. Reverse transcription-PCR analysis of mRNA was performed from total RNA as described previously (29), but intron-spanning primers specific for CaSR (forward primer 5′-TAT AGC TGC TGC TGG GTC CT-3′ and reverse primer 5′-GCT GGG CTG CTG TTT ATC TC-3′; 248-bp fragment) or control β-actin (forward primer 5′-GGA GAA AAT CTG GCA CCA CAC C-3′ and reverse primer 5′-CCA CAT CAG CTG GAA GGT GG-3′; 133-bp fragment) were used. Each primer was amplified using 35 cycles of PCR at 94 °C for 30 s, 58 °C for 45 s, and 72 °C for 1 min with a final extension of 72 °C for 7 min. PCRs were then visualized on a 1.5% agarose gel containing 5 μg/ml ethidium bromide.
Data Analysis
Data are summarized as mean ± SD. Statistical analyses of results were performed by using unpaired Student’s t-tests. P < 0.05 was considered to be significant.
Statement of Financial Support
This work was supported by grants from the National Institutes of Health (RO1 DK 62245 to G.T.F. and T32 DK067009 to V.M.) and the Shell/Mandell Family (to G.T.F.).
References
Furuta GT, Nieuwenhuis EE, Karhausen J, et al. Eosinophils alter colonic epithelial barrier function: role for major basic protein. Am J Physiol Gastrointest Liver Physiol 2005;289:G890–7.
Rothenberg ME, Hogan SP . The eosinophil. Annu Rev Immunol 2006;24:147–74.
Zagai U, Dadfar E, Lundahl J, Venge P, Sköld CM . Eosinophil cationic protein stimulates TGF-beta1 release by human lung fibroblasts in vitro. Inflammation 2007;30:153–60.
Turck CW, Dohlman JG, Goetzl EJ . Immunological mediators of wound healing and fibrosis. J Cell Physiol Suppl 1987:Suppl 5:89–93.
Ngo P, Ramalingam P, Phillips JA, Furuta GT . Collagen gel contraction assay. Methods Mol Biol 2006;341:103–9.
Brown EM, MacLeod RJ . Extracellular calcium sensing and extracellular calcium signaling. Physiol Rev 2001;81:239–97.
Justinich CJ, Mak N, Pacheco I, et al. The extracellular calcium-sensing receptor (CaSR) on human esophagus and evidence of expression of the CaSR on the esophageal epithelial cell line (HET-1A). Am J Physiol Gastrointest Liver Physiol 2008;294:G120–9.
Buchan AM, Squires PE, Ring M, Meloche RM . Mechanism of action of the calcium-sensing receptor in human antral gastrin cells. Gastroenterology 2001;120:1128–39.
Cheng I, Qureshi I, Chattopadhyay N, et al. Expression of an extracellular calcium-sensing receptor in rat stomach. Gastroenterology 1999;116:118–26.
Feng J, Petersen CD, Coy DH, et al. Calcium-sensing receptor is a physiologic multimodal chemosensor regulating gastric G-cell growth and gastrin secretion. Proc Natl Acad Sci USA 2010;107:17791–6.
Liou AP, Sei Y, Zhao X, et al. The extracellular calcium-sensing receptor is required for cholecystokinin secretion in response to L-phenylalanine in acutely isolated intestinal I cells. Am J Physiol Gastrointest Liver Physiol 2011;300:G538–46.
Geibel J, Sritharan K, Geibel R, et al. Calcium-sensing receptor abrogates secretagogue- induced increases in intestinal net fluid secretion by enhancing cyclic nucleotide destruction. Proc Natl Acad Sci USA 2006;103:9390–7.
Chen Y, Shi-Wen X, van Beek J, et al. Matrix contraction by dermal fibroblasts requires transforming growth factor-beta/activin-linked kinase 5, heparan sulfate-containing proteoglycans, and MEK/ERK: insights into pathological scarring in chronic fibrotic disease. Am J Pathol 2005;167:1699–711.
Chen Y, Leask A, Abraham DJ, et al. Heparan sulfate–dependent ERK activation contributes to the overexpression of fibrotic proteins and enhanced contraction by scleroderma fibroblasts. Arthritis Rheum 2008;58:577–85.
Hirano S, Rees RS, Gilmont RR . MAP kinase pathways involving hsp27 regulate fibroblast-mediated wound contraction. J Surg Res 2002;102:77–84.
Mulder DJ, Pacheco I, Hurlbut DJ, et al. FGF9-induced proliferative response to eosinophilic inflammation in oesophagitis. Gut 2009;58:166–73.
Hofer AM, Gerbino A, Caroppo R, Curci S . The extracellular calcium-sensing receptor and cell-cell signaling in epithelia. Cell Calcium 2004;35:297–306.
Woodruff SA, Masterson JC, Fillon S, Robinson ZD, Furuta GT . Role of eosinophils in inflammatory bowel and gastrointestinal diseases. J Pediatr Gastroenterol Nutr 2011;52:650–61.
Masterson JC, Furuta GT, Lee JJ . Update on clinical and immunological features of eosinophilic gastrointestinal diseases. Curr Opin Gastroenterol 2011;27:515–22.
Liu X, Umino T, Cano M, et al. Human bronchial epithelial cells can contract type I collagen gels. Am J Physiol 1998;274(1 Pt 1):L58–65.
Young JD, Peterson CG, Venge P, Cohn ZA . Mechanism of membrane damage mediated by human eosinophil cationic protein. Nature 1986;321:613–6.
Furuta GT, Ackerman SJ, Varga J, Spiess AM, Wang MY, Wershil BK . Eosinophil granule-derived major basic protein induces IL-8 expression in human intestinal myofibroblasts. Clin Exp Immunol 2000;122:35–40.
MacLeod RJ, Hayes M, Pacheco I . Wnt5a secretion stimulated by the extracellular calcium-sensing receptor inhibits defective Wnt signaling in colon cancer cells. Am J Physiol Gastrointest Liver Physiol 2007;293:G403–11.
Peiris D, Pacheco I, Spencer C, MacLeod RJ . The extracellular calcium-sensing receptor reciprocally regulates the secretion of BMP-2 and the BMP antagonist Noggin in colonic myofibroblasts. Am J Physiol Gastrointest Liver Physiol 2007;292:G753–66.
MacLeod RJ, Chattopadhyay N, Brown EM . PTHrP stimulated by the calcium-sensing receptor requires MAP kinase activation. Am J Physiol Endocrinol Metab 2003;284:E435–42.
Zhang Z, Qiu W, Quinn SJ, Conigrave AD, Brown EM, Bai M . Three adjacent serines in the extracellular domains of the CaR are required for L-amino acid-mediated potentiation of receptor function. J Biol Chem 2002;277:33727–35.
Zhang Z, Jiang Y, Quinn SJ, Krapcho K, Nemeth EF, Bai M . L-phenylalanine and NPS R-467 synergistically potentiate the function of the extracellular calcium-sensing receptor through distinct sites. J Biol Chem 2002;277:33736–41.
Hizaki K, Yamamoto H, Taniguchi H, et al. Epigenetic inactivation of calcium-sensing receptor in colorectal carcinogenesis. Mod Pathol 2011;24:876–84.
Furuta GT, Turner JR, Taylor CT, et al. Hypoxia-inducible factor 1-dependent induction of intestinal trefoil factor protects barrier function during hypoxia. J Exp Med 2001;193:1027–34.
Acknowledgements
The authors acknowledge the excellent technical assistance and expertise of Jonathan Phillips, Joanne Masterson, and Raina Ficherova and the generous advice and support of Sean P. Colgan. R.J.M. holds the Canada Research Chair in GI Cell Physiology.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary Figure S1
(TIFF 833 kb)
Rights and permissions
About this article
Cite this article
Ngo, P., MacLeod, R., Mukkada, V. et al. Epithelial calcium–sensing receptor activation by eosinophil granule protein analog stimulates collagen matrix contraction. Pediatr Res 73, 414–419 (2013). https://doi.org/10.1038/pr.2012.198
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2012.198