Abstract
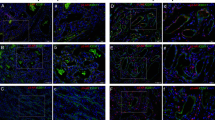
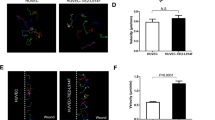
Infantile hemangiomas are localized and rapidly growing regions of disorganized angiogenesis. We show that expression of vascular endothelial growth factor receptor-1 (VEGFR1) in hemangioma endothelial cells (hemECs) and hemangioma tissue is markedly reduced compared to controls. Low VEGFR1 expression in hemECs results in VEGF-dependent activation of VEGFR2 and downstream signaling pathways. In hemECs, transcription of the gene encoding VEGFR1 (FLT1) is dependent on nuclear factor of activated T cells (NFAT). Low VEGFR1 expression in hemECs is caused by reduced activity of a pathway involving β1 integrin, the integrin-like receptor tumor endothelial marker-8 (TEM8), VEGFR2 and NFAT. In a subset of individuals with hemangioma, we found missense mutations in the genes encoding VEGFR2 (KDR) and TEM8 (ANTXR1). These mutations result in increased interactions among VEGFR2, TEM8 and β1 integrin proteins and in inhibition of integrin activity. Normalization of the constitutive VEGFR2 signaling in hemECs with soluble VEGFR1 or antibodies that neutralize VEGF or stimulate β1 integrin suggests that local administration of these or similar agents may be effective in hemangioma treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Boye, E. et al. Clonality and altered behavior of endothelial cells from hemangiomas. J. Clin. Invest. 107, 745–752 (2001).
Mulliken, J. & Young, A. Vascular Birthmarks: Hemangiomas and Malformations (W. B. Saunders Company, Philadelphia, 1988).
Mulliken, J.B. Cutaneous vascular anomalies. Semin. Vasc. Surg. 6, 204–218 (1993).
Walter, J.W. et al. Somatic mutation of vascular endothelial growth factor receptors in juvenile hemangioma. Genes Chromosom. Cancer 33, 295–303 (2002).
North, P.E., Waner, M., Mizeracki, A. & Mihm, M.C., Jr. GLUT1: a newly discovered immunohistochemical marker for juvenile hemangiomas. Hum. Pathol. 31, 11–22 (2000).
Li, Q., Yu, Y., Bischoff, J., Mulliken, J.B. & Olsen, B.R. Differential expression of CD146 in tissues and endothelial cells derived from infantile hemangiomas and normal human skin. J. Pathol. 201, 296–302 (2003).
Barnes, C.M. et al. Evidence by molecular profiling for a placental origin of infantile hemangioma. Proc. Natl. Acad. Sci. USA 102, 19097–19102 (2005).
North, P.E. et al. A unique microvascular phenotype shared by juvenile hemangiomas and human placenta. Arch. Dermatol. 137, 559–570 (2001).
Chiller, K.G., Passaro, D. & Frieden, I.J. Hemangiomas of infancy: clinical characteristics, morphologic subtypes, and their relationship to race, ethnicity and sex. Arch. Dermatol. 138, 1567–1576 (2002).
Haggstrom, A.N. et al. Prospective study of infantile hemangiomas: demographic, prenatal and perinatal characteristics. J. Pediatr. 150, 291–294 (2007).
Ferrara, N. The role of VEGF in the regulation of physiological and pathological angiogenesis. EXS 94, 209–231 (2005).
Roberts, D.M. et al. The vascular endothelial growth factor (VEGF) receptor Flt-1 (VEGFR-1) modulates Flk-1 (VEGFR-2) signaling during blood vessel formation. Am. J. Pathol. 164, 1531–1535 (2004).
Bradley, K.A., Mogridge, J., Mourez, M., Collier, R.J. & Young, J.A. Identification of the cellular receptor for anthrax toxin. Nature 414, 225–229 (2001).
Werner, E., Kowalczyk, A.P. & Faundez, V. Anthrax toxin receptor 1/tumor endothelium marker 8 mediates cell spreading by coupling extracellular ligands to the actin cytoskeleton. J. Biol. Chem. 281, 23227–23236 (2006).
Inoue, T. et al. Identification of a vascular endothelial growth factor (VEGF) antagonist, sFlt-1, from a human hematopoietic cell line NALM-16. FEBS Lett. 469, 14–18 (2000).
Ito, N., Huang, K. & Claesson-Welsh, L. Signal transduction by VEGF receptor-1 wild type and mutant proteins. Cell. Signal. 13, 849–854 (2001).
Wakiya, K., Begue, A., Stehelin, D. & Shibuya, M. A cAMP response element and an Ets motif are involved in the transcriptional regulation of flt-1 tyrosine kinase (vascular endothelial growth factor receptor 1) gene. J. Biol. Chem. 271, 30823–30828 (1996).
Hogan, P.G., Chen, L., Nardone, J. & Rao, A. Transcriptional regulation by calcium, calcineurin and NFAT. Genes Dev. 17, 2205–2232 (2003).
Hesser, B.A. et al. Down syndrome critical region protein 1 (DSCR1), a novel VEGF target gene that regulates expression of inflammatory markers on activated endothelial cells. Blood 104, 149–158 (2004).
Hernandez, G.L. et al. Selective inhibition of vascular endothelial growth factor-mediated angiogenesis by cyclosporin A: roles of the nuclear factor of activated T cells and cyclooxygenase 2. J. Exp. Med. 193, 607–620 (2001).
Satonaka, H. et al. Calcineurin promotes the expression of monocyte chemoattractant protein-1 in vascular myocytes and mediates vascular inflammation. Circ. Res. 94, 693–700 (2004).
Schwartz, M.A. Spreading of human endothelial cells on fibronectin or vitronectin triggers elevation of intracellular free calcium. J. Cell Biol. 120, 1003–1010 (1993).
Leavesley, D.I., Schwartz, M.A., Rosenfeld, M. & Cheresh, D.A. Integrin β1- and β3-mediated endothelial cell migration is triggered through distinct signaling mechanisms. J. Cell Biol. 121, 163–170 (1993).
Jones, N.P., Peak, J., Brader, S., Eccles, S.A. & Katan, M. PLCγ1 is essential for early events in integrin signalling required for cell motility. J. Cell Sci. 118, 2695–2706 (2005).
Aplin, A.E., Howe, A., Alahari, S.K. & Juliano, R.L. Signal transduction and signal modulation by cell adhesion receptors: the role of integrins, cadherins, immunoglobulin-cell adhesion molecules and selectins. Pharmacol. Rev. 50, 197–263 (1998).
Sjaastad, M.D. & Nelson, W.J. Integrin-mediated calcium signaling and regulation of cell adhesion by intracellular calcium. Bioessays 19, 47–55 (1997).
Luque, A. et al. Activated conformations of very late activation integrins detected by a group of antibodies (HUTS) specific for a novel regulatory region (355–425) of the common β1 chain. J. Biol. Chem. 271, 11067–11075 (1996).
Schaller, M.D. & Parsons, J.T. Focal adhesion kinase and associated proteins. Curr. Opin. Cell Biol. 6, 705–710 (1994).
Guan, J.-L. & Shalloway, D. Regulation of focal adhesion-associated protein tyrosine kinase by both cellular adhesion and oncogenic transformation. Nature 358, 690–692 (1992).
Abu-Ghazaleh, R., Kabir, J., Jia, H., Lobo, M. & Zachary, I. Src mediates stimulation by vascular endothelial growth factor of the phosphorylation of focal adhesion kinase at tyrosine 861 and migration and anti-apoptosis in endothelial cells. Biochem. J. 360, 255–264 (2001).
Blei, F., Walter, J., Orlow, S.J. & Marchuk, D.A. Familial segregation of hemangiomas and vascular malformations as an autosomal dominant trait. Arch. Dermatol. 134, 718–722 (1998).
Shinkai, A. et al. Mapping of the sites involved in ligand association and dissociation at the extracellular domain of the kinase insert domain-containing receptor for vascular endothelial growth factor. J. Biol. Chem. 273, 31283–31288 (1998).
Kuriyama, M. et al. Activation and translocation of PKCδ is necessary for VEGF-induced ERK activation through KDR in HEK293T cells. Biochem. Biophys. Res. Commun. 325, 843–851 (2004).
Sun, Y. et al. The kinase insert domain-containing receptor is an angiogenesis-associated antigen recognized by human cytotoxic T lymphocytes. Blood 107, 1476–1483 (2006).
Shenoy, P.S. et al. beta1 Integrin-extracellular matrix protein interaction modulates the migratory response to chemokine stimulation. Biochem. Cell Biol. 79, 399–407 (2001).
Vikkula, M. et al. Vascular dysmorphogenesis caused by an activating mutation in the receptor tyrosine kinase TIE2. Cell 87, 1181–1190 (1996).
Brouillard, P. et al. Four common glomulin mutations cause two thirds of glomuvenous malformations (“familial glomangiomas”): evidence for a founder effect. J. Med. Genet. 42, e13 (2005).
North, P.E., Waner, M., Buckmiller, L., James, C.A. & Mihm, M.C. Jr. Vascular tumors of infancy and childhood: beyond capillary hemangioma. Cardiovasc. Pathol. 15, 303–317 (2006).
Ritter, M.R., Reinisch, J., Friedlander, S.F. & Friedlander, M. Myeloid cells in infantile hemangioma. Am. J. Pathol. 168, 621–628 (2006).
Takahashi, K. et al. Cellular markers that distinguish the phases of hemangioma during infancy and childhood. J. Clin. Invest. 93, 2357–2364 (1994).
Razon, M.J., Kräling, B.M., Mulliken, J.B. & Bischoff, J. Increased apoptosis coincides with onset of involution in infantile hemangioma. Microcirculation 5, 189–195 (1998).
Akuzawa, N., Kurabayashi, M., Ohyama, Y., Arai, M. & Nagai, R. Zinc finger transcription factor Egr-1 activates Flt-1 gene expression in THP-1 cells on induction for macrophage differentiation. Arterioscler. Thromb. Vasc. Biol. 20, 377–384 (2000).
Fragoso, R. et al. VEGFR-1 (FLT-1) activation modulates acute lymphoblastic leukemia localization and survival within the bone marrow, determining the onset of extramedullary disease. Blood 107, 1608–1616 (2006).
Claesson-Welsh, L. Signal transduction by vascular endothelial growth factor receptors. Biochem. Soc. Trans. 31, 20–24 (2003).
Liu, S. & Leppla, S.H. Cell surface tumor endothelium marker 8 cytoplasmic tail-independent anthrax toxin binding, proteolytic processing, oligomer formation and internalization. J. Biol. Chem. 278, 5227–5234 (2003).
Kitamura, T. et al. Retrovirus-mediated gene transfer and expression cloning: powerful tools in functional genomics. Exp. Hematol. 31, 1007–1014 (2003).
Khan, Z.A. et al. Endothelial progenitor cells from infantile hemangioma and umbilical cord blood display unique cellular responses to endostatin. Blood 108, 915–921 (2006).
Picard, A. et al. IFG-2 and FLT-1/VEGF-R1 mRNA levels reveal distinctions and similarities between congenital and common infantile hemangioma. Pediatr. Res. 63, 263–267 (2008).
Acknowledgements
This work was supported by the John B. Mulliken Foundation and grants AR36820 and AR48564 from the US National Institutes of Health (to B.R.O.). We are indebted to J.B. Mulliken (Children's Hospital, Boston) and L. Boon (Universite Catholique de Louvain) for providing essential surgical material (control and hemangioma tissues and blood samples) for these studies. We thank N.A. Clipstone (Feinberg School of Medicine, Northwestern University) for providing the constitutively active form of NFATc1, M. Kurabayashi (Gunma University Graduate School of Medicine) for providing the promoter construct for FLT1, S. Dias (Instituto Portugues de Oncologia Francisco Gentil) for providing expression vectors for FLT1, L. Claesson-Welsh (Uppsala University) for providing expression vectors for KDR and mutant FLT1, S. Liu (US National Institute of Allergy and Infectious Diseases) for providing expression vector for ANTXR1 and T. Kitamura (University of Tokyo,) for the pMXs vector. We thank R. Ruijtenbeek and R. Houtman (both from PamGene Corporation) for providing reagents and equipment for kinase arrays, F. Naji and M. Dankers for kinase array bioinformatics assistance, T. Rector for assistance with protein multiplexing, J. Eastcott and J. Wylie-Sears for flow cytometry and technical assistance, S. Feske (New York University School of Medicine) for antibody to NFATc2 (clone 67.1) and advice and W. Kuo for technical advice. We thank Y. Pittel, S. Plotkina, N. Liu, A. Heilmann, Y. Ishida and Y. Yamamura for technical assistance and D. Glotzer for comments and advice on the manuscript.
Author information
Authors and Affiliations
Contributions
M.J., cell signaling studies, immunoblotting and immunoprecipitation analyses, transcription and promoter studies, integrin studies; D.M., multiplex ELISA and kinase assays, proliferation and migration analyses; L.P., sequencing of candidate genes; N.L., allele-specific DNA sequencing; Y.L., initial signaling studies; E. Boscolo, hemangioma tissue characterization; J.B., isolation of hemEC lines, control cells and tissues; M.V., collection of control and hemangioma tissues and DNAs; E. Boye, planning, NFAT and Ca2+ studies; B.R.O., planning and directing the study, manuscript writing.
Note: Supplementary information is available on the Nature Medicine website.
Corresponding authors
Supplementary information
Supplementary Text and Figures
Supplementary Figs. 1–5, Supplementary Tables 1–3 and Supplementary Methods (PDF 833 kb)
Rights and permissions
About this article
Cite this article
Jinnin, M., Medici, D., Park, L. et al. Suppressed NFAT-dependent VEGFR1 expression and constitutive VEGFR2 signaling in infantile hemangioma. Nat Med 14, 1236–1246 (2008). https://doi.org/10.1038/nm.1877
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.1877
This article is cited by
-
Molecular basis of VEGFR1 autoinhibition at the plasma membrane
Nature Communications (2024)
-
Computational prognostic evaluation of Alzheimer’s drugs from FDA-approved database through structural conformational dynamics and drug repositioning approaches
Scientific Reports (2023)
-
Vascular Anomalies of the Head and Neck: A Pediatric Overview
Head and Neck Pathology (2021)
-
VEGF/Flk1 Mechanism is Involved in Roxarsone Promotion of Rat Endothelial Cell Growth and B16F10 Xenograft Tumor Angiogenesis
Scientific Reports (2019)