Abstract
Increases in brain blood flow, evoked by neuronal activity, power neural computation and form the basis of BOLD (blood-oxygen-level-dependent) functional imaging. Whether blood flow is controlled solely by arteriole smooth muscle, or also by capillary pericytes, is controversial. We demonstrate that neuronal activity and the neurotransmitter glutamate evoke the release of messengers that dilate capillaries by actively relaxing pericytes. Dilation is mediated by prostaglandin E2, but requires nitric oxide release to suppress vasoconstricting 20-HETE synthesis. In vivo, when sensory input increases blood flow, capillaries dilate before arterioles and are estimated to produce 84% of the blood flow increase. In pathology, ischaemia evokes capillary constriction by pericytes. We show that this is followed by pericyte death in rigor, which may irreversibly constrict capillaries and damage the blood–brain barrier. Thus, pericytes are major regulators of cerebral blood flow and initiators of functional imaging signals. Prevention of pericyte constriction and death may reduce the long-lasting blood flow decrease that damages neurons after stroke.
Similar content being viewed by others
Main
Pericytes are isolated contractile cells on capillaries that may regulate cerebral blood flow1,2, in addition to stabilizing newly formed capillaries3, maintaining the blood–brain barrier4,5,6, contributing to the ‘glial scar’ in pathology7, and having stem cell properties8. Pericytes can be constricted and dilated by neurotransmitters in vitro1,9, through poorly understood signalling pathways, and capillary blood flow heterogeneity might reflect differences in pericyte tone10,11,12. Pericytes can constrict in vivo, but it was suggested2 that they do not relax actively to increase blood flow13. Similar controversy surrounds the effect of pericytes on blood flow in pathology14,15. We have now characterized the responses of pericytes in the neocortex and cerebellum to neuronal activity and ischaemia. We demonstrate that, unexpectedly, pericytes are the first vascular elements to dilate during neuronal activity, making them the initiators of functional imaging signals. Furthermore, they die readily in ischaemia, and this is expected to promote brain damage.
Signals that regulate pericyte dilation
We assessed the signalling systems that dilate molecular layer capillaries in cerebellar slices1, using 95% or 20% O2 in the superfusate to produce a supra-normal or a physiological O2 concentration, [O2], in the slice16,17. Capillaries were defined as vessels of less than 10 μm diameter and lacking a continuous layer of smooth muscle. Their diameter was larger (P = 0.00023) at the lower [O2] (5.36 ± 0.30 μm (mean ± s.e.m., n = 59) in 20%, and 4.07 ± 0.14 μm (n = 154) in 95% O2). Capillary pericytes can be identified by labelling for the chondroitin sulphate proteoglycan NG2 or the PDGFRβ receptor (Fig. 1a), or using mice expressing DsRed under control of the NG2 promoter18 (Fig. 1b, c), and are a different cell class from Iba1-expressing perivascular microglia or macrophages19 (Fig. 1c). For neocortical capillaries in postnatal day 21 (P21) rats the pericyte soma density was 2.2 ± 0.2 per 100 μm of capillary length (950 μm of capillary analysed in each of 11 confocal stacks). Pericytes extend processes along and around vessels (Fig. 1a–c), which regulate capillary diameter.
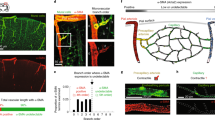
a, Capillaries in the molecular layer of rat cerebellum labelled using isolectin B4; pericytes (arrows) labelled with NG2 or PDGFRβ antibodies. b, Cerebellar capillaries in NG2-DsRed mouse; pericytes are red. c, Neocortical capillaries in NG2-DsRed mouse; microglia labelled for Iba1. d, Rat cerebellar capillary response to 2 μM noradrenaline (NA) and superimposed 500 μM glutamate (Glut). Line shows lumen diameter. e, NA-evoked prolonged constriction (95% O2; a large constriction is shown for clarity). f, Diameter in NA was not affected by [O2] (graphs show percentage of baseline diameter before drugs). g, Glutamate dilates capillaries (20% O2; a large dilation is shown for clarity). h, Dilation was larger in low [O2]. i, NOS blocker L-NNA (100 μM) inhibits Glut-evoked dilation (20% O2). j, Guanylyl cyclase blocker ODQ (10 μM) does not block dilation (20% O2). k, Blocking 20-HETE production (HET0016, 1 μM) abolishes the inhibitory effect of L-NNA (20% O2). l, L-NNA reduces glutamate-evoked dilations at high and low [O2] (P = 0.002, ANOVA on all data; P values at each [O2] from post-hoc t-tests). m ODQ does not affect glutamate-evoked dilation. n, HET0016 abolishes effect of L-NNA. o, p, Blocking EP4 receptors (L161,982, 1 μM) inhibits glutamate-evoked dilation (o, 20% O2) at high and low [O2] (p). Data in d–p are from rat cerebellar capillaries. q, EP4 block abolishes glutamate-evoked dilation in rat neocortical capillaries (20% O2). Drug effects on baseline diameter are in Extended Data Fig. 2. Data shown as mean ± s.e.m.
The capillary diameter was extremely stable over the course of 60 min if no drugs were applied (see below). Application of noradrenaline (2 μM), to mimic its release from the locus coeruleus in vivo, produced a sustained constriction mediated by pericytes1 (Fig. 1d, e), that was not affected by [O2] (Fig. 1f). Superimposing glutamate (500 μM), to mimic neuronal glutamate release13, dilated capillaries at pericyte locations1 (Fig. 1d, g and Supplementary Video 1). As a percentage of the diameter without drugs, this dilation was twice as large with 20% as with 95% O2 (Fig. 1h), possibly due to less production of vasoconstricting 20-HETE (20-hydroxyeicosatetraenoic acid) in low [O2] (see below and Extended Data Fig. 1). Independent of [O2], most pericytes (72% in 95% O2; 70% in 20% O2) constricted >5% to noradrenaline, and dilated >5% to glutamate (63% in 95% O2 (n = 154); 66% in 20% O2 (n = 59)), and most pericytes that constricted to noradrenaline also dilated to glutamate (71% in 95% O2; 78% in 20% O2). Glutamate also dilated some capillaries in the absence of noradrenaline: in 20% O2, 29% (7/24) of pericytes dilated >5%, which is less (P = 0.005, chi-squared test) than the 66% of pericytes that dilated >5% after applying noradrenaline. In subsequent experiments noradrenaline was used to pre-constrict capillaries, to aid analysis of the signalling underlying glutamate-evoked dilation.
These experiments do not establish which cells the noradrenaline and glutamate act on (they may be neurons, astrocytes or pericytes themselves13) to release the downstream messengers that control pericyte tone. However, we can rule out the idea that noradrenaline generates 20-HETE to constrict pericytes, because blocking 20-HETE synthesis with 1 μM HET0016 did not affect the noradrenaline-evoked constriction (Extended Data Fig. 2b, g).
Glutamate releases nitric oxide (NO), a vasodilator, by activating NMDA (N-methyl-d-aspartate) receptors13 and an NO donor (DETA-NONOate, 100 μM) evoked capillary dilation (Extended Data Fig. 2m). Blocking NO synthase with L-NG-nitroarginine (L-NNA, 100 μM) reduced the glutamate-evoked dilation (Fig. 1i, l; P = 0.002 from analysis of variance (ANOVA); L-NNA and other blockers used did not inhibit the noradrenaline-evoked constriction, see Extended Data Fig. 2). Unexpectedly, the dilation was not affected by blocking guanylyl cyclase with ODQ (1H-[1,2,4]Oxadiazolo[4,3-a]quinoxalin-1-one, 10 μM, P = 1, ANOVA), so NO does not act by raising [cGMP] in the pericyte (Fig. 1j, m and Extended Data Fig. 2e). However, when production of vasoconstricting 20-HETE was blocked using HET0016 (1μM), L-NNA no longer inhibited the dilation (Fig. 1k, n; P = 0.0005 from ANOVA on black bars in l and n), implying that NO promotes dilation by preventing 20-HETE formation. As a robust dilation occurs with both NO and 20-HETE synthesis blocked (Fig. 1k, n), another messenger must be active. Blocking synthesis of epoxy derivatives of arachidonic acid with the inhibitor MS-PPOH (10 μM) did not affect the dilation (Extended Data Fig. 2i, ANOVA P = 0.92), but blocking EP4 receptors for prostaglandin E2 (with 1 μM L-161,982) greatly reduced it (Fig. 1o–p, P = 0.001, ANOVA). A similar inhibition of capillary dilation by blocking EP4 receptors was seen in neocortical pericytes (Fig. 1q, P = 0.004). Application of prostaglandin E2 (PGE2) itself dilated cerebellar capillaries (Extended Data Fig. 2n). We therefore identify the messenger that dilates capillaries in response to glutamate as prostaglandin E2 (or a related species active at EP4 receptors), but this dilation requires NO release to suppress 20-HETE formation (Extended Data Fig. 1b).
Glutamate (500 μM) or NMDA (100 μM) (Fig. 2a, b, d), or parallel fibre stimulation (Fig. 2c, d), evoked an outward membrane current in pericytes patch-clamped at −55 to −75 mV (sometimes preceded by a small inward current; Extended Data Fig. 3). The stimulation-evoked outward current was inhibited (P = 0.005, paired t-test) by blocking action potentials with tetrodotoxin (TTX) (Fig. 2c, reduced to 15 ± 12% (n = 4) of its amplitude without TTX, not significantly different from zero, P = 0.28), whereas the NMDA-evoked current was unaffected by TTX (reduced by 12 ± 19%, n = 5, P = 0.56), consistent with stimulation evoking the outward current by generating action potentials that release glutamate. The stimulation-evoked current of approximately 30 pA is expected to hyperpolarize the cells by approximately 9 mV (see Methods) and decrease voltage-gated Ca2+ entry, causing active relaxation9 (although other Ca2+ sources, and cyclic nucleotides, may also regulate contractile tone9,20). Indeed, parallel fibre stimulation produced a dilation of 14.9 ± 3.1% in 21 capillaries in 20% O2 (Fig. 2e–h and Supplementary Video 2), which (unlike the noradrenaline-evoked constriction) was blocked by TTX and by blocking EP4 receptors (Fig. 2g, h).
a, DsRed-labelled patch-clamped pericyte in molecular layer of mouse cerebellum. Lucifer yellow from pipette overlaps with DsRed. b, Glutamate (Glut, 500μM) and NMDA (100μM) evoked outward current (−55mV). c, Parallel fibre stimulation (Stim, 12 Hz)-evoked outward current (−74mV) is blocked by 1 μM TTX. d Mean outward currents evoked by stimulation, glutamate and NMDA (b–d are in 95% O2). e, f, Parallel fibre stimulation (in NA 1 μM) in rat cerebellar slice evokes capillary dilation (20% O2). g, h, Constriction by NA (g) was unaffected by TTX or EP4 block (L161,982), which abolished the stimulation-evoked dilation (h). P values from one-way ANOVA with Dunnett’s post-hoc tests. NA, noradrenaline. Data shown as mean ± s.e.m.
An outward current at negative potentials is not consistent with activation of glutamatergic ionotropic receptors, but is consistent with K+ current activation. These data suggest that glutamate release generates PGE2, which dilates the capillaries by activating an outward K+ current in pericytes. PGE2 similarly activates an outward K+ current in aortic smooth muscle21, and relaxes kidney pericytes22.
Pericytes increase blood flow in vivo
To assess whether pericyte relaxation regulates blood flow in vivo, we electrically stimulated the whisker pad (at 3 Hz) and used two-photon imaging of the vasculature (labelled with FITC-dextran) in somatosensory cortex to monitor dilations of penetrating arterioles (entering the cortex from the pia) and capillaries, in anaesthetized mice expressing DsRed in pericytes (Fig. 3a). The capillary diameter in vivo was 4.4 ± 0.1 μm in 633 capillary regions (Extended Data Table 1). Pericytes were visualized up to 200 μm deep in the cortex (layer 2/3). Brief whisker pad stimulation (2 s) evoked vessel dilations that peaked just after the end of the stimulation (∼2.5 s, Fig. 3b). Longer (15 s) stimulation produced dilations that initially followed the same time course, then dilated further throughout the stimulation (Fig. 3b and Extended Data Fig. 4). Most imaging employed 15 s stimuli, which increased the response magnitude and measurement accuracy. Repeated stimulation gave reproducible responses (Extended Data Fig. 5a, b). We segmented the vasculature by the branching order of the vessels, zero being the penetrating arteriole, one being the primary capillary branching off the arteriole, and so on (Extended Data Fig. 1; see Extended Data Table 1 for resting diameters, dilations and numbers of each vessel order). Whisker-pad stimulation dilated vessels of all orders (Fig. 3c and Extended Data Table 1). The fraction of vessels responding (that is, with a dilation >5%) was similar in penetrating arterioles and in first-order capillaries, whereas the frequency of capillary responses decreased with increasing order (Fig. 3c).
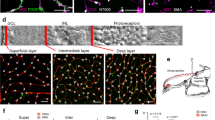
a, Confocal stack (90 μm thick, maximum intensity projection) of FITC-dextran-filled vessels in vivo in somatosensory cortex of NG2-DsRed mouse (pericytes are red). Enlargement (single image) shows a penetrating arteriole (0th order) giving off a capillary (first order) which splits into second-order branches. b, Response of 45 capillary regions to 2-s and 15-s whisker-pad stimulation. c, Percentage of vessel regions of different orders (number studied on bars) showing >5% dilation to stimulation. d, Simultaneous imaging (top, lines show measurement loci) of penetrating arteriole and first-order capillary: capillary dilates 3 s before arteriole (bottom, smoothing in d–g is explained in Methods and Extended Data Fig. 4). e, Dilation time course in simultaneously imaged penetrating arterioles and first-order capillaries. f, Time to 10% of peak dilation for (j–1)th order (third order for j ≥ 4) vessel minus that of jth-order vessel (j is an integer ≥ 1). Capillaries dilate faster than arterioles. g Dilation time course in all responding (>5%) penetrating arterioles and first- and second-order capillaries. Inset expands initial response. h, Time to 10% of peak dilation in all zero- to second-order responding vessels. i, Percentage of capillary locations with or without pericytes showing >5% dilations. j, Cumulative probability of capillary diameter changes (including ‘non-responding’ capillaries with <5% dilations) in 464 pericyte and 168 non-pericyte locations. Diameter changes <0% (constrictions) represent random changes and measurement error. k, Mean responses for distributions in j (P values from Mann–Whitney U-tests). Data shown as mean ± s.e.m.
To establish where vasodilation is initiated, we imaged different orders of vessel simultaneously. Strikingly, first-order capillaries usually dilated before penetrating arterioles (Fig. 3d, e and Supplementary Video 3), with vasodilation onset (assessed as the time to 10% of the maximum dilation) in the capillary being 1.38 ± 0.38 s earlier than for the penetrating arteriole (Fig. 3e, f, P = 0.015). Further along the vascular tree there was no significant difference in the time to dilation of simultaneously imaged capillaries of adjacent order (Fig. 3f and Extended Data Fig. 5c). Thus, capillaries dilate before the penetrating arteriole feeding them. Averaging over all vessels of the same order (not just those imaged simultaneously) showed a similar faster dilation of capillaries than of penetrating arterioles (Fig. 3g), with the time to 10% of the maximum dilation for penetrating arterioles (3.7 ± 0.3 s) being significantly longer than the values (∼2.7 s) obtained for first- and second-order capillaries (P = 0.040 and 0.039 respectively, Fig. 3h and Extended Data Fig. 5d). As expected, the time course of the blood flow increase in capillaries, assessed from the speed of red blood cell movement with line-scanning23, was similar to that of the capillary dilation (Extended Data Fig. 5f).
The faster dilation in capillaries compared to arterioles indicates that capillary dilation is not a passive response to a pressure increase produced by arteriole dilation. To assess whether pericytes generate this dilation, we measured the diameter changes of capillaries at locations where DsRed-labelled pericytes were present (either somata or processes, responses did not differ significantly at these locations; Extended Data Fig. 5e) or where no pericyte was visible. The resting diameter of capillaries was larger where pericyte somata or processes were present (4.62 ± 0.09 μm, n = 464) than in pericyte-free zones (3.72 ± 0.08 μm, n = 168, Mann–Whitney P = 2.7×10−7), suggesting that pericytes induce an increase of capillary diameter. Dilations over 5% were much more frequent at pericyte locations (Fig. 3i; P = 7.5× 10−11, chi-squared test), where the responses were also larger (P = 3.2× 10−5, Kolmogorov–Smirnov test; Fig. 3j, k). These data confirm that pericytes actively relax to generate the capillary dilation.
Pericytes constrict and die in ischaemia
A key question is whether pericyte control of capillary diameter also has a role in pathology. Pericytes constrict some retinal capillaries in ischaemia1, perhaps because pericyte [Ca2+]i rises when ion pumping is inhibited by ATP depletion. Cortical capillaries also constrict following middle cerebral artery occlusion14 (MCAO) in vivo. Clinically, reperfusion of thrombus-occluded arteries using tissue plasminogen activator can be achieved in 1 to 6 h24,25 but, even when arterial flow is restored, a long-lasting reduction of cerebral blood flow can ensue26,27,28,29. This may reflect pericyte constriction outlasting ischaemia14, but it is unclear why the constriction is so prolonged. We examined the effect of ischaemia on pericyte health using propidium iodide to mark cell death.
Live imaging of cerebral cortical slices exposed to simulated ischaemia (oxygen-glucose deprivation with ATP synthesis by glycolysis and oxidative phosphorylation inhibited with iodoacetate and antimycin) revealed that, within approximately 15 min, grey matter capillaries constricted at spatially restricted regions near pericytes (Fig. 4a–c). In contrast, the diameter of capillaries not exposed to ischaemia was stable over 60 min (reduced by 3.2 ± 3.0%, P = 0.31, n = 13; Fig. 4c). Although capillaries that were not exposed to ischaemia showed little pericyte death even after 1 hour (as assessed by propidium iodide labelling), ischaemia led to most pericytes on capillaries dying after approximately 40 min, usually at locations at which the earlier constriction had occurred. All capillaries exposed to ischaemia that we examined showed a consistent response, in which the pericytes first constricted the capillaries, and then died (Fig. 4c). Death of pericytes in rigor, after they have been constricted by a loss of energy supply, should produce a long-lasting increase in the resistance of the capillary bed.
a, Top, capillary in a P21 rat cortical slice in normal solution. Bottom, capillary exposed to simulated ischaemia. Right, propidium iodide (PI, 7.5 μM) labelling after one hour, showing dead pericytes (P) and an endothelial cell (EC). b, Vessel diameters at regions indicated in a, over time (red lines are for diameter near pericytes that die). c, Mean diameter and number of dead pericytes per 100 μm from nine capillaries in ischaemia (measured at 18 locations) and six capillaries in normal solution (13 locations). Diameter in ischaemia was reduced from control (P = 1.3×10−15 and 7.7 × 10−17 at 30 and 60 min). Pericyte death was higher in ischaemia at 40 and 60 min (P = 0.041 and 0.021, Mann–Whitney U-test). A few pericytes also died on capillaries in non-ischaemic slices, but did not constrict capillaries (1.3 ± 1.5% diameter decrease at three dead pericytes on two vessels). Data shown as mean ± s.e.m.
To sample more pericytes than is possible while live imaging the capillary diameter, and to examine mechanisms contributing to their death, we acquired confocal stacks of brain slices exposed to simulated ischaemia, which were then fixed and labelled for NG2 and/or isolectin B4. Ischaemia led to pericytes apposed to capillaries dying rapidly in both the white matter of the cerebellum (Fig. 5a, b) and the grey matter of the cerebral cortex (Fig. 5c, d). For pericytes exposed to simulated ischaemia as above, approximately 90% of pericytes died within 1 hour (Fig. 5b). This was unaffected by blocking action potentials (with TTX, 1μM) but was halved by blocking AMPA(α-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid)/kainate (25μM NBQX) or NMDA receptors (50μM D-AP5, 50μM MK-801 and 100μM 7-chlorokynurenate), implying an excitotoxic contribution to pericyte death. When oxygen-glucose deprivation (OGD) alone was used (without antimycin and iodoacetate), to allow ATP generation when oxygen and glucose were restored, approximately 40% of pericytes died after 1 hour, but OGD-evoked death increased 1.5-fold during 1 h of reperfusion (Fig. 5c, d). Ionotropic glutamate receptor block or removal of external Ca2+ again significantly reduced the death (Fig. 5d), while blocking NO production had a small protective effect and lowering free radical levels by scavenging O2·− had no significant effect (Fig. 5d and Extended Data Fig. 6a). Blocking metabotropic glutamate receptors or 20-HETE production, which might prevent [Ca2+]i rises, or blocking mitochondrial calcium uptake, also had no effect (Extended Data Fig. 6b).
a, Rat cerebellar slice white matter capillaries labelled for NG2 and propidium iodide (PI) after 1 h of control (white arrow, living pericyte) or ischaemia solution containing antimycin and iodoacetate (red arrow, dead pericyte). b, Percentage of pericytes dead in control or after 1 h ischaemia (as in a) alone or with block of action potentials (TTX, 1 μM), AMPA/kainate receptors (25 μM NBQX), or NMDA receptors (50 μM D-AP5, 50 μM MK-801, 100 μM 7-chlorokynurenate); P values from one-way ANOVA with Dunnett’s post-hoc tests. c, Rat neocortical slice grey matter capillaries labelled for IB4, NG2 and PI after 1 h of control solution or oxygen and glucose deprivation (OGD). d, Percentage of pericytes (as in c) dead after 1 h OGD (No-reoxy) or OGD followed by 1 h of control solution (Reoxy) with no drugs, or with iGluR block (NBQX (25 μM), AP5 (50 μM) and 7CK (100 μM)), zero [Ca2+]0, NOS block (100 μM L-NNA), or free radical scavenging (150 μM MnTBAP or 100 μM PBN, pooled data from Extended Data Fig. 5a) throughout. OGD killed pericytes (P = 10−13, ANOVA) and death increased during reperfusion (P = 3.3 ×10−13). iGluR block or zero [Ca2+]0 reduced death (P = 2.7 × 10−4 and 6.0 × 10−7, ANOVA with Dunnett’s post-hoc test). Blocking NOS had a small protective effect (P = 0.026); reactive oxygen species (ROS) scavenging did not (P = 0.99). e, f, Confocal images of striatal capillaries labelled with IB4 and PI (e) and percentage of striatal pericytes and endothelial cells that are dead (f) from the control and lesioned hemisphere of in vivo MCAO-treated rats (90 min, assessed 22.5 h later), sham-operated rats (with or without filament being inserted into the internal carotid artery (ICA)), and naive control animals. More pericytes die than endothelial cells (P = 10−6, repeated measures ANOVA). For pericytes, but not endothelial cells, cell death is greater in lesioned hemisphere (main effect of hemisphere, P = 0.004; hemisphere-cell type interaction P = 0.003) and cell death is greater in MCAO-lesioned animals than in naive or sham animals without ICA occlusion (P = 0.005 and 0.01, Tukey post-hoc tests). See Extended Data Fig. 5 for data from cortex. Data shown as mean ± s.e.m.
Pericytes apposed to capillaries, unlike endothelial cells, also died in vivo after 90 min of MCAO (followed by 22.5 h recovery: Fig. 5e, f, and Extended Data Fig. 6c). In contrast, a sham operation occluding only the internal carotid artery (see Methods) produced less pericyte death, and a sham operation with no artery occlusion (which did not affect blood flow; see Methods) induced no more death than in naive untreated animals. Thus, pericyte death is a rapid response of the cerebral vascular bed to ischaemia, both in brain slices and in vivo.
Discussion
Understanding what initiates the blood-flow increase in response to neuronal activity is crucial for understanding both how information processing is powered and how functional imaging signals are generated30. Most neurons are closer to capillaries (∼8.4 μm distant, in hippocampus31) than to arterioles (70 μm distant31), suggesting that neurons might adjust their energy supply by initially signalling to pericytes (Extended Data Fig. 1a). Our data support this concept: neuronal activity leads to a release of messengers that activate an outward membrane current in pericytes (Fig. 2) and dilate capillaries before arterioles (Fig. 3). Capillary dilation implies that there is a resting tone set by the pericytes, perhaps as a result of noradrenaline release from locus coeruleus axons, two-thirds of the perivascular terminals of which end near capillaries rather than arterioles32. Vascular diameter responses can propagate between adjacent pericytes1,9, but it is not yet known whether arterioles receive a signal to dilate from pericytes, or from vasoactive messengers which reach arterioles later than they reach pericytes. We have identified the cause of pericyte dilation as being EP4 receptor activation, by PGE2 or a related compound, although NO production is also needed to suppress synthesis of vasocontricting 20-HETE (Fig. 1 and Extended Data Fig. 1b). These mechanisms resemble those controlling arteriole dilation, and may reflect glutamate release activating the production of arachidonic acid and its derivatives in astrocytes or neurons13.
The more frequent occurrence of capillary dilation at pericyte locations (Fig. 3i–k), and the faster onset of capillary dilation than of arteriole dilation in vivo (Fig. 3d–h) suggest that pericytes actively relax to dilate capillaries. Our data suggest that capillaries have two conceptually separate roles in regulating cerebral blood flow. First, being closer to neurons, they detect neuronal activity earlier than arterioles can, and may pass a hyperpolarizing vasodilatory signal back to arterioles (through gap junctions between pericytes or endothelial cells)1,9. Second, capillary vasodilation itself contributes significantly to increasing blood flow. To assess the extent to which capillary dilations increase blood flow, we used data on the vascular tree in mouse cortex33 (see Methods). For a mean arteriole dilation of 5.9% during prolonged (15 s) stimulation (Extended Data Table 1), a capillary dilation of 6.7% (averaged over all capillary orders, Extended Data Table 1) and ignoring venule dilation, the steady state blood flow was predicted to increase by 19%. Omitting the capillary dilation predicted a flow increase of only 3%. Thus, capillary dilation is estimated to generate 100× (19 − 3)/19 = 84% of the steady-state increase in blood flow evoked by neuronal activity, and capillaries dilate approximately 1 s before penetrating arterioles (Fig. 3d–h). These results suggest that BOLD functional imaging signals largely reflect capillary dilation by pericytes.
For ischaemia, our data support, but modify, the suggestion that pericyte constriction1,14 may be a cause of the long-lasting decrease of cerebral blood flow that occurs even when a blocked artery is opened up after stroke26,27,28,29. It was previously envisaged that constriction of capillaries was by healthy pericytes and could be reversed by suppressing oxidative stress14, whereas we find that, after ischaemia has constricted them (Fig. 4), pericytes die readily (Fig. 5). This death is mediated in part by glutamate, but is not reduced by free radical scavenging, suggesting that the constriction and death differ at least partly in their causes. Pericyte death in rigor will produce a long-lasting decrease of capillary blood flow26,27,28,29, as well as a breakdown of the (pericyte-maintained4,5,6) blood–brain barrier. Both of these will contribute to ongoing neuronal damage, highlighting the potential importance of preventing pericyte death as a therapeutic strategy after stroke, particularly in the penumbra of an affected region. To develop this approach, it will be necessary to develop small molecule inhibitors of pericyte death that could be administered, perhaps with tissue plasminogen activator, soon after a stroke has occurred.
Methods Summary
Brain slices from rats or NG2-DsRed mice were made and capillaries were imaged as described previously1. The fluorescence of DsRed-labelled capillary pericytes was used to identify pericytes for patch-clamping. Two-photon imaging of FITC-dextran-labelled cortical vessels and DsRed-labelled pericytes in vivo was performed in mice as previously described for cerebellum34.
Online Methods
Animals
Experiments used Sprague-Dawley or Wistar rats and NG2-DsRed C57BL/6J mice of either sex. Animal procedures were carried out in accordance with the guidelines of the UK Animals (Scientific Procedures) Act 1986, the Danish National Ethics Committee and European Directive 2010/63/EU. Each experiment was conducted on tissue from at least three animals on at least three different experimental days.
Brain slice preparation
Slices (200–300 µm thick) were prepared1,35 on a vibratome in ice-cold oxygenated (95% O2, 5% CO2) solution. This solution was usually artificial cerebrospinal fluid (aCSF) containing (in mM) 124 NaCl, 2.5 KCl, 26 NaHCO3, 1 MgCl2, 1 NaH2PO4, 10 glucose, 0.1–1 Na ascorbate, 2 CaCl2 (to which 1 kynurenic acid was added to block glutamate receptors), and slices were incubated at room temperature (21–23 °C) in the same solution until used in experiments. For Fig. 2e–h and 4, the slicing solution contained (mM) 93 N-methyl-d-glucamine chloride, 2.5 KCl, 30 NaHCO3, 10 MgCl2, 1.2 NaH2PO4, 25 glucose, 0.5 CaCl2, 20 HEPES, 5 Na ascorbate, 3 Na pyruvate, 1 kynurenic acid, and the slices were incubated at 34°C in the same solution for 10 min, and then incubated at room temperature (21–23 °C) until used in experiments in a similar solution with the NMDG-Cl, MgCl2, CaCl2 and Na ascorbate replaced by (mM) 92 NaCl, 1 MgCl2 2 CaCl2 and 1 Na ascorbate.
Immunohistochemical labelling of pericytes
Isolectin B4 binds to α-d-galactose residues in the basement membrane secreted by endothelial cells36,37, which surrounds pericytes. Cerebellar slices were incubated in FITC-conjugated 10 µg ml−1 isolectin B4 (Sigma) for 1 h then fixed for 20 min in 4% PFA, and incubated for 4 to 6 h in 0.05% Triton X-100, 10% goat serum in phosphate-buffered saline at 21°C, then with primary antibody at 21°C overnight with agitation, and then for 4 to 8 h at 21°C with secondary antibody. Primary antibodies were: guinea pig NG2 (from W.B. Stallcup, 1:100), rabbit NG2 (Millipore AB5320, 1:300) and rabbit PDGFRβ (Santa Cruz sc432, 1:200). Secondary antibodies (goat) were: anti-rabbit (Molecular Probes, 1:200) and anti-guinea-pig (Jackson Laboratory, 1:100). Pericytes, with a bump-on-a-log morphology on capillaries, or located at the junction of capillaries, labelled for NG2 and PDGFRβ (Fig. 1). As perivascular immune cells are sometimes confused with pericytes19, we labelled the former with antibody to Iba1 (rabbit Iba1, Synaptic Systems 234003, 1:500) in seven cortical and eight cerebellar slices from five NG2-DsRed animals, and found that none of 135 (cortex) and 212 (cerebellum) NG2-DsRed labelled perivascular cells co-labelled for Iba1 (although Iba1 labelled 110 cells in the cortical slices and 136 cells in the cerebellar slices, Fig. 1c), implying that pericytes defined by an on-capillary location and NG2 expression differ from perivascular microglia or macrophages.
Imaging of capillaries in brain slices
Slices were perfused with bicarbonate-buffered aCSF, as described above, but without the kynurenic acid, at 31 to 35°C. In experiments using 20% oxygen, the perfusion solution was bicarbonate-buffered aCSF, gassed with 20% O2, 5% CO2 and 75% N2.
For bright-field recording of capillary diameter, sagittal cerebellar slices were prepared from postnatal day 10 (P10) to P21 Sprague-Dawley rats or coronal cortical slices were prepared from P12 rats. On average 1.3 capillary regions were imaged per slice. Capillaries were imaged1 at approximately 30 µm depth within the molecular layer of cerebellar slices or the grey matter of slices containing the somatosensory and motor cortices, using a ×40 water immersion objective, a Coolsnap HQ2 CCD camera, and ImagePro Plus or Metafluor acquisition software. Images were acquired every 1 to 5 s, with an exposure time of 5 ms. The pixel size was 160 or 300 nm. Vessel internal diameters were measured by manually placing a measurement line (perpendicular to the vessel, Fig. 1d) on the image (at locations near visible pericytes which constricted when noradrenaline was applied), using ImagePro Analyzer, Metamorph or ImageJ software, with the measurer blinded as to the timing of drug applications. The end of the measurement line was placed at locations representing the measurer’s best estimate of where the rate of change of intensity was greatest across pixels under the vessel edge, and the diameter was estimated to a precision of one pixel. Where necessary, images were aligned by manually tracking drift, or by using the Image Pro ‘Align Global Images’ macro. Experiments in which changes in focus occurred were excluded from further analysis. Data in the presence of blockers of signalling pathways were compared with interleaved data obtained without the blockers.
For experiments in which the parallel fibres were stimulated in the molecular layer, coronal slices were used to preserve the parallel fibres, and stimuli of 60 to 100 μs duration, at 50 to 90 V and 12 Hz, were applied for 25 s using a patch-pipette electrode placed approximately 100 μm away from the imaged vessel. To check that parallel fibres were being successfully activated, the field potential was monitored in the molecular layer using a 4 MΩ patch pipette filled with aCSF. To ensure that pericytes were healthy we excluded capillaries that did not constrict to 1 μM noradrenaline. Stimulation evoked dilation (Fig. 2e, f), except in two capillaries that constricted, presumably owing to direct depolarization of a pericyte by the stimulus since when TTX was applied (to one of these vessels) a stimulation-evoked constriction was still seen in TTX: these two vessels were excluded from the analysis.
Patch-clamp recordings of pericytes
Coronal slices of cerebellum were prepared35 from P10 to P17 NG2-DsRed C57BL/6J mice. Slices were superfused with bicarbonate-buffered solution containing (in mM) 124 NaCl, 26 NaHCO3, 1 NaH2PO4, 2.5 KCl, 1 MgCl2, 2.5 CaCl2, 10 glucose, bubbled with 95% O2/5% CO2, pH 7.3, at 21 to 23 °C or 33 to 36 °C (stimulation-evoked currents were not significantly different at the two temperatures and were pooled). Pericytes were identified as DsRed-expressing cells located on capillaries (oligodendrocyte precursor cells also express NG2-DsRed but these can be distinguished from pericytes morphologically and by their position in the parenchyma). Pericytes were whole-cell clamped between −55 and −75 mV with pipettes containing solution comprising (in mM) 130 K-gluconate, 4 NaCl, 0.5 CaCl2, 10 HEPES, 10 BAPTA, 2 Na2ATP, 2 MgCl2, 0.5 Na2GTP, 0.05 Alexa Fluor 488, pH set to 7.3 with KOH. Electrode junction potentials were compensated. Patch-clamped cells were morphologically confirmed to be pericytes by dye filling. Series resistance was 20 to 40 MΩ. In 17 cells the mean resting potential was −47.6 ± 2.1 mV, and the mean input resistance at the resting potential was 292 ± 27 MΩ. A 30-pA outward current evoked by neuronal activity (see main text) is thus expected to hyperpolarize pericytes by approximately 9mV.
Imaging of vessels in vivo: animal preparation
Sixteen adult NG2 DsRed C57BL/6J mice (18–37 g, of either sex) were prepared for experiments by cannulation of the trachea for mechanical ventilation (SAR-830; CWE). Catheters were placed into the left femoral artery and vein and perfused with physiological saline. The end-expiratory CO2 (microCapstar End-tidal CO2 Monitor, CWE) and blood pressure (Pressure Monitor BP-1; World Precision Instruments) were monitored continuously in combination with blood gases in arterial blood samples (pO2 115–130 mm Hg; pCO2 35–40 mm Hg; pH 7.35–7.45; ABL 700 Series; Radiometer Medical) to ensure the animals were kept under physiological conditions. The temperature was measured and maintained at 37°C during the experiment with a rectal thermometer regulated heating pad (TC-1000 Temperature Controller; CWE). The animals were anaesthetized with xylazine (10 mg kg−1 intraperitoneal) and ketamine (60 mg kg−1 intraperitoneal) during surgery, and then switched to alpha-chloralose (50 mg kg−1h−1 intravenous) during the experiment. The skull was glued to a metal plate using cyanoacrylate gel (Loctite Adhesives) and the plate was fixed in the experimental setup. A craniotomy was drilled with a diameter of approximately 4 mm with the centre 0.5 mm behind and 3 mm to the right of the bregma over the sensory barrel cortex region. The dura was removed and the preparation covered with 0.75% agarose (type III-A, low EEO; Sigma-Aldrich) and moistened with artificial cerebrospinal fluid (in mM: 120 NaCl, 2.8 KCl, 22 NaHCO3, 1.45 CaCl2, 1 Na2HPO4, 0.9 MgCl2 and 2.6 glucose; pH 7.4) at 37 °C and bubbled with 95% air, 5% CO2. The craniotomy was covered with a glass coverslip. When experiments were complete, mice were euthanized by intravenous injection of anaesthesia (pentobarbital, 200 mg ml−1 and lidocaine hydrochloride, 20 mg ml−1) followed by decapitation.
Imaging of vessels in vivo: whisker-pad stimulation
The mouse sensory barrel cortex was activated by stimulation of the contralateral ramus infraorbitalis of the trigeminal nerve using a set of custom-made bipolar electrodes inserted percutaneously. The cathode was positioned at the hiatus infraorbitalis, and the anode was inserted into the masticatory muscles38. Thalamocortical infraorbitalis stimulation was performed at an intensity of 1.5 mA (ISO-flex; AMPI) and lasting 1 ms, in trains of 2 s or 15 s at 3 Hz. The stimulation was controlled by a sequencer file running within Spike2 software (version 7.02; Cambridge Electronic Design).
Imaging of vessels in vivo: cortical response imaging
For each animal, the haemodynamic response to stimulation was detected using intrinsic optical imaging (IOS) and used to identify the region of brain activated by whisker-pad stimulation, for further vascular imaging. Two-photon imaging of blood vessels was then conducted near the centre of this activated region. The IOS was recorded on a Leica microscope with ×5 magnification that included the entire preparation in the field of view. The light source consisted of LEDs with green light filters and a fast camera (QuantEM 512SC; Photometrics) sampled 29 images per s before and during 15 s of 3 Hz stimulation. As haemoglobin strongly absorbs green light, the captured light intensity decreases as the total haemoglobin concentration increases during changes in cerebral blood volume and flow39. Images during stimulation were subtracted from control images40, allowing the area of brain where blood flow increases during whisker stimulation to be revealed.
Imaging of vessels in vivo: two-photon imaging
Fluorescein isothiocyanate-dextran (FITC-dextran, 2% w/v, MW 70,000, 50 μl, Sigma-Aldrich) was administered into the femoral vein to label the blood plasma34. In vivo imaging of blood vessel diameter and pericyte location was performed using a commercial two-photon microscope (SP5, Leica), a MaiTai HP Ti:Sapphire laser (Millennia Pro; Spectra Physics, mean output power 10 mW), and a 20 × 1.0 N.A. water-immersion objective (Leica). Tissue was excited at 900 nm wavelength, and the emitted light was filtered to collect red and green light from DsRed (pericytes) and FITC-dextran (vessel lumens). Penetrating arterioles were identified unequivocally in vivo in two ways, first by tracing their connections back to pial arterioles with obvious smooth muscle around them, and second by observing the direction of flow of the red blood cells from the arterioles into the parenchymal capillaries. Z-stack images were taken of the area of interest. XY-time series were taken to image pericytes and blood vessels during stimulation, with a frame size 512 × 300 pixels (170 ms per frame; pixel size was 93 to 201 nm depending on the magnification used, with a mean value of 155 nm; pixel dwell time was 1.1 μs).
Imaging of vessels in vivo: image analysis
The presence of red blood cells (RBCs) leads to apparent holes in the images of the capillary and (to a lesser extent) the arteriole (Extended Data Fig. 4a, b). This image noise was reduced by smoothing images with a maximum intensity 10 frame (1.7 s) running summation of the green channel showing the FITC-labelled vascular lumen (see Extended Data Fig. 4a–d for sample images, and the effect this would have on the apparent timing of a step increase of diameter and on the dilations shown in Fig. 3d). This channel was then processed to extract blood vessel diameters. Lines were placed across the vessel (perpendicular to the vessel wall) at a spacing of approximately 20 µm (for example, Fig. 3d). The edges of the vessel were located using the ImagePro caliper tool, which finds the greatest gradient in light intensity along the line (where d2intensity/dx2 = 0). As for brain slice imaging above, interpolation of the image intensity across pixels allows, in principle, the position of the edge to be estimated to change by less than one pixel, but in practice we measured the diameter with a precision of one pixel. We considered whether the smoothing applied could artefactually preferentially accelerate the dilation seen for capillaries. In fact this is not possible, because the smoothing uses a maximum intensity sum of all the 10 frames: consequently, a black area produced by a passing RBC will not add to the summed image, and any increase in diameter that has occurred will only be detected in a later frame. Thus, passage of an RBC can only delay the apparent time at which dilation is detected, this effect should be larger in capillaries in which the RBCs are moving more slowly, and yet the capillaries dilate before the arterioles (Fig. 3). We conclude that the smoothing cannot cause a preferential acceleration of the time course of dilation in the capillary data. For Fig. 3e, g, the time courses of the measured diameter were also smoothed with a five-point FFT procedure that removes frequencies over 1.16 Hz (OriginLab software), the effect of which is shown in Extended Data Fig. 4e. Responding capillaries were defined as those showing a change upon stimulation of more than 5% of the initial vessel diameter (since 4.99% was twice the standard deviation of the baseline diameter averaged over all vessels studied). Where multiple regions responded on a single vessel, their response times were averaged for comparison between paired vessels (Fig. 3f and Extended Data Fig. 5c). Blood flow in capillaries was assessed from the velocity of RBCs, which appear as dark patches inside FITC-dextran labelled vessels, using line-scan imaging23. Repetitive line-scans (0.358 ms per line of 512 pixels) along the axis of the vessel before, during and after whisker stimulation (3Hz, 15 s) were used to form a space-time image in which moving RBCs produce streaks with a slope that is equal to the inverse of the speed. The slope was calculated using an automated image-processing algorithm41. The baseline speed of RBCs averaged over all capillaries studied was 1.73 ± 0.20 mm s−1 (n = 49).
Cell-death experiments: chemical ischaemia
For chemical ischaemia experiments (Figs 4 and 5a, b), coronal cortical slices from P21 (Fig. 4) or sagittal cerebellar slices from P7 (Fig. 5a, b) Sprague-Dawley rats were incubated at 37°C in an ischaemic solution in which glucose was replaced with 7 mM sucrose and oxygen was removed by equilibrating solutions with 5% CO2 and 95% N2. In addition, 2 mM iodoacetate and 25 µM antimycin were added to the ischaemic solution to block ATP generation by glycolysis and oxidative phosphorylation, respectively42. Control slices were incubated in aCSF, gassed as usual with 5% CO2, 95% O2. Propidium iodide (PI, 37 µM for Fig. 5a-d, but 7.5 μM for Fig. 4) was added to both solutions to label dead cells. For Fig. 5, after 60 min incubation in this ischaemic solution, slices were fixed for 20 min in 4% paraformaldehyde and immunohistochemistry for NG2 was performed, as described above.
Cell-death experiments: oxygen-glucose deprivation
For the oxygen-glucose deprivation experiments shown in Fig. 5c, d and Extended Data Fig. 6a, b, coronal forebrain slices were prepared from P21 Sprague Dawley rats then incubated in aCSF in which glucose was replaced with 7 mM sucrose and oxygen was removed by equilibrating solutions with 5% CO2 and 95% N2. Control slices were incubated in aCSF, gassed as usual with 5% CO2, 95% O2. After 60 min, some slices were immediately fixed in 4% paraformaldehyde, while others were placed in control aCSF, to reoxygenate for a further 60 min. All solutions also contained 37 µM PI and 10 µg ml−1 FITC-conjugated isolectin B4 to label dead cells and blood vessels, respectively. Slices were swiftly washed in aCSF before fixation for 20 min in 4% paraformaldehyde, washed three times in PBS and mounted on microscope slides in Dako hard set mounting medium. Slides were then imaged using a Zeiss LSM 700 or 710 confocal microscope. PI-positive dead vascular and parenchymal cells were counted using ImageJ software, by an experimenter who was blind to their condition. Cells in the 20 µm closest to the slice surface were excluded from analysis to prevent confounds from slicing-induced damage. Dead or alive pericytes were identified by their ‘bump-on-a-log’ morphology on vessels surrounded by isolectin B4 labelling. To check that pericytes could be identified by isolectin B4 labelling alone, in parallel experiments we labelled slices for isolectin B4 and NG2: the great majority (93% of 718 cells assessed) of pericytes identified this way were found to be positive for NG2. Although some pericytes may slightly move away from capillaries after hypoxia or brain injury43,44, we only counted pericytes apposed to capillaries in this study.
Cell-death experiments: middle cerebral artery occlusion
Male Wistar rats (Harlan) weighing 253 to 312g, housed on a 12-h light–dark cycle with ad libitum access to food and water, underwent transient middle cerebral artery occlusion (MCAO) as described previously45. In brief, animals were anaesthetized with 4% isoflurane and maintained in 1.5 to 2% isoflurane carried in 70% N2O and 30% O2. A midline incision was made in the neck, the right external carotid artery was cauterised and cut, and the right common carotid and internal carotid arteries were temporarily ligated. Through a small arteriotomy in the external carotid artery stump, a 4-0 nylon filament coated with silicone at the tip (Doccol) was advanced up the internal carotid artery to occlude the right middle cerebral artery at its origin. For sham animals, the entire procedure was followed except that either: the filament was only advanced up the beginning of the internal carotid artery (ICA) before being withdrawn after 3 min (sham with ICA occlusion); or the external carotid artery was permanently ligated (which had no effect on cerebral blood flow) and the common and internal carotid arteries were exposed but not ligated, and the animals remained under anaesthesia for the same length of time as sham animals (sham without ICA occlusion). Core temperature was maintained at 37°C by a rectal thermister probe attached to a heating pad. Cerebral blood flow was continuously monitored by placing a laser Doppler probe (Oxford Optronix) over a thinned skull of the MCA territory approximately 4 mm lateral and 1.5 mm caudal to bregma. In MCAO animals, averaged over the period of occlusion, cerebral blood flow on the treated side fell to 34.9 ± 7.1% of baseline (n = 6) for 90 min, while in sham animals with ICA occlusion it dropped significantly less to 67.9 ± 11.0% of baseline (P = 0.035, t-test, n = 3) for 16 min (this smaller drop occurs because of occlusion of the ICA), and in sham animals without ICA occlusion blood flow was unaffected (104.0 ± 3.9% of baseline, n = 3). Following 90 min of MCAO, the filament was retracted, and the common carotid artery ligation was released to allow maximal reperfusion. Anaesthesia was then removed, and at 22.5 h of reperfusion, neurological deficit was assessed by investigating limb symmetry, motor function, activity and response to sensory stimulation (modified from ref. 46 by scoring spontaneous movement, symmetry in limb movement and forepaw outstretching on a scale of 0–3 with 0 = normal and 3 = most severely affected, and scoring climbing, body proprioception and response to vibrissae touch on a 0 (normal) to 2 scale). A maximum score of 15 equates to severe neurological deficit, while a minimum score of 0 implies no neurological deficit. MCAO animals had a mean score of 7.5 ± 1.7 (n = 6), which was significantly greater than that of sham animals with ICA occlusion (0.3 ± 0.3, n = 3, P = 0.027) and sham animals without ICA occlusion (0 ± 0, n = 3 P = 0.039, corrected for multiple comparisons). Animals (including an additional three naive control animals) were then anaesthetized, decapitated, and 200 µm forebrain slices were prepared on a vibratome and labelled with PI (37 μM) and FITC-isolectin B4 (10 μg ml−1) in aCSF for 60 min, then washed, fixed, mounted and cortical and striatal images were captured as described above. Live and dead pericytes were counted in both regions as above except that dead endothelial cells were also counted (identified by their elongated nuclei). More pericyte death was seen in brain slices made from naive control animals in this in vivo series of experiments (Fig. 5f) than in experiments studying pericyte death in slices (Fig. 5b, d); this may be because, for the adult rats used for the in vivo experiments, it takes longer to kill the animal and remove its brain, than for the younger animals used for slice experiments. The total number of endothelial cells present, and therefore the percentage of dead endothelial cells, was estimated from the total number of pericytes, assuming a 1:3 ratio of pericytes to endothelial cells47.
Statistics
All data are presented as mean ± s.e.m. P values are from ANOVA (univariate, unless otherwise stated) and post-hoc Dunnett’s or Student’s t-tests, chi-squared tests, Kolmogorov–Smirnov tests or Mann–Whitney U-tests (for non-normally distributed data), as appropriate. Two-tailed tests were used. P values quoted in the text are from independent samples t-tests unless otherwise stated. For multiple comparisons, P values are corrected using a procedure equivalent to the Holm-Bonferroni method (for N comparisons, the most significant P value is multiplied by N, the second-most significant by N-1, the third-most significant by N-2 and so on; corrected P values are considered significant if they are less than 0.05). Normality of data was assessed using Kolmogorov–Smirnov tests. All statistical analysis was conducted using IBM SPSS21, OriginLab or Excel software.
Contribution of capillary dilation to cerebral blood-flow increases
To assess how capillary dilations increase blood flow in the steady state, we used data from a recent analysis of the vascular tree in mouse cortex33. For blood flow from the cortical surface (where for simplicity we assume blood pressure to be constant) through a penetrating arteriole to layer 4 of the cortex, through the array of inter-connected capillaries, and back to the cortical surface through a penetrating venule, that analysis33 concluded that the resistances (at baseline diameter) of the arteriole, capillary and venule segments of this path were, respectively, 0.1, 0.4 (for a path from an arteriole to a venule separated by approximately 200 μm, Figs 2g and 5c of ref. 33) and 0.2 poise per μm3, so that capillaries provide 57% of the total resistance. For a mean neuronal activity evoked arteriole dilation of 5.9% during prolonged (15 s) stimulation (Extended Data Table 1), a capillary dilation of 6.7% (averaged over all capillary orders, Extended Data Table 1) and ignoring venule dilation, then for resistance inversely proportional to the fourth power of diameter (Poiseuille’s law) the blood flow should increase by 19% in the steady state. Omitting the capillary dilation predicts a flow increase of only 3%, while omitting the arteriole dilation (so that only capillaries dilate) predicts a flow increase of 15%. Deviations from Poiseuille’s law in the capillaries33 make only a small correction to these values. Thus, capillary dilation is predicted to generate 84% of the steady state increase in blood flow evoked by prolonged neuronal activity. This figure would be reduced somewhat if pial arteriole dilation48 significantly contributes to the flow increase. For example, if pial arterioles are assumed to dilate by the same 5.9% as penetrating arterioles, and to have the same resistance as penetrating arterioles, then the capillary contribution to the blood flow increase is predicted to be 73% (however the larger diameter of pial vessels and their anastomoses49 suggest that their contribution to the total resistance and blood flow control will be much less than that of the penetrating arterioles).
Relationship to earlier work
A previous failure to observe active capillary dilation2 may reflect two factors. First, in that study2, unlike ours, the authors were unable to reproducibly evoke blood flow increases by whisker-pad stimulation and so used bicuculline to excite neurons: conceivably this induces seizure-like activity which may generate a non-physiological release of vasoconstricting 20-HETE, as well as of dilating messengers. Second, the use of thiopental anaesthetic in that study2 may have reduced blood flow increases, since the same group reported that the closely related anaesthetic thiobutabarbital suppresses neuronally evoked blood flow increases by 40% compared to those seen using α-chloralose (the anaesthetic that we use)50. In addition, the vessels they define as precapillary arterioles2 (their Fig. 4h), which did show active dilations, seem to have isolated pericytes on them (rather than continuous smooth muscle) and would be called first-order capillaries in our nomenclature.
Duration of rigor after pericyte death
Rigor occurs because when the ATP level falls, muscle cells like pericytes cannot detach their myosin heads from actin to relax. At the whole body level rigor mortis following death (the stiffness resulting from skeletal muscles dying in rigor) lasts approximately 18 to 36 h, depending on temperature. We would therefore expect pericytes to stay in rigor for hours (that is, the period after ischaemia for which blood flow is known to be reduced26), unless removed by microglia.
References
Peppiatt, C. M., Howarth, C., Mobbs, P. & Attwell, D. Bidirectional control of CNS capillary diameter by pericytes. Nature 443, 700–704 (2006)
Fernández-Klett, F., Offenhauser, N., Dirnagl, U., Priller, J. & Lindauer, U. Pericytes in capillaries are contractile in vivo, but arterioles mediate functional hyperemia in the mouse brain. Proc. Natl. Acad. Sci. USA 107, 22290–22295 (2010)
Chan-Ling, T. et al. Desmin ensheathment ratio as an indicator of vessel stability: evidence in normal development and in retinopathy of prematurity. Am. J. Pathol. 165, 1301–1313 (2004)
Bell, R. D. et al. Pericytes control key neurovascular functions and neuronal phenotype in the adult brain and during brain aging. Neuron 68, 409–427 (2010)
Armulik, A. et al. Pericytes regulate the blood–brain barrier. Nature 468, 557–561 (2010)
Daneman, R., Zhou, L., Kebede, A. A. & Barres, B. A. Pericytes are required for blood-brain barrier integrity during embryogenesis. Nature 468, 562–566 (2010)
Göritz, C. et al. A pericyte origin of spinal cord scar tissue. Science 333, 238–242 (2011)
Dore-Duffy, P., Katychev, A., Wang, X. & Van Buren, E. CNS microvascular pericytes exhibit multipotential stem cell activity. J. Cereb. Blood Flow Metab. 26, 613–624 (2006)
Puro, D. G. Physiology and pathobiology of the pericyte-containing retinal microvasculature: new developments. Microcirculation 14, 1–10 (2007)
Villringer, A., Them, A., Lindauer, U., Einhäupl, K. & Dirnagl, U. Capillary perfusion of the rat brain cortex. An in vivo confocal microscopy study. Circ. Res. 75, 55–62 (1994)
Schulte, M. L., Wood, J. D. & Hudetz, A. G. Cortical electrical stimulation alters erythrocyte perfusion pattern in the cerebral capillary network of the rat. Brain Res. 963, 81–92 (2003)
Jespersen, S. N. & Østergaard, L. The roles of cerebral blood flow, capillary transit time heterogeneity, and oxygen tension in brain oxygenation and metabolism. J. Cereb. Blood Flow Metab. 32, 264–277 (2012)
Attwell, D. et al. Glial and neuronal control of blood flow. Nature 468, 232–243 (2010)
Yemisci, M. et al. Pericyte contraction induced by oxidative-nitrative stress impairs capillary reflow despite successful opening of an occluded cerebral artery. Nature Med. 15, 1031–1037 (2009)
Vates, G. E., Takano, T., Zlokovic, B. & Nedergaard, M. Pericyte constriction after stroke: the jury is still out. Nature Med. 16, 959 (2010)
Hall, C. N., Klein-Flügge, M. C., Howarth, C. & Attwell, D. Oxidative phosphorylation, not glycolysis, powers presynaptic and postsynaptic mechanisms underlying brain information processing. J. Neurosci. 32, 8940–8951 (2012)
Hall, C. N. & Attwell, D. Assessing the physiological concentration and targets of nitric oxide in brain tissue. J. Physiol. (Lond.) 586, 3597–3615 (2008)
Zhu, X., Bergles, D. E. & Nishiyama, A. NG2 cells generate both oligodendrocytes and gray matter astrocytes. Development 135, 145–157 (2008)
Krueger, M. & Bechmann, I. CNS pericytes: concepts, misconceptions, and a way out. Glia 58, 1–10 (2010)
Hamilton, N. B., Attwell, D. & Hall, C. N. Pericyte-mediated regulation of capillary diameter: a component of neurovascular coupling in health and disease. Front. Neuroenergetics 2, 5 (2010)
Serebryakov, V., Zakharenko, S., Snetkov, V. & Takeda, K. Effects of prostaglandins E1 and E2 on cultured smooth muscle cells and strips of rat aorta. Prostaglandins 47, 353–365 (1994)
Crawford, C. et al. An intact kidney slice model to investigate vasa recta properties and function in situ. Nephron Physiol. 120, 17–31 (2012)
Kleinfeld, D., Mitra, P. P., Helmchen, F. & Denk, W. Fluctuations and stimulus-induced changes in blood flow observed in individual capillaries in layers 2 through 4 of rat neocortex. Proc. Natl. Acad. Sci. USA 95, 15741–15746 (1998)
Khatri, P. et al. Good clinical outcome after ischemic stroke with successful revascularization is time-dependent. Neurology 73, 1066–1072 (2009)
Gupta, E. et al. Higher volume endovascular stroke centers have faster times to treatment, higher reperfusion rates and higher rates of good clinical outcomes. J. Neurointerv. Surg. 5, 294–297 (2013)
Hauck, E. F., Apostel, S., Hoffmann, J. F., Heimann, A. & Kempski, O. Capillary flow and diameter changes during reperfusion after global cerebral ischemia studied by intravital video microscopy. J. Cereb. Blood Flow Metab. 24, 383–391 (2004)
Leffler, C. W., Beasley, D. G. & Busija, D. W. Cerebral ischemia alters cerebral microvascular reactivity in newborn pigs. Am. J. Physiol. 257, H266–H271 (1989)
Nelson, C. W., Wei, E. P., Povlishock, J. T., Kontos, H. A. & Moskowitz, M. A. Oxygen radicals in cerebral ischemia. Am. J. Physiol. 263, H1356–H1362 (1992)
Baird, A. E. et al. Reperfusion after thrombolytic therapy in ischemic stroke measured by single-photon emission computed tomography. Stroke 25, 79–85 (1994)
Attwell, D. & Iadecola, C. The neural basis of functional imaging signals. Trends Neurosci. 25, 621–625 (2002)
Lovick, T. A., Brown, L. A. & Kay, B. J. Neurovascular relationships in hippocampal slices: physiological and anatomical studies of mechanisms underlying flow-metabolism coupling in intraparenchymal microvessels. Neuroscience 92, 47–60 (1999)
Cohen, Z., Molinatti, G. & Hamel, E. Astroglial and vascular interactions of noradrenaline terminals in the rat cerebral cortex. J. Cereb. Blood Flow Metab. 17, 894–904 (1997)
Blinder, P. et al. The cortical angiome: a 3-D interconnected vascular network with noncolumnar patterns of blood flow. Nature Neurosci. 16, 889–897 (2013)
Mathiesen, C., Brazhe, A., Thomsen, K. & Lauritzen, M. Spontaneous calcium waves in Bergmann glia increase with age and hypoxia and may reduce tissue oxygen. J. Cereb. Blood Flow Metab. 33, 161–169 (2013)
Marcaggi, P. & Attwell, D. Endocannabinoid signaling depends on the spatial pattern of synapse activation. Nature Neurosci. 8, 776–781 (2005)
Peters, B. P. & Goldstein, I. J. The use of fluorescein-conjugated Bandeiraea simplicifolia B4-isolectin as a histochemical reagent for the detection of alpha-D-galactopyranosyl groups. Their occurrence in basement membranes. Exp. Cell Res. 120, 321–334 (1979)
Laitinen, L. Griffonia simplicifolia lectins bind specifically to endothelial cells and some epithelial cells in mouse tissues. Histochem. J. 19, 225–234 (1987)
Norup Nielsen, A. & Lauritzen, M. Coupling and uncoupling of activity-dependent increases of neuronal activity and blood flow in rat somatosensory cortex. J. Physiol. (Lond.) 533, 773–785 (2001)
Frostig, R. D., Lieke, E. E., Ts'o, D. Y. & Grinvald, A. Cortical functional architecture and local coupling between neuronal activity and the microcirculation revealed by in vivo high-resolution optical imaging of intrinsic signals. Proc. Natl. Acad. Sci. USA 87, 6082–6086 (1990)
Harrison, T. C., Sigler, A. & Murphy, T. H. Simple and cost-effective hardware and software for functional brain mapping using intrinsic optical signal imaging. J. Neurosci. Methods 182, 211–218 (2009)
Schaffer, C. B. et al. Two-photon imaging of cortical surface microvessels reveals a robust redistribution in blood flow after vascular occlusion. PLoS Biol. 4, e22 (2006)
Allen, N. J., Káradóttir, R. & Attwell, D. A preferential role for glycolysis in preventing the anoxic depolarization of rat hippocampal area CA1 pyramidal cells. J. Neurosci. 25, 848–859 (2005)
Dore-Duffy, P. et al. Pericyte migration from the vascular wall in response to traumatic brain injury. Microvasc. Res. 60, 55–69 (2000)
Gonul, E. et al. Early pericyte response to brain hypoxia in cats: an ultrastructural study. Microvasc. Res. 64, 116–119 (2002)
Nagel, S. et al. Neuroprotection by dimethyloxalylglycine following permanent and transient focal cerebral ischemia in rats. J. Cereb. Blood Flow Metab. 31, 132–143 (2011)
Garcia, J. H., Wagner, S., Liu, K. F. & Hu, X. J. Neurological deficit and extent of neuronal necrosis attributable to middle cerebral artery occlusion in rats. Statistical validation. Stroke 26, 627–635 (1995)
Pardridge, W. M. Blood-brain barrier biology and methodology. J. Neurovirol. 5, 556–569 (1999)
Iadecola, C., Yang, G., Ebner, T. J. & Chen, G. Local and propagated responses evoked by focal synaptic activity in cerebellar cortex. J. Neurophysiol. 78, 651–659 (1997)
Blinder, P., Shih, A. Y., Rafie, C. & Kleinfeld, D. Topological basis for the robust distribution of blood to rodent neocortex. Proc. Natl. Acad. Sci. USA 107, 12670–12675 (2010)
Lindauer, U., Villringer, A. & Dirnagl, U. Characterization of CBF response to somatosensory stimulation: model and influence of anesthetics. Am. J. Physiol. 264, H1223–H1228 (1993)
Acknowledgements
We thank B. Clark, A. Gibb, A. Gourine, C. Howarth, R. Jolivet, C. Madry, P. Mobbs, B. Richardson and A. Silver for comments on the manuscript. This work was supported by the Fondation Leducq, European Research Council, Wellcome Trust, UK Medical Research Council, Rosetrees Trust, Nordea Foundation via the Center for Healthy Aging, the Lundbeck Foundation, NOVO-Nordisk Foundation and Danish Medical Research Council.
Author information
Authors and Affiliations
Contributions
All authors (C.N.H., C.R., B.G., N.B.H., A.M., B.A.S., F.M.O., A.M.B., M.L. and D.A.) contributed to designing the study, doing the experiments, analysing the results and writing the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
Extended Data Figure 1 Signalling to capillary pericytes in health and disease.
a, As vasodilators released from active neurons and their associated astrocytes (1) diffuse through the brain, they encounter pericytes before arteriole smooth muscle (2) because neurons are closer to capillaries than to arterioles31. This may partly explain why capillaries dilate before arterioles (Fig. 3). Pericyte dilation may spread to arteriole smooth muscle by current flow or [Ca2+]i changes passing through gap junctions (3). b, Oxygen-dependent signalling pathways regulating vessel diameter (adapted from ref. 13). Neuronal activity leads to the generation of nitric oxide (NO) and arachidonic acid. Arachidonic acid (AA) is converted into PGE2, which dilates vessels via EP4 receptors, but also into the vasoconstrictor 20-HETE. Production of 20-HETE is inhibited by NO. Together these pathways regulate capillary diameter (Fig. 1). Larger dilations to glutamate in low [O2] may reflect less production of 20-HETE from arachidonic acid. c, In ischaemia, the decrease of ATP concentration leads to a rise of [Ca2+]i in pericytes. This results in some of them contracting and constricting capillaries1, which will prevent the passage of white and red blood cells. Most pericytes then die (Figs 4 and 5). Death of pericytes in rigor will produce a long-lasting decrease of cerebral blood flow, and reduce the ability of the microvasculature to increase blood flow in response to neuronal activity.
Extended Data Figure 2 Drug effects on capillary baseline diameter and constriction to noradrenaline.
a, Rat capillaries are constricted by 100 µM L-NG-nitroarginine (L-NNA), suggesting that there is some tonic release of NO in the slice, with a greater constriction occurring at high [O2] (bars in a–d, f–n show percentage of initial drug-free diameter). b, However, L-NNA does not affect the diameter of vessels preconstricted with noradrenaline (NA; 2 μM, P = 0.81, ANOVA). c, The guanylyl cyclase blocker ODQ (10 µM) does not affect baseline capillary diameter, suggesting that the constricting effect of tonic NO release seen in a is not through the cGMP pathway but is via suppression of 20-HETE release. d, ODQ slightly enhances the constriction achieved with NA (P = 0.003, ANOVA). P values on the graph are from post hoc t-tests. e, As expected, ODQ blocks cGMP production by guanylyl cyclase, as assessed by radioimmunoassay. f, Inhibition of 20-HETE formation with 1 µM HET0016 (HET) does not affect baseline capillary diameter (white bars, at 20% O2, P = 0.78; at 95% O2, P = 0.49), presumably because the tonic NO release (in a) is sufficient to suppress tonic 20-HETE release, and there is no significant difference in baseline diameter in the presence of HET between the two O2 concentrations (P = 0.57, t-test). Unlike application of L-NNA alone (see a), application of L-NNA and HET together (black bars) does not significantly change capillary diameter (P = 0.59, ANOVA compared to HET alone). Indeed, comparing vessel diameters in HET plus L-NNA with those in L-NNA alone (black bars in f versus panel a) reveals that HET significantly relieves the constriction produced by L-NNA (P = 0.03, ANOVA). g, HET does not affect either the constriction to NA (white bars versus white bars in b, P = 0.51, ANOVA) or the diameter of vessels in L-NNA and NA (black bars versus black bars in b, P = 0.26, ANOVA). h, i, Blocking synthesis of epoxy-derivatives of arachidonic acid with MS-PPOH 10 µM does not affect the degree of constriction to NA (h, P = 0.92, ANOVA) or the dilation to glutamate (i; P = 0.92, ANOVA). j–l, Blocking EP4 receptors with 1 µM L161,982 had no effect on baseline diameter in cerebellum (j) or cortex (97.3 ± 1.4% of baseline in 20% O2, P = 0.07, n = 34) and also did not affect the constriction to NA in either area (cerebellum: k, P = 0.90, ANOVA over both [O2]; l, cortex in 20% O2). m, n, Applying DETA-NONOate (m, 100 μM) or prostaglandin E2 (n, 1 μM) dilated cerebellar capillaries preconstricted with noradrenaline (in 20% O2). Data shown as mean ± s.e.m.
Extended Data Figure 3 Pericyte current responses in NG2-DsRed mouse cerebellar slices.
Mean initial inward and later outward currents (as in Fig. 2a–d, 95% O2) evoked in pericytes by stimulation of the parallel fibres, and by superfusion of 500 μM glutamate or 100 μM NMDA. Numbers of cells apply to both black and white bars. Error bars show s.e.m.
Extended Data Figure 4 Smoothing of the in vivo diameter changes.
a, Specimen single frame from the image sequence for Fig. 3d (penetrating arteriole on the right, capillary on the left). The presence of red blood cells (RBC) leads to apparent holes in the image of the capillary diameter. b, RBC movement results in the holes being removed when averaging over 10 frames. c, For a step increase in vessel diameter (top), the effect on the measured diameter time course (bottom) of a running maximum intensity average being calculated over 10 frames starting at each time being considered: the maximum intensity summation results in the largest diameter at any time dominating the smaller diameters at other times, and so the diameter increase is brought forward by 10 frames. If this were not corrected for, the diameter would appear to increase 10 frames (1.72 s) before it actually does. To correct for this, the time axis needs to be advanced by 1.72 s. d, Correction of the 10-frame averaged time courses of the data used for Fig. 3d for the time shift introduced by the averaging. e, Effect of the five-point FFT procedure (which removes frequencies over 1.16 Hz) applied to the averaged time courses in d. The smooth dashed lines are the traces plotted in Fig. 3d.
Extended Data Figure 5 Responses of capillaries in somatosensory cortex in vivo.
a, b, Reproducibility of response to whisker-pad stimulation at 101 capillary locations in NG2-DsRed mice. Mean capillary response time courses are the same on repeated stimulation (a). Responses at 5 and 15 s into 15 s whisker-pad stimulation did not differ significantly between the first and second stimulation (b). c, Time to reach a certain percentage of the maximum dilation in j–1th order vessel minus that in jth order vessel (j is an integer ≥ 1) imaged simultaneously. The time to 10% and 20% of the peak is faster in first-order capillaries than in zero-order penetrating arterioles (see main text and Fig. 3f), although there are no significant differences between vessels of adjacent orders for any of the other bars shown (P = 0.33–1, t-tests; n for each comparison was as in Fig. 3f). d, Time course of responses in all responding (>5%) vessels of different order. Arterioles were significantly slower to reach 10% of their peak response than first- and second-order vessels (see main text). e, The response distributions of capillaries do not differ near pericyte somata or processes (P = 0.24, Kolmogorov–Smirnov test; 172 somata locations, 292 process locations). f, Comparison of time course of dilation of penetrating arterioles and first-order capillaries with that of the blood-flow increase in capillaries (n = 49, all orders averaged) assessed by line-scanning (normalized to the average value at the peak from 11.7 to 13.2 s). Data shown as mean ± s.e.m.
Extended Data Figure 6 Ischaemia-evoked pericyte death in cortical slices and in vivo.
a, Rat pericyte death is not affected by either of the free radical scavengers MnTBAP (150 µM) or PBN (100 µM; P = 0.78 and P = 1, respectively, ANOVA with Dunnett’s post hoc test versus no drug control). The amount of pericyte death did not differ between the two different scavengers (P = 0.88, ANOVA) so the data from the two scavengers were combined for the analysis in the main text (Fig. 4d). b, In addition to the drugs discussed in the main text, none of the following drugs affected pericyte death following OGD and reoxygenation (ANOVA with Dunnett’s post hoc test versus no drug control): an inhibitor of mitochondrial calcium uptake, Ru360 (50 µM, P = 1), the metabotropic glutamate receptor antagonist MCPG (500 µM, P = 0.93) or the 20-HETE synthesis blocker HET0016 (HET, 1 µM, P = 1). c, The percentage of dead cerebral cortical pericytes and endothelial cells after 24 h in the control and treated hemispheres of MCAO-treated rats, sham-operated animals where a filament was inserted into the ICA but was not advanced far enough to completely occlude the vessel (see Methods), sham animals without ICA occlusion, and naive animals that did not experience any surgery before being killed. These data were analysed together with the striatal data in the main Fig. 5f. There was no difference in cell death between cortex and striatum (P = 0.55, repeated measures ANOVA). A much greater proportion of pericytes died than endothelial cells (P = 2.1×10−7, repeated measures ANOVA), and pericyte death, but not endothelial cell death, was greater in the lesioned hemisphere (effect of hemisphere, P = 0.008, repeated measures ANOVA; interaction between hemisphere and cell type, P = 0.007). As expected, most pericyte death occurred in the MCAO treated animals, whereas sham-operated animals with ICA occlusion showed intermediate levels of death between MCAO and naive (or sham with no ICA occlusion) animals (MCAO versus naive animals, P = 0.004; MCAO versus sham without ICA occlusion, P = 0.01; MCAO versus sham with ICA occlusion, P = 0.20; sham with ICA occlusion versus naive, P = 0.13; Tukey post-hoc tests). Data shown as mean ± s.e.m.
Supplementary information
Noradrenaline constricts and glutamate dilates capillaries
Vessel in Figure 1d responding to noradrenaline and glutamate in a rat cerebellar slice. (MOV 9109 kb)
Glutamate release from neurons dilates capillaries
Vessel in Figure 2e-f responding to noradrenaline and parallel fibre stimulation in a rat cerebellar slice. (MOV 3479 kb)
Capillary and arteriole dilation in vivo
Penetrating arteriole and primary capillary in Figure 3d in mouse somatosensory cortex in vivo responding to whisker pad stimulation. The capillary dilates before the arteriole. Green is FITC-dextran; pericytes are labelled with DsRed. (MOV 2744 kb)
Rights and permissions
About this article
Cite this article
Hall, C., Reynell, C., Gesslein, B. et al. Capillary pericytes regulate cerebral blood flow in health and disease. Nature 508, 55–60 (2014). https://doi.org/10.1038/nature13165
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature13165
This article is cited by
-
Sex, hormones and cerebrovascular function: from development to disorder
Fluids and Barriers of the CNS (2024)
-
Induced pluripotent stem cell derived pericytes respond to mediators of proliferation and contractility
Stem Cell Research & Therapy (2024)
-
Exosome-mediated repair of spinal cord injury: a promising therapeutic strategy
Stem Cell Research & Therapy (2024)
-
Profiling human brain vascular cells using single-cell transcriptomics and organoids
Nature Protocols (2024)
-
The role of cardiac pericytes in health and disease: therapeutic targets for myocardial infarction
Nature Reviews Cardiology (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.