Abstract
Objective:
To investigate the effect of placental pathology on neonatal neutrophils, platelets, hematocrit and nucleated red blood cells in very low birthweight (VLBW) infants born to mothers with preeclampsia.
Study Design:
Retrospective cohort study of infants with birthweight < 1500 g born to mothers with preeclampsia from july, 2002 to july, 2006 at a single level III neonatal intensive care unit. Placental pathology was reviewed for the presence of placental infarction and vasculopathy. Hematologic parameters from day of life 0, 1 and 2 were obtained. Statistical analysis included repeated-measures analysis of variance and multivariable analysis using logistic regression.
Result:
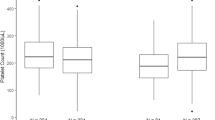
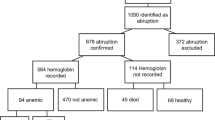
The study sample included 203 infants with estimated gestational age of 28±3 weeks; 45% had placental infarctions and 26% placental vasculopathy. Infants with neutropenia and thrombocytopenia did not have an increased occurrence of placental infarction or maternal vasculopathy but were more likely to be of small gestational age (SGA) and of lower gestational age compared with infants without neutropenia or thrombocytopenia. After multivariable analysis, gestational age and SGA remained associated with both neutropenia and thrombocytopenia whereas placental infarction and vasculopathy did not remain in the models.
Conclusion:
In our population of VLBW infants born to mothers with preeclampsia, placental pathology was common. There was no association of placental infarction or vasculopathy with neonatal neutropenia and thrombocytopenia. The data suggest that neonatal hematologic effects of maternal preeclampsia, if related to the placenta, are associated with factors other than placental histology.
This is a preview of subscription content, access via your institution
Access options
Similar content being viewed by others
References
Koenig JM, Christensen RD . Incidence, neutrophil kinetics, and natural history of neonatal neutropenia associated with maternal hypertension. N Engl J Med 1989; 321: 557–562.
Koenig JM, Christensen RD . The mechanism responsible for diminished neutrophil production in neonates delivered of women with pregnancy-induced hypertension. Am J Obstet Gynecol 1991; 165: 467–473.
Christensen RD, Henry E, Wiedmeier SE, Stoddard RA, Lambert DK . Low blood neutrophil concentrations among extremely low birthweight neonates: data from a multihospital health-care system. Journ of Perinatol 2006; 26: 682–687.
Burrows RF, Andrew M . Neonatal thrombocytopenia in the hypertensive disorders of pregnancy. Obstet Gynecol 1990; 76 (2): 234–238.
Murray NA, Roberts I . Circulating Megakaryocytes and Their Progenitors in Early Thrombocytopenia in Preterm Neonates. Pediatric Research 1996; 40: 112–119.
Beiner M, Simchen M, Sivan E, Chetrit AM, Kuint J, Schiff E . Risk factors for neonatal thrombocytopenia. Am Journ of Perinat 2003; 20: 49–54.
Chakravorty S, Murray N, Roberts I . Neonatal Thrombocytopenia. Early Hum Dev 2005; 81: 35–41.
Fraser SH, Tudehope DI . Neonatal neutropenia and thrombocytopenia following maternal hypertension. Journ of Ped and Child Health 1996; 32: 31–34.
Soma H, Yoshida K, Mukaida T, Tabuchi Y . Morphologic changes in the hypertensive placenta. Contrib Gynecol Obstet 1982; 9: 58–75.
Ghidini A, Salafia CM, Pezullo JC . Placental vascular lerions and likelihood of diagnosis of preeclampsia. Obstet Gynecol 1997; 50: 542–545.
ACOG Committee on Obstetric Practice. ACOG practice bulletin. Diagnosis and management of preeclampsia and eclampsia. No. 33, January 2002. American College of Obstetricians and Gynecologists. Obstet Gynecol 2002; 99: 159–167.
Langston C . Practice guideline for examination of the placenta. Arch Pathol Lab Med 1997; 121: 449–476.
Kurman R . Blaustein's Pathology of the Female Genital Tract 5th edn. Springer: New York, 2002, pp 1103–1192.
Sola M, Del Veechio A, Rimsza L . Evaluation and treatment of thrombocytopenia in the neonatal intensive care unit. Clin Perinatol 2000; 27: 655–679.
Mouzinho A, Rosenfeld CR, Sanchez PJ, Risser R . Revised reference ranges for circulating neutrophils in very-low-birthweight neonates. Pediatrics 1994; 94: 76–82.
Roberts I, Murray NA . Neonatal Thrombocytopenia: causes and management. Arch Dis Child Fetal Neonatal Ed 2003; 88: F359–F364.
Redline RW, Patterson P . Patterns of placental injury. Correlations with gestational age, placental weight and clinical diagnoses. Arch Pathol Lab Med 1994; 118: 698–701.
Salafia CM, Pezullo JC, Ghidini A, Lopez-Zeno JA . Clinical correlations of patterns of placental pathology in preterm preeclampsia. Placenta 1998; 19: 67–72.
Kush ML, Gortner L, Harman CR, Baschat AA . Sustained hematological consequences in the first week of neonatal life secondary to placental dysfunction. Early Hum Devel 2006; 82: 67–72.
Axt-Fleidner R, Hendrik HJ, Schmidt W . Nucleated red blood cell counts in growth-restricted neonates with absent or reversed-end-diastolic umbilical artery velocity. Clin Exp Obst and Gyn 2002; 29: 242–246.
Tauscher MK, Berg D, Brockmann M, Seidenspinner S, Speer CP, Groneck P . Association of histologic chorioamnionitis, increased levels of cord blood cytokines, and intracerebral hemorrhage in preterm neonates. Biology of the Neonate 2003; 83: 166–170.
Kim CJ, Yoon BH, Park SS, Kim MH, Chi JG . Acute funisitis of preterm but not term placentas in associated with severe fetal inflammatory response. Hum Pathol 2001; 32: 623–629.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zook, K., Mackley, A., Kern, J. et al. Hematologic effects of placental pathology on very low birthweight infants born to mothers with preeclampsia. J Perinatol 29, 8–12 (2009). https://doi.org/10.1038/jp.2008.104
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2008.104
Keywords
This article is cited by
-
Association of placental histology and neonatal hematologic outcomes
Journal of Perinatology (2023)
-
Vascular placental pathology and the relationship between hypertensive disorders of pregnancy and neonatal outcomes in very low birth weight infants
Journal of Perinatology (2018)