Abstract
Purpose
To investigate whether interleukine-8 (IL-8) and monocyte chemoattractant protein-1 (MCP-1) are related with macular oedema in patients with branch retinal vein occlusions (BRVOs).
Design
Retrospective case–control study.
Participants
Nineteen patients who had macular oedema due to BRVO and nine patients with non-ischaemic ocular diseases (control group).
Methods
Macular oedema was examined by optical coherence tomography. Both venous blood and vitreous samples were obtained at the time of vitreoretinal surgery. IL-8 and MCP-1 levels in vitreous fluid and plasma were determined with enzyme-linked immunosorbent assay kits. Variables were compared with the Mann–Whitney U-test, Wilcoxon's signed-ranked test, and the χ2-test, when appropriate. To examine correlations, Spearman's rank-order correlation coefficients were calculated. Statistical significance was set at P<0.05.
Results
The vitreous fluid levels of IL-8 (median: 63.5 pg/ml) and MCP-1 (median: 1522.4 pg/ml) were significantly higher in the patients with BRVO than in the control group (median: 5.1 and 746.5 pg/ml respectively; P<0.001 and <0.001 respectively). Vitreous IL-8 and MCP-1 were significantly correlated in patients with BRVO (P=0.009).
Conclusions
Both IL-8 and MCP-1 were elevated in the vitreous fluid of patients with BRVO and macular oedema. Both chemokines may contribute to the pathogenesis of macular oedema in patients with BRVO.
Similar content being viewed by others
Introduction
Macular oedema often complicates branch retinal vein occlusion (BRVO) and causes a reduction in visual acuity.1 Increased vascular permeability due to conformational changes in the tight junctions of retinal vascular endothelial cells is thought to be a fundamental event in the pathogenesis of macular oedema.2 Some cytokines, such as vascular endothelial growth factor (VEGF) and interleukine-6 (IL-6), provoke these changes,2, 3, 4 and their vitreous levels are elevated in patients with BRVO and central retinal vein occlusion (CRVO).5, 6
Chemokines are chemoattractant cytokines involved in the recruitment of inflammatory cells. IL-8 is the most important C-X-C chemokine and monocyte chemoattractant protein-1 (MCP-1) the most important C-C chemokine. Experimental studies have shown that both IL-8 and MCP-1 increase blood–brain barrier permeability, and that MCP-1 causes alteration of tight junctions in brain endothelial cells.7, 8, 9 Moreover, both IL-8 and MCP-1 are expressed by human retinal endothelial cells and retinal pigment epithelial cells (HRPE).10 In this study, we measured the concentrations of IL-8 and MCP-1 in vitreous fluid of patients with macular oedema secondary to BRVO to investigate the relationship between the development of macular oedema and the vitreous levels of these chemokines.
Materials and methods
Subjects
The study included non-diabetic patients with BRVO and secondary macular oedema involving the fovea, who had been enrolled in a study to assess the role of adventitia sheath dissection in the management of this condition. Exclusion criteria for this study were duration of BRVO more than 4 weeks and presence of ischaemic areas on fundus fluorescein angiography (FFA) imaging. If retinal haemorrhages precluded proper assessment of ischaemia but cotton wool spots were observed patients were also excluded. In addition, patients were excluded if they had a history of retinal photocoagulation or intraocular treatment with any drug, steroid use, ocular surgery during the past 3 months, or uveitis or vitreal haemorrhage. Nineteen patients with BRVO were included. Vitreous fluid samples were also obtained from nine patients with non-ischaemic ocular diseases to serve as controls. The same exclusion criteria were applied. The control group included six patients with macular epiretinal membrane and three patients with a macular hole. Baseline characteristics of the patients are shown in Table 1. Characteristics of BRVOs are summarized in Table 2. Informed consent was obtained from each participant following an explanation of the purpose and potential adverse effects of the procedures. This study was performed in accordance with the Declaration of Helsinki Principles and was approved by the ethics committee of our hospital.
Ophthalmologic examinations
Preoperative examinations included determination of visual acuity using Snellen charts, a complete biomicroscopic evaluation, measurement of intraocular pressure with a Goldmann tonometer, and fundus examination using a quadraspheric fundus contact lens (Volk Optical Inc, Mentor, Ohio, USA). Macular oedema was confirmed by FFA performed with a Topcon TRC-50IX fundus camera, and using optical coherence tomography (OCT) (Zeiss-Humphrey Ophthalmic Systems, Dublin, CA, USA), which was also used to measure retinal thickness at the central fovea. This latter parameter was defined as the distance between the inner limiting membrane and the retinal pigment epithelium, including serous detachments.
Idiopathic epiretinal membrane and macular hole were diagnosed on clinical criteria and using OCT.
Vitreous samples
Undiluted vitreous samples (1 ml) were obtained at the start of vitrectomy by aspiration into a 1 ml syringe attached to the vitreous cutter, subsequently transferred to a sterile tube, and then frozen at −80°C until analysis. For plasma determinations, blood samples were collected at the same time as the vitrectomy and centrifuged at 1600 × g for 10 min at 4°C. Aliquots of plasma were obtained and stored at −80°C until assayed.
Measurement of IL-8 and MCP-1
Enzyme-linked immunosorbent assay to measure IL-8 and MCP-1 in vitreous and plasma samples was performed with commercial kits (QuantiGlo Human IL-8 and Quantikine Human CCL2/MCP-1; R&D Systems, Minneapolis, MN, USA). According to the manufacturer the minimum detectable concentrations of IL-8 and MCP-1 were 0.28 pg/ml (inter-assay coefficient of variation (CV) 6.0–11.5%) and 5.0 pg/ml (inter-assay CV 4.6–6.7%) respectively.
Statistical analysis
Data are presented as the mean±standard deviation, or the median and range. Unpaired continuous variables were compared with the Mann–Whitney U-test. Wilcoxon's signed-ranked test was used to compare paired continuous variables, and the χ2-test to compare discrete variables. To examine correlations, we calculated Spearman's rank-order correlation coefficients. Statistical significance was set at P<0.05. All statistical analyses were performed with SPSS, version 13.0 (SPSS Inc, Chicago, IL, USA).
Results
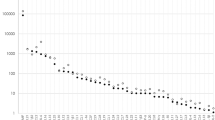
The concentration of IL-8 in vitreous fluid was significantly higher in patients with BRVO than in the control patients (63.5 pg/ml (25–240.1) vs 5.1 pg/ml (2.3–18.3); P<0.001). The vitreous concentration of IL-8 was 8.5-fold higher than the plasma concentration in BRVO patients (63.5 pg/ml (25–240.1) vs 7.5 (1.3–23.8); P<0.001), whereas there were no differences in the control patients (5.1 pg/ml (2.3–18.3) vs 7.4 (4.9–29.4); P=0.8) (Figure 1). The vitreous fluid concentration of MCP-1 was also significantly higher in BRVO patients than in the controls (1522.4 pg/ml (462.7–3445.3) vs 746.5 (479.7–980.3); P<0.001). In BRVO patients, the vitreous concentration of MCP-1 was fivefold higher than the plasma concentration (1522.4 pg/ml (462.7–3445.3) vs 312 pg/ml (134.5–694); P<0.001) and in control patients it was twofold higher than the plasma concentration (746.5 pg/ml (479.7–980.3) vs 369.6 (269.5–436.6); P=0.002) (Figure 2). There was a statistically significant correlation between vitreous concentrations of IL-8 and MCP-1 in patients with BRVO (ρ=0.579, P=0.009; Figure 3).
No correlation was observed between vitreous and plasma concentrations of IL-8 (ρ=0.151, P=0.538) and MCP-1 (ρ=0.070, P=0.775) in patients with BRVO.
There was no significant correlation between vitreous concentrations of either factor or central macular thickness (IL-8, ρ=−0.036, P=0.880; MCP-1, ρ=−0.04, P=0.861).
Conclusion
Branch retinal vein occlusion is the second most common cause of retinal vascular disease after diabetic retinopathy.11 Interruption of venous flow in these eyes almost always occurs at an arteriovenous intersection, where a retinal artery crosses a retinal vein. Thrombus formation or focal endothelial swelling occurs at the crossing site and results in elevated venous pressure, which leads to macular oedema, ischaemia, and haemorrhage. Standard care for macular oedema consists of laser photocoagulation in a grid pattern throughout the leaking area. This treatment is based on the results from the Branch Vein Occlusion Study, which showed that macular grid laser improves visual acuity in selected patients. In patients with persistent BRVO for more than 3 months, visual acuity was less than 20/40 and oedema affected the fovea.11 Nonetheless, although central vision improves after laser treatment, scotomas and reduced retinal function have been reported at follow-up.12, 13, 14 Hence, new therapeutic options may be warranted to avoid this complication.
In recent years, research has focused on the role of cytokines in the pathogenesis of macular oedema. VEGF and IL-6 cause conformational changes in retinal endothelial cells that increase their permeability.2, 3, 4 Vitreous levels of VEGF and IL-6 have been found to be elevated in patients with BRVO and CRVO;5, 6 hence, both cytokines may contribute to oedema formation in these patients. Intravitreal anti-VEGF treatment reduces macular oedema and increases visual acuity, supporting the concept that this peptide is an important contributor to the pathogenesis of oedema.15, 16, 17 Intravitreal triamcinolone also achieves a reduction in macular oedema, and this fact points to inflammation as an important event occurring after BRVO and CRVO.18, 19, 20, 21
The chemokine family of cytokines is mainly considered to be pro-inflammatory; they are inducible in inflammatory conditions and function primarily as chemoattractants and activators of specific leucocytes at the sites of inflammation. The most important chemokine is IL-8, which has been recognized as a potent chemoattractant and activator of neutrophils and T lymphocytes, but not monocytes, and MCP-1, which exhibits chemoattractant potential for monocytes and lymphocytes, but not for neutrophils. Tight junctions of endothelial cells from different tissues are reported to be regulated by both IL-8 and MCP-1. In one study using primary cultures of mouse brain endothelial cells, MCP-1 induced re-organization of actin cytoskeleton and re-distribution of tight junction proteins, ZO-1, ZO-2, occludin, and claudin-5. These morphological changes were associated with an increase in permeability.22 In another study, addition of IL-8 to monolayers of the human dermal microvascular endothelial cell line HMEC-1 caused changes in tight junction structure; the changes were inhibited by IL-8 antibodies.23
The role of IL-8 and MCP-1 in eye disease has also been investigated. In vitro expression and production of IL-8 and MCP-1 by human retinal endothelial cells and HRPE after stimulation by pro-inflammatory cytokines have been reported.10 MCP-1 significantly reduced ZO-1 protein expression in a mouse model of experimental autoimmune uveoretinitis.24 Recently, Funk et al25 reported elevated aqueous humour levels of IL-8 and MCP-1 in patients with CRVO, but not in those with BRVO. In this study we investigated whether IL-8 or MCP-1 are related with macular oedema in patients with BRVO by measuring the vitreous fluid levels of these chemokines. Analysis of vitreous fluid is a better method than aqueous humour analysis to investigate the role of peptides in retinal disease, because of its proximity to retinal tissue. Moreover, it may contain cells that secrete these factors. To investigate the source of MCP-1 and IL-8, we also measured the plasma levels of these chemokines. Vitreous fluid IL-8 and MCP-1 levels were elevated in comparison to plasma levels in patients with BRVO, and there was no statistical correlation between vitreous fluid and plasma levels of either IL-8 or MCP-1. These results suggest that the elevated vitreous concentration of these chemokines is caused by intraocular hyperproduction, a conclusion supported by studies reporting IL-8 and MCP-1 production by human retinal endothelial cells.10 In the control group, comprised of patients with macular hole and macular epiretinal membrane, vitreous MCP-1 was higher than plasma MCP-1, suggesting that there is intraocular production of this chemokine.
We found that vitreous levels of IL-8 and MCP-1 were significantly higher in patients with BRVO than in the control subjects. In the study by Funk et al,25 the levels of both chemokines in aqueous humour were elevated in patients with CRVO, but not BRVO, compared with control subjects. As was stated by the authors, extension of the area of thrombosis may explain the higher concentrations of chemokines in CRVO. Nonetheless, we found elevated vitreous concentrations also in BRVO. As has been mentioned earlier, vitreous fluid analysis is a better specimen for investigating retinal physiology than aqueous humour analysis and this may explain the differences with respect to study by Funk et al. Our findings suggest that IL-8 and MCP-1, and hence inflammation, contribute to the development of macular oedema in BRVO. An inflammatory response has been reported after systemic venous thrombotic events. Roumen-Klappe et al26 found high plasma levels of IL-8 and IL-6 in patients with deep venous thrombosis. In an experimental baboon model, level of IL-6 and IL-8 peaked on day 2 after stasis-induced deep venous thrombosis and was associated with a venous inflammatory response consisting of early neutrophil infiltration into the vein wall, followed by extravasation of monocytes, macrophages, and lymphocytes.27 Interestingly, Yoshida et al28 reported that thrombin, a peptide whose main actions are related with clot formation (ie, converting fibrinogen to fibrin and activating platelet adhesion, aggregation, and secretion), induces secretion and mRNA expression of IL-8 and MCP-1 by HRPE cells. The inflammatory response elicited after a thrombotic event is needed for resolution of the thrombus.29 We speculate that this physiological response may contribute to disruption of the blood–retina barrier and formation of oedema due to the action on tight junctions mentioned earlier.
It should be mentioned that VEGF, probably the best known peptide related with permeability and angiogenesis, induces endothelial cell production of IL-8 and other cytokines, such as IL-6 and growth-related oncogen-α.30
We believe that thrombosis may be the stimulating agent for the increased levels of both chemokines. Moreover, previous reports have shown that retinal ischaemia stimulates IL-8 and MCP-1 production, and both chemokines are involved in retinal neovascularization.31, 32, 33, 34 Although ischaemia as seen using FFA was one of the exclusion criteria, we cannot absolutely exclude that this was present in our patients. So retinal ischaemia may have also contributed to hyperproduction of IL-8 and MCP-1.
We did not find a statistical correlation between macular thickness and vitreous IL-8 and MCP-1 levels. We believe that these chemokines contribute to oedema formation, but that many other peptides may also be involved, and some of them (eg, VEGF) may have a greater and more determinant role in regulating vascular permeability. In fact, Noma et al5 reported a statistical correlation between vitreous fluid levels of VEGF and IL-6 and foveal thickness in patients with BRVO.
Our study has some limitations. First, chemokine levels may have been elevated before the development of retinal vein thrombosis and not afterwards, and acted as risk factors for the development of BRVO. Vitreous samples in patients at risk of developing BRVO should be analysed to exclude this point, but such a study would be ethically unacceptable. Second, we have not corrected the concentration of the peptides under study for the total vitreal protein levels because of a small volume of the sample. However, plasma concentrations of both chemokines were strikingly lower than those obtained in the vitreous (∼8.5 time less for IL-8 and ∼5 time less for MCP-1). Therefore it seems clear that the elevated concentrations found in the vitreous fluid are not derived from blood. Last, further studies should be carried out to elucidate the role of IL-8 and MCP-1 in the regulation of tight junctions of retinal endothelial cells. Exposure of these cells to chemokines and study of the conformational changes occurring in the components of the tight junctions or transendothelial permeability could clarify this point.
In summary, vitreous levels of MCP-1 and IL-8 are elevated in patients with BRVO. Our study results suggest that intraocular synthesis is responsible for this increase. Inflammation associated with thrombotic events might be the stimulating agent for hypersecretion of these chemokines. Retinal ischaemia may also be related to this hypersecretion. IL-8 and MCP-1 may contribute to increased vascular permeability and macular oedema in patients with BRVO.

References
Ryan SJ . Retina. 3rd Vol, 3rd ed. Mosby: St Louis, 2001.
Vinores SA, Derevjanik NL, Ozaki H, Okamoto N, Campochiaro PA . Cellular mechanisms of blood–retinal barrier dysfunction in macular edema. Doc Ophthalmol 1999; 97: 217–228.
Gardner TW, Antonetti DA, Barber AJ, Lieth E, Tarbell JA, Penn State Retina Research Group. The molecular structure and function of the blood–retina barrier. Doc Ophthalmol 1999; 97: 229–237.
Maruo N, Morita I, Shirao M, Murota S . IL-6 increases endothelial permeability in vitro. Endocrinology 1992; 131: 710–714.
Noma H, Minamoto A, Funatsu H, Tsukamoto H, Nakano K, Yamashita H et al. Intravitreal levels of vascular endothelial growth factor and interleukine-6 are correlated with macular edema in branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 2006; 244: 309–315.
Noma H, Funatsu H, Mimura T, Harino S, Hori S . Vitreous levels of interleukine-6 and vascular endothelial growth factor in macular edema with central retinal vein occlusion. Ophthalmology 2009; 116: 87–93.
Theoharides TC, Rozmieki JJ, Sahagian G, Jocobson S, Kempuraj D, Conti P et al. Impact of stress and mast cells on brain metastases. J Neuroimmunol 2008; 205: 1–7.
Veldhuis WB, Floris S, van der Meide PH, Vos IM, de Vries HE, Dijkstra CD et al. Interferon-beta prevents cytokine neutrophil infiltration and attenuates blood–brain barrier disruption. J Cereb Flow Metab 2003; 23: 1060–1069.
Stamatovic SM, Shakui P, Keep RF, Moore BB, Kunkel SL, Van Rooijen N et al. Monocyte chemoattractant protein-1 regulation of blood–brain barrier permeability. J Cereb Blood Flow Metab 2005; 25: 593–606.
Crane IJ, Wallace CA, MCkillop-Smith S, Forrester JV . Control of chemokine production at the blood–retina barrier. Immunology 2000; 101: 426–433.
The Branch Vein Occlusion Study Group. Argon laser photocoagulation for macular edema in branch vein occlusion. Am J Ophthalmol 1984; 98: 271–282.
Hara A, Nagatomo M . Branch retinal vein occlusion decreases the potential of the inner retinal layer. Nippon Ika Daigaku Zasshi 1995; 62: 50–54.
The Branch Vein Occlusion Study Group. Argon laser scatter photocoagulation for prevention of retinal neovascularization and vitreus haemorrhage in branch vein occlusion. A randomized clinical trial. Arch Ophthalmol 1986; 104: 34–41.
Barbazetto IA, Schmidt-Erfurth MD . Evaluation of functional defects in branch retinal vein occlusion before and after treatment with scanning laser perimetry. Ophthalmology 2000; 107: 1089–1098.
Kriechbaum K, Michels S, Prager F, Georgopoulos M, Funk M, Geitzenauer W et al. Intravitreal Avastin for macular oedema secondary to retinal vein occlusion: a prospective study. Br J Ophthalmol 2007; 92: 518–522.
Rosenfeld PJ, Fung AE, Puliafito CA . Optical coherence findings after an intravitreal injection of bevacizumab (Avastin) for macular edema from central retinal vein occlusion. Ophthalmic Surg Lasers Imaging 2005; 36: 336–339.
Iturralde D, Spaide RF, Meyerle CB, Klancnik JM, Yannuzzi LA, Fisher YL et al. Intravitreal bevacizumab (Avastin) treatment for macular edema in central retinal vein occlusion: a short term study. Retina 2006; 26: 279–284.
Roth DB, Cukras C, Radhakrishnan R, Feuer WJ, Yarian DL, Green SN et al. Intravitreal triamcinolone acetonide injections in the treatment of retinal vein occlusions. Ophthalmic Surg Lasers Imaging 2008; 39: 446–454.
Cakir M, Dogan M, Bayraktar Z, Bayraktar S, Acar N, Altan T et al. Efficacy of intravitreal triamcinolone for the treatment of macular edema secondary to branch retinal vein occlusions in eyes with or without grid laser photocoagulation. Retina 2008; 28: 465–472.
Karacorlu M, Karacorlu SA, Ozdemir H, Senturk F . Intravitreal triamcinolone for the treatment of the serous detachment in central retinal vein occlusions. Retina 2007; 27: 1026–1030.
Moschos MM, Brouzas D, Loukianou E, Apostolopoulos M, Moschos M . Intraocular triamcinolone acetonide for macular edema due to CRVO A multifocal-ERG and OCT study. Doc Ophthalmol 2007; 114: 1–7.
Stamatovic SM, Keep RF, Kunkel SL, Andjelkovic AV . Potential role of MCP-1 in endothelial cell tight junction ‘opening’: signaling via Rho and Rho kinase. J Cell Sci 2003; 116: 4615–4628.
Talavera D, Castillo AM, Dominguez MC, Gutierrez AE, Meza I . IL8 release, tight junction and cytoskeleton dynamic reorganization conducive to permeability increase are induced by dengue virus infection of microvascular endothelial monolayers. J Gen Virol 2004; 85: 1801–1813.
Xu H, Dawson R, Crane IJ, Liversidge J . Leucocyte diapedesis in vivo induces transient loss of tight junction protein at the blood–retina barrier. Invest Ophthalmol Vis Sci 2005; 46: 2487–2494.
Funk M, Kriechbaum K, Prager F, Benesch T, Georgopoulos M, Zlabinger GJ et al. Intraocular concentrations of growth factors and cytokines in retinal vein occlusions and the effect of therapy with bevacizumab. Invest Ophthalmol Vis Sci 2009; 50: 1025–1032.
Roumen-Klappe EM, den Heijer M, van Uum SHM, van der Ven-Jongekrijg J, van der Graaf F, Wollersheim H . Inflammatory response in the acute phase of deep vein thrombosis. J Vasc Surg 2002; 35: 701–706.
Wakefield TW, Greenfield LJ, Rolfe MW, DeLucia III A, Strieter RM, Abrams GD et al. Inflammatory and procoagulant mediator interactions in an experimental baboon model of venous thrombosis. Thromb Haemost 1993; 69: 164–172.
Yoshida A, Elner SG, Bian ZM, Kunkel SL, Lukacs NW, Elner VM . Thrombin regulates chemokine induction during human retinal pigment epithelial cell/monocyte interaction. Am J Pathol 2001; 159: 1171–1180.
Shbaklo H, Holcroft CA, Kahn SR . Levels of inflammatory markers and the development of the post-thrombotic syndrome. Thromb Haemost 2009; 101: 505–512.
Hao Q, Wang L, Tang H . Vascular endothelial growth factor induces protein kinase D-dependent production of pro-inflammatory cytokines in endothelial cells. Am J Physiol Cell Physiol 2009; 296 (4): C821–C827.
Jo N, Wu GS, Rao Na . Upregulation of chemokine expression in the retinal vasculature in ischemia- reperfusion injury. Invest Ophthalmol Vis Sci 2003; 44: 4054–4060.
Davies MH, Eubanks JP, Powers MR . Microglia and macrophages are increased in response to ischemia-induced retinopathy in the mouse retina. Mol Vis 2006; 12: 467–477.
Yoshida S, Yoshida A, Ishibashi T, Elner SG, Elner VM . Role of MCP-1 and MIP-alpha in retinal neovascularization during postischemic inflammation in a mouse model of retinal neovascularization. J Leukoc Biol 2003; 73: 137–144.
Yoshida S, Yoshida A, Ishibashi T . Induction of IL-8, MCP-1 and bFGF by TNF in retinal ganglion cells: implications for retinal neovascularization during post-ischemic inflammation. Graefes Arch Clin Exp Ophthalmol 2004; 242: 409–413.
Acknowledgements
This study was financially supported by Instituto de Salud Carlos III, Madrid, Grant number FIS PI/060803.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This study was partially presented in 2009 ARVO meeting as a poster.
Rights and permissions
About this article
Cite this article
Fonollosa, A., Garcia-Arumi, J., Santos, E. et al. Vitreous levels of interleukine-8 and monocyte chemoattractant protein-1 in macular oedema with branch retinal vein occlusion. Eye 24, 1284–1290 (2010). https://doi.org/10.1038/eye.2009.340
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2009.340
Keywords
This article is cited by
-
The correlation between cytokine levels in the aqueous humor and the prognostic value of anti-vascular endothelial growth factor therapy for treating macular edema resulting from retinal vein occlusion
Graefe's Archive for Clinical and Experimental Ophthalmology (2021)
-
Mo-derived perivascular macrophage recruitment protects against endothelial cell death in retinal vein occlusion
Journal of Neuroinflammation (2019)
-
Combination of Bevacizumab and NGF Reduces the Risk of Diabetic Retinopathy
Cell Biochemistry and Biophysics (2015)