Abstract
The clinical value of 131I-MIBG for targeted imaging and targeted radiotherapy is limited to neural crest-derived tumors expressing human norepinephrine transporters (hNET) protein. To extend 131I-MIBG-targeted therapy to other nonexpressed hNET tumors, this study investigated the hNET expression in vitro and in vivo in HepG2 hepatoma mediated by recombinant adenovirus encoding the hNET gene (Ad-hNET). For this purpose, the HepG2 cells showed a 4.87-fold increase in 125I-MIBG uptake after infection with Ad-hNET, and the uptake of 125I-MIBG could be specifically inhibited by maprotiline. Immunohistological analysis, in vivo biological study and 131I-MIBG scintigraphic imaging also revealed the high expression of hNET protein in hepatoma. This in vitro and in vivo studies demonstrate the feasibility of hNET gene transfer, meditated by adenovirus vector, could extend to tumors other than those derived from the neural crest, which provides a sound foundation for further investigation of hepatocellular carcinoma-targeted radiotherapy mediated by adenovirus transfection with hNET gene.
Similar content being viewed by others
Introduction
Hepatocellular carcinoma (HCC) ranks among the deadliest cancers worldwide.1, 2 The traditional treatment for HCC includes surgical resection, liver transplantation, chemotherapy and radiotherapy. Surgical resection or liver transplantation is a curative treatment, but only a minority of patients are eligible; furthermore, recurrence rates for those who undergo resection approach 70%.3 Chemotherapy and radiotherapy can palliate patient's condition, but may lead to acute or chronic side-effects owing to damage to normal structures.4 Despite advances in HCC therapy, overall patients' outcomes have not substantially improved.5
As a metabolically stable false analog of norepinephrine, radioiodine-labeled MIBG has been used for a long time for targeted imaging and radiotherapy in patients with neural crest-derived tumors such as neuroblastomas or pheochromocytomas,6, 7 owing to the high expression of the human norepinephrine transporter (hNET) in the tumors, which can uptake and accumulate radioiodine-labeled MIBG.8, 9, 10 hNET is a transmembrane protein (617 amino acids), which belongs to a family of Na+/Cl–-dependent transporters and mediates the re-uptake transport of norepinephrine, dopamine and epinephrine from the presynaptic membrane.11, 12 Human, bovine, rat and mouse norepinephrine transporter complementary DNAs (cDNAs) have been cloned.11, 13
However, hNET is only expressed in a narrow range of tumor types. For other tumors, which have insufficient expression or nonexpression of hNET, the clinical use of 131I-MIBG radiotherapy is limited. To extend 131I-MIBG-targeted therapy to those nonexpressed hNET tumors, several studies have shown that transfer of the hNET or bovine norepinephrine transporter gene into other nonexpressed tumor cells, either by transfection with a eukaryotic expression vector of NET cDNA14, 15 or with a retroviral vector16, 17, 18 can lead the transduced cells to express hNET protein and uptake of 131I-MIBG to achieve targeted therapy, although the hNET expressive level and transfection efficiency is different in various studies. Coupling delivery of the hNET gene into tumor cells with radioiodine-labeled MIBG administration may, therefore, open new avenues to treat HCC and other tumors.19
The AdEasy system of adenoviral vector is a widely used, simplified system for generating recombinant adenovirus, which delivers foreign-targeted genes to a variety of cell types and tissues.20, 21 They can be easily grown to high titer and can efficiently transfer genes into both dividing and nondividing cells. The expression level of the exogenous gene by recombinant adenovirus-mediated gene delivery can be easily controlled by changing multiplicity of infection (m.o.i.). The transduction is transient but has robust expression of the transgene, whereas the viral genome rarely integrates into the host chromosome.22 Furthermore, toxicity has been reduced in advanced adenoviral vectors warranting stable and high-level transgene expression.22
In a previous study, we successfully constructed a recombinant adenovirus encoding hNET gene (Ad-hNET) using the AdEasy adenovirus system.23 The objective of this study was to further demonstrate the feasibility of using an adenoviral vector to deliver the hNET gene into HepG2 hepatoma cells in vitro and in vivo.
Materials and methods
Chemical and biological reagents
The pCMV5-hNET plasmid was a generous gift from Amara SG.11 The AdEasy adenovirus system was obtained from Qbiogene (Carlsbad, CA). Mouse monoclonal (NET17-1) to noradrenaline transporter was purchased from Abcam Inc. (Cambridge, MA); goat anti-mouse immunoglobulin G antibody, chemically conjugated to horseradish peroxidase, was obtained from Zhongshan Biotech Company (Beijing, China); mouse anti-GAPDH monoclonal immunoglobulin G was obtained from Shanghai Kangcheng Biotech Company (Shanghai, China); Maprotiline was obtained from Ciba Geigy (Basel, Switzerland). 125I-MIBG and 131I-MIBG used in this work were prepared using the method of Vaidyanathan et al.24 All other reagents used were purchased locally.
Instruments and equipments
AA2250 electronic balance was obtained from Denver Instrument (Denver, CO), FJ-2021γ-radioimmunity counter was obtained from Xian NO. 262 Factory (Xian, Shanxi province, China), and also included siemens high-energy mobile γ-camera (Orbiter; Siemens Medical Systems Erlangen, Germany).
Cell lines
HepG2 cell line was obtained from the State Key Laboratory of Biotherapy, Sichuan University of China, and human neuroblastoma cell line SK-N-SH was obtained from American Type Culture Collection (Manassas, VA). HepG2 and SK-N-SH cells were cultured in the RPMI 1640 medium containing 10% heat-inactivated fetal calf serum with 100 IU ml−1 penicillin and 100 μg ml−1 streptomycin. All cells were cultured in a humidified atmosphere with 5% CO2 at 37 °C.
Construction, amplification and purification of the Ad-hNET
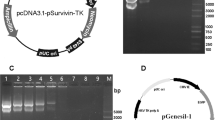
The recombinant adenovirus Ad-hNET was constructed as previously described using AdEasy adenovirus system.20, 21 Briefly, pAdTrack-CMV and pCMV5-hNET were digested with restriction endonucleases KpnI and XbaI, respectively, and then hNET cDNA fragment (approximately 1.8 kb) and pAdTrack-CMV plasmid fragment were connected with T4 DNA ligase. After transformation in colibacillus JM 109, the plasmid was extracted in small quantity, and the shuttle plasmid pAdTrack-CMV-hNET was double-enzyme identified, then it was linearized with PmeI, followed by homologous recombination with bone plasmid pAdEasy-1 in BJ 5183 cells. The DNA of identified recombinant plasmid Ad-hNET was digested with PacI and transfected to HEK 293 cells by liposome-mediated method to package adenovirus. Reverse transcriptase polymerase chain reaction (RT-PCR) has validated the target gene hNET in the recombinant plasmid, and western blot analysis proved the expression of hNET protein.23 The titer of the Ad-hNET was measured with the aid of green fluorescent protein expression after multiplication and purification. On the basis of this, we further purified the Ad-hNET by CsCl gradient ultracentrifugation and obtained the Ad-hNET with its titer of 4.0 × 1011 p.f.u. ml−1.
Optimal multiplicity of infection
To determine the optimal m.o.i. of the Ad-hNET for cell infection, we generally plated 1.0 × 106 HepG2 cells per well in a six-well plate and cultured to approximately 70% confluence the next day. At 2 days after seeding, the cells were infected with adenovirus at various m.o.i. by adding the purified Ad-hNET virus to the cells in fresh culture medium (m.o.i.=0, 10, 50, 100, 200 and 500) for HepG2 cells to confirm optimal m.o.i. Control cells were infected with blank adenovirus Ad. After 2 h of infection, the medium was changed to fresh medium without virus. At 2 days after infection, the medium was aspirated and cells were washed once with phosphate-buffered saline (PBS) (1x solution), all well-plate cells were incubated with 1.0 ml 1 × PBS (contained 0.2 μCi of 125I-MIBG), the cells were then lysed by incubation with 95% ethanol. The radioactivity of the cell lysate was measured by FJ-2021 γ-radioimmunity counter. The optimal m.o.i. in the following experiments was chosen for both the highest green fluorescent protein expression and viability.
Measurement of 125I-MIBG uptake
The HepG2 cells were seeded in six-well plates and infected with optimal m.o.i. of 100 of the Ad-hNET, as confirmed above. At the same time, other HepG2 cells were infected with blank adenovirus Ad. (m.o.i. 100) as controls. At 2 days after infection, every well-plate cells were incubated with 1.0 ml 1 × PBS (contained 0.2 μCi of 125I-MIBG) and incubated in incubator for 5, 10, 15, 20, 30, 60, 90 or 120 min, respectively, then the medium was aspirated and the cells were quickly washed twice with ice-cold Hank's buffered salt solution. Afterward, the cells were lysed by incubation with 95% ethanol, and the radioactivity of the cell lysate was measured by a γ-radioimmunity counter, accordingly.
In vitro competition experiment
The HepG2 cells were seeded in six-well plates and infected with optimal m.o.i. of the Ad-hNET. After 48 h, the cells were incubated with 1.0 ml 1 × PBS containing 0.2 μCi of 125I-MIBG and maprotiline (0, 10 and 30 μmol l−1, respectively), a selective inhibitor of noradrenaline uptake. After 30 min incubation in incubator, the cells were lysed and the radioactivity was measured by a γ-radioimmunity counter, accordingly. As control, the experiment was done in parallel with SK-N-SH cells, which naturally express the hNET protein and concentrate 125I-MIBG.25 All the above in vitro cells experiments were performed in triplicate.
Animal study protocol
BALB/c male nude mice (20±2 g, all in SPF grade, purchased from the laboratory animal center of Sichuan University) were prepared. A volume of 0.2 ml containing 1.0 × 106 suspension cells of the HepG2 cell line, were s.c. injected into both right and left flanks of 15 BALB/c nude mice to set up neoplasm transplantation models, the nude mice-bearing HepG2 hepatoma were divided randomly into five groups, each containing three mice. Experiments were performed at approximately 20 days after implantation. Tumors of the same uniform size (1.0 cm diameter) were employed.
Immunohistological analysis
Immunohistological analysis was used to investigate the expression of hNET protein in the mice model hepatoma. In this study, individual animals were injected intratumorally in one flank with the Ad-hNET and in the opposite flank with the blank adenovirus Ad. At 3 days later, the mice were killed and the bilateral tumors were obtained, and fixed in 10% formalin and embedded in paraffin. The indirect immunoperoxidase method was used to localize hNET in paraffin-embedded sections. Sections were deparaffinized and blocked for nonspecific binding of antibody with PBS containing 3% goat serum albumin for 30 min and then covered with a solution of mouse monoclonal (NET17-1) to noradrenaline transporter (1:500) for 2 h at room temperature. After three rinses with PBS, the sections were incubated for 2 h in a solution containing goat anti-mouse immunoglobulin G conjugated to peroxidase (1:150). The sections were rinsed, stained with diaminobenzidine (Sigma Chemical, St Louis, MO) chromogen, and finally mounted with neutral gum. Slides were stored in the dark at 4 °C until examined with multitrack setting of Nikon Eclipse TE 300 Inverted Microscope (Tokyo, Japan).
Biodistribution studies
A volume of 0.2 ml (corresponding to 1.0 × 1010 p.f.u. ml−1) of the Ad-hNET were injected intratumorally into the left xenograft of the nude mice, and the same titers of blank adenovirus Ad. into the right xenograft of the mice as a control. At 3 days later, 125I-MIBG (5.0 μCi) was injected into the nude mice through vena caudalis. At different time intervals after i.v. injection, the mice were killed; various organs (blood, heart, liver, spleen, lung, kidney, stomach, intestine, bone, muscle and brain) and tumors were excised and weighed; radiocounting of various major organs and tumors were determined with NaI (Tl) flat crystal counter accordingly. The percent-injected dose per gram of tissue (%ID g−1) was calculated for each specimen. The retention of activity as percentage ID in blood and muscle was estimated by the usual assumptions of 6.5% body weight for blood and 40% for muscles.26
In vivo 131I-MIBG scintigraphic imaging
The nude mice-bearing HepG2 hepatoma on both flanks were set up according to the method mentioned above, then the left and right flanks were injected intratumorally 0.2 ml (1.0 × 1010 p.f.u. ml−1) with purified recombinant adenovirus Ad-hNET and blank adenovirus Ad., respectively. At 3 days later, the nude mice were anesthetized with pentobarbital (50 mg kg−1, intraperitoneally) and administered 0.2 ml (corresponding to 500 μCi) 131I-MIBG through vena caudalis. In vivo 131I-MIBG scintigraphy were performed immediately at 30 min, 1, 4 and 24 h after injection by acquiring 5.0 × 105 counts on a 256 × 256 matrix, a 364 (keV) peak and a 20% window using a Siemens high-energy mobile γ-camera equipped with a high-energy, high-resolution parallel-hole collimator. All animal experiences were approved by the animal ethics committee of the Sichuan University.
Statistical analysis
SPSS 10.0 statistical software (SPSS, Chicago, IL) was used for all analyses. All data were expressed as mean ± s.d. values. Two-sided Student's t-tests were used for group comparisons. P<0.05 was considered statistically significant.
Results
The Ad-hNET-infected HepG2 cells
After transfection with the Ad-hNET virus at an m.o.i. of 500, almost all the HepG2 cells died because of the cytotoxicity of adenovirus. The cytopathic effect was obvious in HepG2 cells at m.o.i. of 200. HepG2 cells became round-shaped and detached from the wall in 2 days, and no more than 50% of which were alive, after 5 days. However, adenovirus-mediated hNET gene transduction did not influence the growth characteristics of HepG2 cells at m.o.i.(s) of 10, 50 and 100. Figure 1 shows that the uptake of 125I-MIBG in the Ad-hNET-transfected cells increased with increasing viral titers. The highest transfection efficiency was found to be at m.o.i. of 100 (P<0.05 compared with both m.o.i. of 10 and 50, Figure 1a) and the percentage of green fluorescent protein-positive cells reached a maximum and maintained morphologically to be spindle-shaped or fusiform cells (Figure 1b). After 30 min of incubation with 125I-MIBG, the tracer uptake in hNET-transfected cells at m.o.i. of 100 was 4.87-fold higher than that in cells transfected with control virus. Therefore, the m.o.i. of 100 was used to infect HepG2 cells in the following experiments.
125I-MIBG uptake in HepG2 cells transfected with the recombinant adenoviral Ad-hNET at various m.o.i. A m.o.i. of 0 represents control (cells infected with blank adenovirus Ad.). Two days after transfection, the 125I-MIBG accumulation in HepG2 cells increased rapidly from m.o.i. 10 to 100 (a). At m.o.i. of 100, the percentage of green fluorescent protein (GFP)-positive cells reached a maximum and maintained morphologically to be spindle-shaped or fusiform cells ( × 200) (b). Three independent experiments were performed, either in duplicate or triplicate. Significantly higher uptake of 125I-MIBG uptake at m.o.i. of 100 than that at m.o.i. of 0, 10 and 50 in HepG2 cells (*P<0.05).
125I-MIBG uptake in HepG2 cells
In the dynamic 125I-MIBG uptake study, a significant accumulation of the radiotracer was observed in the HepG2 cells transfected with the Ad-hNET (Figure 2a). At 5 min infection with the Ad-hNET, the HepG2 cells have a visible uptake of 125I-MIBG, and the maximal uptake was measured at 30 min, then it decreased steadily with time. At 120 min, the uptake of 125I-MIBG in the Ad-hNET transfected cells still kept at 64%. In contrast, HepG2 cells infected with blank adenovirus Ad. remained in a relatively certain state of 125I-MIBG uptake within 2 h.
Section A shows the dynamic uptakes of 125I-MIBG in HepG2 cell line transfected with the recombinant adenovirus Ad-hNET or with the blank adenovirus Ad. The intracellular 125I-MIBG concentration in the Ad-hNET-infected HepG2 cells was higher than that in the Ad.-infected HepG2 cell. Section B shows the uptake of 125I-MIBG was inhibited by maprotiline in a dose-dependent manner both in HepG2 cells and SK-N-SH cells transfected with the recombinant adenovirus Ad-hNET. In the presence of 10 and 30 mM maprotiline, the inhibiting rate of 125I-MIBG uptake was from 64.8 to 75.2%, respectively; and in SK-N-SH cells, the inhibiting rate was from 81.2 to 86.7%, respectively. The maprotiline-induced reduction in tracer uptake was statistically significant for both in HepG2 cells and SK-N-SH cells infected with the Ad-hNET (*P<0.05). Three independent experiments were performed in triplicate. Values are expressed as means ± s.d (n=3).
In vitro competition experiment
In the presence of maprotiline, 125I-MIBG uptake in the HepG2 cells was studied. It shows that 125I-MIBG uptake was specially inhibited by maprotiline in a dose-dependent manner in HepG2 cells infected with the Ad-hNET. In the presence of 10 mM maprotiline, 125I-MIBG uptake was inhibited by 64.8%; when incubated with 30 mM maprotiline, the inhibiting rate of 125I-MIBG concentration attained 75.2% (Figure 2b). The maprotiline-induced reduction in tracer uptake was statistically significant for the HepG2 cells infected with the Ad-hNET (P<0.05).
As a control, 125I-MIBG uptake is also specifically inhibited by maprotiline in SK-N-SK cells, whereas the result was quite different from those obtained for HepG2 cells: at an inhibitor concentration of 10 mM, the inhibiting rate already attained 81.2%; at a concentration of 30 mM, it inhibited uptake by 86.7%. The maprotiline-induced reduction in 125I-MIBG uptake was also statistically significant for the SK-N-SK cells (P<0.05) (Figure 2b).
Immunohistochemistry of bearing cancer
At 3 days after injection of the adenovirus Ad-hNET, the immunohistological slices were observed under a fluorescence microscope. It shows that the hepatoma tissue slice had hNET protein expression after intratumoral injection of Ad-hNET (Figure 3a), whereas no immunostaining could be detected in the tumors injected with the blank adenovirus Ad. (Figure 3b). Immunohistological analysis confirmed the expression of hNET protein in the hepatoma cells and localization on the surface of cytomembrane.
The expression of hNET in tumor tissue has been detected by immunohistochemistry after injection recombinant adenovirus Ad-hNET (fluorescence microscope, original magnification × 200). The paraffin-embedded tumor sections were stained with a polyclonal antibody against hNET protein (seen as brownish yellow color on HepG2 hepatoma cytomembrane) (a). No immunoreactant were found in the hepatoma tumor injected with blank adenovirus Ad (b).
Biodistribution studies
The results of biodistribution studies in nude mice model are summarized in Table 1. After 1 h intravenous injection, 125I-MIBG uptake mostly concentrated in blood and Ad-hNET tumor, which were 6.05 and 5.28 (%ID g−1), respectively. Increased activities were also observed in stomach, small intestine, spleen, liver and tumor infected with blank adenovirus Ad. At 2 h after injection, the uptake of 125I-MIBG revealed maximal 14.30 (%ID g−1) accumulation in the Ad-hNET infected tumor, whereas in other organs and tissues, including tumor infected with Ad, the 125I-MIBG uptake decreased all along the time. At 24 h after injection, 125I-MIBG uptake still kept 2.85 (%ID g−1) but more/less left in other organs and tissues, including in Ad-infected tumor. Compared with 125I-MIBG uptake in Ad-hNET-infected tumor, tumor infected with blank adenovirus Ad. showed a relatively low accumulation of 125I-MIBG at the beginning of 1 h post-intravenous injection and decreased with time. As a result, 125I-MIBG uptake in the hNET-transfected tumor was significantly higher than that in tumor transfected with blank adenovirus Ad. within 24 h (paired t-test, P<0.05), and the ratio of 125I-MIBG uptake in Ad-hNET tumor to that in Ad tumor raised with time from 1.93 to 14.33 (Table 1, Figure 4a).
The biodistribution of 125I-MIBG in hepatoma of BALB/c nude mice transfected with recombinant adenovirus Ad-hNET or with blank adenovirus Ad. (a). The uptake ratios of Ad-hNET-infected tumor/blood and Ad-hNET-infected tumor/muscle at different time after injection 125I-MIBG in BALB/c male nude mice transfected with Ad-hNET (b). Values are expressed as means±s.d. (n=3).
The tumor-to-nontumor ratios are shown in Figure 4b. At 1 h after injection, Ad-hNET-infected tumor/blood and Ad-hNET-infected tumor/muscle ratios in HepG2-bearing mice were observed to be 0.87 and 1.34 (%ID g−1), respectively. At 2 h, the ratio of Ad-hNET-infected tumor/muscle rapidly upstroked to 33.26, whereas the ratio of Ad-hNET-infected tumor/blood climbed up to 3.06. As no significant activity was present in other organs, the ratios of Ad-hNET-infected tumor/blood and Ad-hNET-infected tumor/muscle ascended obviously to 47.50 and 55.96 at 24 h after injection of 125I-MIBG, respectively (Figure 4b). The biological half-life of 125I-MIBG was calculated to be 5.47 ± 0.32 h in hepatoma infected with Ad-hNET.
In vivo 131I-MIBG scintigraphic imaging
The γ-camera imaging showed that the Ad-hNET-transfected tumor was visible at 30 min after injection of 131I-MIBG, and then the accumulation increased with time. At 24 h after injection, it was still better visualized in HepG2 tumor on the left blank. In contrast, the control tumor did not exhibit visible radioactivity accumulation compared with background levels within 24 h (Figure 5). 131I-MIBG γ-camera images also showed high tracer uptake in heart, liver, kidney, bladder and gastrointestinal tract. The in vivo scintigraphic imaging study was coincident with the biodistribution study in tumor-bearing nude mice transfected with Ad-hNET and blank adenovirus Ad., which also demonstrated that recombinant adenovirus-mediated hNET gene transfer could specially uptake radioiodine-labeled MIBG.
Scintigraphic images of tumor-bearing BALB/c male nude mice s.c. transplanted with recombinant adenovirus Ad-hNET (left flank) or blank adenovirus Ad. (right flank) at 30 min (a), 1 (b), 4 (c) and 24 h (d) after injection of 131I-MIBG. The accumulation of 131I-MIBG was visible at 30 min after injection of 131I-MIBG, and then the accumulation increased with time, at 24 h post-injection of 131I-MIBG, the tumor still showed intense tracer accumulation (closed arrows). In contrast, the tumor infected with blank adenovirus Ad. is not visible in the γ-camera images from 30 min to 24 h. Focal 131I-MIBG uptake is also seen in heart, liver, kidney, bladder and gastrointestinal tract, whereas the concentration of 131I-MIBG decreased with time and remained little at 24 h.
Discussion
The clinical value of radioiodine-labeled MIBG for targeted imaging and radiotherapy is limited to neural crest-derived tumors expressing hNET protein. To extend the application of radiotracer MIBG, the current study investigated the feasibility of the hNET protein expression in vitro and in vivo in HCC mediated by recombinant adenovirus encoding the hNET gene.
Adenoviral vectors have been widely used for gene therapy and vaccine development.27, 28 In this study, AdEasy-1 system has been selected for generation of recombinant adenoviruses encoding hNET gene. Compared with traditional adenoviral vectors, the AdEasy-1 system incorporates several unusual features. First, the viral backbone containing most of the adenoviral genome is supplied as a supercoiled plasmid rather than as linear viral DNA, which makes backbone amplification of the adenovirus much easier and also provides the possibility of generating stable recombinants. Second, the recombination step is performed in Escherichia coli rather than in mammalian cells, taking advantage of the high efficiency of homologous recombination in bacteria.28 Furthermore, there is no need to carry out laborious plaque purification rounds, which reduce the needed time to generate a recombinant adenovirus, to several weeks.
In previous study, we have successfully constructed such a recombinant adenovirus containing hNET gene by the Adeasy-1 system, and validated by RT-PCR technique and western blot analysis.23 Those works had paved the way for further evaluation of adenovirus-mediated hNET gene transduction to HCC in vitro and in vivo.
The current study convincingly demonstrated that HepG2 cells transfected with Ad-hNET could specifically express the hNET protein and actively uptake 125I-MIBG, this uptake could be specifically inhibited by maprotiline. In vivo biological study and scintigraphic imaging in nude mice model also proved the high expression of hNET protein in hepatoma. Combination of hNET gene transduction with radiopharmaceutical tracer technique develops a new strategy for targeted radiotherapy and therapeutic efficacy monitoring in the tumors other than those derived from the neural crest.
The m.o.i. is the number of viral particles per cell that is desired during the infection reaction. Different types of cells have different m.o.i (s). The optimal m.o.i. should display high transfection efficiency with low cellular toxicity.29 In this study, we found that when the Ad-hNET virus was at an m.o.i. of 100, the growth characteristics of the HepG2 cells was not influenced under conditions, which allowed for higher efficiency and low toxicity of adenoviral infection, and the maximal uptake of 125I-MIBG in transfected HepG2 cells was almost fivefold higher than that cells transfected with control virus. Therefore, the optimal m.o.i. of the Ad-hNET-infected HepG2 cells was confirmed to be 100.
Previous study reported that the hNET-expressing hepatoma cells accumulated up to 36-fold-higher MIBG uptake compared with wild-type cells and eightfold higher compared with hNET-expressing neuroblastoma cell line SK-N-SH after retrovirus-mediated gene transfer of hNET gene into Morris hepatoma cells.16 Furthermore, in a recent study, Anton et al.17 also showed that human A431, HT1080 and murine CMS-5 cells retrovirally transduced with bovine NET cDNA had a 66- to 120-fold higher 131I-MIBG uptake than parental cells. However, in our study, we found a 4.87-fold-higher 125I-MIBG uptake in hepatoma cells transfected with the hNET gene compared with noninfected hepatoma cells. This is quite different from previous studies. The reason for this difference is mainly because of the higher basic uptake in HepG2 cells, transfected with blank adenovirus Ad. in our study, which leads to the reduction in the ratio of 125I-MIBG uptake in hNET transferred HepG2 cells to non-hNET-transferred HepG2 cells. Possible reasons could be explained as follows: (1) hepatoma cells have the general trend of higher hepatic uptake for compounds with greater lipophilicity. As MIBG is a lipophilic and cationic compound,30 the basic uptake of 125I-MIBG was higher in HepG2 cells; (2) the heterogeneity of different tumor cells is cellular and molecular. It is known that different cell types show variable degrees of susceptibility to adenoviral infection, resulting in variable levels of expression of the hNET gene. Adenoviral infection is mediated by the coxsackie adenovirus receptor.31 The difference in infection susceptibility between cell lines is probably caused by differences in expression levels of the coxsackie adenovirus receptor. It has been shown that a deficiency of the primary receptor for adenoviruses on tumor cells limits the efficiency of adenovirus-mediated gene transfer;32 (3) different viral vectors have different transfection efficiency. The transfection efficiency is different between adenovirus and retrovirus-mediated gene transfer, even for the same transferred cells, the expression efficiency is also different.
In previous studies, it was found that selective inhibitors of noradrenaline, such as nisoxetine or imipramine, could specially inhibit the uptake of radioiodine-labeled MIBG in transfected cells.16, 17 In this study, we used maprotiline to validate hNET protein expression in transfected HepG2 cells. Maprotiline is an antidepressant compound with an atypical tetracyclic structure, which can strongly inhibit the re-uptake of noradrenaline in the brain and peripheral tissues, but not of serotonin.33 In the competition experiment, it was shown that hNET-mediated 125I-MIBG uptake was specifically inhibited by maprotiline in a dose-dependent manner. Compared with the inhibiting effect in the control of SK-N-SK cells, 125I-MIBG uptake in HepG2 cells was specially inhibited to the level as in wild-type cells, indicating that the hNET gene products were functionally active.
In the biological study, we found that the uptake of 125I-MIBG in tumor reached maximum at 2 h after injection, and kept 80% in hepatoma after 4 h, this is consistent with a previous report,16 which also revealed that the accumulation of 131I-MIBG was maximal at 2 h in retrovirus-mediated hNET gene transferred tumor after administration of the tracer, and maintained 89.74% in the tumor after 4 h. An ideal agent should localize in the target tissues with a tumor-to-nontumor ratio greater than 3.0;34 our in vivo study shows that the ratios of tumor/blood and tumor/muscle were observed to be 3.06 and 33.26 at 2 h, respectively, then the collection of 125I-MIBG began to decrease with time, whereas because of a more significant decrease in blood and other organs, the ratios of Ad-hNET-infected tumor/blood and tumor/muscle ascended obviously to about 48 and 56 at 24 h, respectively, indicating the favorable targeting of 125I-MIBG to the Ad-hNET-infected tumor; and the increasing tumor-to-nontumor ratios with time extension makes clear that blood had fast clearance for 125I-MIBG, which can be in favor of degrading toxins in the bone marrow and absorbed dose in other normal tissues for future clinical therapy.
Compared with previous studies in normal mice,24, 35 the relative values of 125I-MIBG in nude mice shows lower concentrations in various tissues and organs at 1 h, in which the blood, Ad-hNET tumor and stomach were mainly concentrated locations, this is in coincidence with the scintigraphic imaging in HepG2 nude mice. In contrast, in normal mice, significantly higher level of 125I-MIBG uptake was primarily seen in heart at 1 h, which may attribute to the fact that the heart is the primary uptake-1 target organ.35 In nude mice, however, the Ad-hNET-infected tumor concentrated high 125I-MIBG at 1 h, and owing to possible competitive uptake effects, the relative uptake values descend in other tissues and organs.36 At 24 h, the relative values of 125I-MIBG uptake in nude mice were similar to that in normal mice, including the heart and blood. Of course, the Ad-hNET tumor in nude mice shows a relatively higher level of 125I-MIBG uptake to other tissues and organs, including the blank adenovirus Ad.-infected tumor, which was also consistent with the imaging results.
Previously, hNET has been used as a reported gene for tumor-targeted imaging meditated by retrovirus or vaccinia virus, which demonstrated that hNET was suitable as a reporter gene for noninvasive monitoring of gene transfer.18, 37, 38 In this study, we investigated the scintigraphic imaging in hepatoma nude mice meditated by adenovirus encoding hNET gene transfection; the result revealed that the hepatoma can be clearly visualized in the images from 30 min to 24 h, which also proved that adenoviral vector-meditated hNET gene transfer can also be used for reported gene imaging, optimization of tumor treatment strategies and monitoring of gene expression.
This gene transfer/targeted radiotherapy strategy has potential for 131I-MIBG-mediated cell kill in tumors, yet there are some problems, which need to be solved in the future research. First is the comparatively low infection efficiency of adenovirus, infection of tumor cells in vivo will result in even lower radiation doses. We can choose some specifically high expressive promoter, such as telomerase, to elevate the expression level and infection efficiency of targeted gene.39 Second, there is comparatively large difference between the physical half-life of 131I-MIBG (8 days) and the biological half-life of 125I-MIBG (5.47 h) in hepatoma in vivo. Astatine-211 (211At) is a good choice to overcome this weakness. It has a suitable half-life of 7.2 h; emitting cytotoxic α-particle emitter with a mean energy of 6.8 MeV, and the potency of 211At-MABG is approximately three orders of magnitude greater than that of 131I-MIBG.40 As an analog of MIBG, 211At-MABG has been synthesized with high level using a convenient method,41 this will make 211At-MABG to become one of the most promising radionuclides for targeted tumor radiotherapy.
In conclusion, this study demonstrated that the feasibility of hNET gene transfer meditated by adenovirus vector could extend to the tumors other than those derived from the neural crest. Despite many challenges, such as the improvement of transfection efficiency of gene transfer and the suitable choice of radionuclide label for halobenzylguanidine, this study provides a sound foundation for further in vivo or in vitro investigation of HCC-targeted radiotherapy mediated by adenovirus transferred with the hNET gene.
References
Parkin DM, Bray F, Ferlay J, Pisani P . Global cancer statistics, 2002. CA Cancer J Clin 2005; 55: 74–108.
El-Serag HB, Rudolph KL . Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology 2007; 132: 2557–2576.
Sherman M . Recurrence of hepatocellular carcinoma. N Engl J Med 2008; 359: 2045–2047.
Llovet JM, Burroughs A, Bruix J . Hepatocellular carcinoma. Lancet 2003; 362: 1907–1917.
Omata M, Yoshida H, Shiratori Y . Prevention of hepatocellular carcinoma and its recurrence in chronic hepatitis C patients by interferon therapy. Clin Gastroenterol Hepatol 2005; 3: S141–S143.
Garaventa A, Bellagamba O, Lo Piccolo MS, Milanaccio C, Lanino E, Bertolazzi L et al. 131I-metaiodobenzylguanidine (131I-MIBG) therapy for residual neuroblastoma: a mono-institutional experience with 43 patients. Br J Cancer 1999; 81: 1378–1384.
Sisson JC . Radiopharmaceutical treatment of pheochromocytomas. Ann NY Acad Sci 2002; 970: 54–60.
Kang TI, Brophy P, Hickeson M, Heyman S, Evans AE, Charron M et al. Targeted radiotherapy with submyeloablative doses of 131I-MIBG is effective for disease palliation in highly refractory neuroblastoma. J Pediatr Hematol Oncol 2003; 25: 769–773.
Rose B, Matthay KK, Price D, Huberty J, Klencke B, Norton JA et al. High-dose 131I-metaiodobenzylguanidine therapy for 12 patients with malignant pheochromocytoma. Cancer 2003; 98: 239–248.
Fitzgerald PA, Goldsby RE, Huberty JP, Price DC, Hawkins RA, Veatch JJ et al. Malignant pheochromocytomas and paragangliomas: a phase II study of therapy with high-dose 131I-metaiodobenzylguanidine (131I-MIBG). Ann NY Acad Sci 2006; 1073: 465–490.
Pacholczyk T, Blakely RD, Amara SG . Expression cloning of a cocaine- and antidepressant-sensitive human noradrenaline transporter. Nature 1991; 350: 350–354.
Zahniser NR, Doolen S . Chronic and acute regulation of Na+/Cl−-dependent neurotransmitter transporters: drugs, substrates, presynaptic receptors, and signaling systems. Pharmacol Ther 2001; 92: 21–55.
Porzgen P, Bonisch H, Bruss M . Molecular cloning and organization of the coding region of the human norepinephrine transporter gene. Biochem Biophys Res Commun 1995; 215: 1145–1150.
Boyd M, Cunningham SH, Brown MM, Mairs RJ, Wheldon TE . Noradrenaline transporter gene transfer for radiation cell kill by 131I meta-iodobenzylguanidine. Gene Ther 1999; 6: 1147–1152.
Cunningham S, Boyd M, Brown MM, Carlin S, McCluskey A, Livingstone A et al. A gene therapy approach to enhance the targeted radiotherapy of neuroblastoma. Med Pediatr Oncol 2000; 35: 708–711.
Altmann A, Kissel M, Zitzmann S, Kubler W, Mahmut M, Peschke P et al. Increased MIBG uptake after transfer of the human norepinephrine transporter gene in rat hepatoma. J Nucl Med 2003; 44: 973–980.
Anton M, Wagner B, Haubner R, Bodenstein C, Essien BE, Bonisch H et al. Use of the norepinephrine transporter as a reporter gene for non-invasive imaging of genetically modified cells. J Gene Med 2004; 6: 119–126.
Moroz MA, Serganova I, Zanzonico P, Ageyeva L, Beresten T, Dyomina E et al. Imaging hNET reporter gene expression with 124I-MIBG. J Nucl Med 2007; 48: 827–836.
Mairs RJ, Boyd M . Targeting radiotherapy to cancer by gene transfer. J Biomed Biotechnol 2003; 2003: 102–109.
He TC, Zhou S, da Costa LT, Yu J, Kinzler KW, Vogelstein B . A simplified system for generating recombinant adenoviruses. Proc Natl Acad Sci USA 1998; 95: 2509–2514.
Antolovic D, Koch M, Bohlmann I, Kienle P, Buchler M, Weitz J . Short description of an alternative simplified method for screening recombinant clones within the ‘AdEasy-System’ by duplex-PCR. BMC Biotechnol 2005; 5: 1.
Barzon L, Stefani AL, Pacenti M, Palu G . Versatility of gene therapy vectors through viruses. Expert Opin Biol Ther 2005; 5: 639–662.
Jia ZY, Ou XH, Wei HY, Deng HF, Huang R, Wang JR et al. Construction and expression of replication-deficient recombinant adenovirus vector with hNET gene by adeasy-1 system. Sichuan Da Xue Xue Bao Yi Xue Ban 2008; 39: 523–526.
Vaidyanathan G, Zalutsky MR . No-carrier-added meta-[123I]iodobenzylguanidine: synthesis and preliminary evaluation. Nucl Med Biol 1995; 22: 61–64.
Apparsundaram S, Galli A, DeFelice LJ, Hartzell HC, Blakely RD . Acute regulation of norepinephrine transport: I. protein kinase C-linked muscarinic receptors influence transport capacity and transporter density in SK-N-SH cells. J Pharmacol Exp Ther 1998; 287: 733–743.
Pillai MR, Samuel G, Banerjee S, Mathew B, Sarma HD, Jurisson S . Technetium-99m complexes of polydentate amine-pyrrole and amine-thiophene ligands. Nucl Med Biol 1999; 26: 69–77.
Douglas JT . Adenoviral vectors for gene therapy. Mol Biotechnol 2007; 36: 71–80.
Ferreira TB, Alves PM, Aunins JG, Carrondo MJT . Use of adenoviral vectors as veterinary vaccines. Gene Ther 2005; 12: S73–S83.
Takahashi T, Takahashi K, Daniel TO . Methods in molecular medicine: high-efficiency and low-toxicity adenovirus-assisted endothelial transfection. In: Baker AH (ed). Vascular Disease: Molecular Biology and Gene Therapy Protocols, 1st edn, Humana Press: Totowa, 1999, pp 307–314.
Kiyono Y, Yamashita T, Doi H, Kuge Y, Katsura T, Inui KI et al. Is MIBG a substrate of P-glycoprotein? Eur J Nucl Med Mol Imaging 2007; 34: 448–452.
Bergelson JM, Cunningham JA, Droguett G, Kurt-Jones EA, Krithivas A, Hong JS et al. Isolation of a common receptor for Coxsackie B viruses and adenoviruses 2 and 5. Science 1997; 275: 1320–1323.
Kim M, Zinn KR, Barnett BG, Sumerel LA, Krasnykh V, Curiel DT et al. The therapeutic efficacy of adenoviral vectors for cancer gene therapy is limited by a low level of primary adenovirus receptors on tumour cells. Eur J Cancer 2002; 38: 1917–1926.
Maj J, Przegalinski E, Mogilnicka E . Hypotheses concerning the mechanism of action of antidepressant drugs. Rev Physiol Biochem Pharmacol 1984; 100: 1–74.
Strauss HW, Nunn A, Linder K . Nitroimidazoles for imaging hypoxic myocardium. J Nucl Cardiol 1995; 2: 437–445.
Vaidyanathan G, Welsh PC, Vitorello KC, Snyder S, Friedman HS, Zalutsky MR . A 4-methyl-substituted meta-iodobenzylguanidine analogue with prolonged retention in human neuroblastoma cells. Eur J Nucl Med Mol Imaging 2004; 31: 1362–1370.
Murashima S, Takeda K, Matsumura K, Yamakado K, Sakuma H, Kitano T et al. Increased lung uptake of iodine-123-MIBG in diabetics with sympathetic nervous dysfunction. J Nucl Med 1998; 39: 334–338.
Brader P, Kelly KJ, Chen N, Yu YA, Zhang Q, Zanzonico P et al. Imaging a genetically engineered oncolytic vaccinia virus (GLV-1h99) using a human norepinephrine transporter reporter gene. Clin Cancer Res 2009; 15: 3791–3801.
Chen N, Zhang Q, Yu YA, Stritzker J, Brader P, Schirbel A et al. A novel recombinant vaccinia virus expressing the human norepinephrine transporter retains oncolytic potential and facilitates deep-tissue imaging. Mol Med 2009; 15: 144–151.
Mairs RJ, Ross SC, McCluskey AG, Boyd M . A transfectant mosaic xenograft model for evaluation of targeted radiotherapy in combination with gene therapy in vivo. J Nucl Med 2007; 48: 1519–1526.
Boyd M, Mairs RJ, Keith WN, Ross SC, Welsh P, Akabani G et al. An efficient targeted radiotherapy/gene therapy strategy utilising human telomerase promoters and radioastatine and harnessing radiation-mediated bystander effects. J Gene Med 2004; 6: 937–947.
Zalutsky MR, Vaidyanathan G . Astatine-211-labeled radiotherapeutics: an emerging approach to targeted alpha-particle radiotherapy. Curr Pharm Des 2000; 6: 1433–1455.
Acknowledgements
We thank the anonymous reviewers for their helpful comments. We are grateful to Dr SG Amara (Yale University, USA) for supplying the full-length human NET cDNA. We thank Dr Paul C Knox (University of Liverpool, UK) for revision of the paper. This study was financially supported by the National Natural Science Foundation of China (Grant No. 30400113 and 30900378).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Jia, ZY., Deng, HF., Huang, R. et al. In vitro and in vivo studies of adenovirus-mediated human norepinephrine transporter gene transduction to hepatocellular carcinoma. Cancer Gene Ther 18, 196–205 (2011). https://doi.org/10.1038/cgt.2010.70
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cgt.2010.70