Abstract
OBJECTIVE: To develop a model for identifying women receiving cervical cerclage at risk for spontaneous preterm birth <32 weeks.
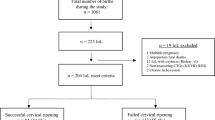
STUDY DESIGN: Retrospective cohort study of high-risk patients based on past obstetric history. Our inclusion criteria involved all patients with singleton gestation who received cerclage between 10 and 24 weeks. They were evaluated for the risk factors associated with preterm birth <32 weeks. Risk factors evaluated include: indication for cerclage, gestational age at cerclage placement, cervical length prior to cerclage, timing of cerclage (emergency or elective) and route of cerclage (abdominal or vaginal). Univariable and multivariable analyses were used to determine the risk factors associated with preterm birth. A risk-scoring model was developed for the prediction of preterm birth <32 weeks in women receiving cerclage.
RESULTS: We identified 256 women receiving cerclage that met our inclusion criteria. Preterm births <32 weeks occurred in 51 (20%). Multivariable analysis revealed a cervical length <25 mm, a history of cone biopsy and emergency cerclage to be significant risk factors associated with preterm birth <32 weeks. The sensitivity, specificity, positive and negative predictive values of the best model for predicting spontaneous preterm birth <32 weeks in women with cerclage are 80%; 96%; 82% and 95%, respectively.
CONCLUSION: The presence of a short cervical length, a history of cone biopsy and emergency cerclage were associated with preterm birth <32 weeks. Our model had a high sensitivity for identifying women who may benefit from a closer surveillance.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Dor J, Shalev J, Mashiach S, Blankstein J, Serr DM . Elective cervical suture of twin pregnancies diagnosed ultrasonically in the first trimester following induced ovulation. Gynecol Obstet Invest 1982;13:55–60.
Forster Von F, During R, Schwarzlos G . Treatment of cervical incompetence — cerclage or pessary? Zbl Gynacol 1986;108:230–237.
MRC/RCOG Working party on cervical cerclage. Final report of the Medical Research Council/Royal College of Obstetricians and Gynecologists Multicentre Randomized trial of cervical cerclage. Br J Obstet Gynaecol 1993;100:516–523.
Rush RW, Isaacs S, McPherson K, Jones L, Chalmers I, Grant A . A randomized controlled trial of cervical cerclage in women at high risk of spontaneous preterm delivery. Br J Obstet Gynaecol 1984;91:724–730.
Lazar P, Gueguen S, Dreyfus J, Renaud R, Pontonnière G, Papiernik E . Multicentred controlled trial of cervical cerclage in women at moderate risk of preterm delivery. Br J Obstet Gynaecol 1984;91:731–735.
Berghella V, Daly SF, Tolosa JE, et al. Prediction of preterm delivery with transvaginal ultrasonography of the cervix in patients with high-risk pregnancies: does cerclage prevent prematurity? Am J Obstet Gynecol 1999;18:809.
Heath VCF, Souka AP, Erasmus I, et al. Cervical length at 23 weeks of gestation: the value of Shirodkar suture of the short cervix. Ultrasound Obstet Gynecol 1998;12:318.
Hassan SS, Romero R, Maymon E, et al. Does cervical cerclage prevent preterm delivery in patients with a short cervix? Am J Obstet Gynecol 2001;184:1325–1331.
Rust OA, Atlas RO, Reed J, van Gaalen J, Balducci J . Revisiting the short cervix detected by transvaginal ultrasound in the second trimester: why cerclage therapy may not help. Am J Obstet Gynecol 2001;185:1098–1105.
Althuisius SM, Dekker GA, Pieter H, Bekedam DJ, van Geijin HP . Final results of the Cervical Incompetence Prevention Randomized Cerclage Trial (CIPRACT): therapeutic cerclage with bed rest versus bed rest alone. Am J Obstet Gynecol 2001;185:1106–1112.
Odibo AO, Elkousy M, Ural SH, Macones GA . Cervical cerclage compared with expectant management for the prevention of preterm birth: a systematic review. Obstet Gynecol Surv 2003;58:130–136.
Treadwell MC, Bronsteen RA, Bottoms SF . Prognostic factors and complication rates for cervical cerclage: a review of 482 cases. Am J Obstet Gynecol 1991;165:555–558.
Charles D, Edwards WR . Infectious complications of cervical cerclage. Am J Obstet Gynecol 1981;141:1065–1071.
Aarnoudse JG, Huisjes HJ . Complications of cerclage. Acta Obstet Gynecol Scand 1979;58:255–257.
Harger JH . Comparison of success and morbidity in cervical cerclage procedures. Obstet Gynecol 1980;56:544–548.
Cardwell MS . Cervical cerclage: a ten year review in a large hospital. South Med J 1988;81:15–19.
Harger JH . Cerclage and cervical insufficiency: an evidenced based analysis. Obstet Gynecol 2002;100:1313–1327.
Odibo AO, Talucci M, Berghella V . Prediction of preterm premature rupture of membranes by transvaginal ultrasound features and risk factors in a high-risk population. Ultrasound Obstet Gynecol 2002;20:245–251.
Iams JD, Goldenberg RL, Meis PJ, et al. for NICHD Maternal-Fetal Medicine Units Network. The length of the cervix and the risk of preterm delivery. N Engl J Med 1996;334:567–572.
Kokia E, Dor J, Blankenstein J, et al. A simple scoring system for the treatment of cervical incompetence diagnosed during the second trimester. Gynecol Obstet Invest 1991;31:12–16.
Laupacis A, Sekar N, Stiell I . Clinical prediction rules: a review and suggested modifications of methodological standards. JAMA 1997;277:488–494.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Odibo, A., Farrell, C., Macones, G. et al. Development of a Scoring System for Predicting the Risk of Preterm Birth in Women Receiving Cervical Cerclage. J Perinatol 23, 664–667 (2003). https://doi.org/10.1038/sj.jp.7211004
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211004