Abstract
Mental disorders affect many different groups around the world, and disadvantaged groups are often more severely affected. Neighbourhood green spaces (GS) can improve mental health, especially in disadvantaged groups. Many countries address social inequality and inequity through GS interventions. However, current evidence shows inconsistencies, which may result from the study site, research design, socio-demographically diverse samples, inclusivity considerations, and the different metrics used to quantify GS exposure and mental health benefits. Few conceptual models explain how neighbourhood greenery can act as a structural intervention. We used the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) method and retrieved 5559 documents from eight databases to examine whether neighbourhood GS can modify mental health associations in disadvantaged groups. We found that neighbourhood GS had substantial protective effects on the mental health of disadvantaged groups. However, disadvantaged people are more influenced by GS quality than by other GS exposures, such as GS usage, distance, and accessibility. Improvements in subjective well-being were most pronounced in terms of mental health outcomes. Mechanistically, neighbourhood GS improves mental health mainly through increased social cohesion and, green visibility, and young people receive further benefits from physical activity (PA). These findings offer a comprehensive understanding of the associations and mechanisms between neighbourhood GS and the mental health of disadvantaged groups, addressing health equities that are induced by the unfair distribution of GS, and thus promoting health-oriented environmental planning and policies.
Similar content being viewed by others
Introduction
Globally, approximately one in eight people suffer from mental disorders, which are the leading cause of years lived with disability (YLD), affecting one in every six YLD globally (World Health Organization 2022). Mental disorders affect people of all ages, cultures, and backgrounds, but the burden of health disorders is unevenly distributed within and among populations (Rogers 2004), especially among disadvantaged groups whose low socioeconomic status (SES) makes them more prone to mental illnesses due to poor living conditions, unemployment, and physio-psychological disparities. These situations increase the difficulty of obtaining high-quality mental health treatments (World Health Organization 2022). Although national authorities are attempting to reduce inequality, disadvantaged groups still face systemic and unavoidable health disparities relative to those with higher SES (Sugiyama et al. 2016). Green spaces (GS)are nature-based solutions for improving health and reducing health inequities (Wendelboe-Nelson et al. 2019), particularly for disadvantaged groups (Nawrath et al. 2021; Rigolon et al. 2021). Additionally, neighbourhood-focused activity engagement is considered a valuable strategy for achieving these goals (Rifkin et al. 2000; Team 2010; Wallerstein and Duran 2006); thus, the availability of neighbourhood GS is critical for promoting residents’ health. Moreover, studies show that neighbourhood GSs have a more pronounced effect on mental than on physical health (Liu et al. 2019; Sugiyama et al. 2008), especially for low-income and poor urban or suburban populations (Maas et al. 2009; Mitchell and Popham 2008; Mitchell et al. 2015). GSs may enhance residents’ mental health through several mechanistic pathways, including instoration (e.g., encouraging physical activity [PA] and promoting social cohesion), restoration, and mitigation (Lachowycz and Jones, 2013; Perrino et al. 2019; Wan et al. 2022). Therefore, previous studies have examined neighbourhood-based GS interventions as leverage to enhance health and reduce health disparities (Anzivino 2019; Astell-Burt et al. 2014; Canberra 2011; de Oliveira et al. 2013). Current evidence is inconsistent, however, potentially due to study site (Nawrath et al. 2021), research design (Wendelboe-Nelson et al. 2019), socio-demographically diverse samples (Rigolon et al. 2021), and various metrics used to quantify GS exposure and mental health benefits(Shuvo et al. 2020). The common practice of characterising vulnerable groups based on SES and race/ethnicity also may lack comprehensive inclusivity. Health disparities are systemic, as noted by Starfield (2001), and are intrinsically linked to systemic social disadvantage. Every group experiencing social disadvantage should have equal opportunities to achieve their optimal health status (Braveman et al. 2011). These factors make comprehensive assessments of the aspects of neighbourhood GS that affect the mental health of the broader vulnerable groups difficult. Thus, a systematic review is necessary to articulate predictable GS exposures, then examine the heterogeneity in the associations between GS and the mental health of broader disadvantaged groups across different study sites and sociodemographic contexts. This study is the first to explore the protective effects and impact pathways of neighbourhood GS on the mental health of disadvantaged groups using different metrics. Through a systematic review of quantitative research, this study discusses the following five questions:
-
1.
Is there a discrepancy between the results of subjective and objective indicators?
-
2.
Which types of green exposure metrics could predict the mental health of disadvantaged groups more efficiently and effectively?
-
3.
Which aspect of mental health is more likely to be improved in the disadvantaged groups via the lens of green exposure?
-
4.
Is the protective effect of greenery exposure consistent across vulnerable populations in different regions worldwide and in different specific environments?
-
5.
What underlying pathways link green exposure to disadvantaged groups’ mental health?
Methods
Search strategy
This systematic review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines(Moher et al. 2009). The literature search was conducted from 1 January 2012 to 26 February 2023 as studies prior to 2012 were concentrated specific developed countries and a small number of related topics. Eight frequently accessed databases—Web of Science, ProQuest, Medline, PsycINFO, CINAHL Plus, Cochrane Library, PubMed, and Embase— were used to search for relevant papers on disadvantaged neighbourhood GS. Table 1 presents the terms used to search the article titles, abstracts, and keywords. The definition of the target population includes terms that appear in relevant systematic reviews (Bonevski et al. 2014; Chenyang et al. 2022; Didsbury et al. 2016; O’Mara-Eves et al. 2015; Rigolon et al. 2021) while covering those who are economically, racially, physically, psychologically, or functionally disadvantaged or, disenfranchised people (Lambert 1990). Because some older adults and are not included in these categories, we did not add them to the search groups for this study. Relevant systematic reviews on green exposure and mental health were also referenced (Astell-Burt et al. 2022; Núñez et al. 2022; Xu et al. 2022). To meet our research objectives, we specifically focused on residential areas and surrounding greenery rather than urban GS in general. Supplementary File 1 includes detailed explanations of the search strategy and inclusion criteria.
Eligibility criteria
The specific criteria for the screening were as follows (Table 2):
Selection process and data extraction
Figure 1 illustrates the process of searching for and selecting articles for this systematic. All articles retrieved from each database were processed using EndNote reference management. Two reviewers independently assessed the titles and abstracts based on the selection criteria (Z.X., K.L.); next, each reviewer (Z.X., K.L., J.Z., YX.L.) examined articles which required full-text assessments. Any disagreements or differences were resolved through discussion and consultation with a third reviewer (T.N., B.Z., JH.Z., JG.Z.). We extracted information from each selected article, including the year of publication, author, region, country, study design, study sample and size, data related to disadvantaged populations, exposure measures and assessments, outcome measures, and measures of association. We could not conduct a meta-analysis of each study’s results due to heterogeneity in study designs, variable GS measurements, and mental health outcomes (Astell-Burt et al. 2022; Van den Berg et al. 2015).
Results
Study selection
Figure 1 shows the results of the systematic search based on PRISMA criteria. We retrieved 5559 documents from eight databases and removed 1550 duplicates. After checking titles and abstracts, full text was screened in 185 of the remaining 4009 documents. We excluded 144 studies, summarised in Supplementary File 2. A total of 41 studies met the inclusion criteria. (Supplementary File 3).
Study characteristics
The reviewed studies were concentrated in the European region (n = 17), with studies from the United Kingdom (UK) (Chalmin-Pui et al. 2021; Flouri et al. 2014; McEachan et al. 2016; McEachan et al. 2018; McElroy et al. 2021; Roberts et al. 2021; Roe et al. 2017; Roe et al. 2013; Sarkar et al. 2018; Thompson et al. 2016; Thompson et al. 2019; Thompson et al. 2012) (n = 12) dominating the group. The remaining studies were conducted in Spain (Subiza-Pérez et al. 2021; Triguero-Mas et al. 2015) (n = 2), Belgium (Mendoza et al. 2023) (n = 1), Norway (Mouratidis 2020) (n = 1), and Finland (Gonzales-Inca et al. 2022) (n = 1). In total, 10 studies were conducted in North American, mostly in the United States (Ambrose et al. 2020; Brown et al. 2018; Kodali et al. 2023; Kondo et al. 2022; Lee et al. 2023; Mennis et al. 2021; Murphy et al. 2022; South et al. 2018) (n = 8), and Canada (Cottagiri et al. 2022; Crouse et al. 2021) (n = 2). The Asian (n = 8) region was dominated by studies from China (Ma et al. 2022; Wang et al. 2022; Wu et al. 2021; Xiao et al. 2021; Yang et al. 2020; Zhang et al. 2020) (n = 6), with studies conducted in South Korea (Won and Lee 2020) (n = 1), Lebanon (Talhouk et al. 2021) (n = 1), Australia (Sugiyama et al. 2016) (n = 1), South Africa (Tomita et al. 2017) (n = 1), Morocco (Afrad and Kawazoe 2020) (n = 1), Peru (Korn et al. 2018) (n = 1), Colombia (Hong et al. 2021) (n = 1), and Brazil (Barreto et al. 2019) (n = 1). (Fig. 2)
In all studies, definitions of neighbourhood GS included internal greenery, private and public gardens, vertical, parks, jungles, and vacant GS. Sample sizes ranged from 25 to 3,549,514 individuals. Approximately 20% of the studies (n = 8) included fewer than 200 participants, and the smallest sample size was obtained from an exploratory study that measured salivary cortisol levels in the UK (n = 25) (Thompson et al. 2012). A Census-based longitudinal study conducted in Belgium had the largest sample size (n = 3,549,514) (Mendoza et al. 2023). Most studies focused on adults (n = 35). Some focused on pregnant women (McEachan et al. 2016; Subiza-Pérez et al. 2021), older adults (Brown et al. 2018; Cottagiri et al. 2022), children (Flouri et al. 2014; McEachan et al. 2018), and adolescents (Mennis et al. 2021). The 41 studies included, one quasi-experimental study (Talhouk et al. 2021) and one randomised trial (RT) (South et al. 2018). The other 39 studies were observational, and all but nine were longitudinal. Epidemiological studies have not examined mental health across geographical units. Most studies used the logistic regression model for analysis (n = 13), followed by (generalised) linear regression (n = 10) and structural equation modelling (SEM) (n = 3) which examined their potential underlying mechanisms.
Green exposure and mental health measures
To facilitate the understanding of green exposure metrics and their correlation with mental health outcomes across all studies, we established metrics for generalised categories of both green exposure and mental health outcomes, relying on the characteristics table (Supplementary File 3). Chord diagrams were generated to clearly convey the relationships among all green exposure metrics, mental health outcomes, and their respective categories, as identified within the studies.
GS measures
Objective evaluation metrics were used in 74% of the studies (n = 31) and 20% used both subjective and objective metrics (n = 8). The objective metrics mainly consisted of availability (incorporating land use/land cover and satellite-derived vegetative metrics [e.g., NDVI and Landsat Enhanced Vegetation Index [EVI]), street greenery visibility (calculated using deep learning method to analyse street view maps), and accessibility (proximity to recreational GS). The subjective indicators, mainly consisted of—— perceived quality, perceived greenery visibility, perceived quantity, perceived distance/accessibility, GS usage (i.e., frequency and duration), horticultural activities, and ownership of private gardens or other forms of small-scale green exposure (Fig. 3). Most studies interchangeably selected one to three green exposure indicators, whereas Thompson et al. (2016), Thompson et al. (2019), Roe et al. (2017), and McEachan et al. (2018) used more diversified green exposure metrics, including not only land cover maps, NDVI, and other remote sensing-based measurement methods, but also paid more attention to human exposure Factors such as GS perception, GS satisfaction, and frequency of use were used to capture actual feelings about the GS.
Mental health measures
To measure mental health, most studies used a single self-reported subjective assessment measure (n = 34); three studies measured only objective indicators (Brown et al. 2018; Lee et al. 2023; Mendoza et al. 2023), and five used both subjective and objective methods (Chalmin-Pui et al. 2021; Cottagiri et al. 2022; Roe et al. 2013; Thompson et al. 2012; Triguero-Mas et al. 2015). Research on the measurement of mental health has been divided into three main categories of well-being, specific mental disorders, and overall mental distress (Fig. 4).
Measurement of disadvantaged groups
The definition of disadvantaged groups in the reviewed studies overwhelmingly (93%) included SES as an important factor; 35 studies considered only SES, and four focused on SES and race (McEachan et al. 2016; McEachan et al. 2018; Mennis et al. 2021; Roberts et al. 2021). Spinal cord injuries (Murphy et al. 2022) and refugee status (Talhouk et al. 2021) have also been studied as key metrics for disadvantaged groups. Disadvantaged groups investigated also included veterans (Lehmann et al. 2018), refugees (Eggert et al. 2015), indigenous people (Hatala et al. 2020), and people with disabilities (Pihl 2015). However, the sample size in these studies was small, and they were conducted qualitatively.
Associations between multiple GS exposures and mental health outcomes
Of the 41 studies, the majority (70%, n = 29) concluded that neighbourhood GS had a protective effect on the mental health of vulnerable populations, 17% (n = 7) did not find this effect, and 12% (n = 5) found a negative effect. (Table 3) Furthermore, 138 associations between metrics were extracted from 41 studies. Most studies used GS exposure metrics that were consistent with the corresponding mental health outcomes as expected, but in seven studies (17%) some green exposure indicators used were inconsistent with expected outcomes despite positive mental health outcomes (e.g., in one study with a positive mental health result, there was no contribution or a negative contribution of some GS metrics to mental health). Among the studies with positive final mental health outcomes, some mental health metrics/outcomes used in 10% (n = 4) of the studies produced unexpected results (e.g. only stress improved, rather than subjective well-being).
Subjective GS metrics
Figure 5 shows the metrics used to assess perceived quality, which yielded positive effects in 78% (n = 7) of the studies. Xiao et al. (2021) and Roe et al. (2017) found that judgements of perceived quality were more influential in shaping perceptions of GS than the number or proximity of available GS. Interestingly, perceiving the presence of high-quality GS, even if they are not used, was shown to improve mental health (Roe et al. 2017), and a study by Kodali et al. (2023) demonstrated a direct association between GS perceptions and quality of life (QoL). However, Sugiyama et al. (2016) assessed neighbourhood park attractiveness using the Public Open Space Auditing Tool (POSDAT) and found that the mental state of residents with different SES was not related to park attractiveness.
Of the metrics used to assess the perceived greenery visibility, 67% (n = 2) had a positive effect. Roe et al. (2017) suggested that older individuals experience sensory contact with nature through larger gardens and/or views from home, leading to reduced stress levels. However, Thompson et al. (2016) found that having a view of GS from home was not significantly correlated with perceived stress in economically deprived communities. A Spanish study of pregnant women also found no significant correlation in low-income groups (Subiza-Pérez et al. 2021).
Regarding horticultural activities, all metrics used in the studies (n = 5) showed positive effects. Three studies focused on site preparation, vegetation planting, and installation of fencing (Korn et al. 2018; South et al. 2018; Talhouk et al. 2021). Two other studies focused on increasing the type and number of plants in existing gardens, their maintenance, and their daily use (Ambrose et al. 2020; Chalmin-Pui et al. 2021).
Of the metrics used to assess perceived quantity, 50% (n = 1) showed a positive effect. Yang et al. (2020) found that social cohesion and perceived environment can indirectly improve mental health. However, there is no direct relationship between perceived quantity, perceived walking distance (Roe et al. 2017), accessibility (Kondo et al. 2022; Subiza-Pérez et al. 2021) and mental health status. Subiza-Pérez et al. (2021) found that the association between perceived greenness (the amount of perceived greenness and walking distance to the GS) and social cohesion was consistent across income groups.
Among the metrics used to assess GS usage, only one study (14%) demonstrated a positive effect. GS interventions, such as providing a place for social activities, did not reduce mental burden, and sometimes and even exacerbated perceived stress. The timing and frequency of visits to nature did not explain the association between the intervention and increased perceived stress (Thompson et al. 2019) or ease the relationship between park use and QoL (Kodali et al. 2023). Children’s time spent outdoors also has no effect on externalising and internalising behavioural difficulties or prosocial behaviours (McEachan et al. 2018). However, McElroy et al. (2021) found that the use of neighbourhood GS by disadvantaged groups as social venues could enhance feelings of intimacy and improve mental well-being.
Two studies on the ownership of GS with regard to private gardens, allotments, or small greenery have shown that the protective effect of neighbourhood GS is influenced more by the district and type of GS in which the disadvantaged group is located 50% (n = 1) showed a positive effect. A study conducted in the UK (Thompson et al. 2016) showed that people who owned gardens or allotments experienced less stress, whereas a study of PSG in deprived areas of Morocco, found that garden owners had higher average depression scores than non-owners (Afrad and Kawazoe 2020).
Objective GS metrics
As shown in Fig. 5, of the metrics used to assess availability, 63% (n = 17) demonstrated positive effects. Neighbourhood GS exposure to significantly reduced the risk of depression or major depression in disadvantaged groups (Brown et al. 2018; Sarkar et al. 2018). However, this protective effect on mental health was not significant among high-income groups (Barreto et al. 2019; Zhang et al. 2020). Residential GS also alleviated the stress of residents in disadvantaged neighbourhoods (Thompson et al. 2016; Thompson et al. 2012), with higher levels of neighbourhood GS (>43% of the area) associated with lower perceived stress and a sharp decrease in cortisol secretion (Roe et al. 2013). In addition to mental health disorders, such as depression and stress, the health benefits of neighbourhood GS are reflected in prescription rates (Roberts et al. 2021) and suicide rates (Lee et al. 2023; Mendoza et al. 2023). McEachan et al. (2018) also found that GS availability alleviated mental health problems among non-white children in the UK. However, the NDVI effect was not significant in any buffer zone when GS satisfaction and time spent outdoors were included. The protective effect of GS availability may be diminished by simultaneous assessment of multiple subjective or objective indicators. Wang et al. (2022) found that GS quality moderated the relationship between SES indicators and mental health after simultaneously assessing NDVI, street-view greenness (SVG) quantity, and SVG quality, whereas NDVI had no moderating effect.
Regarding visibility metrics, 60% (n = 3) showed positive effects. For low-income populations, SVG were negatively associated with the probability of lower life satisfaction (OR = 0.597, 95% CI = 0.298–0.965) (Wu et al. 2021). Wang et al. (2022) assessed both SVG quality and quantity, and found that SVG quality was more important in disadvantaged groups. Mennis et al. (2021) assessed SVG and found that GS may play an important role in moderating the peer impact of substance use among disadvantaged urban youth. However, objective GS indicators, such as the streetscape Vegetation Index [VGI], NDVI, and park area, did not have a significant impact on the mental health of disadvantaged groups in high-density disadvantaged communities (Xiao et al. 2021). Regarding accessibility metrics, 60% (n = 3) showed positive effects. Ma et al. (2022) and Xiao et al. (2021) found that park distance and accessibility are significantly associated with mental health effects among those with lower incomes. However, the samples in McEachan et al. (2016) and McEachan et al. (2018) all lived near a GS, but no association was found between the distance to a GS and mental health.
Associations between different measures of mental health and mental health outcomes
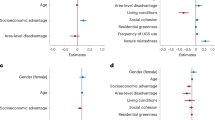
As shown in Fig. 6 of the metrics used to assess well-being, 72% (n = 13) showed positive effects. Nine metrics directly assessed emotional well-being (EWB), and only two did not show a positive effect of GS on the subjective well-being from disadvantaged groups. Studies assessing life satisfaction (n = 4) are more likely to indicate improvements in subjective well-being among vulnerable individuals (Wu et al. 2021) as well as reduced depression (Afrad and Kawazoe 2020; Cottagiri et al. 2022). Mouratidis (2020) found no significant association between anxiety symptoms and quality of life for residents in deprived communities, even when infrastructure, such as GS and public transport were relatively evenly distributed.
In contrast, the improvement effect of neighbourhood GS on overall mental distress and specific mental disorders was relatively low, at 61% (n = 11) and 63% (n = 20), respectively. Individuals across different age groups, including children (Flouri et al. 2014), adolescents (Mennis et al. 2021), and middle-aged and older adults (Cottagiri et al. 2022), all benefit from neighbourhood GS. Furthermore, compared to depression and anxiety (n = 8, 57%), alleviation of stress (n = 7, 70%) was significantly more prominent, regardless of whether stress was self-reported (access to gardens and allotments, neighbourhood GS, horticulture, and park perception) (Kodali et al. 2023; Korn et al. 2018; Thompson et al. 2016) or based on biological markers (saliva cortisol) (Chalmin-Pui et al. 2021; Roe et al. 2013; Thompson et al. 2012).
Types of disadvantaged people and differences in mental health outcomes
Of the 30 studies conducted in developed countries, 73% (n = 22) reported positive results. However, protective effects were not observed in three of the four studies conducted in developed countries with high welfare. In a cohort study conducted in Finland (Gonzales-Inca et al. 2022), only moderate neighbourhood-level mental health was found to be associated with green exposure. Two studies conducted in Canada (Crouse et al. 2021) and Norway (Mouratidis, 2020) found no such correlations.
Regional differences were more pronounced in developing countries than in developed ones; the studies conducted in China (n = 5) all observed better protection effects, while half of the remaining six studies reported no or negative effects of GS on disadvantaged groups. The beneficial effects of neighbourhood greenery appear to be much stronger for people living in middle- and high-SES communities in South Africa (Tomita et al. 2017), and Colombia (Hong et al. 2021) than for low-income groups.
GS often has negative impacts when a sample includes individuals with disabilities or long-term illnesses. For people with spinal cord injuries, neighbourhoods with more GS reported higher levels of depression (Murphy et al. 2022). In addition, GS has the potential to provide a venue for trading and substance use for individuals with active substance use disorders (Mennis et al. 2021).
In studies involving both SES and race (n = 6), racial factors showed the same results as SES ones. Only one study found that neighbourhood GS failed to improve the mental health of ethnic minority residents (Mendoza et al. 2023). Among studies involving informal settlements (n = 5), three reflected positive effects. In Xiao et al. (2021), mental health status was only positively associated with subjective GS satisfaction, not with objective metrics. In Korean public housing communities, GS did not increase social capital or improve mental health (Won and Lee, 2020). In densely populated settlements with high poverty rates in Morocco, a small amount of GS contributes to higher levels of depression among owners (Chalmin-Pui et al. 2021).
Potential pathways and mechanisms by which a neighbourhood GS affects the mental health of disadvantaged people
Numerous studies have explored the pathways by which GS affects health, with well recognised pathways including noise reduction, air pollution reduction, psychological recovery and stress reduction, encouraging health-promoting behaviours (e.g. social interaction, PA) (Dzhambov et al. 2018; Hartig et al. 2014; White et al. 2013). Some indirect effects are seen, such as social cohesion, although corresponding mediating effects were found in studies by Dadvand et al. (2016), De Vries et al. (2013), and Maas et al. (2009), others failed to identify them. Some studies found that stress reduction (Triguero-Mas et al. 2017) and mitigation of traffic emissions (Gascon et al. 2018) were more important than PA and social cohesion. This may occur because the heterogeneity of the individual and group characteristics of the target population was not considered (Chen et al. 2021),and cross-sectional studies do not adequately consider various pathways. Therefore, a comprehensive summary for disadvantaged groups is required.
Yang et al. (2020) demonstrated that social cohesion is an important mediator between perceived GS and mental health in disadvantaged groups, with pathways involving environmental disturbances and social cohesion. This was further confirmed by Subiza-Pérez et al. (2021), who found that social cohesion positively influenced mental health in low- (−0.20) and middle-income (−0.28) groups. Thompson et al. (2016) discovered that a sense of place belonging, social isolation, and social well-being were mediators of neighbourhood GS and perceived stress. Wang et al. (2022) confirmed the quality of GS moderated the relationship between SES and mental health. In addition, for some vulnerable people, the perception of the presence of high-quality GS in the neighbourhood can improve their psychological condition (Roe et al. 2017). Similarly, McEachan et al. (2018) found that satisfaction with GS independently predicted mental health in South Asian children. Neither Mendoza et al. (2023) nor Yang et al. (2020) found evidence that residential outdoor air pollution was a potential mediator in the association between neighbourhood GS, mental health, and suicide mortality. GS does not appear to contribute to enhanced PA for relieving stress (Thompson et al. 2016). Among residents of deprived neighbourhoods, PA was found to be significantly associated with stress through measures of cortisol slope, but not with self-reported stress (PSS), suggesting that GS may be associated with subjective perceived stress through mechanisms other than PA (Thompson et al. 2012). During pregnancy, PA is only a partial mediator of the small indirect effects of GS on depressive symptoms (McEachan et al. 2016). Hong et al. (2021) and Barreto et al. (2019) also showed that PA does not mediate mental distress. Roe et al. (2017) confirmed that young people were more likely to improve their social well-being through PA and corresponding social events, whereas middle-aged and older adults were less likely to do so. Older adults are more likely to improve their mental condition by watching GS (Roe et al. 2017).
Synthesis of qualitative studies
While qualitative studies were excluded from our review, it is undeniable that some qualitative studies provide valuable insights, especially because they include a more diverse range of vulnerable groups that are often not captured in quantitative studies. Emphasising productive landscapes, such as community gardens and green roofs as green infrastructure can offer significant physiological and psychological health benefits to vulnerable populations by addressing inequalities. (Anderson et al. 2021; Beavers et al. 2022; Budowle and Porter 2022). This is evident in broader vulnerable groups, such as refugees (Eggert et al. 2015), dementia patients (Hassink et al. 2018), and veterans (Lehmann et al. 2018). Furthermore, GS has been shown to significantly improve the mental state of unhoused individuals (Plane and Klodawsky 2013) and assist indigenous communities (Hatala et al. 2020) in strengthening their connection with the land and nature.
Discussion
Our research indicates that neighbourhood GS has a beneficial effect on individual mental health, a finding that is particularly pronounced among vulnerable populations and in middle- to low- income countries. This aligns with previous systematic reviews (Nawrath et al. 2021; Rigolon et al. 2021). As the understanding of how various components of GS impact the mental health of underprivileged communities remains limited, it is unclear how mental health improvements would be expressed. Furthermore, owing to the varying levels of SES, ethnicity, and mobility among marginalised populations, the corresponding intermediary mechanisms that may account for heterogeneity among these underprivileged groups must be determined. Therefore, appropriate exposure assessments for disadvantaged groups are required to accurately guide relevant research. This study proposes a conceptual framework for classifying greenspace exposure in terms of subjective and objective metrics, considers heterogeneously disadvantaged group types and the characteristics of underprivileged neighbourhoods, explores differences by assessing which aspects of GS exposure are more significant in terms of mental health improvement for disadvantaged groups, assesses the benefits of GS exposure for disadvantaged groups, and reveals a more plausible, potential mediating effect of neighbourhood GS on the mental health of disadvantaged groups (Fig. 7).
This framework diagram categorizes green space exposure in terms of subjective and objective indicators, assesses which aspects of green space exposure are more significant in terms of mental health improvement for disadvantaged groups and why the associated psychological benefits are manifested, and reveals the potential mediating effects of neighbourhood green space that are more credible in terms of disadvantaged groups’ mental health.
Discrepancies in the results of subjective and objective indicators
Unlike subjective measurements, objective measurements more reliably forecast the positive effects of GS exposure on the psychological well-being of underprivileged groups. Among the objective indicators, visibility may be an effective predictor of mental health benefits derived from GS exposure. Accessibility and availability potentially predicted stronger mental health protection benefits of neighbourhood GS for disadvantaged people. When the heterogeneity of GS subjective metrics emerged, some tended to be more pronounced than objective metrics in identifying the protective effect of neighbourhood GS on the mental health of disadvantaged people.
Regarding subjective metrics, perceived quality and horticultural activities may better predict the mental health benefits of GS exposure among disadvantaged people, which is consistent with the results of a systematic review (Nguyen et al. 2021). Ownership, perceived greenery visibility, and perceived quantity also potentially predict the mental health benefits of GS exposure on disadvantaged people but are more influenced by the type of disadvantaged people, the type of GS, and the quality of GS. By contrast, GS usage and perceived distance/accessibility were less likely to predict the protective effects of greenspace exposure.
The uniformity of objective indicators highlights standardised measurements and the environment’s physical features, which are relatively stable across different individuals, often showing consistent and, moderate effectiveness in predicting mental health. However, subjective indicators are affected by factors beyond objective environmental conditions. The Mindsponge Theory states that a person’s cultural background and personal experiences influence how they perceive and interpret their environment and process information according to their psychological models (Vuong 2022). Relationships within an individual’s subjective experience are mental constructs, and may not correspond with those in the objective world (Nguyen et al. 2023).
Therefore, even with set objective environmental factors such as the amount, accessibility, and quality of greenery, people’s individual perceptions and judgements can vary and be influenced by their own ways of seeing and internalising their environments. This can lead to variations in mental health outcomes (Howley 2011; Riemer et al. 2014; Zheng et al. 2023). Individuals’ perceptions are shaped by past experiences, cultural values, and personal preferences. For example, someone who grew up without greenery in their surrounding environment might rate the green spaces in their current surroundings higher, even the greenery is not abundant or high quality. In subjective assessments, some indicators may be more tightly linked to an individual’s specific mental needs and ways of adapting, making them more effective in predicting mental health (Campbell 1976).
Hence, subjective perception is key to assessing mental health, and may even outperform the predictive ability of objective measures. Subjective indicators show considerable variation owing to personal differences, psychological models, and cultural backgrounds. These variances emphasise the importance of considering both the objective traits of the environment and individual subjective views when examining how the environment affects mental health. This is particularly crucial when focusing on vulnerable groups, whose perception of their environment could be shaped by more complex social and economic factors.
Effectiveness and efficiency differences in the composition of GS exposure indicators
Subjective GS metrics
The subjective judgement of the GS is often affected by the heterogeneity of the subjects’ individual differences, evaluation criteria, and questionnaire design. At the same time, due to the inequality of disadvantaged groups in terms of SES, ethnicity, and mobility, the level of planning and construction of GS in their neighbourhoods and their perceptions of facing neighbourhood GS are significantly different from those of non-disadvantaged groups. Therefore, we observed great heterogeneity of different subjective GS indicators in indicating the mental health of disadvantaged groups.
High-quality GS can provide additional resources and motivation for disadvantaged groups to engage in outdoor activities to improve their health and expand their social networks (De Vries et al. 2013; Jim and Shan 2013; Lu et al. 2019; Qin et al. 2021). They are often limited to GS designated for walking, yoga, or socialising, whereas high-SES groups have more options and tend not to use their neighbourhood GS as a first choice (Ma et al. 2022). High-quality GS provides residents with an attractive environment for mutual interaction and enhances their social cohesion. Conversely, low-quality GS may discourage usage due to concerns about safety, antisocial behaviour, cleanliness, and maintenance (Abbasi et al. 2016; Gidlow and Ellis 2011). This may explain why Sugiyama et al. (2016) did not observe a protective effect of GS quality on the mental health of disadvantaged residents, as the tool used to assess GS attractiveness lacked metrics to assess safety and maintenance. In addition, as disadvantages are mainly considered through economic circumstances such as income, job, vehicle, and home ownership, most studies on disadvantaged groups only consider adult samples in their empirical design, while adolescents who are less critical of GS quality are not included in the study; this could lead to results that are more biased towards the quality of GS (Roe et al. 2017). Astell-Burt, Mitchell et al. (2014) also noted that younger adults benefited more from GS quantity than middle-aged adults. The protective effect of GS quantity on disadvantaged groups may be moderated by GS quality, implying that the association between GS quantity and health outcomes is stronger when quality is higher (Lachowycz and Jones 2013).
Based on the results of qualitative and quantitative studies, we found that horticultural activities in neighbourhood GS, such as community gardens and farms, had a significant positive impact on the mental health of different vulnerable groups. Horticultural activities can enhance the sense of social belonging among people in disadvantaged neighbourhoods. By creating and sharing communal spaces, people are more likely to be open and receptive to their surroundings (Cohen et al. 2008). The presence of grass and trees further increases their informal interactions, deepening their understanding of each other and creating weak ties which allow them to help each other in their daily lives (Kuo et al. 1998). Horticultural activities stimulate creativity and self-expression, enhance self-worth, becoming a source of pride (Clayton 2007), and improve the sense of place (Laali et al. 2018). Gardening can be a significant distraction that alleviates mental disorders such as depression (Nolen-Hoeksema et al. 2008). Horticultural activities give individuals a reason to leave their house, providing them with a temporary break from the pain and stress of everyday life as well as tranquillity in the satisfaction gained by making their environment more attractive (Certomà 2015).
A number of systematic reviews investigating GS and mental health (Callaghan et al. 2021; Chen et al. 2021; Jabbar et al. 2021; Labib et al. 2020) have shown that viewing and using GS has a positive effect on mental recovery. However, there may be population heterogeneity in this mental health benefit, particularly for residents of disadvantaged neighbourhoods where the effects of GS visibility and use on mental health are more pronounced. For older adults with limited mobility, appreciating the natural landscape outside their windows can improve their mental state, even if they are often sedentary (Roe et al. 2017). However, for middle-aged people, the protective effect of green visibility is influenced more by the quality of the GS than its amount because lower levels of urbanisation may result in fewer man-made features that support PA or social interaction (Gascon et al. 2019; Marquet et al. 2020). Simply seeing more GS rather than being attracted to quality GS and thus socialising in it does not strengthen neighbourhood ties and interactions or enhance a sense of belonging and social well-being, which in turn reduces stress and improves mental states through social well-being (Thompson et al. 2016). Additionally, middle-aged people have higher expectations of the quality of their local environment (Roe et al. 2017), whereas those in lower-income neighbourhoods often lack adequate GS and GS quality (Space 2010). Issues such as untrimmed trees, presence of litter, and broken public facilities may affect satisfaction with GS use. The impact of neighbourhood GS use on stress should be observed over time; therefore, the results were less evident in the study by Kodali et al. (2023). One of the two studies that assessed GS ownership in the UK found a stronger protective effect of neighbourhood GS on the mental health of disadvantaged people. This was possibly influenced by the type of GS involved, which in the UK existed as part of the dwelling in the form of private gardens or allotments and formed a clearer boundary through fencing. The Moroccan study had PSG as its subject, which usually clings to the façade of the dwelling or to a buffer zone placed at the articulation of the road, leading to a higher risk of theft and vandalism among owners.
For perceived distance/accessibility, such subjective indicators do not capture the true attitudes of disadvantaged groups toward neighbourhood GS because most disadvantaged adults commute long distances and work long hours to support their families, and older people and those with limited mobility may lack appropriate financial and social support. Even if they are aware of the presence of GS in the neighbourhood, it may be difficult for them to access it, and they may not be sufficiently exposed to the green environment of their communities (Yang et al. 2020). Simultaneously, unreasonable planning in disadvantaged neighbourhoods may lead to a longer actual walking distance, which is difficult to measure using satellite- or land-use-derived GS objective indicators. Thus, we observed large differences in the prediction of mental health outcomes between objective accessibility metrics and subjectively perceived distance and accessibility metrics.
Objective GS metrics
Epidemiological studies often use remote sensing measurements to assess the greenness and accessibility of green environments. Examples include the NDVI and land cover. Several review articles have confirmed that these methods are valid and practical for assessing the health impacts of neighbourhood GS (Ekkel and de Vries 2017; Gascon et al. 2015; Holland et al. 2021; Vilcins et al. 2022). However, most studies in this systematic review used data at a 30 m resolution, making it difficult to capture greenery in small-scale cities. Therefore, the accuracy of neighbourhood GS greenness capture is much lower than that of SVG, which comes from a human-perspective. Additionally, owing to the large heterogeneity in buffer size, measurement season, and differences in cloudiness at the time of capture (Geneshka et al. 2021), green exposure measurements can vary significantly. Furthermore, this method can only assess the overall level of vegetation and cannot distinguish between structured and unstructured vegetation, accordingly, it cannot assess GS quality (Markevych et al. 2017). As mentioned earlier, for disadvantaged groups, the quality of a GS is more important than its quantity. Therefore, aspects that reflect the quality of GS exposure such as time, duration, frequency, and intensity (Shanahan et al. 2016) are difficult to capture. Street-view map-based methods combined with deep learning can be used to observe the actual perceived green exposure of residents, which is often overlooked by remotely sensed data (Wang et al. 2019). It is important to note that remote sensing-based greenery may be more relevant to general health than SVG because remote sensing data capture overall vegetation amounts, whereas streetscape greenery may be more relevant to perceptions and behavioural pathways based on actual interactions (Dzhambov et al. 2020; Liu et al. 2020). Thus, street-level human-view angle greenness can be assessed through streetscape greenness to identify associations among GS exposure, reduced risk of mental disorders, and increased sense of place attachment.
The effect of GS exposure on different mental conditions in vulnerable groups
GS is protective in terms of well-being, overall mental distress, and specific mental disorders among disadvantaged individuals. However, mental health improvements in neighbourhood GS for disadvantaged people may be greater in the terms of well-being. Notably, de Keijzer et al. (2020) found an insufficient association between GS and well-being in a systematic review of non-disadvantaged groups; however, we found that the association was significant among disadvantaged groups.
This may be due to the relatively poor quality and quantity of greenery in disadvantaged neighbourhoods, which can lead to a sense of isolation and lack of social support among neighbourhood residents (Maas et al. 2009), for whom assessed indicators of well-being—such as feeling loved or having increased self-confidence,—have a more significant and sustained positive impact. Furthermore, in the context of persistent poverty, multiple social, economic, and poverty-related health problems may be the main drivers of depression, stress, and anxiety, and the impact of these factors may outweigh the potential risk to the surrounding natural environment (Tomita et al. 2017).
It is also important to note that the different instruments and indicators used to assess well-being and mental health may produce different results (Cheng et al. 2021). Studies that used the EWB scale to assess life satisfaction tended to better predict well-being among disadvantaged groups, whereas those that assessed QoL were less predictive. This may be because, when evaluating quality of life and life satisfaction, community residents consider more non-greenery-related differences in neighbourhood quality, such as neighbourhood infrastructure (e.g., ball fields, convenience stores, and bike racks) and environmental health (e.g., air quality, noise, and sewage) (Mouratidis 2020).
Geographic and individual variations in the general protective effect of GS on different vulnerable groups
Our research confirmed that the protective benefits of green exposure were unevenly distributed across the different types and regions of disadvantaged people. At the individual level, vulnerable groups in low and middle-income countries, face high poverty and significant wealth gaps. Although there is a positive correlation between GS and health, having more GS does not necessarily imply better health benefits if socioeconomic health disparities are not addressed. Improving socioeconomic conditions and meeting basic needs can help people escape poverty; after that other non-essential factors, such as the greenness of the living environment may be potential drivers of better mental health (Tomita et al. 2017). In high-income, high-welfare countries, such as the Nordic region, despite the wide distribution of GSs as a social infrastructure, the quality of GS needs further improvement, and the protective benefits of GS might not be sufficient to satisfy mental health needs. An individual’s economic and social including their income, employment status, and education level, can also affect different aspects of their well-being and mental health (Manley et al. 2011), and anxiety, stress and depression symptoms may be more influenced by these factors than by the natural environment.
For neighbourhoods with a high number of people with disabilities, the lack of accessible facilities may result in people with disabilities using GSs less often than able-bodied people, thus hindering their participation in community activities. In such cases, the presence of a neighbourhood GS may exacerbate individuals’ pessimistic perceptions of their disability and negatively impact their mental health. For these people, features or services which meet their basic daily needs, such as accessibility and safety maintenance, may be more important.
On a neighbourhood-level, disadvantaged neighbourhoods formed under the background of rapid urbanisation, with high building density and low neighbourhood greenery, and the biopsychosocial pathways linking neighbourhood GS exposure to mental health, are not active in the same way because of the specific nature of the living space (Liu et al. 2019). In a study conducted in urban villages in Shanghai, China, mental health improved indirectly through residents’ perceptions of private gardens formed by house voids and small open spaces, whereas the risk of vandalism or theft in high-density disadvantaged communities with poor social security and private GS may lead to poorer psychological states. Therefore, for cities where it is difficult to completely demolish and rebuild disadvantaged neighbourhoods, on the premise of improving neighbourhood security, encouraging and supporting the construction of private gardens can allow disadvantaged groups to obtain the health benefits of GS.
Underlying pathways link green exposure to disadvantaged groups’ mental health
We summarised four categories of potential mediators of neighbourhood GS: environmental interference, nature perception, social cohesion, and outdoor activities. Environmental interference (air pollution) may affect mental health by disrupting residents’ perceptions of the quality of green restorations (Von Lindern et al. 2016), and the resulting undesirable odours can affect psychological states through annoyance rather than through pathophysiology (Claeson et al. 2013). Of the reviewed articles considering environmental interferences, such as air pollution, none observed mediating effects; this may be, because measurement, specific attention to immigration, and other mediating adjustments reduced the importance of environmental interferences on mental health (Yang et al. 2020). In addition, the mediating effect of environmental disturbance is based more on aesthetic factors and is reflected in the SVG-tree or SVG-grass at the eye level rather than the NDVI (Wang et al. 2020); therefore, no mediating effect could be observed (Mendoza et al. 2023).
Either viewing or being exposed to nature helps disadvantaged groups relieve stress (Kaplan 1995). The perception that high-quality neighbourhood GS enhances individuals’ satisfaction with the living environment further enhances their motivation to enter GS and engage in activities that encourage health, contributing to social cohesion and corresponding social perceptions, which reduces social isolation, enhances sense of local belonging and social well-being, and improves their mental health. The function of the social-based activities provided by the community is becoming increasingly important, especially as domestic activities (shopping and laundry) are replaced and diverted. Social cohesion often stems from bottom-up social interactions at the local level, which influence health by promoting health-related behaviours within the neighbourhood and, increasing access to services and amenities, or through psychosocial processes (Forrest and Kearns 2001). Neighbourhood greenery and community parks support neighbourhood contact and the maintenance of community ties (Thompson et al. 2016), strengthen the level of connection and solidarity between people in the community, and translate these connections into tangible goals of common interest (Echeverría et al. 2008), thus contributing to social cohesion. Close family ties, mutual aid, and voluntarism are strong characteristics of disadvantaged areas. These qualities make disadvantaged people more willing to participate in maintaining ties and social relationships within a community. Simultaneously, disadvantaged neighbourhoods often imply high levels of unemployment, high levels of single-parent households, or individuals who are older or have disabilities, who can spend more time at home and in community settings (Forrest and Kearns 2001; Henning and Lieberg 1996). Thus, the mediating benefits of social cohesion may be more pronounced in disadvantaged groups.
Furthermore, the potential pathways for green exposure to weakly connected low-SES groups to mental health showed some variation caused by age heterogeneity. PA showed a more pronounced mediating effect in young people, whereas the mediating effect of GS quality was more pronounced in middle- and older-aged adult. Younger people were more likely to be physically active and derive mental health benefits from GS than middle-aged and elderly individuals. A systematic review by Vanaken and Danckaerts (2018) suggested that this may be achieved through PA and the resulting social interactions. For disadvantaged older adult, reduced physical function combined with poor financial circumstances and often poorly treated physical conditions (World Health Organization 2022) make them less able to engage in PA in a GS, and are therefore more likely to engage with GS from home or by entering them for social activities (Roe et al. 2017). Middle-aged disadvantaged people often face significant financial and survival pressures and require more time for work or family commitments, making it clear that sports—which take up more time—are less likely to be their first choice for GS activities. Thus, a high-quality GS will significantly increase their satisfaction with the community and support them in socialising within the GS.
Strengths, implications, and limitations
The main strength of this systematic review was the selection of articles which synthesised keywords from previous systematic evaluations and incorporated a more comprehensive and extensive examination of the definitions of disadvantaged groups. Furthermore, we synthesised qualitative research to provide insights into a broader understanding of disadvantaged groups. Consequently, this review discusses disadvantaged groups other than low-SES groups, which provides a deeper understanding of disadvantaged groups. In addition, we focused more on the results of neighbourhood GS exposure and mental health sub-indicators rather than the positive or negative effects which the study ultimately pointed to, thus providing a more precise assessment of the specific aspects of disadvantaged groups affected by GS exposure.
Neighbourhood GS can help alleviate inequalities in disadvantaged neighbourhoods with disadvantaged groups being more affected by GS quality (perception, satisfaction, etc.) and less affected by distance, access, accessibility, and quantity. Specifically, only disadvantaged adolescents improved their mental health through PA. When new or renovated GSs are built, priority should be given to improving their quality, operation, and maintenance, rather than building a large number of low-quality GS, considering the age composition of the neighbourhood and providing social or sporting facilities accordingly. Additionally, for all vulnerable groups, using productive landscapes and associated gardening activities, such as community farms, is a great way to make GSs more equitable and boost health. We suggest that communities integrate these aspects as key components of their GS infrastructure. Besides, in areas with extremely high or low economic levels, the impact of GS exposure may be limited or even negative. Therefore, in developing countries, efforts should first be made to reduce socioeconomic disparities between classes and avoid gentrification in economically underdeveloped areas. In developed countries, services related to GS in deprived neighbourhoods should be strengthened, and emphasis should be placed on enhancing the overall neighbourhood environment.
This review had several methodological limitations. First, the review of research methods did not include articles published in languages other than English or qualitative studies involving disadvantaged groups, and the quantitative research we looked at mainly used data from general population surveys or health follow-ups, and GS exposure was assessed based on where people lived. This means that disadvantaged groups who could not give home addresses, such as those the unhoused or runaways, were often left out of these studies, which may then have missed specific disadvantaged groups. Also, while we touched on qualitative research involving a wider range of vulnerable groups, the nature of qualitative research mean that its findings are less robust.
Second, for the evidence reviewed, the design of most included studies was cross-sectional and did not support strong causal inferences. Also, our study may have potential publication bias due to the search period and corresponding exclusion criteria. Third, in terms of empirical design, some studies have overlapping and nested definitions of subjective metrics (e.g., assessing satisfaction through accessibility) and a small number of certain metrics, leading to difficulties in classification and assessment. Fourth, most studies included in this review were conducted in developed countries. Despite the discussion of studies conducted in developing countries, they are inadequate in number. Therefore, more designed studies are needed to make confident recommendations on the subjective and objective metrics of GS, mental health outcomes, and the differences in disadvantaged populations across countries and regions.
Conclusions
This systematic review is among the first to assess the links between neighbourhood GS exposure and the mental health of underprivileged groups. It presents a comprehensive analysis of the indicators employed to assess neighbourhood GS exposure, various mental health outcomes for vulnerable people, moderating effects of regions, individual- and neighbourhood-level sociodemographic contexts, and types of disadvantaged residents. In addition, the potential mechanisms by which neighbourhood GS is associated with the mental health of disadvantaged populations were deciphered. We discussed the factors contributing to the variability in the results of subjective and objective indicators and identify several effective subjective and objective indicators which best predict the health benefits of neighbourhood GS exposure in disadvantaged groups. Furthermore, this study specifically analysed the heterogeneous effects of these mental health outcomes. These findings have implications for a comprehensive understanding of the associations and mechanisms be-tween neighbourhood GS and the mental health of disadvantaged groups. Further, it addresses the health equities probably induced by the unfair distribution of GS, and thus promotes health-oriented environmental planning and policies. Finally, more quantitative research should be designed and conducted that focuses on a wider array of vulnerable groups such as the unhoused or run away in the future. This will help researchers more accurately evaluate how neighbourhood GS affects the health of these communities.
Data availability
All data generated or analysed during this study are included in this published article [and its supplementary information files].
References
Abbasi A, Alalouch C, Bramley G (2016) Open space quality in deprived urban areas: user perspective and use pattern. Proc Soc Behav Sci 216:194–205
Afrad A, Kawazoe Y (2020) Can interaction with informal urban green space reduce depression levels? An analysis of potted street gardens in Tangier, Morocco. Public health 186:83–86
Ambrose G, Das K, Fan Y, Ramaswami A (2020) Is gardening associated with greater happiness of urban residents? A multi-activity, dynamic assessment in the Twin-Cities region, USA. Landsc Urban Plann 198. https://doi.org/10.1016/j.landurbplan.2020.103776
Anderson V, Gough WA, Agic B (2021). Nature-Based Equity: An Assessment of the Public Health Impacts of Green Infrastructure in Ontario Canada. Int J Environ Res Public Health, 18(11). https://doi.org/10.3390/ijerph18115763
Anzivino L (2019) The Villeneuve renovation program Health Impact Assessment. Eur J Public Health, 4:29. https://doi.org/10.1093/eurpub/ckz186.297
Astell-Burt T, Mitchell R, Hartig T (2014) The association between green space and mental health varies across the lifecourse. A longitudinal study. J Epidemiol Community Health 68(6):578–583
Astell-Burt T, Feng X, Mavoa S, Badland HM, Giles-Corti B (2014) Do low-income neighbourhoods have the least green space? A cross-sectional study of Australia’s most populous cities. BMC Public Health 14:1–11
Astell-Burt T, Hartig T, Putra IGNE, Walsan R, Dendup T, Feng X (2022) Green space and loneliness: A systematic review with theoretical and methodological guidance for future research. Sci Total Environ. 847:157521
Barreto PA, Lopes CS, da Silveira IH, Faerstein E, Junger WL (2019) Is living near green areas beneficial to mental health? Results of the Pro-Saude Study. Revista De Saude Publica, 53. https://doi.org/10.11606/s1518-8787.2019053001008
Beavers AW, Atkinson A, Varvatos LM, Connolly M, Alaimo K (2022) How Gardening in Detroit Influences Physical and Mental Health. Int J Environ Res Public Health, 19(13). https://doi.org/10.3390/ijerph19137899
Bonevski B, Randell M, Paul C, Chapman K, Twyman L, Bryant J, Brozek I, Hughes C (2014) Reaching the hard-to-reach: a systematic review of strategies for improving health and medical research with socially disadvantaged groups. BMC Med Res Methodol 14:1–29
Braveman PA, Kumanyika S, Fielding J, LaVeist T, Borrell LN, Manderscheid R, Troutman A (2011) Health disparities and health equity: the issue is justice. Am J Public Health 101(S1):S149–S155
Brown SC, Perrino T, Lombard J, Wang K, Toro M, Rundek T, Gutierrez CM, Dong C, Plater-Zyberk E, Nardi MI, Kardys J, Szapocznik J (2018) Health Disparities in the Relationship of Neighborhood Greenness to Mental Health Outcomes in 249,405 US Medicare Beneficiaries. Int J Environ Res Public Health, 15(3). https://doi.org/10.3390/ijerph15030430
Budowle R, Porter CM (2022) Cultivating Community Resilience With Agency and Sociality in Gardens for Health and Healing. Front Sustain Food Syst, 5. https://doi.org/10.3389/fsufs.2021.685384
Callaghan A, McCombe G, Harrold A, McMeel C, Mills G, Moore-Cherry N, Cullen W (2021) The impact of green spaces on mental health in urban settings: a scoping review. J Ment Health 30(2):179–193
Campbell A (1976) Subjective measures of well-being. Am Psychologist 31(2):117
Canberra DOIAT (2011) Australian Government: Our Cities Our Future: A national urban policy for a productive, sustainable and liveable future. https://www.oecd.org/regional/regional-policy/national-urban-policy-Australia.pdf
Certomà C (2015) Critical urban gardening. RCC Perspect 1:13–18
Chalmin-Pui LS, Roe J, Griffiths A, Smyth N, Heaton T, Clayden A, Cameron R (2021) “It made me feel brighter in myself”- The health and well-being impacts of a residential front garden horticultural intervention. Landsc Urban Plann, 205. https://doi.org/10.1016/j.landurbplan.2020.103958
Chen K, Zhang T, Liu F, Zhang Y, Song Y (2021) How Does Urban Green Space Impact Residents’ Mental Health: A Literature Review of Mediators. Int J Environ Res Public Health 18(22):11746
Cheng Y, Zhang J, Wei W, Zhao B (2021) Effects of urban parks on residents’ expressed happiness before and during the COVID-19 pandemic. Landsc Urban Plan 212:104118
Chenyang D, Maruthaveeran S, Shahidan MF (2022) The usage, constraints and preferences of green space at disadvantage neighborhood: a review of empirical evidence. Urban Forestry Urban Green 75:127696
Claeson A-S, Lidén E, Nordin M, Nordin S (2013) The role of perceived pollution and health risk perception in annoyance and health symptoms: a population-based study of odorous air pollution. Int Arch Occup Environ health 86:367–374
Clayton S (2007) Domesticated nature: Motivations for gardening and perceptions of environmental impact. J Environ Psychol 27(3):215–224
Cohen DA, Inagami S, Finch B (2008) The built environment and collective efficacy. Health Place 14(2):198–208
Cottagiri SA, Villeneuve PJ, Raina P, Griffith LE, Rainham D, Dales R, Peters CE, Ross NA, Crouse DL (2022) Increased urban greenness associated with improved mental health among middle-aged and older adults of the Canadian Longitudinal Study on Aging (CLSA). Environ Res 206, https://doi.org/10.1016/j.envres.2021.112587
Crouse DL, Pinault L, Christidis T, Lavigne E, Thomson EM, Villeneuve PJ (2021) Residential greenness and indicators of stress and mental well-being in a Canadian national-level survey. Environ Res 192, https://doi.org/10.1016/j.envres.2020.110267
Dadvand P, Bartoll X, Basagaña X, Dalmau-Bueno A, Martinez D, Ambros A, Cirach M, Triguero-Mas M, Gascon M, Borrell C (2016) Green spaces and general health: roles of mental health status, social support, and physical activity. Environ Int 91:161–167
de Keijzer C, Bauwelinck M, Dadvand P (2020) Long-term exposure to residential greenspace and healthy ageing: A systematic review. Curr Environ Health Rep 7:65–88
de Oliveira ES, Aspinall P, Briggs A, Cummins S, Leyland AH, Mitchell R, Roe J, Thompson CW (2013) How effective is the Forestry Commission Scotland’s woodland improvement programme-‘Woods In and Around Towns’ (WIAT)- at improving psychological well-being in deprived urban communities? A quasi-experimental study. BMJ Open 3(8), https://doi.org/10.1136/bmjopen-2013-003648
De Vries S, Van Dillen SM, Groenewegen PP, Spreeuwenberg P (2013) Streetscape greenery and health: Stress, social cohesion and physical activity as mediators. Social. Sci Med 94:26–33
Didsbury MS, Kim S, Medway MM, Tong A, McTaggart SJ, Walker AM, White S, Mackie FE, Kara T, Craig JC (2016) Socio‐economic status and quality of life in children with chronic disease: a systematic review. J Paediatrics Child Health 52(12):1062–1069
Dzhambov AM, Browning MH, Markevych I, Hartig T, Lercher P (2020) Analytical approaches to testing pathways linking greenspace to health: A scoping review of the empirical literature. Environ Res 186:109613
Dzhambov AM, Markevych I, Hartig T, Tilov B, Arabadzhiev Z, Stoyanov D, Gatseva P, Dimitrova DD (2018) Multiple pathways link urban green-and bluespace to mental health in young adults. Environ Res 166:223–233
Echeverría S, Diez-Roux AV, Shea S, Borrell LN, Jackson S (2008) Associations of neighborhood problems and neighborhood social cohesion with mental health and health behaviors: the Multi-Ethnic Study of Atherosclerosis. Health Place 14(4):853–865
Eggert LK, Blood-Siegfried J, Champagne M, Al-Jumaily M, Biederman DJ (2015) Coalition Building for Health: A Community Garden Pilot Project with Apartment Dwelling Refugees. J Commun Health Nurs 32(3):141–150. https://doi.org/10.1080/07370016.2015.1057072
Ekkel ED, de Vries S (2017) Nearby green space and human health: Evaluating accessibility metrics. Landsc Urban Plan 157:214–220
Flouri E, Midouhas E, Joshi H (2014) The role of urban neighbourhood green space in children’s emotional and behavioural resilience. J Environ Psychol 40:179–186. https://doi.org/10.1016/j.jenvp.2014.06.007
Forrest R, Kearns A (2001) Social cohesion, social capital and the neighbourhood. Urban Stud. 38(12):2125–2143
Gascon M, Triguero-Mas M, Martínez D, Dadvand P, Forns J, Plasència A, Nieuwenhuijsen MJ (2015) Mental health benefits of long-term exposure to residential green and blue spaces: a systematic review. Int J Environ Res Public Health 12(4):4354–4379
Gascon M, Sánchez-Benavides G, Dadvand P, Martínez D, Gramunt N, Gotsens X, Cirach M, Vert C, Molinuevo JL, Crous-Bou M (2018) Long-term exposure to residential green and blue spaces and anxiety and depression in adults: A cross-sectional study. Environ Res 162:231–239
Gascon M, Götschi T, de Nazelle A, Gracia E, Ambròs A, Márquez S, Marquet O, Avila-Palencia I, Brand C, Iacorossi F (2019) Correlates of walking for travel in seven European cities: the PASTA project. Environ Health Perspect 127(9):097003
Geneshka M, Coventry P, Cruz J, Gilbody S (2021) Relationship between green and blue spaces with mental and physical health: a systematic review of longitudinal observational studies. Int J Environ Res Public Health 18(17):9010
Gidlow CJ, Ellis NJ (2011) Neighbourhood green space in deprived urban communities: issues and barriers to use. Local Environ. 16(10):989–1002
Gonzales-Inca C, Pentti J, Stenholm S, Suominen S, Vahtera J, Kayhko N (2022) Residential greenness and risks of depression: Longitudinal associations with different greenness indicators and spatial scales in a Finnish population cohort. Health Place 74, https://doi.org/10.1016/j.healthplace.2022.102760
Hartig T, Mitchell R, De Vries S, Frumkin H (2014) Nature and health. Annu Rev Public Health 35:207–228
Hassink J, de Bruin S, Buist Y, Vaandrager L, Pijls H, Hop P (2018) Co-designing green social care services: Farmers and social entrepreneurs as new social care providers for vulnerable populations. Int J Integr Care 18:1–2. https://doi.org/10.5334/ijic.s2109
Hatala AR, Njeze C, Morton D, Pearl T, Bird-Naytowhow K (2020) Land and nature as sources of health and resilience among Indigenous youth in an urban Canadian context: a photovoice exploration. BMC Public Health, 20(1), https://doi.org/10.1186/s12889-020-08647-z
Henning C, Lieberg M (1996) Strong ties or weak ties? Neighbourhood networks in a new perspective. Scand Hous Plan Res 13(1):3–26
Holland I, DeVille NV, Browning MH, Buehler RM, Hart JE, Hipp JA, Mitchell R, Rakow DA, Schiff JE, White MP (2021) Measuring nature contact: a narrative review. Int J Environ Res Public Health 18(8):4092
Hong A, Martinez L, Patino JE, Duque JC, Rahimi K (2021) Neighbourhood green space and health disparities in the global South: Evidence from Cali, Colombia. Health Place 72:102690–102690. https://doi.org/10.1016/j.healthplace.2021.102690
Howley P (2011) Landscape aesthetics: Assessing the general publics’ preferences towards rural landscapes. Ecol Econ 72:161–169
Jabbar M, Yusoff MM, Shafie A (2021) Assessing the role of urban green spaces for human well-being: A systematic review. Geojournal 87:1–19
Jim CY, Shan X (2013) Socioeconomic effect on perception of urban green spaces in Guangzhou, China. Cities 31:123–131
Kaplan S (1995) The restorative benefits of nature: Toward an integrative framework. J Environ Psychol 15(3):169–182
Kodali HP, Ferris EB, Wyka K, Evenson KR, Dorn JM, Thorpe LE, Huang TTK (2023) The association of park use and park perception with quality of life using structural equation modeling. Front Public Health 11:1038288. https://doi.org/10.3389/fpubh.2023.1038288
Kondo MC, McIntire RK, Bilal U, Schinasi LH (2022) Reduction in socioeconomic inequalities in self-reported mental health conditions with increasing greenspace exposure. Health Place 78, https://doi.org/10.1016/j.healthplace.2022.102908
Korn A, Bolton SM, Spencer B, Alarcon JA, Andrews L, Voss JG (2018) Physical and Mental Health Impacts of Household Gardens in an Urban Slum in Lima, Peru. Int J Environ Res Public Health 15(8), https://doi.org/10.3390/ijerph15081751
Kuo FE, Sullivan WC, Coley RL, Brunson L (1998) Fertile ground for community: Inner‐city neighborhood common spaces. Am J Commun Psychol. 26(6):823–851
Laali KK, Greves WJ, Correa-Smits SJ, Zwarycz AT, Bunge SD, Borosky GL, Manna A, Paulus A, Chanan-Khan A (2018) Novel fluorinated curcuminoids and their pyrazole and isoxazole derivatives: Synthesis, structural studies, Computational/Docking and in-vitro bioassay. J Fluor Chem 206:82–98
Labib S, Lindley S, Huck JJ (2020) Spatial dimensions of the influence of urban green-blue spaces on human health: A systematic review. Environ Res 180:108869
Lachowycz K, Jones AP (2013) Towards a better understanding of the relationship between greenspace and health: Development of a theoretical framework. Landsc Urban Plan 118:62–69
Lambert EY (1990) The collection and interpretation of data from hidden populations (Vol. 98). US Department of Health and Human Services, Public Health Service, Alcohol
Lee S, Lee RJ, Scherr S (2023) How tree canopy cover can reduce urban suicide attempts: A geospatial analysis of the moderating role of area deprivation. Landsc Urban Plan 230, https://doi.org/10.1016/j.landurbplan.2022.104606
Lehmann LP, Detweiler JG, Detweiler MB (2018) Veterans in substance abuse treatment program self-initiate box gardening as a stress reducing therapeutic modality. Complem Therapies Med 36:50–53. https://doi.org/10.1016/j.ctim.2017.10.013
Liu Y, Wang R, Xiao Y, Huang B, Chen H, Li Z (2019) Exploring the linkage between greenness exposure and depression among Chinese people: Mediating roles of physical activity, stress and social cohesion and moderating role of urbanicity. Health Place 58:102168
Liu Y, Wang R, Lu Y, Li Z, Chen H, Cao M, Zhang Y, Song Y (2020) Natural outdoor environment, neighbourhood social cohesion and mental health: Using multilevel structural equation modelling, streetscape and remote-sensing metrics. Urban Forestry Urban Green 48:126576
Lu Y, Yang Y, Sun G, Gou Z (2019) Associations between overhead-view and eye-level urban greenness and cycling behaviors. Cities 88:10–18
Ma L, Huang Y, Liu T (2022) Unequal impact of the COVID-19 pandemic on mental health: Role of the neighborhood environment. Sustain Cities Soc 87, https://doi.org/10.1016/j.scs.2022.104162
Maas J, Van Dillen SM, Verheij RA, Groenewegen PP (2009) Social contacts as a possible mechanism behind the relation between green space and health. Health Place 15(2):586–595
Maas J, Verheij RA, de Vries S, Spreeuwenberg P, Schellevis FG, Groenewegen PP (2009) Morbidity is related to a green living environment. J Epidemiol Commun Health 63(12):967–973
Manley D, van Ham M, Doherty J (2011) Eleven: Social mixing as a cure for negative neighbourhood effects: evidence-based policy or urban myth? In Mixed communities. Policy Press, Bristol, UK, pp 151–168. Retrieved from https://doi.org/10.51952/9781847424952.ch011
Markevych I, Schoierer J, Hartig T, Chudnovsky A, Hystad P, Dzhambov AM, De Vries S, Triguero-Mas M, Brauer M, Nieuwenhuijsen MJ (2017) Exploring pathways linking greenspace to health: Theoretical and methodological guidance. Environ Res 158:301–317
Marquet O, Floyd MF, James P, Glanz K, Jennings V, Jankowska MM, Kerr J, Hipp JA (2020) Associations between worksite walkability, greenness, and physical activity around work. Environ Behav 52(2):139–163
McEachan RRC, Yang TC, Roberts H, Pickett KE, Arseneau-Powell D, Gidlow CJ, Wright J, Nieuwenhuijsen M (2018) Availability, use of, and satisfaction with green space, and children’s mental wellbeing at age 4 years in a multicultural, deprived, urban area: results from the Born in Bradford cohort study. Lancet Planet Health 2(6):E244–E254. https://doi.org/10.1016/S2542-5196(18)30119-0
McEachan RRC, Prady SL, Smith G, Fairley L, Cabieses B, Gidlow C, Wright J, Dadvand P, van Gent D, Nieuwenhuijsen MJ (2016) The association between green space and depressive symptoms in pregnant women: moderating roles of socioeconomic status and physical activity. J Epidemiol Commun Health 70(3):253–259. https://doi.org/10.1136/jech-2015-205954
McElroy E, Ashton M, Bagnall AM, Comerford T, McKeown M, Patalay P, Pennington A, South J, Wilson T, Corcoran R (2021) The individual, place, and wellbeing - a network analysis. BMC Public Health, 21(1). https://doi.org/10.1186/s12889-021-11553-7
Mendoza H, Rodriguez-Loureiro L, Gadeyne S, Lefebvre W, Vanpoucke C, Casas L (2023) Urban green spaces and suicide mortality in Belgium (2001-2011): A census-based longitudinal study. Environ Res 216, https://doi.org/10.1016/j.envres.2022.114517
Mennis J, Li X, Meenar M, Coatsworth JD, McKeon TP, Mason MJ (2021) Residential greenspace and urban adolescent substance use: Exploring interactive effects with peer network health, sex, and executive function. Int J Environ Res Public Health 18(4):1–15. https://doi.org/10.3390/ijerph18041611
Mitchell R, Popham F (2008) Effect of exposure to natural environment on health inequalities: an observational population study. Lancet 372(9650):1655–1660
Mitchell RJ, Richardson EA, Shortt NK, Pearce JR (2015) Neighborhood environments and socioeconomic inequalities in mental well-being. Am J Prevent Med 49(1):80–84
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group*, t. (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151(4):264–269
Mouratidis K (2020) Neighborhood characteristics, neighborhood satisfaction, and well-being: The links with neighborhood deprivation. Land Use Policy 99, https://doi.org/10.1016/j.landusepol.2020.104886
Murphy LF, Kalpakjian C, Charlifue S, Heinemann AW, Slavin M, Rohrbach T, Tulsky DS, Botticello AL (2022) Greener on the other side? an analysis of the association between residential greenspace and psychological well-being among people living with spinal cord injury in the United States. Spinal Cord 60(2):170–176. https://doi.org/10.1038/s41393-021-00736-z
Nawrath M, Guenat S, Elsey H, Dallimer M (2021) Exploring uncharted territory: Do urban greenspaces support mental health in low-and middle-income countries? Environ Res 194:110625
Nguyen M-H, Le T-T, Vuong Q-H (2023) Ecomindsponge: A novel perspective on human psychology and behavior in the ecosystem. Urban Sci 7(1):31
Nguyen P-Y, Astell-Burt T, Rahimi-Ardabili H, Feng X (2021) Green space quality and health: a systematic review. Int J Environ Res Public Health 18(21):11028
Nolen-Hoeksema S, Wisco BE, Lyubomirsky S (2008) Rethinking rumination. Perspect Psychological Sci 3(5):400–424
Núñez M, Suzman L, Maneja R, Bach A, Marquet O, Anguelovski I, Knobel P (2022) Gender and sex differences in urban greenness’ mental health benefits: A systematic review. Health Place 76:102864
O’Mara-Eves A, Brunton G, Oliver S, Kavanagh J, Jamal F, Thomas J (2015) The effectiveness of community engagement in public health interventions for disadvantaged groups: a meta-analysis. BMC Public Health 15:1–23
Perrino T, Lombard J, Rundek T, Wang K, Dong C, Gutierrez CM, Toro M, Byrne MM, Nardi MI, Kardys J, Szapocznik J, Brown SC (2019) Neighbourhood greenness and depression among older adults. Br J Psychiatry 215(2):476–480. https://doi.org/10.1192/bjp.2019.129
Pihl CL (2015) Libby community garden horticulture therapy: Building community belonging and self-worth for individuals with disabilities in Libby, Montana. J Investig Med 63(1):167. https://doi.org/10.1097/JIM.0000000000000133
Plane J, Klodawsky F (2013) Neighbourhood amenities and health: Examining the significance of a local park. Soc Sci Med 99:1–8. https://doi.org/10.1016/j.socscimed.2013.10.008
Qin B, Zhu W, Wang J, Peng Y (2021) Understanding the relationship between neighbourhood green space and mental wellbeing: A case study of Beijing. China Cities 109:103039
Riemer H, Shavitt S, Koo M, Markus HR (2014) Preferences don’t have to be personal: Expanding attitude theorizing with a cross-cultural perspective. Psychological Rev. 121(4):619
Rifkin SB, Lewando-Hundt G, Draper A (2000) Participatory approaches in health promotion and health planning: a literature review. Health Development Agency, London
Rigolon A, Browning MH, McAnirlin O, Yoon H (2021) Green space and health equity: a systematic review on the potential of green space to reduce health disparities. Int J Environ Res Public Health 18(5):2563
Roberts M, Irvine KN, McVittie A (2021) Associations between greenspace and mental health prescription rates in urban areas. Urban Forestry Urban Greening 64, https://doi.org/10.1016/j.ufug.2021.127301
Roe JJ, Aspinall PA, Ward Thompson C (2017) Coping with Stress in Deprived Urban Neighborhoods: What Is the Role of Green Space According to Life Stage? Front Psychol 8:1760. https://doi.org/10.3389/fpsyg.2017.01760
Roe JJ, Thompson CW, Aspinall PA, Brewer MJ, Duff EI, Miller D, Mitchell R, Clow A (2013) Green Space and Stress: Evidence from Cortisol Measures in Deprived Urban Communities. Int J Environ Res Public Health 10(9):4086–4103. https://doi.org/10.3390/ijerph10094086
Rogers WA (2004) Evidence based medicine and justice: a framework for looking at the impact of EBM upon vulnerable or disadvantaged groups. J Med Ethics 30(2):141–145
Sarkar C, Webster C, Gallacher J (2018) Residential greenness and prevalence of major depressive disorders: a cross-sectional, observational, associational study of 94 879 adult UK Biobank participants. Lancet Planet Health 2(4):e162–e173. https://doi.org/10.1016/s2542-5196(18)30051-2
Shanahan DF, Bush R, Gaston KJ, Lin BB, Dean J, Barber E, Fuller RA (2016) Health benefits from nature experiences depend on dose. Sci Rep 6(1):28551
Shuvo FK, Feng X, Akaraci S, Astell-Burt T (2020) Urban green space and health in low and middle-income countries: A critical review. Urban Forestry Urban Green 52:126662
South EC, Hohl BC, Kondo MC, MacDonald JM, Branas CC (2018) Effect of Greening Vacant Land on Mental Health of Community-Dwelling Adults A Cluster Randomized Trial. JAMA Netw Open 1(3), https://doi.org/10.1001/jamanetworkopen.2018.0298
Space C (2010) Urban green nation: Building the evidence base. CABE, London
Starfield B (2001) Improving equity in health: a research agenda. Int J Health Serv 31(3):545–566
Subiza-Pérez M, García-Baquero G, Babarro I, Anabitarte A, Delclòs-Alió X, Vich G, Roig-Costa O, Miralles-Guasch C, Lertxundi N, Ibarluzea J (2021) Does the perceived neighborhood environment promote mental health during pregnancy? Confirmation of a pathway through social cohesion in two Spanish samples. Environ Res 197, https://doi.org/10.1016/j.envres.2021.111192
Sugiyama T, Leslie E, Giles-Corti B, Owen N (2008) Associations of neighbourhood greenness with physical and mental health: do walking, social coherence and local social interaction explain the relationships? J Epidemiol Commun Health 62(5):e9–e9
Sugiyama T, Villanueva K, Knuiman M, Francis J, Foster S, Wood L, Giles-Corti B (2016) Can neighborhood green space mitigate health inequalities? A study of socio-economic status and mental health. Health Place 38:16–21. https://doi.org/10.1016/j.healthplace.2016.01.002
Talhouk SN, Chalak A, Kamareddine Z, Fabian M, Itani M, Ferguson N (2021) Vertical gardening and Syrian women refugees in Lebanon: an exploratory study on motivation for gardening and depression relief. Local Environ 26(10):1235–1249. https://doi.org/10.1080/13549839.2021.1973393
Team MR (2010) Fair society, healthy lives: The Marmot Review: strategic review of health inequalities in England post-2010. Marmot Review Secretariat, London (UK), p 242
Thompson CW, Roe J, Aspinall P, Mitchell R, Clow A, Miller D (2012) More green space is linked to less stress in deprived communities: Evidence from salivary cortisol patterns. Landsc Urban Plan 105(3):221–229. https://doi.org/10.1016/j.landurbplan.2011.12.015
Thompson CW, Aspinall P, Roe J, Robertson L, Miller D (2016) Mitigating Stress and Supporting Health in Deprived Urban Communities: The Importance of Green Space and the Social Environment. Int J Environ Res Public Health 13(4), https://doi.org/10.3390/ijerph13040440
Thompson CW, Elizalde A, Cummins S, Leyland AH, Botha W, Briggs A, Tilley S, de Oliveira ES, Roe J, Aspinall P, Mitchell R (2019) Enhancing Health Through Access to Nature: How Effective are Interventions in Woodlands in Deprived Urban Communities? A Quasi-experimental Study in Scotland, UK. Sustainability 11(12), https://doi.org/10.3390/su11123317
Tomita A, Vandormael AM, Cuadros D, Di Minin E, Heikinheimo V, Tanser F, Slotow R, Burns JK (2017) Green environment and incident depression in South Africa: a geospatial analysis and mental health implications in a resource-limited setting. Lancet Planet Health 1(4):E152–E162. https://doi.org/10.1016/S2542-5196(17)30063-3
Triguero-Mas M, Dadvand P, Cirach M, Martinez D, Medina A, Mompart A, Basagana X, Grazuleviciene R, Nieuwenhuijsen MJ (2015) Natural outdoor environments and mental and physical health: Relationships and mechanisms. Environ Int 77:35–41. https://doi.org/10.1016/j.envint.2015.01.012
Triguero-Mas M, Donaire-Gonzalez D, Seto E, Valentín A, Martínez D, Smith G, Hurst G, Carrasco-Turigas G, Masterson D, van den Berg M (2017) Natural outdoor environments and mental health: Stress as a possible mechanism. Environ Res 159:629–638
Van den Berg M, Wendel-Vos W, van Poppel M, Kemper H, van Mechelen W, Maas J (2015) Health benefits of green spaces in the living environment: A systematic review of epidemiological studies. Urban Forestry Urban Green 14(4):806–816
Vanaken G-J, Danckaerts M (2018) Impact of green space exposure on children’s and adolescents’ mental health: A systematic review. Int J Environ Res Public Health 15(12):2668
Vilcins D, Sly PD, Scarth P, Mavoa S (2022) Green space in health research: an overview of common indicators of greenness. Rev Environ Health https://doi.org/10.1515/reveh-2022-0083
Von Lindern E, Hartig T, Lercher P (2016) Traffic-related exposures, constrained restoration, and health in the residential context. Health Place 39:92–100
Vuong Q-H (2022) A new theory of serendipity: Nature, emergence and mechanism. Walter De Gruyter GmbH, Berlin
Wallerstein NB, Duran B (2006) Using community-based participatory research to address health disparities. Health Promot Pract 7(3):312–323
Wan S, Rojas-Rueda D, Pretty J, Roscoe C, James P, Ji JS (2022) Greenspace and mortality in the UK Biobank: Longitudinal cohort analysis of socio-economic, environmental, and biomarker pathways. SSM Popul Health 19, https://doi.org/10.1016/j.ssmph.2022.101194
Wang R, Helbich M, Yao Y, Zhang J, Liu P, Yuan Y, Liu Y (2019) Urban greenery and mental wellbeing in adults: Cross-sectional mediation analyses on multiple pathways across different greenery measures. Environ Res 176:108535
Wang R, Yang B, Yao Y, Bloom MS, Feng Z, Yuan Y, Zhang J, Liu P, Wu W, Lu Y (2020) Residential greenness, air pollution and psychological well-being among urban residents in Guangzhou, China. Sci Total Environ 711:134843
Wang R, Feng Z, Pearce J (2022) Neighbourhood greenspace quantity, quality and socioeconomic inequalities in mental health. Cities 129, https://doi.org/10.1016/j.cities.2022.103815
Wendelboe-Nelson C, Kelly S, Kennedy M, Cherrie JW (2019) A scoping review mapping research on green space and associated mental health benefits. Int J Environ Res Public Health 16(12):2081
White MP, Alcock I, Wheeler BW, Depledge MH (2013) Would you be happier living in a greener urban area? A fixed-effects analysis of panel data. Psychological Sci 24(6):920–928
Won J, Lee J-S (2020) Impact of residential environments on social capital and health outcomes among public rental housing residents in Seoul, South Korea. Landsc Urban Plan, 203, https://doi.org/10.1016/j.landurbplan.2020.103882
World Health Organization (2022) World mental health report: transforming mental health for all. https://www.who.int/teams/mental-health-and-substance-use/world-mental-health-report
Wu W, Yao Y, Song Y, He D, Wang R (2021) Perceived influence of street-level visible greenness exposure in the work and residential environment on life satisfaction: Evidence from Beijing, China. Urban Forestry Urban Greening 62, https://doi.org/10.1016/j.ufug.2021.127161
Xiao Y, Miao S, Zhang Y, Chen H, Wu W (2021) Exploring the health effects of neighborhood greenness on Lilong residents in Shanghai. Urban Forestry Urban Green 66, https://doi.org/10.1016/j.ufug.2021.127383
Xu T, Nordin NA, Aini AM (2022) Urban Green Space and Subjective Well-Being of Older People: A Systematic Literature Review. Int J Environ Res Public Health 19(21):14227
Yang M, Dijst M, Faber J, Helbich M (2020) Using structural equation modeling to examine pathways between perceived residential green space and mental health among internal migrants in China. Environ Res 183, https://doi.org/10.1016/j.envres.2020.109121
Zhang X, Zhou S, Lin R, Su L (2020) Relationship between Long-Term Residential Green Exposure and Individuals’ Mental Health: Moderated by Income Differences and Residential Location in Urban China. Int J Environ Res Public Health 17(23), https://doi.org/10.3390/ijerph17238955
Zheng L, Zhao Y, Duan R, Yang W, Wang Z, Su J (2023) The influence path of community green exposure index on activity behavior under multi-dimensional spatial perception. Front Public Health 11:1243838
Acknowledgements
The authors would like to thank Prof. Jutta Kehrer of the University of Hong Kong for her support in the writing process.
Author information
Authors and Affiliations
Contributions
Conceptualisation: Z.X., T.N., K.L., B.Z., JH.Z., JG.Z.; Methodology: Z.X., T.N., K.L., JG.Z.; Investigation: Z.X., K.L., JH.Z., JG.Z.; Project administration: Z.X., K.L., B.Z., JH.Z., JG.Z.; Formal analysis: Z.X., J.Z., YX.L., JG.Z.; Data curation: Z.X., K.L., J.Z., YX.L.; Writing—original draft: Z.X., JG.Z.; Writing—review and editing: Z.X., T.N., K.L., B.Z., JH.Z., JG.Z.; Validation: J.Z., YX.L.; Visualisation: Z.X., J.Z., YX.L.;
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Informed consent
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xian, Z., Nakaya, T., Liu, K. et al. The effects of neighbourhood green spaces on mental health of disadvantaged groups: a systematic review. Humanit Soc Sci Commun 11, 488 (2024). https://doi.org/10.1057/s41599-024-02970-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1057/s41599-024-02970-1