Abstract
The cohort consisted of 9400 exposed children diagnosed with ventricular septal defect (VSD). The risk of community-acquired pneumonia (CAP) or asthma with VSD was assessed using the Cox proportional hazard model with an inverse probability of treatment weighting. During a mean follow-up of 6.67 years (starting from 12 months after birth), there were 2100 CAP admission cases among exposed patients (incidence rate: 33.2 per 1000 person-years) and 20,109 CAP admission cases among unexposed children (incidence rate: 29.6 per 1000 person-years), with hazard ration of 1.09 (95% CI 1.04–1.14).
Similar content being viewed by others
Introduction
Community-acquired pneumonia (CAP) is one of the most common infections in the pediatric population and the most frequent reason for hospitalization1,2. It is well known that the leading cause of CAP is a viral infection1,2. Also, patients with ventricular septal defect (VSD) have a higher risk for complications with viral diseases3,4.
A VSD is a defect in the septum separating the two lower chambers of the heart ventricles and is the most common congenital heart malformation5,6. Small VSDs often close independently, and if the opening is small such as pin size, the heart and lungs do not have to work harder7. Meanwhile, VSD with congenital heart failure is a common cyanotic congenital heart disease (CHD) in childhood predisposing to bronchopneumonia8,9,10. CHD increases pulmonary blood flow and is a common predisposing factor for pneumonia in children11. Pulmonary edema of VSD patients can lead to congestive heart failure and become a nidus of infection for lower respiratory tract infection3,4,12.
Moreover, as with CAP, asthma in children is a significant concern because it increases the number of hospital visits and has been an economic burden more than asthma in adults13,14. In particular, asthma medication costs were found to be the largest cost factor in children ($382.09 or 41.3% of total direct cost), whilst they were reported as being lower in adults13. A few studies have suggested that asthma or airway hypersensitivity is more common in children with CHD than in the general population15,16,17.
Based on these results, we assumed that VSD might have some associations with the severity of CAP and asthma in the pediatric population during childhood. However, recently, a few reports have suggested a surge in the risk of hospitalization existence of CAP and asthma in children with VSD18. Thus, the present study aimed to use an extensive national population-based data set that included stratified questionnaires and information on healthcare utilization to determine the association of VSD with risks of CAP and asthma hospitalization in children. Furthermore, we thoroughly analyzed detailed information regarding family income, residency, and birth history.
Methods
Data source
Demographic characteristics, health care utilization, and outcome data of all participants were obtained from the National Health Insurance Service (NHIS) of Korea and the National Health Screening Program for Infants and Children (NHSPIC) database. All residents must participate in the NHIS. It maintains health records regarding healthcare utilization, prescriptions, and national health screening programs for all residents of Korea. Also, before the NHIS of Korea and the NHSPIC, all residents agreed to provide their records to investigators and sign in. The NHSPIC database includes information about developmental screening implemented from the second to the seventh round for children aged 9–71 months.
Ethics approval and consent to participate
Conducted in alignment with the Declaration of Helsinki, the Korea National Institute for Bioethics Policy Institutional Review Board (IRB) approved this study (P01-201603–21-005) due to its retrospective nature. The Korea National Institute for Bioethics Policy IRB approved that all methods in this study were performed according to the relevant guidelines and regulations. Also, because of its retrospective nature, the Korea National Institute for Bioethics Policy Institutional Review Board waived informed consent.
Study population and study design
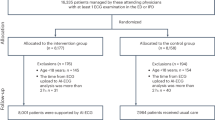
Figure 1 shows the study population’s selection. The present study included 2,395,966 Korean children born between 2008 and 2012. Of these, 121,339 were excluded according to the exclusion criteria (chromosomal abnormalities, congenital malformation of the respiratory system, cleft lip and cleft palate, disorder related to gestation length and fetal growth), leaving 2,274,627 eligible patients for further analyses. The 12,378 individuals received their first diagnosis of a VSD between birth and December 31, 2019. Of them, 2978 children have VSD with complex CHD (ex. Double outlet right ventricle (DORV), transposition of the great arteries (TGA), single ventricle (SV), atrioventricular septal defect (AVSD), pulmonary atresia (PA), pulmonary artery stenosis (PAS), aortic stenosis (AS), coarctation of the aorta (COA), total anomalous pulmonary venous return (TAPVR) plus partial anomalous pulmonary venous return (PAPVR), or tetralogy of Fallot (TOF) were excluded. Finally, 9400 children were assigned to the VSD group. After a 1:10 complete random sampling, 94,000 children were in the non-VSD group. Also, the VSD group was divided into two subgroups: VAD with heart failure (HF) (N = 513) and VAD without HF(N = 8,887).
Disposition of children in the study cohort. Individuals were identified from the National Health Insurance Service (NHIS) of Korea and the National Health Screening Program for Infants and Children (NHSPIC) database. After 1:10 random sampling, 9,400 children were assigned to the VSD group and 94,000 children were assigned to the non-VSD group. DORV double outlet right ventricle, AS aortic stenosis, ASD atrial septal defect, AVSD atrioventricular septal defect, COA coarctation of the aorta, PA pulmonary atresia, PAPVR partial anomalous pulmonary venous return, PAS pulmonary artery stenosis, SV single ventricle, TAPVR total anomalous pulmonary venous return, TOF tetralogy of Fallot, VSD ventricle septal defect.
Definitions and outcomes
The diagnosis was based on codes from the International Classification of Diseases 10th revision (ICD-10). VSD was diagnosed when a child had ICD-10 codes (Q21.0, ventricular septal defect; Q21.00, muscular ventricular septal defect; Q21.01, perimembranous ventricular septal defect; Q21.08, other ventricular septal defect; and Q21.09, ventricular septal defect, unspecified).
The primary endpoint was hospital admission for CAP diagnosed when a child had ICD-10 codes from J12X to J18X from NHIS claims-based data of inpatients. CAP hospital admission was also analyzed when a child had ICD-10 codes from J12X to J18X for inpatients after 12 months. The VSD with HF was analyzed when a child had ICD-10 codes from I50X for inpatients after 12 months.
Asthma was diagnosed when a child had ICD-10 codes of J45X or J46X at least twice and a prescription history of asthma medication (inhalation steroid and anti-leukotriene) from NHIS claims-based data of outpatients or admission history with ICD-10 codes of J45X or J46X for inpatients. The secondary endpoint was hospital admission for asthma diagnosed with ICD-10 codes of J45X or J46X for inpatients after 24 months. Meanwhile, atopic dermatitis (AD) and allergic rhinitis (AR) were diagnosed when a child had ICD-10 codes of L20.9 and J30. 4, respectively, at least five times for outpatients from NHIS claims-based data of outpatients.
Covariate and follow-up
Birthday, birth weight, prematurity, and breast milk feeding information were obtained from answers (by parents) to questionnaire items in the first round of the national health-screening program. Birth residence was used in the eligibility database divided into three regions (Seoul/metropolitan vs. urban vs. rural). Household income was determined based on insurance co-payment amount in eligibility database quintiles. Comorbidity allergic diseases including AD and AR were used in the eligibility database and divided into two classes (yes vs. no).
We separately analyzed subjects' primary (hospital admission for pneumonia) and secondary (hospital admission for asthma) endpoints. All participants were followed up from the index date (= birth date) until the diagnosis of pneumonia or asthma, outpatient visit, admission to the hospital, or the end of the study (December 31, 2019). To reduce risks of reverse causality and surveillance bias, we excluded those with the first year of follow-up for pneumonia and those with the first two years of follow-up for asthma. Follow-up of unexposed children was additionally censored if they were later diagnosed with VSD. These children were then moved to the exposed group.
Statistical analysis
Continuous variables are expressed as mean ± standard deviation (SD) based on data normality. They were compared using an independent sample t-test or Mann–Whitney U test, as appropriate. Cumulative incidence of events at 10 years was calculated based on Kaplan–Meier censoring estimates. Clinical outcomes of two groups were compared with the log-rank test.
Primary analyze was performed after adjusting for confounding factors. First, a multivariable Cox regression model was used. Covariates were sex, birth weight (< 3.2 kg or ≥ 3.2 kg), age at index date (1–5 years or ≥ 5 years), calendar year at index date (2008–2009 or 2010–2012), allergic disease (AR, AD, and asthma), and comorbidity number of hospital admission with any reason or wheezing during the first year after study entry (yes or no). Second, to reduce selection bias and other potential confounding factors, we performed an analysis using the logistic regression model with an inverse probability of treatment weighting (IPTW) for sensitivity analyses17. Adjusted covariates in IPTW analysis included sex, birth weight, calendar year at birth date, birth residence, and income quintile.
We established a multivariable Cox proportional hazards model to identify independent predictors over a median follow-up of 7 years’ pneumonia and major adverse events. Primary end point comparison according to the various exploratory subgroups was then performed. In all analyses, participating centers were included as random effects. All statistical analyses were performed using R (version 3.1.1) and SAS software ver. 9.4 (SAS Institute, Cary, NC, USA).
Institutional review board
The Korea National Institute for Bioethics Policy Institutional Review Board approved this study (P01-201603-21-005) due to retrospective nature.
Results
Baseline characteristics
A total of 103,400 children participated in this study, including 94,000 in the non-VSD group and 9400 in the VSD group. We first examined children's essential sociodemographic and clinical characteristics in VSD and non-VSD groups (Table 1). VSD and non-VSD groups had male gender in 46.26% and 51.23%, respectively. Among the VSD group, the two leading diagnosis types were Q21.09 (ventricular septal defect, unspecified, N = 2,967 (31.56%)) and Q21.0 (ventricular septal defect, N = 2,235 (23.78%)).
The final assessment was on December 31, 2019. The median follow-up was 6.67 (3.14) years for those with pneumonia and 7.65 (2.26) years for those with asthma in the VSD group. It was 6.96 (3.04) year for those with pneumonia and 7.78 (2.24) years for those with asthma. Compared with the control group, children with VSD were more likely to be male portion (P < 0.001), prematurity (P < 0.001), only breast milk feeding (P = 0.019), residency of birth (P < 0.001), and birth date (P < 0.001). However, children with VSD were no more likely to be income level (P = 0.436) and allergic disease comorbidity (AR (P = 0.429) and AD (P = 0.497). The allergic disease comorbidity was found in 2,974 (31.55%) children with AR and 1,359 (14.46%) children with asthma in the VSD group (Table 1).
Risk of CAP among children with VSD compared with matched non-VSD children
Results of comparing follow-up clinical outcomes of CAP between VSD and non-VSD groups are shown in Table 2. During a mean follow-up of 6.67 years (starting from 12 months after birth), we identified 2100 with a newly diagnosed CAP admission among exposed patients (incidence rate: 33.2 per 1000 person-years) and 20,109 CAP admission cases among unexposed children (incidence rate: 29.6 per 1000 person-years). This corresponded to an absolute rate difference of 3.65 (95% confidence interval (CI): 2.20–5.10) per 1000 person-years. After controlling for confounders, the risk for CAP during the second year after study entry was increased among patients with VSD (HR: 1.09, 95% CI 1.04–1.14) compared with matched children without VSD. Consistent results were found in IPTW analyses. After IPTW, the absolute rate difference was 2.96 (95% CI 1.42–4.49) per 1000 person-years.
In subgroup analysis for follow-up period admissions, these associations were not stronger among children with VSD regarding the number of admissions during the second year after study entry (HR: 1.09 [95% CI 0.99–1.19] and 0.84 [95% CI 0.79–0.88] for 0 time and ≥ 1 time, respectively; P for interaction < 0.001) or the number of admission with wheezing during the second year after study entry (HR: 1.06 [95% CI 0.99–1.13] and 0.87 [95% CI 0.81–0.93] for 0 time and ≥ 1 time, respectively; P for interaction < 0.001) (Table 2).
After restricting participants to be more than five years of follow-up, children with VSD had a higher cumulative incidence of CAP than their matched non-VSD children across the follow-up period (log-rank test P < 0.001) (Fig. 2).
Risk of CAP among children with VSD according to HF and operation
During a mean follow-up of 6.79 years (control), 6.27 years (VSD with no HF), and 3.26 years (VSD with HF) (starting from 12 months after birth), we identified 20,109 CAP admission cases among control (incidence rate: 29.6 per 1000 person-years) and 8887 CAP admission cases among VSD with no HF and 513 CAP admission cases among VSD with HF, respectively (Table 3). After controlling for confounders, the risk for CAP during the second year after study entry was increased among patients with VSD with no HF (HR: 1.08, 95% CI 1.03–1.13) and among patients with VSD with HF (HR: 1.42, 95% CI 1.20–1.68), compared with matched children without VSD. Also, the risk for CAP during the second year after study entry was increased in patients with VSD with HF than in patients with VSD with no HF (Table 3).
In subgroup analysis for follow-up period admissions, these associations were stronger among children with VSD operation at the number of admissions during the second year after study entry (HR, 2.85 [95% CI 1.44–5.67] and 1.00 [95% CI 0.75–1.33] for before and after, respectively; P for interaction = 0.003) (Table 3).
Risk of asthma among children with VSD compared with matched non-VSD children
Results of comparing follow-up clinical outcomes in asthma between VSD and non-VSD groups are shown in Table 4. During a mean follow-up of 7.65 years (starting from 24 months after birth), we identified 1010 asthma admission cases among exposed patients (incidence rate: 14.0 per 1000 person-years) and 9820 cases among unexposed children (incidence rate: 13.4 per 1000 person-years). This corresponded to an absolute rate difference of 6.25 (95% CI − 2.81–15.31) per 1000 person-years. After controlling for confounders, the risk for asthma admission or ER visit cases during the second year after study entry was increased among patients with VSD (HR: 1.05 [95% CI 0.99–1.13]) compared with matched children without VSD. Consistent results were also found in IPTW analyses, showing an absolute rate difference of 0.42(95% CI − 0.55–1.38) per 1000 person-years after IPTW.
In subgroup analysis for follow-up period admissions, these associations were not stronger among children with VSD at the number of admissions during the second year after study entry (HR, 1.00[95% CI 0.90–1.10] and 1.04[95% CI 0.95–1.14] for 0 and ≥ 1 time, respectively; P for interaction > 0.05) or the number of admission with wheezing during the second year after study entry (HR, 1.07[95% CI 0.98–1.15] and 0.95[95% CI 0.83–1.07] for 0 and ≥ 1 time, respectively; P for interaction > 0.05) (Table 4).
Discussion
In the present study, we investigated the association of VSD with CAP or asthma hospitalization in children with or without VSD in a large-scale, population-based nationwide pediatric cohort from Korea (n = 103,400). At the beginning of this study, we assumed that VSD might have some associations with the severity of CAP and asthma in the pediatric population during childhood. Thus, the current study had the following principal findings: (1) 12,378 (5.47%) individuals received their first diagnosis of VSD between birth and December 31, 2019, and (2) children with VSD were at elevated risk of hospital admission for CAP but not asthma. Moreover, using population-based comparisons, this is the first study to address VSD and its associations with CAP and asthma in the pediatric population.
CHD is a gross structural abnormality of the heart or intra thoracic great vessels that is actually or potentially of functional significance6,7,18. The incidence of CHD in the general population is about 1%, ranging from 4/1000 to 50/1000 live births18. In childhood, VSD, patent ductus arteriosus (PDA), atrioventricular septal defect (AVSD), and atrial septal defect (ASD) are common acyanotic CHD6,18. The incidence of isolated VSD is about 0.3% of newborns6, but the incidence is significantly lower in adults because > 90% may eventually close spontaneously3. The current study's prevalence of VSD (5.47%) was higher than in previous studies in the newborn registry6 and under five years of age18 because the study period was from birth to December 31, 2019, a short time to close spontaneously.
This study showed that children with VSD were at elevated risk of hospital admission for CAP but not asthma. CAP is the most common cause of death in children under five years old and is responsible for approximately 1.5 million ambulatory visits in children annually in the US 1,19,20. The leading cause of CAP is viral infection 1,19,20, and due to improvements in hygiene and successful vaccination programs, recent Korean statistics indicate that CAP is no longer the leading cause of death among children21.
There is pulmonary overcirculation and pulmonary edema12 because of left to right shunting of blood in children with CHD, including VSD. Due to this mechanism, patients with CHD have a higher risk for complications with viral diseases4,5. It is well-known that influenza infections are associated with high autopsy-confirmed coronary deaths among respiratory infections3. Additionally, in the case‐crossover study from a population‐based cohort4, CHD and ischemic stroke risk is higher after both in‐ and outpatient infection. Adults with infection had higher odds of CHD and ischemic stroke up to 90 days after infections compared with equivalent control periods 1 and 2 years before the event4. Recurrent acute lower respiratory tract infection often occurs in children with CHD18. Also, some CHD may predispose their sufferers to bronchopneumonia8,9,11, and children with pneumonia and CHD stayed significantly longer in the hospital than those without CHD. These results agreed with the present study, showing that children with VSD were at elevated risk of hospital admission for pneumonia compared to non-VSD children, and children with VSD with HF were at elevated risk of hospital admission for pneumonia compared to VSD children with non-HF. Therefore, children with VSD with HF might be at high risk because of their limited cardiopulmonary reserve.
Meanwhile, asthma in children is a significant concern because it increases the number of hospital visits and economic burden more than asthma in adults22. In the present study, we found that children with VSD were not significantly more frequently admitting asthma than non-VSD. This disagreement might be because asthma results from complex gene-environment interactions with heterogeneity in clinical presentation23,24. One study has demonstrated a high prevalence of airway hyperresponsiveness in patients with ASD, suggesting that airway hyperresponsiveness might be a possible mechanism for recurrent attacks of cough variant asthma25. The mechanism for cough variant asthma caused by heart disease is bronchial vascular congestion, resulting in bronchial edema and thickening. Furthermore, left ventricular dysfunction can lead to abnormal pulmonary function, such as airway hyperresponsiveness or restrictive and obstructive dysfunction25. A retrospective cohort study of children has documented that the hazard of recurrent cough variant asthma is higher in children with CHD, especially in children with complex congenital heart disease26. However, these two reports had no data about the relationship between VSD and asthma or data showing that CHD had how many diagnoses25,26.
The greatest strength of this study was that we performed various assessments of risk for VSD with CAP or asthma in a large population of children. However, this study has several limitations. First, children in our study were 11 years or younger. Thus, the generalizability of our findings to older children needs more long-term follow-up, and there may be differential misclassification where some children in the non-VSD group may have undiagnosed VSD, and the opposite is less likely. Second, because this was an observational study, measurement errors or misunderstandings of adjustment factors might have occurred. Additionally, surveillance bias could exist in this study. Third, no comparison exists between the influence of pre-and post-operative VSD on CAP or asthma hospitalization.
Conclusions
In summary, evidence supports that childhood VSD is related to a higher surge in admission rates in children with CAP, not asthma, compared with matched children without VSD. Children with VSD might be at high risk of admission because of their limited cardiopulmonary reserve and thus need more intensive care to prevent viral infection. Further studies are needed to better understand the underlying mechanisms.
Data availability
Data is provided within the manuscript information files.
Change history
10 May 2024
A Correction to this paper has been published: https://doi.org/10.1038/s41598-024-61472-x
References
Sandora, T. J. & Harper, M. B. Pneumonia in hospitalized children. Pediatr. Clin. North. Am. 52, 1059–1081 (2005).
Jain, S. et al. Community-acquired pneumonia requiring hospitalization among U.S. children. N. Engl. J. Med. 372, 835–845 (2015).
Madjid, M., Miller, C. C. & Zarubaev, V. V. Influenza epidemics and acute respiratory disease activity are associated with a surge in autopsy-confirmed coronary heart disease death: results from 8 years of autopsies in 34,892 subjects. Eur. Heart. J. 28, 1205–1210 (2007).
Cowan, L. T. et al. Inpatient and outpatient infection as a trigger of cardiovascular disease: the ARIC study. J Am. Heart. Assoc. 20, 7 (2018).
Pinto, N. M. et al. Early childhood inpatient costs of critical congenital heart disease. J. Pediatr. 203, 371–379 (2018).
Lindinger, A., Schwedler, G. & Hense, H. W. Prevalence of congenital heart defects in newborns in Germany: results of the first registration year of the PAN study (July2006 to June 2007). Klin. Padiatr. 222, 321–326 (2010).
Ventricular Septal Defect. In: The clinical recognition of congenital heart disease 5th edn. (W.B Saunders Company, Philadelphia, 2003).
McDaniel, N. L. & Gutgesell, H. P. Ventricular septal defect. In Moss and Adams Heart disease in infants, children and adolescents, in the fetus and young adults 6th edn (eds Allen, H. D. et al.) 636–651 (Lippincott Williams and Wilkins, Philadelphia, 2001).
Satpathy, M. & Jayarajah, M. Patent ductus arteriosus. In Clinical diagnosis of congenital heart disease (eds Satpathy, M. & Mishra, B. R.) 15–23 (Jaypee brothers, Hyderabad, 2008).
Feldt, R. H. et al. Atrioventricular septal defect. In Moss and Adams Heart disease in infants, children and adolescents, in the fetus and young adults 6th edn (eds Allen, H. D., Gutgesell, H. P., Clark, E. B. et al.) 619–635 (Lippincott Williams and Wilkins, Philadelphia, 2001).
Owayad, A. F., Campbell, D. M. & Wang, E. E. Underlying causes of recurrent pneumonia in children. Arch. Pediatr. Adolesc. Med. 154, 190–194 (2000).
Malviya, A. & Yadav, R. COVID -19 pandemic and paediatric population with special reference to congenital heart disease. Indian. Heart. J. 72, 141–144 (2020).
Bahadori, K. et al. Economic burden of asthma: a systematic review. BMC. Pulm. Med. 9, 24 (2009).
Guillemand, J. P., El-Hakim, H., Richards, S. & Chauhan, N. Airway pathologic abnormalities in symptomatic children with congenital cardiac and vascular disease. Arch. Otolaryngol. Head. Neck. Surg. 133, 672–676 (2007).
Tsubata, S. et al. Bronchial hyper-responsiveness to inhaled histamine in children with congenital heart disease. Acta. Paediatr. Jpn. 37, 336–340 (1995).
Hayes, D. Idiopathic pulmonary arterial hypertension misdiagnosed as asthma. J Asthma. 44, 19–22 (2007).
Lee, O. H. et al. Safety and efficacy of contemporary drug-eluting stents in patients with ST-segment elevation myocardial infarction and a high ischemic risk. Front. Cardiovasc. Med. 9, 880351 (2022).
Jat, N. K. et al. Assessment of the prevalence of congenital heart disease in children with pneumonia in tertiary care hospital: a cross-sectional study. Ann. Med. Surg. 73, 103111 (2022).
Roh, E. J., Shim, J. Y. & Chung, E. H. Epidemiology and surveillance implications of community-acquired pneumonia in children. Clin. Exp. Pediatr. 65, 563–573 (2022).
Williams, D. J. et al. Short- vs standard-course outpatient antibiotic therapy for community-acquired pneumonia in children: The SCOUT-CAP randomized clinical trial. JAMA. Pediatr. 176, 253–261 (2022).
Dong, I. S. Community-acquired pneumonia in Korean children: time to read between the lines. Clin. Exp. Pediatr. 66, 22–23 (2023).
Lee-Sarwar, K. A., Bacharier, L. B. & Litonjua, A. A. Strategies to alter the natural history of childhood asthma. Curr. Opin. Allergy. Clin. Immunol. 17, 139–145 (2017).
Papi, A., Brightling, C., Pedersen, S. E. & Reddel, H. K. Asthma. Lancet. 391, 783–800 (2018).
Lim, J. E., Kim, H. M., Kim, J. H., Baek, H. S. & Han, M. Y. Association between dyslipidemia and asthma in children: A systematic review and multicenter cohort study using a common data model. Clin. Exp. Pediatr. 66, 357–365 (2023).
Nassif, M. et al. Atrial septal defect in adults is associated with airway hyperresponsiveness. Cong. Heart. Dis. 13, 959–966 (2018).
Feng, B. W., He, C. Y., Liu, X. Q., Chen, Y. S. & He, S. R. Effect of congenital heart disease on the recurrence of cough variant asthma in children. BMC. Cardiovasc. Disord. 21, 130 (2021).
Funding
This work was supported by Korea Health Technology R&D through the Korea (HR22C1605030022). This work was also supported by Soonchunhyang University Research Fund.
Author information
Authors and Affiliations
Contributions
M.S. and M.Y.H. designed the present study, drafted the article, analyzed the data, interpreted the data and drafted the manuscript. M.Y.H. interpreted the data and revised the article critically for important intellectual content. M.S. interpreted the data and revised the article critically for important intellectual content. All authors designed the present study, interpreted the data and revised the article critically for important intellectual content. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this Article was revised: The original version of this Article contained an error in the name of Eun Kyo Ha, which was incorrectly given as Eun Gyo Ha.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sung, M., Kim, J.H., Ha, E.K. et al. Population-based retrospective cohort study on community-acquired pneumonia hospitalization in children with a ventricular septal defect. Sci Rep 14, 9307 (2024). https://doi.org/10.1038/s41598-024-59510-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-59510-9
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.