Abstract
Inhaled NO (iNO) may be protective against hyperoxic injury in the premature lung, but the mechanism is unknown. We hypothesized that NO would prevent hyperoxia-induced nuclear factor kappa B (NF-κB) activation in neonatal pulmonary microvascular endothelial cells [human pulmonary microvascular endothelial cell (HPMEC)] and prevent the up-regulation of target genes. After hyperoxic exposure (O2 >95%), nuclear NF-κB consensus sequence binding increased and was associated with IκBα degradation. Both of these findings were prevented by exposure to NO. Furthermore, intracellular adhesion molecule (ICAM)-1 mRNA and protein levels increased in cells exposed to hyperoxia, an effect abrogated by NO. To evaluate the potentially toxic effect of NO plus hyperoxia, cell viability and proliferation were assessed. Cells exposed to NO plus hyperoxia demonstrated improved survival as measured by trypan blue exclusion when compared with cells exposed to hyperoxia alone. These differences in cell death could not be attributed to apoptosis measured by caspase-3 activity. Finally, cellular proliferation inhibited by hyperoxia was rescued by concurrent exposure to NO. These data demonstrate that NO prevents hyperoxia-induced NF-κB activation in HPMEC and results in decreased expression of adhesion molecules and decreased cellular toxicity. This may help to explain the protective effects of NO on hyperoxic injury in the developing lung vasculature.
Similar content being viewed by others
Main
Oxidative and inflammatory stimuli encountered after preterm birth injure the immature lung and contribute to the pathogenesis of bronchopulmonary dysplasia (BPD) (1). Strategies aimed at preventing BPD, including inhaled NO (iNO), have been minimally successful thus far (2).
Studies using animal models have shown that NO is protective against hyperoxic lung injury (3). However, NO can react with oxygen to form nitrogen dioxide (NO2) or with superoxide (O2−) to form peroxynitrite (ONOO−), both of which are toxic to the respiratory system (4). A better understanding of the mechanism by which NO protects the neonatal lung from hyperoxia could lead to a more targeted use of this therapy.
The transcription factor nuclear factor kappa B (NF-κB) activates genes in response to inflammatory and oxidative stress (5). In preterm infants, NF-κB activation has been linked to BPD (6). However, whether this increased activation is a protective response or whether it is causative to the injury remains unexplored.
After inflammatory stimuli, such as TNF-α, NO can inhibit canonical NF-κB signaling in a cell type and concentration-dependent manner (5). Posttranslational modifications of proteins in the NF-κB activation cascade, including s-nitrosylation of NF-κB subunits (7,8) and s-nitrosylation of inhibitory κB kinase (IKK) (9), account for this inhibition. In contrast, oxidant stress-induced NF-κB activation occurs via the atypical pathway and involves unique kinases, including PI3 kinase and c-Src, that are not involved in the canonical pathway (5). Less is known regarding the effect of NO on NF-κB activation after oxidant stress. In adult rats exposed to hyperoxia, iNO inhibited NF-κB activation in the lung (10). However, hyperoxia-induced NF-κB activation is maturationally regulated (11), and it is not known whether NO has a similar inhibitory effect in the newborn lung.
In this study, primary neonatal pulmonary microvascular endothelial cells [human pulmonary microvascular endothelial cell (HPMEC)] were exposed to hyperoxia and NO, and NF-κB activation was evaluated. Hyperoxia-induced NF-κB activation was inhibited by concurrent exposure to NO. In addition, NO prevented NF-κB-regulated intracellular adhesion molecule (ICAM)-1 expression. Oxygen toxicity, manifesting as increased cell death after 48 h of exposure, was limited by concurrent exposure to NO. Furthermore, in contrast to hyperoxia, NO plus hyperoxia preserved HPMEC proliferation. Overall, the data provide new insights on the potential mechanism by which NO limits hyperoxic injury in the newborn lung.
METHODS
Cell culture and exposures.
HPMEC (ScienCell, San Diego, CA), primary cells derived from human neonatal lung, were exposed to hyperoxia (95% O2/5% CO2), NO alone (5% CO2, 95% room air, 20 ppm NO), or hyperoxia plus NO (5% CO2, 95% O2, 20 ppm NO) in a C-Chamber (Biospherix, Redfield, NY). NO was delivered via an iNOvent (Ikaria, Clinton, NJ) using a gas flow of 3.5 L/min to prevent the accumulation of NO within the C-Chamber. Levels of NO2 were checked at the expiratory port on the C-chamber. Canonical NF-κB signaling was induced with TNF-α (12), and NF-κB activity was inhibited by using BAY 11–7082 as previously described (11). To evaluate the effect of cGMP on NF-κB activity, the cell permeable and phosphodiesterase-resistant cGMP analog 8-bromo-cGMP (1 mm; Sigma Chemical Co.) was added to cells 1 h before exposures.
Preparation of cytosolic and nuclear extractions.
Nuclear and cytosolic fractions were extracted and protein content determined as previously described (12).
Evaluation of nuclear NF-κB binding by electrophoretic mobility shift assay (EMSA).
EMSA was performed as detailed elsewhere (12).
Western blot analysis.
Immunoblotting was performed as previously described (12). The following antibodies were used: anti-IκBα (catalog no. sc-371; Santa Cruz Biotechnology, Santa Cruz, CA), anti-ICAM1 antibodies (catalog no. ab2213; Abcam, Cambridge, CA), anticaspase-3 (Calbiochem), antinitrotyrosine (609, a kind gift from Dr. Harry Ischiropolous), anticalnexin (Stressgen, Ann Arbor, MI), or anti-TBP (Aviva, San Diego, CA).
Detection of intracellular reactive oxygen species.
Cells were incubated with 10-μm CM-H2DCFDA in serum-free medium for 1 h. Medium was replaced before exposures. Cell lysate was prepared, and fluorescence was measured (excitation 492 nm, emission wavelength 525 nm) using the SpectraMax Gemini Spectrophotometer and analyzed using Softmax Pro Software (Molecular Devices, Sunnyvale, CA).
Evaluation of ICAM-1 mRNA levels.
Total RNA was isolated using the RNeasy Kit (Quiagen). Reverse transcription was performed with Superscript II Reverse Transcriptase (Invitrogen). ICAM-1 mRNA (#Hs00164932_m1, Applied Biosystems) levels were analyzed with the Taqman Gene Expression Assay according to the manufacturer's instructions and normalized to 18s rRNA (Hs99999901.s1, Applied Biosystems).
Evaluation of cell death using trypan blue exclusion.
The trypan blue exclusion assay, as a measure of cell viability, was performed as described previously (11).
Evaluation of caspase-3 activity.
Caspase-3 activity, as a measure of apoptosis, was performed as described previously (12).
Evaluation of cellular proliferation using bromodeoxyuridine ELISA.
A cellular proliferation ELISA kit was used according to the manufacturer's instructions (Roche). Light emitted by the chemiluminescent reaction was quantified using the In Vivo Imaging System (Xenogen, Alameda, CA).
Statistical analysis.
For comparison between treatment groups, the null hypothesis in which no difference existed between treatment means was tested by ANOVA for multiple groups or t test for two groups (InStat, GraphPad, San Diego, CA). The results are given as mean ± SEM.
RESULTS
Hyperoxia-induced NF-κB activation is prevented by NO in HPMEC.
Nuclear extracts from HPMEC exposed to 24 h of hyperoxia demonstrated significantly increased NF-κB consensus sequence binding when compared with control (Fig. 1A and B). The band that appeared after exposure to hyperoxia was completely dissipated by an unlabeled oligonucleotide, but was not affected by the addition of a mutant oligonucleotide, suggesting this newly appearing band represented hyperoxia-induced NF-κB DNA binding. In contrast, no increased binding was observed in HPMEC exposed to NO plus hyperoxia or NO alone at this same time point. Densitometric analysis revealed a statistically significant increase in NF-κB consensus sequence binding only in cells exposed to hyperoxia, with no differences in any group at 4 or 8 h of exposure (data not shown). The increased binding was similar in pattern but lower in intensity to binding induced by TNF-α, used here as a positive control. Differences between inflammatory and oxidant stress-induced NF-κB consensus sequence binding are demonstrated by the modest binding in response to hyperoxia when compared with TNF-α and are consistent with previous reports (12). Furthermore, a supershift after incubation with both anti-p50 and -p65 antibodies was observed, indicating activation of the p50-p65 heterodimer (Fig. 1C). Supporting this data, significant increases in nuclear p65 occurred only after exposure to hyperoxia (Fig. 1D and E). These results suggest that NO inhibits hyperoxia-induced NF-κB activation before nuclear translocation of activated subunits.
NO prevents hyperoxia-induced NF-κB consensus sequence binding of nuclear proteins. HPMEC were exposed to 24 h of room air, hyperoxia, NO plus hyperoxia, NO alone, or TNF-α (4 h). A, Representative EMSA; mutant, mutant oligonucleotide plus TNF-α sample; cold, unlabeled oligonucleotide plus TNF-α sample. Bands representing NF-κB consensus sequence binding, nonspecific binding, and free probe are labeled. B, Densitometric evaluation of fold change in the induced NF-κB band showing increased binding after hyperoxia is prevented by NO. n = 3 for each group. *p < 0.001 vs air, O2 + NO, and NO. C, Representative EMSA showing supershift experiments of nuclear extracts from fetal cells exposed to 24 h of hyperoxia. Hyperoxia, 24 h of exposure; p50 ab, supershift with anti-p50 antibody; p65, supershift with anti-p65 antibody; mutant, mutant oligonucleotide plus hyperoxia-exposed sample; cold, unlabeled oligonucleotide plus hyperoxia-exposed sample. Bands representing NF-κB consensus sequence binding, NF-κB supershift, nonspecific binding and free probe are labeled. D, Representative Western blot showing p65 in nuclear extracts exposed to hyperoxia or NO plus hyperoxia with TBP as loading control. M = marker. E, Densitometric evaluation of fold change in nuclear p65 after exposure to hyperoxia or NO plus hyperoxia. n = 3 for each group. *p < 0.001 vs air.
NO prevents prolonged hyperoxia-induced IκBα degradation.
To further define the signaling events leading to NF-κB activation, levels of cytoplasmic immunoreactive IκBα were evaluated (Fig. 2A and B). HPMEC exposed to hyperoxia showed significantly decreased IκBα levels after 4 h of hyperoxia that remained low throughout the 24-h exposure. In contrast, levels of IκBα returned to baseline by 24 h in cells exposed to NO plus hyperoxia. Cells exposed to NO alone showed no change in the level of immunoreactive IκBα. These data suggest that NO prevents sustained hyperoxia-induced degradation of IκBα and that NO may inhibit hyperoxia-induced NF-κB activation by stabilizing the inhibitory protein IκBα.
Prolonged degradation of IκBα in HPMEC exposed to hyperoxia is abrogated by NO. HPMEC were exposed to room air, hyperoxia, hyperoxia plus NO, or NO alone. A, Representative Western blot showing IκBα in HPMEC, with 40 kD marker labeled and calnexin as loading control. B, Densitometric evaluation of IκBα after exposure to room air (□), hyperoxia (▪), NO plus hyperoxia ( ), or NO alone (
), or NO alone ( ) n = 3 for each group. *p < 0.01 vs time 0 and †p < 0.05 vs time 0.
) n = 3 for each group. *p < 0.01 vs time 0 and †p < 0.05 vs time 0.
NO prevents NF-κB-regulated ICAM-1 expression.
To better understand the consequences of hyperoxia-induced NF-κB activation in this primary endothelial cell model, the expression of the adhesion molecule ICAM-1 was evaluated. NF-κB regulates the expression of ICAM-1 (13), an adhesion molecule that mediates neutrophil adhesion and transmigration across the endothelium. Hyperoxic exposure for 24 h resulted in a significant increase in the amount of ICAM-1 protein expressed by HPMEC when compared with control (Fig. 3A and B). In contrast, no increased ICAM-1 was observed in cells exposed to NO plus hyperoxia. To demonstrate ICAM-1 expression is dependent on NF-κB in our model system, Bay 11–7082, an inhibitor of IκBα phosphorylation, was added to cells before exposure with TNF-α. The addition of Bay 11–7082 completely prevented IκBα degradation after a 30-min exposure to TNF-α (Fig. 3C). Furthermore, Bay 11–7082 prevented increased ICAM-1 expression after a 4-h exposure to TNF-α and had no effect on hyperoxia-induced ICAM-1 expression. These results show that hyperoxia-induced NF-κB activation occurs via a pathway independent from canonical NF-κB signaling. Further supporting the finding is that ICAM-1 expression is dependent on NF-κB activation, modest but significant increases in ICAM-1 mRNA was observed in cells exposed to hyperoxia (Fig. 3D). In contrast, cells exposed to NO plus hyperoxia showed no increase in ICAM-1 mRNA. These data suggest that NO inhibits hyperoxia-induced NF-κB regulated ICAM-1 expression.
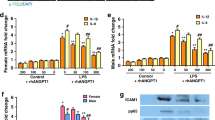
NO prevents NF-κB regulated-ICAM-1 expression. HPMEC were exposed to room air, hyperoxia, NO plus hyperoxia, or TNF-α. A, Representative Western blot showing ICAM-1 expression in HPMEC exposed to hyperoxia, NO plus hyperoxia or TNF-α, with 100 kD marker labeled and calnexin as loading control. B, Densitometric evaluation of ICAM-1 after exposure to room air, hyperoxia, or NO plus hyperoxia. n = 3 for each group. *p < 0.05 vs time 0. C, IκBα and ICAM-1 protein after exposure to BAY 11–7082, TNF-α, TNF-α plus BAY 11–7082, hyperoxia, or hyperoxia plus BAY 11–7082. Calnexin is shown as loading control. C, control; BAY, 10 μm BAY 11–7082; TNF 30 m, TNF-α exposure for 30 min; TNF 4 h, TNF-α exposure for 30 min; TNF + BAY, TNF exposure plus 10 μm BAY 11–7082; O2, hyperoxia for 24 h, O2 + BAY, hyperoxia plus 10 μm BAY 11–7082. D, ICAM-1 mRNA levels as determined by quantitative RT-PCR in cells exposed to room air (□), hyperoxia (▪), or NO plus hyperoxia ( ). Measurements are first normalized to 18s and expressed as a ratio to air-exposed control. n = 3 for each group. *p < 0.05 vs time 0 and †p < 0.05 vs hyperoxic exposure of same duration.
). Measurements are first normalized to 18s and expressed as a ratio to air-exposed control. n = 3 for each group. *p < 0.05 vs time 0 and †p < 0.05 vs hyperoxic exposure of same duration.
Hyperoxia plus NO does not affect NF-κB signaling through increased cGMP, by increasing nitrotyrosine posttranslational modifications or decreasing reactive oxygen species (ROS) formation.
To determine whether the effect of NO on hyperoxia-induced NF-κB activation was mediated through increased levels of cGMP, cells were treated with 8-bromo-cGMP (1 mm) 1 h before exposure to hyperoxia. This cell permeable and phosphodiesterase-resistant cGMP analog was unable to replicate that ability of NO to prevent IκBα degradation (Fig. 4A). This suggests that the effect of NO does not occur because of an increase in intracellular levels of cGMP. To further define the events leading to inhibition of hyperoxia-induced NF-κB activation by NO, levels of immunoreactive nitrotyrosine posttranslational modifications were evaluated. No difference in the global amount of nitrotyrosine modifications in cells exposed to hyperoxia or NO plus hyperoxia for 24 h was observed (Fig. 4B). Human-nitrated fibrinogen, isolated as described elsewhere, was used as a positive control (14). This indicates the effect of NO on NF-κB signaling was independent of this specific protein modification. Finally, as NO itself is a free radical and thus can act to scavenge other free radicals (15), ROS generation after exposures to hyperoxia and NO plus hyperoxia were evaluated. After 24 h, the time point at which cells exposed to hyperoxia or NO plus hyperoxia demonstrate different NF-κB activation, there was a 1.2-fold increase in ROS formation in cells exposed to hyperoxia (Fig. 4C). In contrast, there was a 2-fold increase in ROS in cells exposed NO plus hyperoxia. These data suggest that NO does not inhibit hyperoxia-induced NF-κB activation by acting as an antioxidant.
NO does not affect NF-κB signaling by increasing cGMP, nitrotyrosine posttranslational modifications or by inhibiting ROS production. HPMEC were exposed to room air, hyperoxia, or NO plus hyperoxia. A, Representative Western blot showing no effect of 8-bromo-cGMP (1 mm) on hyperoxia-induced IκBα degradation. Calnexin is shown as loading control. C, control; cGMP, 8-bromo-cGMP; O2 24 h, hyperoxia for 24 h; O2 + cGMP, 8-bromo-cGMP plus hyperoxia for 24 h. B, Representative Western blot showing global nitrotyrosine protein modifications in HPMEC exposed to air (A), hyperoxia (O2), or NO plus hyperoxia (NO + O2) for 24 h. Nitrated fibrinogen (N-Fib) was used as a positive control. C, Fold induction of DCFDA oxidation in cells exposed to air, hyperoxia, or NO plus hyperoxia. *p < 0.05 vs air and hyperoxia.
NO limits oxygen toxicity in neonatal pulmonary endothelial cells.
To assess the potential effect of NO plus hyperoxia on endothelial cell death, trypan blue exclusion assays were performed. No significant difference in the percentage of dead cells was found between HPMEC exposed to room air, hyperoxia, or NO plus hyperoxia after 24 h of exposure (data not shown). In contrast, HPMEC exposed to 48 h of hyperoxia demonstrated 60% mortality, whereas cells exposed to hyperoxia plus NO showed no difference from control (Fig. 5). Using this assay, control cells demonstrated 25% mortality, an effect attributed to the use of a primary cell culture for this study. This suggests that NO delivered at a constant level of 20 ppm does not increase oxygen toxicity in neonatal pulmonary endothelial cells and in fact protects cells from the toxic effects of hyperoxia.
NO decreases cell death in HPMEC exposed to hyperoxia. HPMEC were exposed to room air, hyperoxia, or NO plus hyperoxia. Viability was assessed by trypan blue exclusion as described. Graph represents percent viable cells after exposure. n = 3 for each group. *p < 0.001 vs air and NO plus hyperoxia and †p < 0.05 vs air.
NO plus hyperoxia does not increase apoptosis in HPMEC.
To evaluate whether the increase in cell death after exposure to hyperoxia was because of apoptosis, caspase-3 activity was assessed. A significant decrease in caspase-3 activity was found in cells exposed to hyperoxia for 24 h, with a return to baseline by 48 h (Fig. 6A). In contrast, although cells exposed to NO plus hyperoxia demonstrated a significant decrease in caspase-3 activity at 24 h, this activity was inhibited even further by 48 h. Western analysis of procaspase-3 performed on cells exposed to room air, hyperoxia, or NO plus hyperoxia for 48 h supported these findings (Fig. 6B). Densitometric analysis revealed there was no significant change in procaspase-3 after any exposure, thus no cleavage and caspase activation, supporting the data found by caspase-3 activity assay (Fig. 6C). These data suggest that neither hyperoxia nor NO plus hyperoxia induce apoptosis in HPMEC, implicating necrosis as the cause of cell death.
NO plus hyperoxia does not increase apoptosis in HPMEC. HPMEC were exposed to room air, hyperoxia, or NO plus hyperoxia. A, Graph represents fold change in caspase-3 activity in cells after exposure to room air (□), hyperoxia (▪), or NO plus hyperoxia ( ); *p < 0.05 vs air and †p < 0.051 vs air and hyperoxia of same time point. B, Representative Western blot showing procaspase 3 expression in HPMEC exposed to hyperoxia or NO plus hyperoxia for 48 h, with 30 kD marker labeled and calnexin as loading control. C, Densitometric evaluation of procaspase 3 after exposure to air, hyperoxia, or NO plus hyperoxia for 48 h. n = 4 for each group.
); *p < 0.05 vs air and †p < 0.051 vs air and hyperoxia of same time point. B, Representative Western blot showing procaspase 3 expression in HPMEC exposed to hyperoxia or NO plus hyperoxia for 48 h, with 30 kD marker labeled and calnexin as loading control. C, Densitometric evaluation of procaspase 3 after exposure to air, hyperoxia, or NO plus hyperoxia for 48 h. n = 4 for each group.
NO abrogates the effect of hyperoxia on HPMEC proliferation.
As inhibition of NF-κB activity has been shown to promote angiogenesis (16), bromodeoxyuridine (BrdU) labeling was assessed to determine whether the inhibition of hyperoxia-induced NF-κB activity by NO-affected cellular proliferation. Decreased proliferation was seen in cells exposed to hyperoxia for 24 h (Fig. 7). In contrast, cells exposed to NO plus hyperoxia had increased cellular proliferation when compared with hyperoxia alone (Fig. 7). Exposure to NO alone resulted in no changes in proliferation when compared with room air control (data not shown). Thus, NO abrogates the effect of hyperoxia on endothelial cell proliferation. As inhibition of NF-κB activation has been implicated in stimulating angiogenesis (16), we speculate the effect observed here may be related to the effect of NO on NF-κB activity.
NO abrogates the effect of hyperoxia on HPMEC proliferation. HPMEC were exposed to 24 h of room air, hyperoxia, NO plus hyperoxia, or NO alone. Cellular proliferation was assessed using BrdU incorporation as described. Graph represents BrdU incorporation as a ratio of air control. n = 3 for each group. *p < 0.01 vs air control.
DISCUSSION
We show here, for the first time, that NO delivered at a steady state of 20 ppm inhibits hyperoxia-induced NF-κB activation. We chose 20 ppm as this is the maximum dose administered in recent randomized control trials evaluating the role of iNO in preventing BPD and seems to limit the adverse effects of the gas (17). In addition, NO donors have variable half-lives, making it difficult to deliver a continuous steady-state in cell culture (18). We found that cells exposed to NO plus hyperoxia expressed less ICAM-1 and exhibited less death compared with cells exposed to hyperoxia alone. Thus, NO may help to prevent inflammatory cell recruitment and prevent hyperoxic lung injury.
For this study, we chose to evaluate the effect of NO on hyperoxic injury in primary endothelial cells derived from human neonates. Our interest in evaluating this specific cell type stems from previous work showing that the pulmonary endothelium is uniquely sensitive to hyperoxic injury. These cells are the first to demonstrate morphologic changes in response to hyperoxia and contribute to the early inflammatory stage of injury by binding neutrophils and platelets (19). Pulmonary endothelial cells of newborn mice exposed to hyperoxia demonstrate structural alterations including polymorphonuclear leukocyte and platelet adhesion (20). Fewer inflammatory cells were seen in newborn rats exposed to NO plus hyperoxia when compared with oxygen-exposed controls (21). Thus, it seems that NO acts partly by limiting inflammatory cell recruitment in the newborn lung, thus limiting the extent of hyperoxic lung injury. Our study supports these findings and defines a mechanism by which this occurs.
One important mediator of inflammation in the lung is NF-κB. This transcription factor regulates the expression of adhesion molecules, including ICAM-1 (22). ICAM-1 mediates interactions between endothelial cells and cells expressing β2 integrins, including neutrophils, monocytes, lymphocytes, and natural killer cells. After exposure to inflammatory stimuli, including TNF-α, endothelial cells increase ICAM-1 expression via NF-κB activation (22). Hyperoxia increases ICAM-1 expression in pulmonary endothelium in neonatal models (23). To this point, only one report has linked hyperoxia-induced NF-κB activation and ICAM-1 expression. In that study, inhibiting hyperoxia-induced NF-κB activation with glucocorticoids prevented ICAM-1 up-regulation in cultured human adult pulmonary artery endothelial cells (24). Hyperoxia-induced NF-κB activation is maturationally regulated (11), with a more robust response occurring in neonatal animals. Our report shows NO inhibits hyperoxia-induced NF-κB activation in a neonatal model. Our data suggest that NO, through inhibition of hyperoxia induced-NF-κB up-regulation of ICAM-1 expression, could decrease inflammatory cell influx into the neonatal lung and prevent injury. In vivo studies are needed to confirm these findings.
Previous work has shown that NO inhibits NF-κB-regulated adhesion cell molecule expression in endothelial cells after inflammatory stimuli (25). This inhibition has been attributed to stabilization of the inhibitory protein IκBα (26) and multiple posttranslational modifications of proteins in the NF-κB activation cascade. These modifications include s-nitrosylation of NF-κB subunits (7,8). To this point, much of the work on how NO affects NF-κB activation has focused on canonical signaling. However, oxidant stress-induced NF-κB activation occurs via the atypical pathway, distinct from the canonical pathway responsible for inflammatory induction of NF-κB activation (5). Previous work from our laboratory has identified a role for phosphorylation of IκBα on tyrosine 42 in mediating hyperoxia-induced NF-κB activation (12). In this study, we asked whether posttranslational modifications of IκBα, specifically nitrotyrosine, accounted for the inhibition of hyperoxia-induced NF-κB activation seen in cells exposed to NO plus hyperoxia. However, there was no evidence of nitrotyrosine modifications of IκBα (via immunoprecipitation, data not shown), or of a global increase in nitrotyrosine posttranslational modifications in cells exposed to NO plus hyperoxia. Furthermore, we could not find evidence to support the effect of NO on hyperoxia-induced NF-κB signaling occurred because of the increases in cGMP or decreased ROS formation. We speculate that NO causes other posttranslational modifications of the proteins in the pathway leading the hyperoxia-induced NF-κB activation. Further work to identify the exact mechanism of inhibition of hyperoxia-induced NF-κB activation needs to be performed.
Many studies have raised the concern of potential synergistic toxicity of hyperoxia and NO. Fetal type II pneumocytes and lung fibroblasts demonstrate increased cell death with concurrent NO and hyperoxic exposure (27,28). Herein, cultured primary neonatal pulmonary endothelial cells showed no evidence of synergistic toxicity between hyperoxia and NO. Rather, these cells had preserved cellular proliferation, less cell death, and inhibition of apoptosis with the dose of NO we used for up to 48 h. We speculate that the response to NO plus hyperoxia is cell type specific and depends on how NO is delivered and accounts for these differences. In studies using other cell culture models, NF-κB activation has been shown to inhibit angiogenesis (16). We speculate the increased cellular proliferation seen in cells exposed to NO plus hyperoxia may be due in part to inhibition of NF-κB activity, but other factors may play a role. The physiologic implications of these findings must be evaluated using in vivo models. Furthermore, we limited our exposures to hyperoxia and NO to 48 h. Toxicity may increase with longer exposures, and this may have clinical relevance for premature infants with hypoxic respiratory failure treated with NO and oxygen for prolonged periods of time.
In summary, we report that hyperoxia-induced NF-κB activation is inhibited by NO resulting in decreased ICAM-1 expression in endothelial cells. Furthermore, NO has protective effects against hyperoxia-induced cell death and inhibition of cellular proliferation. We speculate that the ability of NO to inhibit hyperoxia-induced NF-κB activation may partly explain the protective effect of iNO in preventing BPD in some preterm infants.
Abbreviations
- BPD:
-
bronchopulmonary dysplasia
- BrdU:
-
bromodeoxyuridine
- EMSA:
-
electrophoretic mobility shift assay
- HPMEC:
-
human pulmonary microvascular endothelial cells
- IκBα:
-
inhibitory kappa b alpha
- iNO:
-
inhaled NO
- NF-κB:
-
nuclear factor kappa B
- RA:
-
room air
- ROS:
-
reactive oxygen species
References
Baraldi E, Filippone M 2007 Chronic lung disease after premature birth. N Engl J Med 357: 1946–1955
Barrington KJ, Finer NN 2007 Inhaled nitric oxide for preterm infants: a systematic review. Pediatrics 120: 1088–1099
ter Horst SA, Walther FJ, Poorthuis BJ, Hiemstra PS, Wagenaar GT 2007 Inhaled nitric oxide attenuates pulmonary inflammation and fibrin deposition and prolongs survival in neonatal hyperoxic lung injury. Am J Physiol Lung Cell Mol Physiol 293: L35–L44
Ricciardolo FL, Sterk PJ, Gaston B, Folkerts G 2004 Nitric oxide in health and disease of the respiratory system. Physiol Rev 84: 731–765
Janssen-Heininger YM, Poynter ME, Baeuerle PA 2000 Recent advances towards understanding redox mechanisms in the activation of nuclear factor kappaB. Free Radic Biol Med 28: 1317–1327
Bourbia A, Cruz MA, Rozycki HJ 2006 NF-kappaB in tracheal lavage fluid from intubated premature infants: association with inflammation, oxygen, and outcome. Arch Dis Child Fetal Neonatal Ed 91: F36–F39
Kelleher ZT, Matsumoto A, Stamler JS, Marshall HE 2007 NOS2 regulation of NF-kappaB by S-nitrosylation of p65. J Biol Chem 282: 30667–30672
Marshall H, Stamler J 2001 Inhibition of NF-kappa B by S-nitrosylation. Biochemistry 40: 1688–1693
Reynaert NL, Ckless K, Korn SH, Vos N, Guala AS, Wouters EF, van der Vliet A, Janssen-Heininger YM 2004 Nitric oxide represses inhibitory kappaB kinase through S-nitrosylation. Proc Natl Acad Sci U S A 101: 8945–8950
Howlett CE, Hutchison JS, Veinot JP, Chiu A, Merchant P, Fliss H 1999 Inhaled nitric oxide protects against hyperoxia-induced apoptosis in rat lungs. Am J Physiol 277: L596–L605
Yang G, Abate A, George A, Weng Y, Dennery PA 2004 Maturational differences in lung NF-kappaB activation and their role in tolerance to hyperoxia. J Clin Invest 114: 669–678
Wright CJ, Zhuang T, La P, Yang G, Dennery PA 2009 Hyperoxia-induced NF-kappaB activation occurs via a maturationally sensitive atypical pathway. Am J Physiol Lung Cell Mol Physiol 296: L296–L306
van de Stolpe A, Caldenhoven E, Stade BG, Koenderman L, Raaijmakers JA, Johnson JP, van der Saag PT 1994 12-O-tetradecanoylphorbol-13-acetate- and tumor necrosis factor alpha-mediated induction of intercellular adhesion molecule-1 is inhibited by dexamethasone. Functional analysis of the human intercellular adhesion molecular-1 promoter. J Biol Chem 269: 6185–6192
Heijnen HF, van Donselaar E, Slot JW, Fries DM, Blachard-Fillion B, Hodara R, Lightfoot R, Polydoro M, Spielberg D, Thomson L, Regan EA, Crapo J, Ischiropoulos H 2006 Subcellular localization of tyrosine-nitrated proteins is dictated by reactive oxygen species generating enzymes and by proximity to nitric oxide synthase. Free Radic Biol Med 40: 1903–1913
Halliwell B, Gutteridge J 2007 Free Radicals in Biology and Medicine. Oxford University Press, Oxford, England
Tabruyn SP, Griffioen AW 2007 A new role for NF-kappaB in angiogenesis inhibition. Cell Death Differ 14: 1393–1397
Arul N, Konduri GG 2009 Inhaled nitric oxide for preterm neonates. Clin Perinatol 36: 43–61
Aga RG, Hughes MN 2008 The preparation and purification of NO gas and the use of NO releasers: the application of NO donors and other agents of nitrosative stress in biological systems. Methods Enzymol 436: 35–48
Crapo JD 1986 Morphologic changes in pulmonary oxygen toxicity. Annu Rev Physiol 48: 721–731
Bonikos DS, Bensch KG, Ludwin SK, Northway WH 1975 Oxygen toxicity in the newborn. The effect of prolonged 100 per cent O2 exposure on the lungs of newborn mice. Lab Invest 32: 619–635
Couroucli XI, Wei YH, Jiang W, Muthiah K, Evey LW, Barrios R, Moorthy B 2006 Modulation of pulmonary cytochrome P4501A1 expression by hyperoxia and inhaled nitric oxide in the newborn rat: implications for lung injury. Pediatr Res 59: 401–406
Collins T, Read MA, Neish AS, Whitley MZ, Thanos D, Maniatis T 1995 Transcriptional regulation of endothelial cell adhesion molecules: NF-kappa B and cytokine-inducible enhancers. FASEB J 9: 899–909
Suzuki Y, Aoki T, Takeuchi O, Nishio K, Suzuki K, Miyata A, Oyamada Y, Takasugi T, Mori M, Fujita H, Yamaguchi K 1997 Effect of hyperoxia on adhesion molecule expression in human endothelial cells and neutrophils. Am J Physiol 272: L418–L425
Suzuki Y, Nishio K, Takeshita K, Takeuchi O, Watanabe K, Sato N, Naoki K, Kudo H, Aoki T, Yamaguchi K 2000 Effect of steroid on hyperoxia-induced ICAM-1 expression in pulmonary endothelial cells. Am J Physiol Lung Cell Mol Physiol 278: L245–L252
De Caterina R, Libby P, Peng HB, Thannickal VJ, Rajavashisth TB, Gimbrone MA, Shin WS, Liao JK 1995 Nitric oxide decreases cytokine-induced endothelial activation. Nitric oxide selectively reduces endothelial expression of adhesion molecules and proinflammatory cytokines. J Clin Invest 96: 60–68
Peng HB, Libby P, Liao JK 1995 Induction and stabilization of I kappa B alpha by nitric oxide mediates inhibition of NF-kappa B. J Biol Chem 270: 14214–14219
Raghuram N, Fortenberry JD, Owens ML, Brown LA 1999 Effects of exogenous nitric oxide and hyperoxia on lung fibroblast viability and DNA fragmentation. Biochem Biophys Res Commun 262: 685–691
Bhandari V, Johnson L, Smith-Kirwin S, Vigliotta G, Funanage V, Chander A 2002 Hyperoxia and nitric oxide reduce surfactant components (DSPC and surfactant proteins) and increase apoptosis in adult and fetal rat type II pneumocytes. Lung 180: 301–317
Acknowledgements
Patrick Fernando provided technical assistance for completion of this article.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by a Grant K12-HD00850 from the Pediatric Scientist Development Program [C.J.W.], the iNO Therapeutics Advancing Newborn Medicine Fellowship Grant [C.J.W.], the Marshall-Klaus Perinatal Research Award [C.J.W.], and a Grant RO-1 HL-58752 [P.A.D.].
Rights and permissions
About this article
Cite this article
Wright, C., Agboke, F., Chen, F. et al. NO Inhibits Hyperoxia-Induced NF-κB Activation in Neonatal Pulmonary Microvascular Endothelial Cells. Pediatr Res 68, 484–489 (2010). https://doi.org/10.1203/PDR.0b013e3181f917b0
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3181f917b0
This article is cited by
-
Molsidomine decreases hyperoxia-induced lung injury in neonatal rats
Pediatric Research (2023)
-
Oxygen toxicity: cellular mechanisms in normobaric hyperoxia
Cell Biology and Toxicology (2023)
-
Protective Effects of 18β-Glycyrrhetinic Acid on Neonatal Rats with Hyperoxia Exposure
Inflammation (2022)
-
Astragalus polysaccharides mediated preventive effects on bronchopulmonary dysplasia in rats
Pediatric Research (2014)