Abstract
Glans hypermobility (GH) is a well-described clinical entity that can have significant implications for cosmesis and function, resulting in sexual dissatisfaction, penile pain, and early device erosion, with an estimated incidence of 0.04% to 10%. We developed a novel grading scale to assess GH severity intraoperatively during primary inflatable penile prosthesis (IPP) placement and describe a modified glanspexy technique to correct GH when encountered during IPP placement. 530 patients who underwent primary IPP placements from two high-volume prosthetic surgeons between February 2018 – November 2019 were retrospectively reviewed in order to identify the incidence of GH. Of these, 139 (26.2%) had hypermobility. Employing our new scaling system, grade 1, 2, and 3 GH was seen in 86 (16.2%), 29 (5.5%), and 24 (4.5%) cases, respectively. Increased implant size correlated with a decreased likelihood of GH incidence. Each increase in implant size by 1 cm decreased the incidence of detecting GH by 11.0% (OR = 0.89; p = 0.015). 11 patients underwent primary GH repair using our described technique. At one-year follow-up, one patient required repeat glanspexy for recurrent bothersome GH and a second patient developed a suture granuloma at the glanspexy incision requiring unilateral cylinder explant. Our modified glanspexy technique can be used to correct GH in any direction and is a useful tool for the prosthetic surgeon’s armamentarium.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
None.
References
Deveci S, Martin D, Parker M, Mulhall JP. Penile length alterations following penile prosthesis surgery. Eur Urol. 2007;51:1128–31.
Habous M, Muir G, Soliman T, Farag M, Williamson B, Binsaleh S, et al. Outcomes of variation in technique and variation in accuracy of measurement in penile length measurement. Int J Impot Res. 2018;30:21–26.
Porena M, Mearini L, Mearini E, Marzi M, Zucchi A. Penile prosthesis implantation and couple’s satisfaction. Urol Int. 1999;63:185–7.
Kramer AC, Schweber A. Patient expectations prior to coloplast titan penile prosthesis implant predicts postoperative satisfaction. J Sex Med. 2010;7:2261–6.
Minervini A, Ralph DJ, Pryor JP. Outcome of penile prosthesis implantation for treating erectile dysfunction: experience with 504 procedures. BJU Int. 2006;97:129–33.
Skrodzka M, Heffernan Ho D, Ralph D. Floppy glans-classification, diagnosis and treatment. Sex Med Rev. 2020;8:303–13.
Ziegelmann MJ, Alom M, Bole R, Kohler T, Trost L. Modified Glanulopexy technique for supersonic transporter deformity and glanular hypermobility in men with penile prostheses. J Sex Med. 2018;15:914–9.
Mulhall JP, Kim FJ. Reconstructing penile supersonic transporter (SST) deformity using glanulopexy (glans fixation). Urology. 2001;57:1160–2.
Kim J, Drury R, Morenas R, Raheem O. Pathophysiology and grayscale ultrasonography of penile corporal fibrosis. Sex Med Rev. 2022;10:99–107.
Bickell M, Manimala N, Parker J, Steixner B, Wiegand L, Carrion R. Floppy Glans syndrome: Pathogenesis and treatment. Sex Med Rev. 2016;4:149–56.
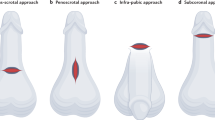
Jayadevan R, Eleswarapu SV, Mills JN. Infrapubic approach for placement of inflatable penile prosthesis: contemporary review of technique and implications. Int J Impot Res. 2020;32:10–17.
Gupta NK, Ring J, Trost L, Wilson SK, Kohler TS. The penoscrotal surgical approach for inflatable penile prosthesis placement. Transl Androl Urol. 2017;6:628–38.
De Stefani S, Simonato A, Capone M, Ciampalini S, Maffezzini M, Carmignani G. The benefit of glans fixation in prosthetic penile surgery. J Urol. 1994;152:1533–4.
Morey AF. Reconstructing penile supersonic transporter (SST) deformity using glanulopexy (glans fixation). J Urol. 2005;174:969.
Martínez-Salamanca JI, Mueller A, Moncada I, Carballido J, Mulhall JP. Penile prosthesis surgery in patients with corporal fibrosis: a state of the art review. J Sex Med. 2011;8:1880–9.
Trost L, Wanzek P, Bailey G. A practical overview of considerations for penile prosthesis placement. Nat Rev Urol. 2016;13:33–46.
Mulcahy JJ. The prevention and management of noninfectious complications of penile implants. Sex Med Rev. 2015;3:203–13.
Mulhall JP, Jahoda A, Aviv N, Valenzuela R, Parker M. The impact of sildenafil citrate on sexual satisfaction profiles in men with a penile prosthesis in situ. BJU Int. 2004;93:97–9.
Chew KK, Stuckey BG. Use of transurethral alprostadil (MUSE) (prostaglandin E1) for glans tumescence in a patient with penile prosthesis. Int J Impot Res. 2000;12:195–6.
Wallen, JJ, Madiraju S, Tayon K, Gross M, Carrion R, Perito P. Durasphere as new agent for the treatment of hypermobile glans. J Urol. 2017. Elsevier Science Inc 360 Park Ave South, New York, NY 10010-1710 USA.
Ball TP Jr. Surgical repair of penile “SST” deformity. Urology. 1980;15:603–4.
Acknowledgements
None.
Funding
None.
Author information
Authors and Affiliations
Contributions
TK contributed to the conceptual design of the study, manuscript review, and writing. MZ and AM were responsible for writing and reviewing the manuscript. ND and RM were responsible for data collection. SH contributed to the study’s conceptual design and in manuscript review. SSJ, MB, and PP also contributed to the conceptual design and participated in the manuscript review.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Köhler, T., Mian, A., Ziegelmann, M. et al. Glans hypermobility scale (GHS): A simple grading scale and description of a modified glanspexy technique. Int J Impot Res (2024). https://doi.org/10.1038/s41443-024-00843-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41443-024-00843-4