Abstract
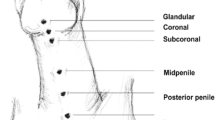
Hypospadias is a common abnormality of the urogenital tract with a wide range of variety in its presentation and severity. The primary aim to correct hypospadias is to restore normal penile function and appearance. Although it can be corrected at any age, early correction between the 6 and 18 months of life is recommended. The functional and cosmetic outcomes have been very-well presented in the literature, although the aspects of sexuality and fertility of hypospadias repair in the long term are vague. In this narrative review, we aimed to gather the data around the sexuality and fertility outcomes of hypospadias repair and acknowledge urologists and parents of boys with hypospadias who will have a correction surgery about future sexual and fertility concerns.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Yu X, Nassar N, Mastroiacovo P, Canfield M, Groisman B, Bermejo-Sánchez E, et al. Hypospadias prevalence and trends in international birth defect surveillance systems, 1980-2010. Eur Urol. 2019;76:482–90.
Tack L, Praet M, Van Dorpe J, Haid B, Buelens S, Hoebeke P, et al. Androgen receptor expression in preputial dartos tissue correlates with physiological androgen exposure in congenital malformations of the penis and in controls. J Pediatr Urol. 2020;16:43.e41–43.e48.
van der Zanden LF, van Rooij IA, Feitz WF, Franke B, Knoers NV, Roeleveld N. Aetiology of hypospadias: a systematic review of genes and environment. Hum Reprod Update. 2012;18:260–83.
Radmayr C, Bogaert G, Dogan HS, Nijman R, Silay MS, Stein R, et al. EAU guidelines on paediatric urology 2020. In: European association of urology guidelines. Presented at the EAU Annual Congress Amsterdam 2020. Arnhem, The Netherlands: European Association of Urology Guidelines Office; 2020.
Sommerlad BC. A long-term follow-up of hypospadias patients. Br J Plast Surg. 1975;28:324–30.
Deibert CM, Hensle TW. The psychosexual aspects of hypospadias repair: a review. Arab J Urol. 2011;9:279–82.
Fraumann SA, Stephany HA, Clayton DB, Thomas JC, Pope JCT, Adams MC, et al. Long-term follow-up of children who underwent severe hypospadias repair using an online survey with validated questionnaires. J Pediatr Urol. 2014;10:446–50.
Bracka A. A long-term view of hypospadias. Br J Plast Surg. 1989;42:251–5.
Aho MO, Tammela OK, Tammela TL. Aspects of adult satisfaction with the result of surgery for hypospadias performed in childhood. Eur Urol. 1997;32:218–22.
Mor Y, Ramon J, Jonas P. Is only meatoplasty a legitimate surgical solution for extreme distal hypospadias? A long-term follow-up after adolescence. BJU Int. 2000;85:501–3.
Kumar S, Tomar V, Yadav SS, Priyadarshi S, Vyas N, Agarwal N. Fertility potential in adult hypospadias. J Clin Diagn Res. 2016;10:Pc01–05.
Miller MA, Grant DB. Severe hypospadias with genital ambiguity: adult outcome after staged hypospadias repair. Br J Urol. 1997;80:485–8.
Mondaini N, Ponchietti R, Bonafè M, Biscioni S, Di Loro F, Agostini P, et al. Hypospadias: incidence and effects on psychosexual development as evaluated with the Minnesota Multiphasic Personality Inventory test in a sample of 11,649 young Italian men. Urol Int. 2002;68:81–5.
Bubanj TB, Perovic SV, Milicevic RM, Jovcic SB, Marjanovic ZO, Djordjevic MM. Sexual behavior and sexual function of adults after hypospadias surgery: a comparative study. J Urol. 2004;171:1876–9.
Aho MO, Tammela OK, Somppi EM, Tammela TL. Sexual and social life of men operated in childhood for hypospadias and phimosis. a comparative study. Eur Urol. 2000;37:95–100.
Moriya K, Kakizaki H, Tanaka H, Furuno T, Higashiyama H, Sano H, et al. Long-term cosmetic and sexual outcome of hypospadias surgery: norm related study in adolescence. J Urol. 2006;176:1889–92.
Schönbucher VB, Landolt MA, Gobet R, Weber DM. Psychosexual development of children and adolescents with hypospadias. J Sex Med. 2008;5:1365–73.
Rynja SP, Wouters GA, Van Schaijk M, Kok ET, De Jong TP, De Kort LM. Long-term followup of hypospadias: functional and cosmetic results. J Urol. 2009;182:1736–43.
Vandendriessche S, Baeyens D, Van Hoecke E, Indekeu A, Hoebeke P. Body image and sexuality in adolescents after hypospadias surgery. J Pediatr Urol. 2010;6:54–9.
Chertin B, Natsheh A, Ben-Zion I, Prat D, Kocherov S, Farkas A, et al. Objective and subjective sexual outcomes in adult patients after hypospadias repair performed in childhood. J Urol. 2013;190:1556–60.
Jiao C, Wu R, Xu X, Yu Q. Long-term outcome of penile appearance and sexual function after hypospadias repairs: situation and relation. Int Urol Nephrol. 2011;43:47–54.
Wang WW, Tu XA, Deng CH, Mo JC, Zhao L, Chen LW. Long-term sexual activity status and influencing factors in men after surgery for hypospadias. Asian J Androl. 2009;11:417–22.
Rynja SP, de Jong T, Bosch J, de Kort LMO. Proximal hypospadias treated with a transverse preputial island tube: long-term functional, sexual, and cosmetic outcomes. BJU Int. 2018;122:463–71.
Tack LJW, Springer A, Riedl S, Tonnhofer U, Weninger J, Hiess M, et al. Psychosexual outcome, sexual function, and long-term satisfaction of adolescent and young adult men after childhood hypospadias repair. J Sex Med. 2020;17:1665–75.
Kiss A, Sulya B, Szász AM, Romics I, Kelemen Z, Tóth J, et al. Long-term psychological and sexual outcomes of severe penile hypospadias repair. J Sex Med. 2011;8:1529–39.
Örtqvist L, Fossum M, Andersson M, Nordenström A, Frisén L, Holmdahl G, et al. Sexuality and fertility in men with hypospadias; improved outcome. Andrology. 2017;5:286–93.
Örtqvist L, Fossum M, Andersson M, Nordenström A, Frisén L, Holmdahl G, et al. Long-term followup of men born with hypospadias: urological and cosmetic results. J Urol. 2015;193:975–81.
Liu G, Yuan J, Feng J, Geng J, Zhang W, Zhou X, et al. Factors affecting the long-term results of hypospadias repairs. J Pediatr Surg. 2006;41:554–9.
Hoag CC, Gotto GT, Morrison KB, Coleman GU, Macneily AE. Long-term functional outcome and satisfaction of patients with hypospadias repaired in childhood. Can Urol Assoc J. 2008;2:23–31.
Stein DM, Gonzalez CM, Barbagli G, Cimino S, Madonia M, Sansalone S. Erectile function in men with failed hypospadias repair. Arch Esp Urol. 2014;67:152–6.
Ciancio F, Lo Russo G, Innocenti A, Portincasa A, Parisi D, Mondaini N. Penile length is a very important factor for cosmesis, function and psychosexual development in patients affected by hypospadias: results from a long-term longitudinal cohort study. Int J Immunopathol Pharm. 2015;28:421–5.
Andersson M, Sjöström S, Wängqvist M, Örtqvist L, Nordenskjöld A, Holmdahl G. Psychosocial and sexual outcomes in adolescents following surgery for proximal hypospadias in childhood. J Urol. 2018;200:1362–70.
Adams J, Bracka A. Reconstructive surgery for hypospadias: a systematic review of long-term patient satisfaction with cosmetic outcomes. Indian J Urol. 2016;32:93–102.
Thiry S, Saussez T, Dormeus S, Tombal B, Wese FX, Feyaerts A. Long-term functional, cosmetic and sexual outcomes of hypospadias correction performed in childhood. Urol Int. 2015;95:137–41.
Mureau MAM, Slijper FME, Slob AK, Verhulst FC. Genital perception of children, adolescents, and adults operated on for hypospadias: a comparative study. J Sex Res. 1995;32:289–98.
Mureau MA, Slijper FM, van der Meulen JC, Verhulst FC, Slob AK. Psychosexual adjustment of men who underwent hypospadias repair: a norm-related study. J Urol. 1995;154:1351–5.
Jones BC, O’Brien M, Chase J, Southwell BR, Hutson JM. Early hypospadias surgery may lead to a better long-term psychosexual outcome. J Urol. 2009;182:1744–9.
Dodds PR, Batter SJ, Shield DE, Serels SR, Garafalo FA, Maloney PK. Adaptation of adults to uncorrected hypospadias. Urology. 2008;71:682–5.
Schlomer B, Breyer B, Copp H, Baskin L, DiSandro M. Do adult men with untreated hypospadias have adverse outcomes? A pilot study using a social media advertised survey. J Pediatr Urol. 2014;10:672–9.
Basile Fasolo C, Mirone V, Gentile V, Parazzini F, Ricci E, on behalf of the Andrology Prevention Week c. Premature ejaculation: prevalence and associated conditions in a sample of 12,558 men attending the andrology prevention week 2001—A Study of the Italian Society of Andrology (SIA). J Sex Med. 2005;2:376–82.
Aulagne MB, Harper L, de Napoli-Cocci S, Bondonny JM, Dobremez E. Long-term outcome of severe hypospadias. J Pediatr Urol. 2010;6:469–72.
Arendt LH, Lindhard MS, Kjersgaard C, Henriksen TB, Olsen J, Ramlau-Hansen CH. Parental subfertility and hypospadias and cryptorchidism in boys: results from two Danish birth cohorts. Fertil Steril. 2018;110:826–32.
Fritz G, Czeizel AE. Abnormal sperm morphology and function in the fathers of hypospadiacs. J Reprod Fertil. 1996;106:63–6.
Asklund C, Jørgensen N, Skakkebaek NE, Jensen TK. Increased frequency of reproductive health problems among fathers of boys with hypospadias. Hum Reprod. 2007;22:2639–46.
Moriya K, Mitsui T, Tanaka H, Nakamura M, Nonomura K. Long-term outcome of pituitary-gonadal axis and gonadal growth in patients with hypospadias at puberty. J Urol. 2010;184:1610–4.
Moriya K, Nakamura M, Kon M, Nishimura Y, Kanno Y, Kitta T, et al. Risk factors affecting post-pubertal high serum follicle-stimulating hormone in patients with hypospadias. World J Urol. 2019;37:2795–9.
Asklund C, Jensen TK, Main KM, Sobotka T, Skakkebaek NE, Jørgensen N. Semen quality, reproductive hormones and fertility of men operated for hypospadias. Int J Androl. 2010;33:80–7.
Skakkebaek NE, Rajpert-De Meyts E, Main KM. Testicular dysgenesis syndrome: an increasingly common developmental disorder with environmental aspects. Hum Reprod. 2001;16:972–8.
Sharpe RM. Pathways of endocrine disruption during male sexual differentiation and masculinization. Best Pr Res Clin Endocrinol Metab. 2006;20:91–110.
Fredell L, Kockum I, Hansson E, Holmner S, Lundquist L, Läckgren G, et al. Heredity of hypospadias and the significance of low birth weight. J Urol. 2002;167:1423–7.
Mieusset R, Soulié M. Hypospadias: psychosocial, sexual, and reproductive consequences in adult life. J Androl. 2005;26:163–8.
Schneuer FJ, Milne E, Jamieson SE, Pereira G, Hansen M, Barker A, et al. Association between male genital anomalies and adult male reproductive disorders: a population-based data linkage study spanning more than 40 years. Lancet Child Adolesc Health. 2018;2:736–43.
Skarin Nordenvall A, Chen Q, Norrby C, Lundholm C, Frisén L, Nordenström A, et al. Fertility in adult men born with hypospadias: a nationwide register-based cohort study on birthrates, the use of assisted reproductive technologies and infertility. Andrology. 2020;8:372–80.
Berg R, Svensson J, Aström G. Social and sexual adjustment of men operated for hypospadias during childhood: a controlled study. J Urol. 1981;125:313–7.
Cortes D. Cryptorchidism-aspects of pathogenesis, histology and treatment. Scand J Urol Nephrol Suppl. 1998;196:1–54.
Spinoit A-F, Tack L, Mahmoud A, Tilleman K, Springer A, Riedl S, et al. Endocrine and reproductive outcome of men born with various degrees of hypospadias. Eur Urol Open Sci. 2020;19:e2089.
Aksglaede L, Olesen IA, Carlsen E, Petersen JH, Juul A, Jørgensen N. Serum concentration of anti-Müllerian hormone is not associated with semen quality. Andrology. 2018;6:286–92.
Rohayem J, Luberto A, Nieschlag E, Zitzmann M, Kliesch S. Delayed treatment of undescended testes may promote hypogonadism and infertility. Endocrine. 2017;55:914–24.
Rey RA, Codner E, Iñíguez G, Bedecarrás P, Trigo R, Okuma C, et al. Low risk of impaired testicular Sertoli and Leydig cell functions in boys with isolated hypospadias. J Clin Endocrinol Metab. 2005;90:6035–40.
Kumar MV, Harris DL. A long term review of hypospadias repaired by split preputial flep technique (Harris). Br J Plast Surg 1994;47:236–40.
Marrocco G, Vallasciani S, Fiocca G, Calisti A. Hypospadias surgery: a 10-year review. Pediatr Surg Int. 2004;200–3.
Lam PN, Greenfield SP, Williot P. 2-stage repair in infancy for severe hypospadias with chordee: long-term results after puberty. J Urol. 2005;174:1567–72.
Nelson CP, Bloom DA, Kinast R, Wei JT, Park JM. Long-term patient reported outcome and satisfaction after oral mucosa graft urethroplasty for hypospadias. J Urol. 2005.
Örtqvist L, Fossum M, Andersson M, Nordenström A, Frisen L, Holmdahl G, Nordenskjöld A. Sexuality and fertility in men with hypospadias; improved outcome. Andrology. 2017;5:286–93.
Majstorovic M, Bizic M, Nikolic D, Stojanovic B, Bencic M, Joksic I, Djordjevic M. Psychosexual functioning outcome testing after hypospadias repair. Healthcare (Basel). 2020;8:32.
Acknowledgements
The authors acknowledge the participants for their cooperation.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. SH is a PhD fellow supported by Novo Nordisk Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gul, M., Hildorf, S. & Silay, M.S. Sexual functions and fertility outcomes after hypospadias repair. Int J Impot Res 33, 149–163 (2021). https://doi.org/10.1038/s41443-020-00377-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-020-00377-5
This article is cited by
-
Intracavernosal pressure of the erect penis in children with hypospadias
International Journal of Impotence Research (2024)
-
Clinical characteristics, socioeconomic factors and COVID-19 were associated with delayed surgery in children with hypospadias: a retrospective study of 4439 cases in a single center
European Journal of Medical Research (2022)
-
Out of the dark, into the light: sexuality and fertility in pediatric urological conditions
International Journal of Impotence Research (2021)
-
Why look back in anger? Masculinizing surgery in patients with DSD
Nature Reviews Urology (2021)