Abstract
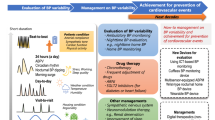
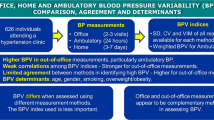
Blood pressure variability (BPV) is an important indicator in risk stratification for hypertension. Among the daily BPVs assessed using a 24-h ambulatory blood pressure (BP) monitor nocturnal systolic BPV has been suggested to predict cardiovascular risks. We hypothesized that very short-term BPV at rest would correlate with nocturnal BPV because of the shared autonomic BP regulatory system under no daily exertion. Thirty untreated normotensive and hypertensive adults underwent 30-min continuous beat-by-beat BP recordings in the supine position, followed by 24-h ambulatory blood pressure monitoring (ABPM). The relationship between very short-term BPV (standard deviation (SD), coefficient of variation (CV)) and daytime and nocturnal BPV (SD, CV, average real variability (ARV), and standardized ARV (CV-ARV)) was assessed with Pearson’s correlation coefficients. Very short-term BPV correlated significantly with nocturnal BPV (ARV, r = 0.604, p < 0.001) but not with daytime BPV. These trends were more pronounced with the increasing data length of continuous beat-by-beat BP recording. Using a data segment from the last 10 min of a 30-min continuous beat-by-beat BP recording resulted in a stronger correlation between very short-term BPV and nocturnal BPV than using earlier segments. The findings of this study suggest that very short-term BPV in the supine position at rest may predict nocturnal BPV. Since the burden of ABPM for patients has hindered clinical dissemination, very short-term BPV has the potential to develop a novel index of BPV.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Fujiyoshi A, Ohkubo T, Miura K, Murakami Y, Nagasawa SY, Okamura T, et al. Blood pressure categories and long-term risk of cardiovascular disease according to age group in Japanese men and women. Hypertens Res. 2012;35:947–53.
Bundy JD, Li C, Stuchlik P, Bu X, Kelly TN, Mills KT, et al. Systolic blood pressure reduction and risk of cardiovascular disease and mortality: a systematic review and network meta-analysis. JAMA Cardiol. 2017;2:775–81.
Madden JM, O’Flynn AM, Fitzgerald AP, Kearney PM. Correlation between short-term blood pressure variability and left-ventricular mass index: a meta-analysis. Hypertens Res. 2016;39:171–7.
Mena LJ, Felix VG, Melgarejo JD, Maestre GE. 24-Hour blood pressure variability assessed by average real variability: a systematic review and meta-analysis. J Am Heart Assoc. 2017;6:e006895. https://doi.org/10.1161/JAHA.117.006895.
Stevens SL, Wood S, Koshiaris C, Law K, Glasziou P, Stevens RJ, et al. Blood pressure variability and cardiovascular disease: systematic review and meta-analysis. BMJ. 2016;354:i4098. https://doi.org/10.1136/bmj.i4098.
Filomena J, Riba-Llena I, Vinyoles E, Tovar JL, Mundet X, Castañé X, et al. Short-term blood pressure variability relates to the presence of subclinical brain small vessel disease in primary hypertension. Hypertension. 2015;66:634–40.
Parati G, Ochoa JE, Lombardi C, Bilo G. Assessment and management of blood-pressure variability. Nat Rev Cardiol. 2013;10:143–55.
Chadachan VM, Ye MT, Tay JC, Subramaniam K, Setia S. Understanding short-term blood-pressure-variability phenotypes: from concept to clinical practice. Int J Gen Med. 2018;11:241–54.
Pringle E, Phillips C, Thijs L, Davidson C, Staessen JA, de Leeuw PW, et al. Systolic blood pressure variability as a risk factor for stroke and cardiovascular mortality in the elderly hypertensive population. J Hypertens. 2003;21:2251–7.
Palatini P, Reboldi G, Beilin LJ, Casiglia E, Eguchi K, Imai Y, et al. Added predictive value of night-time blood pressure variability for cardiovascular events and mortality: the Ambulatory Blood Pressure-International Study. Hypertension. 2014;64:487–93.
Viera AJ, Lingley K, Hinderliter AL. Tolerability of the Oscar 2 ambulatory blood pressure monitor among research participants: a cross-sectional repeated measures study. BMC Med Res Methodol. 2011;11:59. https://doi.org/10.1186/1471-2288-11-59.
van der Steen MS, Lenders JW, Graafsma SJ, den Arend J, Thien T. Reproducibility of ambulatory blood pressure monitoring in daily practice. J Hum Hypertens. 1999;13:303–8.
Hall JE, Guyton AC. Role of the kidneys in long-term control of arterial pressure and in hypertension. In Hall JE, Guyton AC, Guyton and Hall textbook of medical physiology, 11th edn. Philadelphia, PA: Saunders Elsevier 2011, 216–31.
Kario K. Evidence and perspectives on the 24-hour management of hypertension: hemodynamic biomarker-initiated ‘anticipation medicine’ for zero cardiovascular event. Prog Cardiovasc Dis. 2016;59:262–81.
Kokubo A, Kuwabara M, Nakajima H, Tomitani N, Yamashita S, Shiga T, et al. Automatic detection algorithm for establishing standard to identify “surge blood pressure”. Med Biol Eng Comput. 2020;58:1393–404.
Mano J, Saku K, Kinoshita H, Mannoji H, Kanaya S, Sunagawa K. Aging steepens the slope of power spectrum density of 30-minute continuous blood pressure recording in healthy human subjects. PLoS One. 2021;16:e0248428. https://doi.org/10.1371/journal.pone.0248428.
Kinoshita H, Mannoji H, Saku K, Mano J, Miyamoto T, Todaka K, et al. Power spectral analysis of short-term blood pressure recordings for assessing daily variations of blood pressure in human. Annu Int Conf IEEE Eng Med Biol Soc. 2018;2018:1–4. https://doi.org/10.1109/EMBC.2018.8513040.
JCS Joint Working Group. Guidelines for the clinical use of 24 h ambulatory blood pressure monitoring (ABPM) (JCS 2010)—digest version. Circ J. 2012;76:508–19.
Mena L, Pintos S, Queipo NV, Aizpúrua JA, Maestre G, Sulbarán T. A reliable index for the prognostic significance of blood pressure variability. J Hypertens. 2005;23:505–11.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;2018:3021–104.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Fan Y, Hou C, Peng L, Gao X, Xu Y. Twenty-four-hour ambulatory blood pressure variability associated with cerebral small vessel disease mri burden and its progression in inpatients with cerebrovascular disease. Front Neurol. 2020;11:513067. https://doi.org/10.3389/fneur.2020.513067.
Peixoto AJ, White WB. Circadian blood pressure: clinical implications based on the pathophysiology of its variability. Kidney Int. 2007;71:855–60.
Smolensky MH, Hermida RC, Portaluppi F. Circadian mechanisms of 24-hour blood pressure regulation and patterning. Sleep Med Rev. 2017;33:4–16.
Sakamoto K, Hosokawa K, Saku K, Sakamoto T, Tobushi T, Oga Y, et al. Baroreflex failure increases the risk of pulmonary edema in conscious rats with normal left ventricular function. Am J Physiol Heart Circ Physiol. 2016;310:H199–205.
Dworkin BR, Tang X, Snyder AJ, Dworkin S. Carotid and aortic baroreflexes of the rat: II. Open-loop frequency response and the blood pressure spectrum. Am J Physiol Regul Integr Comp Physiol. 2000;279:R1922–33.
Kawada T, Shimizu S, Kamiya A, Sata Y, Uemura K, Sugimachi M. Dynamic characteristics of baroreflex neural and peripheral arcs are preserved in spontaneously hypertensive rats. Am J Physiol Regul Integr Comp Physiol. 2011;300:R155–65.
Kamiya A, Kawada T, Sugimachi M. Systems physiology of the baroreflex during orthostatic stress: from animals to humans. Front Physiol. 2014;5:256. https://doi.org/10.3389/fphys.2014.00256.
Mannoji H, Saku K, Nishikawa T, Tohyama T, Kamada K, Abe K, et al. Estimation of the baroreflex total loop gain by the power spectral analysis of continuous arterial pressure recordings. Am J Physiol Heart Circ Physiol. 2019;316:H828–H839.
Ruiz J, Monbaron D, Parati G, Perret S, Haesler E, Danzeisen C, et al. Diabetic neuropathy is a more important determinant of baroreflex sensitivity than carotid elasticity in type 2 diabetes. Hypertension. 2005;46:162–7.
Wensel R, Jilek C, Dörr M, Francis DP, Stadler H, Lange T, et al. Impaired cardiac autonomic control relates to disease severity in pulmonary hypertension. Eur Respir J. 2009;34:895–901.
Casali KR, Schaan BD, Montano N, Massierer D, M F Neto F, Teló GH, et al. Correlation between very short and short-term blood pressure variability in diabetic-hypertensive and healthy subjects. Arq Bras Cardiol. 2018;110:157–65.
Manios E, Michas F, Stamatelopoulos K, Barlas G, Koroboki E, Tsouma I, et al. Short-term beat-to-beat but not ambulatory blood pressure variability is correlated to carotid intima-media thickness. Blood Press Monit. 2014;19:288–93.
Wei FF, Li Y, Zhang L, Xu TY, Ding FH, Wang JG, et al. Beat-to-beat, reading-to-reading, and day-to-day blood pressure variability in relation to organ damage in untreated Chinese. Hypertension. 2014;63:790–6.
Berry M, Lairez O, Fourcade J, Roncalli J, Carrié D, Pathak A, et al. Prognostic value of systolic short-term blood pressure variability in systolic heart failure. Clin Hypertens. 2016;22:16. https://doi.org/10.1186/s40885-016-0051-z.
Acknowledgements
This work was supported by a Medical-Engineering Collaboration project and research and development of supportive device technology for medicine using ICT from the Japan Agency for Medical Research and Development (18he1102003h0004, 20he1302033j0002), the Japan Foundation for Applied Enzymology. (VBIC: Vascular Biology of Innovation), the Intramural Research Fund for Cardiovascular Diseases of National Cerebral and Cardiovascular Center (31-6-4, 21-2-9) and a research grant from Omron Healthcare Co., Ltd.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Hiroyuki Kinoshita and Jumpei Mano are employees of Omron Healthcare Co., Ltd. Kenji Sunagawa worked at the Department of Therapeutic Regulation of Cardiovascular Homeostasis, Center for Disruptive Cardiovascular Medicine, Kyushu University, which was endowed by Omron Healthcare Co., Ltd., and works at the Circulatory System Research Foundation, which is endowed by Omron Healthcare Co., Ltd. Kenji Sunagawa also serves as a consultant of Omron Healthcare Co., Ltd. Keita Saku worked at the Department of Cardiovascular Medicine, Graduate School of Medical Sciences, Kyushu University, which was endowed by Omron Healthcare Co., Ltd., and receives a research grant from Omron Healthcare Co., Ltd. Hiroshi Mannoji and Shigehiko Kanaya declare no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Kinoshita, H., Saku, K., Mano, J. et al. Very short-term beat-by-beat blood pressure variability in the supine position at rest correlates well with the nocturnal blood pressure variability assessed by ambulatory blood pressure monitoring. Hypertens Res 45, 1008–1017 (2022). https://doi.org/10.1038/s41440-022-00911-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-00911-6
Keywords
This article is cited by
-
More moderate-intensity physical activity and less prolonged sedentary time are associated with better very short-term systolic blood pressure variability in healthy adults
Journal of Human Hypertension (2023)
-
Novel blood pressure monitoring methods: perspectives for achieving “perfect 24-h blood pressure management”
Hypertension Research (2023)
-
Short- to long-term blood pressure variability: Current evidence and new evaluations
Hypertension Research (2023)