Abstract
As an effective medicine for jaundice in traditional Chinese medicine, Cucumis melo L. has been widely used in China. However, its effect on vascular function is still unclear. In this study, we extracted the compounds of Cucumis melo L., and the major ingredients were identified as cucurbitacins (CuEC, cucurbitacins extracted from Cucumis melo L.), especially cucurbitacin B. We replicated the toxicity in mice by intraperitoneal injection of a high dose of CuEC (2 mg/kg) and demonstrated that the cause of death was CuEC-induced impairment of the endothelial barrier and, thus, increased vascular permeability via decreasing VE-cadherin conjunction. The administration of low doses of CuEC (1 mg/kg) led to a decline in systolic blood pressure (SBP) without causing toxicity in mice. More importantly, CuEC dramatically suppressed angiotensin II (Ang II)-induced SBP increase. Further studies demonstrated that CuEC facilitated acetylcholine-mediated vasodilation in mesenteric arteries of mice. In vitro studies showed that CuEC induced vasodilation in a dose-dependent manner in mesenteric arteries of both mice and rats. Pretreatment with CuEC inhibited phenylephrine-mediated vasoconstriction. In summary, a moderate dose of CuEC reduced SBP by improving blood vessel tension. Therefore, our study provides new experimental evidence for developing new antihypertensive drugs.
Similar content being viewed by others
Introduction
Cardiovascular diseases remain the primary killer in Western countries [1]. Cardiovascular diseases with high mortality and disability cause great harm to human life and health, of which hypertension is one of the most common cardiovascular diseases and constitutes the world’s largest burden of disease [2]. Many factors can cause hypertension, such as gene mutations, drug effects, vascular endothelial dysfunction, high-salt diet, and vascular aging [3,4,5]. At present, the main antihypertensive drugs are diuretics, beta-receptor blockers, calcium channel blockers and angiotensin-converting enzyme inhibitors (ACEI) [6,7,8]. The process of medication is often accompanied by side effects; long-term medication causes varying degrees of damage to the body. Therefore, it is very necessary to discover new antihypertensive drugs [9,10,11,12].
Many herbs in traditional Chinese medicine are beneficial for the cardiovascular system. However, many of these compounds have been poorly studied in a direct manner with respect to vascular tone, especially the effective components in herbs. Dry muskmelon pedicel, with the scientific name Cucumis melo L., is an effective herb, and the main application is jaundice treatment. Cucumis melo L. also has an emetic effect and can be used to treat jaundiced infectious hepatitis, diabetes, central hiccup, and psycho-neurological diseases, as well as to improve immunity and exert anti-inflammation functions [13, 14]. Cucumis melo L. contains many cucurbitacins, which are highly oxidized tetracyclic triterpenoids containing 12 classes from A to T with over 200 derivatives that possess strong biological activity [15, 16]. The main compounds of cucurbitacins from Cucumis melo L. are cucurbitacin B (CuB), cucurbitacin D (CuD), cucurbitacin E (CuE), and 2-O-β-D-glucopyranosyl cucurbitacin B, and also contains some sterols, saponins and amino acids [17, 18]. A previous study revealed that CuB [19,20,21,22,23,24,25,26], CuD [27, 28] and CuE [29,30,31] exert anti-tumor effects in many types of cancer, including hepatoma, leukemia, breast cancer, pancreatic cancer, non-small cell lung cancer, gastric carcinoma, cervical cancer, and so on. The mechanisms of the anti-tumor effect includes inhibition of migration and invasion, anti-proliferation, increased apoptosis, promotion of cell cycle arrest and inhibition of tumor angiogenesis. The extracts of Cucumis melo L. improved insulin resistance in ob/ob mice, and CuB also causes hypoglycemic effects by inducing glucagon-like peptide-1 [32, 33]. In addition, CuB and CuE attenuate hepatic fibrosis [34, 35]. There have been few studies of cucurbitacins in cardiovascular research. Recently, CuB was found to protect against pressure overload-induced cardiac hypertrophy and fibrosis by increasing the autophagy level in cardiomyocytes [36]. However, the effect of cucurbitacins on blood pressure regulation and the cardiovascular system are largely unknown.
Vascular tone, especially that of the small arteries and arterioles, is important in blood pressure regulation. The mesenteric artery is widely used in vascular tone studies. In the present study, we extracted cucurbitacins (CuEC, cucurbitacins extracted from Cucumis melo L.), identified the main compound and used it to validate the hypotensive effect on animals and mesenteric arteries. We found that CuEC exerted a hypotensive effect by inducing vasodilation.
Materials and methods
Extraction and isolation
The dried pedicle of Cucumis melo L. was powdered and the powder was soaked in 6 times to 70% ethanol for 30 min. Reflux extraction was performed three times at 80 °C for 1 h each time. After combined extraction solution, filtering and drying, the extract was obtained. The dried extraction was diluted with 100 ml water to make a suspension and was separated by macroporous resin of D101. Two hundred milliliters of distilled water (2BV), 400 ml of 30% ethanol (4BV), 400 ml of 50% ethanol (4BV), and 600 ml of 70% ethanol (6BV) were used to elute the samples. The fraction eluted with 70% ethanol was collected, concentrated, and dried to a constant weight. Next, the fraction was subjected to a silica gel (300–400 mesh), and the eluted solvent was petroleum ether–ethyl acetate (10:1-1:1) and chloroform–methanol (5:1). The target compounds were eluted in the chloroform–methanol fraction.
UPLC-Q/TOF-MS analysis
UPLC analysis was carried out on an ACQUITYTM UPLC I-Class system comprising a quaternary pump, a diode-array detector (DAD), an autosampler, and a column compartment. Samples were separated on an Acquity UPLC BEH C18 Column (2.1 mm × 100 mm, 1.7 m) at a temperature of 40 °C. The mobile phases consisted of eluent A (0.1% formic acid in water, v/v) and eluent B (0.1% formic acid in acetonitrile, v/v) using a gradient program as follows: 2% B from 0 to 1 min, 2–70% B from 1 to 18 min, 70–100% B from 18 to 20 min. After holding 100% B for the next 2 min, the column was returned to its starting condition. The flow rate was kept at 0.4 ml/min, and the injection volume was 2 μl for all the samples.
The UPLC system was coupled to quadrupole time-of-flight tandem mass spectrometry (SYNAPTTM G2 HDMS, Waters, Manchester, UK) equipped with electrospray ionization (ESI). The operating parameters were set as follows: capillary voltage of 3 kV (ESI+); sample cone voltage of 35 V; extraction cone voltage of 4 V, source temperature of 100 °C, desolvation temperature 400 °C, cone gas flow of 50 L/h and desolvation gas flow of 800 L/h. In MSE mode, the trap collision energy was 4 eV for low energy function and 20–50 eV for high energy function. Argon was used as the collision gas for CID in MSE mode. The mass spectrometer was calibrated over a range of 50–1500 Da using a solution of sodium formate. Argon was used as the collision gas. All data were processed with Masslynx V4.1 software (Waters, Manchester, UK).
UPLC-MS/MS analysis
The system consisted of two pumps (LC-30ADvp, Shimadzu, Toyoto, Japan), an on-line degasser (DGU-12A, Shimadzu), and a triple quadrupole mass spectrometer equipped with an ESI source (QTRAP 5500, AB SCIEX, MA, USA). The mass spectrometer was controlled by ANALYST software (AB SCIEX). A C18 reversed-phase column (Shim-pack GIS C18®, 2 μm particle size, 10 cm × 2.1 mm, Shimadzu, Toyoto, Japan) was used for separation. The column temperature was 40 °C, and a MeOH/water mixture (71/29, v/v) with 0.1% formic acid was used as the mobile phase at a flow rate of 0.10 ml/min. The sample injection volume was 5 μl. The MS detector was operated in positive ion mode with the following settings: IonSpray voltage (IS) 5.5 KV, Curtain Gas (CUR) 20.0, Ion Source Gas 1 (GS1) 15 psi, Ion Source Gas 2 (GS2) 0 psi, Declustering Potential (DP) 68 volts, and Collision Energy (CE) 34 volts. Quantitative analysis was carried out in multiple reaction monitoring (MRM) on transitions 581.1/521.0 m/z for CuEC.
Animals and materials
Adult (8–10 weeks) male C57BL/6 mice and rats (200 g) maintained at the Animal Center of Dalian Medical University were used in all studies. Animals were kept in a temperature-controlled (23 °C) room with a 12-h light-dark cycle and given a fresh diet and sterile water every 2 days. The study procedures and the use of the animals were reviewed and approved by the Animal Care and Use Review Committee of Dalian Medical University. The study conformed to the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH publication no. 85-23, revised 1996). Phenylephrine, acetylcholine and MTT were purchased from Sigma-Aldrich (St. Louis, MO, USA). The VE-cadherin antibody was obtained from Abcam, and the FITC-tag secondary antibody was obtained from ThermoFisher Scientific.
Evans blue assay
The mice were randomly divided into two groups and pretreated with CuEC (1 mg/kg or 2 mg/kg) or vehicle for 30 min by acute intraperitoneal injection. Then, mice were intravenously injected with Evans blue (200 μl, 0.5% in PBS) in the mouse lateral tail vein. Half an hour later, mice were killed using CO2 and perfused with PBS in the right ventricle to remove the intravascular Evans blue. Pictures of organs (pancreas, liver, kidney, lung and heart, testes, and epididymal fat) were taken to show differences in Evans blue extravasation. The organs were weighed, and Evans blue in the organs was extracted in 1 ml formamide at 55 °C for 24 h. The Evans blue content was quantified with OD 620 nm and the tissue weight.
En face immunostaining
The mice were euthanized with CO2 by inhalation overdose. The abdomen and thorax were exposed, and the circulatory system was perfused in the right ventricle with PBS containing heparin (40 U/ml). Then, the mice were perfused with the fixation solution containing 4% paraformaldehyde in PBS for 5 min. The aorta was harvested, and the endothelium was exposed. The aorta was treated with permeabilizing solution (0.1% Triton X-100 in PBS) for 10 min with slight rocking at room temperature and washed with PBS briefly. The samples were blocked in blocking buffer (10% BSA in TBST) for half an hour at room temperature and then incubated with the VE-cadherin primary antibodies diluted in TBST with 10% BSA (1:500) overnight with rocking at 4 °C. The blood vessels were washed three times with TBST for 10 min with slight rocking at room temperature. The samples were incubated with fluorescently labeled secondary antibodies diluted in TBST with 10% BSA for 1 h with rocking at room temperature. Nuclear staining with DAPI was simultaneously performed at this stage by adding 1/1000 of a DAPI stock solution containing 5 mg/ml DAPI in H2O. The samples were washed three times with TBST for 10 min with rocking at room temperature and rinsed with PBS. The aorta was placed with anti-fade reagent with the endothelium facing the cover glass, and the en face blood vessel sample was flattened. The coverslip was completely sealed using nail polish. Microscopy was performed with a Leica SP8 laser scanning confocal microscope.
Blood pressure measurement
Male C57BL/6 mice aged 8–10 weeks and with 23–25 g body weight were used. Following a 1-week training period, blood pressure was measured in conscious mice using the tail-cuff apparatus (Softron, BP-2010A). Basal SBP was measured for 3 days. After the basal SBP measurements, the mice were treated with CuEC every day (1 mg/kg/day) with intraperitoneal injection for 3 days. The SBP was monitored every day. After the blood pressure measurement, mice were killed, and mesenteric artery vascular reactivity was measured using the following methods.
Ang II-infused mouse model
Adult (8–10 weeks) male C57BL/6 mice were trained for SBP measurement for 1 week and then treated with Ang II at 1000 ng per kg body weight per min (1000 ng/kg/min) using subcutaneous osmotic minipumps (Alzet Corp). The mice were randomly divided into two groups, which were treated with CuEC (1 mg/kg/48 h) and vehicle. After surgery, SBP was recorded on different days via the tail-cuff method.
Mesenteric arterial vascular reactivity
Mesenteric arteries were dissected immediately from mice or rats after being anesthetized with CO2 by inhalation overdose and cut into rings 2 mm long in ice-cold Krebs bicarbonate buffer. Each segment was suspended between two tungsten wires in chambers of a Multi Myograph System (610 M, Danish Myo Technology A/S, Aarhus N, Denmark) for the measurement of isometric force. Each chamber was filled with 5 ml of Krebs bicarbonate buffer and maintained at 37 °C. During the entire experiment, the buffer was continuously oxygenated with 95% O2 plus 5% CO2 gas. To determine the vasodilatory effect, phenylephrine (Phe, 10 μM) was used to constrict vessel rings in advance. After sustained contraction was obtained, the concentration-dependent responses of acetylcholine (Ach) or CuEC were examined. To examine the effect of CuEC on the contractile response of arteries to phenylephrine, the arteries were incubated with CuEC (2 and 10 μg/ml) for 30 min, and the incremental concentration of phenylephrine was performed every 2 min [37].
Cell culture and MTT assay
HUVECs and VSMCs in the exponential growth phase were implanted in 96-well plates with 1 × 104 cells per well and cultured for 12 h in 37 °C and 5% CO2 incubators. Then, different concentrations of CuEC (0.035–10 μg/ml) were added, and the cells were cultured for 24 h in a 37 °C and 5% CO2 incubator. Then, 10 μl MTT (5 mg/ml) was added to each well of the 96-well plate and incubated for 4 h at 37 °C in a 5% CO2 incubator. After incubation, the supernatant was discharged, 150 μl dimethyl sulfoxide (DMSO) was added, and the mixture was shaken for 15 min. Optical density (OD) was measured at 490 nm.
Statistical analysis
Quantitative data are expressed as the mean ± SEM. Student’s t test and ANOVA were used to analyze the statistical significance for the differences between two or among more groups, respectively. The dose response curves were analyzed using two-way ANOVA followed by Bonferroni posttests. P < 0.05 was considered significant. Nonquantitative results are representative of at least three independent experiments.
Results
Isolation and identification of active compounds from Cucumis melo L.
Using chloroform extraction and chromatography, we isolated active compounds from Cucumis melo L. The compounds appeared as white powders, which were soluble in chloroform and DMSO but insoluble in water (Fig. 1a). We analyzed the components using UPLC-Q/TOF-MS preliminarily. Among the components, the most abundant compound was cucurbitacin B (CuB) (~56.9%). The other compounds were cucurbitacin E (CuE) (~12.2%) and cucurbitacin D (CuD) (~1.08%) (Fig. 1b). Furthermore, the exact content of CuB in CuEC was 62.6% measured by UPLC-MS/MS using a CuB standard, which was similar to the UPLC-Q/TOF-MS measurement (Table 1). This result demonstrated that CuB was the predominant compound in CuEC.
Isolation and identification of CuEC from Cucumis melo L. a Picture of muskmelon, Cucumis melo L. (dry muskmelon pedicel) and extracted compound powder. The fresh muskmelon pedicel was air-dried and extracted using chloroform. b Identification of the extract. The extract was identified as cucurbitacins by UPLC-Q/TOF-MS
One milligram/kg of CuEC treatment was safe for animals
As previously reported, large doses of CuEC or Cucumis melo L. can cause poisoning or even death in animals [15, 16]. A low dose (1 mg/kg) and high dose (2 mg/kg) were administered by i.p. injection to C57BL/6 male mice. The animals who received 2 mg/kg CuEC began to die three hours later, and ~94% of the mice died within 12 h. However, the low-dose-treated animals exhibited zero deaths, which was the same as the vehicle group (Fig. 2a). To verify whether CuEC caused vascular cell injury, we further performed MTT on endothelial cells (HUVECs) and vascular smooth muscle cells (VSMCs). The results showed that CuEC had no obvious cytotoxicity in a wide range of doses of 0.035–10 μg/ml (Fig. 2b, c).
A high dose of CuEC caused toxic death in mice by increasing vascular permeability. a Survival curve of CuEC-treated mice. Intraperitoneal injection of control (DMSO) or CuEC (1 mg/kg or 2 mg/kg) followed by monitoring of the mice for 24 h. n = 10–16. b Cytotoxicity of CuEC measured by an MTT assay. Primary VSMCs were used. n = 3. c Cytotoxicity of CuEC checked by an MTT assay. Primary HUVECs were used. n = 3. d Representative picture of organs after Evans blue i.v. injection. e Quantitation of Evans blue dye in tissues. n = 4. *p < 0.05, **p < 0.01 vs. control. f Representative confocal picture of en face immunostaining of VE-cadherin in the mouse aorta
A high dose of CuEC increased vascular permeability
To confirm the cause of CuEC-induced animal death, we dissected the mice and found massive pleural effusion and cerebral edema. Thus, we speculated that CuEC could increase vascular permeability. We found that pretreatment of CuEC (2 mg/kg) for 30 min increased the leakage of intravenously administered Evans blue dye into the tissues, especially the pancreas (Fig. 2d, e). Furthermore, we checked the aortic endothelium integrity by en face immunostaining of VE-cadherin and found that the CuEC-treated mice displayed disorganization of the adherent junction (Fig. 2f). Thus, our study demonstrated that CuEC or Cucumis melo L. caused poisoning effects that were attributed to leakage of blood content because of increased vascular permeability.
A low dose of CuEC decreased the blood pressure in mice
As mentioned above, low doses of CuEC did not cause death within 24 h. We wondered whether long-term treatment with CuEC would lead to death from poisoning in mice. To our surprise, 3 days of i.p. administration of low-dose CuEC did not lead to pleural effusion, edema or other phenomena in mice, with no difference in the leakage of intravenously administered Evans blue dye into the tissues (Fig. 3a, b). However, the blood pressure was significantly reduced in those mice by the tail sleeve test (Fig. 3c, d).
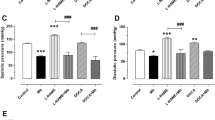
CuEC (1 m/kg) decreased SBP in mice. a Representative picture of the pancreas, liver and kidney after Evans blue i.v. injection. b Quantitation of Evans blue dye in tissues. n = 6. c Experimental schematic of blood pressure measurements in CuEC-treated mice. After 1 week of the blood pressure measurement training period, SBP was recorded every day at a fixed time for 3 days. When the third SBP measurement was completed, the mice were immediately given CuEC (1 mg/kg) by intraperitoneal injection. The CuEC was administered whenever the SBP measurement was finished, for a total of three times. On the fourth day, the SBP was measured, and the mice were used to excise the mesenteric artery directly, without injection of CuEC. d SBP was measured by the tail-cuff method. n = 3–4, **p < 0.01 vs. control. e SBP was measured by the tail-cuff method in a CuEC-treated Ang II-infused mouse model. n = 4-5, ***p < 0.001 vs. control
In addition, we used Ang II osmotic minipumps (1000 ng/kg/min) planted in mice subcutaneously to establish the hypertensive mouse model. We found that the control group displayed increased SBP, which reached ~180 mmHg after 4 weeks, while the CuEC (1 mg/kg/48 h)-treated group exhibited a significantly ameliorated SBP increase in the course of Ang II infusion (~140 mmHg after 4 weeks) compared to the control group (Fig. 3e). These results suggest that low doses of CuEC can reduce blood pressure in normal mouse and hypertensive mouse models and that this effect is not achieved by reducing the blood volume.
CuEC ameliorated acetylcholine-mediated vasodilation
The mesenteric arteries of the mice that received 3 days of low-dose CuEC administration were used to analyze vascular tone. We found that the CuEC pretreatment group showed a significantly enhanced vasodilatory effect of acetylcholine (Fig. 4a).
CuEC accelerated acetylcholine-induced mesenteric arterial vasodilatation and directly mediated mesenteric artery relaxation. a Mice were treated with CuEC for 3 days, and their mesenteric arteries were used to measure the reactivity to acetylcholine. The left panel shows representative traces of acetylcholine-induced relaxation. The right panel is a statistical graph. n = 6. **p < 0.01 vs. control. Ach, acetylcholine. b CuEC-mediated mouse mesenteric artery relaxation. The left panel shows representative traces of CuEC-induced relaxation. The right panel is a statistical graph. n = 4. ***p < 0.001 vs. control. c Representative traces of CuEC-induced relaxation of rat mesenteric arteries. The left panel shows representative traces of CuEC-induced relaxation. The right panel is a statistical graph. n = 4. ***p < 0.001 vs. control
CuEC induced relaxation of mesenteric arteries in a concentration-dependent manner
Next, we used CuEC to act on the mouse mesenteric artery rings directly and found that CuEC could induce the vasodilation of the mesenteric artery in mice (Fig. 4b). The same phenomenon also appeared in the mesenteric artery of rats (Fig. 4c). This result indicated that CuEC mediated vasodilation at least partly by improving endothelial function.
CuEC suppressed phenylephrine-induced vasoconstriction
Could CuEC play a direct role in vascular smooth muscle cells (VSMCs) and cause vasodilation? Compared with the control, 30 min treatment of endothelium-denuded rings with CuEC (2 or 10 μg/ml) attenuated phenylephrine-induced contractions in the arterial rings (Fig. 5a, b). Similar effects were also obtained in endothelium-denuded mesenteric arteries from male rats (Fig. 5c, d). This result indicated that CuEC could act on VSMCs and reduce phenylephrine-mediated vasoconstriction.
CuEC suppressed phenylephrine-induced mesenteric arterial vasoconstriction. a Representative traces of phenylephrine-induced mouse mesenteric artery constriction after treatment with different concentrations of CuEC (2 μg/ml and 10 μg/ml). Phe, phenylephrine. b Statistical graph of phenylephrine-induced constriction after treatment with different concentrations of CuEC (2 μg/ml and 10 μg/ml). n = 4. ***p < 0.001 vs. control. c Representative traces of phenylephrine-induced rat mesenteric artery constriction after treatment with different concentrations of CuEC (2 μg/ml and 10 μg/ml). d Statistical graph of phenylephrine-induced rat mesenteric artery constriction after treatment with different concentrations of CuEC (2 μg/ml and 10 μg/ml). n = 4. ***p < 0.001 vs. control
Discussion and conclusion
Cucumis melo L., as an effective herb for treating jaundice in traditional Chinese medicine, is widely used in all parts of China. However, there are few studies on its active ingredients in cardiovascular research, especially on blood pressure regulation. Similarly to the previous study, we extracted and identified cucurbitacins as the main active ingredients in Cucumis melo L., most of which were CuB. There have been reports that administration of a large dose of Cucumis melo L. leads to death from poisoning [15, 16], but the causes and mechanisms of death are not clear. Indeed, we found that administration of a high dose of CuEC (2 mg/kg) led the majority of mice to die within 12 h because of poisoning. We found that the mice displayed massive pleural effusion, ascites and severe brain edema. Further study found that cucurbitacins could increase vascular permeability in mice and impair vascular barrier function. Our study demonstrated that the direct cause of Cucumis melo L. or CuEC-induced poisoning was vascular endothelial dysfunction.
Since a high dose of CuEC could cause changes in endothelial barrier function in a short time, did it affect other functions of the endothelium? As we know, the vascular endothelium plays an important role in controlling blood pressure by synthesizing and releasing nitric oxide (NO) (endothelium-derived relaxing factor, EDRF) [38]. A previous study reported that Cucumis melo L. decreased blood pressure by increasing vascular permeability and reducing blood volume [39], which is similar to the poisoning dose in our study. However, whether CuEC affects blood pressure directly by regulating endothelial cell-mediated vasodilation needed to be determined. Our study showed that 1 mg/kg of CuEC could decrease blood pressure but did not cause changes in vascular permeability or death from poisoning. Acetylcholine-mediated vasodilation was dependent on the release of endothelial NO [40]. Our studies on mesenteric arteries showed that CuEC treatment for 3 days significantly promoted acetylcholine-mediated vasodilation. This result demonstrated that CuEC may improve the capability of NO synthesis in endothelial cells. In addition, CuEC induced vasodilation in a dose-dependent manner in contracted mesenteric arteries by phenylephrine, which acts on α1-adrenoceptors and raises Ca2+ and leads to contraction in vascular smooth muscle cells (VSMCs) [41]. Next, we checked the contractile response of endothelium-denuded mesenteric artery rings pretreated with CuEC (2 μg/ml and 10 μg/ml) to phenylephrine. CuEC significantly suppressed phenylephrine-mediated vasoconstriction. This result indicated that CuEC may also act on VSMCs and mediate vasodilation. However, the molecular mechanism of CuEC-induced vasodilation is unclear, and more studies are needed.
Although our studies have shown that CuEC increased permeability by reducing endothelial cell junctions at high doses and lowered blood pressure by improving vascular function at low doses, it was unclear which component of CuEC increased vascular permeability and improved vascular diastolic and contractile function. The dominant and most important component in CuEC is CuB (~62.6%). Therefore, the first possibility is that CuB played a role in lowering blood pressure. Only a large dose of CuEC led to death from poisoning. It could be that other components led to increased vascular permeability and impaired endothelial barrier function, but further experiments are still needed to verify this deduction.
Hypertension is an important disease endangering human beings in modern society. There are many studies on the occurrence and development of hypertension, but antihypertensive drugs without side effects are very few [42]. Hypertensive patients often also exhibit hyperlipidemia, fatty liver, and other lipid metabolism disorder-related diseases. Liver lesions can lead to jaundice and other complications [43, 44]. Cucumis melo L., as an effective medicine for the treatment of jaundice, may have a significant role in improving glucose and lipid metabolism, and it will be promising for use in patients with liver disease complicated with hypertension.
In summary, our study demonstrated that CuEC can reduce blood pressure by increasing vasodilation and inhibiting vasoconstriction, which may be an effective clinical drug for the treatment of hypertension (Fig. 6).
References
Van Camp G. Cardiovascular disease prevention. Acta Clin Belg. 2014;69:407–11.
Poulter NR, Prabhakaran D, Caulfield M. Hypertension. Lancet (Lond, Engl). 2015;386:801–12.
Gkaliagkousi E, Gavriilaki E, Triantafyllou A, Douma S. Clinical significance of endothelial dysfunction in essential hypertension. Curr Hypertens Rep. 2015;17:85.
Boegehold MA. The effect of high salt intake on endothelial function: Reduced vascular nitric oxide in the absence of hypertension. J Vasc Res. 2013;50:458–67.
Rubio-Ruiz ME, Perez-Torres I, Soto ME, Pastelin G, Guarner-Lans V. Aging in blood vessels. Medicinal agents for systemic arterial hypertension in the elderly. Ageing Res Rev. 2014;18:132–47.
Hocht C, Bertera FM, Mayer MA, Taira CA. Issues in drug metabolism of major antihypertensive drugs: Beta-blockers, calcium channel antagonists and angiotensin receptor blockers. Expert Opin drug Metab Toxicol. 2010;6:199–211.
Wright JM, Musini VM, Gill R. First-line drugs for hypertension. Cochrane database Syst Rev. 2018;4:Cd001841.
Laurent S. Antihypertensive drugs. Pharmacol Res. 2017;124:116–25.
Wiysonge CS, Bradley HA, Volmink J, Mayosi BM, Opie LH. Beta-blockers for hypertension. Cochrane database Syst Rev. 2017;1:Cd002003.
Roush GC, Sica DA. Diuretics for hypertension: a review and update. Am J Hypertens. 2016;29:1130–7.
Chrysant SG. Antihypertensive therapy causes erectile dysfunction. Curr Opin Cardiol. 2015;30:383–90.
Thomopoulos C, Parati G, Zanchetti A. Effects of blood pressure-lowering on outcome incidence in hypertension: 5. Head-to-head comparisons of various classes of antihypertensive drugs - overview and meta-analyses. J Hypertens. 2015;33:1321–41.
Na L, Ang G, Jiang G, Lei D, Xu J, Hui Z, et al. Research advance on pharmaceutical science of melon pedicle. J Anhui Agric Sci. 2011;39:8369–70.
Liu X, Fu Y. Clinical application of melon pedicle and understanding of poisoning. Gansu J Tradit Chin Med. 2008;21:7–9.
Cai Y, Fang X, He C, Li P, Xiao F, Wang Y et al. Cucurbitacins: a systematic review of the phytochemistry and anticancer activity. Am J Chin Med. 2015;43:1331–50.
Kaushik U, Aeri V, Mir SR. Cucurbitacins - an insight into medicinal leads from nature. Pharmacogn Rev. 2015;9:12–18.
Chen W, Sun Y, Yuan Z, Li Y, Wang L, Wu L. Isolation and identification of the chemical constituents of pedicellus melo. J Shenyang Pharm Univ. 2014;31:351–4.
Lan T, Ya Z, Hai-feng S, Weiguang S. Studies on the separation of cucurbitacins from the fruit base of cucumis melo l. And their antitumor activities. J Zhejiang Univ Technol. 2012;449:388–391.
Sun Y, Zhang J, Zhou J, Huang Z, Hu H, Qiao M et al. Synergistic effect of cucurbitacin b in combination with curcumin via enhancing apoptosis induction and reversing multidrug resistance in human hepatoma cells. Eur J Pharmacol. 2015;768:28–40.
Zheng Q, Liu Y, Liu W, Ma F, Zhou Y, Chen M et al. Cucurbitacin b inhibits growth and induces apoptosis through the jak2/stat3 and mapk pathways in shsy5y human neuroblastoma cells. Mol Med Rep. 2014;10:89–94.
Zhu JS, Ouyang DY, Shi ZJ, Xu LH, Zhang YT, He XH. Cucurbitacin b induces cell cycle arrest, apoptosis and autophagy associated with g actin reduction and persistent activation of cofilin in jurkat cells. Pharmacology. 2012;89:348–346.
Iwanski GB, Lee DH, En-Gal S, Doan NB, Castor B, Vogt M et al. Cucurbitacin b, a novel in vivo potentiator of gemcitabine with low toxicity in the treatment of pancreatic cancer. Br J Pharmacol. 2010;160:998–1007.
Shukla S, Khan S, Kumar S, Sinha S, Farhan M, Bora HK et al. Cucurbitacin b alters the expression of tumor-related genes by epigenetic modifications in nsclc and inhibits nnk-induced lung tumorigenesis. Cancer Prev Res (Phila, Pa). 2015;8:552–62.
Shukla S, Sinha S, Khan S, Kumar S, Singh K, Mitra K et al. Cucurbitacin b inhibits the stemness and metastatic abilities of nsclc via downregulation of canonical wnt/beta-catenin signaling axis. Sci Rep. 2016;6:21860.
Xie YL, Tao WH, Yang TX, Qiao JG. Anticancer effect of cucurbitacin b on mkn-45 cells via inhibition of the jak2/stat3 signaling pathway. Exp Ther Med. 2016;12:2709–15.
Promkan M, Dakeng S, Chakrabarty S, Bogler O, Patmasiriwat P. The effectiveness of cucurbitacin b in brca1 defective breast cancer cells. PloS ONE. 2013;8:e55732.
Sikander M, Hafeez BB, Malik S, Alsayari A, Halaweish FT, Yallapu MM et al. Cucurbitacin d exhibits potent anti-cancer activity in cervical cancer. Sci Rep. 2016;6:36594.
Hall JA, Seedarala S, Rice N, Kopel L, Halaweish F, Blagg BS. Cucurbitacin d is a disruptor of the hsp90 chaperone machinery. J Nat Prod. 2015;78:873–9.
Dong Y, Lu B, Zhang X, Zhang J, Lai L, Li D et al. Cucurbitacin e, a tetracyclic triterpenes compound from chinese medicine, inhibits tumor angiogenesis through vegfr2-mediated jak2-stat3 signaling pathway. Carcinogenesis. 2010;31:2097–104.
Attard E, Martinoli MG. Cucurbitacin e, an experimental lead triterpenoid with anticancer, immunomodulatory and novel effects against degenerative diseases. A mini-review. Curr Top Med Chem. 2015;15:1708–13.
Zha QB, Zhang XY, Lin QR, Xu LH, Zhao GX, Pan H et al. Cucurbitacin e induces autophagy via downregulating mtorc1 signaling and upregulating ampk activity. PloS ONE. 2015;10:e0124355.
Lee D, Yoo JH, Lee BC. Therapeutic effect of cucumis melo l. Extract on insulin resistance and the gut microbiome in lep(ob)/lep(ob) mice. Evid Based Complement Altern Med. 2018;2018:8159261.
Kim KH, Lee IS, Park JY, Kim Y, An EJ, Jang HJ. Cucurbitacin b induces hypoglycemic effect in diabetic mice by regulation of amp-activated protein kinase alpha and glucagon-like peptide-1 via bitter taste receptor signaling. Front Pharmacol. 2018;9:1071.
Sallam AM, Esmat A, Abdel-Naim AB. Cucurbitacin-b attenuates ccl4 -induced hepatic fibrosis in mice through inhibition of stat-3. Chem Biol Drug Des. 2018;91:933–41.
Wu YL, Zhang YJ, Yao YL, Li ZM, Han X, Lian LH et al. Cucurbitacin e ameliorates hepatic fibrosis in vivo and in vitro through activation of ampk and blocking mtor-dependent signaling pathway. Toxicol Lett. 2016;258:147–58.
Xiao Y, Yang Z, Wu QQ, Jiang XH, Yuan Y, Chang W et al. Cucurbitacin b protects against pressure overload induced cardiac hypertrophy. J Cell Biochem. 2017;118:3899–910.
Zhang Z, Jiang M, Xie X, Yang H, Wang X, Xiao L et al. Oleanolic acid ameliorates high glucose-induced endothelial dysfunction via ppardelta activation. Sci Rep. 2017;7:40237.
Tousoulis D, Kampoli AM, Tentolouris C, Papageorgiou N, Stefanadis C. The role of nitric oxide on endothelial function. Curr Vasc Pharmacol. 2012;10:4–18.
Hong J. Cucurbitacins and its pharmacological studies. Foreign Med Sci. 1996;18:13–14.
Kamper AM, de Craen AJ, Westendorp RG, Blauw GJ. Endothelium-dependent no-mediated vasodilation in humans is attenuated by peripheral alpa1-adrenoceptor activation. Vasc health risk Manag. 2005;1:251–6.
Amberg GC, Navedo MF. Calcium dynamics in vascular smooth muscle. Microcirculation . 2013;20:281–9.
Mancia G, Grassi G, Zanchetti A. New-onset diabetes and anti hypertensive drugs. J Hypertens. 2006;24:3–10.
Redon J, Cifkova R, Laurent S, Nilsson P, Narkiewicz K, Erdine S et al. Mechanisms of hypertension in the cardiometabolic syndrome. J Hypertens. 2009;27:441–51.
Fouad YM, Yehia R. Hepato-cardiac disorders. World J Hepatol. 2014;6:41–54.
Acknowledgements
We thank Dr. Hua Chen for the mesenteric artery study. The expert technical assistance of Dr. Xue Sui is gratefully acknowledged. This work was supported by the basic research projects of higher education institutions in the Liaoning Province Department of Education (LQ2017045).
Author information
Authors and Affiliations
Contributions
RQY extracted the CuEC and performed the animal experiments. LQ performed the mesenteric arterial vascular reactivity assay. WJY performed the UPLC-Q/TOF-MS and UPLC-MS/MS analyses. XHC performed the cell experiments and the en face immunostaining. GXL analyzed the data. WQT and RCC prepared the materials. HX designed the experiments, analyzed the data and wrote the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yuan, RQ., Qian, L., Yun, WJ. et al. Cucurbitacins extracted from Cucumis melo L. (CuEC) exert a hypotensive effect via regulating vascular tone. Hypertens Res 42, 1152–1161 (2019). https://doi.org/10.1038/s41440-019-0258-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-019-0258-y
Keywords
This article is cited by
-
Apoptotic and antimetastatic effect of cucurbitacins in cancer: recent trends and advancement
Naunyn-Schmiedeberg's Archives of Pharmacology (2023)