Abstract
Background/objectives
Retinal vein occlusion (RVO) is the second most common retinal vascular disorder. Despite promising advances with anti-VEGF therapy, select patients are unresponsive to therapy. A precision medicine-based approach for therapeutic decision-making based on underlying biomarkers may facilitate treatment based on the underlying pathway. This study aims to identify the baseline and longitudinal cytokine profiles of RVO-related macular oedema and correlating these expression profiles with higher order OCT features using a novel retinal segmentation and feature extraction platform.
Subjects/methods
The IMAGINE study is a post-hoc assessment of aqueous humour cytokines with correlation to higher level analysis of imaging studies. OCT scans underwent machine learning enhanced segmentation of the internal limiting membrane (ILM), ellipsoid zone (EZ) and retinal pigment epithelium (RPE), as well as evaluating volumetric fluid metrics. Samples of aqueous humour were obtained at baseline, as well as months 4 and 9 prior to treatment. These samples were analysed for the expression of multiple cytokines. Patients were divided into Responders and Non-Responders based on OCT profiles. Additionally, patients were categorised as a Rebounder if their CST increased by 50% after initial improvement.
Results
Twenty-six eyes were included. The OCT-based response schema identified 21 Responders (81%) and 5 Non-Responders (19%). VEGF levels directly correlated with intraretinal fluid volume and angiogenin was inversely correlated with fluid indices. Multiple cytokines, including ANGPTL4, were directly correlated with ellipsoid zone disruption. The baseline VEGF levels were significantly higher in all responders compared to Non-Responders (p = 0.02). Rebounders tended to have significantly decreased levels of angiogenin and TIMP-1 (p = 0.019, p = 0.015).
Conclusions
Cytokine expression was linked to specific OCT features and treatment response in RVO. Identification of an imaging phenotype that could serve as a surrogate for underlying active disease pathways could enhance treatment decision-making and precision medicine.
Similar content being viewed by others
Introduction
Retinal vein occlusion (RVO) is the second most common retinal vascular disorder in the middle-aged and elderly population, following diabetic retinopathy [1,2,3]. Population-based studies estimate the prevalence of RVO between 0.6 and 1.1% of the population, with branch retinal vein occlusions (BRVOs) occurring three to fourfold more frequently than central retinal vein occlusions (CRVOs) [2, 4, 5]. RVOs are caused by obstruction to venous drainage, leading to a multitude of sequelae, including retinal haemorrhages, cotton wool spots, oedema, and exudates [1, 6]. The major cause of vision loss in RVO is macular oedema, which results from a cascade of cytokines originating from the injured, hypoxic tissue, subsequently causing endothelial cell dysfunction and break down of the blood–retinal barrier [1, 2, 7, 8].
A critical cytokine involved in RVO sequelae, including macular oedema, is vascular endothelial growth factor (VEGF) [8, 9]. VEGF inhibitors, such as aflibercept (Eylea, Regeneron, Tarrytown, NY) and ranibizumab, (Lucentis, Genentech, San Francisco, CA), are now the first-line treatment for macular oedema secondary to RVO. The major phase III trials for VEGF inhibitors for macular oedema following RVO (i.e., COPERNICUS/GALILEO, VIBRANT, BRAVO, CRUISE) demonstrated significant improvement in macular oedema and visual acuity in RVO patients [9, 10]. While these results have been a breakthrough in pharmacotherapy for RVO, a subset of patients continue to have macular oedema despite continued therapy [6, 11]. A possible explanation for this phenomenon is the co-existence of multiple pathways: a predominantly VEGF dependent cycle as well as alternative, inflammatory-based pathways [12, 13]. A more personalized and precise approach utilizing surrogate biomarkers to help identify for the dominant underlying pathway may allow for patient therapy stratification based on their profile.
Concurrent with the wide-ranging biologic expression pathways, the phenotypic OCT features of RVOs is varied with increased central subfield thickness (CST) only partially explaining vision changes from RVO [14]. Studies have explored the other OCT findings in RVO, including ganglion cell layer cysts and hyperreflective foci [14]. Inner retinal disorganisation as well as loss of outer retinal integrity are both correlated to final visual acuity [15]. Quantifying and characterising OCT biomarkers in patients with RVOs may help predict individual responses to particular therapies, especially if these OCT biomarkers can be linked to the underlying biologic pathway.
Prior reports have demonstrated elevated concentrations of VEGF concentrations and other inflammatory cytokines in the aqueous and vitreous humour of patients with RVOs [12, 16]. However, the long term follow up and sample size in these studies is often limited, and the cytokine analysis was not extensive. A deeper analysis of aqueous humour cytokine expression profile in RVO-related macular oedema combined with OCT higher order imaging biomarkers may provide unique opportunities for phenotyping the disease and predicting treatment response. To best determine treatment regimens for RVO patients, further investigations of intraocular cytokine expression are necessary to clarify their role in RVO pathology.
This study aims to identify the baseline and longitudinal cytokine profiles of RVO-related macular oedema and evaluate the association of these profiles with higher order features, such as retinal fluid index and ellipsoid zone (EZ) integrity, as well as the association with treatment response.
Methods
Study design
The IMAGINE study is a post-hoc assessment of aqueous humour cytokines with correlation to higher level analysis of imaging studies obtained through clinical trials, including the WAVE (Wide-Field Angiography Guided Targeted Retinal Photocoagulation Combined with Anti-VEGF Intravitreal Injections for the Treatment of Ischaemic Retinal Occlusion) study [17]. The IMAGINE study was determined to be exempt by the Cleveland Clinic’s IRB. The data provided within this analysis include only data analysed as part of the IMAGINE study that came exclusive from the WAVE study.
The WAVE study was an IRB-approved prospective, randomized trial to assess if targeted panretinal photocoagulation (TRP), applied to areas of nonperfusion in eyes with ischaemic central or branch RVOs decreased the treatment burden of intravitreal ranibizumab. All participants provided written informed consent. All 30 eyes were treated with 0.5 mg of ranibizumab for 6 months before transitioning to pro re nata (PRN) treatments for either intraretinal or subretinal fluid on optical coherence tomography (OCT) or evidence of neovascularization. Patients were randomized at a 1:4 ratio for monotherapy (ranibizumab only, n = 6) or combination therapy (ranibizumab plus TRP, n = 24). TRP was placed at 1 week after the first ranibizumab injection and again at month 4 if necessary. Treatments were centred on areas of nonperfusion outside of the macula. Complete eligibility criteria are detailed within the original report [17].
OCT software platform and imaging feature extraction
Spectral domain OCT macular cube scans were imported into previously described machine-learning enhanced segmentation and feature extraction software [18,19,20,21]. The macular OCT scans underwent automated analysis to generate intraretinal and subretinal fluid extraction metrics as well as segmentation of the internal limiting membrane (ILM), EZ, and retinal pigment epithelium (RPE). These delineations were used to calculate thickness, area and volume measurements of various retinal sections. Automated segmentation for each B–scan was reviewed by two expert readers.
Retinal thickness was assessed (ILM to RPE). The photoreceptor outer segment compartment (EZ to RPE) was also measured. Additionally, en-face EZ-RPE topographic maps were generated to visualize EZ changes such as total attenuation (measuring 0 micron thick), or attenuation (measuring 20 microns or less in thickness). In addition, fluid segmentation of intraretinal fluid (IRF) and subretinal fluid (SRF) was also performed [20,21,22]. Measurements were taken over panmacular scans, as well as the central macular zone (i.e., 1 millimetre (mm) radius from the fovea) and central subfield (i.e., 0.5 mm radius) from the fovea. Previously reported retinal fluid indices (RFI) that measure the proportion of fluid to retinal tissue in either the entire macular cube, 1 mm central subfield, and central macular (2 mm subfield) were also measured [22, 23].
Cytokine analysis
Samples of aqueous humour were obtained from patients at their baseline visit before injection, as well as months 4 and 9 prior to treatment. A multiplex ELISA based assay (RayBioTech, Peachtree Corners, GA) measured the levels of 54 cytokines, including: Activin A, AgRP, Angiogenin, ANG-2, ANGPTL4, bFGF, ENA-78, GRO, HB-EGF, HGF, IFNg, IGF-1, IL-1a, IL-2, IL-6, IL-8, IL-17, IP-10, Leptin, LIF, MCP-1, PDGF-BB, PIGF, RANTES, TGFb1, TIMP-1, TIMP-2, ANG-1, Angiostatin, CXCL16, EGF, FGF-4, Follistatin, G-CSF, GM-CSF, I-309, IL-1b, IL-4, IL-10, IL-12p40, IL-12p70, I-TAC, MCP-2, MCP-3, MCP-4, MMP-1, MMP-9, PECAM-1, TGFa, TGFb3, Tie-1, Tie-2, uPAR, VEGF. The mean value of each sample, measured in quadruplicate, was normalised and any values that resulted below the limit of detection were pushed to 0 to avoid false positives. Only cytokines detected in at least 20% of all subjects.
Categorisation of eyes by response and rebound profiles
As previously described and based on OCT profiles, four categories of response patterns were identified and classified [22].
-
1.
Super Responders: Defined as ≥80% reduction of the baseline IRF volume, SRF volume <0.001 mm3 and/or a ≥ 80% or decrease in excess thickening of the CST. Excess thickening was defined as CST beyond 300 µm. This response must have been obtained within 1 injection.
-
2.
Early Responders: If the above parameters were met within 3 injections.
-
3.
Slow Responders: If the parameters described in #1 were met between months 3 and 12.
-
4.
Non-Responders/Minimal Responders: If 50% or more of the initial IRF or CST was maintained by month 12 (Fig. 1).
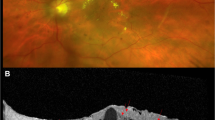
Fig. 1: Composite image of B-scans showing Super Responders (Row 1), Early Responders (Row 2), Slow Responders (Row 3), and Non Responders (Row 4).
Furthermore, eyes identified as a Super Responder, Early Responder or Slow Responder were subcategorized as a Rebounder if they developed a subsequent increase in CST by at least 50% over the treatment course from the best achieved CST.
Statistical analysis
Statistical assessment was performed with non-parametric testing given the non-normal distributions and smaller group sizes due to the larger number of cytokines investigated. Wilcoxon signed rank tests were performed to determine longitudinal changes in aqueous humour cytokine concentrations from baseline to month 4 or 9. Mann Whitney U Tests were used to compare the average cytokine levels within responder and rebounder groups, as well as to assess the effect of monotherapy or combination therapy. Spearman’s correlation coefficients were calculated to measure the association between OCT features and baseline aqueous humour cytokines. The effect of RVO phenotype [BRVO versus a hemi-retinal (HRVO) or CRVO] on cytokine levels was analysed with Wilcoxon Rank Sum. For the purposes of this analysis, HRVO and CRVO patients were grouped together.
Results
Baseline clinical characteristics and demographics
Thirty eyes were studied in WAVE, with 26 (87%) patients having sufficient aqueous samples for analysis. Therefore, the analysis focuses on these 26 eyes. Of these, 13 (50%) were men. The mean age of presentation was 64.7 ± 9.7 years (range: 44–79 years). Monotherapy was performed in 6 eyes (23%) and combination therapy was performed in 20 eyes (77%). Baseline best-corrected visual acuity (BCVA) averaged 50.6 ± 21.7 ETDRS letters (range: 7 to 77). In terms of RVO subtypes, 16 (62%) had CRVOs, including 1 patient with a HRVO, and 10 (38%) had BRVOs (Table 1).
Baseline and longitudinal cytokine dynamics
Of 54 cytokines evaluated, 27 had levels above detection threshold. (Table 2) Across the entire cohort, VEGF concentrations were significantly lower at month 4 compared to baseline (24.3 vs 827.3 pg/mL, p < 0.000001). Though higher than month 4, concentrations trended towards significant reduction at month 9 following the transition to PRN dosing (153.7 pg/mL, n = 23, p = 0.06). Leptin also decreased significantly at month 4 compared to baseline (p = 0.05) with a slight increase in values by month 9, which were not statistically significantly different from baseline. No other cytokines demonstrated a significant change at month 4 or 9.
Baseline correlation of aqueous humour cytokines with OCT imaging biomarkers
Retinal fluid indices and fluid parameters
VEGF had a positive relationship with intraretinal fluid volume, measured across the panmacular scan and central macular intraretinal fluid volume (i.e., central 2-mm; r = 0.4, p = 0.03; r = 0.39, p = 0.05, respectively). VEGF also trended towards significance with macular intraretinal fluid volume (r = 0.4, p = 0.06); macular total retinal fluid index (r = 0.4, p = 0.06), and central macular total retinal fluid index (r = 0.4, p = 0.07) (Table 3). Angiogenin had an inverse relationship with central subfield intraretinal fluid index that trended towards significance (r = −0.4, p = 0.07). TIMP-1 also had an inverse relationship with central subfield intraretinal fluid index that trended towards significance (r = −0.4, p = 0.07).
Outer retinal integrity
Multiple cytokines correlated with total EZ attenuation, including ANG-1 (r = 0.5, p < 0.01), ANGPTL4 (r = 0.5, p < 0.01), CXCL16 (r = 0.4, p = 0.04), HGF (r = 0.2, p < 0.01), IL-12 (r = 0.4, p = 0.02), IP-10 (r = 0.6, p < 0.01), leptin (r = 0.5, p = 0.01), and uPAR (r = 0.4, p = 0.04). Additionally, many were associated with partial EZ attenuation ANG-1 (r = 0.4, p < 0.05), ANGPTL4 (r = 0.5, p = 0.02), HGF (r = 0.4, p = 0.03), IP-10 (r = 0.5, p = 0.01), and leptin (r = 0.4, p = 0.036). In addition, EZ-RPE Central subfield volume and thickness was correlated with decreased IP-10 (r = −0.4, p = 0.05; r = −0.4, p = 0.05, respectively), and leptin (r = −0.4, p = 0.02; r = 0.4, p = 0.03, respectively) (Table 3).
Responders and Non-Responders
The OCT-based response classification schema identified 21 responders (81%) and 5 Non-Responders (19%). There were no patients that fell outside of these categories. The responders were split into 16 (62%) Super Responders, 3 (12%) Early Responders and 2 (8%) Slow Responders. At baseline, Super Responders had significantly increased VEGF levels compared to Non-Responders (1128.1 vs 158.1 pg/mL, p = 0.019). (Table 2) Several other cytokines trended towards significance when comparing Super Responders to Non-Responders including increased ANGPTL-4 in (928.6 vs 197.7 pg/ml, p = 0.07) and decreased EGF and FGF (0.03 vs 0.06 pg/ml, p = 0.076 and 296.8 vs 487.6 pg/ml, p = 0.06), respectively. When combining Super Responders and Early Responders, they displayed a similar significant increase in baseline VEGF compared to Non-Responders (981.8 vs 158.1 pg/ml, p = 0.024) in addition to significantly lowered EGF (0.03 vs 0.06 pg/ml, p = 0.05) concentration. ANGPTL-4 trended towards significance with a higher baseline level in Super Responders/Early Responders as compared to Non-Responders (855.9 versus 197.7 pg/ml, p = 0.075). The baseline VEGF levels remained high when grouping together all responders and comparing their values to Non-Responders (924.9 vs 158.1 pg/ml, p = 0.02) and baseline EGF remained significantly decreased (0.02 vs 0.06 pg/ml, p = 0.032) (Table 2).
Analyses comparing baseline values to month 4 and 9 were completed between response groups. Firstly, Super Responders were compared to Non Responders. At month 4, EGF levels significantly differed: in Super Responders the levels increased by 0.004 pg/ml while they decreased by 0.04 pg/ml in Non-Responders (p = 0.024). Angiogenin levels also trended towards decreasing less in Super Responders than in Non-Responders (−255.2 vs −3029.0 pg/ml, p = 0.06); and VEGF decreased more in Super Responders than Non-Responders (−1146.6 vs −148.6 pg/ml, p = 0.06). In an analysis comparing all responders versus Non-Responders at month 4, angiogenin significantly decreased in responders less than in Non-Responders (−98.3 vs −3028 pg/ml, p = 0.04). EGF significantly increased in all responders compared Non-Responders (+0.009 vs −0.05 pg/ml, p = 0.013). VEGF changes from baseline approached significance with a greater decrease in responders than in Non-Responders (−952.4 vs −148.6 pg/ml, p = 0.06). When assessing changes from baseline to month 9, only changes in VEGF trended towards significance. When comparing change in Super Responders against Non-Responders (−1114.8 vs 202.8 pg/ml, p = 0.07), and all responders against Non-Responders (−825.7 vs +202.8 pg/ml, p = 0.076) there was a trend towards greater reduction in VEGF levels at month 9 in the responder categories.
Rebounders and Non-Rebounders
Among the 21 responders, 13 met the definition of Rebounder. At baseline, two cytokines were significantly decreased at baseline in Rebounders; angiogenin (5219.7 vs 6043.6 pg/ml, p = 0.019) and TIMP-1 (13,189.9 vs 14,944.9 pg/ml, p = 0.015). VEGF levels were similar between the 2 groups (954.3 vs 877.2, p = 0.24)
Effect of RVO morphology and targeted retinal photocoagulation on cytokines
An analysis of cytokine levels was completed at month 9 assessing the impact of TRP. Subjects receiving combination therapy had increased EGF (p = 0.02) compared to ranibizumab alone (p = 0.02). There was no significant difference in reduction in VEGF between the groups at month 9 (p = 0.95). In terms of RVO morphology, the levels of PECAM-1 and VEGF were significantly lower in the BRVO group compared to the combined HRVO and CRVO group (p = 0.04, p = 0.01, respectively).
OCT-derived imaging biomarkers in Responders and Non Responders
When compared to Non-Responders, Super Responders at baseline had increased panmacular retinal volume (13.5 mm3 vs 10.3 mm3, p = 0.015) and increased panmacular intraretinal fluid volume (1.3 vs 0.3, p = 0.03) (Table 4). Macular measurements for fluid indexes approached significance, with Super Responders having increased macular IRF index (8.4% vs 2.4%, p = 0.06), and macular total retinal fluid index (9.5% vs 2.4%, p = 0.06). Central macular IRF index also approached significance with Super Responders having an increased value (18.3% vs 9.0% p = 0.09), and central macular total retinal fluid significantly higher (21.8% vs 9.0%, p = 0.04). (Table 2) When comparing subretinal fluid parameters, 8 of the 16 Super Responders had baseline subretinal fluid compared to 0 of the 5 Non-Responders (50% vs 0%, p = 0.045), and 10 of the 21 Responders had baseline subretinal fluid compared to 0 of the 5 Non-Responders (47.6% vs 0%, p = 0.049).
When comparing all Responders to Non-Responders, all Responders had significantly increased panmacular retinal volume (13.3 mm3 vs 10.3 mm3, p = 0.008). Intraretinal fluid volume approached significance (1.2 mm3 vs 0.3 mm3, p = 0.06). The central macular retinal fluid index, macular total retinal fluid index and macular IRF index all trended towards significance as well (19.9% vs 9.0%, p = 0.06; 8.4% vs 2.4%, p = 0.09; 7.6% vs 2.4%, p = 0.09) (Table 4).
Discussion
This study seeks to identify which aqueous humour cytokines are associated with links between higher order OCT features and underlying cytokine expression/treatment response. The heterogeneity of response to anti-VEGF treatments and success with intravitreal steroids in prior literature speaks to a need for a better initial assessment of potential responders to traditional anti-VEGF therapy versus other, broader anti-inflammatory avenues [24, 25]. A more precise classification of potential responders may be possible through intraocular cytokine analyses and imaging biomarker surrogates. The rationale for intraocular cytokine assessment is well documented; samples provide an estimate of the retinal and choroidal excretion, and the intraocular concentrations do not correlate with systemic levels [7]. Studies have shown a strong correlation between cytokine levels in the aqueous and vitreous [26]. Additionally, the need for further analysis of OCT morphology in RVO is essential, as changes in OCT are widespread with retinal vein occlusions, with central subfield thickness only explaining a portion of the visual acuity changes from RVO [14].
Due to its multifactorial impact on the retina, VEGF has been heavily focused on for the treatment of RVO related macular oedema. VEGF release is partially stimulated from hypoxic retina and is involved in the formation of macular oedema and angiogenesis [8, 27, 28]. It promotes the migration of inflammatory factors, as well as causing actin filament rearrangement in endothelial cells, causing increased endothelial cell permeability [29, 30]. Multiple reports have assessed intraocular VEGF levels in patients with RVOs. This study further supports prior findings of elevated VEGF levels at baseline which decrease following anti-VEGF pharmacotherapy [12, 16, 31,32,33,34,35,36,37].
When assessing the connections between aqueous humour cytokines and OCT imaging patterns, VEGF was directly correlated with increasing fluid parameters. Previous studies have linked elevation of VEGF in various retinal disorders to increased retinal thickness and retinal fluid [31,32,33,34,35, 37, 38]. Few reports have evaluated retinal fluid volumes. However, one study did show that central retinal fluid index measurements have been correlated to visual acuity in diabetic retinopathy and may serve as a predictive value for tracking response and improving visual acuity [18]. These metrics may also provide valuable information on tracking progress and visual improvement in RVO patients.
In contrast to VEGF levels, angiogenin demonstrated an inverse relationship with central subfield intraretinal fluid index. Furthermore, angiogenin was found to be lower in the patients who rebounded when switching to PRN treatment, which may also speak to a protective property of angiogenin. In our review of the literature, we were unable to identify previous reports regarding the relationship between intraocular angiogenin expression and macular oedema in RVOs. However, the decreased levels of angiogenin in the setting of increased VEGF levels have been reported in the vitreous of patients with diabetic retinopathy, similar to the findings of this present study [39].
TIMP-1, was also inversely correlated with central subfield intraretinal fluid index. In this study, increasing TIMP-1 was related to decreasing fluid volume metrics, which may reveal a neuroprotective effect of TIMP-1 on the integrity of the retina, retinal vasculature, and extracellular matrix. Moreover, TIMP-1 was higher in patients who did not rebound when switching to PRN treatment, which may reveal a protective effect against macular oedema.
The link between underlying cytokine expression and outer retinal integrity has not been explored in depth in the prior literature. In this analysis, EZ attenuation correlated with several cytokines, including Ang-1, Angiopoietin like protein-4, hepatocyte growth factor (HGF), interferon gamma produced protein 10 (IP-10), and leptin. This analysis also revealed that increasing IL-10 and leptin levels also negatively correlated with EZ integrity. It remains unclear if these cytokines are directly responsible for the outer retinal changes or if they are a reflection of the deregulation of cytokine balance within the eye following an RVO. Overall severity that may be linked to retinal atrophy. Leptin is also co-expressed with VEGF and unregulated with chronic VEGF exposure, which may explain its increase in our patient cohort and its potential impact on the ellipsoid zone [40]. Further analyses into the link between cytokine expression and outer retinal metrics may provide valuable information into the pathology behind RVO related macular oedema and visual prognosis.
When considering treatment response characteristics, VEGF was significantly elevated at baseline in all responder groups, with Super Responders demonstrating the highest VEGF levels. The decrease in VEGF levels from baseline approached significance when analysing Super Responders against Non-Responders and when grouping all Responders against Non-Responders at months 4 and 9. It should be mentioned that at month 9, the VEGF levels in Non-Responders started to rise slightly. This may be secondary to accumulating VEGF levels preceding the development of clinically apparent macular oedema in the setting of decreased anti-VEGF injections during the PRN period before treatment, if necessary.
As expected, VEGF levels were significantly lower in the BRVO group compared to the CRVO group [38]. Additionally, previous literature has shown a decrease in VEGF levels in CRVO patients treated with photocoagulation [41]. While not statistically significant, our analysis did show more of a decrease in VEGF levels from baseline to month 9 in the combination group as compared to the monotherapy treatment group.
In terms of other cytokine changes, leptin decreased significantly from baseline to month 4 and increased by month 9 when eyes were switched to PRN treatment. Leptin is linked to the VEGF pathway and is co-expressed with VEGF during neovascularization of the retina, and unregulated with chronic VEGF expression [40]. Therefore, inhibition of the VEGF pathway with constant injections at month 4 may have also occur with decreased leptin production, and with increasing VEGF levels by month 9, leptin may have also risen.
Overall, EGF tended to be lower at baseline in all of the Responder groups as compared to Non-Responders. EGF however, did increase from baseline in Super Responders and in all responders when compared to Non-Responders at month 4. This may speak to an inverse relationship between EGF and VEGF expression, as VEGF was initially significantly increased in the responders and decreased by month 4. Alternatively, EGF may have a protective effect against macular oedema formation as shown in models with diabetic retinopathy, and the patients who have increased their EGF production after an RVO may be able to better inhibit or resolve their macular oedema [42].
Two cytokines, angiogenin and TIMP-1, were significantly decreased in Rebounders at baseline, which may speak to their protective effects against macular oedema. TIMP-1, also known as tissue inhibitors of metalloproteinase, works on extracellular matrix remodelling and its expression prevents apoptotic cell death. It has also been shown to have neuroprotective effects in the retina in retinitis pigmentosa [43, 44]. The decrease of this level at baseline in patients who rebound may speak to a deregulation of the pathways that protect the retina from damage and macular oedema formation.
This study is not without limitations. Subject numbers are small which limits the statistical power of some analyses. The classification system may lead to inherent bias as responder groups may have a higher level of baseline fluid, resulting in an increased likelihood to display improvement. Furthermore, the use of ranibizumab limits the generalisation of these results to other anti-VEGF medications.
Overall, this study assessed the association of aqueous humour cytokine profiles to OCT biomarkers in RVO, as well as a link to treatment response profiles. In exploring the anatomic- biologic bridge, VEGF, angiogenin, and TIMP-1 were related to retinal fluid features, while other cytokines correlated with outer retinal integrity. This analysis additionally assessed the baseline OCT morphology of patients who responded to intravitreal ranibizumab and found that certain intraretinal fluid, thickness and volume parameters were likely to predict response. When evaluating response characteristics and cytokine levels, Responders tended to have higher levels of VEGF, leptin and angiopoietin like −4 protein, while having lower levels of EGF. Conversely, Non-Responders tend to have lower levels of VEGF and higher levels of EGF, which may speak to a more inflammation driven pathologic state. Interestingly, over 50% of patients rebounded after successful improvement with fixed dosing of intravitreal ranibizumab, and these patients had lower expression of angiogenin and TIMP-1 at presentation. Integrating both of these into future analyses of cytokine dynamics in RVO may provide additional information into defining potential treatment responders.
SUMMARY
What was known before
-
Retinal vein occlusion (RVO) is the second most common retinal vascular disorder.
-
Despite anti-VEGF therapy, select patients are unresponsive to therapy.
What this study adds
-
VEGF levels directly correlated with intraretinal fluid volume and angiogenin was inversely correlated with fluid indices.
-
Multiple cytokines, including ANGPTL4, were directly correlated with ellipsoid zone disruption.
Data availability
Additional data are available upon request.
References
Michels RG, Gass JD. The natural course of retinal branch vein obstruction. Trans Am Acad Ophthalmol Otolaryngol. 1974;78:Op166–77.
Ehlers JP, Fekrat S. Retinal vein occlusion: beyond the acute event. Surv Ophthalmol. 2011;56:281–99.
Mitchell P, Smith W, Chang A. Prevalence and associations of retinal vein occlusion in Australia. The Blue Mountains Eye Study. Arch Ophthalmol 1996;114:1243–7.
Klein R, Klein BE, Moss SE, Meuer SM. The epidemiology of retinal vein occlusion: the Beaver Dam Eye Study. Trans Am Ophthalmol Soc. 2000;98:133–41. discussion 41-3
Cheung N, Klein R, Wang JJ, Cotch MF, Islam AF, Klein BE, et al. Traditional and novel cardiovascular risk factors for retinal vein occlusion: the multiethnic study of atherosclerosis. Investig Ophthalmol Vis Sci. 2008;49:4297–302.
Noma H, Mimura T, Yasuda K, Shimura M. Functional-morphological parameters, aqueous flare and cytokines in macular oedema with branch retinal vein occlusion after ranibizumab. Br J Ophthalmol. 2017;101:180–5.
Noma H, Funatsu H, Yamasaki M, Tsukamoto H, Mimura T, Sone T, et al. Pathogenesis of macular edema with branch retinal vein occlusion and intraocular levels of vascular endothelial growth factor and interleukin-6. Am J Ophthalmol. 2005;140:256–61.
Scholl S, Kirchhof J, Augustin AJ. Pathophysiology of macular edema. Ophthalmologica J Int d’ophtalmologie. 2010;224:8–15.
Campochiaro PA, Heier JS, Feiner L, Gray S, Saroj N, Rundle AC, et al. Ranibizumab for macular edema following branch retinal vein occlusion: six-month primary end point results of a phase III study. Ophthalmology. 2010;117:1102–12.e1.
Varma R, Bressler NM, Suner I, Lee P, Dolan CM, Ward J, et al. Improved vision-related function after ranibizumab for macular edema after retinal vein occlusion: results from the BRAVO and CRUISE trials. Ophthalmology. 2012;119:2108–18.
Heier JS, Campochiaro PA, Yau L, Li Z, Saroj N, Rubio RG, et al. Ranibizumab for macular edema due to retinal vein occlusions: long-term follow-up in the HORIZON trial. Ophthalmology. 2012;119:802–9.
Modi A, Sharma K, Sudhakar NP, Yadav NK. Aqueous humor cytokines and therapeutic customization in nonresponding macular edema secondary to retinal vein occlusion. Retin Cases Brief Rep. 2021;15:127–30.
Zeng Y, Cao D, Yu H, Zhuang X, Yang D, Hu Y, et al. Comprehensive analysis of vitreous chemokines involved in ischemic retinal vein occlusion. Mol Vis. 2019;25:756–65.
Narayanan R, Stewart MW, Chhablani J, Panchal B, Pappuru RR, Das T, et al. Baseline morphological characteristics as predictors of final visual acuity in patients with branch retinal vein occlusions: MARVEL report no. 3. Indian J Ophthalmol. 2018;66:1291–4.
Chan EW, Eldeeb M, Sun V, Thomas D, Omar A, Kapusta MA, et al. Disorganization of retinal inner layers and ellipsoid zone disruption predict visual outcomes in central retinal vein occlusion. Ophthalmol Retin. 2019;3:83–92.
Kotake O, Noma H, Yasuda K, Motohashi R, Goto H, Shimura M. Comparing cytokine kinetics between ranibizumab and aflibercept in central retinal vein occlusion with macular edema. Ophthalmic Res. 2018:1–8.
Wykoff CC, Ou WC, Wang R, Brown DM, Cone C, Zamora D, et al. Peripheral laser for recalcitrant macular edema owing to retinal vein occlusion: the WAVE trial. Ophthalmology. 2017;124:919–21.
Ehlers JP, Uchida A, Hu M, Figueiredo N, Kaiser PK, Heier JS, et al. Higher-order assessment of OCT in diabetic macular edema from the VISTA study: ellipsoid zone dynamics and the retinal fluid index. Opthalmol Retina. 2019;3:1056–66.
Itoh Y, Vasanji A, Ehlers JP. Volumetric ellipsoid zone mapping for enhanced visualisation of outer retinal integrity with optical coherence tomography. Br J Ophthalmol. 2016;100:295–9.
Ehlers JP, Clark J, Uchida A, Figueiredo N, Babiuch A, Talcott KE, et al. Longitudinal higher-order OCT assessment of quantitative fluid dynamics and the total retinal fluid index in neovascular AMD. Transl Vis Sci Technol 2021;10:29.
Ehlers JP, Zahid R, Kaiser PK, Heier JS, Brown DM, Meng X, et al. Longitudinal assessment of ellipsoid zone integrity, subretinal hyperreflective material, and subretinal pigment epithelium disease in neovascular age-related macular degeneration. Ophthalmol Retina. 2021;5:1204–13.
Abraham JR, Wykoff CC, Arepalli S, Lunasco L, Yu HJ, Hu M, et al. Aqueous cytokine expression and higher-order OCT biomarkers: assessment of the anatomic-biologic bridge in the IMAGINE DME study. Am J Ophthalmol. 2021;222:328–39.
Ehlers JP, Uchida A, Hu M, Figueiredo N, Kaiser PK, Heier JS, et al. Higher-order assessment of OCT in diabetic macular edema from the VISTA study: ellipsoid zone dynamics and the retinal fluid index. Ophthalmol Retin. 2019;3:1056–66.
Scott IU, Ip MS, VanVeldhuisen PC, Oden NL, Blodi BA, Fisher M, et al. A randomized trial comparing the efficacy and safety of intravitreal triamcinolone with standard care to treat vision loss associated with macular Edema secondary to branch retinal vein occlusion: the Standard Care vs Corticosteroid for Retinal Vein Occlusion (SCORE) study report 6. Arch Ophthalmol. 2009;127:1115–28.
Campochiaro PA, Hafiz G, Mir TA, Scott AW, Zimmer-Galler I, Shah SM, et al. Pro-permeability factors in diabetic macular edema; the diabetic macular edema treated with ozurdex trial. Am J Ophthalmol. 2016;168:13–23.
Noma H, Funatsu H, Yamasaki M, Tsukamoto H, Mimura T, Sone T, et al. Aqueous humour levels of cytokines are correlated to vitreous levels and severity of macular oedema in branch retinal vein occlusion. Eye. 2008;22:42–8.
Suzuki Y, Nakazawa M, Suzuki K, Yamazaki H, Miyagawa Y. Expression profiles of cytokines and chemokines in vitreous fluid in diabetic retinopathy and central retinal vein occlusion. Jpn J Ophthalmol. 2011;55:256–63.
Aiello LP, Avery RL, Arrigg PG, Keyt BA, Jampel HD, Shah ST, et al. Vascular endothelial growth factor in ocular fluid of patients with diabetic retinopathy and other retinal disorders. N Engl J Med. 1994;331:1480–7.
Vinores SA, Derevjanik NL, Ozaki H, Okamoto N, Campochiaro PA. Cellular mechanisms of blood-retinal barrier dysfunction in macular edema. Doc Ophthalmol Adv Ophthalmol. 1999;97:217–28.
Campochiaro PA, Wykoff CC, Shapiro H, Rubio RG, Ehrlich JS. Neutralization of vascular endothelial growth factor slows progression of retinal nonperfusion in patients with diabetic macular edema. Ophthalmology. 2014;121:1783–9.
Noma H, Mimura T, Eguchi S. Association of inflammatory factors with macular edema in branch retinal vein occlusion. JAMA Ophthalmol. 2013;131:160–5.
Funatsu H, Noma H, Mimura T, Eguchi S. Vitreous inflammatory factors and macular oedema. Br J Ophthalmol. 2012;96:302–4.
Lim JW. Intravitreal bevacizumab and cytokine levels in major and macular branch retinal vein occlusion. Ophthalmol J Int d’ophtalmologie Int J Ophthalmol Z fur Augenheilkd. 2011;225:150–4.
Matsushima R, Noma H, Yasuda K, Goto H, Shimura M. Role of cytokines in ranibizumab therapy for macular edema in patients with central retinal vein occlusion. J Ocul Pharmacol Ther. 2019;35:407–12.
Wen J, Jiang Y, Zheng X, Zhou Y. Six-month changes in cytokine levels after intravitreal bevacizumab injection for diabetic macular oedema and macular oedema due to central retinal vein occlusion. Br J Ophthalmol. 2015;99:1334–40.
Park SP, Ahn JK. Changes of aqueous vascular endothelial growth factor and pigment epithelium-derived factor following intravitreal bevacizumab for macular oedema secondary to branch retinal vein occlusion. Clin Exp Ophthalmol. 2009;37:490–5.
Funk M, Kriechbaum K, Prager F, Benesch T, Georgopoulos M, Zlabinger GJ, et al. Intraocular concentrations of growth factors and cytokines in retinal vein occlusion and the effect of therapy with bevacizumab. Investig Ophthalmol Vis Sci. 2009;50:1025–32.
Noma H, Mimura T, Yasuda K, Shimura M. Role of soluble vascular endothelial growth factor receptor signaling and other factors or cytokines in central retinal vein occlusion with macular edema. Investig Ophthalmol Vis Sci. 2015;56:1122–8.
Marek N, Raczyńska K, Siebert J, Myśliwiec M, Zorena K, Myśliwska J, et al. Decreased angiogenin concentration in vitreous and serum in proliferative diabetic retinopathy. Microvasc Res. 2011;82:1–5.
Coroniti R, Fario R, Nuno DJ, Otvos L, Scolaro L, Surmacz E. Designer leptin receptor antagonist allo-aca inhibits VEGF effects in ophthalmic neoangiogenesis models. Front Mol Biosci. 2016;3:67.
Noma H, Funatsu H, Mimura T, Harino S, Hori S. Vitreous levels of interleukin-6 and vascular endothelial growth factor in macular edema with central retinal vein occlusion. Ophthalmology. 2009;116:87–93.
Sugimoto M, Cutler A, Shen B, Moss SE, Iyengar SK, Klein R, et al. Inhibition of EGF signaling protects the diabetic retina from insulin-induced vascular leakage. Am J Pathol. 2013;183:987–95.
Kim HS, Vargas A, Eom YS, Li J, Yamamoto KL, Craft CM, et al. Tissue inhibitor of metalloproteinases 1 enhances rod survival in the rd1 mouse retina. PloS One. 2018;13:e0197322.
Baker AH, Zaltsman AB, George SJ, Newby AC. Divergent effects of tissue inhibitor of metalloproteinase-1, -2, or -3 overexpression on rat vascular smooth muscle cell invasion, proliferation, and death in vitro. TIMP-3 promotes apoptosis. J Clin Investig. 1998;101:1478–87.
Funding
Funding was in part provided by NIH/NEI K23-EY022947-01A1 (JPE).
Author information
Authors and Affiliations
Contributions
Study design: JPE, CCW; Funding: CCW, JPE; Data Acquisition: JRA, SAA, LL, HJY, CCW, JPE; Manuscript drafting: SA; Manuscript Editing/Revision: All authors; Supervision: JPE, CCW, SKS, JLR; Statistical support: MH.
Corresponding author
Ethics declarations
Competing interests
CCW has research support from the following: Adverum, Allergan, Apellis, Clearside, EyePoint, Genentech/Roch, Neurotech, Novartis, Opthea, Regeneron, Regenxbio, Samsung, Santen; is a consultant for the following: Alimera Sciences, Allegro, Allergan, Alynylam, Apellis, Bayer, Clearside, D.O.R.C., EyePoint, Genentech/Roche, Kodiak, Notal Vision, Novartis, ONL Therapeutics, PolyPhotonix, RecensMedical, Regeneron, Regenxbio, Santen; and is a speaker for Regeneron. SKS has research support from Regeneron, Allergan, and Gilead; is a consultant for Bausch and Lomb, Novartis, and Regeneron. DMB has research support from the following: Adverum, Allergan, Apellis, Clearside, Genentech/Roch, Novartis, Opthea, Regeneron, Regenxbio, Samsung, Santen; is a consultant for the following: Regeneron, Bayer, Senju, Allergan, Optos, Zeiss, Heidelberg, OHR, Biotime, Gemini, Genentech/Roche, Novartis, Apellis, Regenxbio, Chengdu Kanghong Biotechnology. JPE has research support from the following: Aerpio, Alcon, Thrombogenics/Oxurion, Regeneron, Genentech, Novartis, Allergan; is a consultant for the following: Aerpio, Alcon, Allegro, Allergan, Adverum, Genentech/Roche, Novartis, Thrombogenics/Oxurion, Leica, Zeiss, Regeneron, Stealth; and holds a patent with Leica. JRA, SA, LL, HJY, MH, JLR have no financial disclosures to report. The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arepalli, S., Wykoff, C.C., Abraham, J.R. et al. Longitudinal analysis of aqueous humour cytokine expression and OCT-based imaging biomarkers in retinal vein occlusions treated with anti-vascular endothelial growth factor therapy in the IMAGINE study. Eye 37, 1928–1935 (2023). https://doi.org/10.1038/s41433-022-02265-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02265-2