Abstract
Background/objectives
Patients undergoing maintenance hemodialysis dialysis (MHD) are at high risk of sarcopenia. Diagnosing sarcopenia requires measurement of both muscle mass and muscle function. However, few studies have rigorously evaluated the best timing for assessment. This study aimed to evaluate the changes in body composition following hemodialysis in an Asian population.
Subjects/methods
Overall, 87 MHD patients were included. Body composition was estimated using bioelectrical impedance analysis. Handgrip strength was measured using a quantitative handgrip dynamometer, and physical performance was assessed using the 6-m usual gait speed. All measurements were performed pre and post dialysis. Blood samples were collected before and after the same dialysis session.
Results
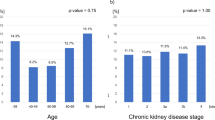
The prevalence of sarcopenia ranged from 6.9% to 18.8% pre dialysis (40–59-year group, 6.9%; 60–80-year group, 16.7%; >80-year group, 18.8%) and from 13.8% to 62.5% post dialysis. The body weight decreased from 59.32 ± 11.20 kg pre dialysis to 57.71 ± 11.05 kg post dialysis. Both the extracellular and intracellular water levels decreased post dialysis (from 14.70 ± 3.81 to 13.6 ± 2.82 L, P < 0.001, and from 21.30 ± 4.20 to 20.8 ± 4.13 L, P < 0.001, respectively). Albumin and creatinine levels were significantly lower in patients with sarcopenia. Elevated high-sensitivity C-reactive protein and interleukin-6 levels were observed in sarcopenia patients.
Conclusion
The prevalence of sarcopenia in MHD patients varies greatly according to the timing of measurements. Although predialysis measurement is preferred, it underestimates the prevalence of sarcopenia in MHD patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Change history
09 August 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41430-021-00966-7
References
Hankin JH. Development of a diet history questionnaire for studies of older persons. Am J Clin Nutr. 1989;50:1121–7.
Edwina A, Johansson L. Old age and frailty in the dialysis population. J Nephro. 2010;23:502–7.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010;39:412–23.
Noori N, Kopple JD, Kovesdy CP, Feroze U, Sim JJ, Murali SB, et al. Mid-arm muscle circumference and quality of life and survival in maintenance hemodialysis patients. Clin J Am Soc Nephrol. 2010;5:2258–68.
Pollock CA, Lloyd IS, Barry AJ, Widad A, Caterson RJ, Waugh DA, et al. Total body nitrogen as a prognostic marker in maintenance dialysis. J Am Soc Nephrol. 1995;6:82–8.
Zhu F, Levin NW. Estimation of body composition and normal fluid status using a calf bioimpedance technique. Blood Purif. 2015;39:25–31.
Davies SJ, Davenport A. The role of bioimpedance and biomarkers in helping to aid clinical decision-making of volume assessments in dialysis patients. Kidney Int. 2014;86:489–96.
Furstenberg A, Davenport A. Comparison of multifrequency bioelectrical impedance analysis and dual-energy X-ray absorptiometry assessments in outpatient hemodialysis patients. Am J Kidney Dis. 2011;57:123–9.
Furstenberg A, Davenport A. Assessment of body composition in peritoneal dialysis patients using bioelectrical impedance and dual-energy x-ray absorptiometry. Am J Nephrol. 2011;33:150–6.
Moissl UM, Wabel P, Chamney PW, Bosaeus I, Levin NW, Bosy-Westphal A, et al. Body fluid volume determination via body composition spectroscopy in health and disease. Physiol Meas. 2006;27:921–33.
Tangvoraphonkchai K, Davenport A. Changes in body composition following haemodialysis as assessed by bioimpedance spectroscopy. Eur J Clin Nutr. 2017;71:169–72.
El-Kateb S, Davenport A. Changes in intracellular water following hemodialysis treatment lead to changes in estimates of lean tissue using bioimpedance spectroscopy. Nutr Clin Pr. 2016;31:375–7.
Yang M, Zhao J, Xing L, Shi L. The association between angiotensin-converting enzyme 2 polymorphisms and essential hypertension risk: A meta-analysis involving 14,122 patients. J Renin Angiotensin Aldosterone Syst. 2015;16:1240–4.
Isoyama N, Qureshi AR, Avesani CM, Lindholm B, Barany P, Heimburger O, et al. Comparative associations of muscle mass and muscle strength with mortality in dialysis patients. Clin J Am Soc Nephrol. 2014;9:1720–8.
Kim JK, Choi SR, Choi MJ, Kim SG, Lee YK, Noh JW, et al. Prevalence of and factors associated with sarcopenia in elderly patients with end-stage renal disease. Clin Nutr. 2014;33:64–8.
Lamarca F, Carrero JJ, Rodrigues JDC, Bigogno FG, Fetter RL, Avesani CM. The prevalence of sarcopenia in elderly maitenance hemodialysis patients: the impact of different diagnosistic criteria. J Nutr Health Aging. 2014;18:710–7.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2015;16:233–70.
Chen LK, Liu LK, Woo J, Assantachai P, Auyeung TW, Bahyah KS, et al. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc. 2014;15:95–101.
Hinton BJ, Fan B, Ng BK, Shepherd JA. Dual energy X-ray absorptiometry body composition reference values of limbs and trunk from NHANES 1999-2004 with additional visualization methods. PLoS One. 2017;12:e0174180.
Baumgartner RichardN, Koehler KathleenM, Gallagher Dympna, Romero Linda, Heymstleld StevenB, Ross RobertR, et al. Epidemiology of Sarcopenia among the Elderly in New Mexico. Am J Epidemiol. 1998;147:755–63.
Chua HR, Xiang L, Chow PY, Xu H, Shen L, Lee E, et al. Quantifying acute changes in volume and nutritional status during haemodialysis using bioimpedance analysis. Nephrology. 2012;17:695–702.
Panorchan K, Nongnuch A, El-Kateb S, Goodlad C, Davenport A. Changes in muscle and fat mass with haemodialysis detected by multi-frequency bioelectrical impedance analysis. Eur J Clin Nutr. 2015;69:1109–12.
Abbas SR, Zhu F, Kaysen GA, Kotanko P, Levin NW. Effect of change in fluid distribution in segments in hemodialysis patients at different ultrafiltration rates on accuracy of whole body bioimpedance measurement. J Appl Physiol. 2014;116:1382–9.
Dahlmann A, Dorfelt K, Eicher F, Linz P, Kopp C, Mossinger I, et al. Magnetic resonance-determined sodium removal from tissue stores in hemodialysis patients. Kidney Int. 2015;87:434–41.
Cunningham JohnJ. Body composition as a determinant of energy expenditure: a synthetic review and proposed general prediction equation. Am J Clin Nutr. 1991;54:963–9.
Ravussin Eric, Bogardus Clifton. Relationship of genetics, age, and physical fitness to daily energy expenditure and fuel utilization. Am J Clin Nutr. 1989;49:968–75.
Acknowledgements
This study was supported by grants from the Project of Scientific Research Foundation of Chinese Medicine (2017ZA012) and General Project Funds from the Health Department of Zhejiang Province (2017KY213).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, M., Liu, L., Shen, X. et al. Assessing lean tissue by bioelectrical impedance analysis pre hemodialysis underestimates the prevalence of sarcopenia in maintenance hemodialysis patients. Eur J Clin Nutr 75, 1407–1413 (2021). https://doi.org/10.1038/s41430-020-00835-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-00835-9