Abstract
Background
Although prenatal iron-containing supplements have been associated with lower anemia prevalence in later pregnancy, few trials have examined the effect of supplements on the anemia status of post-partum women and their infants.
Objective
We compared the effects of folic acid alone (FA), iron-folic acid (IFA) and multiple micronutrients (MMN) when provided to pregnant women with no or mild anemia on the hemoglobin levels of post-partum women and their infants at 6 and 12 months of age. We also examined the potential modifying effect of maternal hemoglobin concentration at enrollment.
Methods
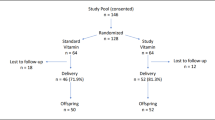
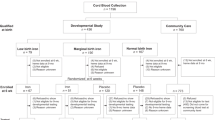
A double-blind randomized controlled trial was conducted in China; 18,775 nulliparous women with a hemoglobin concentration > 100 g/L were randomly assigned to receive daily FA (400 μg); IFA (FA, Fe 30 mg), or MMN (FA, Fe and 13 micronutrients) from before 20 gestational weeks until delivery.
Results
Compared with daily prenatal FA, supplementation with IFA or MMN did not affect the prevalence of anemia at 4–6 weeks post-partum (27.2%, 26.8%, and 26.3%, respectively). At 6 months of age, the anemia prevalence in infants was 6.9%, 6.7%, and 6.7%, respectively. Findings were similar at 12 months of age. Among both post-partum women and infants, findings were similar across all levels of hemoglobin at enrollment.
Conclusions
Compared to FA alone, prenatal IFA and MMN provided to women with no or mild anemia did not affect anemia in women post-partum or their infants regardless of baseline maternal hemoglobin concentration at enrollment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Pena-Rosas JP, De-Regil LM, Garcia-Casal MN, Dowswell T. Daily oral iron supplementation during pregnancy. Cochrane Database Syst Rev. 2015:Cd004736.
Preziosi P, Prual A, Galan P, Daouda H, Boureima H, Hercberg S. Effect of iron supplementation on the iron status of pregnant women: consequences for newborns. Am J Clin Nutr. 1997;66:1178–82.
Zhou SJ, Gibson RA, Makrides M. Routine iron supplementation in pregnancy has no effect on iron status of children at six months and four years of age. J Pediatr. 2007;151:438–40.
Siu AL. Screening for iron deficiency anemia and iron supplementation in pregnant women to improve maternal health and birth outcomes: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2015;163:529–36.
Du SF, Wang HJ, Zhang B, Zhai FY, Popkin BM. China in the period of transition from scarcity and extensive undernutrition to emerging nutrition-related non-communicable diseases, 1949-1992. Obes Rev. 2014;15(Suppl 1):8–15.
Liu JM, Mei Z, Ye R, Serdula MK, Ren A, Cogswell ME. Micronutrient supplementation and pregnancy outcomes: double-blind randomized controlled trial in China. JAMA Intern Med. 2013;173:276–82.
WHO. Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity Geneva: World Health Organization 2011 (WHO/NMH/NHD/MNM/11.1). http://www.who.int/vmnis/indicators/haemoglobin.
Eskeland B, Malterud K, Ulvik RJ, Hunskaar S. Iron supplementation in pregnancy: is less enough? A randomized, placebo controlled trial of low dose iron supplementation with and without heme iron. Acta Obstet Gynecol Scand. 1997;76:822–8.
Makrides M, Crowther CA, Gibson RA, Gibson RS, Skeaff CM. Efficacy and tolerability of low-dose iron supplements during pregnancy: a randomized controlled trial. Am J Clin Nutr. 2003;78:145–53.
Ziaei S, Mehrnia M, Faghihzadeh S. Iron status markers in nonanemic pregnant women with and without iron supplementation. Int J Gynaecol Obstet. 2008;100:130–2.
Zhang Y, Jin L, Liu JM, Ye R, Ren A. Maternal hemoglobin concentration during gestation and risk of anemia in infancy: secondary analysis of a randomized controlled trial. J Pediatr. 2016;175:106–10.e2.
Mei Z, Serdula MK, Liu JM, Flores-Ayala RC, Wang L, Ye R, et al. Iron-containing micronutrient supplementation of Chinese women with no or mild anemia during pregnancy improved iron status but did not affect perinatal anemia. J Nutr. 2014;144:943–8.
Pena-Rosas JP, De-Regil LM, Dowswell T, Viteri FE. Daily oral iron supplementation during pregnancy. Cochrane Database Syst Rev. 2012;12:Cd004736.
Acknowledgements
The study was supported by a cooperative agreement between Peking University Health Science Center and the Centers for Disease Control and Prevention.
Author contributions
MKS, JL, ZM designed the project; JL and HL conducted data collection; YZ and HL analyzed data or performed statistical analysis; MKS, YZ, and ZM wrote the paper. MKS, YZ, and ZM had primary responsibility for the final content. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Serdula, M.K., Zhou, Y., Li, H. et al. Prenatal iron containing supplements provided to Chinese women with no or mild anemia had no effect on hemoglobin concentration in post-partum women or their infants at 6 and 12 months of age. Eur J Clin Nutr 73, 1473–1479 (2019). https://doi.org/10.1038/s41430-018-0365-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-018-0365-x
This article is cited by
-
Folic Acid Affects Iron Status in Female Rats with Deficiency of These Micronutrients
Biological Trace Element Research (2020)