Abstract
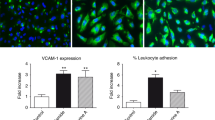
Engraftment syndrome (ES) is a common complication after autologous hematopoietic cell transplantation (auto-HCT) whose pathophysiological substrate remains unclear. We investigated whether endothelial damage could contribute to ES. Circulating ECs-damage biomarkers were measured in plasma from patients with (ES; n = 14) or without ES (non-ES; n = 20), collected at different time points: before HCT, 5 (S5) and 10 days (S10) after HCT, and at either the ES onset (SON) or the discharge day (SDIS). Also, cultured endothelial cells (ECs) were exposed to serum samples, obtained at the same points, to evaluate changes in ECs-activation (ICAM-1, VE-Cadherin) biomarkers, the reactivity of ECs towards leukocytes, and activation of intracellular signaling proteins related to inflammation (p38MAPK) and proliferation (Erk1/2). Results showed that circulating VWF, sTNFR1 and sVCAM-1 levels were higher in ES patients at all the points assessed, especially at SON. In vitro results showed an increased ICAM-1 expression on ECs exposed to ES samples vs. non-ES samples, especially to S5, with elevated leukocyte adhesion. Also, a lower VE-Cadherin expression and an increased phosphorylation of p38MAPK and Erk1/2 proteins were observed in ECs exposed to ES vs. non-ES samples. Our results indicate that endothelial activation precedes ES development and could be one of its pathophysiological substrates.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Carreras E, Fernández-Avilés F, Silva L, Guerrero M, Fernández de Larrea C, Martínez C, et al. Engraftment syndrome after auto-SCT: analysis of diagnostic criteria and risk factors in a large series from a single center. Bone Marrow Transplant. 2010;45:1417–22. https://doi.org/10.1038/bmt.2009.363.
Sheth V, Jain R, Gore A, Ghanekar A, Saikia T. Engraftment syndrome: clinical features and predictive factors in autologous stem cell transplant. Indian J Hematol Blood Transfus. 2018;34:448–53. https://doi.org/10.1007/s12288-017-0899-4.
Maiolino A, Biasoli I, Lima J, Portugal AC, Pulcheri W, Nucci M. Engraftment syndrome following autologous hematopoietic stem cell transplantation: definition of diagnostic criteria. Bone Marrow Transplant. 2003;31:393–7. https://doi.org/10.1038/sj.bmt.1703855.
Cornell RF, Hari P, Zhang MJ, Zhong X, Thompson J, Fenske TS, et al. Divergent effects of novel immunomodulatory agents and cyclophosphamide on the risk of engraftment syndrome after autologous peripheral blood stem cell transplantation for multiple myeloma. Biol Blood Marrow Transplant. 2013;19:1368–73. https://doi.org/10.1016/j.bbmt.2013.06.017.
Lee CK, Gingrich RD, Hohl RJ, Ajram KA. Engraftment syndrome in autologous bone marrow and peripheral stem cell transplantation. Bone Marrow Transplant. 1995;16:175–82.
Goldberg RB. Cytokine and cytokine-like inflammation markers, endothelial dysfunction, and imbalanced coagulation in development of diabetes and its complications. J Clin Endocrinol Metab. 2009;94:3171–82. https://doi.org/10.1210/jc.2008-2534.
Mauro AK, Khurshid N, Berdahl DM, Ampey AC, Adu D, Shah DM, et al. Cytokine concentrations direct endothelial function in pregnancy and preeclampsia. J Endocrinol. 2021;248:107–17. https://doi.org/10.1530/joe-20-0397.
Fernández S, Palomo M, Molina P, Díaz-Ricart M, Escolar G, Téllez A, et al. Progressive endothelial cell damage in correlation with sepsis severity. Defibrotide as a contender. J Thromb Haemost. 2021. https://doi.org/10.1111/jth.15343
Carreras E, Diaz-Ricart M. The role of the endothelium in the short-term complications of hematopoietic SCT. Bone Marrow Transplant. 2011;46:1495–502. https://doi.org/10.1038/bmt.2011.65.
Cordes S, Mokhtari Z, Bartosova M, Mertlitz S, Riesner K, Shi Y, et al. Endothelial damage and dysfunction in acute graft-versus-host disease. Haematologica. 2020. https://doi.org/10.3324/haematol.2020.253716
Martinez-Sanchez J, Hamelmann H, Palomo M, Mir E, Moreno-Castaño AB, Torramade S, et al. Acute graft-vs.-host disease-associated endothelial activation in vitro is prevented by defibrotide. Front Immunol. 2019;10:2339 https://doi.org/10.3389/fimmu.2019.02339.
Mir E, Palomo M, Rovira M, Pereira A, Escolar G, Penack O, et al. Endothelial damage is aggravated in acute GvHD and could predict its development. Bone Marrow Transplant. 2017;52:1317–25. https://doi.org/10.1038/bmt.2017.121.
Martinez-Sanchez J, Palomo M, Torramade-Moix S, Moreno-Castaño AB, Rovira M, Gutiérrez-García G, et al. The induction strategies administered in the treatment of multiple myeloma exhibit a deleterious effect on the endothelium. Bone Marrow Transplant. 2020;55:2270–8. https://doi.org/10.1038/s41409-020-0947-9.
Gutiérrez-García G, Rovira M, Magnano L, Rosiñol L, Bataller A, Suárez-Lledó M, et al. Innovative strategies minimize engraftment syndrome in multiple myeloma patients with novel induction therapy following autologous hematopoietic stem cell transplantation. Bone Marrow Transplant. 2018;53:1541–7. https://doi.org/10.1038/s41409-018-0189-2.
Cornell RF, Hari P, Drobyski WR. Engraftment syndrome after autologous stem cell transplantation: an update unifying the definition and management approach. Biol Blood Marrow Transplant. 2015;21:2061–8. https://doi.org/10.1016/j.bbmt.2015.08.030.
Rodríguez-Lobato LG, Martínez-Roca A, Castaño-Díez S, Palomino-Mosquera A, Gutiérrez-García G, Pedraza A, et al. The avoidance of G-CSF and the addition of prophylactic corticosteroids after autologous stem cell transplantation for multiple myeloma patients appeal for the at-home setting to reduce readmission for neutropenic fever. PLoS ONE. 2020;15:e0241778 https://doi.org/10.1371/journal.pone.0241778.
Palomo M, Diaz-Ricart M, Carbo C, Rovira M, Fernandez-Aviles F, Escolar G, et al. The release of soluble factors contributing to endothelial activation and damage after hematopoietic stem cell transplantation is not limited to the allogeneic setting and involves several pathogenic mechanisms. Biol Blood Marrow Transplant. 2009;15:537–46. https://doi.org/10.1016/j.bbmt.2009.01.013.
Palomo M, Diaz-Ricart M, Rovira M, Escolar G, Carreras E. Defibrotide prevents the activation of macrovascular and microvascular endothelia caused by soluble factors released to blood by autologous hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2011;17:497–506. https://doi.org/10.1016/j.bbmt.2010.11.019.
Schindelin J, Arganda-Carreras I, Frise E, Kaynig V, Longair M, Pietzsch T, et al. Fiji: an open-source platform for biological-image analysis. Nat Methods. 2012;9:676–82. https://doi.org/10.1038/nmeth.2019.
Sakariassen KS, Aarts PA, de Groot PG, Houdijk WP, Sixma JJ. A perfusion chamber developed to investigate platelet interaction in flowing blood with human vessel wall cells, their extracellular matrix, and purified components. J Lab Clin Med. 1983;102:522–35.
Edenfield WJ, Moores LK, Goodwin G, Lee N. An engraftment syndrome in autologous stem cell transplantation related to mononuclear cell dose. Bone Marrow Transplant. 2000;25:405–9. https://doi.org/10.1038/sj.bmt.1702155.
Takamatsu Y, Akashi K, Harada M, Teshima T, Inaba S, Shimoda K, et al. Cytokine production by peripheral blood monocytes and T cells during haemopoietic recovery after intensive chemotherapy. Br J Haematol. 1993;83:21–27. https://doi.org/10.1111/j.1365-2141.1993.tb04625.x.
Baiocchi G, Scambia G, Benedetti P, Menichella G, Testa U, Pierelli L, et al. Autologous stem cell transplantation: sequential production of hematopoietic cytokines underlying granulocyte recovery. Cancer Res. 1993;53:1297–303.
Lissoni P, Barni S, Cattaneo G, Archili C, Crispino S, Tancini G, et al. Activation of the complement system during immunotherapy of cancer with interleukin-2: a possible explanation of the capillary leak syndrome. Int J Biol Markers. 1990;5:195–7.
Downie GH, Ryan US, Hayes BA, Friedman M. Interleukin-2 directly increases albumin permeability of bovine and human vascular endothelium in vitro. Am J Respir Cell Mol Biol. 1992;7:58–65. https://doi.org/10.1165/ajrcmb/7.1.58.
Khandelwal P, Mellor-Heineke S, Rehman N, Lane A, Smiley K, Villanueva J, et al. Cytokine profile of engraftment syndrome in pediatric hematopoietic stem cell transplant recipients. Biol Blood Marrow Transplant. 2016;22:690–7. https://doi.org/10.1016/j.bbmt.2015.12.016.
Palomo M, Diaz-Ricart M, Carbo C, Rovira M, Fernandez-Aviles F, Martine C, et al. Endothelial dysfunction after hematopoietic stem cell transplantation: role of the conditioning regimen and the type of transplantation. Biol Blood Marrow Transplant. 2010;16:985–93. https://doi.org/10.1016/j.bbmt.2010.02.008.
Giannotta M, Trani M, Dejana E. VE-cadherin and endothelial adherens junctions: active guardians of vascular integrity. Dev Cell. 2013;26:441–54. https://doi.org/10.1016/j.devcel.2013.08.020.
Duong CN, Vestweber D. Mechanisms ensuring endothelial junction integrity beyond VE-cadherin. Front Physiol. 2020;11:519 https://doi.org/10.3389/fphys.2020.00519.
Dejana E, Bazzoni G, Lampugnani MG. Vascular endothelial (VE)-cadherin: only an intercellular glue? Exp Cell Res. 1999;252:13–19. https://doi.org/10.1006/excr.1999.4601.
Lampugnani MG, Dejana E, Giampietro C. Vascular endothelial (VE)-cadherin, endothelial adherens junctions, and vascular disease. Cold Spring Harb Perspect Biol. 2018;10. https://doi.org/10.1101/cshperspect.a029322
Colás-Algora N, García-Weber D, Cacho-Navas C, Barroso S, Caballero A, Ribas C, et al. Compensatory increase of VE-cadherin expression through ETS1 regulates endothelial barrier function in response to TNFα. Cell Mol Life Sci. 2020;77:2125–40. https://doi.org/10.1007/s00018-019-03260-9.
Mercado N, To Y, Kobayashi Y, Adcock IM, Barnes PJ, Ito K. p38 mitogen-activated protein kinase-γ inhibition by long-acting β2 adrenergic agonists reversed steroid insensitivity in severe asthma. Mol Pharmacol. 2011;80:1128–35. https://doi.org/10.1124/mol.111.071993.
Rogatsky I, Logan SK, Garabedian MJ. Antagonism of glucocorticoid receptor transcriptional activation by the c-Jun N-terminal kinase. Proc Natl Acad Sci USA. 1998;95:2050–5. https://doi.org/10.1073/pnas.95.5.2050.
Su JB. Vascular endothelial dysfunction and pharmacological treatment. World J Cardiol. 2015;7:719–41. https://doi.org/10.4330/wjc.v7.i11.719.
Tiurenkov IN, Voronkov AV, Slietsans AA, Volotova EV. Endothelial protection drugs-a new class of pharmacological agents. Vestn Ross Akad Med Nauk. 2012;7:50–7.
Palomo M, Mir E, Rovira M, Escolar G, Carreras E, Diaz-Ricart M. What is going on between defibrotide and endothelial cells? Snapshots reveal the hot spots of their romance. Blood. 2016;127:1719–27. https://doi.org/10.1182/blood-2015-10-676114.
Zielińska KA, Van Moortel L, Opdenakker G, De Bosscher K, Van den Steen PE. Endothelial Response to Glucocorticoids in Inflammatory Diseases. Front Immunol. 2016;7:592 https://doi.org/10.3389/fimmu.2016.00592.
Verhoeven F, Prati C, Maguin-Gaté K, Wendling D, Demougeot C. Glucocorticoids and endothelial function in inflammatory diseases: focus on rheumatoid arthritis. Arthritis Res Ther. 2016;18:258 https://doi.org/10.1186/s13075-016-1157-0.
Poterucha TJ, Libby P, Goldhaber SZ. More than an anticoagulant: Do heparins have direct anti-inflammatory effects? Thromb Haemost. 2017;117:437–44. https://doi.org/10.1160/th16-08-0620.
Acknowledgements
We would like to thank Estefanía Garcia and Lidia Martin for their technical assistance. This study was supported by Premi Fi de Residencia “Emili Letang”, Hospital Clinic Barcelona and, by German José Carreras Leukaemia Foundation (03R/ 2019) and Instituto de Salud Carlos III (FIS PI19/00888). The results from the present study were partially presented at the EBMT Annual Meeting (Frankfurt, 2019) and at the XXXVII SETH Annual Congress (Pamplona, 2021).
Author information
Authors and Affiliations
Contributions
ABMC, MP, GGG, FFA, and MDR designed the study. ABMC and TS contributed to sample collection. ABMC, MP, JMS, STM, AR, PM, MPi, PG, and LB performed the laboratory tests and analysis. ABMC and MP analyzed the clinical data and ABMC performed the statistical analysis. FFA, GE, MR, and EC contributed with interpretation of data and its correlation with the clinical setting. ABMC and MDR wrote the manuscript and all authors contributed in the editing of the final manuscript.
Corresponding author
Ethics declarations
Competing interests
ABMC has been an advisory board member for Siemens in subjects not related to the submitted work. MDR and EC have been granted by and received honoraria from Jazz Pharmaceuticals. The rest of the authors have not any conflict of interest to declare.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Moreno-Castaño, A.B., Palomo, M., Torramadé-Moix, S. et al. An endothelial proinflammatory phenotype precedes the development of the engraftment syndrome after autologous Hct. Bone Marrow Transplant 57, 721–728 (2022). https://doi.org/10.1038/s41409-022-01610-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-022-01610-z