Abstract
Background
Cyp2c70-/- mice with a human-like bile acid (BA) composition display features of neonatal cholestasis. We assessed whether perinatal ursodeoxycholic acid (UDCA) exposure prevents neonatal cholestasis in Cyp2c70-/- mice and reduces cholangiopathy development later in life.
Methods
Cyp2c70+/- males were crossed with Cyp2c70+/- females fed either a regular chow diet or a 0.1% UDCA-containing diet during breeding, gestation, and suckling. Cholestasis and liver function parameters were assessed in their Cyp2c70-/- and wild-type offspring at 3 and 8 weeks of age.
Results
Three-week-old Cyp2c70-/- pups showed features of neonatal cholestasis, including elevated plasma BAs and transaminases, which were completely prevented in Cyp2c70-/- pups upon perinatal UDCA exposure. In addition, UDCA administration to the dams corrected altered hepatic gene expression patterns in Cyp2c70-/- pups, reduced markers of fibrogenesis and inflammation, and prevented cholangiocyte proliferation. Yet, these beneficial effects of perinatal UDCA exposure were not retained into adulthood upon discontinuation of treatment.
Conclusion
Perinatal exposure of Cyp2c70-/- mice to UDCA has beneficial effects on liver function parameters, supporting a direct role of BA hydrophobicity in the development of neonatal cholestasis in these mice. However, prevention of neonatal cholestasis in Cyp2c70-/- mice has no long-lasting effects on liver pathophysiology.
Impact
-
This is the first study showing that perinatal UDCA exposure prevents features of neonatal cholestasis that are observed in mice with a human-like bile acid composition, i.e., Cyp2c70-/- mice.
-
Perinatal UDCA exposure of Cyp2c70-/- pups leads to UDCA enrichment in their circulating bile acid pool and, consequently, to a reduced hydrophobicity of biliary bile acids.
-
Perinatal UDCA exposure of Cyp2c70-/- pups has no long-lasting effects on the development of cholangiopathy after discontinuation of treatment.
-
The results in this study expand current knowledge regarding acute and long-lasting effects of UDCA treatment in early life.
Similar content being viewed by others
Introduction
Bile acids (BAs) are amphipathic molecules that are synthesized in the liver, stored in the gallbladder, and released into the intestine upon ingestion of a meal to facilitate lipid absorption. Due to their lipid-solubilizing properties, high intra- and extracellular concentrations of BAs can cause liver damage.1 BAs also act as hormones through activation of several nuclear and membrane-bound receptors and thereby modulate metabolism and immune functions.2 Elevated plasma BA concentrations are frequently observed in human newborns, without evident underlying pathological conditions.3 In most cases, BA levels decrease within two weeks without further intervention. This relatively benign phenomenon, sometimes referred to as “physiological neonatal cholestasis”, is hypothesized to be caused by an underdeveloped BA transport system.4,5,6
Cholestasis is characterized by impaired bile flow, leading to the accumulation of bile constituents, including BAs, in the liver and blood.7 In case of persisting symptoms, neonatal cholestasis can result in severe liver disease. Various underlying causes have been described, ranging from genetic defects in BA synthesis and transport enzyme systems to viral infections and blockage or malformation of bile ducts.8
Ursodeoxycholic acid (UDCA), a hydrophilic BA, is often used for the treatment of various cholestatic liver diseases.9 UDCA is proposed to improve cholestasis by stimulating bile canalicular efflux pumps as well as by reducing the hydrophobicity and, hence, the cytotoxic potential of the BA pool.10 Furthermore, UDCA is hypothesized to stimulate bicarbonate secretion from cholangiocytes, which creates an alkaline environment at the apical membrane. This so-called “bicarbonate umbrella” protects cholangiocytes from cytotoxic molecules such as hydrophobic BAs.11 In addition, UDCA is reported to have cytoprotective, anti-inflammatory, antifibrotic,12 and endoplasmic reticulum (ER) stress-reducing properties.13 UDCA is FDA-approved for the treatment of primary biliary cholangitis in adults and is applied to alleviate pruritus in pregnant women diagnosed with intrahepatic cholestasis of pregnancy.14
BA metabolism, as well as the consequences of disturbance of BA homeostasis, has been extensively studied in mouse models despite the abundant presence of specific murine BAs that are absent in humans.15 Unlike the hydrophobic BA species that are abundantly present in humans, these murine BA species, i.e., the primary α-, β- and the secondary ω-muricholic acids (MCAs), are extremely hydrophilic and have cytoprotective rather than cytotoxic effects.16,17 Furthermore, MCAs have limited capacity to promote lipid absorption and exert antagonistic activity toward the BA receptor farnesoid X receptor (FXR/NR1H4),18 which is in sharp contrast to the FXR activating BA species that are abundant in the human pool.19,20 In order to improve the translational potential of pre-clinical data to humans, mouse models with a more human-like BA composition are essential. Recently, CYP2C70 was demonstrated to be responsible for the synthesis of α- and β-MCA from chenodeoxycholic acid (CDCA).21,22 Since then, we and others have generated Cyp2c70-deficient mice that lack MCAs and, consequently, have a more hydrophobic, human-like, BA profile consisting of mainly cholic acid, CDCA, deoxycholic acid, and lithocholic acid.23,24,25
Cyp2c70-deficient mice show features of “physiological neonatal cholestasis”, characterized by very high plasma BA and transaminase levels at weaning,23 that may initiate a cascade of events that contributes to the acceleration of liver pathology in Cyp2c70-KO mice. Although plasma BA and transaminase concentrations in Cyp2c70-/- mice drop markedly between the age of 3 and 12 weeks, particularly adult female Cyp2c70-/- mice develop cholangiopathy with bridging fibrosis in adulthood that can be prevented by UDCA treatment.23 We hypothesized that UDCA exposure at an early age would prevent characteristics of neonatal cholestasis in Cyp2c70-deficient mice and thereby delay or (partly) prevent the development of liver fibrosis in later life. Therefore, we fed female Cyp2c70+/- mice a diet supplemented with 0.1% UDCA during pregnancy and suckling and evaluated parameters of cholestasis and liver pathophysiology in their Cyp2c70-/- offspring during the suckling period as well as in young-adult mice 4 weeks after they had been weaned to a non-UDCA-containing diet.
Materials and methods
Animals and diet
Cyp2c70+/- male and female mice on a C57BL/6J background (C57BL/6J-Cyp2c70em3Umcg) were used for breeding, generating wild-type (WT), Cyp2c70+/- and Cyp2c70-/- offspring, the latter having a human-like BA pool that is devoid of MCAs.23
Cyp2c70+/- dams received either normal chow (Ssniff® 1554R/M-H maintenance diet; crude protein: 19.3%, crude fat: 3.3%, crude fiber: 4.4%, crude ash: 6.0%, starch: 36.1%, sugar: 3.1%) or chow containing 0.1% UDCA (w/w) (Sigma-Aldrich, St Louis, MO). Mice had unlimited access to food and drinking water during the experiment and were housed under climate-controlled conditions (21 °C) with a 12-h light/dark cycle. Food intake was monitored during pregnancy and suckling.
Dams were between 7 and 22 weeks of age during breeding and received their diet at least 4 days prior to mating. Either one or two females were co-housed with one male for 4 consecutive day/night cycles and housed individually after the 4th night. Pregnancy was confirmed between gestational days 9.5 and 13.5. Of all included female mice in this study, 88% were pregnant after 1 or 2 rounds of mating.
At the age of 3 weeks, WT and Cyp2c70-/- offspring and their dams were sacrificed and blood and organs were collected as described below. Cyp2c70+/- offspring were excluded from this study since their phenotype is indistinguishable from WT.23 In order to determine the long-term effects of perinatal UDCA exposure, part of the offspring was weaned to a non-UDCA-containing chow diet and housed individually at the age of 4 weeks. Blood samples from the tail vein were taken at 1 and 3 weeks after weaning, thus at the age of 5 and 7 weeks, respectively, to determine plasma UDCA concentrations. At the age of 8 weeks, these mice were sacrificed by cardiac puncture under isoflurane anesthesia. The liver was excised and the large lobe was immediately fixed in 4% formalin for histology. The remainder of the liver, the small intestine, and plasma were snap-frozen in liquid nitrogen and stored at −80 °C until further analyses.
All animal experiments were executed in accordance with the Dutch law and approved by the Dutch Central Committee for Animal Experiments, as well as by the Animal Welfare Body of the University of Groningen.
Plasma parameters
Alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), and bilirubin in plasma were quantified using a Cobas 6000 analyzer with standard reagents (Roche Diagnostics, Netherlands). BAs in plasma were measured with ultra (U)HPLC-MS/MS on a Nexera X2 UHPLC system (Shimadzu, Kyoto, Japan), coupled to a SCIEX QTRAP 4500 MD triple quadrupole mass spectrometer (SCIEX, Framingham, MA) and quantified using stable isotopically labeled internal standards.23
Liver histology
Formalin-fixed paraffin-embedded liver sections (4 µm) were stained with hematoxylin and eosin to assess liver morphology. In order to visualize collagen deposition, Sirius Red/Fast Green staining was performed according to standard protocols. Cholangiocytes were stained using an anti-Cytokeratin 19 (CK19) rabbit monoclonal antibody (ab52625; Abcam, Cambridge, UK). Photomicrographic images were obtained using a Hamamatsu NanoZoomer (Hamamatsu Photonics, Almere, the Netherlands). Stained areas were quantified with Image J software26 and expressed as a percentage of the total image field.
Hepatic gene expression
Snap-frozen livers were ground and total RNA was isolated by TRI-Reagent (Sigma-Aldrich, St. Louis, MO) according to the manufacturer’s protocol. RNA was reverse-transcribed using Moloney Murine Leukemia Virus Reverse Transcriptase (Life Technologies, Bleiswijk, The Netherlands) and Random Nonamers (Sigma-Aldrich). Real-time quantitative PCR was performed on a QuantStudio-3 system (Applied Biosystems, Foster City, CA) using TaqMan primer-probe combinations. Relative gene expression levels were calculated based on a dilution curve. All gene expression levels were normalized to 18S and further normalized to the average expression of WT pups from chow-fed dams, which served as the reference group for the 3-week-old mice. Female WT offspring from chow-fed dams served as the reference group in 8-week-old mice.
Statistical analyses
Statistical analyses between two groups were performed by Mann–Whitney U tests (GraphPad Software, San Diego, CA, version 8). Multiple comparisons were analyzed using the Kruskal–Wallis H test, followed by Conover post hoc comparisons with Brightstat online software.27 Differences were considered statistically significant when p values were <0.05.
Results
UDCA treatment of dams does not affect litter size and body weight of their offspring
In order to determine whether macronutrient intake during pregnancy and suckling differed between dams fed a regular chow diet or a chow diet supplemented with 0.1% UDCA, we monitored their food intake over time. Since dams with larger litters need more nutrients to provide sufficient energy for their pups, we evaluated the food intake of 15 dams on the chow diet and 18 dams on UDCA diet with a similar average litter size of 6.7 and 6.5 pups per litter, respectively, varying between 2 and 9 pups per litter in both diet groups (Fig. 1a).
a Litter sizes in the different treatment groups. b Cumulative food intake during pregnancy (19 days) and suckling (21 days) on either chow diet (n = 15) or UDCA diet (n = 18). c Body weights and d liver weights of 3-week-old WT and Cyp2c70-/- pups of chow-fed and UDCA-fed dams. Dots (a, c, and d) represent individual values with mean and SD, whereas lines (b) represent mean values per diet group with SD.
Over the course of the experiment, the cumulative food intake during pregnancy and suckling was similar between chow- and UDCA-fed dams (Fig. 1b). In both groups, food intake during pregnancy remained relatively stable with an average of ~5.5 g/day (data not shown). After delivery, food intake of dams increased in both groups to peak at 2 weeks postpartum and gradually decreased thereafter. No significant differences were found in daily food intake between the diet groups. These results indicate that any differences found between pups from dams of either diet group are not caused by differences in macronutrient intake and are therefore most likely directly related to UDCA exposure.
WT and Cyp2c70-/- pups from chow-fed as well as from UDCA-fed dams were sacrificed at the age of 3 weeks to assess the effects of perinatal UDCA treatment on features of neonatal cholestasis and liver pathophysiology. Genotypes of pups were according to normal Mendelian distribution in both diet groups (data not shown). The heterozygous offspring, accounting for ~50% of pups, was not included in the study because Cyp2c70+/- mice have previously been shown to be phenotypically indistinguishable from WT.23 There were no differences between sexes within the 4 groups for any of the parameters that were determined at the age of 3 weeks. Therefore, in the results discussed below, data of males and females were combined for offspring from the same treatment groups and genotypes. Importantly, no differences were found in body weights (Fig. 1c) and liver weights (Fig. 1d) between WT and Cyp2c70-/- pups or between pups from chow-fed dams and UDCA-fed dams at this age.
Features of neonatal cholestasis in 3-week-old Cyp2c70 -/- pups are prevented by the addition of UDCA to the diet of their dams
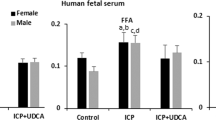
In line with previous observations,23 newborn Cyp2c70-/- mice displayed features of neonatal cholestasis. Cyp2c70-/- mice of 3 weeks old showed significantly higher total BA levels in plasma than WT mice of the same age (Fig. 2a). However, when their dams were fed the UDCA-containing diet, plasma BAs in their Cyp2c70-/- pups were reduced to normal levels, i.e., concentrations were comparable to those found in WT pups. The percentages of UDCA as part of total BAs in plasma and bile were increased in pups from UDCA-fed dams as compared to pups from chow-fed dams, with averages of 24.7% (WT) and 36.8% (Cyp2c70-/-) in plasma (Fig. 2b) and 19.7% (WT) and 33.6% (Cyp2c70-/-) in bile (Fig. 2c), while UDCA constituted <5% of BAs in plasma and bile of pups from chow-fed dams. No significant differences were observed in the ratio of conjugated versus unconjugated BAs in plasma (Fig. 2d). In addition to high BA levels, 3-week-old Cyp2c70-/- mice showed markedly increased transaminase levels, indicating liver damage. Plasma AST and ALT (Fig. 2e, f), as well as ALP (Supplementary Fig. S1a), were significantly increased in Cyp2c70-/- pups compared to WT. Interestingly, plasma transaminase levels in Cyp2c70-/- pups from UDCA-fed dams were strongly decreased compared to Cyp2c70-/- pups from chow-fed dams though still somewhat higher than in WT pups, whereas ALP levels were normalized. Plasma bilirubin levels displayed a similar pattern although with substantial variation in Cyp2c70-/- pups from chow-fed dams (Supplementary Fig. S1b). The improved liver function parameters in Cyp2c70-/- pups from UDCA-fed dams coincided with reduced hydrophobicity of their biliary BAs as compared to Cyp2c70-/- pups from chow-fed dams. However, the hydrophobicity index was still higher in Cyp2c70-/- pups from UDCA-fed dams than in WT pups from dams that were either fed chow or the UDCA-supplemented diet (Fig. 2g).
a Total plasma BA levels in 3-week-old pups. b Composition of total BAs in plasma and c bile. d Percentage of conjugated and unconjugated BAs in plasma. e Plasma AST and f ALT levels. g Hydrophobicity index of biliary BAs. Dots represent individual values with mean and SD. *P < 0.05 using Kruskal–Wallis H test followed by Conover post hoc comparisons. ALT alanine aminotransferase, AST aspartate aminotransferase, BA bile acids, conj conjugated BAs, unconj unconjugated BAs.
Perinatal UDCA exposure corrects dysregulated expression of genes encoding BA transporters and synthesis enzymes and reduces hepatic expression of pro-inflammatory cytokines
In order to evaluate whether perinatal UDCA exposure affects BA homeostasis or inflammation, we assessed the expression patterns of BA-related genes and pro-inflammatory cytokines in the pups. Cyp2c70-/- pups from chow-fed dams possess a more hydrophobic BA pool containing potent FXR agonists, including CDCA, which may lead to altered expression of FXR-controlled genes. However, the expression of the FXR target small heterodimer partner (Shp/Nr0b2) remained unchanged in pups from all groups (Fig. 3a), while the expression of Fxr (Nr1h4) itself was decreased in Cyp2c70-/- pups from chow-fed dams compared to their WT littermates and was restored to normal levels upon addition of UDCA to the diet of their dams.
Next, gene expression of BA synthesis enzymes catalyzing key steps in the classic (Cyp7a1, Cyp8b1) and the alternative (Cyp27a1, Cyp7b1) pathway was measured (Fig. 3b). Despite a decrease in Fxr and similar Shp expression, Cyp2c70-/- pups from chow-fed dams showed decreased expression of all measured BA synthesis genes. Expression levels of Cyp7a1, Cyp8b1, and Cyp7b1 were partially restored in Cyp2c70-/- pups from UDCA-fed dams, while the expression of Cyp27a1 was completely normalized.
Furthermore, hepatic mRNA expression of transporters that mediate uptake of BAs from the portal vein into the hepatocytes (Ntcp/Slc10a1 and Oatp1/Slco1a1), as well as expression of transporters that export BAs from hepatocytes into the bile (Bsep/Abcb11 and Mrp2/Abcc2) was measured (Fig. 3c). No differences in Oatp1 expression were present. However, compared to their WT littermates, the expression of Ntcp was significantly decreased in Cyp2c70-/- pups from chow-fed dams, while its expression was restored in Cyp2c70-/- pups from UDCA-fed dams. Similarly, compared to WT, Mrp2 and Bsep transcripts were decreased and tended to decrease, respectively, in Cyp2c70-/- pups from chow-fed dams and were restored in Cyp2c70-/- pups from UDCA-fed dams. These findings suggest an overall improvement of the capacity to transport BAs from the portal vein into the bile in Cyp2c70-/- pups from UDCA-fed dams as compared to Cyp2c70-/- pups from dams that did not receive treatment.
In addition, we investigated the potential involvement of inflammatory pathways and ER stress in UDCA-associated improvement of liver function. Expression of macrophage marker F4/80 (Adgre1) and the inflammation markers Tnfα and monocyte attractant protein Mcp1 (Ccl2) was significantly increased in Cyp2c70-/- pups from chow-fed dams and was normalized in Cyp2c70-/- pups from UDCA-fed dams (Fig. 3d), whereas expression of T-cell marker Cd3e remained unaffected in all groups. Moreover, no significant differences in the expression of ER stress markers Bip (Hspa5) and Dnajc3 (Hsp40) were observed between the groups (Fig. 3e).
Perinatal UDCA exposure prevents cholangiopathy in Cyp2c70 -/- pups
Next, we evaluated markers of fibrogenesis and ductular reactions. Hepatic expression of collagen type I alpha-1 (Col1a1) was substantially increased in Cyp2c70-/- pups from chow-fed dams as compared to WT pups (Fig. 4a), indicating augmented fibrogenesis in these pups. Hepatic Col1a1 expression levels in Cyp2c70-/- pups from UDCA-fed dams were restored, but remained significantly elevated compared to WT pups. Moreover, hepatic mRNA expression of the cholangiocyte marker keratin-19 (Krt19, encoding the cholangiocyte marker CK19) was significantly increased in Cyp2c70-/- pups from chow-fed dams and completely normalized in pups from UDCA-fed dams (Fig. 4b). Histological quantification confirmed an increase in CK19-positive cells in Cyp2c70-/- pups from chow-fed dams compared to WT, which tended to be reduced in Cyp2c70-/- pups from dams fed the UDCA-containing diet (Fig. 4c, d). Only limited collagen deposition was observed in these 3-week-old pups, without significant differences between the groups (Fig. 4c, e). No differences in overall liver morphology were evident between Cyp2c70-/- pups from chow- and UDCA-fed dams (Fig. 4c).
Hepatic mRNA expression levels of a Col1a1 and b Krt19 in 3-week-old pups. c Representative histological photomicrographs of livers stained with hematoxylin and eosin (H&E), Sirius Red/Fast Green, and anti-CK19. Quantification of d CK19 positively stained areas and e collagen deposition in livers of the 3-week-old pups. Bars represent 200 µm. *P < 0.05 using Kruskal–Wallis H test followed by Conover post hoc comparisons.
In summary, the combined data obtained from 3-week-old pups demonstrate that perinatal exposure to UDCA prevents the development of liver injury in Cyp2c70-/- mice at this age.
Perinatal UDCA exposure does not confer long-lasting protection from liver pathology in Cyp2c70 -/- mice
To investigate potential long-lasting beneficial effects of UDCA exposure early in life, WT and Cyp2c70-/- pups from chow- and UDCA-fed dams were weaned to a non-UDCA-containing diet and housed individually at the age of 4 weeks. In order to determine the time window in which the additional UDCA is cleared from the circulating BA pool in pups from UDCA-fed dams, UDCA levels in plasma were determined at multiple timepoints after weaning. Already one week after weaning, the amounts of UDCA in plasma of Cyp2c70-/- pups from UDCA-fed dams had dropped to levels that were fairly comparable to those found in pups from chow-fed dams, indicating that UDCA is cleared from the enterohepatic circulation within days after discontinuation of treatment. After that, the levels of UDCA remained relatively stable (Fig. 5).
Based on the relatively rapid clearance of UDCA from the BA pool of the pups after weaning, it was decided to study the long-lasting effects of perinatal UDCA treatment at the age of 8 weeks. For all parameters described below, males and females were analyzed separately, since sex has been shown to impact liver pathophysiology in Cyp2c70-/- mice.23 No major differences in body weight development from 4 until 8 weeks of age were observed between the groups (Fig. 6a and Supplementary Fig. S2). Liver weights were significantly increased in male and female Cyp2c70-/- mice compared to WT. However, no effect of perinatal UDCA treatment was observed at this age (Fig. 6b). Hepatic expression of genes encoding BA transporters and BA synthesis enzymes in Cyp2c70-/- offspring of chow-fed dams and UDCA-fed dams was similar (Fig. 6c). Total plasma BA concentrations were significantly increased in female but not in male Cyp2c70-/- mice compared to WT littermates, yet were comparable in Cyp2c70-/- offspring that had been perinatally exposed to UDCA and in offspring that had not been exposed to UDCA (Fig. 6d). Transaminase levels in plasma were significantly increased in both male and female Cyp2c70-/- compared to WT offspring (Fig. 6e, f), but no effects of perinatal UDCA exposure were detected. Finally, no changes in hepatic collagen deposition, CK19-positive cells, or liver morphology were observed between offspring of chow-fed or UDCA-fed dams (data not shown).
a Body weights and b liver weights of 8-week-old WT and Cyp2c70-/- offspring from chow- and UDCA-fed dams. c Hepatic gene expression levels of Cyp2c70-/- offspring from chow- and UDCA-fed dams. Only Cyp2c70-/- mice are shown, and expression of female WT offspring from chow-fed dams was used as a reference group, see the dotted line. d Total BA concentrations, e AST, and f ALT levels in the plasma of Cyp2c70-/- offspring from chow- and UDCA-fed dams. For panels a, b, d, e, and f, dots represent individual values with mean and SD, while only mean and SD are depicted in panel c. *P < 0.05 using Kruskal–Wallis H test followed by Conover post hoc comparisons. ALT alanine aminotransferase, AST aspartate aminotransferase, BA bile acids.
Taken together, although perinatal exposure to UDCA conferred protection from hypercholemia and cholangiopathy in 3-week-old Cyp2c70-/- pups, livers of Cyp2c70-/- offspring of UDCA-fed dams were phenotypically indistinguishable from offspring of untreated dams by the age of 8 weeks. These findings indicate that perinatal UDCA exposure does not translate into long-lasting effects on liver pathophysiology in these mice after discontinuation of the treatment.
Discussion
Cyp2c70-/- mice that are devoid of mouse/rat-specific MCAs show features of neonatal cholestasis, including elevated plasma BAs and transaminases.23 In the current study, we show that the addition of UDCA to the diet of dams during gestation and lactation prevents elevation of plasma BAs and transaminases in their 3-week-old Cyp2c70-/- offspring. However, perinatal exposure to UDCA did not confer long-lasting protection against the development of liver pathology in Cyp2c70-/- offspring after discontinuation of treatment.
Even though BAs are not required for lipid uptake in the human fetus, development of the BA synthesis and transport systems starts during fetal development.28,29 After delivery, the activities of these systems rapidly increase in both humans and murine newborns.30,31 Similar to adults, the primary BAs CA and CDCA are synthesized in fetal hepatocytes. However, differences in BA synthesis between fetuses, newborns, and adults do exist. The classical BA synthesis pathway produces most primary BAs in human adults, while in fetuses a significant contribution of the “Yamasaki pathway” has been postulated.29 BA synthesis via this pathway mainly produces CDCA, with 3β,7α-dihydroxy-5-cholenoic acid as an intermediate.32 In addition, unusual BA species, such as 1β- and 6α-hydroxylated BAs, have been found in the BA pool of human fetuses and newborns.28,33 It is currently unknown whether these BAs fulfill specific functions. Recently, it was described that BAs drive the gut microbiota maturation,34 underlining the important role of BAs during early development. Lastly, while BAs are mainly conjugated to glycine in human adults, taurine conjugation predominates in fetuses and newborns.28,35,36
In humans, fetal BAs are exported through the placenta in order to be cleared from the circulation by the maternal liver.37,38,39 Vice versa, it has been reported that BAs from the maternal serum cross the placenta and end up in the circulation of the fetus.37 Transporters from the MRP-, ABC- and OATP families have been identified in the placenta and have been proposed to be involved in BA transport between mother and fetus.37,40 We did not quantify UDCA levels in the fetuses in the current study, but in vitro studies have shown that UDCA can be transported across the placenta bidirectionally.41 It is therefore conceivable that UDCA treatment of the dams during gestation leads to elevated concentrations of UDCA in the circulation and livers of Cyp2c70-/- fetuses.
It has been described that fetal exposure to high BA levels leads to a higher risk of developing metabolic disease in later life, including obesity, increased hepatic inflammatory responses, and insulin resistance.42 Studies showed that UDCA treatment during pregnancy can prevent this predisposition effect in both human and animal models.43,44,45 Intriguingly, in a study by Pataia et al., even offspring of male mice with cholestasis were shown to be more susceptible to adiposity-related metabolic diseases in later life, which could be prevented by UDCA treatment of the father.46 Several studies in humans have evaluated the efficacy of UDCA treatment during pregnancy and report that UDCA is safe for the offspring without any adverse effects in later life.47,48 Data on the effects of UDCA treatment in newborns with neonatal cholestasis have been less conclusive.49,50 In the current study, we show that perinatal exposure to UDCA had beneficial effects on features of cholestasis and liver pathology in 3-week-old Cyp2c70-/- mice. Prophylactic UDCA administration may be beneficial for neonates that are at risk of developing cholestasis, such as preterm neonates that receive parenteral nutrition (PN). Long-term PN is applied in extreme preterm neonates and in neonates that cannot receive enteral nutrition due to illness or surgery. PN is associated with an increased risk of developing cholestasis, i.e., parenteral nutrition-associated cholestasis (PNAC), which in turn is associated with an increased risk of complications and mortality.51 However, the effects of UDCA administration on PNAC in preterm infants have been studied mainly in small cohorts and are therefore incompletely established.52,53,54 Furthermore, as discussed above, exposure to high BA levels early in life is associated with an increased risk of developing metabolic diseases in later life.42 Prevention of PNAC by UDCA in preterm neonates might therefore reduce the risk of metabolic diseases in later life. However, the metabolic consequences of perinatal UDCA treatment were not investigated in the current study.
In our study, we did not find any indications of long-lasting effects of perinatal exposure to UDCA. However, it may be that UDCA has long-term effects on parameters that were not measured in this study, e.g., metabolic parameters.
In this study, dams received UDCA not only during gestation but also during the lactation period. Milk production in dams peaks when their pups are around 2 weeks of age and it has been shown that BAs are transported from the blood into milk via BA transporters in the mammary glands.55,56 BAs can be detected in human milk, but there is no evidence of naturally occurring UDCA in milk.57 Yet, UDCA could be detected in the milk of mothers treated with UDCA during their pregnancy,58 indicating that UDCA can indeed be transported from the blood into milk. These findings support the notion that UDCA-fed dams in the current study transfer UDCA to their pups via milk during the suckling period. Since pups gradually start consuming solid food from approximately 2 weeks of age onwards, pups from UDCA-fed dams may have ingested some additional UDCA directly via the diet.
Despite high plasma concentrations of the strong FXR agonist CDCA in Cyp2c70-/- pups, the current study shows no effect of Cyp2c70-deficiency on the expression of its direct target genes Shp and Bsep in the liver. Nevertheless, hepatic mRNA levels of BA synthesis enzymes, including those of the rate-controlling enzyme Cyp7a1, are decreased in Cyp2c70-/- pups, suggesting inhibition of BA synthesis via mechanisms other than FXR signaling. Instead, inhibition of the expression of BA synthesis enzymes as well as the BA importer Ntcp in 3-week-old Cyp2c70-/- pups, might be driven by inflammatory pathways. Pro-inflammatory cytokines have been shown to decrease CYP7A1 expression in human primary hepatocytes59 and to decrease Ntcp expression in primary rat hepatocytes.60 In our study, we observed a substantially decreased expression of pro-inflammatory cytokines in livers of Cyp2c70-/- pups from UDCA-fed dams compared to those originating from dams fed regular chow, which coincided with normalization of the expression of BA synthesis enzymes and Ntcp. Taken together, these findings suggest a direct role for inflammatory signaling pathways in the development of neonatal cholestasis in Cyp2c70-/- pups, which can be modulated by UDCA. The absence of clear FXR activation in Cyp2c70-/- mice, despite the high abundance of CDCA in the BA pool of these mice, can possibly be explained by the relatively low sensitivity of murine FXR for CDCA as compared to human FXR,61 underscoring the presence of substantial differences between FXR signaling in humans and mice.
In conclusion, in the current study we show that the addition of UDCA to the diet of the dams during gestation and suckling leads to the incorporation of UDCA into the circulating BA pool of Cyp2c70-/- pups, leading to a considerably more hydrophilic composition. The increased hydrophilicity conceivably effectively counteracts the impact of high concentrations of hydrophobic BAs like CDCA on liver function in Cyp2c70-/- pups, while anti-inflammatory effects of UDCA likely also contribute to the improvements of liver physiology upon perinatal exposure in these mice. Despite the robust direct effects on neonatal cholestasis and liver pathology in the suckling pups, the effects of perinatal UDCA exposure are not maintained after discontinuation of treatment.
Data availability
All data generated or analyzed during this study are included in this published article.
References
Chiang, J. Y. L. Regulation of bile acid synthesis. Front. Biosci. 3, d176–d193 (1998).
Kuipers, F., Bloks, V. & Groen, A. Beyond intestinal soap-bile acids in metabolic control. Nat. Publ. Gr. 10, 488–498 (2014).
Suchy, F. J., Balistreri, W. F., Heubi, J. E., Searcy, J. E. & Levin, R. S. Physiologic cholestasis: elevation of the primary serum bile acid concentrations in normal infants. Gastroenterology 80, 1037–1041 (1981).
Suchy, F. J. Neonatal cholestasis. Pediatr. Rev. 25, 388–396 (2004).
Colombo, C. et al. Correlation between fetal and maternal serum bile acid concentration. Pediatr. Res. 19, 227–231 (1985).
Grijalva, J. & Vakili, K. Neonatal liver physiology. Semin. Pediatr. Surg. 22, 185–189 (2013).
Feldman, A. G. & Sokol, R. J. Neonatal cholestasis. Neoreviews 14, 10.1542/neo.14-2-e63 (2013).
Feldman, A. G. & Sokol, R. J. Recent developments in diagnostics and treatment of neonatal cholestasis. Semin. Pediatr. Surg. 29, 150945 (2020).
Cabrera, D., Arab, J. P. & Arrese, M. UDCA, NorUDCA, and TUDCA in liver diseases: a review of their mechanisms of action and clinical applications. In Fiorucci, S. & Distrutti, E. (ed.), Handbook of Experimental Pharmacology 256 237–264 (Springer, Cham, 2019).
Beuers, U. Drug insight: mechanisms and sites of action of ursodeoxycholic acid in cholestasis. Nat. Clin. Pract. Gastroenterol. Hepatol. 3, 318–328 (2006).
Beuers, U., Trauner, M., Jansen, P. & Poupon, R. New paradigms in the treatment of hepatic cholestasis: from UDCA to FXR, PXR and beyond. J. Hepatol. 62, S25–S37 (2015).
Paumgartner, G. & Beuers, U. Ursodeoxycholic acid in cholestatic liver disease: mechanisms of action and therapeutic use revisited. Hepatology 36, 525–531 (2002).
Xie, Q. et al. Effect of tauroursodeoxycholic acid on endoplasmic reticulum stress-induced caspase-12 activation. Hepatology 36, 592–601 (2002).
Kong, X., Kong, Y., Zhang, F., Wang, T. & Yan, J. Evaluating the effectiveness and safety of ursodeoxycholic acid in treatment of intrahepatic cholestasis of pregnancy: a meta-analysis (a prisma-compliant study). Medicine (Baltimore) 95, e4949 (2016).
Hofmann, A. F. & Hagey, L. R. Key discoveries in bile acid chemistry and biology and their clinical applications: history of the last eight decades. J. Lipid Res. 55, 1553–1595 (2014).
Denk, G. U. et al. Tauro-β-muricholic acid restricts bile acid-induced hepatocellular apoptosis by preserving the mitochondrial membrane potential. Biochem. Biophys. Res. Commun. 424, 758–764 (2012).
Heuman, D. M. Quantitative estimation of the hydrophilic-hydrophobic balance of mixed bile salt solutions. J. Lipid Res. 30, 719–730 (1989).
Sayin, S. I. et al. Gut microbiota regulates bile acid metabolism by reducing the levels of tauro-beta-muricholic acid, a naturally occurring FXR antagonist. Cell Metab. 17, 225–235 (2013).
Wang, H., Chen, J., Hollister, K., Sowers, L. C. & Forman, B. M. Endogenous bile acids are ligands for the nuclear receptor FXR/BAR. Mol. Cell 3, 543–553 (1999).
Parks, D. J. et al. Bile acids: natural ligands for an orphan nuclear receptor. Science 284, 1365–1368 (1999).
Takahashi, S. et al. Cyp2c70 is responsible for the species difference in bile acid metabolism between mice and humans. J. Lipid Res. 57, 2130–2137 (2016).
De Boer, J. F. et al. A human-like bile acid pool induced by deletion of hepatic Cyp2c70 modulates effects of FXR activation in mice. J. Lipid Res. 61, 291–305 (2020).
de Boer, J. F. et al. Cholangiopathy and biliary fibrosis in Cyp2c70-deficient mice are fully reversed by ursodeoxycholic acid. Cell Mol. Gastroenterol. Hepatol. 11, 1045–1069 (2021).
Honda, A. et al. Regulation of bile acid metabolism in mouse models with hydrophobic bile acid composition. J. Lipid Res. 61, 54–69 (2020).
Straniero, S. et al. Of mice and men: murine bile acids explain species differences in the regulation of bile acid and cholesterol metabolism. J. Lipid Res. 61, 480–491 (2020).
Schneider, C. A., Rasband, W. S. & Eliceiri, K. W. NIH Image to ImageJ: 25 years of image analysis. Nat. Methods 9, 671–675 (2012).
Stricker D. BrightStat.com: free statistics online. Comput. Methods Prog. Biomed. 92, 135–143 (2008).
Setchell, K. D. R., Dumaswala, R., Colombo, C. & Ronchi, M. Hepatic bile acid metabolism during early development revealed from the analysis of human fetal gallbladder bile. J. Biol. Chem. 263, 16637–16644 (1988).
Nakagawa, M. & Setchell, K. D. R. Bile acid metabolism in early life: studies of amniotic fluid. J. Lipid Res. 31, 1089–1098 (1990).
Balistreri, W. F., Heubi, J. E. & Suchy, F. J. Immaturity of the enterohepatic circulation in early life. J. Pediatr. Gastroenterol. Nutr. 2, 346–354 (1983).
Yue Cui, J. et al. Bile acids via FXR initiate the expression of major transporters involved in the enterohepatic circulation of bile acids in newborn mice. Am. J. Physiol. Gastroin-test. Liver Physiol. 302, 979–996 (2012).
Yamasaki, K. Alternative biogenetic pathways of C24-bile acids with special reference to chenodeoxycholic acid. Kawasaki Med. J. 4, 227–264 (1978).
Kimura, A. et al. Profile of urinary bile acids in infants and children: developmental pattern of excretion of unsaturated ketonic bile acids and 7 β-hydroxylated bile acids. Pediatr. Res. 45, 603–609 (1999).
van Best, N. et al. Bile acids drive the newborn’s gut microbiota maturation. Nat. Commun. 11, 3692 (2020).
Itoh, S. & Onishi, S. Hepatic taurine, glycine and individual bile acids in early human fetus. Early Hum. Dev. 57, 71–77 (2000).
Zöhrer, E. et al. Serum bile acids in term and preterm neonates: a case–control study determining reference values and the influence of early-onset sepsis. Medicine (Baltimore). 95, e5219 (2016).
McIlvride, S., Dixon, P. H. & Williamson, C. Bile acids and gestation. Mol. Asp. Med. 56, 90–100 (2017).
Dumaswala, R., Setchell, K. D. R., Moyer, M. S. & Suchy, F. J. An anion exchanger mediates bile acid transport across the placental microvillous membrane. Am. J. Physiol. 264, G1016–23 (1993).
Macias, R. I. R. et al. Effect of maternal cholestasis on bile acid transfer across the rat placenta-maternal liver tandem. Hepatology 31, 975–983 (2000).
Patel, P. et al. Semi quantitative expression analysis of MDR3, FIC1, BSEP, OATP-A, OATP-C,OATP-D, OATP-E and NTCP gene transcripts in 1st and 3rd trimester human placenta. Placenta 24, 39–44 (2003).
Xia, Y., Dong, Y., Zhao, X., Di, L. & Li, J. Transport mechanism of ursodeoxycholic acid in human placental BeWo cells. Biopharm. Drug Dispos. 39, 335–343 (2018).
Papacleovoulou, G. et al. Maternal cholestasis during pregnancy programs metabolic disease in offspring. J. Clin. Invest. 123, 3172–3181 (2013).
Borges Manna, L. et al. Ursodeoxycholic acid improves feto-placental and offspring metabolic outcomes in hypercholanemic pregnancy. Sci. Rep. 10, 1–14 (2020).
Macias, R. I. R. et al. Long-term effect of treating pregnant rats with ursodeoxycholic acid on the congenital impairment of bile secretion induced in the pups by maternal cholestasis. J. Pharmacol. Exp. Ther. 312, 751–758 (2005).
Bacq, Y. et al. Efficacy of ursodeoxycholic acid in treating intrahepatic cholestasis of pregnancy: a meta-analysis. Gastroenterology 143, 1492–1501 (2012).
Pataia, V. et al. Paternal cholestasis exacerbates obesity-associated hypertension in male offspring but is prevented by paternal ursodeoxycholic acid treatment. Int. J. Obes. 43, 319–330 (2019).
Chappell, L. C. et al. Ursodeoxycholic acid versus placebo in women with intrahepatic cholestasis of pregnancy (PITCHES): a randomised controlled trial. Lancet 394, 849–860 (2019).
Zapata, R. et al. Ursodeoxycholic acid in the treatment of intrahepatic cholestasis of pregnancy. A 12-year experience. Liver Int. 25, 548–554 (2005).
Catzola, A. & Vajro, P. Management options for cholestatic liver disease in children. Expert Rev. Gastroenterol. Hepatol. 11, 1019–1030 (2017).
Kotb, M. A. et al. Ursodeoxycholic acid use is associated with significant risk of morbidity and mortality in infants with cholestasis: a strobe compliant study. Medicine (Baltimore) 99, 1–7 (2020).
Lee, H. H., Jung, J. M., Nam, S. H., Lim, G. & Chung, M. L. Risk factor analysis of parenteral nutrition-associated cholestasis in extremely low birth weight infants. Acta Paediatr. 105, e313–e319 (2016).
Liu, S. Y. et al. Ursodeoxycholic acid prevention on cholestasis associated with total parenteral nutrition in preterm infants: a randomized trial. World J. Pediatr. 18, 100–108 (2022).
Simić, D. et al. Preventive effect of ursodeoxycholic acid on parenteral nutrition-associated liver disease in infants. Srp. Arh. Celok. Lek. 142, 184–188 (2014).
Arslanoglu, S., Moro, G. E., Tauschel, H. D. & Boehm, G. Ursodeoxycholic acid treatment in preterm infants: a pilot study for the prevention of cholestasis associated with total parenteral nutrition. J. Pediatr. Gastroenterol. Nutr. 46, 228–231 (2008).
Jara-Almonte, M. & White, J. M. Milk production in laboratory mice. J. Dairy Sci. 55, 1502–1505 (1972).
Blazquez, A. M. G. et al. Lactation during cholestasis: Role of ABC proteins in bile acid traffic across the mammary gland. Sci. Rep. 7, 7475 (2017).
Forsyth, J. S., Donnet, L. & Ross, P. E. A study of the relationship between bile salts, bile salt-stimulated lipase, and free fatty acids in breast milk: normal infants and those with breast milk jaundice. J. Pediatr. Gastroenterol. Nutr. 11, 205–210 (1990).
Brites, D. & Rodriguez, C. M. P. Elevated levels of bile acids in colostrum of patients with cholestasis of pregnancy are decreased following ursodeoxycholic acid therapy. J. Hepatol. 29, 743–751 (1998).
Li, T., Jahan, A. & Chiang, J. Y. L. Bile acids and cytokines inhibit the human cholesterol 7α-hydroxylase gene via the JNK/c-Jun pathway. Hepatology 43, 1202 (2006).
Sturm, E. et al. Endotoxin-stimulated macrophages decrease bile acid uptake in WIF-B cells, a rat hepatoma hybrid cell line. Hepatology 31, 124–130 (2000).
Cui, J. et al. The amino acid residues asparagine 354 and isoleucine 372 of human farnesoid X receptor confer the receptor with high sensitivity to chenodeoxycholate. J. Biol. Chem. 277, 25963–25969 (2002).
Acknowledgements
The authors thank Rick Havinga for expert technical assistance during experiments.
Funding
H.D.d.V. is supported by the PhD program of Campus Fryslân, University of Groningen, and Medical Center Leeuwarden. A.P. is supported by the European Union’s Horizon 2020 research and innovation program under the Marie Skłodowska-Curie grant agreement no. 754425. R.L. is supported by China Scholarship Council (no. 201806100216). F.K. is supported by the Netherlands Heart Foundation (IN CONTROL, CVON2018-27) and the Noaber Foundation (Lunteren, the Netherlands). J.F.d.B. is supported by the Nutrition and Health initiative of the University of Groningen.
Author information
Authors and Affiliations
Contributions
H.D.d.V., V.W.B., F.K., and J.F.d.B. contributed to conceptualization and design; H.D.d.V., A.P., R.L., M.V.H., V.W.B., N.L.M., and M.K. contributed to the acquisition and analysis of data; all authors contributed to the interpretation of data; H.D.d.V. drafted the article; T.v.Z., J.F.d.B., and F.K. critically revised the article; all authors approved the final version for publication.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
de Vries, H.D., Palmiotti, A., Li, R. et al. Perinatal exposure to UDCA prevents neonatal cholestasis in Cyp2c70-/- mice with human-like bile acids. Pediatr Res 93, 1582–1590 (2023). https://doi.org/10.1038/s41390-022-02303-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02303-5