Abstract
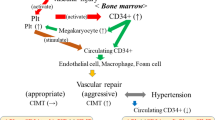
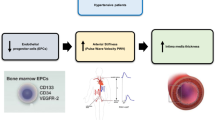
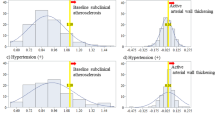
Populations of CD34− and VEGFR2-expressing cells are responsible for regeneration of damaged endothelium and vascular remodelling. As their quantity and activity changes during cardiovascular diseases, they are potentially useful markers of cardiovascular health. The aim of our study was to investigate changes of various CD34+ and CD34+ VEGFR2+ populations in subjects with newly recognised hypertension and to evaluate whether observed alterations are influenced by clinical parameters and angiotensin II. Circulating CD34+ and CD34+ VEGFR2+ cells were analysed in peripheral blood samples by flow cytometry. Serum levels of angiotensin II were determined using immunoenzymatic assay. We discovered increased proportions of various CD34+ populations and CD34+ VEGFR2+ c-Kit+ cells in newly diagnosed patients. CD34+ cells seem to be influenced by angiotensin II, but we did not observe comparable results when populations co-expressing VEGFR2 were analysed. The quantity of CD34+ VEGFR2+ cells in patients with newly recognised primary hypertension ought to be determined by other factors. Increased proportions of CD34+ progenitors in blood could comprise compensatory mechanism for increased endothelial damage in hypertension.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Van Zonneveld AJ, Rabelink TJ. Endothelial progenitor cells: biology and therapeutic potential in hypertension. Curr Opin Nephrol Hypertens. 2006;15:167–72.
Asahara T, Murohara T, Sullivan A, Silver M, van der Zee R, Li T, et al. Isolation of putative progenitor endothelial cells for angiogenesis. Science. 1997;14:964–7.
Caiado F, Dias S. Endothelial progenitor cells and integrins: adhesive needs. Fibrogenesis Tissue Repair. 2012;5:4.
Lennartsson J, Ronnstrand L. Stem cell factor receptor/c-Kit: from basic science to clinical implications. Physiol Rev. 2012;92:1619–49.
Kocher AA, Schuster MD, Szabolcs MJ, Takuma S, Burkhoff D, Wang J, et al. Neovascularization of ischemic myocardium by human bone-marrow-derived angioblasts prevents cardiomyocyte apoptosis, reduces remodeling and improves cardiac function. Nat Med. 2001;7:430–6.
Girbl T, Lunzer V, Greil R, Namberger K, Hartmann TN. The CXCR4 and adhesion molecule expression of CD34+ hematopoietic cells mobilized by “on-demand” addition of plerixafor to granulocyte-colony-stimulating factor. Transfusion. 2014;54:2325–35.
Seeger FH, Rasper T, Koyanagi M, Fox H, Zeiher AM, Dimmeler S. CXCR4 expression determines functional activity of bone marrow-derived mononuclear cells for therapeutic neovascularization in acute ischemia. Arterioscler Thromb Vasc Biol. 2009;29:1802–9.
Emdin M, Fatini C, Mirizzi G, Poletti R, Borrelli C, Prontera C, et al. Biomarkers of activation of renin-angiotensin-aldosterone system in heart failure: how useful, how feasible? Clin Chim Acta. 2015;443:85–93.
Kokot F, Ficek R. Role of the renin-angiotensjon-aldosterone system in the pathogenesis of arterial hypertension. Postępy Nauk Med. 2002;15:117–112.
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Böhm M, et al. 2013 ESH/ESC guidelines for the management of arterial hypertension: the task force for the Management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34:2159–219.
Skrzypkowska M, Myśliwska J, Słomiński B, Siebert J, Gutknecht P, Ryba-Stanisławowska M. Quantitative and functional characteristics of endothelial progenitor cells in newly diagnosed hypertensive patients. J Hum Hypertens. 2015;29:324–30.
Mackie A, Losordo D. CD34-Positive stem cells in the treatment of heart and vascular disease in human beings. Tex Heart Inst J. 2011;38:474–85.
Mandraffino G, Imbalzano E, Sardo MA, D’Ascola A, Mamone F, Lo Gullo A, et al. Circulating progenitor cells in hypertensive patients with different degrees of cardiovascular involvement. J H Hyperten. 2014;28:543–50.
Marketou ME, Kalyva A, Parthenakis FI, Pontikoglou C, Maragkoudakis S, Kontaraki JE. Circulating endothelial progenitor cells in hypertensive patients with increased arterial stiffness. J Clin Hypertens. 2014;16:295–300.
Kim SY, Park SY, Kim JM, Kim JW, Kim MY, Yang JH, et al. Differentiation of endothelial cells from human umbilical cord blood AC133-CD14+ cells. Ann Hematol. 2005;84:417–22.
Zhang Y, Foudi A, Geay JF, Berthebaud M, Buet D, Jarrier P, et al. Intracellular localization and constitutive endocytosis of CXCR4 in human CD34+ hematopoietic progenitor cells. Stem Cells. 2004;22:1015–29.
Vasa M, Fichtlscherer S, Aicher A, Adler K, Urbich C, Martin H, et al. Number and migratory activity of circulating endothelial progenitor cells inversely correlate with risk factors for coronary artery disease. Circ Res. 2001;89:1–7.
Lee CW, Huang PH, Huang SS, Leu HB, Huang CC, Wu TC, et al. Decreased circulating endothelial progenitor cell levels and function in essential hypertensive patients with electrocardiographic left ventricular hypertrophy. Hypertens Res. 2011;34:999–1003.
Zhong HL, Lu XZ, Chen XM, Yang XH, Zhang HF, Zhou L, et al. Relationship between stem cell factor/c-kit expression in peripheral blood and blood pressure. J H Hypertens. 2010;24:220–5.
Rodgers KE, Xiong S, Steer R, Dizerega GS. Effect of angiotensin II on hematopoietic progenitor cell proliferation. Stem Cells. 2000;18:287–94.
Yin T, Ma X, Zhao L, Cheng K, Wang H. Angiotensin II promotes NO production, inhibits apoptosis and enhances adhesion potential of bone marrow-derived endothelial progenitor cells. Cell Res. 2008;18:792–9.
Brunet de la Grange P, Ivanovic Z, Leprivey-Lorgeot V, Praloran V. Angiotensin II that reduces the colony-forming ability of hematopoietic progenitors in serum free medium has an inverse effect in serum-supplemented medium. Stem Cells. 2002;20:269–71.
Tamarat R, Silvestre JS, Kubis N, Benessiano J, Duriez M, deGasparo M. Endothelial nitric oxide synthase lies downstream from angiotensin II-induced angiogenesis in ischemic hindlimb. Hypertension. 2002;39:830–5.
Roks AJ. Angiotensin II deteriorates endothelial progenitor cells: good intentions with bad consequences. Hypertension. 2011;58:356–8.
Zhu XY, Urbieta Caceres VH, Favreau FD, Krier JD, Lerman A, Lerman LO. Enhanced endothelial progenitor cell angiogenic potency, present in early experimental renovascular hypertension, deteriorates with disease duration. J Hypertens. 2011;29:1972–9.
Mandraffino G, Aragona CO, Cairo V, Scuruchi M, Lo Gullo A, D’Ascola A, et al. Circulating progenitor cells in hypertensive subjects: Effectiveness of treatment with olmesartan in improving cell number and miR profile in addition to expected pharmacologicaleffects. PLoS ONE. 2017;12:e0173030.
Sata M, Saiura A, Kunisato A, Tojo A, Okada S, Tokuhisa T, et al. Hematopoietic stem cells differentiate into vascular cells that participate in the pathogenesis of atherosclerosis. Nat Med. 2002;8:403–9.
Yamada T, Kondo T, Numaguchi Y, Tsuzuki M, Matsubara T, Manabe I, et al. Angiotensin II receptor blocker inhibits neointimal hyperplasia through regulation of smooth muscle-like progenitor cells. Arterioscler Thromb Vasc Biol. 2007;27:2363–9.
Acknowledgements
The paper was subsided by the grants of National Science Centre Nr 2011/01/B/NZ5/00345. The funders had no role in the study design, data collection and analysis, decision to publish or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Skrzypkowska, M., Ryba-Stanisławowska, M.E., Słomiński, B. et al. Association of circulating progenitor cells with angiotensin II in newly diagnosed hypertensive patients. J Hum Hypertens 32, 46–53 (2018). https://doi.org/10.1038/s41371-017-0020-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-017-0020-3