Abstract
Background
Few studies have assessed associations between allergic diseases and antibacterial agents in Taiwanese children.
Objective
This study aimed to investigate the association of triclosan (TCS) exposure with allergic diseases among preschoolers, disease-specific IgE titers, and a child’s sex.
Methods
Pediatric data were obtained from the Childhood Environment and Allergic Diseases Study (CEAS; 2010) cohort, and their urine and blood samples were used to analyze TCS and IgE concentrations (age 3 group). Three years later, clinical data were obtained again from the age 3 group (age 6 group). Correlations of TCS levels at ages 3 and 6 years with IgE levels and allergic diseases were evaluated.
Results
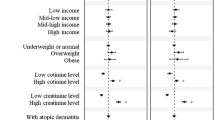
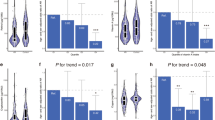
The TCS levels were higher at age 3 than at age 6 (geometric mean, 1.05 ng/ml vs 0.37 ng/ml). TCS levels were positively correlated with serum IgE levels at ages 3 and 6 years. Asthma and atopic dermatitis were significantly associated with TCS (adjusted OR 1.14, 95% confidence interval [CI] 1.01–1.29; OR 1.22, 95% CI 1.05–1.41). Sex-stratified analysis revealed that TCS levels were positively correlated with IgE levels among boys in the age 6 group and significantly associated with asthma, allergic rhinitis, and atopic dermatitis among boys.
Significance
TCS exposure is associated with IgE levels and a potentially high risk of pediatric atopic disorders.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Wu WF, Wan KS, Wang SJ, Yang W, Liu WL. Prevalence, severity, and time trends of allergic conditions in 6- to-7-year-old schoolchildren in Taipei. J Investig Allergol Clin Immunol. 2011;21:556–62.
Wang IJ, Guo YL, Hwang KC, Hsieh WS, Chuang YL, Lin SJ. et al. Genetic and environmental predictors for pediatric atopic dermatitis. Acta Paediatr Taiwanica. 2006;47:238–42.
Wang IJ, Huang LM, Guo YL, Hsieh WS, Lin TJ, Chen PC. Haemophilus influenzae type b combination vaccines and atopic disorders: a prospective cohort study. J Formos Med Assoc. 2012;111:711–8.
Jackson-Browne MS, Henderson N, Patti M, Spanier A, Braun J. M. The impact of early-life exposure to antimicrobials on asthma and eczema risk in children. Curr. Environ. Health Rep. 2019;6:214–24.
Strachan DP. Family size, infection and atopy: the first decade of the “hygiene hypothesis”. Thorax. 2000;55:S2–10.
Mitsui-Iwama M, Yamamoto-Hanada K, Fukutomi Y, Hirota R, Muto G, Nakamura T, et al. Exposure to paraben and triclosan and allergic diseases in Tokyo: a pilot cross-sectional study. Asia Pac Allergy. 2019;9:e5.
Hampton T. Research provides new insights on how hygiene affects asthma and allergies. JAMA 2011;305:1400–1.
McMurry LM, Oethinger M, Levy SB. Triclosan targets lipid synthesis. Nature. 1998;394:531–2.
Dann AB, Hontela A. Triclosan: environmental exposure, toxicity and mechanisms of action. J Appl Toxicol. 2011;31:285–311.
SCCS. Opinion on Triclosan antimicrobial resistance. http://ec.europa.eu/health/scientific_committees/consumer_safety/docs/sccs_o_023. 2010.
Pasch E, Voltmer L, Gemmell S, Walter J, Walton KLW. Effects of Triclosan on the normal intestinal microbiota and on susceptibility to experimental murine colitis. FASEB J. 2009;23:977.10.
EFSA. European Food Safety Authority. Opinion of the Scientific Panel on food additives, flavourings, processing aids and materials in contact with food (AFC) related to 2,2-bis(4-hydroxyphenyl) propane. EFSA J. 2006;428:1–75.
Frei R, Lauener RP, Crameri R, O’Mahony L. Microbiota and dietary interactions – an update to the hygiene hypothesis? Allergy. 2012;67:451–61.
Levy SB. Antibacterial household products: cause for concern. Emerg Infect Dis. 2001;7:512–5.
Weatherly LM, Gosse JA. Triclosan exposure, transformation, and human health effects. J Toxicol Environ Health B Crit Rev. 2017;20:447–69.
Taiwan Food drug administration. I heard that cosmetics containing triclosan (triclosan) are carcinogenic. Is it really that scary? Available at: https://www.fda.gov.tw/tc/newsContent.aspx?id=19821&chk=48f4baa8-327a-4e34-a968-9320f8ea8626 (accessed on 25 April 2016).
Dann AB, Hontela A. Triclosan: environmental exposure, toxicity and mechanisms of action. J Appl Toxicol. 2011;31:285–311.
Wang C-F, Tian Y. Reproductive endocrine-disrupting effects of triclosan: population exposure, present evidence and potential mechanisms. Environ Pollut. 2015;206:195–201.
Geens T, Neels H, Covaci A. Distribution of bisphenol-A, triclosan and n-nonylphenol in human adipose tissue, liver and brain. Chemosphere. 2012;87:796–802.
Huang C-L, Abass OK, Yu C-P. Triclosan: a review on systematic risk assessment and control from the perspective of substance flow analysis. Sci Total Environ. 2016;566:771–85. https://doi.org/10.1016/j.scitotenv.2016.05.002
Bertelsen RJ, Longnecker MP, Løvik M, Calafat AM, Carlsen K-H, London SJ, et al. Triclosan exposure and allergic sensitization in Norwegian children. Allergy. 2013;68:84–91.
Savage JH, Matsui EC, Wood RA, Keet CA. Urinary levels of triclosan and parabens are associated with aeroallergen and food sensitization. J Allergy Clin Immunol. 2012;130:453–60.
Bertelsen RJ, Longnecker MP, Løvik M, Calafat AM, Carlsen KH, London SJ, et al. Triclosan exposure and allergic sensitization in Norwegian children. Allergy. 2013;68:84–91.
Spanier AJ, Fausnight T, Camacho TF, Braun JM. The associations of triclosan and paraben exposure with allergen sensitization and wheeze in children. Allergy Asthma Proc. 2014;35:475–81.
Ye X, Kuklenyik Z, Needham LL, Calafat AM. Automated on-line column-switching HPLC-MS/MS method with peak focusing for the determination of nine environmental phenols in urine. Anal Chem. 2005;77:5407–13.
Cayman Chemical Company. Creatinine (urinary). https://www.caymanchem.com/pdfs/500701.pdf. 2012.
Hanifin JM, Rajka G. Disgnostic features of atopic dermatitis. Acta Derm Venereol Suppl. 1980;92:44–7.
Brozek JL, Bousquet J, Baena-Cagnani CE, Bonini S, Canonica GW, Casale TB, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J Allergy Clin Immunol. 2010;126:466–76.
Soto-Martinez ME, Avila L, Soto-Quiros ME. New criteria for the diagnosis and management of asthma in children under 5 years old: GINA Guidelines. Pediatr. 2009;71:91–4.
Iyer AP, Xue J, Honda M, Robinson M, Kumosani TA, Abulnaja K, et al. Urinary levels of triclosan and triclocarban in several Asian countries, Greece and the USA: association with oxidative stress. Environ Res Vol. 2018;160:91–6.
Calafat AM, Ye X, Wong LY, Reidy JA, Needham LL. Urinary concentrations of triclosan in the U.S. population: 2003-4. Environ Health Perspect. 2008;116:303–7.
Mulla SI, Wang H, Sun Q, Hu A, Yu C-P. Characterization of triclosan metabolism in Sphingomonas sp. strain YL-JM2C. Sci Rep. 2016;6:21965.
Jackson-Browne MedinaS, Henderson Noelle, Patti Marisa, Spanier Adam, Braun JosephM. The impact of early-life exposure to antimicrobials on asthma and eczema risk in children. Curr Environ Health Rep. 2019;6:214–24.
Spanier AJ, Fausnight T, Camacho TF, Braun JM. The associations of triclosan and paraben exposure with allergen sensitization and wheeze in children. Allergy Asthma Proc. 2014;35:475–81.
Quirós-Alcalá L, Hansel NN, Mc Cormack MC, Matsui EC. Paraben exposures and asthma-related outcomes among children from the US general population. J Allergy Clin Immunol. 2019;143:948.e4–56.e4.
Aung MT, Ferguson KK, Cantonwine DE, Bakulski KM, Mukherjee B, Loch-Caruso R, et al. Corrigendum to “Associations between maternal plasma measurements of inflammatory markers and urinary levels of phenols and parabens during pregnancy: a repeated measures study”. [Sci. Total Environ. 650 (Pt 1) (2019) 1131–1140]. Sci Total Environ. 2019;658:1640.
Ashley-Martin J, Dodds L, Arbuckle TE, Marshall J. Prenatal triclosan exposure and cord blood immune system biomarkers. Int J Hyg Environ Health. 2016;219:454–7. https://doi.org/10.1016/j.ijheh.2016.04.010
Anderson SE, Franko J, Kashon ML, Anderson KL, Hubbs AF, Lukomska E, et al. Exposure to triclosan augments the allergic response to ovalbumin in a mouse model of asthma. Toxicol Sci. 2013;132:96–106.
Ahn KC, Zhao B, Chen J, Cherednichenko G, Sanmarti E, Denison MS, et al. In vitro biologic activities of the antimicrobials triclocarban, its analogs, and triclosan in bioassay screens: receptor-based bioassay screens. Environ Health Perspect. 2008;116:1203–10.
Paul KB, Hedge JM, DeVito MJ, Crofton KM. Short-term exposure to triclosan decreases thyroxine in vivo via upregulation of hepatic catabolism in young Long-Evans rats. Toxicol Sci. 2010;113:367–79.
Stoker TE, Gibson EK, Zorrilla LM. Triclosan exposure modulates estrogen-dependent responses in the female Wistar rat. Toxicol Sci. 2010;117:45–53.
Dann AB, Hontelam A. Triclosan: environmental exposure, toxicity and mechanisms of action. J Appl Toxicol 2011;31:285–311.
Laffont S, Blanquart E, Guéry J-C. Sex differences in asthma: a key role of androgen-signaling in group 2 innate lymphoid cells. Front Immunol. 2017;8:1069.
Yung JA, Fuseini H, Newcomb DC. Hormones, sex, and asthma. Ann Allergy Asthma Immunol. 2018;120:488–94.
Wijga A, Tabak C, Postma DS, Kerkhof M, Wieringa MH, Hoekstra MO, et al. Sex differences in asthma during the first 8 years of life: the Prevention and Incidence of Asthma and Mite Allergy (PIAMA) birth cohort study. J Allergy Clin Immunol. 2011;127:275–7.
Almqvist C, Worm M, Leynaert B, Working group of GALEN WP 2.5 Gender. Impact of gender on asthma in childhood and adolescence: a GA2LEN review. Allergy. 2008;63:47–57.
Bertelsen RJ, Longnecker MP, Løvik M, Calafat AM, Carlsen KH, London SJ, et al. Triclosan exposure and allergic sensitization in Norwegian children. Allergy. 2013;68:84–91.
Hong S, Kwon HJ, Choi WJ, Lim WR, Kim J, Kim K. Association between exposure to antimicrobial household products and allergic symptoms. Environ Health Toxicol. 2014;29:e2014017. https://doi.org/10.5620/eht.e2014017.
Hitota R, Ohya Y, Yamamoto-Hanada K, Fukutomi Y. Triclosan-induced alteration of gut microbiome and aggravation of asthmatic airway response in aeroallergen-sensitized mice. Allergy. 2018;74:996–9. https://www.researchgate.net/publication/328494239.
U.S. Food & Drug Administration, Department of Health and Human Services. Triclosan [CAS 3380-34-5] supporting information for toxicological evaluation by the National Toxicology Program. https://ntp.niehs.nih.gov/ntp/htdocs/chem_background/exsumpdf/triclosan_508.pdf (2008).
Acknowledgements
The authors are very thankful to the Editors and the anonymous reviewers for their constructive comments to improve the quality of this article. The authors also thank the CEAS study group (Mr. Han-Hsing Tsou for urine analysis and Professor Meilien Chen, our colleague, for data collection).This manuscript was edited by Wallace Academic Editing.
Funding
This study was supported by grants from theMinistry of Science and Technology (MOST 106-2314-B-192 -001 -MY3) and Taipei Hospital, Ministry of Health and Welfare in Taiwan.
Author information
Authors and Affiliations
Contributions
Conceptualization: M.-H.L., S.-Y.C.; methodology: I.-J.W., W.-C.H.; formal analysis: I.-J.W., T.-Y.L., K.-H.C.; data curation: I.-J.W., M.-H.L., K.-H.C. T.-Y.L.; writing—original draft preparation: M.-H.L., S.-Y.C., I.-J.W.; writing—review and editing: I.-J.W., M.-H.L., S.-Y.C.; supervision: I.-J.W., W.-C.H.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval and consent to participate
The Institutional Review Board of Taipei Hospital Protocol Number: IRB serial number: TH-IRB-0016-0019.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lin, MH., Chiu, SY., Ho, WC. et al. Effect of triclosan on the pathogenesis of allergic diseases among children. J Expo Sci Environ Epidemiol 32, 60–68 (2022). https://doi.org/10.1038/s41370-021-00304-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-021-00304-w
Keywords
This article is cited by
-
Asthma and Environmental Exposures to Phenols, Polycyclic Aromatic Hydrocarbons, and Phthalates in Children
Current Environmental Health Reports (2023)