Abstract
Background
Multicomponent family-based behavioral treatment (FBT) program for pediatric obesity includes nutrition and physical activity education, as well as behavior therapy techniques. Studies suggest that parent weight loss is the best predictor of child weight loss in FBT. However, given the important role that parents play in the implementation of FBT for their child, isolating the effects of specific FBT treatment component requires consideration of parent influences over time.
Methods
The following treatment components were assessed: stimulus control (high/low-fat food items in home), nutrition knowledge, energy intake, physical activity, and parental monitoring, as well as weekly anthropometric measures. Adjusted models of interest using inverse probability weights were used to evaluate the effect of specific FBT components on time-varying child weight loss rate, adjusting for time-varying influence of parent weight loss.
Results
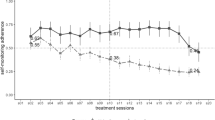
One hundred thirty-seven parent–child dyads (CHILD: mean BMI = 26.4 (3.7) and BMIz = 2.0 (0.3); mean age = 10.4 (1.3); 64.1% female; ADULT: mean BMI = 31.9 (6.3); mean age = 42.9 (6.5); 30.1% Hispanic parents; 87.1% female) participated in an FBT program. In traditional model, adult BMI change (b = 0.08; p < 0.01) was the most significant predictor of child weight loss rates and no other treatment components were significant (p’s > 0.1). In models that accounted for potential influences from parental weight loss and differential attendance during treatment period, lower availability of high-fat items (b = 1.10, p < 0.02), higher availability of low-fat items (b = 3.73; p < 0.01), and higher scores on parental monitoring practices (b = 1.10, p < 0.01) were associated with greater rates of weight loss, respectively.
Conclusion
Results suggest that outside of parent weight change, changes in stimulus control strategies at home and improved parental-monitoring practices are important FBT components for child weight loss.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Ogden C, Carroll M, Kit B, Flegal K. Prevalence of childhood and adult obesity in the United States, 2011-2012. J Am Med Assoc. 2014;311:806–14.
Skinner A, Ravanbakht S, Skelton J, Perrin E, Armstrong S. Prevalence of obesity and severe obesity in US Children, 1999-2016. Pediatrics. 2018;141:e20173459.
Dietz W. Health consequences of obesity in youth: childhood predictors of adult disease. Pediatrics. 1998;101:518–25.
Key T, Schatzkin A, Willett W, Allen N, Spencer E, Travis R. Diet, nutrition and the prevention of cancer. Pub Health Nutr. 2004;7:187–200.
Micic D. Obesity in children and adolescents—a new epidemic? Consequences in adult life. J Pediatr Endocrinol Metab. 2001;14(Suppl 5):1345–52.
Must A, Spadano J, Coakley E, Field A, Colditz G, Dietz W. The disease burden associated with overweight and obesity. J Am Med Assoc. 1999;282:1523–9.
Skinner A, Perrin E, Skelton J. Cardiometabolic risks and obesity in the young. New Engl J Med. 2016;374:592–3.
Freedman D, Ogden C, Kit B. Interrelationships between BMI, skinfold thicknesses, percent body fat, and cardiovascular disease risk factors among U.S. children and adolescents. BMC Pediatr. 2015;15:188.
Ul-Haq Z, Mackay D, Fenwick E, Pell J. Meta-analysis of the association between body mass index and health-related quality of life among children and adolescents, assessed using the pediatric quality of life inventory index. J Pediatr. 2013;162:280–6.
Weihrauch-Bluher S, Schwarz P, Klusmann J. Childhood obesity: increased risk for cardiometabolic disease and cancer in adulthood. Metabolism. 2019;92:147–52.
Franks PW, Hanson RL, Knowler WC, Sievers ML, Bennett PH, Looker HC. Childhood obesity, other cardiovascular risk factors, and premature death. N Engl J Med. 2010;362:485–93.
Guo S, Chumlea W. Tracking of body mass index in children in relation to overweight in adulthood. Am J Clin Nutr. 1999;70:145S–8S.
Simmonds M, Llewllyn A, Owen C, Woolacott N. Predicting adult obesity from childhood obesity: a systematic review and meta-analysis. Obes Rev. 2016;17:95–107.
Janicke D, Harman J, Jamoom E, Simon S, Zhang J, Dumont-Driscoll M. The relationship among child weight status, psychosocial functioning, and pediatric health care expenditures in a medicaid population. J Pediatr Psychol. 2010;35:883–91.
Boutelle K, Rhee K, Liang J, Braden A, Douglas J, Strong D, et al. Effect of attendance of the child on body weight, energy intake, and physical activity in childhood obesity treatment: a randomized clinical trial. JAMA Pediatr. 2017;171:622–8.
Epstein L. Development of evidence-based treatments for pediatric obesity. In: Kazdin A, Weisz J, editors. Evidence-based psychotherapies for children and adolescents. New York: Guilford Publications; 2003. p. 374–88.
Wilfley D, Tibbs T, Van Buren D, Reach K, Walker M, Epstein L. Lifestyle interventions in the treatment of childhood overweight: a meta-analytic review of randomized controlled trials. Health Psychol. 2007;26:521–32.
Epstein L, Paluch R, Roemmich J, Beecher M. Family-based obesity treatment, then and now: twenty-five years of pediatric obesity treatment. Health Psychol. 2007;26:381–91.
O’Connor E, Evans C, Burda B, Walsh E, Eder M, Loranzo P. Screening for obesity and intervention for weight management in children and adolescents: evidence report and systematic review for the United States Preventive Services Task Force. J Am Med Assoc. 2017;317:2427–44.
Whitlock E, O’Connor E, Williams S, Beil T, Lutz K. Effectiveness of weight management interventions in children: a targeted systematic review for the United States Preventive Services Task Force. Pediatrics. 2010;125:e396–428.
Boutelle K, Cafri G, Crow S. Parent predictors of child weight change in family based behavioral obesity treatment. Obesity. 2012;20:1539–43.
Wrotniak B, Epstein H, Paluch R, Roemmich J. Parent weight change as a predictor of child weight change in family-based behavioral obesity treatment. Arch Pediatr Adolesc Med. 2004;158:342–7.
Boutelle K, Braden A, Douglas J, Rhee K, Strong D, Rock C, et al. Design of the FRESH study: a randomized controlled trial of a parent-only and parent-child family-based treatment for childhood obesity. Contemp Clin Trials. 2015;45:364–70.
Graffeo N, Latouche A, Geskus R, Chevret S. Modeling time-varying exposure using inverse probability of treatment weights. Biom J. 2018;60:323–32.
Imai K, Ratkovic M. Robust estimation of inverse probability weights for marginal structural models. J Am Stat Assoc. 2015;110:1013–23.
Kuczmarski R, Ogden C, Grummer-Strawn L, Flegal K, Guo S, Wei R, et al. CDC growth charts: United States. Adv Data. 2000;314:1–27.
Harnack L, Stevens M, Van Heel N, Schakel S, Dwyer J, Himes J. A computer-based approach for assessing dietary supplement use in conjunction with dietary recalls. J Food Compost Anal. 2008;21(Suppl 1):S78–82.
Actigraph. Actigraph GT1M Monitor/ActiTrainer and ActiLife Lifestyle Monitor software user manual. In: Actigraph. FL: LLC Pensacola; 2007.
Raynor H, Polly B, Wing R, Jeffery R. Is dietary fat intake related to liking or household availability of high- and low-fat foods? Obes Res. 2004;12:816–23.
Epstein L. The traffic light childhood weight control program: traffic light: kids program. NY: University of Buffalo; 2005.
Birch L, Fisher J, Grimm-Thomas K, Markey C, Sawyer R, Johnson S. Confirmatory factor analysis of the Child Feeding Questionnaire: a measure of parental attitudes, beliefs and practices about child feeding and obesity proneness. Appetite. 2001;36:201–10.
Kaur H, Li C, Nazir N, Choi W, Resnicow K, Birch L, et al. Confirmatory factor analysis of the child-feeding questionnaire among parents of adolescents. Appetite. 2006;47:36–45.
Muggeo V, Atkins D, Gallop R, Dimidjian S. Segmented mixed models with random changepoints: a maximum likelihood approach with application to treatment for depression study. Statis Modeling. 2014;14:293–313.
Grajeda L, Ivanescu A, Saito M, Crainiceanu C, Jaganath D, Gilman R, et al. Modelling subject-specific childhood growth using linear mixed-effect models with cubic regression splines. Emerg Themes Epidemiol. 2016;13:1.
Gorter R, Fox J, Twisk J. Why item response theory should be used for longitudinal questionnaire data analysis in medical research. BMC Med Methodol. 2015;15:55.
van der Wal W, Geskus R. Ipw: an R package for inverse probability weighting. J Stat Software. 2011;43:1–23.
Grund S, Ludtke O, Robitzsch A. Multiple imputation of missing data for multilevel models: simulations and recommendations. Organiz Res Methods. 2018;21:111–49.
Pinheiro J, Bates D, DebRoy S, Sarkar D, Team RC. nlme: Linear and nonlinear mixed-effects models. R package version; 2012.
Horgan M., Horgan, A. (2016). Food availability in the homes of overweight children (Thesis, Master of Dietetics). University of Otago, New Zealand; 2016.
Ihmels M, Welk G, Eisenmann J, Nusser S. Development and preliminary validation of a family nutrition and physical activity (FNPA) screening tool. Int J Behav Nutr Phys Act. 2009;6:14.
Ihmels M, Welk G, Eisenmann J, Nusser S, Myers E. Prediction of BMI change in young children with the family nutrition and physical activity (FNPA) screening tool. Ann Behav Med. 2009;38:60–8.
Nepper M, Weiwen C. Assessment of home food environment among healthy weight and overweight school-age children. Health Behav Policy Rev. 2016;3:568–80.
Ong J, Ullah S, Margary A, Leslie E. Positive influences of home food environment on primary-school children’s diet and weight status: a structural equation model approach. Public Health Nutr. 2016;19:2525–34.
Martin J, Chater A, Lorencatto F. Effective behaviour change techniques in the prevention and management of childhood obesity. Int J Obes. 2013;37:1287–94.
Kim K, Wallander J, Felt J, Elliott M, Schuster M. Associations of parental general monitoring with adolescent weight-related behaviors and weight status. Obesity. 2019;27:280–7.
Casey B, Tottenham N, Liston C, Durston S. Imaging the developing brain: what have we learned about cognitive development? Trends Cogn Sci. 2005;9:104–10.
Burrows T, Martin R, Collins C. A systematic review of the validity of dietary assessment methods in children when compared with the method of doubly labeled water. J Am Diet Assoc. 2010;110:1501–10.
Johns D, Hartmann-Boyce J, Jebb S, Aveyard P, Behavioural Weight Management Review Group. Diet or exercise interventions vs combined behavioral weight management programs: a systematic review and meta-analysis of direct comparisons. J Acad Nutr Diet. 2014;114:1557–68.
United States Preventive Services Task Force. Screening for obesity in children and adolescents: US Preventive Services Task Force recommendation statement. Pediatrics. 2010;125:361–7.
Whitlock E, O’Connor E, Williams S, Beil T, Lutz K. Effectiveness of weight management interventions in children: a targeted systematic review for the United States Preventive Services Task Force. Pediatrics. 2010;125:e396–418.
Acknowledgements
This work was supported by the National Institute of health [grant numbers R01DK075861 and K02HL1120242, PI: Boutelle].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Boutelle, K.N., Kang Sim, D.E., Rhee, K.E. et al. Family-based treatment program contributors to child weight loss. Int J Obes 45, 77–83 (2021). https://doi.org/10.1038/s41366-020-0604-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-020-0604-9
This article is cited by
-
Translating the Recommended Multicomponent Intervention for Childhood Overweight and Obesity into Practice: Implementation Challenges
Journal of Contemporary Psychotherapy (2023)