Abstract
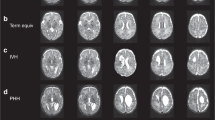
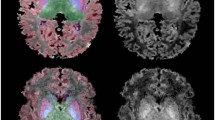
Owing to improved survival rates of premature newborns, the number of very low birth weight infants is rising. Preterm infants display a greater propensity for brain injury caused by hypoxic or ischemic events, infection and/or inflammation that results in prominent white matter injury (WMI) than infants carried to full term. The intrinsic vulnerability of developing oligodendroglia to excitotoxic, oxidative and inflammatory forms of injury is a major factor in the pathogenesis of this condition. Furthermore, activated microglia and astrogliosis are critically involved in triggering WMI. Currently, no specific treatment is available for this kind of injury. Injury to the premature brain can substantially influence brain development and lead to disability. Impairment of the main motor pathways, such as the corticospinal tract, in the perinatal period contributes substantially to clinical outcome. Advanced neuroimaging techniques have led to greater understanding of the nature of both white and gray matter injury in preterm infants. Further research is warranted to examine the translational potential of preclinical therapeutic strategies for controlling such injury and preserving the integrity of motor pathways in preterm infants.
Key Points
-
Premature birth remains a substantial economic and public health burden
-
Periventricular leukomalacia is the predominant form of white matter injury (WMI) and the leading cause of cerebral palsy in premature infants
-
Maturation-dependent vulnerability of developing oligodendroglia to excitotoxicity and oxidative and inflammatory forms of injury is an important factor in the pathogenesis of WMI
-
Activated microglia and astrogliosis are critically involved in triggering WMI
-
Impairment of corticospinal tract development and function in the perinatal period contributes extensively to abnormalities of motor system function
-
Advanced neuroimaging techniques have led to greater understanding of the nature of white and gray matter injury in preterm infants
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Volpe, J. J. (Ed.) Neurology of the Newborn (Saunders, Philadelphia, 2001).
Volpe, J. J. Brain injury in premature infants: a complex amalgam of destructive and developmental disturbances. Lancet Neurol. 8, 110–124 (2009).
Pleasure, D., Soulika, A., Singh, S. K., Gallo, V. & Bannerman, P. Inflammation in white matter: clinical and pathophysiological aspects. Ment. Retard. Dev. Disabil. Res. Rev. 12, 141–146 (2006).
Deng, W., Pleasure, J. & Pleasure, D. Progress in periventricular leukomalacia. Arch. Neurol. 65, 1291–1295 (2008).
Inder, T. E. et al. Periventricular white matter injury in the premature infant is followed by reduced cerebral cortical gray matter volume at term. Ann. Neurol. 46, 755–760 (1999).
Inder, T. E., Wells, S. J., Mogridge, N. B., Spencer, C. & Volpe, J. J. Defining the nature of the cerebral abnormalities in the premature infant: a qualitative magnetic resonance imaging study. J. Pediatr. 143, 171–179 (2003).
Sizonenko, S. V. et al. Selective cortical alteration after hypoxic-ischemic injury in the very immature rat brain. Pediatr. Res. 54, 263–269 (2003).
Nagae, L. M. et al. Diffusion tensor imaging in children with periventricular leukomalacia: variability of injuries to white matter tracts. AJNR Am. J. Neuroradiol. 28, 1213–1222 (2007).
Neil, J., Miller, J., Mukherjee, P. & Huppi, P. S. Diffusion tensor imaging of normal and injured developing human brain—a technical review. NMR Biomed. 15, 543–552 (2002).
Larroque, B. et al. Neurodevelopmental disabilities and special care of 5-year-old children born before 33 weeks of gestation (the EPIPAGE study): a longitudinal cohort study. Lancet 371, 813–820 (2008).
Banker, B. Q. & Larroche, J. C. Periventricular leukomalacia of infancy. A form of neonatal anoxic encephalopathy. Arch. Neurol. 7, 386–410 (1962).
Leviton, A. & Gilles, F. H. Acquired perinatal leukoencephalopathy. Ann. Neurol. 16, 1–8 (1984).
Follett, P. L. et al. Glutamate receptor-mediated oligodendrocyte toxicity in periventricular leukomalacia: a protective role for topiramate. J. Neurosci. 24, 4412–4420 (2004).
Follett, P. L., Rosenberg, P. A., Volpe, J. J. & Jensen, F. E. NBQX attenuates excitotoxic injury in developing white matter. J. Neurosci. 20, 9235–9241 (2000).
Jensen, F. E. Developmental factors regulating susceptibility to perinatal brain injury and seizures. Curr. Opin. Pediatr. 18, 628–633 (2006).
Sizonenko, S. V., Kiss, J. Z., Inder, T., Gluckman, P. D. & Williams, C. E. Distinctive neuropathologic alterations in the deep layers of the parietal cortex after moderate ischemic-hypoxic injury in the P3 immature rat brain. Pediatr. Res. 57, 865–872 (2005).
Bemelmans, A. P. et al. Lentiviral-mediated gene transfer of brain-derived neurotrophic factor is neuroprotective in a mouse model of neonatal excitotoxic challenge. J. Neurosci. Res. 83, 50–60 (2006).
Carpentier, P. A., Duncan, D. S. & Miller, S. D. Glial toll-like receptor signaling in central nervous system infection and autoimmunity. Brain Behav. Immun. 22, 140–147 (2008).
Coban, C. et al. Pathological role of Toll-like receptor signaling in cerebral malaria. Int. Immunol. 19, 67–79 (2007).
Jung, D. Y. et al. TLR4, but not TLR2, signals autoregulatory apoptosis of cultured microglia: a critical role of IFN-β as a decision maker. J. Immunol. 174, 6467–6476 (2005).
Lee, S. J. & Lee, S. Toll-like receptors and inflammation in the CNS. Curr. Drug Targets Inflamm. Allergy 1, 181–191 (2002).
Jack, C. S. et al. TLR signaling tailors innate immune responses in human microglia and astrocytes. J. Immunol. 175, 4320–4330 (2005).
Esen, N. & Kielian, T. Central role for MyD88 in the responses of microglia to pathogen-associated molecular patterns. J. Immunol. 176, 6802–6811 (2006).
Griffiths, M., Neal, J. W. & Gasque, P. Innate immunity and protective neuroinflammation: new emphasis on the role of neuroimmune regulatory proteins. Int. Rev. Neurobiol. 82, 29–55 (2007).
Nakanishi, K., Yoshimoto, T., Tsutsui, H. & Okamura, H. Interleukin-18 regulates both Th1 and Th2 responses. Annu. Rev. Immunol. 19, 423–474 (2001).
Lehnardt, S. et al. The toll-like receptor TLR4 is necessary for lipopolysaccharide-induced oligodendrocyte injury in the CNS. J. Neurosci. 22, 2478–2486 (2002).
Coumans, A. B. et al. Intracisternal application of endotoxin enhances the susceptibility to subsequent hypoxic-ischemic brain damage in neonatal rats. Pediatr. Res. 53, 770–775 (2003).
Volpe, J. J. Cerebral white matter injury of the premature infant—more common than you think. Pediatrics 112, 176–180 (2003).
Vollmer, B. et al. Predictors of long-term outcome in very preterm infants: gestational age versus neonatal cranial ultrasound. Pediatrics 112, 1108–1114 (2003).
Raff, M. C., Miller, R. H. & Noble, M. A glial progenitor cell that develops in vitro into an astrocyte or an oligodendrocyte depending on culture medium. Nature 303, 390–396 (1983).
Pfeiffer, S. E., Warrington, A. E. & Bansal, R. The oligodendrocyte and its many cellular processes. Trends Cell Biol. 3, 191–197 (1993).
Levine, J. M., Reynolds, R. & Fawcett, J. W. The oligodendrocyte precursor cell in health and disease. Trends Neurosci. 24, 39–47 (2001).
Deng, W. & Poretz, R. D. Oligodendroglia in developmental neurotoxicity. Neurotoxicology 24, 161–178 (2003).
Back, S. A. et al. Late oligodendrocyte progenitors coincide with the developmental window of vulnerability for human perinatal white matter injury. J. Neurosci. 21, 1302–1312 (2001).
Kinney, H. C. & Back, S. A. Human oligodendroglial development: relationship to periventricular leukomalacia. Semin. Pediatr. Neurol. 5, 180–189 (1998).
Sizonenko, S. V., Camm, E. J., Dayer, A. & Kiss, J. Z. Glial responses to neonatal hypoxic-ischemic injury in the rat cerebral cortex. Int. J. Dev. Neurosci. 26, 37–45 (2008).
Juurlink, B. H. Response of glial cells to ischemia: roles of reactive oxygen species and glutathione. Neurosci. Biobehav. Rev. 21, 151–166 (1997).
Folkerth, R. D. et al. Developmental lag in superoxide dismutases relative to other antioxidant enzymes in premyelinated human telencephalic white matter. J. Neuropathol. Exp. Neurol. 63, 990–999 (2004).
Li, J. et al. Tumor necrosis factor alpha mediates lipopolysaccharide-induced microglial toxicity to developing oligodendrocytes when astrocytes are present. J. Neurosci. 28, 5321–5330 (2008).
Oka, A., Belliveau, M. J., Rosenberg, P. A. & Volpe, J. J. Vulnerability of oligodendroglia to glutamate: pharmacology, mechanisms, and prevention. J. Neurosci. 13, 1441–1453 (1993).
DeSilva, T. M., Kabakov, A. Y., Goldhoff, P. E., Volpe, J. J. & Rosenberg, P. A. Regulation of glutamate transport in developing rat oligodendrocytes. J. Neurosci. 29, 7898–7908 (2009).
Back, S. A. et al. Hypoxia-ischemia preferentially triggers glutamate depletion from oligodendroglia and axons in perinatal cerebral white matter. J. Cereb. Blood Flow Metab. 27, 334–347 (2007).
Desilva, T. M. et al. The glutamate transporter EAAT2 is transiently expressed in developing human cerebral white matter. J. Comp. Neurol. 501, 879–890 (2007).
Deng, W., Rosenberg, P. A., Volpe, J. J. & Jensen, F. E. Calcium-permeable AMPA/kainate receptors mediate toxicity and preconditioning by oxygen-glucose deprivation in oligodendrocyte precursors. Proc. Natl Acad. Sci. USA 100, 6801–6806 (2003).
Patneau, D. K., Wright, P. W., Winters, C., Mayer, M. L. & Gallo, V. Glial cells of the oligodendrocyte lineage express both kainate- and AMPA-preferring subtypes of glutamate receptor. Neuron 12, 357–371 (1994).
Gallo, V. & Ghiani, C. A. Glutamate receptors in glia: new cells, new inputs and new functions. Trends Pharmacol. Sci. 21, 252–258 (2000).
Alberdi, E., Sanchez-Gomez, M. V., Marino, A. & Matute, C. Ca2+ influx through AMPA or kainate receptors alone is sufficient to initiate excitotoxicity in cultured oligodendrocytes. Neurobiol. Dis. 9, 234–243 (2002).
Sánchez-Gómez, M. V. & Matute, C. AMPA and kainate receptors each mediate excitotoxicity in oligodendroglial cultures. Neurobiol. Dis. 6, 475–485 (1999).
Karadottir, R., Cavelier, P., Bergersen, L. H. & Attwell, D. NMDA receptors are expressed in oligodendrocytes and activated in ischaemia. Nature 438, 1162–1166 (2005).
Salter, M. G. & Fern, R. NMDA receptors are expressed in developing oligodendrocyte processes and mediate injury. Nature 438, 1167–1171 (2005).
Micu, I. et al. NMDA receptors mediate calcium accumulation in myelin during chemical ischaemia. Nature 439, 988–992 (2006).
Bergles, D. E., Roberts, J. D., Somogyi, P. & Jahr, C. E. Glutamatergic synapses on oligodendrocyte precursor cells in the hippocampus. Nature 405, 187–191 (2000).
Ge, W. P. et al. Long-term potentiation of neuron–glia synapses mediated by Ca2+-permeable AMPA receptors. Science 312, 1533–1537 (2006).
Pende, M. et al. Neurotransmitter- and growth factor-induced cAMP response element binding protein phosphorylation in glial cell progenitors: role of calcium ions, protein kinase C, and mitogen-activated protein kinase/ribosomal S6 kinase pathway. J. Neurosci. 17, 1291–1301 (1997).
Yuan, X., Eisen, A. M., McBain, C. J. & Gallo, V. A role for glutamate and its receptors in the regulation of oligodendrocyte development in cerebellar tissue slices. Development 125, 2901–2914 (1998).
Kukley, M., Capetillo-Zarate, E. & Dietrich, D. Vesicular glutamate release from axons in white matter. Nat. Neurosci. 10, 311–320 (2007).
Ziskin, J. L., Nishiyama, A., Rubio, M., Fukaya, M. & Bergles, D. E. Vesicular release of glutamate from unmyelinated axons in white matter. Nat. Neurosci. 10, 321–330 (2007).
Lehnardt, S. et al. Activation of innate immunity in the CNS triggers neurodegeneration through a Toll-like receptor 4-dependent pathway. Proc. Natl Acad. Sci. USA 100, 8514–8519 (2003).
Kauppinen, T. M. & Swanson, R. A. The role of poly(ADP-ribose) polymerase-1 in CNS disease. Neuroscience 145, 1267–1272 (2007).
Butovsky, O. et al. Induction and blockage of oligodendrogenesis by differently activated microglia in an animal model of multiple sclerosis. J. Clin. Invest. 116, 905–915 (2006).
Kim, S. S. et al. Inhibitory action of minocycline on lipopolysaccharide-induced release of nitric oxide and prostaglandin E2 in BV2 microglial cells. Arch. Pharm. Res. 27, 314–318 (2004).
Pitt, D., Nagelmeier, I. E., Wilson, H. C. & Raine, C. S. Glutamate uptake by oligodendrocytes: implications for excitotoxicity in multiple sclerosis. Neurology 61, 1113–1120 (2003).
Billiards, S. S. et al. Development of microglia in the cerebral white matter of the human fetus and infant. J. Comp. Neurol. 497, 199–208 (2006).
Takahashi, J. L., Giuliani, F., Power, C., Imai, Y. & Yong, V. W. Interleukin-1beta promotes oligodendrocyte death through glutamate excitotoxicity. Ann. Neurol. 53, 588–595 (2003).
Wender, R. et al. Astrocytic glycogen influences axon function and survival during glucose deprivation in central white matter. J. Neurosci. 20, 6804–6810 (2000).
McQuillen, P. S. & Ferriero, D. M. Perinatal subplate neuron injury: implications for cortical development and plasticity. Brain Pathol. 15, 250–260 (2005).
Gressens, P. Mechanisms and disturbances of neuronal migration. Pediatr. Res. 48, 725–730 (2000).
Kostovic, I. & Rakic, P. Developmental history of the transient subplate zone in the visual and somatosensory cortex of the macaque monkey and human brain. J. Comp. Neurol. 297, 441–470 (1990).
McQuillen, P. S., Sheldon, R. A., Shatz, C. J. & Ferriero, D. M. Selective vulnerability of subplate neurons after early neonatal hypoxia-ischemia. J. Neurosci. 23, 3308–3315 (2003).
Hanganu, I. L., Kilb, W. & Luhmann, H. J. Functional synaptic projections onto subplate neurons in neonatal rat somatosensory cortex. J. Neurosci. 22, 7165–7176 (2002).
Nguyen, V. & McQuillen, P. S. AMPA and metabotropic excitoxicity explain subplate neuron vulnerability. Neurobiol. Dis. 37, 195–207 (2010).
Weiss, J. et al. Neonatal hypoxia suppresses oligodendrocyte Nogo-A and increases axonal sprouting in a rodent model for human prematurity. Exp. Neurol. 189, 141–149 (2004).
Ligam, P. et al. Thalamic damage in periventricular leukomalacia: novel pathologic observations relevant to cognitive deficits in survivors of prematurity. Pediatr. Res. 65, 524–529 (2009).
Pendlebury, S. T., Blamire, A. M., Lee, M. A., Styles, P. & Matthews, P. M. Axonal injury in the internal capsule correlates with motor impairment after stroke. Stroke 30, 956–962 (1999).
Manning, S. M. et al. NMDA receptor blockade with memantine attenuates white matter injury in a rat model of periventricular leukomalacia. J. Neurosci. 28, 6670–6678 (2008).
Deng, W., Wang, H., Rosenberg, P. A., Volpe, J. J. & Jensen, F. E. Role of metabotropic glutamate receptors in oligodendrocyte excitotoxicity and oxidative stress. Proc. Natl Acad. Sci. USA 101, 7751–7756 (2004).
Keller, M. et al. Erythropoietin is neuroprotective against NMDA-receptor-mediated excitotoxic brain injury in newborn mice. Neurobiol. Dis. 24, 357–366 (2006).
Sakanaka, M. et al. In vivo evidence that erythropoietin protects neurons from ischemic damage. Proc. Natl Acad. Sci. USA 95, 4635–4640 (1998).
Kumral, A. et al. Neuroprotective effect of erythropoietin on hypoxic-ischemic brain injury in neonatal rats. Biol. Neonate 83, 224–228 (2003).
Sola, A., Rogido, M., Lee, B. H., Genetta, T. & Wen, T. C. Erythropoietin after focal cerebral ischemia activates the Janus kinase-signal transducer and activator of transcription signaling pathway and improves brain injury in postnatal day 7 rats. Pediatr. Res. 57, 481–487 (2005).
Chang, Y. S. et al. Erythropoietin improves functional and histological outcome in neonatal stroke. Pediatr. Res. 58, 106–111 (2005).
Yatsiv, I. et al. Erythropoietin is neuroprotective, improves functional recovery, and reduces neuronal apoptosis and inflammation in a rodent model of experimental closed head injury. FASEB J. 19, 1701–1703 (2005).
Arvin, K. L. et al. Minocycline markedly protects the neonatal brain against hypoxic-ischemic injury. Ann. Neurol. 52, 54–61 (2002).
Amin, A. R. et al. A novel mechanism of action of tetracyclines: effects on nitric oxide synthases. Proc. Natl Acad. Sci. USA 93, 14014–14019 (1996).
Brundula, V., Rewcastle, N. B., Metz, L. M., Bernard, C. C. & Yong, V. W. Targeting leukocyte MMPs and transmigration: minocycline as a potential therapy for multiple sclerosis. Brain 125, 1297–1308 (2002).
Chen, M. et al. Minocycline inhibits caspase-1 and caspase-3 expression and delays mortality in a transgenic mouse model of Huntington disease. Nat. Med. 6, 797–801 (2000).
Diguet, E. et al. Neuroprotective agents for clinical trials in Parkinson's disease: a systematic assessment. Neurology 62, 158 (2004).
Du, Y. et al. Minocycline prevents nigrostriatal dopaminergic neurodegeneration in the MPTP model of Parkinson's disease. Proc. Natl Acad. Sci. USA 98, 14669–14674 (2001).
Kriz, J., Nguyen, M. D. & Julien, J. P. Minocycline slows disease progression in a mouse model of amyotrophic lateral sclerosis. Neurobiol. Dis. 10, 268–278 (2002).
Lee, S. M. et al. Minocycline reduces cell death and improves functional recovery after traumatic spinal cord injury in the rat. J. Neurotrauma 20, 1017–1027 (2003).
Tikka, T. M. et al. Minocycline prevents neurotoxicity induced by cerebrospinal fluid from patients with motor neurone disease. Brain 125, 722–731 (2002).
Teng, Y. D. et al. Minocycline inhibits contusion-triggered mitochondrial cytochrome c release and mitigates functional deficits after spinal cord injury. Proc. Natl Acad. Sci. USA 101, 3071–3076 (2004).
Fan, L. W. et al. Minocycline reduces lipopolysaccharide-induced neurological dysfunction and brain injury in the neonatal rat. J. Neurosci. Res. 82, 71–82 (2005).
Cai, Z., Lin, S., Fan, L. W., Pang, Y. & Rhodes, P. G. Minocycline alleviates hypoxic-ischemic injury to developing oligodendrocytes in the neonatal rat brain. Neuroscience 137, 425–435 (2006).
Zhang, K. & Sejnowski, T. J. A universal scaling law between gray matter and white matter of cerebral cortex. Proc. Natl Acad. Sci. USA 97, 5621–5626 (2000).
Olney, J. W., Ikonomidou, C., Mosinger, J. L. & Frierdich, G. MK-801 prevents hypobaric-ischemic neuronal degeneration in infant rat brain. J. Neurosci. 9, 1701–1704 (1989).
Rothman, S. M. & Olney, J. W. Glutamate and the pathophysiology of hypoxic–ischemic brain damage. Ann. Neurol. 19, 105–111 (1986).
Lipton, S. A. & Rosenberg, P. A. Excitatory amino acids as a final common pathway for neurologic disorders. N. Engl. J. Med. 330, 613–622 (1994).
Choi, D. W. & Rothman, S. M. The role of glutamate neurotoxicity in hypoxic-ischemic neuronal death. Annu. Rev. Neurosci. 13, 171–182 (1990).
Choi, D. W. Excitotoxic cell death. J. Neurobiol. 23, 1261–1276 (1992).
Yoshioka, A., Bacskai, B. & Pleasure, D. Pathophysiology of oligodendroglial excitotoxicity. J. Neurosci. Res. 46, 427–437 (1996).
Yoshioka, A. et al. Non-N-methyl-D-aspartate glutamate receptors mediate oxygen–glucose deprivation-induced oligodendroglial injury. Brain Res. 854, 207–215 (2000).
Itoh, T. et al. AMPA glutamate receptor-mediated calcium signaling is transiently enhanced during development of oligodendrocytes. J. Neurochem. 81, 390–402 (2002).
Itoh, T. et al. Diminished calcium homeostasis and increased susceptibility to excitotoxicity of JS 3/16 progenitor cells after differentiation to oligodendroglia. Glia 31, 165–180 (2000).
Matute, C., Sanchéz-Goméz, M. V., Martinez-Millán, L. & Miledi, R. Glutamate receptor-mediated toxicity in optic nerve oligodendrocytes. Proc. Natl Acad. Sci. USA 94, 8830–8835 (1997).
McDonald, J. W., Althomsons, S. P., Hyrc, K. L., Choi, D. W. & Goldberg, M. P. Oligodendrocytes from forebrain are highly vulnerable to AMPA/kainate receptor-mediated excitotoxicity. Nat. Med. 4, 291–297 (1998).
Fern, R. & Moller, T. Rapid ischemic cell death in immature oligodendrocytes: a fatal glutamate release feedback loop. J. Neurosci. 20, 34–42 (2000).
Baumann, N. & Pham-Dinh, D. Biology of oligodendrocyte and myelin in the mammalian central nervous system. Physiol. Rev. 81, 871–927 (2001).
Haynes, R. L. et al. Oxidative and nitrative injury in periventricular leukomalacia: a review. Brain Pathol. 15, 225–233 (2005).
Haynes, R. L. et al. Nitrosative and oxidative injury to premyelinating oligodendrocytes in periventricular leukomalacia. J. Neuropathol. Exp. Neurol. 62, 441–450 (2003).
Dommergues, M. A., Plaisant, F., Verney, C. & Gressens, P. Early microglial activation following neonatal excitotoxic brain damage in mice: a potential target for neuroprotection. Neuroscience 121, 619–628 (2003).
Noda, M., Nakanishi, H., Nabekura, J. & Akaike, N. AMPA-kainate subtypes of glutamate receptor in rat cerebral microglia. J. Neurosci. 20, 251–258 (2000).
Ivacko, J. A., Sun, R. & Silverstein, F. S. Hypoxic-ischemic brain injury induces an acute microglial reaction in perinatal rats. Pediatr. Res. 39, 39–47 (1996).
Silverstein, F. S. et al. Cytokines and perinatal brain injury. Neurochem. Int. 30, 375–383 (1997).
Debillon, T. et al. Patterns of cerebral inflammatory response in a rabbit model of intrauterine infection-mediated brain lesion. Brain Res. Dev. Brain Res. 145, 39–48 (2003).
Debillon, T. et al. Effect of maternal antibiotic treatment on fetal periventricular white matter cell death in a rabbit intrauterine infection model. Acta Paediatr. 92, 81–86 (2003).
Saliba, E. & Henrot, A. Inflammatory mediators and neonatal brain damage. Biol. Neonate 79, 224–227 (2001).
Park, S. Y., Billiar, T. R. & Seol, D. W. Hypoxia inhibition of apoptosis induced by tumor necrosis factor-related apoptosis-inducing ligand (TRAIL). Biochem. Biophys. Res. Commun. 291, 150–153 (2002).
Pang, Y., Cai, Z. & Rhodes, P. G. Disturbance of oligodendrocyte development, hypomyelination and white matter injury in the neonatal rat brain after intracerebral injection of lipopolysaccharide. Brain Res. Dev. Brain Res. 140, 205–214 (2003).
Hermann, G. E., Rogers, R. C., Bresnahan, J. C. & Beattie, M. S. Tumor necrosis factor-alpha induces cFOS and strongly potentiates glutamate-mediated cell death in the rat spinal cord. Neurobiol. Dis. 8, 590–599 (2001).
Barger, S. W. & Basile, A. S. Activation of microglia by secreted amyloid precursor protein evokes release of glutamate by cystine exchange and attenuates synaptic function. J. Neurochem. 76, 846–854 (2001).
Golde, S., Chandran, S., Brown, G. C. & Compston, A. Different pathways for iNOS-mediated toxicity in vitro dependent on neuronal maturation and NMDA receptor expression. J. Neurochem. 82, 269–282 (2002).
Murphy, S. Production of nitric oxide by glial cells: regulation and potential roles in the CNS. Glia 29, 1–13 (2000).
Bernardo, A., Greco, A., Levi, G. & Minghetti, L. Differential lipid peroxidation, Mn superoxide, and bcl-2 expression contribute to the maturation-dependent vulnerability of oligodendrocytes to oxidative stress. J. Neuropathol. Exp. Neurol. 62, 509–519 (2003).
Tikka, T., Fiebich, B. L., Goldsteins, G., Keinanen, R. & Koistinaho, J. Minocycline, a tetracycline derivative, is neuroprotective against excitotoxicity by inhibiting activation and proliferation of microglia. J. Neurosci. 21, 2580–2588 (2001).
Lechpammer, M. et al. Minocycline treatment following hypoxic/ischaemic injury attenuates white matter injury in a rodent model of periventricular leucomalacia. Neuropathol. Appl. Neurobiol. 34, 379–393 (2008).
Acknowledgements
The author thanks Dr. V. Selvaraj for his critical reading of this manuscript. This work was in part supported by grants from the NIH (RO1 NS059043 and RO1 ES015988), the National Multiple Sclerosis Society, the Roche Foundation for Anemia Research, the Feldstein Medical Foundation, and Shriners Hospitals for Children.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Deng, W. Neurobiology of injury to the developing brain. Nat Rev Neurol 6, 328–336 (2010). https://doi.org/10.1038/nrneurol.2010.53
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2010.53
This article is cited by
-
Atorvastatin Promotes Pro/anti-inflammatory Phenotypic Transformation of Microglia via Wnt/β-catenin Pathway in Hypoxic-Ischemic Neonatal Rats
Molecular Neurobiology (2024)
-
Akt/mTOR Pathway Agonist SC79 Inhibits Autophagy and Apoptosis of Oligodendrocyte Precursor Cells Associated with Neonatal White Matter Dysplasia
Neurochemical Research (2023)
-
Caffeine treatment started before injury reduces hypoxic–ischemic white-matter damage in neonatal rats by regulating phenotypic microglia polarization
Pediatric Research (2022)
-
Oligodendrocyte lineage cells and depression
Molecular Psychiatry (2021)
-
MiRNA-210 induces microglial activation and regulates microglia-mediated neuroinflammation in neonatal hypoxic-ischemic encephalopathy
Cellular & Molecular Immunology (2020)