Abstract
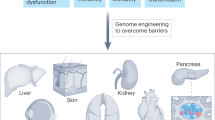
Exciting new technologies, such as cellular transplantation, organogenesis and xenotransplantation, are thought to be promising approaches for the treatment of human disease. The feasibility of applying these technologies, however, might be limited by biological and immunological hurdles. Here, we consider whether, and how, xenotransplantation and various other technologies might be applied in future efforts to replace or supplement the function of human organs and tissues.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
SoRelle, R. Totally contained AbioCor artificial heart implanted. Circulation 104, E9005–E9006 (2001).
Murry, C. E., Wiseman, R. W., Schwartz, S. M. & Hauschka, S. D. Skeletal myoblast transplantation for repair of myocardial necrosis. J. Clin. Invest. 98, 2512–2523 (1996).
Taylor, D. A. et al. Regenerating functional myocardium: improved performance after skeletal myoblast transplantation. Nature Med. 4, 929–933 (1998).
Menasche, P. et al. Myoblast transplantation for heart failure. Lancet 357, 279–280 (2001).
Fox, I. et al. Treatment of the Crigler–Najjar syndrome type I with hepatocyte transplantation. N. Engl. J. Med. 338, 1422–1426 (1998).
Gunsalus, J. R., Brady, D. A., Coulter, S. M., Gray, B. M. & Edge, A. Reduction of serum cholesterol in watanabe rabbits by xenogeneic hepatocellular transplantation. Nature Med. 3, 48–53 (1997).
Lagasse, E. et al. Purified hematopoietic stem cells can differentiate into hepatocytes in vivo. Nature Med. 6, 1229–1234 (2000).
Clarke, D. L. et al. Generalized potential of adult neural stem cells. Science 288, 1660–1663 (2000).
Zuk, P. A. et al. Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng. 7, 211–228 (2001).
Thomson, J. A. et al. Embryonic stem cell lines derived from human blastocysts. Science 282, 1145–1147 (1998).
Grobstein, C. Inductive epithelio–mesenchymal interaction in cultured organ rudiments of the mouse. Science 118, 52–55 (1953).
Ekblom, P. Formation of basement membranes in the embryonic kidney: an immunohistological study. J. Cell Biol. 91, 1–10 (1981).
Hammerman, M. R. Growing kidneys. Curr. Opin. Nephrol. Hypertens. 10, 13–17 (2001).
Cascalho, M. & Platt, J. L. The immunological barrier to xenotransplantation. Immunity 14, 437–446 (2001).
Dorling, A., Lombardi, G., Binns, R. & Lechler, R. I. Detection of primary direct and indirect human anti-porcine T cell responses using a porcine dendritic cell population. Eur. J. Immunol. 26, 1378–1387 (1996).
Gritsch, H. A. et al. The importance of nonimmune factors in reconstitution by discordant xenogeneic hematopoietic cells. Transplantation 57, 906–917 (1994).
Bennet, W. et al. Expression of complement regulatory proteins on islets of Langerhans: a comparison between human islets and islets isolated from normal and hDAF transgenic pigs. Transplantation 72, 312–319 (2001).
Murray, A. G., Khodadoust, M. M., Pober, J. S. & Bothwell, A. L. M. Porcine aortic endothelial cells activate human T cells: direct presentation of MHC antigens and costimulation by ligands for human CD2 and CD28. Immunity 1, 57–63 (1994).
Yamada, K., Sachs, D. H. & DerSimonian, H. Human anti-porcine xenogeneic T cell response. Evidence for allelic specificity of mixed leukocyte reaction and for both direct and indirect pathways of recognition. J. Immunol. 155, 5249–5256 (1995).
Platt, J. L. New directions for organ transplantation. Nature 392 (Suppl.), 11–17 (1998).
Auchincloss, H. Jr & Sachs, D. H. Xenogeneic transplantation. Annu. Rev. Immunol. 16, 433–470 (1998).
Marchetti, P. et al. Prolonged survival of discordant porcine islet xenografts. Transplantation 61, 1100–1102 (1996).
Deacon, T. et al. Histological evidence of fetal pig neural cell survival after transplantation into a patient with Parkinson's disease. Nature Med. 3, 350–353 (1997).
Platt, J. L. Hyperacute xenograft rejection (RG Landes Co., Austin, Texas, 1995).
Galili, U., Clark, M. R., Shohet, S. B., Buehler, J. & Macher, B. A. Evolutionary relationship between the natural anti-Gal antibody and the Gal α1-3Gal epitope in primates. Proc. Natl Acad. Sci. USA 84, 1369–1373 (1987).
Zaidi, A. et al. Life-supporting pig-to-primate renal xenotransplantation using genetically modified donors. Transplantation 65, 1584–1590 (1998).
Lachmann, P. J. The control of homologous lysis. Immunol. Today 12, 312–315 (1991).
Hourcade, D., Holers, V. M. & Atkinson, J. P. The regulators of complement activation (RCA) gene cluster. Adv. Immunol. 45, 381–416 (1989).
Platt, J. L. et al. Transplantation of discordant xenografts: a review of progress. Immunol. Today 11, 450–456 (1990).
Van den Berg, C. W. & Morgan, B. P. Complement-inhibiting activities of human CD59 and analogues from rat, sheep, and pig are not homologously restricted. J. Immunol. 152, 4095–4101 (1994).
Diamond, L. E. et al. Characterization of transgenic pigs expressing functionally active human CD59 on cardiac endothelium. Transplantation 61, 1241–1249 (1996).
Saadi, S. & Platt, J. L. Transient perturbation of endothelial integrity induced by natural antibodies and complement. J. Exp. Med. 181, 21–31 (1995).
McCurry, K. R. et al. Human complement regulatory proteins protect swine-to-primate cardiac xenografts from humoral injury. Nature Med. 1, 423–427 (1995).
Leventhal, J. R. et al. The immunopathology of cardiac xenograft rejection in the guinea pig-to-rat model. Transplantation 56, 1–8 (1993).
Blakely, M. L. et al. Activation of intragraft endothelial and mononuclear cells during discordant xenograft rejection. Transplantation 58, 1059–1066 (1994).
Shimizu, A. et al. Acute humoral xenograft rejection: destruction of the microvascular capillary endothelium in pig-to-nonhuman primate renal grafts. Lab. Invest. 80, 815–830 (2000).
Sachs, D. H. & Sablinski, T. Tolerance across discordant xenogeneic barriers. Xenotransplantation 2, 234–239 (1995).
Sablinski, T. et al. Long-term discordant xenogeneic (porcine-to-primate) bone marrow engraftment in a monkey treated with porcine-specific growth factors. Transplantation 67, 972–977 (1999).
Ierino, F. L. et al. Disseminated intravascular coagulation in association with the delayed rejection of pig-to-baboon renal xenografts. Transplantation 66, 1439–1450 (1998).
Onishi, A. et al. Pig cloning by microinjection of fetal fibroblast nuclei. Science 289, 1188–1190 (2000).
Polejaeva, I. A. et al. Cloned piglets produced by nuclear transfer from adult somatic cells. Nature 407, 86–90 (2000).
Betthauser, J. et al. Production of cloned pigs from in vitro systems. Nature Biotechnol. 18, 1055–1059 (2000).
Denning, C. et al. Deletion of the α(1,3) galactosyl transferase (GGTA1) gene and the prion protein (PrP) gene in sheep. Nature Biotechnology 19, 559–562 (2001).
Lin, S. S. et al. The role of anti-Galα1-3Gal antibodies in acute vascular rejection and accommodation of xenografts. Transplantation 70, 1667–1674 (2000).
Bach, F. H., Winkler, H., Ferran, C., Hancock, W. W. & Robson, S. C. Delayed xenograft rejection. Immunol. Today 17, 379–384 (1996).
Chopek, M. W., Simmons, R. L. & Platt, J. L. ABO-incompatible renal transplantation: initial immunopathologic evaluation. Transplant. Proc. 19, 4553–4557 (1987).
Bannett, A. D., McAlack, R. F., Morris, M., Chopek, M. & Platt, J. L. ABO incompatible renal transplantation: a qualitative analysis of native endothelial tissue ABO antigens after transplant. Transplant. Proc. 21, 783–785 (1989).
Lin, Y., Vandeputte, M. & Waer, M. Accommodation and T-independent B cell tolerance in rats with long term surviving hamster heart xenografts. J. Immunol. 160, 369–375 (1998).
Hancock, W. W., Buelow, R., Sayegh, M. H. & Turka, L. A. Antibody-induced transplant arteriosclerosis is prevented by graft expression of anti-oxidant and anti-apoptotic genes. Nature Med. 4, 1392–1396 (1998).
Schmoeckel, M. et al. Orthotopic heart transplantation in a transgenic pig-to-primate model. Transplantation 65, 1570–1577 (1998).
Sablinski, T. et al. Xenotransplantation of pig kidneys to nonhuman primates: I. Development of the model. Xenotransplantation 2, 264–270 (1995).
Daggett, C. W. et al. Total respiratory support from swine lungs in primate recipients. J. Thorac. Cardiovasc. Surg. 115, 19–27 (1998).
Ramirez, P. et al. Life-supporting human complement regulator decay accelerating factor transgenic pig liver xenograft maintains the metabolic function and coagulation in the nonhuman primate for up to 8 days. Transplantation 70, 989–998 (2000).
Patience, C., Takeuchi, Y. & Weiss, R. A. Infection of human cells by an endogenous retrovirus of pigs. Nature Med. 3, 282–286 (1997).
Patience, C. et al. No evidence of pig DNA or retroviral infection in patients with short-term extracorporeal connection to pig kidneys. Lancet 352, 699–701 (1998).
Paradis, K. et al. Search for cross-species transmission of porcine endogenous retrovirus in patients treated with living pig tissue. Science 285, 1236–1241 (1999).
Andres, G. et al. Cellular mechanisms of adaptation of grafts to antibody. Transpl. Immunol. 4, 1–17 (1996).
Dalmasso, A. P., Benson, B. A., Johnson, J. S., Lancto, C. & Abrahamsen, M. S. Resistance against the membrane attack complex of complement induced in porcine endothelial cells with a Gal α(1-3)Gal binding lectin: up-regulation of CD59 expression. J. Immunol. 164, 3764–3773 (2000).
Delikouras, A., Hayes, M., Malde, P., Lechler, R. I. & Dorling, A. Nitric oxide-mediated expression of Bcl-2 and Bcl-xl and protection from TNFα–mediated apoptosis in porcine endothelial cells after exposure to low concentrations of xenoreactive natural antibody. Transplantation 71, 599–605 (2001).
Bach, F. H. et al. Accommodation of vascularized xenografts: expression of 'protective genes' by donor endothelial cells in a host TH2 cytokine environment. Nature Med. 3, 196–204 (1997).
Soares, M. P. et al. Expression of heme oxygenase-1 can determine cardiac xenograft survival. Nature Med. 4, 1073–1077 (1998).
Imai, T. et al. Vascular smooth muscle cell-directed overexpression of heme oxygenase-1 elevates blood pressure through attenuation of nitric oxide-induced vasodilation in mice. Circ. Res. 89, 55–62 (2001).
Holzknecht, Z. E. & Platt, J. L. Accommodation and the reversibility of biological systems. Transplantation 71, 594–595 (2001).
Magee, J. C. et al. Immunoglobulin prevents complement mediated hyperacute rejection in swine-to-primate xenotransplantation. J. Clin. Invest. 96, 2404–2412 (1995).
Nagayasu, T. et al. Expression of tissue factor mRNA in cardiac xenografts: clues to the pathogenesis of acute vascular rejection. Transplantation 69, 475–482 (2000).
Parker, W. et al. Transplantation of discordant xenografts: a challenge revisited. Immunol. Today 17, 373–378 (1996).
Cooper, D. K. C. et al. Effects of cyclosporine and antibody adsorption on pig cardiac xenograft survival in the baboon. J. Heart Transplant. 7, 238–246 (1988).
Lin, S. S. et al. The role of natural anti-Galα1-3Gal antibodies in hyperacute rejection of pig-to-baboon cardiac xenotransplants. Transpl. Immunol. 5, 212–218 (1997).
Leventhal, J. R. et al. Prolongation of cardiac xenograft survival by depletion of complement. Transplantation 55, 857–866 (1993).
Pruitt, S. K. et al. The effect of soluble complement receptor type 1 on hyperacute rejection of porcine xenografts. Transplantation 57, 363–370 (1994).
Cozzi, E. et al. in Xenotransplantation: The Transplantation of Organs and Tissues Between Species (eds Cooper, D. K. C., Kemp, E., Platt, J. L. & White, D. J. G.) 665–682 (Springer, Berlin, 1997).
Diamond, L. E. et al. A human CD46 transgenic pig model system for the study of discordant xenotransplantation. Transplantation 71, 132–142 (2001).
Bracy, J. L., Sachs, D. H. & Iacomini, J. Inhibition of xenoreactive natural antibody production by retroviral gene therapy. Science 281, 1845–1847 (1998).
Acknowledgements
Work in the laboratories of the authors is supported by grants from the National Institutes of Health and by the Von Liebig Foundation.
Author information
Authors and Affiliations
Corresponding author
Related links
Related links
DATABASES
FURTHER INFORMATION
Glossary
- ALLOGENEIC
-
Of, or relating to, the same species; for example, allogeneic transplants are transplants between individuals of the same species.
- ISCHAEMIA
-
A condition in which the flow of blood to a tissue or organ is less than normal, and which results in injury to that tissue or organ.
- ISLETS OF LANGERHANS
-
The tissue of the pancreas that contains endocrine cells, including the β-cells that secrete insulin.
- SUBSTANTIA NIGRA
-
A part of the brain affected by Parkinson's disease.
- XENOGENEIC
-
Of, or relating to, a foreign species.
Rights and permissions
About this article
Cite this article
Cascalho, M., Platt, J. Xenotransplantation and other means of organ replacement. Nat Rev Immunol 1, 154–160 (2001). https://doi.org/10.1038/35100578
Issue Date:
DOI: https://doi.org/10.1038/35100578
This article is cited by
-
Novel Immunomodulatory Approaches for Porcine Islet Xenotransplantation
Current Diabetes Reports (2021)
-
The production of UL16-binding protein 1 targeted pigs using CRISPR technology
3 Biotech (2018)
-
Regenerating a kidney in a lymph node
Pediatric Nephrology (2016)
-
Regeneration and Bioengineering of the Kidney: Current Status and Future Challenges
Current Urology Reports (2014)
-
Survival of Partially Differentiated Mouse Embryonic Stem Cells in the Scala Media of the Guinea Pig Cochlea
Journal of the Association for Research in Otolaryngology (2005)