Abstract
Mesolimbic dopamine (DA) controls drug- and alcohol-seeking behavior, but the role of specific DA receptor subtypes is unclear. We tested the hypothesis that D3R gene deletion or the D3R pharmacological blockade inhibits ethanol preference in mice. D3R-deficient mice (D3R−/−) and their wild-type (WT) littermates, treated or not with the D3R antagonists SB277011A and U99194A, were tested in a long-term free choice ethanol-drinking (two-bottle choice) and in a binge-like ethanol-drinking paradigm (drinking in the dark, DID). The selectivity of the D3R antagonists was further assessed by molecular modeling. Ethanol intake was negligible in D3R−/− and robust in WT both in the two-bottle choice and DID paradigms. Treatment with D3R antagonists inhibited ethanol intake in WT but was ineffective in D3R−/− mice. Ethanol intake increased the expression of RACK1 and brain-derived neurotrophic factor (BDNF) in both WT and D3R−/−; in WT there was also a robust overexpression of D3R. Thus, increased expression of D3R associated with activation of RACK1/BDNF seems to operate as a reinforcing mechanism in voluntary ethanol intake. Indeed, blockade of the BDNF pathway by the TrkB selective antagonist ANA-12 reversed chronic stable ethanol intake and strongly decreased the striatal expression of D3R. Finally, we evaluated buspirone, an approved drug for anxiety disorders endowed with D3R antagonist activity (confirmed by molecular modeling analysis), that resulted effective in inhibiting ethanol intake. Thus, DA signaling via D3R is essential for ethanol-related reward and consumption and may represent a novel therapeutic target for weaning.
Similar content being viewed by others
INTRODUCTION
The mesolimbic dopamine (DA) pathway mediates the rewarding effects of drugs of abuse (Bowers et al, 2010; Ikemoto and Bonci, 2013; Koob, 1992; Robbins and Everitt, 1996; Wise and Bozarth, 1987), including ethanol and opiates (Pierce and Kumaresan, 2006; Wise and Bozarth, 1987). Both oral self-administration (Weiss et al, 1992) and systemic administration of ethanol increase the firing rate of mesolimbic dopaminergic neurons (Gessa et al, 1985; Mereu et al, 1984) and stimulate extracellular DA release in the striatum and in the nucleus accumbens (Imperato and Di Chiara, 1986; Yoshimoto et al, 1992). In a recent meta-analysis on published data sets of in vivo microdialysis in rat brain, the acute administrations of ethanol appear to increase the level of monoamines, including DA, globally and independent of the brain sites up to 270% of the basal concentrations (Brand et al, 2013). DA exerts its action through five receptor subtypes (D1–5R); the D3 receptor (D3R) subtype has an important role in the modulation of the mesolimbic DA pathway and in the control of drug-seeking behavior (Heidbreder et al, 2005; Joyce and Millan, 2005). The D3R is located both at pre- and post-synapses, in the ventral striatum (nucleus accumbens and island of Calleja (Bouthenet et al, 1991; Murray et al, 1994)); in these structures, stimulation of presynaptic D3R may modulate DA synthesis and release (Levant, 1997). Several studies have explored the involvement of D3R in ethanol-drinking paradigms (Cohen et al, 1998; Harrison and Nobrega, 2009; Heidbreder et al, 2007; Rice et al, 2012; Silvestre et al, 1996; Thanos et al, 2005), but their precise role remains unclear. Indeed, pharmacological studies generally report that D3R blockade decreases ethanol consumption (Heidbreder et al, 2007; Rice et al, 2012; Silvestre et al, 1996; Vengeliene et al, 2006); in contrast, genetic manipulation studies did not find a change in ethanol intake following D3R gene deletion (McQuade et al, 2003).
In the present study, we tested the hypothesis that D3R gene deletion or the D3R pharmacological blockade inhibits the ethanol preference and the voluntary intake in mice. Mice D3R−/− and their wild-type (WT) littermates, treated or not with D3R selective antagonists, were tested in a long-term free choice ethanol-drinking paradigm (two-bottle choice) (McQuade et al, 2003; Wise, 1973) and in a binge-like ethanol-drinking paradigm (drinking in the dark, DID). Activation of the RACK1/BDNF (brain-derived neurotrophic factor)/D3R pathway (Jeanblanc et al, 2006) and activation of DA transmission were assessed at the end of behavioral experiments. The RACK1/BDNF/D3R pathway was here considered because D3R expression is related to BDNF (Guillin et al, 2001; Le Foll et al, 2005b) and ethanol exposure is able to increase RACK1 translocation into the nucleus of neurons, which increases expression of BDNF (Jeanblanc et al, 2006; McGough et al, 2004). Finally, the effect of buspirone was evaluated in the drinking paradigms. Because buspirone is an already approved drug for anxiety disorders, endowed with D3R antagonist activity, it may be easier to translate to the clinic practice.
MATERIALS AND METHODS
Animals
Mice D3R null (D3R−/−) and WT littermates (males, 8–12 weeks old) were individually housed, with free access to chow and water (except in the ethanol-drinking procedures), in an air-conditioned room, with a 12-h light–dark cycle. Mice D3R−/− were 10th–12th generation of congenic C57BL/6J mice, generated by a back-crossing strategy (Accili et al, 1996). All experiments were carried out according to the Directive 2010/63/EU and to the Institutional Animal Care and Use Committee of the Catania University.
Two-Bottle Choice Paradigm
Mice D3R−/− (n=30) and WT (n=30) received 24 h free access to tap water and 10% ethanol solution (v/v), contained in 100 ml graduated tubes with stainless steel drinking spouts; the position of tubes was interchanged (left/right) every 24 h, to prevent acquisition of position bias. Ethanol and water intake was measured as daily consumption in grams. The experiments lasted 59 days. For the first 15 days, (habituation period) animals received 24 h free access to two tubes containing only tap water (time 0 in Figure 1a). After the habituation period (from 15 to 59 days), 10% ethanol solution was available in one of the bottles.
In the two-bottle choice paradigm, D3−/− mice show a lower voluntary ethanol intake as compared with wild-type (WT). D3 pharmacological antagonism inhibits ethanol intake in WT mice. (a, b) Voluntary ethanol intake was measured every 24 h, for 44 days, in WT (n=30) and D3−/− (n=30) mice that had free access to water and ethanol solution (10%). (c) Shows total fluid intake that was not different in the two groups. (d, e), Voluntary ethanol intake was measured as in a, but in mice that had received the day before and kept receiving daily i.p. injection of either saline (vehicle, VEH, n=10), U99194A (n=10) or SB277011A (n=10), either drug at 10 mg/kg. (f) Total fluid intake in either group that was not affected by drug treatment. ***p<0.001 vs water or vehicle (VEH). One-way ANOVA and Newman–Keuls post hoc test.
In the forced alcohol-drinking procedure, D3R−/− (n=12) and WT (n=18) received for the first 15 days (habituation period) tap water only (time 0), followed (from 15 to 59 days) by 10% ethanol only.
DID Paradigm
The 4 h version of the behavioral paradigm was used, as described by Rhodes et al (2005). The procedure started 3 h after lights off in the animal room. Water bottles were replaced with graduated tubes with stainless steel drinking spouts containing 20% (v/v) ethanol in tap water. This was done in home cages where animals were singly housed (Rhodes et al, 2005). The ethanol tubes remained in place for 2 h. After the 2-h period, intakes were recorded, and the ethanol tubes were replaced with water tubes. This procedure was repeated on days 2 and 3. On day 4, the procedure was again repeated except that the ethanol tubes were left in place for 4 h, and intakes were recorded after 4 h.
Drugs and Treatments
Ethanol, U99194A maleate, SB277011A hydrochloride, buspirone hydrochloride, 8-OH-DPAT and ANA-12 were from Sigma (St Louis, MO). All drugs were dissolved in saline and intraperitoneally (i.p.) injected (in a volume of 10 ml/kg), except ANA-12 that was dissolved in 10% dimethyl sulfoxide. U99194A was used at 10 mg/kg (Harrison and Nobrega, 2009), SB277011A was used at 10 mg/kg (Song et al, 2012), buspirone was used in the range 0.1–10 mg/kg (Martin et al, 1992), 8-OH-DPAT was used at 1 mg/kg (Martin et al, 1992), and ANA-12 was used at 0.5 mg/kg (Cazorla et al, 2011).
In the two-bottle choice paradigm, after 30 days of voluntary alcohol-drinking procedure, D3R−/− and WT were randomly allocated to the eight experimental groups (n=6/10 per group): WT/vehicle, WT/U99194A, WT/SB277011A, WT/buspirone, D3R−/−/vehicle, D3R−/−/U99194A, D3R−/−/SB277011A, and D3R−/−/buspirone. Animals were i.p. injected once a day, for 14 consecutive days. On day 14, animals were sacrificed 1 h after the last administration and brain tissues were taken. In another set of experiments, after 30 days of voluntary alcohol-drinking procedure, mice were randomly allocated to five experimental groups (n=5/7 per group): WT naïve, WT/vehicle, WT/ANA-12, D3R−/−/vehicle, and D3R−/−/ANA-12. Animals were i.p. injected once a day, for 4 consecutive days with the selective Trkb antagonist ANA-12 at 0.5 mg/kg (Cazorla et al, 2011; Vassoler et al, 2013). On day 4, animals were sacrificed 1 h after the last administration and brain tissues were taken.
In the DID paradigm, mice were allocated to 10 experimental groups (n=5/6 per group): WT naïve, D3R−/− naïve, WT/vehicle, D3R−/−/vehicle, WT/SB277011A, D3R−/−/SB277011A, WT/buspirone 0.1 mg/kg, WT/buspirone 1 mg/kg, WT/buspirone 3 mg/kg, and WT/buspirone 10 mg/kg. In another set of experiments, mice were allocated to four experimental groups (n=5/6 per group): WT/vehicle, WT/8-OH-DPAT, D3R−/−/vehicle, and D3R−/−/8-OH-DPAT, and they were tested in the DID paradigm. Animals were i.p. injected 1 h before the behavioral procedure.
8-OH-DPAT-Induced Hypothermia
Body temperature was measured intrarectally using a lubricated probe inserted ∼2 cm and a digital thermometer (CEM advanced thermometer; DT-610B). Mice were moved to the behavioral room and two baseline temperature measurements were taken. After 10 min, animals received an i.p. injection of vehicle or 1 mg/kg 8-OH-DPAT or 3 mg/kg buspirone. The body temperature was recorded every 15 min for a total of 45 min.
Analysis of mRNA Expression by Real-Time Quantitative RT-PCR
Total RNA was isolated by TRIzol (Invitrogen, Carlsbad, CA). Single-stranded cDNA was synthesized with SuperScript III (Invitrogen), by priming with oligo-(dT)20. Aliquots of cDNA were amplified in parallel reactions with external standards at known amounts, using specific primer pairs for D3R, RACK1, BDNF, and S18 ribosomal RNA (reference gene). Each PCR reaction (20 μl final volume) contained 0.5 μM primers, 1.6 mM Mg2+, and 1 × Light Cycler-Fast Start DNA Master SYBR Green I (Roche Diagnostics, Indianapolis, IN). Amplifications were carried out in a Light Cycler 1.5 instrument (Roche Diagnostics). Quantification was obtained by the ΔCt comparative method.
Western Blot Analysis
Protein extracts from striatum and cerebellum were run in SDS-PAGE, blotted, and probed for non-phosphorylated and phosphorylated forms of DARPP-32, GSK-3β, and Trkb, with primary antibodies (Cell Signalling Technology, Beverly, MA), diluted at 1:1000, and secondary antibody (goat anti-rabbit IRDye; Li-Cor Biosciences, Lincoln, NE). Blots were scanned with an Odyssey Infrared Imaging System (Li-Cor Biosciences) and analyzed with ImageJ software (NIH, Bethesda, MD; http://rsb.info.nih.gov/ij/index.html).
Statistical Analysis
Data were analyzed using one- or two-way analysis of variance (ANOVA). The post hoc Newman–Keuls test was used for multiple comparisons; p-values <0.05 were considered as significant.
RESULTS
D3R−/− Mice Exhibited Lower Ethanol Intake
As shown in Figure 1a and b, WT mice exhibited a high intake of ethanol-containing solution. In contrast, D3R−/− mice showed a low ethanol intake (Figure 1a and b). During the entire period of observation (44 days), WT mice maintained their preferential intake of ethanol, whereas D3R−/− mice maintained a preferential intake of water (F(1,307)=1170.08, p<0.001). There was no difference between WT and D3R−/− in terms of total amount of fluid intake (ethanol+water) (Figure 1c). In the DID paradigm, D3R−/− mice also showed a lower ethanol intake compared with their WT counterparts (F(3,97)=13.90, p<0.01, 2nd day; F(3,97)=21.04, p<0.001, 3rd day; Figure 2a).
In the drinking in the dark (DID) paradigm, D3−/− mice show a lower ethanol intake as compared with their wild-type (WT) littermates. The D3 antagonist SB277011A inhibits ethanol intake of WT but not in D3−/− mice. (a) DID was measured, for 4 days, in WT (n=12) and D3−/− (n=12) mice that had limited access (2 h/day for 3 days and 4 h the 4th day) to ethanol solution (20%). (b, c) Voluntary ethanol intake was measured as in a, but in mice that had received the day before and kept receiving daily i.p. injection of either saline (vehicle, VEH, n=10), or SB277011A (n=10), at 10 mg/kg. *p<0.05, **p<0.01, ***p<0.001 vs wild-type (WT) or vehicle (VEH). One-way ANOVA and Newman–Keuls post hoc test.
Blockade of D3R Inhibited Ethanol Intake
In the two-bottle choice paradigm, after 30 days of stable ethanol/water intake, mice were treated with D3R antagonists (U99194A or SB277011A). As shown in Figure 1d and e, treatment of WT with each D3R antagonist decreased voluntary ethanol intake (F(2,56)=55.23 p<0.01, for both U99194A and SB277011A). Treatment of D3R−/− with U99194A and SB277011A did not change ethanol intake (data not shown). Neither in WT nor in D3R−/− total fluid intake was affected by treatments (Figure 1f and data not shown). SB277011A also significantly decreased ethanol intake in WT mice tested in the DID (F(3,48)=8.67, p<0.01, 1st day; p<0.05 2nd day; Figure 2b), while it did not change ethanol intake of D3R−/− in the DID paradigm (Figure 2c).
RACK1, BDNF, and DA D3R Expression were Increased in the Striatum of WT Mice Following Chronic Ethanol Intake
BDNF induces D3 receptor expression in the ventral striatum, both during development and in adulthood (Guillin et al, 2001). RACK1, a mediator of chromatin remodeling, regulates in an exon-specific manner the expression of the BDNF gene (He et al, 2010) and the RACK1/BDNF pathway is activated upon exposure to ethanol (McGough et al, 2004). We therefore assessed D3R, BDNF, and RACK1 mRNA expression in striatum of WT that had free access to either water only or to both water and ethanol. Figure 3a shows that chronic ethanol intake increased D3R mRNA expression in striatum (F(3,23)=170.4, p<0.05). Long-term access to ethanol also increased BDNF (Figure 3b, F(7,47)=48.05, p<0.01) and RACK1 (Figure 3c, F(7,47)=21.14, p<0.01) mRNA in striatum of WT mice.
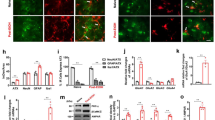
Chronic ethanol intake induces D3 upregulation, associated with the activation of BDNF/RACK1 pathway. Abundance of transcripts in striatum was assessed by quantitative RT-PCR after 44 days of free access to water only (white columns), or to both water and ethanol (black columns, upper panels) or forced ethanol intake (black columns lower panels). In the forced alcohol-drinking procedure (d–h), D3R−/− and WT received 10% ethanol only, with or without SB277011A or buspirone for 14 days. (a, f) D3 Expression profile in WT; (b, d, g) brain-derived neurotrophic factor (BDNF) expression profile in WT and D3−/−; (c, e, h) RACK1 expression profile in WT and D3−/−. Mean fold changes are expressed relative to transcript levels in controls (WT having access to water only). Each column is the mean (± SEM) from five different samples. *p<0.05, **p<0.01 vs water. One-way ANOVA and Newman–Keuls post hoc test.
Long-term ethanol exposure appeared to be associated with BDNF/RACK1 overexpression, but interpretation of these data was made difficult by the different ethanol intake in the two genetic groups, as it was very high in WT and very low in D3R−/−. To address this issue, some WT and D3R−/− mice were subjected to forced ethanol intake, that is, they had access to ethanol 10% solution only. As shown in Figure 3d and e, forced ethanol intake induced a significant overexpression of BDNF (F(7,47)=48.05, p<0.05, p<0.01) and RACK1 (F(7,47)=21.14, p<0.05, p<0.05) mRNAs in striatum of both WT and D3R−/− mice. We also tested the effects of the D3R antagonists SB277011A and buspirone (see also below) on mRNA expression of D3R, BDNF, and RACK1. None of these values were changed by a 14-day treatment with SB277011A or buspirone (Figure 3f–h).
Blockade of the BDNF Receptor TrkB Inhibited Ethanol Intake and Decreased D3R Expression
TrkB is the high affinity receptor for BDNF, belonging to the family of tyrosine kinase receptors, that undergo autophosphorylation upon agonist binding (Soppet et al, 1991). In order to assess the role of BDNF pathway in ethanol intake, we used the recently available TrkB selective antagonist ANA-12 (Cazorla et al, 2011). After 30 days of stable ethanol/water intake, mice received daily i.p. injections of either vehicle or ANA-12 (Figure 4a and b). ANA-12 reversed the stable ethanol intake of WT mice (F(7,42)=30.53, p<0.001) but did not change the voluntary and the forced ethanol intake of D3R−/− (data not shown). Neither in WT nor in D3R−/− total fluid intake was affected by treatment with ANA-12 (Figure 4c and data not shown). Also in the DID paradigm ANA-12 was effective in reducing ethanol intake in WT mice (F(3,55)=6.64, P<0.05, Figure 4d), whereas it did not change ethanol intake in D3R−/− (Figure 4e).
The selective TrKB antagonist, ANA-12 reverses ethanol intake of WT mice and induces D3 receptor downregulation but does not change ethanol intake of D3−/− mice. (a, b and c) Voluntary ethanol intake was measured every 24 h, for 34 days, in WT (n=30) and D3−/− (n=20) mice that had free access to water and ethanol solution (10%). At day 31, mice received daily i.p. injection of either vehicle (VEH), or ANA-12 at 0.5 mg/kg. (d, e) Drinking in the dark (DID) was measured, for 4 days, in WT (n=9) and D3−/− (n=9) mice that had limited access (2 h/day for 3 days and 4 h the 4th day) to ethanol solution (20%), daily injected with vehicle or ANA-12 1 h before the test. *p<0.05, **p<0.01, ***p<0.001 vs VEH, one-way ANOVA and Newman–Keuls post hoc test. (f) The abundance of transcripts of D3 receptor in striatum was assessed by quantitative RT-PCR in WT mice exposed to chronic voluntary ethanol intake. Mean fold changes are expressed relative to transcript levels in controls. The abundance of phosphorylated TrkB was assessed by immunoblot, in the striatum WT treated with ANA-12 and exposed to the voluntary ethanol intake. Bars show mean (± SEM). **p<0.01, ***p<0.001 vs vehicle. One-way ANOVA and Newman–Keuls post hoc test.
To assess the selective blockade of the BDNF receptor in striatum by ANA-12, we determined, by immunoblot, the abundance of phosphorylated TrkB. As shown in Figure 4f, treatment of WT with ANA-12 significantly decreased phosphorylation of TrkB (F(3,35)=184.5, p<0.01). Finally and more interestingly, ANA-12 strongly decreased D3R mRNA expression in the striatum of WT mice exposed to voluntary ethanol intake (Figure 4f, F(3,35)=184.5, P<0.001).
Buspirone Inhibited Ethanol Intake
In the two-bottle choice paradigm, after 30 days of stable ethanol/water intake, mice were treated with buspirone (1 mg/kg/day). As shown in Figure 5a and b, treatment of WT with buspirone significantly decreased voluntary ethanol intake (F(1,28)=20.88, p<0.05). Treatment of D3R−/− with buspirone did not change ethanol intake (data not shown). Neither in WT nor in D3R−/− total fluid intake was affected by treatment (Figure 5c and data not shown). The treatment with buspirone also significantly decreased ethanol intake in WT mice when tested in the DID. Dose ranging of buspirone (0.1, 1, 3, and 10 mg/kg) showed that treatment of WT with buspirone at the doses of 3 and 10 mg/kg significantly decreased ethanol intake both in the 1st day (F(4,75)=31.24, p<0.05) and in the 2nd day (F(4,75)=31.24, p<0.01 3 mg/kg; p<0.05 10 mg/kg) of the behavioral paradigm (Figure 5d). Buspirone did not change ethanol intake of WT in the 3rd and 4th days of DID (Figure 5d). Furthermore, in the DID paradigm, 3 mg/kg buspirone did not change ethanol intake in D3R−/− (data not shown). Because buspirone is also known as a 5-HT1A agonist, the D3R specific effect of buspirone in decreasing ethanol intake was confirmed by using the selective 5-HT1A agonist, 8-OH-DPAT. As shown in Figure 5e, treatment with 8-OH-DPAT (1 mg/kg, i.p.) in WT and D3R−/− mice did not affect ethanol intake (Figure 5e and data not shown). As expected, the 5-HT1 A selective agonist 8-OH-DPAT decreased the body temperature of WT mice (F(2,39)=14.99, p<0.001) (Figure 5f). Buspirone (3 mg/kg) decreased the body temperature of WT mice only transiently (Figure 5f).
Buspirone inhibits ethanol intake in WT mice both in the two bottle choice and DID paradigm. (a, b) Voluntary ethanol intake was measured every 24 h, for 44 days, in WT (n=20) and D3−/− (n=20) mice that had free access to water and ethanol solution (10%). Mice received for 14 days, from day 31, daily i.p. injection of either vehicle (VEH) or buspirone at 1 mg/kg. (c) Total fluid intake that was not changed by buspirone. *p<0.05, ***p<0.01 vs VEH. One-way ANOVA and Newman–Keuls post hoc test. (d) The dose ranging of buspirone (0.1, 1, 3, and 10 mg/kg) in WT mice exposed to the drinking in the dark (DID) paradigm. DID was measured, for 4 days, in WT (n=33) that had limited access (2 h/day for 3 days and 4 h the 4th day) to ethanol solution (20%). *p<0.05, **p<0.01 vs VEH. One-way ANOVA and Newman–Keuls post hoc test. (e) The effect of the selective 5-HT1A agonist, 8-OH-DPAT in DID paradigm. 8-OH-DPAT at 1 mg/kg did not change ethanol intake. (f) The action on 5-HT1A of 3 mg/kg buspirone was compared with 1 mg/kg 8-OH-DPAT by assessing the pharmacologically induced hypothermia. ***p<0.001 vs VEH. One-way ANOVA and Newman–Keuls post hoc test.
DA Receptor Signaling in Striatum of WT and D3R−/− Mice Exposed to Ethanol
Activation of D1 receptor results in activation of adenylyl cyclase/cAMP/protein kinase A (PKA) signaling; a major substrate for PKA in the striatum is DARPP-32. D2-like receptors regulate the activity of the protein kinases Akt and GSK3β; stimulation of either D2 or D3 receptors results in phosphorylation of Akt and GSK3β (Mannoury la Cour et al, 2011). In order to assess activation of dopaminergic transmission in striatum, we determined, by immunoblot, the abundance of phosphorylated DARPP-32 (Thr 34) and of phosphorylated GSK3β (Ser 9). As shown in Figure 6, posphoGSK3β was more abundant in striatum of D3R−/− than in WT mice, whereas phosphoDARPP-32 showed the same tendency, though it did not reach statistical significance. Treatment of WT mice with SB277011A induced phosphorylation of DARPP-32 and GSK3β, up to the level seen in D3R−/− mice. In contrast, in cerebellum, there was no difference in the level phosphoDARPP-32 and posphoGSK3β between WT e D3R−/−, nor it was influenced by SB277011A treatment in WT.
DA receptor signaling is enhanced in striatum of D3R−/− mice and of SB277011A-treated WT mice. The abundance of phosphorylated DARPP-32 (Thr 34) (a) and phosphorylated GSK3β (Ser 9) (b) was assessed by immunoblot, in the striatum of WT mice exposed to the long-term voluntary ethanol intake (white columns) and injected i.p. for 14 days with either vehicle or 10 mg/kg SB277011A and in D3−/− (black columns). Brain tissues were taken 1 h after the last administration of either vehicle or SB277011A. Bar graphs show mean (± SEM) of intensities normalized against the respective non-phosphorylated protein. Each column is the mean (± SEM) from five different samples. *p<0.05 vs control (vehicle-injected WT). Two-way ANOVA and Newman–Keuls post hoc test.
DISCUSSION
This study demonstrates that D3R is necessary for ethanol consumption in mice, because either D3R gene deletion or D3R pharmacological blockade by selective D3R experimental antagonists or the approved drug buspirone, inhibits alcohol intake. The D3R overexpression induced by ethanol intake associated with the activation of RACK1/BDNF may represent the basis for a reinforcing mechanism of ethanol intake. Indeed, although selective blockade of the TrkB reversed stable intake of ethanol in WT mice and decreased D3R expression levels in their striatum, it was ineffective in D3−/− mice.
It seems that D3R, among D2-like receptors, is the key player in addiction, particularly in reward mechanisms. Indeed, although the D2R is associated with mesocortical and mesohippocampal DA pathway, the D3R is associated with the ventral mesolimbic DA system (Sokoloff et al, 1990). Previous studies reported low levels of D2R both in animal models and in patients addicted to cocaine, alcohol, metamphetamine, and nicotine (Volkow et al, 2009). Conversely, upregulation of D3R expression has been reported following exposure to DA elevating drugs (Boileau et al, 2012; Heidbreder and Newman, 2010; Le Foll et al, 2005b; Mash, 1997; Segal et al, 1997; Staley and Mash, 1996).
An important interpretative issue is the genetic background on which the D3R null mutation was placed. Specific behavioral phenotypes are differently expressed in different strains of mice (Nelson and Young, 1998). The D3R−/− mice we used are on the C57BL/6J background (Accili et al, 1996), a strain where ethanol preference and sensitivity is well documented (Crabbe et al, 1983). Interestingly, D3R−/− mice have extracellular DA levels twice as high as their WT littermates (Joseph et al, 2002; Koeltzow et al, 1998); this enhanced DA tone and the resulting adaptations may reflect removal of the inhibitory influence of D3R in the control of basal extracellular DA levels (Le Foll et al, 2005a), giving support to an autoreceptor role for D3R in the mesolimbic areas of the brain (Diaz et al, 2000). The increased DA activity in D3R−/− mice is consistent with their phenotype, including higher basal levels of grooming behavior, hyper-locomotion, and reactivity to drug-paired environmental cues (Accili et al, 1996; Le Foll et al, 2005a; Le Foll et al, 2002).
Here we found that D3R−/− mice chronically exposed to the voluntary ethanol intake paradigm, drink very low quantities of ethanol in comparison with their WT littermates. This observation cannot be attributed to differences in metabolism (McQuade et al, 2003), locomotor activity (Harrison and Nobrega, 2009), or taste reactivity (McQuade et al, 2003) between WT and D3R−/− mice. The lower ethanol intake of D3R−/− in comparison with their WT control mice seems apparently in contrast with the only two previous studies testing D3R−/− mice in the ethanol voluntary intake paradigm (Boyce-Rustay and Risinger, 2003; McQuade et al, 2003). This may be due, at least in part, to some important differences in experimental procedures used. Indeed, McQuade et al (2003), that have shown no difference between D3R−/− and WT in the 24-h access paradigm, used a different experimental procedure in the two-bottle choice paradigm. First, they used just 4 days of adaptation period before ethanol exposure. Second, they tested both D3R−/− and WT animals with increasing concentrations of ethanol in subsequent 7-day steps. In the first step, 3% ethanol, in the second step 6%, in the third step 10%, in the 4th 15%, and finally, in the 5th 20% ethanol. Thus, the behavioral paradigm used by McQuade and co-workers is quite different from our paradigm. From our experience, for these mice it is to have a long period of habituation in the two-bottle paradigm (15 days) before to start with the ethanol access procedure. It is likely that the progressive increase of the ethanol concentration every 7 days, may induce an adaptation to the ethanol that damps the difference between D3R−/− and WT mice. Furthermore, in the McQuade’s study, the relative positions of the ethanol and water bottle were determined randomly each day, whereas in our experiments the position of tubes was interchanged (left/right) every 24 h, to prevent acquisition of position bias. The random change of bottles may expose a given animal to access the same solution (either ethanol or water) in the same position for two/three days consecutively, which may interfere with the results of the experiment during a short period of observation (7 days).
In the study by Boyce-Rustay and Risinger (2003), C57 animals were used as control of D3R−/− mice. These experiments are not comparable to our experiments using WT littermates as controls. Moreover, again, in this study increasing concentrations of ethanol were used in 8-day steps (3 and 10%). Thus, (i) the behavioral procedure is different; (ii) an adaptation to ethanol may occur and damp the difference between genotypes.
To obtain pharmacological evidence for a functional role of D3R in the control of voluntary ethanol intake, we tested two D3R antagonists, U99194A and SB277011A at doses reported to selectively target the D3R (Carr et al, 2002; Reavill et al, 2000). Before administering these drugs, we performed a molecular modeling study to gain information on the interaction of U99194A and SB277011A with D3R. As illustrated in Supplementary Information, in silico analysis showed that the two D3R antagonists were (i) highly selective for the D3R subtype and (ii) displayed a distinct interaction (different binding energy, different interaction patterns) with D3R, consistent with their distinct chemical structure. We found that both U99194A and SB277011A induced a significant decrease in voluntary ethanol intake in WT but not in D3R−/−. This pharmacological evidence reinforces the view that the D3R is necessary for ethanol consumption in mice and is consistent with rat data showing that D3R antagonism reduces relapse-like drinking and cue-induced ethanol-seeking behavior (Vengeliene et al, 2006).
We confirmed the primary role of D3R in the control of ethanol-drinking behavior in a binge-like ethanol-drinking paradigm (Crabbe et al, 2011; Rhodes et al, 2005; Rhodes et al, 2007). Here, again, D3R−/− mice exposed to DID drank lower quantities of ethanol in comparison with their WT littermates, and D3R blockade by SB277011A decreased ethanol intake in WT but not in D3R−/−. No differences were recorded in the DID at day 4. Indeed, there was neither a genotype effect between WT and D3R−/− nor a treatment effect with the SB277011A in WT mice. In general, the binge-like behavior is captured by the 2 h time window that detects differences between treatments/genotypes better than the 4 h window, because the cumulative intake over 4 h makes smaller the proportion of differences (Rhodes et al, 2005). Thus, it is likely that, the lack of differences on day 4 is due to the longer lasting access to ethanol that produced overall a higher consumption, potentially masking the genotype/treatment effect on binge-like drinking behavior occurring in the first 2 h.
Enhanced D3R expression in striatum following long-term alcohol consumption has been previously reported in both mice and rats (Jeanblanc et al, 2006; Vengeliene et al, 2006). Our data show and confirm that chronic voluntary ethanol intake upregulated D3R mRNA expression in the striatum of WT mice. Interestingly, D3R expression is increased by exposure to other addictive drugs, such as nicotine and cocaine, in caudate–putamen (Neisewander et al, 2004) and in nucleus accumbens of rats (Le Foll et al, 2003, 2005b) and humans (Staley and Mash, 1996). Expression of D3R therefore appears to be a potential basis for a reinforcing mechanism in reward-related behavior associated with voluntary intake of addictive drugs and ethanol.
A number of studies have linked D3R expression in the nucleus accumbens to BDNF derived from cortical sources (Guillin et al, 2001; Le Foll et al, 2005b); furthermore, ethanol exposure increases both BDNF and D3R within the striatum itself (Jeanblanc et al, 2006; McGough et al, 2004). The scaffolding protein RACK1 is a key regulator of BDNF expression; RACK1 translocates to the nucleus after exposure of neurons to ethanol and increases expression of BDNF (McGough et al, 2004). Jeanblanc et al (2006) proposed that the RACK1/BDNF/D3R pathway is involved in the control of ethanol consumption in mice. Our hypothesis is that activation of RACK1/BDNF by ethanol may induce expression of D3R, which in turn controls and maintains ethanol consumption. This hypothesis is supported by the data we generated showing that: (i) ethanol intake is negligible in D3R−/− and robust in WT; (ii) increase in RACK1/BDNF/D3R is maintained during chronic ethanol intake in WT; (iii) forced ethanol intake increases RACK1/BDNF even in D3R−/−. Furthermore, chronic voluntary ethanol intake increased D3R expression in striatum concomitant with increased expression of BDNF. It is noteworthy that, in the basal condition, D3R−/− mice exhibited higher BDNF than WT, consistent with a tendency reported in a recent study (Xing et al, 2012). When subjected to forced ethanol intake, D3R−/− mice showed a robust increase in BDNF expression in the striatum. Therefore, chronic ethanol intake increases BDNF independently of D3R receptor stimulation. The finding that chronic ethanol intake increased RACK1 in striatum of both WT and D3R−/− provides additional evidence for the role of RACK1/BDNF/D3R pathway in ethanol intake; chronic ethanol intake stimulates RACK1/BDNF pathway leading to D3R overexpression and addictive behavior in WT, but not in D3R−/−, because this latter lacks D3R.
To provide additional evidence, we blocked the BDNF pathway by using the TrkB specific antagonist, ANA-12. We found that ANA-12 reversed ethanol intake both in the two-bottle choice and DID paradigms and strongly decreased the expression of D3R in the striatum of WT-treated mice. Recently, D3R on VTA-SN dopaminergic neurons were found to mediate neuroplasticity effects of several addictive drugs (Collo et al, 2012; Collo et al, 2013). Therefore, our conclusion about the engagement of striatal RACK1, BDNF, and D3R in mediating ethanol consumption may be only a part of a more complex mechanism, whose elucidation may require an assessment of the effects of ethanol intake in the VTA-SN dopaminergic neurons.
Finally, in a translational perspective, we tested buspirone, a drug marketed for anxiety disorders, endowed with D3R antagonist (Bergman et al, 2013; Le Foll and Boileau, 2013; Newman et al, 2012) and 5-HT1A partial agonist activity (Wong et al, 2007). Notably, buspirone shows also high affinity for other D2-like receptors (Bergman et al, 2013; Kula et al, 1994; Tallman et al, 1997). D3R antagonists may be effective for treating substance use disorders and buspirone has proven effective in several preclinical model of drug abuse (Heidbreder and Newman, 2010; Higley et al, 2011; Song et al, 2012), but no studies have, so far, investigated its D3R antagonist action in ethanol consumption. By both radioligand binding and molecular modeling studies (see Supplementary Information), we found that buspirone: (i) shows slight higher affinity at D3R than at D2R (Ki, 29 vs 62 nM, respectively) and may form interactions comparable with those of SB277011A in D3R, having the antagonist binding mode at D3 receptor, (ii) displays a distinct interaction from the other two antagonists SB277011A and U99194A (different binding energy, different interaction patterns) with D3R, consistent with their distinct chemical structure. Thereafter, we found that buspirone induced a significant decrease in ethanol intake in both two-bottle choice and DID paradigms. The dose of 1 mg/kg inhibited ethanol intake in both paradigms, though its effect did not reach statistical significance in DID; 3 and 10 mg/kg, however produced a significant effect in DID. We confirmed the specificity of D3R effect by using a selective 5-HT1A agonist, 8-OH-DPAT, in the DID. Treatment with 8-OH-DPAT did not impact ethanol intake, whereas, as expected, decreased the body temperature in a stable manner. In a translational perspective, an important issue is the actual availability of buspirone to bind D3R in human CNS. Reported buspirone’s affinity toward human recombinant D3R ranges from 3.5 to 98 nM (Bergman et al, 2013; Newman et al, 2012), which partially overlaps its affinity for 5-HT1A receptors; because buspirone binding to 5-HT1A is considered the basis of its anxiolytic activity in humans, it is likely that anxiolytic doses are sufficient to occupy also D3R in human CNS. However, the D3R-related therapeutic potential of buspirone requires more detailed information, including measurements of D3R receptor occupancy in human PET studies, as an essential prerequisite to clinical application.
Finally, as D3R−/− mice have been shown to exhibit extracellular DA levels substantially higher than WT, as assessed by microdialysis (Koeltzow et al, 1998), a phenomenon related to the lack of autoreceptor function (Joseph et al, 2002), we hypothesized that ethanol intake effectively stimulates DA release and transmission in WT, but not in D3R−/−, presumably because this latter already displays high extracellular DA levels. To test the hypothesis that treatment with D3R antagonists mimicked the high DA phenotype documented in D3R−/− (Koeltzow et al, 1998), we assessed phosphorylation of DARPP32, that is increased by different addictive drugs, including ethanol (Nuutinen et al, 2011; Svenningsson et al, 2005), and of GSK3β, that is linked to D2-like receptors signaling cascade (Beaulieu et al, 2007; Li et al, 2009), particularly under hyper-DAergic conditions (Li et al, 2009). Treatment with SB277011A increased phosphorylation of DARPP32 and of GSK3β to a level similar to that of D3R−/−. Thus, chronic blockade of the D3R or its genetic deletion increased DA transmission in striatum, consistent with increased extracellular DA (Joseph et al, 2002; Koeltzow et al, 1998).
In conclusion, either D3R gene deletion or D3R pharmacological blockade inhibit ethanol intake. Thus, pharmacological antagonism selectively targeting D3R may provide a basis for novel weaning treatments to inhibit ethanol consumption. In this context, buspirone, a drug marketed as anxiolytic since more than 25 years and endowed with D3R antagonist activity, exhibits, translational potential for treating alcohol addiction.
FUNDING AND DISCLOSURE
This work was supported in part by a National Grant PON01-00110. Dr Camillieri, Dr Platania and Dr Torrisi were supported by the International PhD Program in Neuropharmacology, University of Catania Medical School, Catania, Italy; they declare no potential conflict of interest. Dr Leggio and Dr Marrazzo were full-time research fellows of Catania University; they declare no potential conflict of interest. Dr Castorina, Dr D’Agata, Dr Bucolo, Dr Drago, and Dr Salomone were full-time employees of Catania University. Dr Drago was member of the board of the Italian Medicinal Agency (AIFA). Dr Castorina, Dr D’Agata, and Dr Drago declare no potential conflict of interest. Dr Bucolo has received unrestricted research funding from Novartis. Dr Salomone has received unrestricted research funding from Novartis, Bayer, Gilead. Dr Le Foll has received grant and salary support from Pfizer and was a consultant for Richter Pharmaceuticals, Lundbeck, Mylan, Ethypharm and Pfizer. Dr Le Foll research is supported by CAMH, the Campbell Family Mental Health Research Institute, CIHR and the National Institute on Drug Abuse at the National Institutes of Health (1R21DA033515-01). José Nobrega was supported in part by an operating grant from the National Science and Engineering Research Council of Canada (NSERC). Christina N. Nona was the recipient of a Vanier Canada Graduate Scholarship. Dr Stark is an employee of Heinrich-Heine-University Duesseldorf. None of the authors have competing financial interests in relation to the work described.
References
Accili D, Fishburn CS, Drago J, Steiner H, Lachowicz JE, Park BH et al (1996). A targeted mutation of the D3 dopamine receptor gene is associated with hyperactivity in mice. Proc Natl Acad Sci USA 93: 1945–1949.
Beaulieu JM, Gainetdinov RR, Caron MG (2007). The Akt-GSK-3 signaling cascade in the actions of dopamine. Trends Pharmacol Sci 28: 166–172.
Bergman J, Roof RA, Furman CA, Conroy JL, Mello NK, Sibley DR et al (2013). Modification of cocaine self-administration by buspirone (buspar(R)): potential involvement of D3 and D4 dopamine receptors. Int J Neuropsychopharmacol 16: 445–458.
Boileau I, Payer D, Houle S, Behzadi A, Rusjan PM, Tong J et al (2012). Higher binding of the dopamine D3 receptor-preferring ligand [11C]-(+)-propyl-hexahydro-naphtho-oxazin in methamphetamine polydrug users: a positron emission tomography study. J Neurosci 32: 1353–1359.
Bouthenet ML, Souil E, Martres MP, Sokoloff P, Giros B, Schwartz JC (1991). Localization of dopamine D3 receptor mRNA in the rat brain using in situ hybridization histochemistry: comparison with dopamine D2 receptor mRNA. Brain Res 564: 203–219.
Bowers MS, Chen BT, Bonci A (2010). AMPA receptor synaptic plasticity induced by psychostimulants: the past, present, and therapeutic future. Neuron 67: 11–24.
Boyce-Rustay JM, Risinger FO (2003). Dopamine D3 receptor knockout mice and the motivational effects of ethanol. Pharmacol Biochem Behav 75: 373–379.
Brand I, Fliegel S, Spanagel R, Noori HR (2013). Global ethanol-induced enhancements of monoaminergic neurotransmission: a meta-analysis study. Alcohol Clin Exp Res 37: 2048–2057.
Carr KD, Yamamoto N, Omura M, Cabeza de Vaca S, Krahne L (2002). Effects of the D(3) dopamine receptor antagonist, U99194A, on brain stimulation and d-amphetamine reward, motor activity, and c-fos expression in ad libitum fed and food-restricted rats. Psychopharmacology (Berl) 163: 76–84.
Cazorla M, Premont J, Mann A, Girard N, Kellendonk C, Rognan D (2011). Identification of a low-molecular weight TrkB antagonist with anxiolytic and antidepressant activity in mice. J Clin Invest 121: 1846–1857.
Cohen C, Perrault G, Sanger DJ (1998). Preferential involvement of D3 versus D2 dopamine receptors in the effects of dopamine receptor ligands on oral ethanol self-administration in rats. Psychopharmacology (Berl) 140: 478–485.
Collo G, Bono F, Cavalleri L, Plebani L, Merlo Pich E, Millan MJ et al (2012). Pre-synaptic dopamine D(3) receptor mediates cocaine-induced structural plasticity in mesencephalic dopaminergic neurons via ERK and Akt pathways. J Neurochem 120: 765–778.
Collo G, Bono F, Cavalleri L, Plebani L, Mitola S, Merlo Pich E et al (2013). Nicotine-induced structural plasticity in mesencephalic dopaminergic neurons is mediated by dopamine D3 receptors and Akt-mTORC1 signaling. Mol Pharmacol 83: 1176–1189.
Crabbe JC, Kosobud A, Young ER, Janowsky JS (1983). Polygenic and single-gene determination of responses to ethanol in BXD/Ty recombinant inbred mouse strains. Neurobehav Toxicol Teratol 5: 181–187.
Crabbe JC, Spence SE, Brown LL, Metten P (2011). Alcohol preference drinking in a mouse line selectively bred for high drinking in the dark. Alcohol 45: 427–440.
Diaz J, Pilon C, Le Foll B, Gros C, Triller A, Schwartz JC et al (2000). Dopamine D3 receptors expressed by all mesencephalic dopamine neurons. J Neurosci 20: 8677–8684.
Gessa GL, Muntoni F, Collu M, Vargiu L, Mereu G (1985). Low doses of ethanol activate dopaminergic neurons in the ventral tegmental area. Brain Res 348: 201–203.
Guillin O, Diaz J, Carroll P, Griffon N, Schwartz JC, Sokoloff P (2001). BDNF controls dopamine D3 receptor expression and triggers behavioural sensitization. Nature 411: 86–89.
Harrison SJ, Nobrega JN (2009). A functional role for the dopamine D3 receptor in the induction and expression of behavioural sensitization to ethanol in mice. Psychopharmacology (Berl) 207: 47–56.
He DY, Neasta J, Ron D (2010). Epigenetic regulation of BDNF expression via the scaffolding protein RACK1. J Biol Chem 285: 19043–19050.
Heidbreder CA, Andreoli M, Marcon C, Hutcheson DM, Gardner EL, Ashby CR Jr. (2007). Evidence for the role of dopamine D3 receptors in oral operant alcohol self-administration and reinstatement of alcohol-seeking behavior in mice. Addict Biol 12: 35–50.
Heidbreder CA, Gardner EL, Xi ZX, Thanos PK, Mugnaini M, Hagan JJ et al (2005). The role of central dopamine D3 receptors in drug addiction: a review of pharmacological evidence. Brain Res Brain Res Rev 49: 77–105.
Heidbreder CA, Newman AH (2010). Current perspectives on selective dopamine D(3) receptor antagonists as pharmacotherapeutics for addictions and related disorders. Ann N Y Acad Sci 1187: 4–34.
Higley AE, Kiefer SW, Li X, Gaal J, Xi ZX, Gardner EL (2011). Dopamine D(3) receptor antagonist SB-277011A inhibits methamphetamine self-administration and methamphetamine-induced reinstatement of drug-seeking in rats. Eur J Pharmacol 659: 187–192.
Ikemoto S, Bonci A (2013). Neurocircuitry of drug reward. Neuropharmacology 76: 329–341.
Imperato A, Di Chiara G (1986). Preferential stimulation of dopamine release in the nucleus accumbens of freely moving rats by ethanol. J Pharmacol Exp Ther 239: 219–228.
Jeanblanc J, He DY, McGough NN, Logrip ML, Phamluong K, Janak PH et al (2006). The dopamine D3 receptor is part of a homeostatic pathway regulating ethanol consumption. J Neurosci 26: 1457–1464.
Joseph JD, Wang YM, Miles PR, Budygin EA, Picetti R, Gainetdinov RR et al (2002). Dopamine autoreceptor regulation of release and uptake in mouse brain slices in the absence of D(3) receptors. Neuroscience 112: 39–49.
Joyce JN, Millan MJ (2005). Dopamine D3 receptor antagonists as therapeutic agents. Drug Discov Today 10: 917–925.
Koeltzow TE, Xu M, Cooper DC, Hu XT, Tonegawa S, Wolf ME et al (1998). Alterations in dopamine release but not dopamine autoreceptor function in dopamine D3 receptor mutant mice. J Neurosci 18: 2231–2238.
Koob GF (1992). Drugs of abuse: anatomy, pharmacology and function of reward pathways. Trends Pharmacol Sci 13: 177–184.
Kula NS, Baldessarini RJ, Kebabian JW, Neumeyer JL (1994). S-(+)-aporphines are not selective for human D3 dopamine receptors. Cell Mol Neurobiol 14: 185–191.
Le Foll B, Boileau I (2013). Repurposing buspirone for drug addiction treatment. Int J Neuropsychopharmacol 16: 251–253.
Le Foll B, Diaz J, Sokoloff P (2003). Increased dopamine D3 receptor expression accompanying behavioral sensitization to nicotine in rats. Synapse 47: 176–183.
Le Foll B, Diaz J, Sokoloff P (2005a). Neuroadaptations to hyperdopaminergia in dopamine D3 receptor-deficient mice. Life Sci 76: 1281–1296.
Le Foll B, Diaz J, Sokoloff P (2005b). A single cocaine exposure increases BDNF and D3 receptor expression: implications for drug-conditioning. Neuroreport 16: 175–178.
Le Foll B, Frances H, Diaz J, Schwartz JC, Sokoloff P (2002). Role of the dopamine D3 receptor in reactivity to cocaine-associated cues in mice. Eur J Neurosci 15: 2016–2026.
Levant B (1997). The D3 dopamine receptor: neurobiology and potential clinical relevance. Pharmacol Rev 49: 231–252.
Li YC, Xi D, Roman J, Huang YQ, Gao WJ (2009). Activation of glycogen synthase kinase-3 beta is required for hyperdopamine and D2 receptor-mediated inhibition of synaptic NMDA receptor function in the rat prefrontal cortex. J Neurosci 29: 15551–15563.
Mannoury la Cour C, Salles MJ, Pasteau V, Millan MJ (2011). Signaling pathways leading to phosphorylation of Akt and GSK-3beta by activation of cloned human and rat cerebral D(2)and D(3) receptors. Mol Pharmacol 79: 91–105.
Martin KF, Phillips I, Hearson M, Prow MR, Heal DJ (1992). Characterization of 8-OH-DPAT-induced hypothermia in mice as a 5-HT1A autoreceptor response and its evaluation as a model to selectively identify antidepressants. Br J Pharmacol 107: 15–21.
Mash DC (1997). D3 receptor binding in human brain during cocaine overdose. Mol Psychiatry 2: 5–6.
McGough NN, He DY, Logrip ML, Jeanblanc J, Phamluong K, Luong K et al (2004). RACK1 and brain-derived neurotrophic factor: a homeostatic pathway that regulates alcohol addiction. J Neurosci 24: 10542–10552.
McQuade JA, Xu M, Woods SC, Seeley RJ, Benoit SC (2003). Ethanol consumption in mice with a targeted disruption of the dopamine-3 receptor gene. Addict Biol 8: 295–303.
Mereu G, Fadda F, Gessa GL (1984). Ethanol stimulates the firing rate of nigral dopaminergic neurons in unanesthetized rats. Brain Res 292: 63–69.
Murray AM, Ryoo HL, Gurevich E, Joyce JN (1994). Localization of dopamine D3 receptors to mesolimbic and D2 receptors to mesostriatal regions of human forebrain. Proc Natl Acad Sci USA 91: 11271–11275.
Neisewander JL, Fuchs RA, Tran-Nguyen LT, Weber SM, Coffey GP, Joyce JN (2004). Increases in dopamine D3 receptor binding in rats receiving a cocaine challenge at various time points after cocaine self-administration: implications for cocaine-seeking behavior. Neuropsychopharmacology 29: 1479–1487.
Nelson RJ, Young KA (1998). Behavior in mice with targeted disruption of single genes. Neurosci Biobehav Rev 22: 453–462.
Newman AH, Blaylock BL, Nader MA, Bergman J, Sibley DR, Skolnick P (2012). Medication discovery for addiction: translating the dopamine D3 receptor hypothesis. Biochem Pharmacol 84: 882–890.
Nuutinen S, Kiianmaa K, Panula P (2011). DARPP-32 and Akt regulation in ethanol-preferring AA and ethanol-avoiding ANA rats. Neurosci Lett 503: 31–36.
Pierce RC, Kumaresan V (2006). The mesolimbic dopamine system: the final common pathway for the reinforcing effect of drugs of abuse? Neurosci Biobehav Rev 30: 215–238.
Reavill C, Taylor SG, Wood MD, Ashmeade T, Austin NE, Avenell KY et al (2000). Pharmacological actions of a novel, high-affinity, and selective human dopamine D(3) receptor antagonist, SB-277011-A. J Pharmacol Exp Ther 294: 1154–1165.
Rhodes JS, Best K, Belknap JK, Finn DA, Crabbe JC (2005). Evaluation of a simple model of ethanol drinking to intoxication in C57BL/6J mice. Physiol Behav 84: 53–63.
Rhodes JS, Ford MM, Yu CH, Brown LL, Finn DA, Garland T Jr. et al (2007). Mouse inbred strain differences in ethanol drinking to intoxication. Genes Brain Behav 6: 1–18.
Rice OV, Patrick J, Schonhar CD, Ning H, Ashby CR Jr. (2012). The effects of the preferential dopamine D(3) receptor antagonist S33138 on ethanol binge drinking in C57BL/6J mice. Synapse 66: 975–978.
Robbins TW, Everitt BJ (1996). Neurobehavioural mechanisms of reward and motivation. Curr Opin Neurobiol 6: 228–236.
Segal DM, Moraes CT, Mash DC (1997). Up-regulation of D3 dopamine receptor mRNA in the nucleus accumbens of human cocaine fatalities. Brain Res Mol Brain Res 45: 335–339.
Silvestre JS, O'Neill MF, Fernandez AG, Palacios JM (1996). Effects of a range of dopamine receptor agonists and antagonists on ethanol intake in the rat. Eur J Pharmacol 318: 257–265.
Sokoloff P, Giros B, Martres MP, Bouthenet ML, Schwartz JC (1990). Molecular cloning and characterization of a novel dopamine receptor (D3) as a target for neuroleptics. Nature 347: 146–151.
Song R, Yang RF, Wu N, Su RB, Li J, Peng XQ et al (2012). YQA14: a novel dopamine D3 receptor antagonist that inhibits cocaine self-administration in rats and mice, but not in D3 receptor-knockout mice. Addict Biol 17: 259–273.
Soppet D, Escandon E, Maragos J, Middlemas DS, Reid SW, Blair J et al (1991). The neurotrophic factors brain-derived neurotrophic factor and neurotrophin-3 are ligands for the trkB tyrosine kinase receptor. Cell 65: 895–903.
Staley JK, Mash DC (1996). Adaptive increase in D3 dopamine receptors in the brain reward circuits of human cocaine fatalities. J Neurosci 16: 6100–6106.
Svenningsson P, Nairn AC, Greengard P (2005). DARPP-32 mediates the actions of multiple drugs of abuse. Aaps J 7: E353–E360.
Tallman JF, Primus RJ, Brodbeck R, Cornfield L, Meade R, Woodruff K et al (1997). I. NGD 94-1: identification of a novel, high-affinity antagonist at the human dopamine D4 receptor. J Pharmacol Exp Ther 282: 1011–1019.
Thanos PK, Katana JM, Ashby CR Jr., Michaelides M, Gardner EL, Heidbreder CA et al (2005). The selective dopamine D3 receptor antagonist SB-277011-A attenuates ethanol consumption in ethanol preferring (P) and non-preferring (NP) rats. Pharmacol Biochem Behav 81: 190–197.
Vassoler FM, White SL, Schmidt HD, Sadri-Vakili G, Pierce RC (2013). Epigenetic inheritance of a cocaine-resistance phenotype. Nat Neurosci 16: 42–47.
Vengeliene V, Leonardi-Essmann F, Perreau-Lenz S, Gebicke-Haerter P, Drescher K, Gross G et al (2006). The dopamine D3 receptor plays an essential role in alcohol-seeking and relapse. Faseb J 20: 2223–2233.
Volkow ND, Fowler JS, Wang GJ, Baler R, Telang F (2009). Imaging dopamine's role in drug abuse and addiction. Neuropharmacology 56 (Suppl 1): 3–8.
Weiss F, Hurd YL, Ungerstedt U, Markou A, Plotsky PM, Koob GF (1992). Neurochemical correlates of cocaine and ethanol self-administration. Ann N Y Acad Sci 654: 220–241.
Wise RA (1973). Voluntary ethanol intake in rats following exposure to ethanol on various schedules. Psychopharmacologia 29: 203–210.
Wise RA, Bozarth MA (1987). A psychomotor stimulant theory of addiction. Psychol Rev 94: 469–492.
Wong H, Dockens RC, Pajor L, Yeola S, Grace JE Jr., Stark AD et al (2007). 6-Hydroxybuspirone is a major active metabolite of buspirone: assessment of pharmacokinetics and 5-hydroxytryptamine1A receptor occupancy in rats. Drug Metab Dispos 35: 1387–1392.
Xing B, Guo J, Meng X, Wei SG, Li SB (2012). The dopamine D1 but not D3 receptor plays a fundamental role in spatial working memory and BDNF expression in prefrontal cortex of mice. Behav Brain Res 235: 36–41.
Yoshimoto K, McBride WJ, Lumeng L, Li TK (1992). Alcohol stimulates the release of dopamine and serotonin in the nucleus accumbens. Alcohol 9: 17–22.
Acknowledgements
We are indebted to Dr G. Tanda for reading the manuscript and giving his invaluable advice.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on the Neuropsychopharmacology website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Leggio, G., Camillieri, G., Platania, C. et al. Dopamine D3 Receptor Is Necessary for Ethanol Consumption: An Approach with Buspirone. Neuropsychopharmacol 39, 2017–2028 (2014). https://doi.org/10.1038/npp.2014.51
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2014.51
This article is cited by
-
GPCR and Alcohol-Related Behaviors in Genetically Modified Mice
Neurotherapeutics (2020)
-
Receptor Tyrosine Kinases as Therapeutic Targets for Alcohol Use Disorder
Neurotherapeutics (2020)
-
5-HT1A receptor-dependent modulation of emotional and neurogenic deficits elicited by prolonged consumption of alcohol
Scientific Reports (2018)
-
Brain Renin–Angiotensin System Blockade Attenuates Methamphetamine-Induced Hyperlocomotion and Neurotoxicity
Neurotherapeutics (2018)