Abstract
Pneumococcal carriage is common in children that may account for the high incidence of disease in this age group. Recent studies in animals suggest an important role for CD4+ T cells, T helper type 17 (Th17) cells in particular, in pneumococcal clearance. Whether this Th17-mediated mechanism operates in humans and what pneumococcal components activate Th17 are unknown. We investigated the ability of domain 4 pneumolysin (D4Ply) to activate CD4+ T cells including Th17 in human nasopharynx-associated lymphoid tissue (NALT) and peripheral blood. We show that D4Ply elicited a prominent CD4+ T-cell proliferative response. More importantly, D4Ply elicited a significant memory Th17 response in NALT, and a moderate response in peripheral blood mononuclear cells (PBMCs). This D4Ply-elicited memory Th17 response was more marked in carriage− than in carriage+ children in both NALT and PBMCs. In contrast, no difference was shown in D4Ply-induced Th1 response between the two groups. We also show D4Ply activated human monocytes and murine macrophages that was in part dependent on Toll-like receptor 4 (TLR-4). Our results support a protective role of Th17 against pneumococcal carriage in human nasopharynx, and identify a novel property of D4Ply to activate Th17 in NALT that may offer an attractive vaccine candidate in intranasal immunization against pneumococcal infection.
Similar content being viewed by others
INTRODUCTION
Streptococcus pneumonia (pneumococcus) is a leading cause of community-acquired bacterial meningitis and septicemia worldwide.1, 2 Pneumococcus also causes large numbers of cases of pneumonia and otitis media, especially in children. Pneumococcal carriage is particularly common in young children that may account for the high incidence of pneumococcal disease observed in this age group. Young children are also considered a major source of spread of pneumococcal disease. Reduction of nasopharyngeal carriage through vaccination may therefore be an effective strategy against pneumococcal diseases in humans.
Pneumococcus is serotyped based on surface capsular polysaccharides (PSs) that are the main components of current vaccines. However, PS-based vaccines against pneumococcal infection either lack efficacy in young children (PS vaccines) or are limited in serotype coverage (conjugate vaccines). Pneumococcal serotype replacement by nonvaccine serotypes following conjugate vaccination is also a cause for concern.3, 4 Recent efforts have been made to identify pneumococcal protein antigens, as they are likely to induce protection against most serotypes and are cheaper to produce. Data in mice show that immunization with protein antigens can protect against pneumococcal infection.5
Although PS-specific antibodies are known to be protective against pneumococcal colonization, recent data suggest that the age-dependent decrease in pneumococcal carriage rate in humans due to natural immunity is unlikely because of anti-PS antibodies. Natural immunity develops with age to multiple serotypes of pneumococcus simultaneously and before natural acquisition of anticapsular antibodies, which suggests other mechanisms provide natural immunity to pneumococcus.6 Also, recent data in animal studies suggest an important role of CD4+ T cells,7, 8, 9 and T helper type 17 (Th17) cells in particular, in mediating the clearance of nasopharyngeal colonization of pneumococcus.10, 11 However, whether this Th17-mediated mechanism operates in humans and what components of pneumococcus activate Th17 are unknown.
Th17 cells that express cytokines interleukin (IL)-17A, IL-17F, and IL-22 have been shown in mouse models to protect against different respiratory pathogens.12 A crucial role for IL-17A signaling in microbial clearance has been observed in mouse models of infection for a number of mucosal pathogens, suggesting the Th17 pathway may represent a major mechanism in clearance of pathogens at mucosal surfaces.12, 13 Patients with signal transducer and activator of transcription 3 mutations associated with autosomal dominant hyperimmunoglobulin E syndrome were found to have diminished Th17 cells and susceptible to mucosal infections such as Staphylococcus aureus and S. pneumonia.14 This suggest that Th17 cells may also play a role in human natural immunity to mucosal pathogens, although it remains unclear to what extent the hyperimmunoglobulin E syndrome phenotype is due to Th17 deficiency or to diminished signal transducer and activator of transcription 3 signaling in other cells.
As pneumococcus normally colonizes the nasopharynx, the local mucosal immune system is likely to play an important role in mediating immunity against pneumococcal colonization and carriage. The adenoids and tonsils are major components of nasopahrynx-associated lymphoid tissue (NALT) that are part of the mucosal immune system, and are known to be important induction sites for immunity against respiratory pathogens.15, 16 Recent studies suggest that adenoidectomy increases the risk of pneumococcal carriage in children and that appeared to be associated with impaired protein-specific but not with polysaccharide-specific immunity.17, 18 We previously demonstrated the presence of large numbers of naturally developed antigen-specific T and B cells to pneumococcal proteins in NALT in children.19, 20 Pneumolysin (Ply) is a protein toxin expressed by virtually all pneumococcal strains and is considered an important virulence factor in invasive pneumococcal disease.21, 22 Ply and its toxoids have been explored as vaccine candidates and have been shown to induce protective immunity against invasive infection and colonization in animal models.23, 24 We have shown previously that Ply and its toxoid F433 induce CD4+ T-cell responses in adenoidal tissue from children. Furthermore, naturally developed immunity against Ply appears protective against pneumococcal carriage.25, 26 However, as wild-type Ply is toxic and F433 has residual toxicity, both are unsuitable for use as vaccines. Structurally, Ply has four domains. Domain 4 pneumolysin (D4Ply) is involved in binding to the host cell membrane through cholesterol and is essential for Ply-induced toxicity to mammalian cells. It has been shown that the whole three-dimensional structure of Ply is required for its toxicity, whereas individual domains such as D4Ply and domain 123 do not induce cellular toxicity.27
In this study, we investigated the capacity of D4Ply to activate CD4 T cells, and in particular Th17 cells, in human NALT and peripheral blood. We found that D4Ply stimulation elicits a significant proliferative response of CD4 T cells in both NALT and peripheral blood mononuclear cells (PBMCs). More importantly, we showed D4Ply activates a prominent memory Th17 response in NALT and this memory Th17 response appeared to be more marked in carriage− than in carriage+ subjects in both NALT and PBMCs. These findings provide support for a protective role of Th17 cells against pneumococcal carriage, and suggest a novel property of D4Ply that may offer an attractive vaccine candidate in mucosal immunization against pneumococcal infection in humans.
RESULTS
Patients’ demographic data
A total of 38 patients (age 2–12 years) were recruited into the study, and pneumococcal carriage rates were assessed by pneumococcal culture of nasopharyngeal swabs. Table 1 shows the demographic data of the study subjects. As shown in Table 1, younger children (2–3 years old: 45%) tended to have higher carriage rates than older children (4–6 years old: 29%, and 7–12 years old: 20%). No difference was found in carriage rates between males (35%) and females (28%) (P>0.05). Out of 38, 28 (73.7%) received pneumococcal conjugate vaccination, and there was no difference in pneumococcal immunization rate between carriage-positive (75.0%) and carriage-negative subjects (73.1%).
D4Ply but not D123Ply induces CD4+ T-cell activation and proliferation
To study whether D4Ply activates human CD4+ T cells, both tonsillar mononuclear cells (MNCs) and PBMCs were stimulated by D4Ply or D123Ply and analyzed for CD69 expression and proliferation of CD3+CD4+ T cells. As shown in Figure 1a, stimulation with D4Ply, but not with D123Ply, induced significant upregulation of CD69 expression on CD4+ T cells in both tonsillar MNCs and PBMCs (P<0.01). D4Ply also induced a dose-dependent CD4+ T-cell proliferative response in both tonsillar MNCs and PBMCs, whereas no proliferative response was observed after stimulation by either D123Ply (1 or 2 μg ml−1) or lipopolysaccharide (LPS; Figure 1b). Further analysis showed that D4Ply induced both memory and naive CD4+ T-cell proliferation in naive T cell (CD45RA+)-depleted and memory T cell (CD45RO+)-depleted tonsillar MNCs, respectively (Supplementary Figure S1a online).
Domain 4 pneumolysin (D4Ply) but not domain 123 pneumolysin (D123Ply) induces CD4+ T-cell activation and proliferation. (a, b) CD69 expression and proliferative response of CD4+ T cells was analyzed by flow cytometry following D4Ply stimulation in peripheral blood mononuclear cells (PBMCs) and tonsillar mononuclear cells (MNCs). (a) Upregulation of CD69 expression by D4Ply (dark gray) but not by D123Ply (black bold) compared with unstimulated control (gray-shaded) (one of six representative experiments is shown), and (b) dose-dependent CD4+ T-cell proliferation (measured with carboxyfluorescein diacetate 5,6 succinimidyl ester CFSE staining technique) in tonsillar MNCs and PBMCs induced by D4Ply but not by D123Ply and lipopolysaccharide (LPS; n=6, only CD3+CD4+ T cells were gated and shown). (c) CD4+ T-cell proliferation induced by D4Ply was not inhibited by polymyxin B (#P>0.05, n=6). (d) D4Ply-induced CD4 T-cell proliferation was inhibited by anti-human major histocompatibility complex II (MHC II) antibodies and partially inhibited by anti-human Toll-like receptor 4 (TLR-4) antibody (*P<0.01 and #P<0.05, respectively, compared with D4Ply stimulated, n=6). Ab, antibody. (e) Production of cytokines (interleukin (IL)-4, IL-17A, interferon-γ (IFN-γ), and IL-22) in tonsillar MNCs induced by D4Ply (*P<0.001 compared with medium control, n=6).
To rule out any possible effect of LPS contamination in the recombinant D4Ply on the CD4+ T-cell response, polymixin B-treated D4Ply was used as a control to stimulate tonsillar MNCs. No difference was seen between the CD4+ T-cell proliferation induced by polymixin B-treated D4Ply and that by untreated D4Ply (Figure 1c).
Coincubation of anti-major histocompatibility complex II (MHC II) monoclonal antibodies with tonsillar MNCs diminished D4Ply-induced CD4+ T-cell proliferation, whereas coincubation with anti-Toll-like receptor 4 (TLR-4) antibody partially inhibited the CD4+ T-cell proliferative response (Figure 1d). Significant production of IL-17A, IL-22, and interferon-γ (IFN-γ), but not IL-4, was observed following D4Ply stimulation in both tonsillar MNCs (Figure 1e) and PBMCs (Supplementary Figure S1b).
Activation of memory Th17 cells by D4Ply
The induction of IL-17A and IFN-γ, but not IL-4, suggests that D4Ply elicited a Th17 and Th1 but not Th2 cytokine profile. To verify that D4Ply activates memory Th17 cells, intracellular cytokine staining was performed in tonsillar MNCs and PBMCs after short-term (overnight) stimulation with D4Ply. For detection of Th17 cells, the following gating strategy was used as shown in Figure 2a. Lymphocytes were gated (R1) based on typical forward and sideward scatter plot. CD4+ T cells (R2) were then gated based on CD3+ and CD4+ staining and percentage of IL-17A+ CD4+ T cells was finally calculated (R3). As shown in Figure 2b, overnight stimulation with D4Ply elicited a prominent increase in the number of IL-17A-producing CD4+T cells (Th17) in tonsillar MNCs, and a modest increase in Th17 cells in PBMCs, compared with unstimulated controls (P<0.01). D4Ply also induced an increase in IFN-γ-producing CD4+ T cells (Th1) in both tonsillar MNCs and PBMCs (Figure 2c). In contrast, stimulation with D123Ply did not induce any increase in IL-17A and IFN-γ-producing cells compared with controls (Figure 2c). As a comparison, wild-type Ply was also tested for its ability to activate Th17 cells. At low concentrations (<20 ng ml−1). it induced a modest increase in Th17 cells in both MNCs and PBMCs, whereas at higher concentrations it caused a dose-dependent cell death (data not shown).
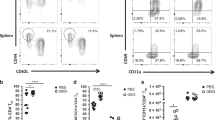
Activation of memory T helper type 17 (Th17) cells by domain 4 pneumolysin (D4Ply). Intracellular cytokine staining (ICS) was performed in tonsillar mononuclear cells (MNCs) and peripheral blood mononuclear cells (PBMCs) after overnight stimulation with D4Ply. Number of Th17 cells was expressed as % of interleukin (IL)-17A-producing cells in CD3+CD4+ T cells. (a) Gating strategy: lymphocytes were gated (R1) based on typical forward and sideward scatter (FSC and SSC) plots; CD4+ T cells (R2) were then gated based on CD3+ and CD4+ staining and percentage of IL-17A+ CD4+ T cells was calculated in R3. (b) Representative fluorescence-activated cell sorting (FACS) dot plots show numbers of IL-17A-producing CD4+T cells in tonsillar MNCs and PBMCs following D4Ply stimulation compared with unstimulated control. (c) Summarized results (n=10) on Th17 and interferon-γ (IFN-γ)-producing CD4+T cells in tonsillar MNCs and PBMCs following D4Ply or D123Ply stimulation (*P<0.001 compared with unstimulated control). (d) ICS dot plots demonstrate proportions of CD4+IL-17A+ cells coexpressing IL-17F and IL-22 following D4Ply stimulation, whereas most of theIL17A-producing CD4+T cells activated by D4Ply did not coexpress IFN-γ. (e) D4Ply-activated Th17 cells were present in unfractionated MNCs and in CD45RO+ (*P<0.01, D4Ply vs. unstimulated control) but not in CD45RO− fractionated MNCs (#P>0.05, D4Ply vs. unstimulated control). (f) D4Ply induced CD4+ T-cell proliferation in both IL-17A+ and IL-17A− cells (right) compared with unstimulated control (left) (one of four representative experiments is shown). CFSE, carboxyfluorescein diacetate 5,6 succinimidyl ester.
Costaining of intracellular cytokines demonstrated that a substantial proportion of the IL-17A-producing cells elicited by D4Ply coexpressed IL-17F, although only a small fraction coexpressed IL-22, whereas most of these Th17 cells did not express IFN-γ (Figure 2d). Similar to IL-22, IL-26 staining showed a small fraction of IL-17A-producing cells coexpressed IL-26 (data not shown). Co-staining of IL-17A, CD3, CD4, and CD45RO in both tonsillar MNCs and PBMCs showed that IL-17A-producing cells elicited by overnight stimulation with D4Ply were of CD3+CD4+CD45RO+ phenotype (data not shown). Depletion of CD45RO+ cells from tonsillar MNCs before stimulation abolished the D4Ply-activated Th17 cells observed in undepleted MNCs and in CD45RO+ cells (Figure 2e). This suggests that stimulation by D4Ply activated memory/effector Th17 cells in tonsillar MNCs.
It is worth noting that this short-term (overnight) stimulation by D4Ply induced a different profile of IL-17A production from that induced by phorbol 12-myristate 13-acetate (PMA)/inomycin. The IL-17A-producing cells elicited by D4Ply were almost exclusively from CD3+CD4+ T-cell population, whereas that induced by PMA/inomycin were from both CD4+ and non-CD4+ T cells, although predominantly from the former. In addition, PMA/inomycin stimulated cells produced a higher proportion of IL-17F+, IL-22+, and IFNγ+ cells coproducing IL-17A than D4Ply (Supplementary Figure S2a).
To determine whether D4Ply induces memory Th17 proliferation, tonsillar MNCs were stained with carboxyfluorescein diacetate 5,6 succinimidyl ester (CFSE) followed by co-culture with D4Ply for 5 days. Figure 2f shows that stimulation with D4Ply induced a proliferative response in both IL-17A+ and IL-17A- CD4+ T-cell population. However, in CD45RO+ cell-depleted tonsillar MNCs, no proliferation of IL-17-producing cells was seen after stimulation with D4Ply (data not shown). This further supports that D4Ply activated memory Th17 cells.
We next examined whether MHCs and TLR-4 were involved in D4Ply-induced activation of Th17 cells. Coincubation of either anti-MHC II or anti-TLR4 monoclonal antibodies with tonsillar MNCs significantly inhibited the number of Th17 (Figure 3a) and cytokine concentrations of IL-17A (Figure 3b) and of IL-17F (data not shown) in MNC culture supernatants elicited by D4Ply. IL-22 secretion elicited by D4Ply was also inhibited by anti-MHC II antibody (Supplementary Figure S2b). On the other hand, prior incubation of LPS with tonsillar MNCs before stimulation by D4Ply enhanced the numbers of Th17 elicited by D4Ply stimulation (Figure 3a).
Major histocompatibility complex II (MHC II), Toll-like receptor 4 (TLR-4), and interleukin (IL)-1β are involved in domain 4 pneumolysin (D4Ply)-induced activation of T helper type 17 (Th17) cells. (a, b) Coincubation of anti-MHC II or anti-TLR-4 monoclonal antibodies with tonsillar mononuclear cells (MNCs) inhibited the number of (a) Th17 and (b) cytokine concentrations of IL-17A in MNC culture supernatants elicited by D4Ply. Ab, antibody. Prior incubation of lipopolysaccharide (LPS) enhanced Th17 and IL-17A elicited by D4Ply, *P<0.05, **P<0.01, and #P<0.05 compared with D4Ply-stimulated cells, n=6. (c) Coincubation with neutralizing antibody to IL-1β or IL-1 receptor antagonist (IL-1RA) before D4Ply stimulation inhibited the number of Th17 cells elicited by overnight stimulation with D4Ply (*P<0.05, n=6).
Previous studies demonstrated that IL-1β was important in the activation of human Th17 cells.28, 29 To determine whether IL-1β was involved in the activation of memory Th17 cells by D4Ply, tonsillar cells were coincubated with neutralizing antibody to IL-1β or IL-1 receptor antagonist before stimulation with D4Ply. As shown in Figure 3c, both anti-IL-1β antibody and IL-1 receptor antagonist inhibited the number of Th17 cells elicited by overnight stimulation with D4Ply (P<0.01). Similarly, D4Ply-induced IL-17A and IL-22 secretion in tonsillar cell culture supernatants was also inhibited by IL-1 receptor antagonist (Supplementary Figure S2c).
Association of D4Ply-elicited memory Th17 response and pneumococcal carriage
To determine whether there is any relationship between D4Ply-elicited memory Th17 response and pneumococcal carriage, numbers of memory Th17 in both tonsillar MNCs and PBMCs were measured following overnight stimulation by D4Ply and analyzed in association with the presence or absence of pneumococcus in nasopharyngeal swabs from 38 children. In unstimulated tonsillar MNCs, numbers of Th17 were shown to be slightly higher in culture-positive (+) children than in those who were culture negative (−) (Figure 4a, ≠P<0.05). D4Ply stimulation elicited a memory Th17 response in tonsillar MNCs in both culture− and culture+ children (Figure 4a, **P<0.01 and *P<0.05 compared with unstimulated controls, respectively). However, the Th17 response appeared to be more marked in pneumococcal culture− subjects than in those who were culture+, with a mean % increase of 0.66 vs. of 0.33% respectively from unstimulated controls (Figure 4a, #P<0.05). In PBMCs, whereas the numbers of Th17 were minimal in unstimulated cells from both culture− and culture+ children, overnight stimulation with D4Ply elicited a significant increase in Th17 in culture− subjects, but no such increase in culture+ subjects (Figure 4b). In contrast, there was no difference in the number of IFN-γ-producing CD4+ T cells induced by D4Ply between culture+ and culture− children, neither in tonsillar MNCs nor in PBMCs (Figure 4c). As shown in Table 1, there was no significant difference in ages between culture− and culture+ children (P>0.05). Using a two-way analysis of variance, we found the difference in Th17 response between the two groups was independent of age in this study population.
Association of D4Ply-elicited memory T helper type 17 (Th17) response and pneumococcal carriage. Numbers of Th17 cells in (a) tonsillar mononuclear cells (MNCs) and (b) peripheral blood mononuclear cells (PBMCs) were examined following overnight stimulation by domain 4 pneumolysin (D4Ply) and analyzed in association with carriage status of pneumococcus (n=38). (a) In unstimulated MNCs, % Th17 was relatively higher in culture+ than culture− patients (≠P<0.05). D4Ply elicited an increase in Th17 cells in both culture− and culture+ patients compared with unstimulated controls (**P<0.01 and *P<0.05, respectively). The % increase of Th17 in tonsillar MNCs was higher in culture− (0.66%) than in culture+ patients (0.33%) (#P<0.05). (b) D4Ply stimulation elicited an increase in Th17 (in PBMCs from culture− patients (*P<0.05), but not in culture+ patients (ΦP>0.05). (c, d) D4Ply induced CD4+IFN-γ-producing cells (Th1) in both tonsillar MNCs (*P<0.05) and PBMCs (**P<0.01), but no difference in the % increase between culture− and culture+ patients (P>0.05).
Activation of CD4+ T cells and Th17 by D4Ply is associated with cholesterol binding
It is known that pneumolysin induces cellular toxicity through binding to the cholesterol component on cell surface, and D4Ply is involved in this cholesterol-mediated binding.27 Therefore, we asked whether cholesterol binding is important in the activation of CD4+ T-cell proliferation and Th17 cells. We used a recombinant noncholesterol-binding mutant of D4Ply (D4PlyLT) that is unable to recognize cholesterol in the cell membrane. The D4PlyLT mutant was coincubated with tonsillar MNCs and PBMCs, and the responses were compared with that activated by D4Ply. As shown in Figure 5a–c, there was no activation of CD4+ T-cell proliferation by D4PlyLT (Figure 5a), nor was there any significant Th17 and IFN-γ response in tonsillar MNCs (Figure 5b) and PBMCs (Figure 5c), respectively, after D4PlyLT stimulation.
Activation of T helper type 17 (Th17) and Th1 by domain 4 pneumolysin (D4Ply) is associated with cholesterol binding. (a) CD4+ T-cell proliferation was analyzed by carboxyfluorescein diacetate 5,6 succinimidyl ester (CFSE) staining, and (b) Th17 and (c) interferon-γ (IFN-γ)-producing CD4+ T cells were analyzed by intracellular cytokine staining in tonsillar mononuclear cells (MNCs) and peripheral blood mononuclear cells (PBMCs) following stimulation by D4Ply and a noncholesterol-binding mutant of D4Ply (D4PlyLT) (*P<0.01, #P>0.05 compared with unstimulated medium control, n=6).
D4Ply promotes Th17 differentiation from naive T cells
Having shown that D4Ply activates memory Th17 cells, we next examined whether D4Ply could also promote Th17 differentiation from naive T cells. Tonsillar MNCs depleted of CD45RO+ memory and effector T cells were co-cultured with D4Ply for 7 days in the presence of transforming growth factor-β and IL-21. The induction of Th17 from naive T cells was then examined by intracellular staining of IL-17A following the addition of PMA/ionomycin and Brefeldin A for 4 h before flow cytometry. As shown in Figure 6, D4Ply stimulation induced a significant increase in the numbers of IL-17A-producing CD4+ T cells (Th17) from naive T cells in tonsillar MNCs compared with medium control with transforming growth factor-β and IL-21 (Figure 6a). In contrast, there was no increase in Th17 cells following stimulation by D123Ply under the same culture condition (Figure 6a). Measurement of IL-17A production in the cell culture supernatant by enzyme-linked immunosorbent assay (ELISA) also confirmed the induction of IL-17A by D4Ply but not D123Ply (Figure 6c).
Induction of T helper type 17 (Th17) cells by domain 4 pneumolysin (D4Ply). Tonsillar mononuclear cells (MNCs) depleted of CD45RO+ memory and effector T cells were co-cultured with D4Ply for 7 days in the presence of transforming growth factor-β (TGF-β; 5 ng ml−1) and interleukin-21 (IL-21; 25 ng ml−1). The induction of Th17 from naive T cells was then examined by intracellular cytokine staining of IL-17A following the addition of phorbol 12-myristate 13-acetate (PMA)/ionomycin. (a, b) D4Ply but not D123Ply induced Th17 differentiation from naive T cells. (a) Dot plots of one of six representative experiments, and % of Th17 in CD4+ T cells are shown; (b) summarized data on induction of Th17 by D4Ply, *P<0.001 compared with either D123Ply or medium control with TGF-β and IL-21 (n=6). (c) Measurement of IL-17A secretion in cell culture supernatant after D4Ply stimulation (*P<0.01 compared with medium control and D123Ply, n=6).
D4Ply activates human monocytes
Previous studies showed that monocytes promote Th1 and Th17 responses to pneumococcus,30 and that monocytes/macrophages are key effectors in clearing primary bacterial colonization at mucosal surface.11 To determine whether D4Ply activates human monocytes, peripheral blood monocytes (CD14+) were stimulated with D4Ply and analyzed for expression of costimulatory molecules and cytokines. Stimulation with D4Ply (1 μg ml−1), but not D123Ply (data not shown), induced a significant increase in the expression of CD40, CD54, and CD80 in monocytes (Figure 7a) with production of cytokines including tumor necrosis factor-α (TNF-α), IL-1β, IL-6, and IL-10 (Figure 7c, P<0.01).
Domain 4 pneumolysin (D4Ply) activates human monocytes. Monocytes purified from peripheral blood mononuclear cells (PBMCs) were co-cultured with or without D4Ply for 48 h. (a, b) Upregulation of expression of costimulatory molecules CD40, CD80, and intercellular adhesion molecule-1 (ICAM-1; CD54) by monocytes stimulated by D4Ply. (a) Fluorescence-activated cell sorting (FACS) histogram showing one representative experiment, D4Ply (bold line) compared with unstimulated control (gray-shaded area); (b) summary of six experiments (*P<0.01). MFI, mean fluorescence intensity. (c) Production of tumor necrosis factor-α (TNF-α), interleukin (IL)-1β, IL-6, and IL-10 in monocytes induced by D4Ply compared with unstimulated control (*P<0.001, n=6). (d) Induction of IL-1β in monocytes by D4Ply (but not D123Ply) was inhibited by caspase-1 inhibitor Z-VAD-FMK (10 μg ml−1; #P<0.01 compared with D4Ply stimulated), and enhanced by coincubation with lipopolysaccharide (LPS; **P<0.01 compared with D4Ply stimulated).
As shown in Figure 7d, D4Ply induced IL-1β production in peripheral blood monocytes and coincubation with caspase-1 inhibitor Z-VAD-FMK (10 μg ml−1) inhibited the IL-1β production induced by D4Ply. Coincubation with LPS seemed to have an additive effect on D4Ply-induced IL-1β production in the monocytes (Figure 7d).
Induction of TNF-α production in murine macrophages by D4Ply is partly dependent on TLR-4
To determine whether the activation of monocytes/macrophages by D4Ply is mediated through TLRs, wild-type murine cells expressing MyD88, TLR-2, or TLR-4 as well as the respective gene-knockout mutant cell lines (MyD88−/−, TLR-2−/−, or TLR-4−/−) were studied for their ability to produce TNF-α. As shown in Figure 8a, there was a reduced level of TNF-α production in MyD88−/− than wild-type microglial cells after stimulation with D4Ply (P<0.01). As a control, Figure 8b shows the induction of TNF-α by LPS and bacterial lipopeptide was diminished in MyD88−/− compared with wild-type microglial cells (P<0.001). Subsequent analysis showed that there was approximately a 50% reduction of TNF-α production in TLR4−/− compared with wild-type macrophages following stimulation by D4Ply (Figure 8c). In contrast, there was no difference in D4Ply-induced TNF-α production between TLR2−/− and wild-type macrophages. Figure 8d shows that induction of TNF-α by LPS and bacterial lipopeptide was diminished in TLR4−/− and TLR2−/− macrophages respectively compared with wild-type macrophages.
Induction of tumor necrosis factor-α (TNF-α) production in murine macrophages by domain 4 pneumolysin (D4Ply) is associated with Toll-like receptor 4 (TLR-4). (a, b) Wild-type (Wt) and isogenic gene knockout (KO) murine microglial cells for MyD88−/− and (c, d) macrophages for TLR2−/− and TLR4−/− were stimulated with D4PLY, lipopolysaccharide (LPS), or bacterial lipopeptide (BLP) for 48 h. (a) D4Ply-induced TNF-α production in MyD88−/− was reduced by ∼70% compared with wild-type microglial cells (*P<0.001), and (c) that in TLR4−/− reduced by ∼50% compared with wild-type macrophages (*P<0.01). As controls, BLP and LPS stimulated TNF-α production in respective KO (b: MyD88−/− and d: TLR2−/− and TLR4−/−, respectively) and wild-type murine cells is shown (#P<0.001 compared with wild type; n=6).
DISCUSSION
Recent data from animal studies suggest an important role of CD4+ T cells, particularly Th17 cells in mediating the clearance of nasopharyngeal colonization of pneumococcus.7, 8, 9 Identification of pneumococcal component(s) that induces Th17 activation in humans may provide novel vaccination strategy against pneumococcal infection.
In this study, we showed that D4Ply induced CD4+ T-cell activation and proliferation in human NALT and PBMCs. Furthermore, we found that a short-term (overnight) stimulation with D4Ply activated a prominent memory Th17 cell response in human NALT. The findings that these IL-17A-producing cells were primarily CD4+CD45RO+ T cells and that depletion of CD45RO+ cells abolished the D4Ply-activated Th17 cells in tonsillar MNCs confirm they were memory/effector Th17 cells. This was consistent with a recent report that the IL-17A detected in PBMCs following stimulation by a pneumococcal whole cell antigen originated from effector/memory T cells.31 Our finding that IL-17A-producing CD4+ T cells in tonsillar MNCs could proliferate upon D4Ply stimulation also supports a memory Th17 response.
We further demonstrated that this memory Th17 response following D4Ply stimulation appeared to be more marked in pneumococcal culture-negative than in culture-positive children in both NALT and PBMCs, whereas there was no such difference in IFN-γ-producing Th1 response between the two groups. These results provide supporting evidence that Th17 cells may be protective against pneumococcal carriage or colonization in human nasopharynx.
Th17 lineage is a recently described subset of CD4+ T cells. In addition to their association with autoimmunity, it is becoming apparent that IL-17 may play protective roles in immunity against infectious diseases, especially at the mucosa.32 There is growing evidence of Th17 cells playing an important role in mediating host mucosal immunity to a number of pathogens including Klebsiella pneumoniae, Mycoplasma pulmonis, Pseudomonas aeruginosa, Pneumocystis sp., and Candida albicans.33, 34 In addition, recent evidences suggest that the Th17 lineage may be critical for vaccine-induced memory immune responses against infectious diseases.35 Memory Th17 cells have been shown to confer heterologous and antibody-independent mucosal immune protection against several serotypes of K. pneumoniae.36 Our results may provide further support to a protective role of mucosal memory Th17 cells against extracellular bacteria.37, 38
A recent study showed that a pneumococcal whole cell antigen and a pneumolysin toxoid could induce IL17 production in cultured human PBMCs, although the frequency of Th17 cell in PBMCs detected by intracellular cytokine staining was low.31 In this study, we observed a modest memory Th17 cell response in PBMCs after D4Ply stimulation. However, a more marked memory Th17 response was found in tonsillar MNCs following D4Ply stimulation (Figure 2b). This is in agreement with the notion that Th17 cells are important in host mucosal immunity against extracellular bacterial infections.37, 38 Higher frequency of Th17 cells at the mucosal site than the systemic compartment reported in previous studies also suggests an important role of Th17 cells in mucosal protection.39 The human nasopharynx is the site of colonization of many microorganisms that may prime for memory Th17 cells. We hypothesize that previous colonization of pneumococcus in early childhood may prime for the generation of memory Th17 in the nasopharynx, and the presence of such memory Th17 cells may provide protection against pneumococcal colonization or carriage in later childhood. The finding in this study that stimulation of NALT cells and PBMC by D4Ply activated memory Th17 and that the Th17 response appeared to be more marked in carriage-negative than in culture-positive children may support this hypothesis. Previous reports that T cells were primed for IL-17A production by pneumococcal whole cell antigen vaccination in mice, and that the protection against colonization correlated well with the IL-17A concentrations in blood samples elicited by whole cell antigen just before challenge10 would also be in agreement with this hypothesis.
Th17 cytokines IL-17A and IL-17F are known to play a critical role in the recruitment and activation of neutrophils possibly through the induction of granulocyte colony-stimulating factor and CXC chemokines from epithelial cells or fibroblasts, and neutrophil-mediated killing is a crucial effector in immunity against a number of pathogens.38, 40 Recent studies in mice also showed the importance of IL-17A in the activation of monocyte/macrophages that resulted in the clearance of primary pneumococcal colonization.11 It has been suggested that monocyte/macrophages and neutrophils recruited to the mucosal surface mediated by chemokines induced by IL-17A are key effectors in clearing primary and secondary bacterial colonization, respectively.11 It is possible that memory Th17 cells in human nasopharynx may elicit a chemokine and granulocyte colony-stimulating factor-mediated recruitment and activation of neutrophils that leads to killing of pneumococcus and reduction of carriage.
Our results showed that in unstimulated tonsillar MNCs, the number of Th17 cells was relatively higher in carriage-positive than in carriage-negative children, which suggests pneumococcal colonization induces Th17 cells in vivo, and that is consistent with a recent report that experimental human volunteer carriage augmented Th17 cell numbers.41 Following D4Ply stimulation of tonsillar MNCs, there was a greater increase in Th17 numbers (from unstimulated baseline) in carriage-negative (0.66%) than in carriage-positive children (0.33%). Although the respective numbers of Th17 following stimulation did not seem to differ significantly between the two groups, the relatively weaker Th17 response (lower increase in Th17) in culture-positive children, coupled with a higher number/activity of local T regulatory cells (Tregs) in these children, may favor a carriage status.42 It is possible that the balance between Th17 and Tregs in the nasopharynx is a crucial determinant factor in pneumococcal carriage. We showed previously that in pneumococcal carriage-positive children there was a higher number and activity of Tregs in the NALT tissue than culture-negative children,42 which we also observed in this study (data not shown).
It is possible that an early increase in inducible Tregs in NALT (because of exposure to pneumococcus) in early childhood may inhibit the development and/or activity of Th17 cells and that favors the carriage or persistence of carriage in the nasopharynx. In this case, an early priming of memory Th17 cells in early life may interrupt the Treg-mediated carriage, as suggested recently that an increased priming for IL17A production in early life may be an important mechanism of pneumococcal clearance from the nasopharynx.43 As inducible Tregs are likely to increase overtime with repeated pneumococcal exposure, priming for Th17 cells in early childhood when Treg activity is low may be an attractive vaccination strategy.
The finding that a noncholesterol-binding mutant of D4Ply (D4Ply-LT) failed to activate CD4+ T cells suggests that the cholesterol-binding property of D4Ply is crucial in CD4+ T-cell activation. However, it remains to be determined as to how D4Ply activates human CD4+ T cells including Th17. The inhibition of D4Ply-induced CD4+ T-cell proliferation and Th17 activation by anti-MHC II antibodies suggests that D4Ply activates MHC/TCR complex that involves antigen processing and presentation by antigen-presenting cells. The partial inhibition of CD4+ T-cell proliferation and IL-17A by anti-TLR4 antibody suggests D4Ply induces CD4+ T-cell activation including Th17 in part through a TLR4-dependent innate immune mechanism. In addition, the finding that prior incubation with TLR-4 ligand LPS enhanced the Th17 response elicited by D4Ply further supports the involvement of TLR-4. Pneumolysin has been shown to activate murine macrophages to secrete inflammatory cytokines through TLR-4.44 We show here that D4Ply-induced TNF-α production was reduced in MyD88−/− and TLR-4−/− (∼50%) but not in TLR-2−/− murine macrophages. This again suggests that the activation of macrophage/monocytes by D4Ply is in part dependent on the TLR-4 pathway.
The partial inhibition of D4Ply activity by TLR4 blocking also suggests the involvement of other mechanisms other than TLR-4. It has been reported recently that pneumolysin can activate the inflammasome pathway that mediate the activation of caspase-1 and promote IL-1β production in dendritic cells.45 We showed in this study that D4Ply induces IL-1β production in human monocytes and blocking IL-1β function by neutralizing antibody or IL-1 receptor antagonist partially inhibited the D4Ply-induced memory Th17 response. The induction of IL-1β by D4Ply appeared to be contrary to a previous study that D4Ply did not induce IL-1β induction in PBMCs.46 This apparent difference could be because of the fact that a different concentration of D4Ply was used (≤0.5 μg ml−1) and it was in PBMCs in the previous study rather than a concentration of D4Ply at ≥1 μg ml−1 and purified monocytes were used in our study. Our results also showed that D4Ply-induced IL-1β production in monocytes was inhibited by caspase-1 inhibitor. These results suggest D4Ply may also be able to activate inflammasome pathway to promote IL-1β production in innate immune cells through which contribute to Th17 activation. These findings also suggest an important property of D4Ply to activate innate immune cells such as antigen-presenting cells. Indeed, D4Ply was shown to activate human monocytes, as evidenced by a significant upregulation of costimulatory molecules and cytokine production.
In this study, we only observed a modest Th17 response in tonsillar cells and PBMCs induced by native Ply at lower concentrations (<20 ng ml−1), which was much lower than D4Ply-induced Th17 response (data not shown). With increasing doses of native Ply, there was no enhancement in Th17 response but it induced a dose-dependent cell death. It is likely that the CD4+ T-cell response (including Th17) induced by the native Ply or derivatives was not only governed by cell proliferation but also influenced by the rates of cell loss because of cell toxicity. For D4Ply, it induced a significant CD4+ T-cell, including Th17, proliferation but no significant cell loss.
Th17-targeted vaccine strategy has been proposed and explored recently33, 35, 47 including that against pneumococcal infection,48, 49 and these will continue to add to our understanding of Th17-mediated immune protection. We showed in this study that D4Ply has the capacity to both activate memory Th17 and promote Th17 differentiation. Considering that Th17 cells may be crucial in the clearance of pneumococcal carriage, this capacity of D4Ply makes it an attractive vaccine candidate against pneumococcal infection.
Taken together, we report here a novel property of D4Ply to induce a potent CD4+ T-cell response and, in particular, a prominent memory Th17 response in human NALT. Our results support the hypothesis that mucosal Th17 cells in NALT are involved in the modulation of pneumococcal colonization/carriage in human nasopharynx. Our results also lend support to the novel strategy of Th17-based vaccine design for prevention of pneumococcal infection.48 The property of D4Ply to activate and promote Th17 cells in NALT may offer an attractive vaccine candidate in mucosal immunization against pneumococcal infection in humans.
METHODS
Patients and samples. Adenoidal and tonsillar tissues and peripheral blood samples were obtained from patients (age 2–12 years old) undergoing adenoidectomy and/or tonsillectomy due to adenoidal hypertrophy and/or upper airway obstruction. Patients with known immunodeficiency or who were prescribed antibiotics in the 3 weeks before surgery and who had a previous history of frequent use of antibiotics were excluded from the study. Nasopharyngeal swabs were taken on the day of operation for bacterial culture to determine pneumococcal carriage as described previously.26 In brief, swabs were placed in tubes containing skim milk–tryptone–glucose–glycerin broth, and stored at −70 °C until bacterial culture was performed by inoculating 50 μl of the broth onto a blood agar plate. After incubation was performed overnight at 37 °C, pneumococcal colonies were identified on the basis of typical morphologic findings, α-hemolysis, and subculture with optochin disk testing. The pneumococcal load was assessed semiquantitatively by grading growth density as described elsewhere26, 50 The Liverpool Paediatric Research Ethics Committee approved the study and written informed consent was obtained in all cases.
Cell separation, culture, and stimulation. MNCs from adenotonsillar tissues and PBMCs were isolated using methods described elsewhere.25, 51 Briefly, adenotonsillar tissue was minced using a sterile scalpel and passed through a nylon mesh (30 μm). MNCs and PBMCs were isolated by Ficoll density gradient centrifugation (GE Healthcare, Little Chalfont, UK). Cells subsequently washed in phosphate-buffered saline and resuspended in RPMI-1640 culture medium supplemented with 2 mmol l−1 glutamine, 10 μg ml−1 gentamycin, and 10% fetal bovine serum (Sigma, Dorset, UK). In some experiments, MNCs or PBMCs were separated into CD45RO+ and CD45RO− populations by either positive or negative selection using magnetic cell sorting (Miltenyi Biotec, Surrey, UK) according to the manufacturer’s instructions. Adenotonsillar MNCs and PBMCs were cultured at 4 × 106 cells per ml in 96-well plate (Corning, Flintshire, UK) in the presence or absence of stimulant, e.g., D4Ply or D123Ply, at 1–2 μg ml−1. In some experiments, neutralizing antibodies were coincubated with MNCs for 30 min before addition of D4Ply. The functional grade neutralizing antibodies included anti-human HLA-DR, -DP, and -DQ (anti-MHCII) (BD Biosciences, Oxford, UK), anti-human TLR-4 and TLR-2, and isotype control antibodies (eBioscience, Oxford, UK), anti-human IL-1β, and isotype control antibodies (R&D Systems, Oxford, UK). Paired analysis of adenoidal and tonsillar MNCs showed similar results in CD4 T-cell proliferation and Th17 response, and hence only results of tonsillar MNCs are presented in this paper.
Intracellular cytokine staining. Intracellular cytokine staining of IFN-γ, IL-17A, IL-17F, IL-22, and IL-26 was performed as described previously42 in tonsillar MNCs and PBMCs after stimulation with D4Ply. For assessment of memory Th17 response, tonsillar MNCs and PBMCs were cultured overnight (short-term stimulation) with D4Ply in the presence of brefeldin A (eBioscience) followed by intracellular staining for IL-17A. For assessment of Th17 induction, CD45RO+ cell-depleted tonsillar MNCs were co-cultured with D4Ply for 7 days in the presence of transforming growth factor-β and IL-21. Cells were harvested and stained with fluorescence-labeled anti-human CD3 and CD4 (BD Biosciences), followed by fixation and permeabilization (eBioscience) and staining with fluorescence-labeled IL-17A, IFNγ, IL-17F, or IL-22 (BD Biosciences). Intracellular expression of individual cytokines was subsequently analyzed by flow cytometry.
Flow cytometric analysis. Multicolor flow cytometry was performed for analysis of cell phenotypes, intracellular cytokine expression, cell proliferation, and expression of costimulatory molecules on a FACScalibur (BD Biosciences) as described previously.42 Cell proliferation was examined through staining adenoidal MNCs or PBMCs with CFSE (Molecular Probes, Paisley, UK) before cell stimulation, followed by culture for 5 days before analysis by flow cytometry.26 Flow cytometric data were analyzed using CellQuest Pro (BD Biosciences) and WinMDI software (The Scripps Institute, La Jolla, CA).
Human monocytes. Human peripheral blood CD14+ monocytes were isolated from PBMCs by magnetic cell sorting following the manufacturer’s instructions (Miltenyi Biotec). Purified monocytes were cultured in RPMI-1640 supplemented with 2 mmol l−1 glutamine, 10 μg ml−1 gentamycin, and 10% fetal bovine serum (Sigma) in a 96-well cell culture plate at 106 cells per ml, with or without D4Ply, caspase inhibitor Z-VAD-FMK (carbobenzoxy-valyl-alanyl-aspartyl-[Omethyl]-fluoromethylketone) (Invivogen, Toulouse, France) at 10 μg ml−1, and TLR-4 ligand LPS (Invivogen) at 1 μg ml−1.
Murine macrophage cell lines. Murine macrophage and microglial cell lines were obtained through the NIH Biodefense and Emerging Infections Research Resources Repository, NIAID (Manassas, VA). The cell lines were derived from C57BI6/J mice and included wild-type (NR-9456), TLR2 knock-out (KO) (NR-9457), and TLR4 KO (NR-9458) macrophages, and wild type (NR-9460) and MAL/MyD88 KO (NR-9904) microglial cells. Both macrophage and microglial cells were used here as they were available and included all the KO cells as described. Murine macrophage and microglial cells were cultured in Dulbecco’s modified Eagle’s medium supplemented with 2 mmol l−1 glutamine, 10 μg ml−1 gentamycin, and 10% fetal bovine serum (Sigma). Cells were seeded at 1 × 106 cells per ml in a 48-well plate (Corning) overnight before stimulation by D4Ply. TLR-2 ligand bacterial lipopeptide (pam3CSK4, Invivogen) and TLR-4 ligand LPS were used as stimulation controls at 1 μg ml−1.
Recombinant pneumolysin truncation proteins. Wild-type pneumolysin and truncated mutants including D4Ply and domain 123 (D123) were purified as previously described.46 The domain 4 mutant deficient in cholesterol binding (D4Ply LT) was generated through site-directed mutagenesis to mutate Threonine 459 and Leucine 460 residues in domain 4 to Glycine (459,460 TL-GG) (using the quick change SDM Kit; Stratagene, Paisley, UK). These residues were selected based on the finding of Farrand et al.52 that the amino acid residue pair Threonine 459 and Leucine 460 are crucial for the interaction of pneumolysin with cholesterol, and these residues are conserved in the pneumolysin sequence. The resultant mutant protein was purified and shown to have a binding capacity for red blood cells reduced by >99% as judged by fluorescence-activated cell sorting (FACS) analysis (data not shown). Endotoxin levels of these recombinant proteins were <0.1 EU ml−1 of protein as determined by limulus assay (BioWhittaker, Walkersville, MD). Hemolytic assay was performed as described previously,53 with the exception that human peripheral blood samples were used instead of sheep blood. Native Ply showed hemolytic activity at concentrations ≥5 ng/ml−1, whereas D4Ply and D123Ply did not show any hemolytic activity at concentrations tested up to 5 μg ml−1.
Sodium dodecyl sulfate–polyacrylamide gel electrophoresis gel electrophoresis and western blotting were performed and all the recombinant proteins used were shown to be of good quality with no obvious degradation and reactive to specific antipneumolysin antibody (Supplementary Figure S3).
Measurement of cytokine production. Cell culture supernatants were collected for analysis of cytokines 48 h after stimulation. Cell culture supernatants from MNCs and PBMCs were assayed for human IL-2, IL-4, IL-6, IL-10, IL-17A, IFN-γ, and TNF-α using cytometric bead array (BD Biosciences) and for IL-1β using ELISA (eBioscience) according to the manufacturer’s instructions. Induction of mouse TNFα in wild-type and KO macrophages or microglial cells was measured by ELISA (eBioscience).
Statistical analysis. Two-group comparisons were analyzed using Student’s t test and multiple comparisons using analysis of variance. Statistical analysis was performed using GraphPad Prism (La Jolla, CA). P<0.05 was considered statistically significant.
References
Siber, G.R. Pneumococcal disease: prospects for a new generation of vaccines. Science 265, 1385–1387 (1994).
Peltola, H. Burden of meningitis and other severe bacterial infections of children in Africa: implications for prevention. Clin. Infect. Dis. 32, 64–75 (2001).
Weinberger, D.M., Malley, R & Lipsitch, M. Serotype replacement in disease after pneumococcal vaccination. Lancet 378, 1962–1973 (2011).
Spratt, B.G. & Greenwood, B.M. Prevention of pneumococcal disease by vaccination: does serotype replacement matter? Lancet 356, 1210–1211 (2000).
Paton, J.C. Novel pneumococcal surface proteins: role in virulence and vaccine potential. Trends Microbiol. 6, 85–87 (1998).
Lipsitch, M, Whitney, C.G., Zell, E, Kaijalainen, T, Dagan, R & Malley, R. Are anticapsular antibodies the primary mechanism of protection against invasive pneumococcal disease? PLoS Med. 2, e15 (2005).
Kadioglu, A, Gingles, N.A., Grattan, K, Kerr, A, Mitchell, T.J. & Andrew, P.W. Host cellular immune response to pneumococcal lung infection in mice. Infect. Immun. 68, 492–501 (2000).
Kadioglu, A, Coward, W, Colston, M.J., Hewitt, C.R. & Andrew, P.W. CD4-T-lymphocyte interactions with pneumolysin and pneumococci suggest a crucial protective role in the host response to pneumococcal infection. Infect. Immun. 72, 2689–2697 (2004).
Malley, R, Trzcinski, K, Srivastava, A, Thompson, C.M., Anderson, P.W. & Lipsitch, M. CD4 T cells mediate antibody-independent acquired immunity to pneumococcal colonization. Proc. Natl. Acad. Sci. USA 102, 4848–4853 (2005).
Lu, Y.J. et al. Interleukin-17A mediates acquired immunity to pneumococcal colonization. PLoS Pathog. 4, e1000159 (2008).
Zhang, Z, Clarke, T.B. & Weiser, J.N. Cellular effectors mediating Th17-dependent clearance of pneumococcal colonization in mice. J. Clin. Invest. 119, 1899–1909 (2009).
O'Connor, W, Zenewicz, L.A. & Flavell, R.A. The dual nature of TH17 cells: shifting the focus to function. Nat. Immunol. 11, 471–476 (2010).
Curtis, M.M. & Way, S.S. Interleukin-17 in host defence against bacterial, mycobacterial and fungal pathogens. Immunology 126, 177–185 (2009).
Milner, J.D. et al. Impaired TH17 cell differentiation in subjects with autosomal dominant hyper-IgE syndrome. Nature 452, 773–776 (2008).
Kiyono, H, Fukuyama, S, Kiyono, H & Fukuyama, S. NALT- versus Peyer’s-patch-mediated mucosal immunity. [Review; 102 refs]. Nat. Rev. Immunol. 4, 699–710 (2004).
Bernstein, J.M., Gorfien, J & Brandtzaeg, P. The immunobiology of the tonsils and adenoids In: Ogra P.L., Mestecky J, Lamm M.E., Strober W., McGhee J.R., & Bienenstock J (eds). Mucosal Immunology, Academic Press: San Diego pp 1339–1362 (1999).
Mattila, P.S., Hammarén-Malmi, S, Saxen, H, Kaijalainen, T, Käyhty, H & Tarkkanen, J. Adenoidectomy and nasopharyngeal carriage of Streptococcus pneumoniae in young children. Arch. Dis. Child. 95, 696–702 (2010).
Mattila, P.S., Hammarén-Malmi, S, Saxen, H, Kaijalainen, T, Käyhty, H & Tarkkanen, J. Adenoidectomy in young children and serum IgG antibodies to pneumococcal surface protein A and choline binding protein A. Int. J. Pediatr. Otorhinolaryngol. 76, 1569–1574 (2012).
Zhang, Q, Choo, S & Finn, A. Immune responses to novel pneumococcal proteins (Pneumolysin, PspA, PsaA and CbpA) in adenoidal B cells from children. Infect. Immun. 70, 5363–5369 (2002).
Zhang, Q. et al. Bacterial lipoproteins differentially regulate human primary and memory CD4+ T and B cell responses to pneumococcal protein antigens through Toll-like receptor 2. J. Infect. Dis. 201, 1753–1763 (2010).
Berry, A.M., Alexander, J.E., Mitchell, T.J., Andrew, P.W., Hansman, D & Paton, J.C. Effect of defined point mutations in the pneumolysin gene on the virulence of Streptococcus pneumoniae. Infect. Immun. 63, 1969–1974 (1995).
Alexander, J.E. et al. Amino acid changes affecting the activity of pneumolysin alter the behaviour of pneumococci in pneumonia. Microb. Pathog. 24, 167–174 (1998).
Ogunniyi, A.D., Woodrow, M.C., Poolman, J.T. & Paton, J.C. Protection against Streptococcus pneumoniae elicited by immunization with pneumolysin and CbpA. Infect. Immun. 69, 5997–6003 (2001).
Kirkham, L.A. et al. Construction and immunological characterization of a novel nontoxic protective pneumolysin mutant for use in future pneumococcal vaccines. Infect. Immun. 74, 586–593 (2006).
Zhang, Q. et al. Serum and mucosal antibody responses to pneumococcal protein antigens in children: relationships with carriage status. Eur. J. Immunol. 36, 46–57 (2006).
Zhang, Q. et al. Low CD4 T cell immunity to pneumolysin is associated with nasopharyngeal carriage of pneumococci in children. J. Infect. Dis. 195, 1194–1202 (2007).
Baba, H. et al. Essential role of domain 4 of pneumolysin from Streptococcus pneumoniae in cytolytic activity as determined by truncated proteins. Biochem. Biophys. Res. Commun. 281, 37–44 (2001).
Yang, L. et al. IL-21 and TGF-[bgr] are required for differentiation of human TH17 cells. Nature 454, 350–352 (2008).
Louten, J, Boniface, K & de Waal Malefyt, R. Development and function of TH17 cells in health and disease. J. Allergy Clin. Immunol. 123, 1004–1011 (2009).
Olliver, M, Hiew, J, Mellroth, P, Henriques-Normark, B & Bergman, P. Human monocytes promote Th1 and Th17 responses to Streptococcus pneumoniae. Infect. Immun. 79, 4210–4217 (2011).
Lundgren, A. et al. Characterization of Th17 responses to Streptococcus pneumoniae in humans: comparisons between adults and children in a developed and a developing country. Vaccine 30, 3897–3907 (2012).
Khader, S.A., Gaffen, S.L. & Kolls, J.K. Th17 cells at the crossroads of innate and adaptive immunity against infectious diseases at the mucosa. Mucosal Immunol. 2, 403–411 (2009).
Dubin, P.J. & Kolls, J.K. Th17 cytokines and mucosal immunity. Immunol. Rev. 226, 160–171 (2008).
Acosta-Rodriguez, E.V. et al. Surface phenotype and antigenic specificity of human interleukin 17-producing T helper memory cells. Nat. Immunol. 8, 639–646 (2007).
Lin, Y, Slight, S & Khader, S. Th17 cytokines and vaccine-induced immunity. Semin. Immunopathol. 32, 79–90 (2010).
Chen, K. et al. Th17 cells mediate clade-specific, serotype-independent mucosal immunity. Immunity 35, 997–1009 (2011).
Happel, K.I. et al. Divergent roles of IL-23 and IL-12 in host defense against Klebsiella pneumoniae. J. Exp. Med. 202, 761–769 (2005).
Kolls, J.K. & Lindén, A. Interleukin-17 family members and inflammation. Immunity 21, 467–476 (2004).
Cecchinato, V. et al. Altered balance between Th17 and Th1 cells at mucosal sites predicts AIDS progression in simian immunodeficiency virus-infected macaques. Mucosal. Immunol. 1, 279–288 (2008).
Aujla, S.J., Dubin, P.J. & Kolls, J.K. Th17 cells and mucosal host defense. Semin. Immunol. 19, 377–382 (2007).
Wright, A.K.A. et al. Experimental human pneumococcal carriage augments IL-17A-dependent T-cell defence of the lung. PLoS Pathog. 9, e1003274 (2013).
Zhang, Q, Leong, S.C., McNamara, P.S., Mubarak, A, Malley, R & Finn, A. Characterisation of regulatory T cells in nasal associated lymphoid tissue in children: relationships with pneumococcal colonization. PLoS Pathog. 7, e1002175 (2011).
Malley, R & Anderson, P.W. Serotype-independent pneumococcal experimental vaccines that induce cellular as well as humoral immunity. Proc. Natl. Acad Sci. USA 109, 3623–3627 (2012).
Malley, R. et al. Recognition of pneumolysin by Toll-like receptor 4 confers resistance to pneumococcal infection. Proc. Natl. Acad Sci. USA 100, 1966–1971 (2003).
McNeela, E.A. et al. Pneumolysin activates the NLRP3 inflammasome and promotes proinflammatory cytokines independently of TLR4. PLoS Pathog. 6, e1001191 (2010).
Witzenrath, M. et al. The NLRP3 inflammasome is differentially activated by pneumolysin variants and contributes to host defense in pneumococcal pneumonia. J. Immunol. 187, 434–440 (2011).
Belyakov, I.M. & Ahlers, J.D. What role does the route of immunization play in the generation of protective immunity against mucosal pathogens? J. Immunol. 183, 6883–6892 (2009).
Moffitt, K.L. et al. TH17-based vaccine design for prevention of streptococcus pneumoniae colonization. Cell Host Microbe 9, 158–165 (2011).
Moffitt, K.L., Malley, R & Lu, Y.-J. Identification of protective pneumococcal TH17 antigens from the soluble fraction of a killed whole cell vaccine. PLoS One 7, e43445 (2012).
O'Brien, K.L. & Nohynek, H. Report from a WHO Working Group: standard method for detecting upper respiratory carriage of Streptococcus pneumoniae. Pediatr. Infect. Dis. J. 22, e1–11 (2003).
Zhang, Q, Choo, S & Finn, A. Immune responses to novel pneumococcal proteins pneumolysin, PspA, PsaA, and CbpA in adenoidal B cells from children. Infect. Immun. 70, 5363–5369 (2002).
Farrand, A.J., LaChapelle, S, Hotze, E.M., Johnson, A.E. & Tweten, R.K. Only two amino acids are essential for cytolytic toxin recognition of cholesterol at the membrane surface. Proc. Natl. Acad Sci. USA 107, 4341–4346 (2010).
Benton, K.A., Paton, J.C. & Briles, D.E. Differences in virulence for mice among Streptococcus pneumoniae strains of capsular types 2, 3, 4, 5, and 6 are not attributable to differences in pneumolysin production. Infect. Immun. 65, 1237–1244 (1997).
Acknowledgements
We thank the patients who took part in the study and the theatre staff in the Liverpool Children’s Hospital for helping the collection of samples. We also acknowledge funding support from Action Medical Research, UK.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Additional information
SUPPLEMENTARY MATERIAL is linked to the online version of the paper
Rights and permissions
About this article
Cite this article
Gray, C., Ahmed, M., Mubarak, A. et al. Activation of memory Th17 cells by domain 4 pneumolysin in human nasopharynx-associated lymphoid tissue and its association with pneumococcal carriage. Mucosal Immunol 7, 705–717 (2014). https://doi.org/10.1038/mi.2013.89
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2013.89
This article is cited by
-
Differential IL-17A response to S. pneumoniae in adenoid tissue of children with sleep disordered breathing and otitis media with effusion
Scientific Reports (2019)
-
IL-17A expression in the adenoid tissue from children with sleep disordered breathing and its association with pneumococcal carriage
Scientific Reports (2018)
-
Morphine compromises bronchial epithelial TLR2/IL17R signaling crosstalk, necessary for lung IL17 homeostasis
Scientific Reports (2015)