Abstract
Objective:
To explore appetite-related hormones following stress in overweight individuals, and their relationship with night eating (NE) status.
Method:
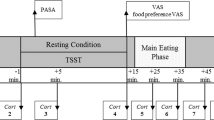
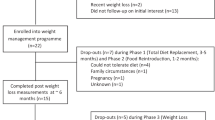
We measured plasma cortisol and ghrelin concentrations, and recorded ratings of stress and hunger in response to a physiological laboratory stressor (cold pressor test, CPT), in overweight women with (n=11; NE) and without (n=17; non-NE) NE.
Results:
Following the CPT, cortisol (P<0.001) and ghrelin (P<0.05) levels increased, as did stress and hunger ratings (all P<0.001), across all subjects (NE and non-NE). NE exhibited higher baseline cortisol (P<0.05) levels than non-NE. NE also had greater cortisol area under the curve (AUC) than non-NE (P=0.019), but not when controlling for baseline cortisol levels. Ghrelin baseline and AUC did not differ between groups. NE showed higher AUC stress (P<0.05), even when controlling for baseline stress.
Discussion:
Overweight individuals showed increased cortisol, ghrelin, stress and hunger following a laboratory stressor, and there was some evidence for greater increases in cortisol and subjective stress among NE. The greater AUC cortisol level in NE was due to higher baseline levels, but the group difference in stress was in direct response to the stressor. Our results support a role for cortisol and stress in NE.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Allison KC, Lundgren JD, Reardon JP, Geliebter A, Gluck ME, Vinai P et al. Proposed diagnosed criteria for night eating syndrome. Int J Eating Disorder 2010; 43: 6.
Rand CS, Macgregor AM, Stunkard AJ . The night eating syndrome in the general population and among postoperative obesity surgery patients. Int J Eat Disord 1997; 22: 65–69.
Gluck ME, Geliebter A, Satov T . Night eating syndrome is associated with depression, low self-esteem, reduced daytime hunger, and less weight loss in obese outpatients, 2001 Obes Res 9: 264–267.
Thompson OM, Ballew C, Resnicow K, Gillespie C, Must A, Bandini LG et al. Dietary pattern as a predictor of change in BMI z-score among girls. Int J Obes (Lond) 2006; 30: 176–182.
Marshall HM, Allison KC, O’Reardon JP, Birketvedt G, Stunkard AJ . Night eating syndrome among nonobese persons. Int J Eat Disord 2004; 35: 217–222.
Andersen GS, Stunkard AJ, Sorensen TI, Petersen L, Heitmann BL . Night eating and weight change in middle-aged men and women. Int J Obes Relat Metab Disord 2004; 28: 1338–1343.
Pike KM, Wilfley D, Hilbert A, Fairburn CG, Dohm FA, Striegel-Moore RH . Antecedent life events of binge-eating disorder. Psychiatry Res 2006; 142: 19–29.
Crowther JH, Sanftner J, Bonifazi DZ, Shepherd KL . The role of daily hassles in binge eating. Int J Eat Disord 2001; 29: 449–454.
Tuschen-Caffier B, Vogele C . Psychological and physiological reactivity to stress: an experimental study on bulimic patients, restrained eaters and controls. Psychother Psychosom 1999; 68: 333–340.
Allison KC, Ahima RS, O’Reardon JP, Dinges DF, Sharma V, Cummings DE et al. Neuroendocrine profiles associated with energy intake, sleep, and stress in the night eating syndrome. J Clin Endocrinol Metab 2005; 90: 6214–6217.
Stunkard A, Birketvedt GS . Night eating and nosology. Int J Obes Relat Metab Disord 2002; 26: 588.
Pawlow LA, O’Neil PM, Malcolm RJ . Night eating syndrome: effects of brief relaxation training on stress, mood, hunger, and eating patterns. Int J Obes Relat Metab Disord 2003; 27: 970–978.
George SA, Khan S, Briggs H, Abelson JL . CRH-stimulated cortisol release and food intake in healthy, non-obese adults. Psychoneuroendocrinology 2010; 35: 607–612.
Bray GA . Autonomic and endocrine factors in the regulation of food intake. Brain Res Bull 1985; 14: 505–510.
Dallman M . Fast glucocorticoid favors 'the munchies. Trends Endocrinol Metab 2003; 14: 394–396.
Koo-Loeb J, Costello N, Light K, Girdler S . Women with eatigng disorder tendencies display altered cardiovascular, neuroendocrine, and psychosocial profiles. Psychosom Med 2000; 62: 10.
Gluck M, Geliebter A, Hung J, Yahav E . Cortisol, hunger, and desire to binge eat following a cold stress test in obese women with binge eating disorder. Psychosom Med 2004; 66: 6.
Diz-Chaves Y . Ghrelin, appetite regulation, and food reward: interaction with chronic stress. Int J Pept 2011; 2011: 898450.
Currie PJ, Khelemsky R, Rigsbee EM, Dono LM, Coiro CD, Chapman CD et al. Ghrelin is an orexigenic peptide and elicits anxiety-like behaviors following administration into discrete regions of the hypothalamus. Behav Brain Res 2012; 226: 96–105.
Stengel A, Wang L, Tache Y . Stress-related alterations of acyl and desacyl ghrelin circulating levels: mechanisms and functional implications. Peptides 2011; 32: 2208–2217.
Chuang JC, Perello M, Sakata I, Osborne-Lawrence S, Savitt JM, Lutter M et al. Ghrelin mediates stress-induced food-reward behavior in mice. J Clin Invest 2011; 121: 2684–2692.
Lambert E, Lambert G, Ika-Sari C, Dawood T, Lee K, Chopra R et al. Ghrelin modulates sympathetic nervous system activity and stress response in lean and overweight men. Hypertension 2011; 58: 43–50.
Geliebter A, Gluck ME, Hashim SA . Plasma ghrelin concentrations are lower in binge-eating disorder. J Nutr 2005; 135: 1326–1330.
Monteleone P, Fabrazzo M, Tortorella A, Martiadis V, Serritella C, Maj M . Circulating ghrelin is decreased in non-obese and obese women with binge eating disorder as well as in obese non-binge eating women, but not in patients with bulimia nervosa. Psychoneuroendocrinology 2005; 30: 243–250.
Tschop M, Weyer C, Tataranni PA, Devanarayan V, Ravussin E, Heiman ML . Circulating ghrelin levels are decreased in human obesity. Diabetes 2001; 50: 707–709.
Kristensson E, Sundqvist M, Hakanson R, Lindstrom E . High gastrin cell activity and low ghrelin cell activity in high-anxiety Wistar Kyoto rats. J Endocrinol 2007; 193: 245–250.
Rouach V, Bloch M, Rosenberg N, Gilad S, Limor R, Stern N et al. The acute ghrelin response to a psychological stress challenge does not predict the post-stress urge to eat. Psychoneuroendocrinology 2007; 32: 693–702.
Birketvedt GS, Florholmen J, Sundsfjord J, Osterud B, Dinges D, Bilker W et al. Behavioral and neuroendocrine characteristics of the night-eating syndrome. JAMA 1999; 282: 657–663.
Schwabe L, Haddad L, Schachinger H . HPA axis activation by a scoially evaluated cold-pressor test. Psychoneuroendocrimology 2008; 33: 6.
Steptoe A, Kunz-Ebrecht SR, Brydon L, Wardle J . Central adiposity and cortisol responses to waking in middle-aged men and women. Int J Obes Relat Metab Disord 2004; 28: 1168–1173.
Steptoe A, Wardle J . Cardiovascular stress responsivity, body mass and abdominal adiposity. Int J Obes (Lond) 2005; 29: 1329–1337.
Gluck ME, Geliebter A, Satov T . Night eating syndrome is associated with depression, low self-esteem, reduced daytime hunger, and less weight loss in obese outpatients. Obes Res 2001; 9: 264–267.
Dempster P, Aitkens S . A new air displacement method for the determination of human body composition. Med Sci Sports Exerc 1995; 27: 1692–1697.
Lustyk MK, Olson KC, Gerrish WG, Holder A, Widman L . Psychophysiological and neuroendocrine responses to laboratory stressors in women: Implications of menstrual cycle phase and stressor type. Biol Psychol 2010; 83: 84–92.
Newman E, O’Connor DB, Conner M . Daily hassles and eating behaviour: the role of cortisol reactivity status. Psychoneuroendocrinology 2007; 32: 125–132.
O'Connor DB, Jones F, Conner M, McMillan B, Ferguson E . Effects of daily hassles and eating style on eating behavior. Health Psychol 2008; 27 (Suppl): S20–S31.
Bose M, Olivan B, Laferrere B . Stress and obesity: the role of the hypothalamic-pituitary-adrenal axis in metabolic disease. Curr Opin Endocrinol Diabetes Obes 2009; 16: 340–346.
Marzullo P, Verti B, Savia G, Walker GE, Guzzaloni G, Tagliaferri M et al. The relationship between active ghrelin levels and human obesity involves alterations in resting energy expenditure. J Clin Endocrinol Metab 2004; 89: 936–939.
Al'Absi M, Bongard S, Buchanan T, Pincomb GA, Licinio J, Lovallo WR . Cardiovascular and neuroendocrine adjustment to public speaking and mental arithmetic stressors. Psychophysiology 1997; 34: 266–275.
Buchanan TW, al’Absi M, Lovallo WR . Cortisol fluctuates with increases and decreases in negative affect. Psychoneuroendocrinology 1999; 24: 227–241.
Schlotz W, Kumsta R, Layes I, Entringer S, Jones A, Wust S . Covariance between psychological and endocrine responses to pharmacological challenge and psychosocial stress: a question of timing. Psychosom Med 2008; 70: 787–796.
Epel E, Lapidus R, McEwen B, Brownell K . Stress may add bite to appetitie in women: a laboratory study of stress-induced cortisol and eating behavior. Psychoneuroendocrimology 2001; 26: 13.
Tataranni P, Larson D, Snitker S, Young J, Flatt J, Ravussin E . Effects of glucocorticoids on energy metabolism and food intake in humans. Am J Physiol 1996; 271 (Part 1): 9.
Acknowledgements
We thank Sami A Hashim, MD for medical supervision, Margarita Lorence for assistance, and Leora Benson and Ku-Yu (Virginia) Chang for help with manuscript preparation. Support was provided in part by NIH grants R01 DK 54318, R01 DK 074046 (AG), K99 088360 (SC), DK 07559 (MG) and MO1 RROO64529 (Columbia University GCRC). Anthropometrics and UWW results were provided by the Body Composition Lab, and cortisol and ghrelin assays were provided by the Hormone-Metabolite Lab, core service labs of the New York Obesity Center, DK 26687.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Geliebter, A., Carnell, S. & Gluck, M. Cortisol and ghrelin concentrations following a cold pressor stress test in overweight individuals with and without night eating. Int J Obes 37, 1104–1108 (2013). https://doi.org/10.1038/ijo.2012.166
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2012.166
Keywords
This article is cited by
-
Examining the Relationship Between Pain Intensity and Emotional Eating Among Latinos in a Federally Qualified Health Center: The Role of Anxiety Sensitivity
Journal of Immigrant and Minority Health (2019)
-
Stress does not affect ghrelin secretion in obese and normal weight women
Eating and Weight Disorders - Studies on Anorexia, Bulimia and Obesity (2017)
-
Stress-related cortisol response and laboratory eating behavior in obese women
Eating and Weight Disorders - Studies on Anorexia, Bulimia and Obesity (2016)
-
Hormonal Factors and Disturbances in Eating Disorders
Current Psychiatry Reports (2016)
-
Using the Neuroscience of Obesity, Eating Behavior, and Sleep to Inform the Neural Mechanisms of Night Eating Syndrome
Current Obesity Reports (2014)