Abstract
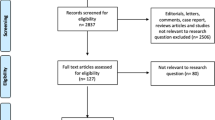
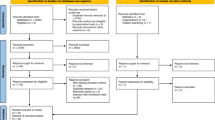
A systematic review of the literature about the causal relationship between priapism and adrenergic α-blockers used for the treatment of lower urinary tract symptoms (LUTS) and arterial hypertension was accomplished. While opportunely describing a case of tamsulosin-induced priapism, we reviewed the literature using MEDLINE, COCHRANE and LILACS libraries, selecting all the articles until the present time addressing the association between priapism and α-blockers. Our patient was a healthy 32-year-old man who reported LUTS. His prostate was firm and moderately enlarged on digital rectal examination, measuring 30 grams on transabdominal ultrasound. Empirical treatment with tamsulosin was initiated and he developed priapism the day after the first dose of the drug. Erection was reverted by aspiration of the corpora and intracavernosal injection of adrenaline. Despite the late presentation (40 h of erection), he had no ED on follow-up. In the systematic review, among 2157 articles on priapism, only 13 similar cases reported α-blockers as the etiology of priapism. Therefore, adrenergic α-blockers are effective and safe drugs, with few serious adverse reactions. Nevertheless the association with priapism is well documented and related to substantial morbidity, this is an infrequent event and should not preclude their use, considering that the patient be sufficiently informed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Hofner K, Claes H, De Reijke TM, Folkestad B, Speakman MJ . Tamsulosin 0.4 mg once daily: effect on sexual function in patients with lower urinary tract symptoms suggestive of benign prostatic obstruction. Eur Urol 1999; 36: 335–341.
Marberger M, Harkaway R, de la Rosette J . Optimising the medical management of benign prostatic hyperplasia. Eur Urol 2004; 45: 411–419.
Gilling P, Jacobi G, Tammela T . Efficacy of dutasteride and finasteride for the treatment of benign prostatic hyperplasia: results of the 1-year Enlarged Prostate International Comparative Study (EPICS). Br J Urol 2005; 95: 1–104.
McConnell JD, Roehrborn CG, Bautista OM, Andriole Jr GL, Dixon CM, Kusek JW et al. The long-term effect of doxazosin, finasteride, and combination therapy on the clinical progression of benign prostatic hyperplasia. N Engl J Med 2003; 349: 2387–2398.
Roehrborn CG, Siami P, Barkin J, Damiao R, Major-Walker K, Morrill B et al. The effects of dutasteride, tamsulosin and combination therapy on lower urinary tract symptoms in men with benign prostatic hyperplasia and prostatic enlargement: 2-year results from the CombAT study. J Urol 2008; 179: 616–621; discussion 621.
Siegel S, Streem SB, Steinmuller DR . Prazosin-induced priapism. Pathogenic and therapeutic implications. Br J Urol 1988; 61: 165.
Bhalla AK, Hoffbrand BI, Phatak PS, Reuben SR . Prazosin and priapism. Br Med J 1979; 2: 1039.
Kilinc M, Piskin M, Guven S, Gurbuz R, Odev K, Kaynar M . Partial priapism secondary to tamsulosin: a case report and review of the literature. Andrologia 2009; 41: 199–201.
Banos JE, Bosch F . Prazosin-induced priapism. Br J Urol 1989; 64: 205–206.
Shamloul R, Atteya A, Elnashaar A, Gadallah A, Zohdy W, Abdelsalam W . Intracavernous sodium nitroprusside (SNP) versus papaverine/phentolamine in erectile dysfunction: a comparative study of short-term efficacy and side-effects. J Sex Med 2005; 2: 117–120.
Goldstein I . Oral phentolamine: an alpha-1, alpha-2 adrenergic antagonist for the treatment of erectile dysfunction. Int J Impot Res 2000; 12 (Suppl 1): S75–S80.
Padma-Nathan H, Goldstein I, Klimberg I, Coogan C, Auerbach S, Lammers P . Long-term safety and efficacy of oral phentolamine mesylate (Vasomax) in men with mild to moderate erectile dysfunction. Int J Impot Res 2002; 14: 266–270.
Zorgniotti AW . Experience with buccal phentolamine mesylate for impotence. Int J Impot Res 1994; 6: 37–41.
Pahuja A, Bashir J, Williamson EM, Barber N . Unresolved priapism secondary to tamsulosin. Int J Impot Res 2005; 17: 293–294.
Dodds PR, Batter SJ, Serels SR . Priapism following ingestion of tamsulosin. J Urol 2003; 169: 2302.
Platz EA, Smit E, Curhan GC, Nyberg LM, Giovannucci E . Prevalence of and racial/ethnic variation in lower urinary tract symptoms and noncancer prostate surgery in US men. Urology 2002; 59: 877–883.
Burke JR, Hirst G . Priapism and prazosin. Med J Aust 1980; 1: 382–383.
Bullock N . Prazosin-induced priapism. Br J Urol 1988; 62: 487–488.
Ylitalo P, Pasternack A . Priapism-side-effect of prazosin in patients with renal failure. Acta Med Scand 1983; 213: 319–320.
Qazi HA, Ananthakrishnan K, Manikandan R, Fordham MV . Stuttering priapism after ingestion of alfuzosin. Urology 2006; 68: 890–896.
Vaidyanathan S, Soni BM, Singh G, Sett P, Krishnan KR . Prolonged penile erection association with terazosin in a cervical spinal cord injury patient. Spinal Cord 1998; 36: 805.
Yaqoob M, Parys B, Ahmad R . Prazosin induced priapism in a patient on continuous ambulatory peritoneal dialysis (CAPD). Perit Dial Int 1991; 11: 363–364.
Sateghi-Nejad H, Jackson I . New onset priapism associated with ingestion of terazosin in otherwise healthy men. J Sex Med 2007; 4: 1766–1768.
Avisrror MU, Fernandez IA, Sanchez AS, Garcia-Pando AC, Arias LM, Del Pozo JG . Doxazosin and priapism. J Urol 2000; 163: 238.
Acknowledgements
This paper received no funding or any type of financial support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Article not being considered for publication by any other Journal.
Rights and permissions
About this article
Cite this article
Spagnul, S., Cabral, P., Verndl, D. et al. Adrenergic α-blockers: an infrequent and overlooked cause of priapism. Int J Impot Res 23, 95–98 (2011). https://doi.org/10.1038/ijir.2011.12
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2011.12
Keywords
This article is cited by
-
Blasenspeicher- und Entleerungsstörungen
Der Urologe (2017)