Summary:
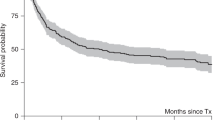
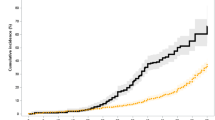
The role of allogeneic bone marrow transplantation in lymphoma remains uncertain. We have analyzed 1185 allogeneic transplants for lymphoma reported to the EBMT registry between 1982 and 1998 and compared the results with those of 14 687 autologous procedures performed over the same period. Patients receiving allogeneic transplants were subdivided according to histology: low-grade non-Hodgkin's lymphoma (NHL) 231 patients; intermediate-grade NHL 147 patients; high-grade NHL 255 patients; lymphoblastic NHL 314 patients; Burkitt's lymphoma 71 patients; and Hodgkin's disease 167 patients. These patients received allogeneic transplants as their first transplant procedure. Actuarial overall survival (OS) at 4 years from transplantation was: low-grade NHL 51.1%; intermediate-grade NHL 38.3%; high-grade NHL 41.2%; lymphoblastic lymphoma 42.0% years; Burkitt's lymphoma 37.1%; and Hodgkin's disease 24.7% years. These outcomes are relatively poor because of the high procedure-related mortality associated with these procedures, particularly in patients with Hodgkin's disease (51.7% actuarial procedure-related mortality at 4 years). Multivariate analysis showed that for all lymphomas apart from Hodgkin's disease, status at transplantation significantly affected outcome. A matched analysis was performed: for all categories of lymphoma, OS was better for autologous than for allogeneic transplantation. Relapse rate was better in the allogeneic group for low-, intermediate- and high-grade, and lymphoblastic NHL. It was equivalent for Burkitt's lymphoma and worse in the allogeneic group for Hodgkin's disease. Allogeneic transplantation appears to be superior to autologous procedures in terms of producing a lower relapse rate. The toxicity of allogeneic procedures must however be reduced before this translates into an improvement in OS.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Chopra R, McMillan AK, Linch DC et al. The place of high-dose BEAM therapy and autologous bone marrow transplantation in poor-risk Hodgkin's disease. A single-center eight-year study of 155 patients. Blood 1993; 81: 1137–1145.
Linch DC, Winfield D, Goldstone AH et al. Dose intensification with autologous bone-marrow transplantation in relapsed and resistant Hodgkin's disease: results of a BNLI randomised trial. Lancet 1993; 341: 1051–1054.
Mills W, Chopra R, McMillan A et al. BEAM chemotherapy and autologous bone marrow transplantation for patients with relapsed or refractory non-Hodgkin's lymphoma. J Clin Oncol 1993; 13: 588–595.
Philip T, Armitage JO, Spitzer G et al. High-dose therapy and autologous bone marrow transplantation after failure of conventional chemotherapy in adults with intermediate-grade or high-grade non-Hodgkin's lymphoma. N Engl J Med 1987; 316: 1493–1498.
Philip T, Guglielmi C, Hagenbeek A et al. Autologous bone marrow transplantation as compared with salvage chemotherapy in relapses of chemotherapy-sensitive non-Hodgkin's lymphoma [see comments]. N Engl J Med 1995; 333: 1540–1545.
Leonard BM, Hetu F, Busque L et al. Lymphoma cell burden in progenitor cell grafts measured by competitive polymerase chain reaction: less than one log difference between bone marrow and peripheral blood sources. Blood 1998; 91: 331–339.
Verdonck LF . Allogeneic versus autologous bone marrow transplantation for refractory and recurrent low-grade non-Hodgkin's lymphoma: updated results of the Utrecht experience. Leuk Lymphoma 1999; 34: 129–136.
Sykes M, Preffer F, McAfee S et al. Mixed lymphohaemopoietic chimerism and graft-versus-lymphoma effects after non-myeloablative therapy and HLA-mismatched bone-marrow transplantation. Lancet 1999; 353: 1755–1759.
Milpied N, Fielding AK, Pearce RM et al. Allogeneic bone marrow transplant is not better than autologous transplant for patients with relapsed Hodgkin's disease. European Group for Blood and Bone Marrow Transplantation. J Clin Oncol 1996; 14: 1291–1296.
Chopra R, Goldstone AH, Pearce R et al. Autologous versus allogeneic bone marrow transplantation for non-Hodgkin's lymphoma: a case-controlled analysis of the European Bone Marrow Transplant Group Registry data. J Clin Oncol 1992; 10: 1690–1695.
National Cancer Institute. Sponsored study of classifications of non-Hodgkin's lymphomas. Summary and description of Working Formulation for clinical usage. Cancer 1982; 29: 2112–2129.
Harris NL, Jaffe ES, Stein H et al. A revised European–American classification of lymphoid neoplasms: a proposal from the International Lymphoma Study Group. Blood 1994; 84: 1361–1392.
de Lima M, van Besien K, Giralt SA et al. Bone marrow transplantation after failure of autologous transplant for non-Hodgkin's lymphoma. Bone Marrow Transplant 1997; 19: 121–127.
Moreau P, Mechinaud F, Mahe B et al. Successful allogeneic bone marrow transplantation for early relapse after autologous bone marrow transplantation in two cases of aggressive high-grade non-Hodgkin's lymphoma. Bone Marrow Transplant 1996; 18: 665–667.
Tsai T, Goodman S, Saez R et al. Allogeneic bone marrow transplantation in patients who relapse after autologous transplantation. Bone Marrow Transplant 1997; 20: 859–863.
Jones RJ, Ambinder RF, Piantadosi S et al. Evidence of a graft-versus-lymphoma effect associated with allogeneic bone marrow transplantation. Blood 1991; 7: 649–653.
Dann EJ, Daugherty CK, Larson RA . Allogeneic bone marrow transplantation for relapsed and refractory Hodgkin's disease and non-Hodgkin's lymphoma. Bone Marrow Transplant 1997; 20: 369–374.
Ratanatharathorn V, Uberti J, Karanes C et al. Prospective comparative trial of autologous versus allogeneic bone marrow transplantation in patients with non-Hodgkin's lymphoma. Blood 1994; 84: 1050–1055.
Copelan EA, Kapoor N, Gibbins B et al. Allogeneic marrow transplantation in non-Hodgkin's lymphoma. Bone Marrow Transplant 1990; 5: 47–50.
Schouten IC, Raemaekers JJ, Kluin NH et al. High-dose therapy followed by bone marrow transplantation for relapsed follicular non-Hodgkin's lymphoma. Dutch HOVON Group. Ann Hematol 1996; 73: 273–277.
van Besien KW, Khouri IF, Giralt SA et al. Allogeneic bone marrow transplantation for refractory and recurrent lowgrade lymphoma: the case for aggressive management. J Clin Oncol 1995; 13: 1096–1102.
van Besien KW, Mehra RC, Giralt SA et al. Allogeneic bone marrow transplantation for poor-prognosis lymphoma: response, toxicity and survival depend on disease histology. Am J Med 1996; 100: 299–307.
van Besien KW, Sobocinski KA, Rowlings PA et al. Allogeneic bone marrow transplantation for low-grade lymphoma. Blood 1998; 92: 1832–1836.
Attal M, Socie G, Molina L et al. Allogeneic bone marrow transplantation for refractory and recurrent follicular lymphoma: a case-matched analysis with autologous transplantation from the French bone marrow transplant group registry data. Blood 1997; 20: 1120a.
Mandigers CM, Raemaekers JM, Schattenberg AV et al. Allogeneic bone marrow transplantation with T-cell-depleted marrow grafts for patients with poor-risk relapsed low-grade non-Hodgkin's lymphoma. Br J Haematol 1998; 100: 198–206.
Sullivan KM, Weiden PL, Storb R et al. Influence of acute and chronic graft-versus-host disease on relapse and survival after bone marrow transplantation from HLA-identical siblings as treatment of acute and chronic leukemia. Blood 1989; 73: 1720–1728.
van Besien KW, de Lima M, Giralt SA et al. Management of lymphoma recurrence after allogeneic transplantation: the relevance of graft-versus-lymphoma effect. Bone Marrow Transplant 1997; 19: 977–982.
Khouri IF, Keating M, Champlin R et al. Transplant-lite: induction of graft-versus-malignancy using fludarabine-based nonablative chemotherapy and allogeneic blood progenitor-cell transplantation as treatment for lymphoid malignancies. J Clin Oncol 1998; 16: 2817–2824.
Kottaridis PD, Chakraverty R, Milligan D et al. A non-myeloablative regimen for allografting high-risk patients: low toxicity, stable engraftment without GVHD, disease control and potential for GVL with adoptive immunotherapy. Blood. 1999; 94 (Suppl 1): 348a.
Khouri I, Lee M-S, Palmer L et al. Transplant-lite using fludarabine-cyclophosphamide (FC) and allogeneic stem cell transplant (AlloSCT) for low-grade lymphoma (LGL). Blood. 1999; 94 (Suppl 1): 348a.
Russell NH, Cull G, Byrne JL et al. Evaluation of non-myeloablative conditioning combining BEAM within vivo pre-transplant Campath-IG for allogeneic transplantation in patients with lymphoma. Blood 1999; 94 (Suppl. 1): 348a.
Korbling M, Przepiorka D, Huh YO et al. Allogeneic blood stem cell transplantation for refractory leukemia and lymphoma: potential advantage of blood over marrow allografts. Blood 1995; 85: 1659–1665.
Bensinger W, Martin P, Clift R et al. A prospective randomised trial of peripheral blood stem cells or marrow for patients undergoing allogeneic transplantation for hematologic malignancies. Blood 1999; 94 (Suppl. 1): 368a.
Acknowledgements
We gratefully acknowledge the collaboration of the large number of contributing transplant centers throughout and outside Europe. The following centers have registered over 50 lymphoma transplants with the EBMT, which have been used in this study:
Australia: Alfred Hospital, Melbourne; Royal Perth Hospital, Perth. Austria: AKH, Wein. Belgium: University Hospital, Leuven; Institut Jules Bordet, Brussels; Cliniques Universitaires St. Luc, Brussels; A.Z. Sint-Jan, Brugge; University of Liege, Liege. Croatia: University Hospital Centre-Rebro, Zagreb. Czech Republic: Charles University Hospital, Pilsen; Charles University Hospital, Praha. Denmark: Rigshospitalet, Copenhagen; Herlev Hospital, Herlev. Finland: Central Hospital, Turku; University Central Hospital, Helsinki. France: Hôpital Necker, Paris; Hôpital E. Herriot, Lyon Cedex 08; Hôpital Saint Antoine, Paris; Hotel Dieu, Paris; Institut Paoli Calmettes, Marseille; Hôpital St Jacques, Besançon; Centre Leon Berard, Lyon; Hôpital Nord, Saint Etienne; Centre Hospitalier Intercommunal, Creteil; Hotel Dieu, Nantes; Pitie-Salpetriere, Paris; Hôpital La Miletrie, Poitiers; Hôpital du Haut Leveque, Pessac; Hôpital A. Michallon, Grenoble; Hôpital Bretonneau, Tours; Centre Jaen Perrin, Clermont Ferrand; Hôpital Claude Huriez, Lille; Institut Gustave Roussy, Villejuif; Hôpital de Purpan, Toulouse; CHRU, Angers; Hôpital Percy, Clamart; Institut Gustave Roussy, Villejuif; Hôpital St. Louis, Paris. Germany: Universität Ulm, Ulm; Christian-Albrechts-University, Kiel; University Hospital, Essen; Medical School, Hannover; Universität Frankfurt, Frankfurt; Klinikum Nürnberg, Nürnberg; University of Saarland, Homburg/Saarland. Greece: The George Papanicolaou, Exokhi; Evangelismos Hospital, Athens. Italy: Ospedale San Martino, Genova; Centro Trapianti di Midollo Osseo, Cremona; Azienda Ospedaliera S. Giovanni, Torino; La Sapienza, Rome; Hospital San Orsola, Bologna; Centro Trapianti Midollo Osseo, Parma; IRCCS, Milano; Policlinico San Matteo, Pavia; Ospedale S. Camillo, Rome; Hospital San Maurizio, Bolzano; Ospedale di Careggi, Firenze; Ospedale Civile, Ravenna; Ospedale V. Cervello, Palermo; Hospital Casa Sollievo, San Giovanni Rotondo; Universita di Modena, Modena; Istituto Nazionale Tumori, Milano; Universita di Verona, Verona; Universita'degli Studi di Bari, Bari; Ospedale Bergamo, Bergamo; Universita di Udine, Udine; Universita Tor Vergata, Rome; Ospedale di Torrette, Ancona; Ospedale Oncologico, Cagliari. Netherlands: University Hospital, Utrecht; Daniel den Hoed Cancer Centre, Rotterdam; University Hospital St Radboud, Nijmegen; University Hospital Maastricht, Maastricth. Norway: The Norwegian Radium Hospital, Oslo. Portugal: Centro Porto, Porto. Spain: Hospital Clinic, Barcelona; Hospital de la Princesa, Madrid; Marqués de Valdecilla, Santander; Hospital Santa Creu i Sant Pau, Barcelona; Hospital Universitario ‘La Fé’, Valencia; Hospital Clinico, Salamanca; Hospital Duran i Reynals, Barcelona; Hospital Universitario ‘Virgen delR, Sevilla. Sweden: Huddinge University, Huddinge; University Hospital, Uppsala; University Hospital, Lund; Sahlgrenska University, Goeteborg. Switzerland: University Hospital, Zurich. United Kingdom: Royal Free Hospital, London; Royal Marsden Hospital, Sutton; University College London Hospital, London; Western General Hospital, Edinburgh; Glasgow Royal Infirmary, Glasgow; Newcastle General Hospital, Newcastle upon Tyne; Heartlands Hospital, Birmingham; Department of Haematology, Liverpool; Addenbrookes Hospital, Cambridge; University of Southampton, Southampton; City Hospital, Nottingham; Guy's Hospital, London; City Hospital, Belfast; St Bartholomews Hospital, London; Christie NHS Trust Hospital, Manchester.
Author information
Authors and Affiliations
Consortia
Rights and permissions
About this article
Cite this article
Peniket, A., Ruiz de Elvira, M., Taghipour, G. et al. An EBMT registry matched study of allogeneic stem cell transplants for lymphoma: allogeneic transplantation is associated with a lower relapse rate but a higher procedure-related mortality rate than autologous transplantation. Bone Marrow Transplant 31, 667–678 (2003). https://doi.org/10.1038/sj.bmt.1703891
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1703891
Keywords
This article is cited by
-
Ofatumumab as part of reduced intensity conditioning in high risk B-cell lymphoma patients: final long-term analysis from a prospective multicenter Phase-II Trial
Bone Marrow Transplantation (2024)
-
Outcome after autologous stem cell transplantation in primary refractory or relapsed Hodgkin lymphoma—a long-term follow-up single center experience
Annals of Hematology (2020)
-
The role of stem cell transplantation in the management of relapsed follicular lymphoma in the era of targeted therapies
Bone Marrow Transplantation (2019)
-
Hematopoietic stem cell transplantation in children and adolescents with relapsed or refractory B-cell non-Hodgkin lymphoma
International Journal of Hematology (2019)