Abstract
Objective:
Individual urinary iodine concentration (UIC) reflects iodine intake over a short time prior to sampling. Since eating habits are relatively constant in single subjects, UIC should be relatively constant in a given individual. The aim of our study was to verify this hypothesis by assessing UIC in repeated single urine samples from a group of healthy subjects.
Design and Setting:
A prospective sequential investigation was performed in 131 volunteer health workers or students recruited in our University hospital.
Interventions:
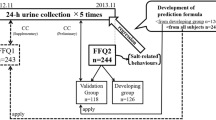
Single urine samples were taken in a nonfasting state, between 0900 and 1100 hours. Group 1 was composed by 131 subjects who collected one urine sample. Group 2 was composed by 11 subjects of the group 1, who collected multiple repeated urine samples (as a whole 158 urine samples, mean 14 samples each). UIC mean±s.d., median and coefficient of variation (CV%) was measured in both groups.
Results:
Interindividual UIC variation was wide, UIC ranging from 21 to 382 μg/l, mean 136±84 μg/l, median 124 μg/l, CV 62%. Also in the 11 subjects repeatedly sampling there were considerable differences among individual UIC average levels (ranging from 37±15 to 221±91 μg/l). However, in this second group, the intraindividual variation was considerably restricted (CV% 36).
Conclusions:
The present study shows that in a nonfasting state in mid-morning UIC is more stable from day to day in a single subject, depending on his eating habits, than in various subjects. Thus, a single urine sample even in nonfasting state may give some rough information about the individual's iodine status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Als C, Gerber H, Brander L, Luscher D, Lauber K, Rosler H (1994). Iodine supply varies over time in an affluent society such as Switzerland. Exp Clin Endocrinol 102 (Suppl 1), S189.
Als C, Haldimann M, Burgi E, Donati F, Gerber H, Zimmerli B (2003a). Swiss pilot study of individual seasonal fluctuations of urinary iodine concentration over two years: is age-dependency linked to the major source of dietary iodine? Eur J Clin Nutr 57, 636–646.
Als C, Helbling A, Peter K, Haldimann M, Zimmerli B, Gerber H (2000). Urinary iodine concentration follows a circadian rhythm: a study with 3023 spot urine samples in adults and children. J Clin Endocrinol Metab 85, 1367–1369.
Als C, Lauber K, Brander L, Luscher D, Rosler H (1995). The instability of dietary iodine supply over time in an affluent society. Experientia (Basel) 6, 623–633.
Als C, Minder C, Willems D, Van Thi HV, Gerber H, Bourdoux P (2003b). Quantification of urinary iodine: a need for revised thresholds. Eur J Clin Nutr 57, 1181–1188.
Andersen S, Pedersen KM, Perdersen IB, Laurberg P (2001). Variations in urinary iodine excretion and thyroid function. A 1-year study in healthy men. Europ J Endocrinol 144, 461–465.
Bourdoux P (1998). Evaluation of the iodine intake: problems of the iodine/creatinine ratio-comparison with iodine excretion and daily fluctuations of iodine concentration. Exp Clin Endocrinol Diabetes 106 (Suppl 3), S17–S20.
Busnardo B, Nacamulli D, Frigato F, Vianello-Dri A, De Vido D, Mian C et al. (2003). Normal values for thyroid ultrasonography, goitre prevalence, and urinary iodine concentration in school-children of the Veneto Region, Italy. J Endocrinol Invest 26, 991–996.
Dunn JT (1996). Seven deadly sins in confronting endemic iodine deficiency, and how to avoid them. J Clin Endocrinol Metab 81, 1332–1335.
Frigato F, Cerisara D, De Vido D, Garola E, Girelli ME, Insolia C et al. (1996). Epidemiological survey of goiter and iodine deficiency in Veneto region. J Endocrinol Invest 19, 734–738.
Garry PJ, Lashey DW, Owen GM (1973). Automated measurement of urinary iodine. Clin Chem 19, 950–953.
Girelli ME, Coin P, Mian C, Nacamulli D, Zambonini L, Piccolo M et al. (2004). Milk represents an important source of iodine in school-children of the Veneto region, Italy. J Endocrinol Invest 27, 709–713.
Guttikonda K, Burgess JR, Hynes K, Boyages S, Byth K, Parameswaran V (2002). Recurrent iodine deficiency in Tasmania, Australia: a salutary lesson in sustainable iodine prophylaxis and its monitoring. J Clin Endocrinol Metab 87, 2809–2815.
Hollowell JG, Staehling NW, Hannon WH, Flander DW, Gunter EW, Maberly GF et al. (1998). Iodine nutrition in the United States. Trends and public health implications: iodine excretion data from National Health and Nutrition Examination Surveys I and III (1971–1974 and 1988–1994). J Clin Endocrinol Metab 83, 3401–3408.
Hurrell RF (1997). Bioavailability of iodine. Eur J Clin Nutr 51 (Suppl 1), S9–S12.
Rasmussen LB, Larsen EH, Ovesen L (2000). Iodine content in drinking water and other beverages in Denmark. Eur J Clin Nutr 54, 57–60.
Rasmussen LB, Ovesen L, Bulow I, Jorgensen T, Knudsen N, Laurberg P et al. (2002). Dietary iodine intake and urinary iodine excretion in a Danish population: effect of geography, supplements and food choice. Br J Nutr 87, 61–69.
Rasmussen LB, Ovesen L, Christiansen E (1999). Day-to-day and within-day variation in urinary iodine excretion. Eur J Clin Nutr 52, 401–407.
Saxholt E (1996). Levnedsmiddeltabeller. 4. udgave, Levnedsmiddelstyrelsen.
Thomson CD, Colls AJ, Conaglen JV, Macormack M, Stiles M, Mann J (1997). Iodine status of New Zealand residents as assessed by urinary iodine excretion and thyroid hormones. Br J Nutr 78, 901–912.
Vought RL, Londom WT, Lutwak L, Dublin TD (1963). Reliability of estimates of serum inorganic iodine and daily faecal and urinary iodine excretion from single causal specimens. J Clin Endocrinol Metab 23, 1218–1228.
WHO, UNICEF, ICCIDD (1994). Indicators for Assessing Iodine Deficiency Disorders and their Control through Salt Iodization. World Health Organization: Geneva.
WHO UNICEF ICCIDD (2001). Assessment of the iodine Deficiency Disorders and Monitoring their Elimination 2d edn. World Health Organization: Geneva.
World Health Organization (1996). Trace Elements in Human Nutrition and Health. WHO: Geneva.
Acknowledgements
This work was supported by a Grant, ‘Ricerca sanitaria finalizzata’ n.572/01/95, from the Veneto Regional Authority, Italy. We also thank F Coburn for her help in editing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guarantors: B Busnardo, C Mian and ME Girelli.
Contributors: BB, CM and MEG are co-principal investigators and are responsible for writing the manuscript; LZ and MP performed the UIC analyses, DN abstracted and analysed the data, performed the statistics and graphs.
Rights and permissions
About this article
Cite this article
Busnardo, B., Nacamulli, D., Zambonin, L. et al. Restricted intraindividual urinary iodine concentration variability in nonfasting subjects. Eur J Clin Nutr 60, 421–425 (2006). https://doi.org/10.1038/sj.ejcn.1602334
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602334
Keywords
This article is cited by
-
Salivary iodine concentration in pregnant women and its association with iodine status and thyroid function
European Journal of Nutrition (2024)
-
Pre-analytical Factors Influence Accuracy of Urine Spot Iodine Assessment in Epidemiological Surveys
Biological Trace Element Research (2018)
-
Recommended number of participants in iodine nutrition studies is similar before and after an iodine fortification programme
European Journal of Nutrition (2014)