Abstract
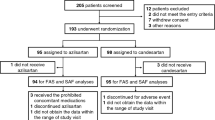
Antihypertensive efficacy, effects on left ventricular mass index (LVMI) and tolerability of telmisartan, an angiotensin II receptor blocker, were compared with those of hydrochlorothiazide (HCTZ). Adult patients with mild-to-moderate hypertension and an optimal acoustic window by two-dimensional echocardiography were randomised at baseline to 12 months' double-blind, once-daily treatment with telmisartan 80 mg or HCTZ 25 mg. Two-dimensional echocardiography and freehand precordial three-dimensional echocardiography and 24-h ambulatory blood pressure monitoring were performed at baseline and after treatment. Of the 41 telmisartan group patients and 28 HCTZ group patients, 40 and 25, respectively, completed the study. Following treatment, 24-h mean SBP (telmisartan 157 ± 11 vs 133 ± 7 mmHg, P<0.001; HCTZ 154 ± 10 vs 144 ± 11 mmHg, P<0.003) and DBP (telmisartan 96 ± 6 vs 83 ± 5 mmHg, P<0.001; HCTZ 95 ± 7 vs 87 ± 8 mmHg, P<0.003) were significantly reduced. Telmisartan produced significantly greater 24-h mean SBP and DBP reductions than HCTZ (P<0.001). LVMI was significantly reduced by telmisartan (141 ± 16 vs 125 ± 19 g/m2, P<0.001), but not by HCTZ (139 ± 20 vs 135 ± 22 g/m2). Incidences of adverse events in both the treatment groups were low; two cases of hypokalaemia occurred with HCTZ. In conclusion, telmisartan 80 mg was well tolerated and significantly reduced SBP, DBP and LVMI after 12 months' treatment compared with HCTZ.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Verdecchia P et al. Ambulatory blood pressure. An independent predictor of prognosis in essential hypertension. Hypertension 1994; 24: 793–801.
Verdecchia P et al. Left ventricular mass and cardiovascular morbidity in essential hypertension: the MAVI study. J Am Coll Cardiol 2001; 38: 1829–1835.
Dahlöf B, Pennert K, Hansson L . Reversal of left ventricular hypertrophy in hypertensive patients. A meta-analysis of 109 treatment studies. Am J Hypertens 1992; 5: 95–101.
Hollenberg NK, Fisher ND, Price DA . Pathways for angiotensin II generation in intact human tissue: evidence from comparative pharmacological interruption of the renin system. Hypertension 1998; 32: 387–392.
Semple PF . Putative mechanisms of cough after treatment with angiotensin converting enzyme inhibitors. J Hypertens 1995; 13 (Suppl 3): S17–S21.
Unger T . The role of the renin–angiotensin system in the development of cardiovascular disease. Am J Cardiol 2002; 89 (Suppl 2A): 3A–10A.
Dahlöf B . Left ventricular hypertrophy and angiotensin II antagonists. Am J Hypertens 2001; 14: 174–182.
Okin PM et al. Regression of electrocardiographic left ventricular hypertrophy by losartan versus atenolol. The Losartan Intervention For Endpoint reduction in hypertension (LIFE) Study. Circulation 2003; 108: 684–690.
Devereux RB et al. Prognostic significance of left ventricular hypertrophy during treatment of hypertension: The LIFE Study. J Am Coll Cardiol 2003; 41 (Suppl. A): 228A [abstract 1011-135].
Maillard MP et al. In vitro and in vivo characterisation of the activity of telmisartan: an insurmountable angiotensin II receptor antagonist. J Pharmacol Exp Ther 2002; 302: 1089–1095.
Sharpe M, Jarvis B, Goa KL . Telmisartan: a review of its use in hypertension. Drugs 2001; 61: 1501–1529.
Lijnen PJ, Petrov VV, Fagard RH . Angiotensin II-induced stimulation of collagen secretion and production in cardiac fibroblasts is mediated via angiotensin II subtype 1 receptors. J Renin Angiotensin Aldosterone Syst 2001; 2: 117–122.
Böhm M et al. Reduction of cardiac hypertrophy in TGR(mREN2)27 by angiotensin II receptor blockade. Mol Cell Biochem 1996; 163/164: 217–221.
Wagner J et al. Effects of AT1 receptor blockade on blood pressure and the renin–angiotensin system in spontaneously hypertensive rats of the stroke prone strain. Clin Exp Hypertens 1998; 20: 205–221.
Wienen W, Richard S, Champeroux P, Audeval-Gerard C . Comparative antihypertensive and renoprotective effects of telmisartan and lisinopril after long-term treatment in hypertensive diabetic rats. J Renin Angiotensin Aldosterone Syst 2001; 2: 31–36.
Ivanova OV et al. Angiotensin II receptor blocker telmisartan: effect on 24-hour blood pressure profile and left ventricular hypertrophy in patients with hypertension. Kardiologiia 2002; 42: 45–49.
Martina B et al. Effects of telmisartan and losartan on left ventricular mass in mild-to-moderate hypertension. Cardiology 2003; 99: 160–170.
Papademetriou V . Effect of diuretics on cardiac arrhythmias and left ventricular hypertrophy in hypertension. Cardiology 1994; 84 (Suppl 2): 43–47.
Klingbeil AU et al. A meta-analysis of the effects of treatment of left ventricular mass in essential hypertension. Am J Med 2003; 115: 41–46.
Gopal AS et al. Freehand three-dimensional echocardiography for determination of left ventricular volume and mass in patients with abnormal ventricles: comparison with magnetic resonance imaging. J Am Soc Echocardiogr 1997; 10: 853–861.
Bachenberg TC, Shub C, Hauck AJ, Edwards WD . Can anatomical left ventricular mass be estimated reliably by M-mode echocardiography? A clinicopathological study of ninety-three patients. Echocardiography 1991; 8: 9–15.
Richtscheid M, Grimm M, Sakas G . Freehand scanning for precordial data acquisition in three-dimensional echocardiography. In: Roeslandt JRTC (ed). Three-dimensional Echocardiography of the Heart and Coronary Arteries. Van Zuiden Communications: Alphen aan den Rijn, 2000, pp 31–36.
Galzerano D et al. Reproducibility of assessment of left ventricular mass and function by a novel echocardiographic technique: freehand three-dimensional echocardiography. J Am Coll Cardiol 2002; 39: 40B [abstract].
Mannaerts HF et al. Quantification of left ventricular volumes and ejection fraction using freehand three-dimensional echocardiography: comparison with magnetic resonance imaging. J Am Soc Echocardiogr 2003; 16: 101–109.
Neutel J, Smith D . Evaluation of angiotensin II receptor blockers for 24-h blood pressure control: meta-analysis of a clinical database. J Clin Hypertens 2003; 5: 58–63.
Shimada K et al. Early morning surge in blood pressure. Blood Press Monit 2001; 6: 349–353.
Mancia G et al. Ambulatory blood pressure is superior to clinic blood pressure in predicting treatment-induced regression of left ventricular hypertrophy. Circulation 1997; 95: 1464–1470.
Devereux RB et al. Progressive hypertrophy regression with sustained pressure reduction in hypertension: the Losartan Intervention For Endpoint Reduction study. J Hypertens 2002; 20: 1445–1450.
Tedesco MA et al. Effects of losartan on hypertension and left ventricular mass: a long-term study. J Hum Hypertens 1998; 12: 505–510.
Friedrich MG et al. Rationale and design of telmisartan effectiveness on left ventricular mass reduction (TELMAR) study. J Hypertens 2003; 21 (Suppl. 4): S185 [abstract P2.226].
Galzerano D, Tuccillo B, Capogrosso P . Precordial dynamic freehand three-dimensional echocardiography:accuracy and feasiility of a new technique for assessing left ventricular volume and mass: comparison with NMR. Ital Heart J 2001; 2 (Suppl 2): C176 [abstract].
McCarron DA . Step-one antihypertensive therapy: a comparison of a centrally acting agent and a diuretic. J Cardiovasc Pharmacol 1984; 6 (Suppl 5): S853–S858.
Acknowledgements
We express our thanks to Michele A Tedesco for the review of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Galzerano, D., Tammaro, P., Cerciello, A. et al. Freehand three-dimensional echocardiographic evaluation of the effect of telmisartan compared with hydrochlorothiazide on left ventricular mass in hypertensive patients with mild-to-moderate hypertension: a multicentre study. J Hum Hypertens 18, 53–59 (2004). https://doi.org/10.1038/sj.jhh.1001637
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jhh.1001637
Keywords
This article is cited by
-
The role of renin–angiotensin–aldosterone system inhibition in the regression of hypertensive left ventricular hypertrophy: the evidence of the last three decades
Drugs & Therapy Perspectives (2020)
-
Diastolic blood pressure reduction contributes more to the regression of left ventricular hypertrophy: a meta-analysis of randomized controlled trials
Journal of Human Hypertension (2013)