Abstract
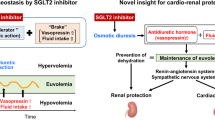
An epidemic of chronic kidney disease (CKD) in Mesoamerica is providing new insights into the mechanisms by which salt and water might drive hypertension and CKD. Increasingly, evidence suggests that recurrent dehydration and salt loss might be a mechanism that causes CKD, and experimental studies suggest a key role for increased plasma osmolarity in activating both intrarenal (polyol–fructokinase) and extrarenal (vasopressin) pathways that drive renal injury. Thus, we propose that water and salt might influence blood pressure and kidney disease through the timing and combination of their intake, which affect plasma osmolarity as well as intrarenal and extrarenal mechanisms of renal injury. The type of fluid intake might also be important, as fluids containing fructose can trigger activation of these pathways. Future studies should investigate the effects of salt, sugar and fluid intake on plasma osmolarity as a potential pathogenetic mechanism in renal injury and high blood pressure.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Torres, C. et al. Decreased kidney function of unknown cause in Nicaragua: a community-based survey. Am. J. Kidney Dis. 55, 485–496 (2010).
Weiner, D. E., McClean, M. D., Kaufman, J. S. & Brooks, D. R. The Central American epidemic of CKD. Clin. J. Am. Soc. Nephrol. 8, 504–511 (2013).
Wesseling, C. et al. Resolving the enigma of the Mesoamerican nephropathy: a research workshop summary. Am. J. Kidney Dis. 63, 396–404 (2013).
Correa-Rotter, R., Wesseling, C. & Johnson, R. J. Chronic kidney disease of unknown origin in Central America: the case for a Mesoamerican nephropathy. Am. J. Kidney Dis. 63, 506–520 (2014).
O'Donnell, J. K. et al. Prevalence of and risk factors for chronic kidney disease in rural Nicaragua. Nephrol. Dial Transplant 26, 2798–2805 (2011).
Wijkstrom, J. et al. Clinical and pathological characterization of mesoamerican nephropathy: a new kidney disease in Central America. Am. J. Kidney Dis. 62, 908–918 (2013).
Dominguez, J., Moya Perez, C. & Jansa, J. M. Análisis de Prevalencia y Determinantes de la Insuficiencia Renal Crónica en la costa del Océano Pacífico: Sur de México, Guatemala, El Salvador y Honduras [Spanish]. (Agencia Municipal de Salut Pública, 2003).
Garcia Trabiano, R. Nefropatía terminal en pacientes de un hospital de referencia en El Salvador [Spanish]. Rev. Panam. Salud Publica 12, 202–206 (2002).
Peraza, S. et al. Decreased kidney function among agricultural workers in El Salvador. Am. J. Kidney Dis. 59, 531–540 (2012).
Solis, G. in Impacto de las medidas preventivas para evitar el deterioro de la función renal por el Síndrome de Golpe por Calor en trabajadores agrícolas del Ingenio San Antonio del Occidente de Nicaragua, Ciclo Agrícola 2005–2006 [Spanish]. Thesis, Universidad Nacional Autonoma de Nicaragua (2007).
Roncal Jimenez, C. A. et al. Fructokinase activity mediates dehydration-induced renal injury. Kidney Int. http://dx.doi.org/10.1038/ki.2013.492 (2013).
Nanayakkara, S. et al. Tubulointerstitial damage as the major pathological lesion in endemic chronic kidney disease among farmers in North Central Province of Sri Lanka. Environ. Health Prev. Med. 17, 213–221 (2012).
Schrier, R. W., Henderson, H. S., Tisher, C. C. & Tannen, R. L. Nephropathy associated with heat stress and exercise. Ann. Intern. Med. 67, 356–376 (1967).
Crowe, J. et al. Heat exposure in sugarcane harvesters in Costa Rica. Am. J. Ind. Med. 56, 1157–1164 (2013).
Bankir, L., Bouby, N. & Ritz, E. Vasopressin: a novel target for the prevention and retardation of kidney disease? Nat. Rev. Nephrol 9, 223–239 (2013).
Bankir, L., Bichet, D. G. & Bouby, N. Vasopressin V2 receptors, ENaC, and sodium reabsorption: a risk factor for hypertension? Am. J. Physiol. Renal Physiol. 299, F917–F928 (2010).
Bardoux, P. et al. Vasopressin increases urinary albumin excretion in rats and humans: involvement of V2 receptors and the renin-angiotensin system. Nephrol. Dial. Transplant. 18, 497–506 (2003).
Bardoux, P. et al. Vasopressin contributes to hyperfiltration, albuminuria, and renal hypertrophy in diabetes mellitus: study in vasopressin-deficient Brattleboro rats. Proc. Natl Acad. Sci. USA 96, 10397–10402 (1999).
Burg, M. B. Molecular basis of osmotic regulation. Am. J. Physiol. 268, F983–F996 (1995).
Schmolke, M., Schilling, A., Keiditsch, E. & Guder, W. G. Intrarenal distribution of organic osmolytes in human kidney. Eur. J. Clin. Chem. Clin. Biochem. 34, 499–501 (1996).
Bouby, N., Bachmann, S., Bichet, D. & Bankir, L. Effect of water intake on the progression of chronic renal failure in the 5/6 nephrectomized rat. Am. J. Physiol. 258, F973–F979 (1990).
Bardoux, P., Bruneval, P., Heudes, D., Bouby, N. & Bankir, L. Diabetes-induced albuminuria: role of antidiuretic hormone as revealed by chronic V2 receptor antagonism in rats. Nephrol. Dial. Transplant. 18, 1755–1763 (2003).
Bouby, N. et al. Vasopressin increases glomerular filtration rate in conscious rats through its antidiuretic action. J. Am. Soc. Nephrol. 7, 842–851 (1996).
Schrier, R. W., Harris, D. C., Chan, L., Shapiro, J. I. & Caramelo, C. Tubular hypermetabolism as a factor in the progression of chronic renal failure. Am. J. Kidney Dis. 12, 243–249 (1988).
Lehninger, A. L. & Neubert, D. Effect of oxytocin, vasopressin, and other disulfide hormones on uptake and extrusion of water by mitochondria. Proc. Natl Acad. Sci. USA 47, 1929–1936 (1961).
Assimacopoulos-Jeannet, F., McCormack, J. G. & Jeanrenaud, B. Vasopressin and/or glucagon rapidly increases mitochondrial calcium and oxidative enzyme activities in the perfused rat liver. J. Biol. Chem. 261, 8799–8804 (1986).
Bolignano, D. & Zoccali, C. Vasopressin beyond water: implications for renal diseases. Curr. Opin. Nephrol. Hypertens. 19, 499–504 (2010).
Burger-Kentischer, A. et al. Hypertonicity-induced accumulation of organic osmolytes in papillary interstitial cells. Kidney Int. 55, 1417–1425 (1999).
Diggle, C. P. et al. Both isoforms of ketohexokinase are dispensable for normal growth and development. Physiol. Genomics 42A, 235–243 (2010).
Cirillo, P. et al. Ketohexokinase-dependent metabolism of fructose induces proinflammatory mediators in proximal tubular cells. J. Am. Soc. Nephrol. 20, 545–553 (2009).
Ishimoto, T. et al. Opposing effects of fructokinase C and A isoforms on fructose-induced metabolic syndrome in mice. Proc. Natl Acad. Sci. USA 109, 4320–4325 (2012).
Bergheim, I. et al. Antibiotics protect against fructose-induced hepatic lipid accumulation in mice: role of endotoxin. J. Hepatol. 48, 983–992 (2008).
Johnson, R. J. et al. Fructokinase, fructans, intestinal permeability, and metabolic syndrome: an equine connection? J. Equine Vet. Sci. 33, 120–126 (2013).
Ishimoto, T. et al. High fat and high sucrose (western) diet induce steatohepatitis that is dependent on fructokinase. Hepatology 58, 1632–1643 (2013).
Diggle, C. P. et al. Ketohexokinase: expression and localization of the principal fructose-metabolizing enzyme. J. Histochem. Cytochem. 57, 763–774 (2009).
Nakayama, T. et al. Dietary fructose causes tubulointerstitial injury in the normal rat kidney. Am. J. Physiol. Renal Physiol. 298, F712–F720 (2010).
Johner, S. A. et al. Urinary fructose: a potential biomarker for dietary fructose intake in children. Eur. J. Clin. Nutr. 64, 1365–1370 (2010).
Luceri, C. et al. Urinary excretion of sucrose and fructose as a predictor of sucrose intake in dietary intervention studies. Cancer Epidemiol. Biomarkers Prev. 5, 167–171 (1996).
Aoyama, M. et al. Fructose induces tubulointerstitial injury in the kidney of mice. Biochem. Biophys. Res. Commun. 419, 244–249 (2012).
Gersch, M. S. et al. Fructose, but not dextrose, accelerates the progression of chronic kidney disease. Am. J. Physiol. Renal Physiol. 293, F1256–F1261 (2007).
Ko, B. C., Ruepp, B., Bohren, K. M., Gabbay, K. H. & Chung, S. S. Identification and characterization of multiple osmotic response sequences in the human aldose reductase gene. J. Biol. Chem. 272, 16431–16437 (1997).
Lanaspa, M. A. et al. Endogenous fructose production and fructokinase activation mediate renal injury in diabetic nephropathy. J. Am. Soc. Nephrol. (in press).
de Wardener, H. E., He, F. J. & MacGregor, G. A. Plasma sodium and hypertension. Kidney Int. 66, 2454–2466 (2004).
Imig, J. D. & Ryan, M. J. Immune and inflammatory role in renal disease. Compr. Physiol. 3, 957–976 (2013).
Shapiro, L. & Dinarello, C. A. Osmotic regulation of cytokine synthesis in vitro. Proc. Natl Acad. Sci. USA 92, 12230–12234 (1995).
Shapiro, L. & Dinarello, C. A. Hyperosmotic stress as a stimulant for proinflammatory cytokine production. Exp. Cell Res. 231, 354–362 (1997).
Ying, W. Z. & Sanders, P. W. Dietary salt modulates renal production of transforming growth factor-β in rats. Am. J. Physiol. 274, F635–F641 (1998).
Gu, J. W. et al. Sodium induces hypertrophy of cultured myocardial myoblasts and vascular smooth muscle cells. Hypertension 31, 1083–1087 (1998).
Toney, G. M. & Stocker, S. D. Hyperosmotic activation of CNS sympathetic drive: implications for cardiovascular disease. J. Physiol. 588, 3375–3384 (2010).
Mathai, M. L., Evered, M. D. & McKinley, M. J. Central losartan blocks natriuretic, vasopressin, and pressor responses to central hypertonic NaCl in sheep. Am. J. Physiol. 275, R548–R554 (1998).
O'Donaughy, T. L. & Brooks, V. L. Deoxycorticosterone acetate-salt rats: hypertension and sympathoexcitation driven by increased NaCl levels. Hypertension 47, 680–685 (2006).
Friedman, S. M., McIndoe, R. A. & Tanaka, M. The relation of blood sodium concentration to blood pressure in the rat. J. Hypertens. 8, 61–66 (1990).
Suckling, R. J., He, F. J., Markandu, N. D. & MacGregor, G. A. Dietary salt influences postprandial plasma sodium concentration and systolic blood pressure. Kidney Int. 81, 407–411 (2012).
Dickinson, K. M., Clifton, P. M., Burrell, L. M., Barrett, P. H. & Keogh, J. B. Postprandial effects of a high salt meal on serum sodium, arterial stiffness, markers of nitric oxide production and markers of endothelial function. Atherosclerosis 232, 211–216 (2014).
Wenner, M. M., Rose, W. C., Delaney, E. P., Stillabower, M. E. & Farquhar, W. B. Influence of plasma osmolality on baroreflex control of sympathetic activity. Am. J. Physiol. Heart Circ. Physiol. 293, H2313–H2319 (2007).
Charkoudian, N., Eisenach, J. H., Joyner, M. J., Roberts, S. K. & Wick, D. E. Interactions of plasma osmolality with arterial and central venous pressures in control of sympathetic activity and heart rate in humans. Am. J. Physiol. Heart Circ. Physiol. 289, H2456–H2460 (2005).
Kopp, C. et al. 23Na magnetic resonance imaging of tissue sodium. Hypertension 59, 167–172 (2012).
Beduschi, G. C., Telini, L. S., Caramori, J. C., Martin, L. C. & Barretti, P. Effect of dialysate sodium reduction on body water volume, blood pressure, and inflammatory markers in hemodialysis patients—a prospective randomized controlled study. Ren. Fail. 35, 742–747 (2013).
Bourque, C. W. Central mechanisms of osmosensation and systemic osmoregulation. Nature Rev. Neurosci. 9, 519–531 (2008).
Lechner, S. G. et al. The molecular and cellular identity of peripheral osmoreceptors. Neuron 69, 332–344 (2011).
McMahon, E. J. et al. A randomized trial of dietary sodium restriction in CKD. J. Am. Soc. Nephrol. 24, 2096–2103 (2013).
Krikken, J. A., Laverman, G. D. & Navis, G. Benefits of dietary sodium restriction in the management of chronic kidney disease. Curr. Opin. Nephrol. Hypertens. 18, 531–538 (2009).
Lambers Heerspink, H. J., Navis, G. & Ritz, E. Salt intake in kidney disease- a missed therapeutic opportunity? Nephrol. Dial. Transplant. 27, 3435–3442 (2012).
Aaron, K. J. & Sanders, P. W. Role of dietary salt and potassium intake in cardiovascular health and disease: a review of the evidence. Mayo Clin. Proc. 88, 987–995 (2013).
Jones-Burton, C. et al. An in-depth review of the evidence linking dietary salt intake and progression of chronic kidney disease. Am. J. Nephrol. 26, 268–275 (2006).
Cook, N. R. et al. Long term effects of dietary sodium reduction on cardiovascular disease outcomes: observational follow-up of the trials of hypertension prevention (TOHP). BMJ 334, 885–894 (2007).
Vegter, S. et al. Sodium intake, ACE inhibition, and progression to ESRD. J. Am. Soc. Nephrol. 23, 165–173 (2012).
Alderman, M. H., Madhavan, S., Cohen, H., Sealey, J. E. & Laragh, J. H. Low urinary sodium is associated with greater risk of myocardial infarction among treated hypertensive men. Hypertension 25, 1144–1152 (1995).
Ekinci, E. I. et al. Dietary salt intake and mortality in patients with type 2 diabetes. Diabetes Care 34, 703–709 (2011).
Thomas, M. C. et al. The association between dietary sodium intake, ESRD, and all-cause mortality in patients with type 1 diabetes. Diabetes Care 34, 861–866 (2011).
Clark, W. F. et al. Urine volume and change in estimated GFR in a community-based cohort study. Clin. J. Am. Soc. Nephrol. 6, 2634–2641 (2011).
Strippoli, G. F. et al. Fluid and nutrient intake and risk of chronic kidney disease. Nephrology 16, 326–334 (2011).
Sontrop, J. M. et al. Association between water intake, chronic kidney disease, and cardiovascular disease: a cross-sectional analysis of NHANES data. Am. J. Nephrol. 37, 434–442 (2013).
Palmer, S. C. et al. Fluid intake and all-cause mortality, cardiovascular mortality, and kidney function: a population-based longitudinal cohort study. Nephrol. Dial Transplant http://dx.doi.org/10.1093/ndt/gft507 (2014).
Hebert, L. A., Greene, T., Levey, A., Falkenhain, M. E. & Klahr, S. High urine volume and low urine osmolality are risk factors for faster progression of renal disease. Am. J. Kidney Dis. 41, 962–971 (2003).
McMahon, E. J., Campbell, K. L., Mudge, D. W. & Bauer, J. D. Achieving salt restriction in chronic kidney disease. Int. J. Nephrol. 2012, 720429 (2012).
Choukroun, G., Schmitt, F., Martinez, F., Drueke, T. B. & Bankir, L. Low urine flow reduces the capacity to excrete a sodium load in humans. Am. J. Physiol. 273, R1726–R1733 (1997).
Perucca, J., Bouby, N., Valeix, P. & Bankir, L. Sex difference in urine concentration across differing ages, sodium intake, and level of kidney disease. Am. J. Physiol. Regul. Integr. Comp. Physiol. 292, R700–R705 (2007).
Zerbe, R. L. & Robertson, G. L. Osmoregulation of thirst and vasopressin secretion in human subjects: effect of various solutes. Am. J. Physiol. 244, E607–E614 (1983).
Wolf, J. P., Nguyen, N. U., Dumoulin, G. & Berthelay, S. Influence of hypertonic monosaccharide infusions on the release of plasma arginine vasopressin in normal humans. Horm. Metab. Res. 24, 379–383 (1992).
Shafiee, M. A. et al. Defining conditions that lead to the retention of water: the importance of the arterial sodium concentration. Kidney Int. 67, 613–621 (2005).
Robertson, G. L. Abnormalities of thirst regulation. Kidney Int. 25, 460–469 (1984).
Zerbe, R. L., Miller, J. Z. & Robertson, G. L. The reproducibility and heritability of individual differences in osmoregulatory function in normal human subjects. J. Lab. Clin. Med. 117, 51–59 (1991).
Acknowledgements
R.J.J.'s research work is funded by the University of Colorado, Denver, CO, USA, and NIH grant funding. L.G.S.-L.'s work is funded by CONACyT Mexico (No. 133232).
Author information
Authors and Affiliations
Contributions
R.J.J., L.B. and L.G.S.-L. researched the data for the article. All authors contributed to the discussion of the article's content, after which R.J.J., B.R.-I., L.B. and L.G.S.-L. wrote the manuscript. R.J.J., B.R.-I., T.I., T.N., R.C.-R., C.W., L.B. and L.G.S.-L. edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
R.J.J. and M.A.L. are inventors on patent applications related to blocking fructokinase in the treatment of kidney disease and metabolic syndrome from the University of Colorado (US2013/0195886 and US2013/0224218). R.J.J. is on the Scientific Advisory Board of Amway, the Scientific Board of XORT Therapeutics and of Rivermend Health. R.J.J. has also received research funding from Danone Research and Amway. R.J.J., C.R. J., M.A.L. and L.G.S. L. are members of Colorado Research Partners. The other authors declare no competing interests.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Johnson, R., Rodriguez-Iturbe, B., Roncal-Jimenez, C. et al. Hyperosmolarity drives hypertension and CKD—water and salt revisited. Nat Rev Nephrol 10, 415–420 (2014). https://doi.org/10.1038/nrneph.2014.76
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneph.2014.76
This article is cited by
-
A study on the early metabolic effects of salt and fructose consumption: the protective role of water
Hypertension Research (2024)
-
Pharmacokinetic Evaluation of Intravenous Vitamin C: A Classic Pharmacokinetic Study
Clinical Pharmacokinetics (2022)
-
Recent advances in the pathogenesis of hereditary fructose intolerance: implications for its treatment and the understanding of fructose-induced non-alcoholic fatty liver disease
Cellular and Molecular Life Sciences (2020)
-
Serum osmolarity as a potential predictor for contrast-induced nephropathy following elective coronary angiography
International Urology and Nephrology (2020)
-
Estimated plasma osmolarity and risk of end-stage kidney disease in patients with IgA nephropathy
Clinical and Experimental Nephrology (2020)