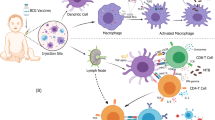
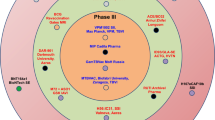
Abstract
Over the past 50 years, the Mycobacterium bovis bacille Calmette–Guérin (BCG) vaccine against tuberculosis (TB) has maintained its position as the world's most widely used vaccine, despite showing highly variable efficacy (0–80%) in different trials. The efficacy of BCG in adults is particularly poor in tropical and subtropical regions. Studies in animal models of TB, supported by data from clinical BCG trials in humans, indicate that this failure is related to pre-existing immune responses to antigens that are common to environmental mycobacteria and Mycobacterium tuberculosis. Here, we discuss the potential mechanisms behind the variation of BCG efficacy and their implications for an improved TB vaccination strategy.
Similar content being viewed by others
Main
Tuberculosis is one of the leading causes of mortality from an infectious disease worldwide and current estimates indicate that more than 2 million people die from this disease each year1. Mycobacterium bovis bacille Calmette–Guérin (BCG) is the only vaccine currently available against TB. BCG is an attenuated strain of M. bovis that was derived from a virulent strain at the start of the last century, after more than 13 years of continuous in vitro passage. The first clinical studies took place from 1921 to 1927 in France and Belgium, and showed that BCG was highly efficient in protecting against TB in children2. In France, BCG was soon thereafter introduced as an oral vaccine administered in milk, but further dissemination of the vaccine was stopped in 1930 as a consequence of the Lubeck disaster, in which 67 of 249 babies given the vaccine died owing to inadvertent contamination of the vaccine with virulent Mycobacterium tuberculosis 3. Throughout the 1930s, Scandinavian countries pioneered the use of BCG administered by the intradermal route and provided the necessary proof of its safety for mass vaccination4. After the Second World War, the vaccine was offered to children throughout Europe. In the early 1950s, the WHO recommended that the vaccination campaigns be expanded to cover TB-endemic areas outside Europe.
Initially, the vaccine was restricted to tuberculin-negative children, as it was not expected to have a positive effect (and initially was feared to have a negative effect) in individuals already infected with M. tuberculosis. Prior immune reactivity to mycobacteria was therefore tested for, before vaccination, by injecting a sterile extract of M. tuberculosis proteins (tuberculin) just under the skin. A delayed-type hypersensitivity response (DTH), detectable as swelling and reddening at the site of injection after 24–48 hours, indicated mycobacterial sensitization — often assumed to be due to infection with M. tuberculosis, although the test is not very specific. Later studies coordinated by the WHO indicated that it was safe to give BCG to those who had already skin-test converted. This opened the door to mass vaccination even in TB-endemic areas, and in many of the subsequent vaccination campaigns no prior skin test was conducted5, which substantially decreased the workload involved. Subsequently, vaccine coverage has been maintained by immunizing newborn children and/or schoolchildren as part of routine health-care systems.
To meet the growing worldwide demand for the vaccine, the initial strain was distributed to a large number of local producers both from the original source at the Institut Pasteur and from BCG reference centres in Europe, such as the Statens Serum Institute in Copenhagen. As this dissemination and local production took place before the introduction of standardized seed lots, many local BCG strains were established with subtle — or in some cases dramatic — differences in genetic and antigenic composition6,7.
The WHO recommends that infants should be immunized as soon after birth as possible with a single intradermal dose of BCG in all countries with a high risk of TB infection. However, the existence of different strains of BCG and the different immunization policies that were put into place decades before the existence of global recommendations have complicated the task of assessing vaccine efficacy. Today, >3 billion people have received BCG, which makes it the most widely used vaccine worldwide. However, although the vaccine is well established, discussion of its benefits and drawbacks has never ceased and includes safety aspects, loss of sensitivity to tuberculin as a diagnostic reagent and, in particular, the fact that although it is credited with helping to end the TB epidemic in Europe, the efficacy of this vaccine has generally been disappointing in trials conducted in the developing world8.
Although a consensus is developing that BCG protects children efficiently against the early manifestations of TB9,10,11,12,13, estimates of protection against adult pulmonary TB range from 0–80% based on large, well-controlled field trials. The global impact of this variation is accentuated by the fact that, in general, the lowest levels of protection have been found in countries with the highest incidence of TB14. This indicates that, globally, BCG prevents only ∼5% of all potentially vaccine-preventable deaths due to TB1. At present, TB affects not only the developing world, where co-infection with HIV has dramatically increased its incidence15, but the incidence is also increasing in parts of Europe. In some countries (for example, Russia and other members of the former Soviet Union), the threat to public health and the consequent social problems associated with TB require urgent action. A novel, effective vaccination strategy against adult pulmonary TB has therefore become an international research priority.
Novel TB vaccines
The leading TB vaccine candidates fall into two broad categories: live mycobacterial vaccines and subunit vaccines (Table 1). Live mycobacterial vaccines are developed either by attenuating M. tuberculosis or by genetically modifying BCG. The main rationale for the development of genetically augmented BCG is the hypothesis that BCG has been weakened by continuing attenuation and gene loss16. Adding deleted genes back to BCG or increasing the expression of immunodominant genes might improve the effects of BCG vaccination, as suggested by studies in animal models17,18. A recombinant BCG strain that overexpresses Ag85B from M. tuberculosis is one example of this strategy that is currently in clinical trials.
Another approach has been to optimize antigen export from BCG, in the hope of increasing the immune response. The rBCG::ΔureC-llo+ vaccine strain is a urease-deficient mutant that is unable to arrest phagosome maturation and expresses the lysteriolysin O gene from Listeria monocytogenes , which is thought to damage the phagosome membrane, potentially increasing the amount of bacterial-derived antigen available for presentation to CD8 T cells through the cytosolic scavenger pathways19,20. The rBCG::ΔureC-llo+ vaccine is tentatively expected to enter clinical testing in 2005/2006 (S.H.E. Kaufmann, personal communication).
The development of subunit vaccines has benefited tremendously from the sequencing of the M. tuberculosis genome21, and the accelerated identification of novel antigens has led to the identification of defined antigens that are protective in animal models. In addition to the antigens selected, any subunit vaccine depends on additional factors to stimulate a cell-mediated immune (CMI) response. Many live vectors, such as recombinant vaccinia or adenovirus vectors, generate strong CMI responses themselves and therefore need no adjuvant. Vaccines based on both of these viruses have induced short-term protection in animal models comparable to that obtained with BCG22,23, and a vaccinia-based vaccine has already entered human trials24 (Table 1). The two leading recombinant vaccine antigens are similar in their design philosophy and are both fusion molecules consisting of selected immunodominant antigens with proven vaccine efficacy. The Mtb72f vaccine is a fusion molecule comprising two proteins, with the PPE family member Rv1196 inserted into the middle of the putative serine protease Rv0125 (Ref. 25). The second vaccine is also a fusion molecule composed of two immunodominant, secreted proteins from M. tuberculosis (ESAT-6 and Ag85B). Both have proven safe and efficacious in various animal models, including non-human primates26,27,28.
The success of these subunit vaccines is underpinned by advances in adjuvant development. Until recently, the only adjuvants appropriate for use in a TB vaccine were either ineffective at stimulating CMI responses or too toxic for human use. This situation is now being remedied by the arrival of new adjuvants, such as the IC31 adjuvant from Intercell and the AS2 adjuvant developed by GlaxoSmithKline, both with proven efficacy and safety in animal models25,29 (Table 1). Other adjuvants, which combine liposomes and immunostimulants, are under development30,31.
BCG: replace or repair?
The main burden of TB, in terms of both morbidity and mortality, is associated with adult pulmonary disease, which is also the main source of new infections. As mentioned above, neonatal vaccination with BCG seems to consistently provide protection against the most severe childhood manifestations of the disease, such as TB meningitis, regardless of the setting. However, as with most other vaccines, the protection given by BCG vaccination is not life-long. Although still the subject of debate32, most studies have reported that BCG is protective for only 10–20 years9,33,34. The time-frame for waning of BCG-induced protection through childhood and young adult life coincides with the gradual increase in TB incidence, which in some highly TB-endemic regions, such as sub-Saharan Africa, reaches a peak of >500 cases per 100,000 individuals in the 25–35-year-old age group1. In hyper-endemic regions, such as crowded shanty towns and urban slums, the incidence in this age group can be at least double the national average. Therefore, it would seem that the primary reason for the ineffectiveness of the BCG vaccine against adult pulmonary TB is that vaccination in childhood only provides protection for a limited period of time. The most efficient global TB control might therefore not be achieved through the development of a better vaccine to replace BCG for neonatal vaccination (Fig. 1a), but by the development of a booster vaccine to 'repair' failing BCG-induced immunity and prevent it from falling below the point at which it is effective (Fig. 1b), or a combination of the two strategies.
Hypothetical curve showing waning of Mycobacterium bovis bacille Calmette–Guérin (BCG)-induced immune responses (solid green line) and the proposed action of improved priming (a) and boosting (b) vaccines (red dashed line). When immunity drops under an arbitrary threshold for immunological protection against tuberculosis (TB) (black line), immune surveillance will fail to protect against the resurgence of TB. Improved priming vaccines aim to keep the immune response above this threshold for longer, whereas intervention in the form of a booster vaccine is hypothesized to restore immunity to levels above the threshold.
As BCG confers reliable protection against disseminated disease in childhood, it might be considered unethical to test and deploy a vaccine strategy that does not include BCG. The BCG booster strategy has attracted a lot of recent interest from researchers35,36,37,38, and the first booster vaccine based on MVA-Ag85A (Table 1) recently proved strongly immunogenic (boosting immune responses over that obtained with BCG alone) and was relatively well-tolerated in Phase 1 clinical trials24. Importantly, if the aim is to boost immunity in BCG-vaccinated adults or adolescents, we must understand why most BCG vaccination campaigns in tropical regions have failed in this age group.
Environmental mycobacteria
In sharp contrast to its varying efficacy in human trials, BCG consistently provides efficient protection in animal models of TB39. In fact, many of the experimental TB vaccines developed and tested in recent years have had difficulty surpassing the efficacy of BCG in animal models26,40,41,42. The reason for the failure of BCG in some human clinical trials has been a subject of debate since the 1950s and although many different explanations have been proposed13,43,44, today, the two prevailing hypotheses centre on the close relationship of species within the genus Mycobacterium. The mycobacteria, to which both M. bovis and M. tuberculosis belong, comprise many closely related species, of which most are non-pathogenic soil saprophytes. Although environmental mycobacteria represent markedly different microbial lifestyles from the intracellular pathogens M. tuberculosis and M. bovis, they have several features in common, such as a lipid-rich outer cell wall, genomes with a high GC content and many similar gene families21,45,46. At the antigen level, many mycobacterial species are also cross-reactive47,48,49,50, with some of the major immunodominant antigens (such as the Ag85 complex) being highly conserved. This is the reason why BCG, although derived from M. bovis and not M. tuberculosis, provides efficient protection against the latter in animal models as well as in some human trials. The same 'family resemblance' also underlies the efficient protection provided by Mycobacterium microti (the so-called vole bacillus) in both human clinical trials and animal models51. However, for BCG vaccination, the close relationship between many mycobacterial species has turned out to be a double-edged sword.
A wide range of mycobacterial species (often referred to as environmental mycobacteria) are found in soil and water52,53. Most are non-pathogenic, although marginally invasive strains such as Mycobacterium avium and Mycobacterium kansasii, which can give rise to disease in immunosuppressed individuals, are also found. It is known that repeated exposure to these environmental mycobacteria can sensitize individuals and stimulate CMI responses that can be measured both in vitro54,55 and in the skin test56,57,58. The high levels of responsiveness to antigens derived from these species that are observed in many individuals from tropical regions indicate that they have a high level of prior exposure to these mycobacteria54,56,57, although it is unclear whether this is owing to higher exposure (for example, through untreated water) or whether it reflects a difference in the microbial fauna of these regions. Whatever the cause, responsiveness to antigens from non-pathogenic mycobacteria is generally lower in populations from developed settings at higher latitudes.
That prior sensitization to environmental mycobacteria affects the efficacy of human BCG vaccination in some areas is suggested by several classical epidemiological observations. First, BCG is efficacious in trials from which tuberculin-skin-test-positive (and therefore sensitized) donors have been rigorously excluded33. As a note of caution, the cut-off used in the UK trial (5 mm) to identify negative recipients is completely different from the criteria generally used in the tropics where, owing to the higher level of general sensitization in the population, a cut-off of 10–15 mm is used to exclude donors with active disease before vaccination8. This difference makes the direct comparison between trials conducted in these two regions difficult. Second, BCG vaccination of neonates before there has been significant sensitization from environmental mycobacteria shows consistent success against paediatric forms of TB33,59,60. The importance of this observation cannot be overemphasized. If vaccine efficacy in BCG trials targeting different populations is compared, BCG consistently does well in neonates, whereas the BCG 'failures' are found in trials that target adults from tropical regions with many years of potential exposure to mycobacteria from the environment61. Another factor important for the mycobacterial sensitization of the adult population in high incidence areas is that, owing to the chronic nature of TB, the incidence of active TB is only the tip of the iceberg and covers a large reservoir of latent, subclinical TB in the population. This pool of latent TB is also a considerable source of mycobacterial sensitization and might, in some of the most affected areas, be an even larger single source of sensitization than environmental mycobacteria.
BCG failure — hypotheses
The hypothesis that prior sensitization to mycobacteria can have a deleterious effect on the efficacy of BCG vaccination has given rise to two different interpretations of the possible role of the pre-existing CMI response to mycobacterial antigens and its interaction with BCG.
The masking hypothesis. The masking hypothesis suggests that exposure to environmental mycobacteria offers some level of protective immunity to TB and that any additional protective effect of a subsequent BCG vaccine superimposed on this baseline anti-mycobacterial immune response is limited. This hypothesis was suggested by Palmer and colleagues, based on large-scale experiments in guinea pigs, in which immunization with environmental mycobacteria induced appreciable levels of protective immunity to M. tuberculosis challenge and the effects of a subsequent BCG vaccine were markedly reduced62. In one such study, immunization with strains of M. avium isolated from soil or humans from the Chingleput area of India gave anywhere from 24% to 91% of the maximum protection provided by BCG53, thereby leaving a limited — and highly variable — window for an improved immune response by adding BCG (Fig. 2). Given the close relationship between many mycobacteria, these findings seem logical. If BCG vaccination (under optimal conditions) can protect against infections caused by the related mycobacterial pathogen M. tuberculosis and even the distantly related pathogen Mycobacterium leprae 63,64, then the possibility that other mycobacteria can generate some level of cross-reactive protection must be considered. Incidentally, these data explain why BCG has been consistently efficacious in animal models, as the animals used are normally protected from exposure to other mycobacteria and are immunologically naive, like human neonates. One of the confusing interpretations of this hypothesis is that it intuitively suggests that areas with high levels of mycobacterial sensitization should have a lower incidence of TB. This is obviously not the case (as exemplified by the high incidence of disease in many tropical regions). However, although impossible to investigate, the devastating consequences of the introduction of TB into the northern Inuit populations a century ago65 might indicate that populations in the tropics would have been even worse off without their natural immunizations from the environment.
The dotted line shows the level of immunity to tuberculosis (TB) generated by Mycobacterium bovis bacille Calmette–Guérin (BCG). In the blocking hypothesis, the level of protection provided by environmental mycobacteria need not be high — by interfering with the replication of BCG, it reduces the efficacy of BCG in sensitized individuals. To show efficacy, therefore, a new vaccine need only be as good as BCG to have a measurable effect — as long as it is not also blocked by presensitization (for example, a vaccine based on a non-mycobacterial vector, such as a virus, recombinant protein or naked DNA). By contrast, the masking hypothesis posits that the protective effect of sensitizing mycobacteria is nearly as good as that of BCG, so improvement by adding BCG is minimal. In this case, a novel vaccine would have to be significantly better than BCG to have any measurable effect.
The blocking hypothesis. The blocking hypothesis suggests that pre-existing immune responses to antigens common for the mycobacteria block the replication of BCG and therefore vaccine 'take'. This hypothesis was suggested by P.A. and colleagues, based on studies of BCG vaccine replication and TB protection in a model of environmental sensitization66. In the mouse model of aerosol infection with M. tuberculosis, it was shown that prior exposure to atypical mycobacterial species (notably M. avium) results in an immune response that is recalled rapidly after BCG vaccination, and which controls the replication of the vaccine strain, thereby abrogating vaccine take and the induction of immunity to subsequent M. tuberculosis infection. As a live vaccine, replication of BCG in vaccine recipients is a precondition for the induction and maintenance of protective immunity67,68. According to the blocking hypothesis, prior sensitization to non-tuberculous mycobacteria blocks BCG dissemination by inducing an immune response to antigens that are cross-reactive with BCG antigens69. Other recent studies have also presented a case for the detrimental influence of prior sensitization on the activity of BCG70,71,72. In agreement with the findings in the mouse model, cattle with prior PPD (purified protein derivative) reactivity to sensitins from atypical mycobacteria showed no BCG-induced protection and in this study, sensitization to M. avium was acquired from exposure to the environment, therefore reflecting the proposed situation in humans70.
An important aspect of the blocking hypothesis is the understanding that the partial immunity induced by environmental mycobacteria has only a minimal influence on the more virulent M. tuberculosis66 (Fig. 2). These findings differ from the masking hypothesis, according to which sensitization would also be expected to provide significant levels of protection against virulent challenge. Of relevance in this regard is the observation that an experimental vaccine strain based on M. bovis, attenuated by mutagenesis but still more virulent than BCG, offered some protection in sensitized animals70. Similarly, Demangel and colleagues recently showed in animal models that recombinant BCG vaccine expressing RD1 antigens (more virulent than BCG) overrides immunity imparted by prior contact with environmental mycobacteria72. This suggests that the heterologous immunity induced by atypical mycobacteria is sufficient to inhibit the growth of the attenuated BCG but not of more-virulent strains. This might explain both why sensitization can decrease the effectiveness of BCG vaccination but not infection with the more virulent M. tuberculosis, and why BCG vaccination can protect against the less virulent pathogen M. leprae, even in areas where its effect on M. tuberculosis is not significant63.
Evidence from human clinical trials
The consistent efficacy of BCG in neonates and non-sensitized individuals clearly indicates an interaction between sensitization and BCG efficacy, but does not distinguish between the two hypotheses presented above, as both masking and blocking will give the same net outcome, namely a lack of detectable BCG efficacy in sensitized individuals. The two hypotheses are not mutually exclusive, and in reality both mechanisms probably have a role to play. However, there are several lines of evidence from human clinical trials that seems to favour blocking as the main mechanism responsible for BCG failure.
The first of these is the observation of a lower rate of skin-test conversion and smaller average DTH reaction following BCG vaccination (in this context interpreted as reduced BCG vaccine take) in areas with high levels of sensitization to atypical or environmental mycobacteria compared with areas where there is minimal evidence of environmental exposure73,74,75,76. However, it is important to note that this reflects a difference not so much in the maximal DTH size in tropical versus temperate regions, but an accelerated waning of DTH responses after BCG vaccination in tropical areas. In a recently published large study from Malawi, BCG-induced DTH peaked 2–3 months after vaccination, at which time-point most vaccinated individuals had a substantial DTH response that was not significantly different from skin-test conversion in areas such as the UK or Denmark57. The DTH responses in Malawians, however, waned rapidly and were close to pre-vaccination levels after 2.5 years, whereas most individuals in temperate regions maintain tuberculin hypersensitivity for several years without waning57,58,77. This accelerated waning was also found in the large southern India BCG vaccine trial74. A simple interpretation of the different kinetics of the emergence and waning of the skin-test response in temperate and tropical regions is that BCG-induced responses in the tropics are transient, secondary responses; that is, responses recalled from prior BCG vaccination, sensitization to environmental mycobacteria or latent M. tuberculosis infection. This matches the transient T-cell responses induced by BCG in animals sensitized with environmental mycobacteria66. Therefore, analogous to observations in animal models, these BCG-vaccinated individuals have a limited net increase of the immune response and no improved immunity to TB. In agreement with this hypothesis, another recent publication from the Karonga Prevention Study group convincingly showed impaired interferon-γ responses one year post-BCG in sensitized Malawians compared with non-sensitized children from the UK55.
Implications for a novel TB vaccine
As long as a novel TB vaccine is intended to be given to neonates as a replacement for BCG, it should theoretically avoid any negative effects owing to pre-existing immunity from environmental mycobacteria. In particular, live mycobacterial vaccines, such as the genetically modified BCGs discussed above, might prime the immune system more efficiently than BCG, thereby generating improved and more sustained immunity against TB (Fig. 1a). By contrast, a vaccine to boost BCG-induced immunity in adults in tropical regions would be administered to individuals that have repeatedly encountered mycobacterial antigens over the previous 10–20 years, and it is therefore relevant to discuss the implications of the two hypotheses for the design and prospects of a novel BCG booster vaccination strategy.
The masking hypothesis leaves limited room for optimism, as it stipulates that, because environmental sensitization is almost as efficient as BCG in preventing TB, for any booster vaccine to have an effect in sensitized individuals it needs a higher absolute efficacy than that of BCG. Only such a hypothetical 'hyper-effective' vaccine would allow the detection of improvement compared to the protection provided by conventional BCG in sensitized individuals (Fig. 2). It is possible that the high transmission rate in many highly TB-endemic regions might be sufficient to overwhelm levels of immunity that would have been sufficient in regions with a lower transmission rate78. Certainly, such an effect can be modelled in animals79. This would mean that we need a radically different vaccine strategy in these regions, as even the most effective of the new vaccines tested so far26,80 do not have such marked superiority compared with BCG. It should be noted in this regard that not even a fully cured prior TB infection seems to give complete protection against re-infection81, and it might therefore be unrealistic to expect any vaccine to do so.
The blocking hypothesis, on the other hand, stipulates that the most important characteristic of a booster vaccine is its ability to function in an individual with pre-existing immune responses against mycobacterial antigens, and that there is room for improving immunity in these individuals (Fig. 2). An important corollary is that live mycobacterial strains, whether recombinant BCG or attenuated M. tuberculosis, probably suffer from the same defect as BCG — they would be inhibited in sensitized adults. Subunit vaccines based on either viral or adjuvant delivery systems, on the other hand, might have potential as booster vaccines, even though their efficacy in non-sensitized individuals might be no better than BCG. Ironically, the viral delivery systems that have proven so useful for prime-boost strategies might in this context suffer from the limitation that a large proportion of the global population might have pre-existing antibodies (for example, from the smallpox vaccination campaign) that can block their activity.
Conclusions and future perspectives
Boosting BCG immunity in adults is one of the most important conceptual advances in the TB vaccine field. However, any booster approach must be carefully considered in the light of the problems presented by the global TB epidemic. The ability of M. tuberculosis to infect an individual and remain latent for many years, perhaps as long as that person lives, is a key feature of the disease82,83. Current estimates indicate that as many as a third of the world's population could be latently infected with M. tuberculosis, with a 5% chance of developing the disease later in life1. This figure is an estimate and includes both a relatively low frequency of latently infected individuals in developed countries and, as eluded to above, a large reservoir of latent infection in TB-endemic regions. In addition to the fact that this pool of latent TB constitutes a considerable source of mycobacterial sensitization, it poses two theoretical problems for any booster vaccine strategy. The first is to design a booster vaccine that is not only effective against primary infection (for preventative use) but that is also effective in latently infected individuals who are expected to be present in any adult population in a TB-endemic region. Only such a vaccine could be expected to be broadly effective in the population as a whole and in particular to affect latently infected individuals, who seem to be at high risk of later disease. The second is that any vaccine that would be given to latently infected individuals must be designed to minimize immunopathology. Recent progress in vaccine delivery systems, such as the development of novel adjuvants29,31,84,85 and viral vectors86, allows efficient targeting of the immune response and should enable future vaccines to be tailored to strike a balance between the induction of strong, protective Th1 responses and amplification of disease — as was unfortunately so clearly shown with the first attempt at a therapeutic vaccine in the early twentieth century (the so-called Koch phenomenon)87.
New vaccines that are effective against primary infection have now entered the early phases of clinical assessment24,84,88,89,90 and some will also be evaluated as boosters for adults. The burning questions for current TB vaccine research have therefore become: can these vaccines boost BCG-induced immunity to higher levels in areas with extensive sensitization from environmental exposure; and are such vaccines safe and effective in latently infected individuals? The answers to these questions will define the course of TB vaccine development in the future.
References
Anon . Global Tuberculosis Control. WHO Report 2001. 181 (World Health Organization, Geneva, 2001).
Calmette, A. & Plotz, H. Protective inoculation against tuberculosis with BCG. Am. Rev. Tuberc. 19, 567–572 (1929).
Calmette, A. Au sujet des accidents de Lübeck chez des nourissons vaccinés au BCG. Presse Med. 44, 748–749 (1930).
Evans, C. C. Historical background. in Clinical Tuberculosis (ed. Davies, P. D. O.) 1–19 (Chapman and Hall Medical, London, 1994).
Smith, P. G. BCG vaccination. in Clinical Tuberculosis (ed. Davies, P. D. O.) 297–310 (Chapman and Hall Medical, London, 1994).
Behr, M. A. Correlation between BCG genomics and protective efficacy. Scand. J. Infect. Dis. 33, 249–252 (2001).
Oettinger, T., Jorgensen, M., Ladefoged, A., Haslov, K. & Andersen, P. Development of the Mycobacterium bovis BCG vaccine: review of the historical and biochemical evidence for a genealogical tree. Tuber. Lung Dis. 79, 243–250 (1999).
Anon . Fifteen year follow up of trial of BCG vaccines in south India for tuberculosis prevention. Indian J. Med. Res. 110, 56–69 (1999).
Sterne, J. A., Rodrigues, L. C. & Guedes, I. N. Does the efficacy of BCG decline with time since vaccination? Int. J. Tuberc. Lung Dis. 2, 200–207 (1998).
Zodpey, S. P., Shrikhande, S. N., Maldhure, B. R., Vasudeo, N. D. & Kulkarni, S. W. Effectiveness of Bacillus Calmette Guerin (BCG) vaccination in the prevention of childhood pulmonary tuberculosis: a case control study in Nagpur, India. Southeast Asian J. Trop. Med. Public Health 29, 285–288 (1998).
Lanckriet, C., Levy, B. D., Bingono, E., Siopathis, R. M. & Guerin, N. Efficacy of BCG vaccination of the newborn: evaluation by a follow-up study of contacts in Bangui. Int. J. Epidemiol. 24, 1042–1049 (1995).
Mittal, S. K., Aggarwal, V., Rastogi, A. & Saini, N. Does B.C.G. vaccination prevent or postpone the occurrence of tuberculous meningitis? Indian J. Pediatr. 63, 659–664 (1996).
Colditz, G. A. et al. The efficacy of bacillus Calmette–Guerin vaccination of newborns and infants in the prevention of tuberculosis: meta-analyses of the published literature. Pediatrics 96, 29–35 (1995).
Fine, P. E. Variation in protection by BCG: implications of and for heterologous immunity. Lancet 346, 1339–1345 (1995).
Kochi, A. Tuberculosis: distribution, risk factors, mortality. Immunobiology 191, 325–336 (1994).
Behr, M. A. & Small, P. M. Has BCG attenuated to impotence? Nature 389, 133–134 (1997).
Horwitz, M. A. & Harth, G. A new vaccine against tuberculosis affords greater survival after challenge than the current vaccine in the guinea pig model of pulmonary tuberculosis. Infect. Immun. 71, 1672–1679 (2003).
Pym, A. S. et al. Recombinant BCG exporting ESAT-6 confers enhanced protection against tuberculosis. Nature Med. 9, 533–539 (2003).
Conradt, P., Hess, J. & Kaufmann, S. H. Cytolytic T-cell responses to human dendritic cells and macrophages infected with Mycobacterium bovis BCG and recombinant BCG secreting listeriolysin. Microbes Infect. 1, 753–764 (1999).
Grode, L., Kursar, M., Fensterle, J., Kaufmann, S. H. & Hess, J. Cell-mediated immunity induced by recombinant Mycobacterium bovis Bacille Calmette–Guerin strains against an intracellular bacterial pathogen: importance of antigen secretion or membrane-targeted antigen display as lipoprotein for vaccine efficacy. J. Immunol. 168, 1869–1876 (2002).
Cole, S. T. et al. Deciphering the biology of Mycobacterium tuberculosis from the complete genome sequence. Nature 393, 537–544 (1998).
Wang, J. et al. Single mucosal, but not parenteral, immunization with recombinant adenoviral-based vaccine provides potent protection from pulmonary tuberculosis. J. Immunol. 173, 6357–6365 (2004).
McShane, H., Brookes, R., Gilbert, S. C. & Hill, A. V. Enhanced immunogenicity of CD4(+) T-cell responses and protective efficacy of a DNA-modified vaccinia virus Ankara prime-boost vaccination regimen for murine tuberculosis. Infect. Immun. 69, 681–686 (2001).
McShane, H. et al. Recombinant modified vaccinia virus Ankara expressing antigen 85A boosts BCG-primed and naturally acquired antimycobacterial immunity in humans. Nature Med. 10, 1240–1244 (2004).
Skeiky, Y. A. et al. Differential immune responses and protective efficacy induced by components of a tuberculosis polyprotein vaccine, Mtb72F, delivered as naked DNA or recombinant protein. J. Immunol. 172, 7618–7628 (2004).
Doherty, T. M. et al. Comparative analysis of different vaccine constructs expressing defined antigens from Mycobacterium tuberculosis. J. Infect. Dis. 190, 2146–2153 (2004).
Weinrich Olsen, A., van Pinxteren, L. A., Meng Okkels, L., Birk Rasmussen, P. & Andersen, P. Protection of mice with a tuberculosis subunit vaccine based on a fusion protein of antigen 85B and ESAT-6. Infect. Immun. 69, 2773–2778 (2001).
Langermans, J. A. et al. Protection of macaques against Mycobacterium tuberculosis infection by a subunit vaccine based on a fusion protein of antigen 85B and ESAT-6. Vaccine 23, 2740–2750 (2005).
Lingnau, K. et al. Poly-L-arginine synergizes with oligodeoxynucleotides containing CpG-motifs (CpG-ODN) for enhanced and prolonged immune responses and prevents the CpG-ODN-induced systemic release of pro-inflammatory cytokines. Vaccine 20, 3498–3508 (2002).
da Fonseca, D. P., Frerichs, J., Singh, M., Snippe, H. & Verheul, A. F. Induction of antibody and T-cell responses by immunization with ISCOMS containing the 38-kilodalton protein of Mycobacterium tuberculosis. Vaccine 19, 122–131 (2000).
Holten-Andersen, L., Doherty, T. M., Korsholm, K. S. & Andersen, P. Combination of the cationic surfactant dimethyl dioctadecyl ammonium bromide and synthetic mycobacterial cord factor as an efficient adjuvant for tuberculosis subunit vaccines. Infect. Immun. 72, 1608–1617 (2004).
Aronson, N. E. et al. Long-term efficacy of BCG vaccine in American Indians and Alaska Natives: a 60-year follow-up study. JAMA 291, 2086–2091 (2004).
Hart, P. D. & Sutherland, I. BCG and vole bacillus vaccines in the prevention of tuberculosis in adolescence and early adult life. Br. Med. J. 2, 293–295 (1977).
Comstock, G. W., Woolpert, S. F. & Livesay, V. T. Tuberculosis studies in Muscogee County, Georgia. Twenty-year evaluation of a community trial of BCG vaccination. Public Health Rep. 91, 276–280 (1976).
Dye, C. A booster for tuberculosis vaccines. JAMA 291, 2127–2128 (2004).
Brooks, J. V., Frank, A. A., Keen, M. A., Bellisle, J. T. & Orme, I. M. Boosting vaccine for tuberculosis. Infect. Immun. 69, 2714–2717 (2001).
Brandt, L. et al. The protective effect of the Mycobacterium bovis BCG vaccine is increased by coadministration with the Mycobacterium tuberculosis 72-kilodalton fusion polyprotein Mtb72F in M. tuberculosis-infected guinea pigs. Infect. Immun. 72, 6622–6632 (2004).
Orme, I. M. Beyond BCG: the potential for a more effective TB vaccine. Mol. Med. Today 5, 487–492 (1999).
Smith, D. W. Protective effect of BCG in experimental tuberculosis. Adv. Tuberc. Res. 22, 1–97 (1985).
Orme, I. M., McMurray, D. N. & Belisle, J. T. Tuberculosis vaccine development: recent progress. Trends Microbiol. 9, 115–118 (2001).
Skeiky, Y. A. et al. T cell expression cloning of a Mycobacterium tuberculosis gene encoding a protective antigen associated with the early control of infection. J. Immunol. 165, 7140–7149 (2000).
Olsen, A. W., Hansen, P. R., Holm, A. & Andersen, P. Efficient protection against Mycobacterium tuberculosis by vaccination with a single subdominant epitope from the ESAT-6 antigen. Eur. J. Immunol. 30, 1724–1732 (2000).
Wilson, M. E., Fineberg, H. V. & Colditz, G. A. Geographic latitude and the efficacy of bacillus Calmette–Guerin vaccine. Clin. Infect. Dis. 20, 982–991 (1995).
Colditz, G. A. et al. Efficacy of BCG vaccine in the prevention of tuberculosis. Meta-analysis of the published literature. JAMA 271, 698–702 (1994).
Cole, S. T. & Barrell, B. G. Analysis of the genome of Mycobacterium tuberculosis H37Rv. Novartis Found. Symp. 217, 160–172 (1998).
Brosch, R. et al. Comparative genomics of the mycobacteria. Int. J. Med. Microbiol. 290, 143–152 (2000).
Chaparas, S. D., Maloney, C. J. & Hedrick, S. R. Specificity of tuberculins and antigens from various species of mycobacteria. Am. Rev. Respir. Dis. 101, 74–83 (1970).
Harboe, M., Mshana, R. N., Closs, O., Kronvall, G. & Axelsen, N. H. Cross-reactions between mycobacteria. II. Crossed immunoelectrophoretic analysis of soluble antigens of BCG and comparison with other mycobacteria. Scand. J. Immunol. 9, 115–124 (1979).
von Reyn, C. F. et al. Skin test reactions to Mycobacterium tuberculosis purified protein derivative and Mycobacterium avium sensitin among health care workers and medical students in the United States. Int. J. Tuberc. Lung Dis. 5, 1122–1128 (2001).
von Reyn, C. F. et al. Dual skin testing with Mycobacterium avium sensitin and purified protein derivative to discriminate pulmonary disease due to M. avium complex from pulmonary disease due to Mycobacterium tuberculosis. J. Infect. Dis. 177, 730–736 (1998).
Manabe, Y. C., Scott, C. P. & Bishai, W. R. Naturally attenuated, orally administered Mycobacterium microti as a tuberculosis vaccine is better than subcutaneous Mycobacterium bovis BCG. Infect. Immun. 70, 1566–1570 (2002).
Brooks, R. W., Parker, B. C., Gruft, H. & Falkinham, J. O., 3rd. Epidemiology of infection by nontuberculous mycobacteria. V. Numbers in eastern United States soils and correlation with soil characteristics. Am. Rev. Respir. Dis. 130, 630–633 (1984).
Kamala, T., Paramasivan, C. N., Herbert, D., Venkatesan, P. & Prabhakar, R. Immune response & modulation of immune response induced in the guinea-pigs by Mycobacterium avium complex (MAC) & M. fortuitum complex isolates from different sources in the south Indian BCG trial area. Indian J. Med. Res. 103, 201–211 (1996).
Black, G. F. et al. Patterns and implications of naturally acquired immune responses to environmental and tuberculous mycobacterial antigens in northern Malawi. J. Infect. Dis. 184, 322–329 (2001).
Black, G. F. et al. BCG-induced increase in interferon-γ response to mycobacterial antigens and efficacy of BCG vaccination in Malawi and the UK: two randomised controlled studies. Lancet 359, 1393–1401 (2002).
Weir, R. E. et al. Interferon-γ and skin test responses of schoolchildren in southeast England to purified protein derivatives from Mycobacterium tuberculosis and other species of mycobacteria. Clin. Exp. Immunol. 134, 285–294 (2003).
Floyd, S. et al. Kinetics of delayed-type hypersensitivity to tuberculin induced by bacille Calmette–Guerin vaccination in northern Malawi. J. Infect. Dis. 186, 807–814 (2002).
Black, G. F. et al. Relationship between IFN-γ and skin test responsiveness to Mycobacterium tuberculosis PPD in healthy, non-BCG-vaccinated young adults in Northern Malawi. Int. J. Tuberc. Lung Dis. 5, 664–672 (2001).
Miceli, I. et al. Evaluation of the effectiveness of BCG vaccination using the case-control method in Buenos Aires, Argentina. Int. J. Epidemiol. 17, 629–634 (1988).
al-Kassimi, F. A., al-Hajjaj, M. S., al-Orainey, I. O. & Bamgboye, E. A. Does the protective effect of neonatal BCG correlate with vaccine-induced tuberculin reaction? Am. J. Respir. Crit. Care Med. 152, 1575–1578 (1995).
Brewer, T. F. Preventing tuberculosis with bacillus Calmette–Guerin vaccine: a meta-analysis of the literature. Clin. Infect. Dis. 31, S64–S67 (2000).
Palmer, C. E. & Long, M. W. Effects of infection with atypical mycobacteria on BCG vaccination and tuberculosis. Am. Rev. Respir. Dis. 94, 553–568 (1966).
Ponnighaus, J. M. et al. Efficacy of BCG vaccine against leprosy and tuberculosis in northern Malawi. Lancet 339, 636–639 (1992).
Brosch, R., Gordon, S. V., Eiglmeier, K., Garnier, T. & Cole, S. T. Comparative genomics of the leprosy and tubercle bacilli. Res. Microbiol. 151, 135–142 (2000).
Grzybowski, S. & Dorken, E. Tuberculosis in Inuit. Ecol. Dis. 2, 145–148 (1983).
Brandt, L. et al. Failure of the Mycobacterium bovis BCG vaccine: some species of environmental mycobacteria block multiplication of BCG and induction of protective immunity to tuberculosis. Infect. Immun. 70, 672–678 (2002).
Francis, J. Natural and experimental tuberculosis in monkeys; with observations on immunization and chemotherapy. J. Comp. Pathol. 66, 123–135 (1956).
Siebenmann, C. O. Effect of BCG vaccination and chemotherapy on experimental tuberculosis in mice. J. Immunol. 67, 137–149 (1951).
Lozes, E. et al. Cross-reactive immune responses against Mycobacterium bovis BCG in mice infected with non-tuberculous mycobacteria belonging to the MAIS-Group. Scand. J. Immunol. 46, 16–26 (1997).
Buddle, B. M., Wards, B. J., Aldwell, F. E., Collins, D. M. & de Lisle, G. W. Influence of sensitisation to environmental mycobacteria on subsequent vaccination against bovine tuberculosis. Vaccine 20, 1126–1133 (2002).
de Lisle, G. W., Wards, B. J., Buddle, B. M. & Collins, D. M. The efficacy of live tuberculosis vaccines after presensitization with Mycobacterium avium. Tuberculosis (Edinb.) 85, 73–79 (2005).
Demangel, C., Garnier, T., Rosenkrands, I. & Cole, S. T. Differential effects of prior exposure to environmental mycobacteria on vaccination with Mycobacterium bovis BCG or a recombinant BCG strain expressing RD1 antigens. Infect. Immun. 73, 2190–2196 (2005).
Palmer, C. E. BCG vaccination and tuberculin allergy. Lancet 1, 935–940 (1952).
Baily, G. V. Tuberculosis prevention Trial, Madras. Indian J. Med. Res. 72, S1–S74 (1980).
Guld, J., Waaler, H., Sundaresan, T. K., Kaufmann, P. C. & ten Dam, H. G. The duration of BCG-induced tuberculin sensitivity in children, and its irrelevance for revaccination. Results of two 5-year prospective studies. Bull. World Health Org. 39, 829–836 (1968).
Horwitz, O. & Bunch-Christensen, K. Correlation between tuberculin sensitivity after 2 months and 5 years among BCG vaccinated subjects. Bull. World Health Org. 47, 49–58 (1972).
Fine, P. E., Sterne, J. A., Ponnighaus, J. M. & Rees, R. J. Delayed-type hypersensitivity, mycobacterial vaccines and protective immunity. Lancet 344, 1245–1249 (1994).
Gomes, M. G., Franco, A. O., Gomes, M. C. & Medley, G. F. The reinfection threshold promotes variability in tuberculosis epidemiology and vaccine efficacy. Proc. Biol. Sci. 271, 617–623 (2004).
Williams, A. et al. Evaluation of vaccines in the EU TB Vaccine Cluster using a guinea pig aerosol infection model of tuberculosis. Tuberculosis (Edinb.) 85, 29–38 (2005).
Reed, S. G., Alderson, M. R., Dalemans, W., Lobet, Y. & Skeiky, Y. A. Prospects for a better vaccine against tuberculosis. Tuberculosis (Edinb.) 83, 213–219 (2003).
van Rie, A. et al. Exogenous reinfection as a cause of recurrent tuberculosis after curative treatment. New Engl. J. Med. 341, 1174–1179 (1999).
O'Regan, A. & Joyce-Brady, M. Latent tuberculosis may persist for over 40 years. BMJ 323, 635 (2001).
Lillebaek, T. et al. Molecular evidence of endogenous reactivation of Mycobacterium tuberculosis after 33 years of latent infection. J. Infect. Dis. 185, 401–404 (2002).
Doherty, T. M. & Andersen, P. Tuberculosis vaccine development. Curr. Opin. Pulm. Med. 8, 183–187 (2002).
Hogarth, P. J., Jahans, K. J., Hecker, R., Hewinson, R. G. & Chambers, M. A. Evaluation of adjuvants for protein vaccines against tuberculosis in guinea pigs. Vaccine 21, 977–982 (2003).
Feng, C. G., Blanchard, T. J., Smith, G. L., Hill, A. V. & Britton, W. J. Induction of CD8+ T-lymphocyte responses to a secreted antigen of Mycobacterium tuberculosis by an attenuated vaccinia virus. Immunol. Cell Biol. 79, 569–575 (2001).
Rook, G. A. & Stanford, J. L. The Koch phenomenon and the immunopathology of tuberculosis. Curr. Top. Microbiol. Immunol. 215, 239–262 (1996).
Anon . New TB vaccine trials set to start in Britain [online], <http://www.aegis.com/news/re/2001/RE011114.html> (2001).
Fruth, U. & Young, D. Prospects for new TB vaccines: Stop TB working group on TB vaccine development. Int. J. Tuberc. Lung Dis. 8, 151–155 (2004).
Thomson, J. New TB vaccines to be tested. Nature Med. 12, 1263 (2001).
Horwitz, M. A., Harth, G., Dillon, B. J. & Maslesa-Galic, S. Recombinant bacillus calmette-guerin (BCG) vaccines expressing the Mycobacterium tuberculosis 30-kDa major secretory protein induce greater protective immunity against tuberculosis than conventional BCG vaccines in a highly susceptible animal model. Proc. Natl Acad. Sci. USA 97, 13853–13858 (2000).
Goonetilleke, N. P. et al. Enhanced immunogenicity and protective efficacy against Mycobacterium tuberculosis of bacille Calmette–Guerin vaccine using mucosal administration and boosting with a recombinant modified vaccinia virus Ankara. J. Immunol. 171, 1602–1609 (2003).
Acknowledgements
The authors would like to thank P. Fine for very helpful discussions and sharing unpublished data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Related links
DATABASES
Entrez
CDC Infectious Disease Information
FURTHER INFORMATION
Peter Andersen and T. Mark Doherty's department website
Global Fund to Fight AIDS, TB and Malaria
Rights and permissions
About this article
Cite this article
Andersen, P., Doherty, T. The success and failure of BCG — implications for a novel tuberculosis vaccine. Nat Rev Microbiol 3, 656–662 (2005). https://doi.org/10.1038/nrmicro1211
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrmicro1211
This article is cited by
-
Engineering potyvirus-like particles to display multiple copies of tuberculosis antigens
Biotechnology and Bioprocess Engineering (2024)
-
Bacillus Calmette-Guérin (BCG)-Induced Protection in Brain Disorders
Inflammation (2024)
-
Phosphatidylinositolmannoside vaccination induces lipid-specific Th1-responses and partially protects guinea pigs from Mycobacterium tuberculosis challenge
Scientific Reports (2023)
-
Safety and Immunogenicity of the ID93 + GLA-SE Tuberculosis Vaccine in BCG-Vaccinated Healthy Adults: A Randomized, Double-Blind, Placebo-Controlled Phase 2 Trial
Infectious Diseases and Therapy (2023)
-
Nanocages engineered from Bacillus Calmette-Guerin facilitate protective Vγ2Vδ2 T cell immunity against Mycobacterium tuberculosis infection
Journal of Nanobiotechnology (2022)