Abstract
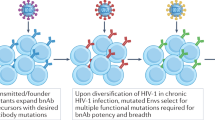
Eliciting protective neutralizing antibodies (NAbs) against HIV-1 is daunting because of the extensive genetic and antigenic diversity of HIV-1. Moreover, broad and potent responses are uncommon even during persistent infection, with only a subset of adults developing broadly neutralizing antibodies (bNAbs) that recognize viral variants from different HIV-1 clades1,2,3,4,5,6,7,8. It is not known whether bNAbs can also arise in HIV-1–infected infants, who typically progress to disease faster than adults9, presumably in part due to an immature immune system10. Here, we show that bNAbs develop at least as commonly in infants as in adults. Cross-clade NAb responses were detected in 20/28 infected infants, in some cases within 1 year of infection. Among infants with breadth of responses within the top quartile, neutralization of tier 2 or 3 variants from multiple clades was detected at 20 months after infection. These findings suggest that, even in early life, there is sufficient B cell functionality to mount bNAbs against HIV-1. Additionally, the relatively early appearance of bNAbs in infants may provide a unique setting for understanding the pathways of B cell maturation leading to bNAbs.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Sather, D.N. et al. Factors associated with the development of cross-reactive neutralizing antibodies during human immunodeficiency virus type 1 infection. J. Virol. 83, 757–769 (2009).
Gray, E.S. et al. The neutralization breadth of HIV-1 develops incrementally over four years and is associated with CD4+ T cell decline and high viral load during acute infection. J. Virol. 85, 4828–4840 (2011).
Mikell, I. et al. Characteristics of the earliest cross-neutralizing antibody response to HIV-1. PLoS Pathog. 7, e1001251 (2011).
Simek, M.D. et al. Human immunodeficiency virus type 1 elite neutralizers: individuals with broad and potent neutralizing activity identified by using a high-throughput neutralization assay together with an analytical selection algorithm. J. Virol. 83, 7337–7348 (2009).
Piantadosi, A. et al. Breadth of neutralizing antibody response to human immunodeficiency virus type 1 is affected by factors early in infection but does not influence disease progression. J. Virol. 83, 10269–10274 (2009).
van Gils, M.J., Euler, Z., Schweighardt, B., Wrin, T. & Schuitemaker, H. Prevalence of cross-reactive HIV-1–neutralizing activity in HIV-1-infected patients with rapid or slow disease progression. AIDS 23, 2405–2414 (2009).
Doria-Rose, N.A. et al. Breadth of human immunodeficiency virus-specific neutralizing activity in sera: clustering analysis and association with clinical variables. J. Virol. 84, 1631–1636 (2010).
Hraber, P. et al. Prevalence of broadly neutralizing antibody responses during chronic HIV-1 infection. AIDS 28, 163–169 (2014).
Richardson, B.A. et al. Comparison of human immunodeficiency virus type 1 viral loads in Kenyan women, men, and infants during primary and early infection. J. Virol. 77, 7120–7123 (2003).
Siegrist, C.A. Neonatal and early life vaccinology. Vaccine 19, 3331–3346 (2001).
Nduati, R. et al. Effect of breastfeeding and formula feeding on transmission of HIV-1: a randomized clinical trial. J. Am. Med. Assoc. 283, 1167–1174 (2000).
Seaman, M.S. et al. Tiered categorization of a diverse panel of HIV-1 Env pseudoviruses for assessment of neutralizing antibodies. J. Virol. 84, 1439–1452 (2010).
Cortez, V., Odem-Davis, K., McClelland, R.S., Jaoko, W. & Overbaugh, J. HIV-1 superinfection in women broadens and strengthens the neutralizing antibody response. PLoS Pathog. 8, e1002611 (2012).
Blish, C.A., Nedellec, R., Mandaliya, K., Mosier, D.E. & Overbaugh, J. HIV-1 subtype A envelope variants from early in infection have variable sensitivity to neutralization and to inhibitors of viral entry. AIDS 21, 693–702 (2007).
Blish, C.A. et al. Cross-subtype neutralization sensitivity despite monoclonal antibody resistance among early subtype A, C, and D envelope variants of human immunodeficiency virus type 1. J. Virol. 83, 7783–7788 (2009).
Wu, X. et al. Neutralization escape variants of human immunodeficiency virus type 1 are transmitted from mother to infant. J. Virol. 80, 835–844 (2006).
Lynch, J.B. et al. The breadth and potency of passively acquired human immunodeficiency virus type 1–specific neutralizing antibodies do not correlate with the risk of infant infection. J. Virol. 85, 5252–5261 (2011).
Blish, C.A., Nguyen, M.-A. & Overbaugh, J. Enhancing exposure of HIV-1 neutralization epitopes through mutations in gp41. PLoS Med. 5, e9 (2008).
Walker, L.M. et al. Broad and potent neutralizing antibodies from an African donor reveal a new HIV-1 vaccine target. Science 326, 285–289 (2009).
Walker, L.M. et al. Broad neutralization coverage of HIV by multiple highly potent antibodies. Nature 477, 466–470. 10.1038/nature10373 (2011).
Wu, X. et al. rational design of envelope identifies broadly neutralizing human monoclonal antibodies to HIV-1. Science 329, 856–861 (2010).
Huang, J. et al. Broad and potent neutralization of HIV-1 by a gp41-specific human antibody. Nature 491, 406–412 (2012).
Georgiev, I.S. et al. Delineating antibody recognition in polyclonal sera from patterns of HIV-1 isolate neutralization. Science 340, 751–756 (2013).
Scharf, O. et al. Immunoglobulin G3 from polyclonal human immunodeficiency virus (HIV) immune globulin is more potent than other subclasses in neutralizing HIV type 1. J. Virol. 75, 6558–6565 (2001).
Cavacini, L.A. et al. Influence of heavy chain constant regions on antigen binding and HIV-1 neutralization by a human monoclonal antibody. J. Immunol. 155, 3638–3644 (1995).
Baba, T.W. et al. Human neutralizing monoclonal antibodies of the IgG1 subtype protect against mucosal simian-human immunodeficiency virus infection. Nat. Med. 6, 200–206 (2000).
Ng, C.T. et al. Passive neutralizing antibody controls SHIV viremia and enhances B cell responses in infant macaques. Nat. Med. 16, 1117–1119 (2010).
Levesque, M.C. et al. Polyclonal B cell differentiation and loss of gastrointestinal tract germinal centers in the earliest stages of HIV-1 infection. PLoS Med. 6, e1000107 (2009).
Hoffenberg, S. et al. Identification of an HIV-1 clade A envelope that exhibits broad antigenicity and neutralization sensitivity and elicits antibodies targeting three distinct epitopes. J. Virol. 87, 5372–5383 (2013).
Lyumkis, D. et al. Cryo-EM structure of a fully glycosylated soluble cleaved HIV-1 envelope trimer. Science 342, 1484–1490 (2013).
Julien, J.-P. et al. Asymmetric recognition of the HIV-1 trimer by broadly neutralizing antibody PG9. Proc. Natl. Acad. Sci. USA 110, 4351–4356 (2013).
Sanders, R.W. et al. A next-generation cleaved, soluble HIV-1 Env trimer, BG505 SOSIP.664 gp140, expresses multiple epitopes for broadly neutralizing but not non-neutralizing antibodies. PLoS Pathog. 9, e1003618 (2013).
Moore, P.L. et al. Evolution of an HIV glycan–dependent broadly neutralizing antibody epitope through immune escape. Nat. Med. 18, 1688–1692. 10.1038/nm.2985 (2012).
Neilson, J.R. et al. Subtypes of human immunodeficiency virus type 1 and disease stage among women in Nairobi, Kenya. J. Virol. 73, 4393–4403 (1999).
Acknowledgements
We are grateful to the participants and staff of the Nairobi Breastfeeding Trial; P. Poignard (International AIDS Vaccine Initiative Neutralizing Antibody Center, The Scripps Research Institute) for providing envelope plasmids used for viruses in Supplementary Figure 2; P. Moore (Centre for HIV and Sexually Transmitted Infections, National Institute for Communicable Diseases of the National Health Laboratory Services, Johannesburg, South Africa) and G. Shaw (Perelman School of Medicine, University of Pennsylvania) for providing 7312-A and 7312-C1 plasmids; X. Wu and J. Mascola (Vaccine Research Center, US National Institutes of Health) for providing RSC3 and RSC3d371I plasmids; N. Doria-Rose, S. O'Dell and J. Mascola (Vaccine Research Center, US National Institutes of Health) for providing JRCSF N160K and N332A plasmids; S. Rainwater and B. Wang for assistance in obtaining viral clade information; V. Cortez for assistance in RSC3 protein purification; C. Milligan for sample database management; G. John-Stewart, I. Georgiev, V. Cortez, D. Lehman, C. Milligan and K. Ronen for helpful discussions; and B. Richardson for advice on statistical analyses. This work was supported by US National Institutes of Health grants AI076105 and AI103981.
Author information
Authors and Affiliations
Contributions
L.G. designed and performed experiments, analyzed data and wrote the manuscript. V.C. performed experiments. R.N. oversaw the cohort and clinical aspects. J.O. conceived of and oversaw the study and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–4 and Supplementary Tables 1 and 2 (PDF 1003 kb)
Rights and permissions
About this article
Cite this article
Goo, L., Chohan, V., Nduati, R. et al. Early development of broadly neutralizing antibodies in HIV-1–infected infants. Nat Med 20, 655–658 (2014). https://doi.org/10.1038/nm.3565
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.3565
This article is cited by
-
More than the Infinite Monkey Theorem: NHP Models in the Development of a Pediatric HIV Cure
Current HIV/AIDS Reports (2024)
-
Elevated binding and functional antibody responses to SARS-CoV-2 in infants versus mothers
Nature Communications (2023)
-
Early treatment regimens achieve sustained virologic remission in infant macaques infected with SIV at birth
Nature Communications (2022)
-
Serum IgG Profiling of Toddlers Reveals a Subgroup with Elevated Seropositive Antibodies to Viruses Correlating with Increased Vaccine and Autoantigen Responses
Journal of Clinical Immunology (2021)
-
Broadly neutralizing plasma antibodies effective against autologous circulating viruses in infants with multivariant HIV-1 infection
Nature Communications (2020)