Abstract
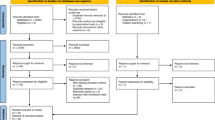
Peyronie’s disease continues to be poorly understood. We characterize the presenting features of Peyronie’s disease within a large cohort and elucidate the factors that correlate with surgical intervention. Univariate and multivariate analyses were performed on 1483 consecutive patients to assess pre-operative predictors of surgical intervention for Peyronie’s disease. Overall, 1263 patients met inclusion criteria. Mean age was 55.4 ± 11.1 years with a mean duration of disease at presentation of 33.2 ± 42.5 months. Mean primary curvature was 49.8 ± 20.8°. Primary ventral curvature was present in 11.4% and 36.5% of patient had a multiplanar curvature. During penile duplex ultrasound evaluation indentation/narrowing deformities were appreciated in 76.0%, hourglass deformity in 10.1%, and hinge effect in 33.0% of patients. Calcification was seen in 30.1% of patients. Operative intervention occurred in 35.3% of patients. Degree of primary curvature (1.03 OR, p < 0.001), hourglass deformity (1.82 OR, p = 0.01), decreased tunical elasticity (1.20 OR, p = 0.03), and prior intralesional collagenase clostridium histolyticum injections (2.94 OR, p < 0.001) predicted surgical correction on multivariate analysis. Compared to historical studies, we found a higher incidence of severe degree of curvature (27.5% >60°), indentation deformities, hinge-effect, multiplanar curvature and penile calcifications. Ultimately, predictors of surgical intervention included those with worse erectile function and more severe characteristics.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
Additional data are available from the corresponding author on request.
References
Al-Thakafi S, Al-Hathal N. Peyronie’s disease: a literature review on epidemiology, genetics, pathophysiology, diagnosis and work-up. Transl Androl Urol. 2016;5:280–9.
Devine CJ Jr., Somers KD, Jordan SG, Schlossberg SM. Proposal: trauma as the cause of the Peyronie’s lesion. J Urol. 1997;157:285–90.
Ziegelmann MJ, Bajic P, Levine LA. Peyronie’s disease: contemporary evaluation and management. Int J Urol. 2020;27:504–16.
Ziegelmann M, Bole R, Avant R, Yang D, Montgomery B, Trost L. Conservatively managed Peyronie’s disease-long-term survey results from patients undergoing nonsurgical and noninjection therapies. Urology. 2018;113:99–104.
Mulhall JP, Schiff J, Guhring P. An analysis of the natural history of Peyronie’s disease. J Urol. 2006;175:2115–8.
Williams JL, Thomas GG. The natural history of Peyronie’s disease. J Urol. 1970;103:75–6.
Ralph D, Gonzalez-Cadavid N, Mirone V, Perovic S, Sohn M, Usta M, et al. The management of Peyronie’s disease: evidence-based 2010 guidelines. J Sex Med. 2010;7:2359–74.
Manka MG, White LA, Yafi FA, Mulhall JP, Levine LA, Ziegelmann MJ. Comparing and contrasting Peyronie’s disease guidelines: points of consensus and deviation. J Sex Med. 2021;18:363–75.
Levine LA, Greenfield JM. Establishing a standardized evaluation of the man with Peyronie’s disease. Int J Impot Res. 2003;15:S103–12.
Pryor JP, Ralph DJ. Clinical presentations of Peyronie’s disease. Int J Impot Res. 2002;14:414–7.
Yafi FA, Hatzichristodoulou G, Delay KJ, Hellstrom WJ. Review of management options for patients with atypical Peyronie’s disease. Sex Med Rev. 2017;5:211–21.
Margolin EJ, Pagano MJ, Aisen CM, Onyeji IC, Stahl PJ. Beyond curvature: prevalence and characteristics of penile volume-loss deformities in men with Peyronie’s disease. Sex Med. 2018;6:309–15.
Ziegelmann MJ, Heslop D, Houlihan M, Bajic P, Helo S, Trost L, et al. The influence of indentation deformity on outcomes with intralesional collagenase clostridium histolyticum monotherapy for Peyronie’s disease. Urology. 2020;139:122–8.
Levine L, Rybak J, Corder C, Farrel MR. Peyronie’s disease plaque calcification–prevalence, time to identification, and development of a new grading classification. J Sex Med. 2013;10:3121–8.
Levine LA, Lenting EL. A surgical algorithm for the treatment of Peyronie’s disease. J Urol. 1997;158:2149–52.
Levine LA, Dimitriou RJ. A surgical algorithm for penile prosthesis placement in men with erectile failure and Peyronie’s disease. Int J Impot Res. 2000;12:147–51.
Nesbit RM. Congenital curvature of the phallus: report of three cases with description of corrective operation. J Urol. 1965;93:230–2.
Levine LA, Estrada CR. Human cadaveric pericardial graft for the surgical correction of Peyronie’s disease. J Urol. 2003;170:2359–62.
Gholami SS, Lue TF. Correction of penile curvature using the 16-dot plication technique: a review of 132 patients. J Urol. 2002;167:2066–9.
Wilson SK, Delk JR 2nd. A new treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol. 1994;152:1121–3.
Gelbard M, Goldstein I, Hellstrom WJ, McMahon CG, Smith T, Tursi J, et al. Clinical efficacy, safety and tolerability of collagenase clostridium histolyticum for the treatment of Peyronie disease in 2 large double-blind, randomized, placebo controlled phase 3 studies. J Urol. 2013;190:199–207.
Kadioglu A, Tefekli A, Erol B, Oktar T, Tunc M, Tellaloglu S. A retrospective review of 307 men with Peyronie’s disease. J Urol. 2002;168:1075–9.
Perimenis P, Athanasopoulos A, Gyftopoulos K, Katsenis G, Barbalias G. Peyronie’s disease: epidemiology and clinical presentation of 134 cases. Int Urol Nephrol. 2001;32:691–4.
Kadioglu A, Sanli O, Akman T, Canguven O, Aydin M, Akbulut F, et al. Factors affecting the degree of penile deformity in Peyronie disease: an analysis of 1001 patients. J Androl. 2011;32:502–8.
Moghalu OI, Das R, Horns J, Campbell A, Hotaling JM, Pastuszak AW. Trends in treatment of Peyronie’s disease in adult men in the United States from 2008 to 2017-results from an encounter and claims database. Int J Impot Res. 2022;34:280–8.
Valente EG, Vernet D, Ferrini MG, Qian A, Rajfer J, Gonzalez-Cadavid NF. L-arginine and phosphodiesterase (PDE) inhibitors counteract fibrosis in the Peyronie’s fibrotic plaque and related fibroblast cultures. Nitric Oxide. 2003;9:229–44.
Cakan M, Akman T, Oktar T, Gurkan L, Celtik M, Kadioglu A. The clinical characteristics of Peyronie’s patients with notching deformity. J Sex Med. 2007;4:1174–8.
Mulhall JP, Alex B, Choi JM. Predicting delay in presentation in men with Peyronie’s disease. J Sex Med. 2010;7:2226–30.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Study conceptualization was performed by DR, VW, and LL. Methodology, formal data collection, and investigation were performed by DR, VW, AB. Formal data analysis was performed by DR, VW, AB, and LL. Writing of original manuscript draft was performed by DR and AB. Review and editing of subsequent drafts were performed by VW and LL.
Corresponding author
Ethics declarations
Competing interests
The author declares no competing interests.
Ethical approval
Institutional Review Board approval was obtained.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Roadman, D., Wang, V., Beer, A. et al. A contemporary assessment of the evaluation and management of patients presenting to a tertiary medical center with Peyronie’s disease. Int J Impot Res 36, 118–124 (2024). https://doi.org/10.1038/s41443-023-00738-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-023-00738-w
This article is cited by
-
Unveiling treatment horizons and contemporary perspectives in Peyronie’s disease – take home messages from Laurance A. Levine special issue
International Journal of Impotence Research (2024)