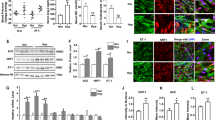
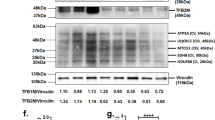
Abstract
In recent years, the increase in blood pressure at high altitudes has become an interesting topic among high-altitude researchers. In our animal studies using Wistar rats, we observed the existence of two rat populations that exhibit differential physiological responses during hypoxic exposure. These rats were classified as hypoxia-induced hypertensive rats and nonhypertensive rats. A decrease in nitric oxide levels was reported in different hypertension models associated with increased concentrations of asymmetric dimethylarginine (ADMA) and homocysteine, and we recently described an increase in arginase type II expression under hypoxia. ADMA and homocysteine decrease nitric oxide (NO) bioavailability; however, whether ADMA and homocysteine have a regulatory effect on arginase activity and therefore regulate another NO synthesis pathway is unknown. Therefore, the aim of this study was to measure basal ADMA and homocysteine levels in hypoxia-induced hypertensive rats and evaluate their effect on arginase II activity. Our results indicate that hypoxia-induced hypertensive rats presented lower nitric oxide concentrations than nonhypertensive rats, associated with higher concentrations of homocysteine and ADMA. Hypoxia-induced hypertensive rats also presented lower dimethylarginine dimethylaminohydrolase-2 and cystathionine β-synthase levels, which could explain the high ADMA and homocysteine levels. In addition, we observed that both homocysteine and ADMA had a significant effect on arginase II activation in the hypertensive rats. Therefore, we suggest that ADMA and homocysteine have dual regulatory effects on NO synthesis. The former has an inhibitory effect on eNOS, and the latter has a secondary activating effect on arginase II. We propose that arginase II is activated by AMDA and homocysteine in hypoxia-induced hypertensive rats.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout









Similar content being viewed by others
References
Parati G, Bilo G, Faini A. Changes in 24 h ambulatory blood pressure and effects of angiotensin II receptor blockade during acute and prolonged high-altitude exposure: a randomized clinical trial. Eur Heart J. 2014;35:3113–22.
Moraga FA, López I, Morales A, Soza D, Noack J. The effect of oxygen enrichment on cardiorespiratory and neuropsychological responses in workers with chronic intermittent exposure to high altitude (ALMA, 5,050 m). Front Physiol. 2018;23:187. 9
Norboo T, Stobdan T, Tsering N, Angchuk N, Tsering P, Ahmed I, et al. Prevalence of hypertension at high altitude: cross-sectional survey in Ladakh, Northern India. BMJ Open. 2015;5:e007026.
Negi PC, Bhardwaj R, Kandoria A, Asotra S, Ganju N, Marwaha R, et al. Epidemiological study of hypertension in natives of Spiti Valley in Himalayas and impact of hypobaric hypoxemia; a cross-sectional study. J Assoc Physicians India. 2012;60:21–5.
Levine BD, Zuckerman JH, de Filippi CR. Effect of high-altitude exposure in the elderly: the tenth mountain division study. Circulation. 1997;96:1224–32.
Baggish AL, Wolfel EE, Levine BD. Cardiovascular system. In: Swenson ER, Bartsch P, editors. High altitude: human adaptation to hypoxia. New York: Springer; 2014. p. 103–40.
López V, Siques P, Brito J, Vallejos C, Naveas N. Upregulation of arginase expression and activity in hypertensive rats exposed to chronic intermittent hypobaric hypoxia. High Alt Med Biol. 2009;10:373–81.
Landmesser U, Drexler H. Endothelial function and hypertension. Curr Opin Cardiol. 2007;22:316–20.
Ignarro LJ, Cirino G, Casini A, Napoli C. Nitric oxide as a signaling molecule in the vascular system: an overview. J Cardiovasc Pharm. 1999;34:879–86.
Klinger JR, Abman SH, Gladwin MT. Nitric oxide deficiency and endothelial dysfunction in pulmonary arterial hypertension. Am J Respir Crit Care Med. 2013;188:639–46.
Arrigoni FI, Vallance P, Haworth SG, Leiper JM. Metabolism of asymmetric dimethylarginines is regulated in the lung developmentally and with pulmonary hypertension induced by hypobaric hypoxia. Circulation. 2003;107:1195–201.
Pullamsetti S, Kiss L, Ghofrani HA, Voswinckel R, Haredza P. Increased levels and reduced catabolism of asymmetric and symmetric dimethylarginines in pulmonary hypertension. FASEB J. 2005;19:1175–7.
Sasaki A, Doi S, Mizutani S, Azuma H. Roles of accumulated endogenous nitric oxide synthase inhibitors, enhanced arginase activity, and attenuated nitric oxide synthase activity in endothelial cells for pulmonary hypertension in rats. Am J Physiol Lung Cell Mol Physiol. 2007;292:L1480–7.
Wierzbicki AS. Homocysteine and cardiovascular disease: a review of the evidence. Diab Vasc Dis Res. 2007;4:143–50.
Sun L, Sun S, Li Y, Pan W, Xie Y. Potential biomarkers predicting risk of pulmonary hypertension in congenital heart disease: the role of homocysteine and hydrogen sulfide. Chin Med J. 2014;127:893–9.
Böger RH, Maas R, Schulze F, Schwedhelm E. Asymmetric dimethylarginine (ADMA) as a prospective marker of cardiovascular disease and mortality-an update on patient populations with a wide range of cardiovascular risk. Pharm Res. 2009;60:481–7.
Lüneburg N, Siques P, Brito J, De La Cruz JJ, León-Velarde F, Hannemann J, et al. Long-term intermittent exposure to high altitude elevates asymmetric dimethylarginine in first exposed young adults. High Alt Med Biol. 2017;18:226–33.
Siques P, Brito J, Schwedhelm E, Pena E, León-Velarde F, De La Cruz JJ, et al. Asymmetric dimethylarginine at sea level is a predictive marker of hypoxic pulmonary arterial hypertension at high altitude. Front Physiol. 2019;27:651.
López V, Moraga FA, Llanos AJ, Ebensperger G, Taborda MI, Uribe E. Plasmatic concentrations of ADMA and Homocystein in Llama (Lama glama) and Regulation of Arginase Type II: an animal resistent to the development of pulmonary hypertension induced by hypoxia. Front Physiol. 2018;29:606.
Tran CT, Leiper JM, Vallance P. The DDAH/ADMA/NOS pathway. Atheroscler Suppl. 2003;4:33–40.
Xuan C, Xu LQ, Tian QW, Li H, Wang Q, He GW et al. Dimethylarginine dimethylaminohydrolase 2 (DDAH 2) gene polymorphism, asymmetric dimethylarginine (ADMA) concentrations, and risk of coronary artery disease: a case-control study. Sci Rep. 2016;6:33934.
Ding R, Lin S, Chen D. The association of cystathionine β synthase (CBS) T833C polymorphism and the risk of stroke: a meta-analysis. J Neurol Sci 2012;312:26–30.
Pernow J, Jung C. Arginase as a potential target in the treatment of cardiovascular disease: reversal of arginine steal? Cardiovasc Res. 2013;98:334–43.
Huynh NN, Chin-Dusting J. Amino acids, arginase and nitric oxide in vascular health. Clin Exp Pharm Physiol. 2006;33:1–8.
Boger RH. Asymmetric dimethylarginine, an endogenous inhibitor of nitric oxide synthase, explains the “L-arginine paradox” and acts as a novel cardiovascular risk factor. J Nutr. 2004;134:2842S–7S.
Johnson FK, Johnson RA, Peyton KJ, Durante W. Arginase inhibition restores arteriolar endothelial function in Dahl rats with salt-induced hypertension. Am J Physiol Regul Integr Comp Physiol. 2005;288:R1057–62.
Holowatz LA, Kenney WL. Up-regulation of arginase activity contributes to attenuated reflex cutaneous vasodilatation in hypertensive humans. J Physiol. 2007;581:863–72.
Sharma S, Kumar S, Sud N, Wiseman DA, Tian J. Alterations in lung arginine metabolism in lambs with pulmonary hypertension associated with increased pulmonary blood flow. Vasc Pharm. 2009;51:359–64.
Archibald RM. Colorimetric measurement of uric acid. Clin Chem. 1957;3:102–5.
Venkatakrishnan G, Shankar V, Reddy SR. Microheterogeneity of molecular forms of arginase in mammalian tissues. Indian J Biochem Biophys. 2003;40:400–8.
Bradford MM. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem. 1976;72:248–54.
Bredt DS, Schmidt HW. The citrulline assay, in methods in nitric oxide research. John Wiley & Sons: New York; 1996. p. 249–55.
Herrera EA, Reyes RV, Giussani DA, Riquelme RA, Sanhueza EM, Ebensperger G, et al. Carbon monoxide: a novel pulmonary artery vasodilator in neonatal llamas of the Andean altiplano. Cardiovasc Res. 2008;77:197–201.
Gorenflo M, Zheng C, Werle E, Fiehn W, Ulmer HE. Plasma levels of asymmetrical dimethyl-L-arginine in patients with congenital heart disease and pulmonary hypertension. J Cardiovasc Pharm. 2001;37:489–93.
Schulze F, Lenzen H, Hanefeld C, Bartling A, Osterziel KJ. Asymmetric dimethylarginine is an independent risk factor for coronary heart disease: results from the multicenter Coronary Artery Risk Determination investigating the Influence of ADMA Concentration (CARDIAC) study. Am Heart J. 2006;152:493.e1–8.
Jawalekar SL, Karnik A, Bhutey A. Risk of cardiovascular diseases in diabetes mellitus and serum concentration of asymmetrical dimethylarginine. Biochem Res Int. 2013;18:9430.
Iribarren C, Husson G, Sydow K, Wang BY, Sidney S. Asymmetric dimethyl-arginine and coronary artery calcification in young adults entering middle age: the CARDIA Study. Eur J Cardiovasc Prev Rehabil. 2007;14:222–9.
Landim MB, Casella Filho A, Chagas AC. Asymmetric dimethylarginine (ADMA) and endothelial dysfunction: implications for atherogenesis. Clinics. 2009;64:471–8.
Zaciragic A, Huskic J, Mulabegovic N, Avdagic N, Valjevac A. An assessment of correlation between serum asymmetric dimethylarginine and glycated haemoglobin in patients with type 2 diabetes mellitus. Bosn J Basic Med Sci. 2014;14:21–4.
Spasovski D, Latifi A, Osmani B, Krstevska-Balkanov S, Kafedizska I. Determination of the diagnostic values of asymmetric dimethylarginine as an indicator for evaluation of the endothelial dysfunction in patients with rheumatoid arthritis. Arthritis. 2013;2013:818037.
Alpoim PN, Godoi LC, Freitas LG, Gomes KB, Dusse LM. Assessment of L-arginine asymmetric 1 dimethyl (ADMA) in early-onset and late-onset (severe) preeclampsia. Nitric Oxide. 2013;33:81–2.
Guthikonda S, Haynes WG. Homocysteine: role and implications in atherosclerosis. Curr Atheroscler Rep. 2006;8:100–6.
Suhara T, Fukuo K, Yasuda O, Tsubakimoto M, Takemura Y. Homocysteine enhances endothelial apoptosis via upregulation of Fas-mediated pathways. Hypertension. 2004;43:1208–13.
Baszczuk A, Kopczynski Z, Thielemann A. Endothelial dysfunction in patients with primary hypertension and hyperhomocysteinemia. Postepy Hig Med Dosw. 2014;68:91–100.
Davis G, Baboolal N, Nayak S, McRae A. Sialic acid, homocysteine and CRP: potential markers for dementia. Neurosci Lett. 2009;465:282–4.
Cervellati C, Romani A, Seripa D, Cremonini E, Bosi C. Oxidative balance, homocysteine, and uric acid levels in older patients with Late Onset Alzheimer’s Disease or Vascular Dementia. J Neurol Sci. 2014;337:156–61.
Cervellati C, Romani A, Seripa D, Cremonini E, Bosi C, Magon S, et al. Systemic oxidative stress and conversion to dementia of elderly patients with mild cognitive impairment. Biomed Res Int. 2014;2014:309507.
Marcus J, Sarnak MJ, Menon V. Homocysteine lowering and cardiovascular disease risk: lost in translation. Can J Cardiol. 2007;23:707–10.
Sengwayo D, Moraba M, Motaung S. Association of homocysteinaemia with hyperglycaemia, dyslipidaemia, hypertension and obesity. Cardiovasc J Afr. 2013;24:265–9.
Narayanan N, Tyagi N, Shah A, Pagni S, Tyagi SC. Hyperhomocysteinemia during aortic ane urysm, a plausible role of epigenetics. Int J Physiol Pathophysiol Pharm. 2013;5:32–42.
Van Meurs JB, Pare G, Schwartz SM, Hazra A, Tanaka T. Common genetic loci influencing plasma homocysteine concentrations and their effect on risk of coronary artery disease. Am J Clin Nutr. 2013;98:668–76.
Sarov M, Not A, de Baulny HO, Masnou P, Vahedi K. A case of homocystinuria due to CBS gene mutations revealed by cerebral venous thrombosis. J Neurol Sci. 2014;336:257–9.
Zhou S, Zhang Z, Xu G. Notable epigenetic role of hyperhomocysteinemia in atherogenesis. Lipids Health Dis. 2014;21:134–8.
Alessio AC, Siqueira LH, Bydlowski SP, Hoehr NF, Annichino-Bizzacchi JM. Polymorphisms in the CBS gene and homocysteine, folate and vitamin B12 levels: association with polymorphisms in the MTHFR and MTRR genes in Brazilian children. Am J Med Genet. 2008;15:2598–602.
Yakub M, Moti N, Parveen S, Chaudhry B, Azam I. Polymorphisms in MTHFR, MS and CBS genes and homocysteine levels in a Pakistani population. PLoS ONE. 2012;7:33222–5.
Acknowledgements
We acknowledge CONICYT for a scientific research grant from FONDECYT (11075096).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
López, V., Uribe, E. & Moraga, F.A. Activation of arginase II by asymmetric dimethylarginine and homocysteine in hypertensive rats induced by hypoxia: a new model of nitric oxide synthesis regulation in hypertensive processes?. Hypertens Res 44, 263–275 (2021). https://doi.org/10.1038/s41440-020-00574-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-020-00574-1
Keywords
This article is cited by
-
Arginase: shedding light on the mechanisms and opportunities in cardiovascular diseases
Cell Death Discovery (2022)