Abstract
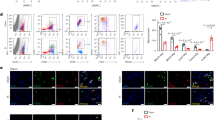
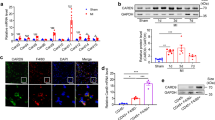
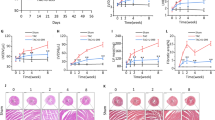
Following acute myocardial ischemia reperfusion (MIR), macrophages infiltrate damaged cardiac tissue and alter their polarization phenotype to respond to acute inflammation and chronic fibrotic remodeling. In this study we investigated the role of macrophages in post-ischemic myocardial fibrosis and explored therapeutic targets for myocardial fibrosis. Male mice were subjected to ligation of the left coronary artery for 30 min. We first detected the levels of chemokines in heart tissue that recruited immune cells infiltrating into the heart, and found that granulocyte-macrophage colony-stimulating factor (GMCSF) released by mouse cardiac microvascular endothelial cells (MCMECs) peaked at 6 h after reperfusion, and c-c motif chemokine ligand 2 (CCL2) released by GMCSF-induced macrophages peaked at 24 h after reperfusion. In co-culture of BMDMs with MCMECs, we demonstrated that GMCSF derived from MCMECs stimulated the release of CCL2 by BMDMs and effectively promoted the migration of BMDMs. We also confirmed that GMCSF promoted M1 polarization of macrophages in vitro, while GMCSF neutralizing antibodies (NTABs) blocked CCL2/CCR2 signaling. In MIR mouse heart, we showed that GMCSF activated CCL2/CCR2 signaling to promote NLRP3/caspase-1/IL-1β-mediated and amplified inflammatory damage. Knockdown of CC chemokine receptor 2 gene (CCR2−/−), or administration of specific CCR2 inhibitor RS102895 (5 mg/kg per 12 h, i.p., one day before MIR and continuously until the end of the experiment) effectively reduced the area of myocardial infarction, and down-regulated inflammatory mediators and NLRP3/Caspase-1/IL-1β signaling. Mass cytometry confirmed that M2 macrophages played an important role during fibrosis, while macrophage-depleted mice exhibited significantly reduced transforming growth factor-β (Tgf-β) levels in heart tissue after MIR. In co-culture of macrophages with fibroblasts, treatment with recombinant mouse CCL2 stimulated macrophages to release a large amount of Tgf-β, and promoted the release of Col1α1 by fibroblasts. This effect was diminished in BMDMs from CCR2−/− mice. After knocking out or inhibiting CCR2-gene, the levels of Tgf-β were significantly reduced, as was the level of myocardial fibrosis, and cardiac function was protected. This study confirms that the acute injury to chronic fibrosis transition after MIR in mice is mediated by GMCSF/CCL2/CCR2 signaling in macrophages through NLRP3 inflammatory cascade and the phenotype switching.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout









Similar content being viewed by others
References
Prabhu SD, Frangogiannis NG. The biological basis for cardiac repair after myocardial infarction: from inflammation to fibrosis. Circ Res. 2016;119:91–112.
Savarese G, Lund LH. Global public health burden of heart failure. Card Fail Rev. 2017;3:7–11.
Chiu J-J, Chien S. Effects of disturbed flow on vascular endothelium: pathophysiological basis and clinical perspectives. Physiol Rev. 2011;91:327–87.
Zuidema MY, Zhang C. Ischemia/reperfusion injury: the role of immune cells. World J Cardiol. 2010;2:325–32.
Venugopal H, Hanna A, Humeres C, Frangogiannis NG. Properties and functions of fibroblasts and myofibroblasts in myocardial infarction. Cells. 2022;11:1386.
Xu L, Sharkey D, Cantley LG. Tubular GMCSF promotes late MCP-1/CCR2-mediated fibrosis and inflammation after ischemia/reperfusion injury. J Am Soc Nephrol. 2019;30:1825–40.
Tan-Garcia A, Lai F, Yeong JPS, Irac SE, Ng PY, Msallam R, et al. Liver fibrosis and CD206+ macrophage accumulation are suppressed by anti-GMCSF therapy. JHEP Rep. 2019;2:100062.
Anzai A, Choi JL, He S, Fenn AM, Nairz M, Rattik S, et al. The infarcted myocardium solicits GMCSF for the detrimental oversupply of inflammatory leukocytes. J Exp Med. 2017;214:3293–310.
Peet C, Ivetic A, Bromage DI, Shah AM. Cardiac monocytes and macrophages after myocardial infarction. Cardiovasc Res. 2020;116:1101–12.
Duncan SE, Gao S, Sarhene M, Coffie JW, Linhua D, Bao X, et al. Macrophage activities in myocardial infarction and heart failure. Cardiol Res Pract. 2020;2020:4375127.
Chen B, Frangogiannis NG. Chemokines in myocardial infarction. J Cardiovasc Transl Res. 2021;14:35–52.
Georgakis MK, Bernhagen J, Heitman LH, Weber C, Dichgans M. Targeting the CCL2–CCR2 axis for atheroprotection. Eur Heart J. 2022;43:1799–808.
Xia Y, Frangogiannis NG. MCP-1/CCL2 as a therapeutic target in myocardial infarction and ischemic cardiomyopathy. Inflamm Allergy Drug Targets. 2007;6:101–7.
Flamini S, Sergeev P, Viana de Barros Z, Mello T, Biagioli M, Paglialunga M, et al. Glucocorticoid-induced leucine zipper regulates liver fibrosis by suppressing CCL2-mediated leukocyte recruitment. Cell Death Dis. 2021;12:421.
Braga TT, Correa-Costa M, Silva RC, Cruz MC, Hiyane MI, da Silva JS, et al. CCR2 contributes to the recruitment of monocytes and leads to kidney inflammation and fibrosis development. Inflammopharmacology. 2018;26:403–11.
Chung S, Overstreet JM, Li Y, Wang Y, Niu A, Wang S, et al. Tgf-β promotes fibrosis after severe acute kidney injury by enhancing renal macrophage infiltration. JCI insight. 2018;3:e123563.
Humeres C, Shinde AV, Hanna A, Alex L, Hernández SC, Li R, et al. Smad7 effects on Tgf-β and ErbB2 restrain myofibroblast activation and protect from postinfarction heart failure. J Clin Invest. 2022;132:e146926.
Zaidi Y, Aguilar EG, Troncoso M, Ilatovskaya DV, DeLeon-Pennell KY. Immune regulation of cardiac fibrosis post myocardial infarction. Cell Signal. 2021;77:109837.
Vierhout M, Ayoub A, Naiel S, Yazdanshenas P, Revill SD, Reihani A, et al. Monocyte and macrophage derived myofibroblasts: Is it fate? A review of the current evidence. Wound Repair Regen. 2021;29:548–62.
Meng X-M, Wang S, Huang X-R, Yang C, Xiao J, Zhang Y, et al. Inflammatory macrophages can transdifferentiate into myofibroblasts during renal fibrosis. Cell Death Dis. 2016;7:e2495.
Haider N, Boscá L, Zandbergen HR, Kovacic JC, Narula N, González-Ramos S, et al. Transition of macrophages to fibroblast-like cells in healing myocardial infarction. J Am Coll Cardiol. 2019;74:3124–35.
Ruberti OM, Rodrigues B. Estrogen deprivation and myocardial infarction: Role of aerobic exercise training, inflammation and metabolomics. Curr Cardiol Rev. 2020;16:292–305.
Liu K, Jin H, Tang M, Zhang S, Tian X, Zhang M, et al. Lineage tracing clarifies the cellular origin of tissue-resident macrophages in the developing heart. J Cell Biol. 2022;221:e202108093.
Nguyen PD, Hsiao ST, Sivakumaran P, Lim SY, Dilley RJ. Enrichment of neonatal rat cardiomyocytes in primary culture facilitates long-term maintenance of contractility in vitro. Am J Physiol Cell Physiol. 2012;303:C1220–8.
Kim Y, Nurakhayev S, Nurkesh A, Zharkinbekov Z, Saparov A. Macrophage polarization in cardiac tissue repair following myocardial infarction. Int J Mol Sci. 2021;22:2715.
Dick SA, Macklin JA, Nejat S, Momen A, Clemente-Casares X, Althagafi MG, et al. Self-renewing resident cardiac macrophages limit adverse remodeling following myocardial infarction. Nat Immunol. 2019;20:29–39.
Revelo XS, Parthiban P, Chen C, Barrow F, Fredrickson G, Wang H, et al. Cardiac resident macrophages prevent fibrosis and stimulate angiogenesis. Circ Res. 2021;129:1086–101.
Bonaventura A, Montecucco F, Dallegri F. Cellular recruitment in myocardial ischaemia/reperfusion injury. Eur J Clin Invest. 2016;46:590–601.
Shapouri‐Moghaddam A, Mohammadian S, Vazini H, Taghadosi M, Esmaeili SA, Mardani F, et al. Macrophage plasticity, polarization, and function in health and disease. J Cell Physiol. 2018;233:6425–40.
Cochain C, Rodero MP, Vilar J, Recalde A, Richart AL, Loinard C, et al. Regulation of monocyte subset systemic levels by distinct chemokine receptors controls post-ischaemic neovascularization. Cardiovasc Res. 2010;88:186–95.
Germano DB, Oliveira SB, Bachi ALL, Juliano Y, Novo NF, do Amaral JB, et al. Monocyte chemokine receptors as therapeutic targets in cardiovascular diseases. Immunol Lett. 2023;256-257:1–8.
Frangogiannis NG. The inflammatory response in myocardial injury, repair, and remodelling. Nat Rev Cardiol. 2014;11:255–65.
Sun K, Li Y-y, Jin J. A double-edged sword of immuno-microenvironment in cardiac homeostasis and injury repair. Signal Transduct Target Ther. 2021;6:79.
Burke RM, Villar KNB, Small EM. Fibroblast contributions to ischemic cardiac remodeling. Cell Signal. 2021;77:109824.
Murray PJ, Wynn TA. Protective and pathogenic functions of macrophage subsets. Nat Rev Immunol. 2011;11:723–37.
Jaguin M, Houlbert N, Fardel O, Lecureur V. Polarization profiles of human M-CSF-generated macrophages and comparison of M1-markers in classically activated macrophages from GM-CSF and M-CSF origin. Cell Immunol. 2013;281:51–61.
Chen B, Yang Y, Yang C, Duan J, Chen L, Lu K, et al. M2 macrophage accumulation contributes to pulmonary fibrosis, vascular dilatation, and hypoxemia in rat hepatopulmonary syndrome. J Cell Physiol. 2021;236:7682–97.
Xi S, Zheng X, Li X, Jiang Y, Wu Y, Gong J, et al. Activated hepatic stellate cells induce infiltration and formation of CD163+ macrophages via CCL2/CCR2 pathway. Front Med. 2021;8:627927.
Acknowledgements
The work was supported by the National Natural Science Foundation of China (82170263, 82200282), the National Key Research and Development Program of China (2021YFA0804904), the Natural Science Foundation of Hefei City (2022043).
Author information
Authors and Affiliations
Contributions
SCS and LKM designed the experiments. SCS and CG performed most of the experiments. JX, CC, XJX, BYH and MZ performed some experiments. SCS and MZ analyzed the results. SCS, CG and LKM wrote the paper with help from other authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shen, Sc., Xu, J., Cheng, C. et al. Macrophages promote the transition from myocardial ischemia reperfusion injury to cardiac fibrosis in mice through GMCSF/CCL2/CCR2 and phenotype switching. Acta Pharmacol Sin 45, 959–974 (2024). https://doi.org/10.1038/s41401-023-01222-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-023-01222-3