Abstract
Background
Emerging evidence suggests that a subset of Black men with National Comprehensive Cancer Network (NCCN) low-risk prostate cancer (PCa) may harbor high volume and genomically aggressive disease. However, limited, and ambiguous research exist to evaluate the risk of extreme Gleason reclassification in Black men with low-risk PCa.
Methods
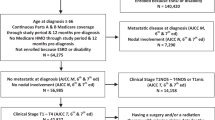
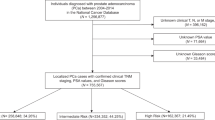
This retrospective cohort study included 45,674 low-risk PCa patients who underwent prostatectomy and were not on active surveillance, from National Cancer Database (NCDB). A propensity score matched-pair design was employed, and the final cohort was limited to 1:1 matched 12,340 patients. Gleason score reclassification was used as primary endpoint. As such, any migration to pathologic Gleason score ≥7(3 + 4) was identified as overall, whereas migration to ≥7(4 + 3) was defined as extreme reclassification. A conditional Poisson regression model was used to estimate the risk of reclassification. Whereas spline model was used to estimate the impact of increasing time to treatment as a non-linear function on Gleason reclassification between race group.
Results
Upon matching there were no differences in the baseline characteristics between race groups. In a matched cohort, higher proportion of low-risk Black men (6.6%) reported extreme reclassification to pathologic Gleason score than White men (5.0%), p < 0.001. In a conditional Poisson regression model adjusted for time to treatment, the risk of overall (RR = 1.09, 95% CI, 1.05–1.13, p < 0.001) and extreme (RR = 1.30, 95% CI, 1.12–1.50, p = 0.004) reclassification was significantly higher in Black men as compared to their White counterpart. In spline model, the probability of Gleason reclassification in Black men was elevated with increasing time to treatment, especially after 180 days (53% vs. 43% between Black and White men).
Conclusion
Risk of Gleason score reclassification is disparately elevated in Black men with low-risk PCa. Furthermore, time to treatment can non-linearly impact Gleason reclassification in Black men.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Wilt TJ, Jones KM, Barry MJ, Andriole GL, Culkin D, Wheeler T, et al. Follow-up of prostatectomy versus observation for early prostate cancer. N. Engl J Med. 2017;377:132–42.
Nevedomskaya E, Baumgart SJ, Haendler B. Recent advances in prostate cancer treatment and drug discovery. Int. J. Mol. Sci. 2018;19:1359.
Williams VL, Awasthi S, Fink AK, Pow-Sang JM, Park JY, Gerke T, et al. African-American men and prostate cancer-specific mortality: A competing risk analysis of a large institutional cohort, 1989-2015. Cancer Med. 2018;7:2160–71.
DeSantis CE, Miller KD, Goding Sauer A, Jemal A, Siegel RL. Cancer statistics for African Americans, 2019. CA: A Cancer J Clinicians. 2019;69:211–33.
Tsodikov A, Gulati R, de Carvalho TM, Heijnsdijk EAM, Hunter-Merrill RA, Mariotto AB, et al. Is prostate cancer different in black men? Answers from 3 natural history models. Cancer. 2017;123:2312–9.
Powell IJ, Bock CH, Ruterbusch JJ, Sakr W. Evidence supports a faster growth rate and/or earlier transformation to clinically significant prostate cancer in black than in white American men, and influences racial progression and mortality disparity. J Urol. 2010;183:1792–6.
Spratt DE, Zhang J, Santiago-Jiménez M, Dess RT, Davis JW, Den RB, et al. Development and validation of a novel integrated clinical-genomic risk group classification for localized prostate cancer. J Clin Oncol. 2018;36:581–90.
Mahal BA, Alshalalfa M, Spratt DE, Davicioni E, Zhao SG, Feng FY, et al. Prostate cancer genomic-risk differences between african-american and white men across Gleason scores. Eur Urol. 2019;75:1038–40.
Deka R, Parsons JK, Simpson DR, Riviere P, Nalawade V, Vitzthum LK, et al. African-American men with low-risk prostate cancer treated with radical prostatectomy in an equal-access health care system: Implications for active surveillance. Prostate Cancer Prostatic Dis. 2020;23:581–8.
Gökce MI, Sundi D, Schaeffer E, Pettaway C. Is active surveillance a suitable option for African American men with prostate cancer? A systemic literature review. Prostate Cancer Prostatic Dis. 2017;20:127–36.
Butler S, Muralidhar V, Chavez J, Fullerton Z, Mahal A, Nezolosky M, et al. Active surveillance for low-risk prostate cancer in Black patients. N. Engl J Med. 2019;380:2070–2.
Katz JE, Chinea FM, Patel VN, Balise RR, Venkatramani V, Gonzalgo ML, et al. Disparities in Hispanic/Latino and non-Hispanic Black men with low-risk prostate cancer and eligible for active surveillance: A population-based study. Prostate Cancer Prostatic Dis. 2018;21:533–8.
Schenk JM, Newcomb LF, Zheng Y, Faino AV, Zhu K, Nyame YA, et al. African American race is not associated with risk of reclassification during active surveillance: Results from the Canary prostate cancer active surveillance study. J Urol. 2020;203:727–33.
Mahal BA, Berman RA, Taplin ME, Huang FW. Prostate cancer-specific mortality across Gleason scores in black vs nonblack men. Jama. 2018;320:2479–81.
Sundi D, Ross AE, Humphreys EB, Han M, Partin AW, Carter HB, et al. African American men with very low-risk prostate cancer exhibit adverse oncologic outcomes after radical prostatectomy: Should active surveillance still be an option for them? J Clin Oncol. 2013;31:2991–7.
Deka R, Courtney PT, Parsons JK, Nelson TJ, Nalawade V, Luterstein E, et al. Association between African American race and clinical outcomes in men treated for low-risk prostate cancer with active surveillance. JAMA. 2020;324:1747–54.
Maurice MJ, Sundi D, Schaeffer EM, Abouassaly R. Risk of pathological upgrading and up staging among men with low risk prostate cancer varies by race: Results from the national cancer database. J Urol. 2017;197:627–31.
Awasthi S, Gerke T, Park JY, Asamoah FA, Williams VL, Fink AK, et al. Optimizing time to treatment to achieve durable biochemical disease control after surgery in prostate cancer: A multi-institutional cohort study. Cancer Epidemiol Biomark Prev. 2019;28:570–7.
Stokes WA, Hendrix LH, Royce TJ, Allen IM, Godley PA, Wang AZ, et al. Racial differences in time from prostate cancer diagnosis to treatment initiation: A population-based study. Cancer. 2013;119:2486–93.
Boffa DJ, Rosen JE, Mallin K, Loomis A, Gay G, Palis B, et al. Using the National cancer database for outcomes research: A review. JAMA Oncol. 2017;3:1722–8.
Flanagin A, Frey T, Christiansen SL. Updated guidance on the reporting of race and ethnicity in medical and science journals. Jama. 2021;326:621–7.
Hall WH, Jani AB, Ryu JK, Narayan S, Vijayakumar S. The impact of age and comorbidity on survival outcomes and treatment patterns in prostate cancer. Prostate Cancer Prostatic Dis. 2005;8:22–30.
Sundi D, Kryvenko ON, Carter HB, Ross AE, Epstein JI, Schaeffer EM. Pathological examination of radical prostatectomy specimens in men with very low risk disease at biopsy reveals distinct zonal distribution of cancer in black American men. J Urol. 2014;191:60–7.
Mygatt JG, Cullen J, Streicher SA, Kuo HC, Chen Y, Young D, et al. Race, tumor location, and disease progression among low-risk prostate cancer patients. Cancer Med. 2020;9:2235–42.
Hoge C, Verma S, Lama DJ, Bergelson I, Haj-Hamed M, Maynor S, et al. Racial disparity in the utilization of multiparametric MRI–ultrasound fusion biopsy for the detection of prostate cancer. Prostate Cancer Prostatic Dis. 2020;23:567–72.
Dinh KT, Mahal BA, Ziehr DR, Muralidhar V, Chen YW, Viswanathan VB, et al. Incidence and predictors of upgrading and up staging among 10,000 contemporary patients with low risk prostate cancer. J Urol. 2015;194:343–9.
Singh RV, Agashe SR, Gosavi AV, Sulhyan KR. Interobserver reproducibility of Gleason grading of prostatic adenocarcinoma among general pathologists. Indian J Cancer. 2011;48:488–95.
Allsbrook WC Jr, Mangold KA, Johnson MH, Lane RB, Lane CG, Epstein JI. Interobserver reproducibility of Gleason grading of prostatic carcinoma: general pathologist. Hum Pathol. 2001;32:81–8.
Funding
This research was supported by the American Cancer Society MRSG‐17‐108‐01‐TBG (to KY), and P20‐CA233255 (to KY and TRR).
Author information
Authors and Affiliations
Contributions
Concept and study design—SA; KY. Data acquisition—VLW SA, KY, Analysis and Interpretation of data—SA, KY, JHC, and TRR. Original draft—SA, KY. Critical revision of paper BM, JYP, JHC, VLW, AE, SOM, JMP, GLY, WKK, DYL, JZ, TRR, and KY. Statistical analysis—SA, JHC. Supervision—JZ, TRR, and KY.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Awasthi, S., Mahal, B.A., Park, J.Y. et al. Substantial Gleason reclassification in Black men with national comprehensive cancer network low-risk prostate cancer – A propensity score analysis. Prostate Cancer Prostatic Dis 25, 547–552 (2022). https://doi.org/10.1038/s41391-022-00510-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-022-00510-z
This article is cited by
-
Tumor upgrading among very favorable intermediate-risk prostate cancer patients treated with robot-assisted radical prostatectomy: how can it impact the clinical course?
International Urology and Nephrology (2024)
-
Oncological outcomes of cribriform histology pattern in prostate cancer patients: a systematic review and meta-analysis
Prostate Cancer and Prostatic Diseases (2023)